SOMATIC SYMPTOM, BODILY DISTRESS and RELATED DISORDERS in CHILDREN and ADOLESCENTS 2019 Edition
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Somatoform Disorders – September 2017
CrackCast Show Notes – Somatoform Disorders – September 2017 www.canadiem.org/crackcast Chapter 103 – Somatoform disorders Episode overview 1. List 5 somatic symptom and related disorders 2. List 5 common presentations of conversion disorders 3. List 6 ddx of somatic symptom disorder Wisecracks 1. List 6 organic diseases that may be mistaken for somatoform disorders 2. Describe the treatment goals of somatoform disorders Somatoform disorders as a diagnosis has been eliminated from the DSM-5! The patient with functional neurological symptom disorder, what was termed conversion disorder previously, requires a careful and complete neurological examination. Rather than miss the subtle presentation of a neurological disorder, it may be appropriate to perform imaging and obtain neurological and psychiatric consultation. Do not assume that the patient with neurological deficits has a psychiatric disorder. Success with the SSD patient depends on establishing rapport with the patient and legitimizing their complaints to avoid a dysfunctional physician-patient interaction. • Avoid telling the SSD patient “it is all in your head” or “there is nothing wrong with you.” These patients are very sensitive to the idea that their suffering is being dismissed. • A useful approach is to discuss recent stressors with the patient and suggest to them that at times our bodies can be smarter than we are, telling us with physical symptoms that we need assistance. This approach alone may transform the ED visit from a standoff between physician and patient, to a grateful patient who develops greater insight and is amenable to referral. • Avoid prescribing unnecessary or addictive medications to the SSD patient. • If you suspect a diagnosis of SSD, refer the patient to primary care or psychiatry for further evaluation and treatment. -

Psychopathology and Somatic Complaints: a Cross-Sectional Study with Portuguese Adults
healthcare Article Psychopathology and Somatic Complaints: A Cross-Sectional Study with Portuguese Adults Joana Proença Becker 1,*, Rui Paixão 1 and Manuel João Quartilho 2 1 Faculty of Psychology and Education Sciences, University of Coimbra, 3000-115 Coimbra, Portugal; [email protected] 2 Faculty of Medicine, University of Coimbra, 3000-548 Coimbra, Portugal; [email protected] * Correspondence: [email protected] or [email protected]; Tel.: +351-910741887 Abstract: (1) Background: Functional somatic symptoms (FSS) are physical symptoms that cannot be fully explained by medical diagnosis, injuries, and medication intake. More than the presence of unexplained symptoms, this condition is associated with functional disabilities, psychological distress, increased use of health services, and it has been linked to depressive and anxiety disorders. Recognizing the difficulty of diagnosing individuals with FSS and the impact on public health systems, this study aimed to verify the concomitant incidence of psychopathological symptoms and FSS in Portugal. (2) Methods: For this purpose, 93 psychosomatic outpatients (91.4% women with a mean age of 53.9 years old) and 101 subjects from the general population (74.3% women with 37.8 years old) were evaluated. The survey questionnaire included the 15-item Patient Health Questionnaire, the 20-Item Short Form Survey, the Brief Symptom Inventory, the Depression, Anxiety and Stress Scale, and questions on sociodemographic and clinical characteristics. (3) Results: Increases in FSS severity were correlated with higher rates of depression, anxiety, and stress symptoms. The findings also suggest that increased rates of FSS are associated with lower educational level and Citation: Becker, J.P.; Paixão, R.; female gender. -

The Clinical Presentation of Psychotic Disorders Bob Boland MD Slide 1
The Clinical Presentation of Psychotic Disorders Bob Boland MD Slide 1 Psychotic Disorders Slide 2 As with all the disorders, it is preferable to pick Archetype one “archetypal” disorder for the category of • Schizophrenia disorder, understand it well, and then know the others as they compare. For the psychotic disorders, the diagnosis we will concentrate on will be Schizophrenia. Slide 3 A good way to organize discussions of Phenomenology phenomenology is by using the same structure • The mental status exam as the mental status examination. – Appearance –Mood – Thought – Cognition – Judgment and Insight Clinical Presentation of Psychotic Disorders. Slide 4 Motor disturbances include disorders of Appearance mobility, activity and volition. Catatonic – Motor disturbances • Catatonia stupor is a state in which patients are •Stereotypy • Mannerisms immobile, mute, yet conscious. They exhibit – Behavioral problems •Hygiene waxy flexibility, or assumption of bizarre • Social functioning – “Soft signs” postures as most dramatic example. Catatonic excitement is uncontrolled and aimless motor activity. It is important to differentiate from substance-induced movement disorders, such as extrapyramidal symptoms and tardive dyskinesia. Slide 5 Disorders of behavior may involve Appearance deterioration of social functioning-- social • Behavioral Problems • Social functioning withdrawal, self neglect, neglect of • Other – Ex. Neuro soft signs environment (deterioration of housing, etc.), or socially inappropriate behaviors (talking to themselves in -

Days out of Role and Somatic, Anxious-Depressive, Hypo-Manic, and Psychotic-Like Symptom Dimensions in a Community Sample of Young Adults Jacob J
Crouse et al. Translational Psychiatry (2021) 11:285 https://doi.org/10.1038/s41398-021-01390-y Translational Psychiatry ARTICLE Open Access Days out of role and somatic, anxious-depressive, hypo-manic, and psychotic-like symptom dimensions in a community sample of young adults Jacob J. Crouse 1, Nicholas Ho 1,JanScott 1,2,3,4, Nicholas G. Martin 5, Baptiste Couvy-Duchesne 5,6,7, Daniel F. Hermens 8,RichardParker 5, Nathan A. Gillespie 9, Sarah E. Medland 5 and Ian B. Hickie 1 Abstract Improving our understanding of the causes of functional impairment in young people is a major global challenge. Here, we investigated the relationships between self-reported days out of role and the total quantity and different patterns of self-reported somatic, anxious-depressive, psychotic-like, and hypomanic symptoms in a community-based cohort of young adults. We examined self-ratings of 23 symptoms ranging across the four dimensions and days out of role in >1900 young adult twins and non-twin siblings participating in the “19Up” wave of the Brisbane Longitudinal Twin Study. Adjusted prevalence ratios (APR) and 95% confidence intervals (95% CI) quantified associations between impairment and different symptom patterns. Three individual symptoms showed significant associations with days out of role, with the largest association for impaired concentration. When impairment was assessed according to each symptom dimension, there was a clear stepwise relationship between the total number of somatic symptoms and the 1234567890():,; 1234567890():,; 1234567890():,; 1234567890():,; likelihood of impairment, while individuals reporting ≥4 anxious-depressive symptoms or five hypomanic symptoms had greater likelihood of reporting days out of role. -

Feldman Transcript Noncompli
“Most of the victims have to move on from these pathological relations”: Interview with Dr. Marc D. Feldman about medical child abuse October 1, 2020 Transcript by Julie Ann Lee. (Theme song – soft piano music) ABK: Hi, welcome to Noncompliant. I’m your host Anne Borden King. Dr. Marc D. Feldman is a clinical professor of Psychiatry and adjunct professor of Psychology at the University of Alabama in Tuscaloosa. A Distinguished Fellow of the American Psychiatric Association, he’s the author of 5 books and more than 100 peer reviewed articles in professional literature. Dr. Feldman is an international expert in Factitious Disorder, Munchausen Syndrome, Munchausen by proxy, and malingering. In his recent book, Dying to be Ill: True Stories of Medical Deception, Dr. Feldman with Gregory Yates has chronicled people’s acts and motivations in fabricating or inducing illness or injury in themselves or their dependents. Welcome to the show, Marc! MDF: Thank you for having me. ABK: Could you start by defining for listeners what Munchausen Syndrome is and Munchausen by proxy and Factitious Disorder - what are these conditions? MDF: Yeah, they’re all inter-related and so that causes a lot of confusion, not just in the general public but among professionals as well, at least at times, and that can be a daunting task to overcome. But to answer your question, Munchausen Syndrome is a term that was coined in 1951 to refer to people who feign, exaggerate or self-induce illness in order to get attention, get care and concern from people whom they don’t know how to mobilize in any other way. -

Factitious Disorder Imposed on Self
CHAPTER 14 Factitious Disorder Imposed on Self Jose M. Gonzalez, DPM HISTORY in this syndrome. Losing a loved one through sickness or death, or experiencing some other traumatic event can all Factitious disorder imposed on self, more commonly lead to development of this disorder. Neurocognitive as well known as Munchausen syndrome, was first coined in 1951. as neuroimaging studies are currently being conducted to Richard Asher first described the syndrome in his article in identify any abnormalities. The Lancet(1). In the article he described a pattern of self harm, where an individual fabricated histories, as well as SYMPTOMS AND DIAGNOSIS signs and symptoms of illness. Due to patients’ accounts of elaborate travel, as well as an uncanny ability to tell dramatic Patients with factitious disorder may feign medical or and untruthful stories, he named this syndrome after Baron psychiatric symptoms or illnesses (7). Even though von Munchausen. A German nobleman Hieronymus Karl patients may feign a symptom, they believe they have a Friedrich Freiherr von Munchausen fought for the Russian medical illness. Any type of symptom or disease may be Empire in the Russo-Turkish War. After retirement he simulated or induced. The more common ones include developed a following among the German aristocrats for abdominal pain, chest pain, hypoglycemia, infections, or his embellishment of tales based on his military career. seizures. Common factitious psychiatric symptoms include In 1785, German writer Rudolf Erich, created Baron depression, psychosis, and suicidal ideation (7). A key Munchausen, whose character is loosely based on Freiherr feature of factitious disorder is deception. There are several von Munchausen. -

Will the Real Pseudodementia Please Stand Up?
Will the Real Pseudodementia Please Stand Up? “Your reality, sir, is lies and balderdash and I'm delighted to say that I have no grasp of it whatsoever” Baron Munchausen By Ron Keren, MD, FRCPC seudodementia is a term that versible dementia which resolved underscored the risk of misdiag- Phas been widely adopted in with treatment and time. Kiloh nosing dementia in individuals clinical practice, yet vastly mis- asserted that endogenous depres- with a potentially reversible disor- understood. As its name suggests, sion was the most frequent cause der. However, over time, it pseudodementia infers a “func- of pseudodementia and cautioned became apparent that all the so- tional artifact” rather than a “true against misdiagnosing it as irre- called reversible dementias, espe- dementia” that is based on neu- versible dementia. He argued that cially the “pseudodementia of ropathological disease. Wernicke1 pseudodementia should be used depression,” were much less first coined the term in the 1880s as a descriptive term and not a prevalent than previously thought. to describe “chronic hysterical diagnosis. In 1979, Wells,4 while A meta-analysis of 39 studies states mimicking mental weak- reporting 10 patients with psy- from 1987 to 20027 identified ness.” It was not widely used chiatric disorders as examples of potentially reversible dementias until it was reintroduced by pseudodementia, was the first to in 9% of patients but only 0.6% Madden2 in 1952 to describe refer to pseudodementia as a actually reversed and only 0.31% patients with signs and symp- diagnosis. In 1981, Caine pro- toms of dementia that disap- posed diagnostic criteria for Table 1 peared with successful treatment pseudodementia (Table 1). -
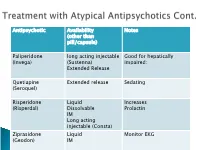
Antipsychotic Availability (Other Than Pill/Capsule) Notes Paliperidone
Antipsychotic Availability Notes (other than pill/capsule) Paliperidone long acting injectable Good for hepatically (Invega) (Sustenna) impaired; Extended Release Quetiapine Extended release Sedating (Seroquel) Risperidone Liquid Increases (Risperdal) Dissolvable Prolactin IM Long acting injectable (Consta) Ziprasidone Liquid Monitor EKG (Geodon) IM Supportive Psychotherapy Club House ACT services NAMI Vocational Rehab Nicotine counseling 1 (or more ) delusions Duration: 1 month or longer Criterion A for Schizophrenia has never been met. Functioning is not markedly impaired Behavior is not obviously odd or bizarre Features: Differential Diagnosis Prevalence: Obsessive-compulsive and ◦ lifetime 0.2 % related disorders ◦ Most frequent is persecutory Delirium • Males > females for Jealous major neurocognitive d/o type psychotic disorder due to • Function is generally better another medical condition than in schizophrenia substance-medication- • Familiar relationship with induced psychotic disorder schizophrenia and Schizophrenia & schizotypal Schizophreniform Depressive and bipolar d/o Schizoaffective Disorder Delusion types Erotomanic Grandiose Jealous Persecutory Somatic Mixed Unspecified • Substance Abuse • Dependence • Withdrawal ◦ Alcohol Divided into 2 ◦ Caffeine groups: ◦ Cannabis ◦ Hallucinogens (with separate ◦ Substance use categories for phencyclidine and other disorders hallucinogens) ◦ Substance-induced ◦ Inhalants disorders ◦ Opioids ◦ Sedatives, hypnotics, and anxiolytics ◦ Stimulants (amphetamine-type -

Pathological Skin Picking
Journal of Mind and Medical Sciences Volume 2 | Issue 1 Article 10 2015 Pathological Skin Picking: Case Presentation and Review of the Literature Maria Isabela Sarbu Victor Babes Hospital for Infectious and Tropical Diseases, [email protected] Mircea Tampa Carol Davila University of Medicine and Pharmacy, [email protected] Diana Leahu Victor Babes Hospital for Infectious and Tropical Diseases Cristina Raileanu Victor Babes Hospital for Infectious and Tropical Diseases Vasile Benea Victor Babes Hospital of Infectious and Tropical Diseases See next page for additional authors Follow this and additional works at: http://scholar.valpo.edu/jmms Part of the Medicine and Health Sciences Commons Recommended Citation Sarbu, Maria Isabela; Tampa, Mircea; Leahu, Diana; Raileanu, Cristina; Benea, Vasile; and Georgescu, Simona Roxana (2015) "Pathological Skin Picking: Case Presentation and Review of the Literature," Journal of Mind and Medical Sciences: Vol. 2 : Iss. 1 , Article 10. Available at: http://scholar.valpo.edu/jmms/vol2/iss1/10 This Case Presentation is brought to you for free and open access by ValpoScholar. It has been accepted for inclusion in Journal of Mind and Medical Sciences by an authorized administrator of ValpoScholar. For more information, please contact a ValpoScholar staff member at [email protected]. Pathological Skin Picking: Case Presentation and Review of the Literature Authors Maria Isabela Sarbu, Mircea Tampa, Diana Leahu, Cristina Raileanu, Vasile Benea, and Simona Roxana Georgescu This case presentation is -

An Association of Primary Psychiatric Disorders with Skin
rev colomb psiquiat. 2019;48(1):50–57 www.elsevier.es/rcp Review Article Psychodermatology: An Association of Primary Psychiatric Disorders With Skin Hassaan Tohid a,∗, Philip D. Shenefelt b, Waqas A. Burney c, Noorulain Aqeel d a Center for Applied Social Neuroscience, Napa State Hospital, Napa, University of California, Davis, California, United States b Department of Dermatology and Cutaneous Surgery, University of South Florida, Tampa, Florida, United States c Department of Dermatology, University of California, Davis, California, United States d Napa State Hospital, Napa, California, United States article info abstract Article history: The association of nervous system with skin is well documented. Many common psychiatric Received 8 February 2017 disorders can involve skin either directly or indirectly. We found an association of 13 primary Accepted 10 July 2017 psychiatric disorders leading to dermatological diseases, with association of 2 of 13 consid- ered to be idiopathic. Association of the mind and body has long been studied. Several skin Keywords: problems lead to psychological and psychiatric symptoms, however not all skin problems Psycho-dermatology lead to psychiatric symptoms. On the contrary, many primary psychiatric illnesses appear Dermal and mental health to have associated skin disorders. Depression and skin © 2017 Asociacion´ Colombiana de Psiquiatrıa.´ Published by Elsevier Espana,˜ S.L.U. All Anxiety and skin rights reserved. Schizophrenia and skin Psicodermatología: asociación de trastornos psiquiátricos primarios con la piel resumen Palabras clave: La asociación del sistema nervioso con la piel está bien documentada. Muchos trastornos Psicodermatología psiquiátricos comunes pueden implicar a la piel directa o indirectamente. Se encontró aso- Salud mental y de la piel ciación de 13 trastornos psiquiátricos primarios que llevan a enfermedades dermatológicas, Depresión y piel y de las 13, asociación de 2 consideradas idiopáticas. -

Factitious Disorder: a Case Report and Literature Review of Treatment
Case notes I Fictitious disorder Factitious disorder: a case report and literature review of treatment Georgios Mousailidis MD, MSc, PhD, Carlo Lazzari MD, Shafalica Bhan-Kotwal MD, MSc, Basavaraja Papanna MD, MSc, Ahmed Shoka MD Diagnosis of factitious disorder motivation for the behaviour factitious disorder, treatment. Our (FD) is frequently difficult and c. absence of external gain, such as main aim is to provide information on patients may present with avoiding legal responsibility or treatment of this disorder whose man- physical symptoms only, improving physical wellbeing, as in agement may be very challenging. psychiatric symptoms only or malingering. Case presentation with a combination of both. As The following subtypes are specified: A 22-year-old female single patient was long as the nature of the a. patients with primarily physical signs admitted in our adult psychiatric ward disease is so secretive and and symptoms, after an unsuccessful serious suicidal large-scale studies are almost b. patients with primarily psychologi- attempt, by taking a significant over- impossible, every case report is cal signs and symptoms, and dose of diazepam. The patient was important. Here, the authors c. mixed subtype. already diagnosed with Emotionally present a case of severe FD and Unstable Personality Disorder the therapeutic approach taken. Patients with FD deceive clinicians in (EUPD) and mild depression. There order to assume the sick role and be was history of emotional dysregulation he term ‘Munchausen syndrome’ treated as patients. They may just since adolescence and occasionally Twas introduced in 1951 by Asher1 exaggerate or false report symptoms self-harming behavior by cutting. -

When Munchausen Becomes Malingering: Factitious Disorders That Penetrate the Legal System
When Munchausen Becomes Malingering: Factitious Disorders That Penetrate the Legal System Stuart J. Eisendrath, MD Psychiatrists and other physicians are usually familiar with factitious disorders, but attorneys and judges usually are not. Cases involving factitious disorders may enter the civil legal system in a number of ways and cause incorrect judgments, financial costs, and inappropriate medical care if these disorders are not identi- fied. Psychiatric consultants may play a key role in identifying these cases and educating legal personnel about factitious disorders. This article describes three cases in which persons with factitious disorders entered the civil litigation sys- tem. The role of the psychiatrist in these cases is discussed. Clues to the identi- fication of factitious disorders are described. The article also discusses the differentiation of factitious disorders from malingering and other forms of abnor- mal illness behavior, such as conversion, hypochondriasis, and somatization disorders. The concepts of primary and secondary gain in relationship to illness behaviors are elaborated. Factitious disorders are those conditions iar with factitious disorders from their in which individuals actively create signs medical training, many attorneys and or symptoms of physical or psychological judges have had not any exposure to such disease states.' Although there are numer- cases. As these cases appear to be devel- ous reports of factitious psychological oping more frequently in legal and other disorders,"-" there is controversy about nonmedical settings,' it is important for the legitimacy of the diagnosk6 This pa- these nonpsychiatrists to become aware per will limit its focus to factitious phys- of the factitious disorders in order to deal ical disorders and how they may enter the with cases appropriately.