Resection of the Primary Osteosarcoma Terminates Self-Seeding and Facilitates Metastasis THESIS Presented in Partial Fulfillment
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Malignant Bone Tumors (Other Than Ewing’S): Clinical Practice Guidelines for Diagnosis, Treatment and Follow-Up by Spanish Group for Research on Sarcomas (GEIS)
Cancer Chemother Pharmacol DOI 10.1007/s00280-017-3436-0 ORIGINAL ARTICLE Malignant bone tumors (other than Ewing’s): clinical practice guidelines for diagnosis, treatment and follow-up by Spanish Group for Research on Sarcomas (GEIS) Andrés Redondo1 · Silvia Bagué2 · Daniel Bernabeu1 · Eduardo Ortiz-Cruz1 · Claudia Valverde3 · Rosa Alvarez4 · Javier Martinez-Trufero5 · Jose A. Lopez-Martin6 · Raquel Correa7 · Josefina Cruz8 · Antonio Lopez-Pousa9 · Aurelio Santos10 · Xavier García del Muro11 · Javier Martin-Broto10 Received: 7 July 2017 / Accepted: 15 September 2017 © The Author(s) 2017. This article is an open access publication Abstract Primary malignant bone tumors are uncommon of a localized bone tumor, with various techniques available and heterogeneous malignancies. This document is a guide- depending on the histologic type, grade and location of the line developed by the Spanish Group for Research on Sar- tumor. Chemotherapy plays an important role in some che- coma with the participation of different specialists involved mosensitive subtypes (such as high-grade osteosarcoma). in the diagnosis and treatment of bone sarcomas. The aim is In other subtypes, historically considered chemoresistant to provide practical recommendations with the intention of (such as chordoma or giant cell tumor of bone), new targeted helping in the clinical decision-making process. The diag- therapies have emerged recently, with a very significant effi- nosis and treatment of bone tumors requires a multidiscipli- cacy in the case of denosumab. Radiation therapy is usually nary approach, involving as a minimum pathologists, radi- necessary in the treatment of chordoma and sometimes of ologists, surgeons, and radiation and medical oncologists. other bone tumors. Early referral to a specialist center could improve patients’ survival. -

Sclerostin Inhibition Alleviates Breast Cancer–Induced Bone Metastases and Muscle Weakness
Sclerostin inhibition alleviates breast cancer–induced bone metastases and muscle weakness Eric Hesse, … , Hiroaki Saito, Hanna Taipaleenmäki JCI Insight. 2019. https://doi.org/10.1172/jci.insight.125543. Research In-Press Preview Bone biology Oncology Breast cancer bone metastases often cause a debilitating non-curable condition with osteolytic lesions, muscle weakness and a high mortality. Current treatment comprises chemotherapy, irradiation, surgery and anti-resorptive drugs that restrict but do not revert bone destruction. In metastatic breast cancer cells, we determined the expression of sclerostin, a soluble Wnt inhibitor that represses osteoblast differentiation and bone formation. In mice with breast cancer bone metastases, pharmacological inhibition of sclerostin using an anti-sclerostin antibody (Scl-Ab) reduced metastases without tumor cell dissemination to other distant sites. Sclerostin inhibition prevented the cancer-induced bone destruction by augmenting osteoblast-mediated bone formation and reducing osteoclast-dependent bone resorption. During advanced disease, NF-κB and p38 signaling was increased in muscles in a TGF-β1-dependent manner, causing muscle fiber atrophy, muscle weakness and tissue regeneration with an increase in Pax7-positive satellite cells. Scl-Ab treatment restored NF-κB and p38 signaling, the abundance of Pax7-positive cells and ultimately muscle function. These effects improved the overall health condition and expanded the life span of cancer-bearing mice. Together, these results demonstrate that pharmacological -

What Is Bone Cancer?
cancer.org | 1.800.227.2345 About Bone Cancer Overview and Types If you have been diagnosed with bone cancer or are worried about it, you likely have a lot of questions. Learning some basics is a good place to start. ● What Is Bone Cancer? Research and Statistics See the latest estimates for new cases of bone cancer and deaths in the US and what research is currently being done. ● Key Statistics About Bone Cancer ● What’s New in Bone Cancer Research? What Is Bone Cancer? The information here focuses on primary bone cancers (cancers that start in bones) that most often are seen in adults. Information on Osteosarcoma1, Ewing Tumors (Ewing sarcomas)2, and Bone Metastases3 is covered separately. Cancer starts when cells begin to grow out of control. Cells in nearly any part of the body can become cancer, and can then spread (metastasize) to other parts of the body. To learn more about cancer and how it starts and spreads, see What Is Cancer?4 1 ____________________________________________________________________________________American Cancer Society cancer.org | 1.800.227.2345 Bone cancer is an uncommon type of cancer that begins when cells in the bone start to grow out of control. To understand bone cancer, it helps to know a little about normal bone tissue. Bone is the supporting framework for your body. The hard, outer layer of bones is made of compact (cortical) bone, which covers the lighter spongy (trabecular) bone inside. The outside of the bone is covered with fibrous tissue called periosteum. Some bones have a space inside called the medullary cavity, which contains the soft, spongy tissue called bone marrow(discussed below). -
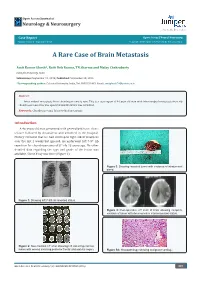
A Rare Case of Brain Metastasis
Open Access Journal of Neurology & Neurosurgery . key to the Researchers Case Report Open Access J Neurol Neurosurg Volume 1 Issue 2 - September 2016 Copyright © All rights are reserved by Katarina Matic A Rare Case of Brain Metastasis Amit Kumar Ghosh*, Rafit Deb Barma, TN Sharma and Malay Chakrabarty Calcutta University, India Submission: September 19, 2016; Published: September 28, 2016 *Corresponding author: Calcutta University, India, Tel: ; Email: Abstract Intracerebral metastasis from chondrosarcoma is rare. This is a case report of 46 year old man with intracerebral metastasis from rib chondrosarcoma who was operated and literature was reviewed. Keywords: Chondrosarcoma; Intracerebral metastasis Introduction A 46 years old man presented with generalised tonic clonic seizure followed by drowsiness and admitted in the hospital. History revealed that he had developed right sided weakness over the last 2 weeks but ignored. He underwent left 7-9th rib resection for chondrosarcoma of 8th rib 13 years ago. No other detailed data regarding the type and grade of the lesion was available. Chest X-ray was done (Figure 1). Figure 3: Showing resected tumor with evidence of intratumoral bleed. Figure 1: Showing left 7-9th rib resected status. Figure 4: Post-operative CT scan of brain showing complete excision of tumor with decompresive craniectomised status. Figure 2: Non-contrast CT scan showing left sided hyperdense lesion with edema involving posterior frontal and parietal region. Figure 5A: Histopathology showing malignant cartilage. Open Access J Neurol Neurosurg 1(2): OAJNN.MS.ID.55560 (2016) 001 Open Access Journal of Neurology & Neurosurgery differentiated chondrosarcoma (Figure 5A, 5B, 5C, 5D, 5E). -

Bone & Soft Tissue
14A ANNUAL MEETING ABSTRACTS and testicular atrophy with aspermatogenia (negative OCT3/OCT4 stain). There was 47 Comparison of Autopsy Findings of 2009 Pandemic Influenza evidence of acute multifocal bronchopneumonia and congestive heart failure. He carried A (H1N1) with Seasonal Influenza in Four Pediatric Patients two heterozygous mutations in ALMS1: 11316_11319delAGAG; R3772fs in exon 16 B Xu, JJ Woytash, D Vertes. State University of New York at Buffalo, Buffalo, NY; Erie and 8164C>T ter; R2722X in exon 10. County Medical Examiner’s Office, Buffalo, NY. Conclusions: This report describes previously undefined cardiac abnormalities in this Background: The swine-origin influenza A (H1N1) virus that emerged in humans rare multisystem disorder. Myofibrillar disarray is probably directly linked to ALMS1 in early 2009 has reached pandemic proportions and cause over 120 pediatric deaths mutation, while fibrosis in multiple organs may be a secondary phenomenon to gene nationwide. Studies in animal models have shown that the 2009 H1N1 influenza virus alteration. Whether and how intracellular trafficking or related signals lead to cardiac is more pathogenic than seasonal A virus, with more extensive virus replication and dysfunction is a subject for further research. shedding occurring the respiratory tract. Design: We report four cases of influenza A-associated deaths (two pandemic and two 45 Sudden Cardiac Death in Young Adults: An Audit of Coronial seasonal) in persons less than fifteen years of age who had no underlying health issues. Autopsy Findings Autopsy finding on isolation of virus from various tissue specimen, cocurrent bacterial A Treacy, A Roy, R Margey, JC O’Keane, J Galvin, A Fabre. -

Osteosarcoma
disease • canine lymphoma • brain tumor • congestive heart failure • feline lymphoma • primary lung tumor • mast cell tumor • kidney disease • transitional cell carcinoma • degenerative myelopathy • cognitive dysfunction syndrome • liver disease • seizures • osteosarcoma • hemangiosarcoma • nasal tumorsdiabetes • Common Signs of Pain • hyperadrenocorticism • hyperthyroidism • osteoarthritis • vestibular disease • canine lymphoma • brain tumor • congestive heart failure • feline lymphoma • Panting • Licking sore spot • primary lung tumor • mast cell tumor • kidney disease • transitional cell • Lameness • Muscle atrophy carcinoma • degenerative myelopathy • cognitive dysfunction syndrome • liver • Difficulty sleeping • Decreased appetite disease • seizures • osteosarcoma • hemangiosarcoma • nasal tumorsdiabetes • • Pacing • Vocalizing/yowling • hyperadrenocorticism • hyperthyroidism • osteoarthritis • vestibular disease • canine lymphoma • brain tumor • congestive heart failure • feline lymphoma • Abnormal posture • Reclusive Behavior • primary lung tumor • mast cell tumor • kidney disease • transitional cell • Body tensing • Aggressive Behavior carcinoma • degenerative myelopathy • cognitive dysfunction syndrome • liver • Poor grooming habits • Avoiding stairs/jumping disease • seizures • osteosarcoma • hemangiosarcoma • nasal tumorsdiabetes • • Tucked tail • Depressed • hyperadrenocorticism • hyperthyroidism • osteoarthritis • vestibular disease • Dilated Pupils • Unable to stand • canine lymphoma • brain tumor • congestive heart failure -

MSK News Summer 2021 Download
SUMMER 2021 SPECIAL ISSUE MSKNewsMEMORIAL SLOAN KETTERING CANCER CENTER Defeating Cancer’s Spread On the 50th anniversary of the War on Cancer, this SPECIAL ISSUE focuses on metastasis: What’s available now — and on the horizon — for patients like Ilene Thompson facing advanced disease. ALSO INSIDE: A Major Advance for Prostate Cancer Patients Seed and Soil: A Cancer Cell’s Journey How to Outsmart Tumor Evolution TABLE OF Dear MSK Community, These are the four most frightening words for a patient to hear: “Your cancer is back.” CONTENTS As we mark the 50th year of the War on Cancer and look to the future, our mission at Memorial Sloan Kettering is nothing less than conquering the most urgent challenge: preventing cancer’s spread. Also called metastasis, it causes 90 percent of cancer deaths. It’s why we are devoting this entire issue to reporting on how we offer hope and help to patients whose cancer has spread. 12 Metastasis: A Roadmap In the clinic, we are developing more targeted drugs, more precise radiation, and more sophisticated See the journey of a cancer cell as it transforms surgical techniques to treat our patients. In the lab, we are learning more every day about why and travels through the body. cancer cells metastasize and how to stop them. Our vision to save more lives requires a commitment to hire and train the brightest minds Multiplying the Army and a significant investment in four key areas of technology, which are already bringing about 17 astonishing advances: of Cancer-Fighting Immune Cells • Better models to study cancer: Conducting research in mice is time-consuming and doesn’t Learn about a new technology taking necessarily reflect cancer biology in humans. -

Current Overview of Treatment for Metastatic Bone Disease
Review Current Overview of Treatment for Metastatic Bone Disease Shinji Tsukamoto 1,* , Akira Kido 2, Yasuhito Tanaka 1 , Giancarlo Facchini 3 , Giuliano Peta 3 , Giuseppe Rossi 3 and Andreas F. Mavrogenis 4 1 Department of Orthopaedic Surgery, Nara Medical University, 840, Shijo-cho, Kashihara 634-8521, Nara, Japan; [email protected] 2 Department of Rehabilitation Medicine, Nara Medical University, 840, Shijo-cho, Kashihara 634-8521, Nara, Japan; [email protected] 3 Department of Radiology and Interventional Radiology, IRCCS Istituto Ortopedico Rizzoli, Via Pupilli 1, 40136 Bologna, Italy; [email protected] (G.F.); [email protected] (G.P.); [email protected] (G.R.) 4 First Department of Orthopaedics, School of Medicine, National and Kapodistrian University of Athens, 41 Ventouri Street, 15562 Athens, Greece; [email protected] * Correspondence: [email protected]; Tel.: +81-744-22-3051 Abstract: The number of patients with bone metastasis increases as medical management and surgery improve the overall survival of patients with cancer. Bone metastasis can cause skeletal complications, including bone pain, pathological fractures, spinal cord or nerve root compression, and hypercalcemia. Before initiation of treatment for bone metastasis, it is important to exclude primary bone malignancy, which would require a completely different therapeutic approach. It is essential to select surgical methods considering the patient’s prognosis, quality of life, postoperative function, and risk of postoperative complications. -

Bone and Soft Tissue Tumors: New Treatment Approaches
cancers Editorial Bone and Soft Tissue Tumors: New Treatment Approaches Shinji Miwa * , Norio Yamamoto and Hiroyuki Tsuchiya Department of Orthopedic Surgery, Graduate School of Medical Science, Kanazawa University, Kanazawa 920-8640, Japan; [email protected] (N.Y.); [email protected] (H.T.) * Correspondence: [email protected]; Tel.: +81-76-265-2374 Bone and soft tissue sarcomas require intensive treatments, including chemotherapy, surgical resection with safe margin, and radiotherapy. Although favorable outcomes have been reported in patients with non-metastatic sarcomas, the outcomes in patients with metastatic or recurrent sarcomas remain unsatisfactory [1]. To overcome the metastatic or recurrent sarcomas, new treatments or modifications of the standard treatment are required. This special issue included recent studies and reviews regarding therapeutic targets, anticancer agents, immunotherapy, and management in patients with bone and soft tissue sarcomas. This special issue included several studies and reviews of abnormal gene expression in bone and soft tissue sarcomas. Simpson et al. reported that a comparison of gene expression between canine osteosarcomas and non-tumor tissue showed 1281 significantly differen- tially expressed genes (839 lower and 442 elevated gene expression), a subset of which were validated by qRT-PCR and immunohistochemistry [2]. Furthermore, Greither et al. investigated the influence of miR-155-5p and miR-203a-3p expression on prognosis in patients with soft tissue sarcomas [3]. This study showed that increased expression of miR-155-5p was significantly associated with increased tumor stage, and that high miR- 155-5p expression and low miR-203a-3p expression were significantly associated with poor survival in patients with soft tissue sarcomas. -

Canine Bone Tumors
MEDICAL ONCOLOGY Canine Bone Tumors CLASSIFICATION OF BONE TUMORS Bone tumors can arise directly from bone or may occur as a metastatic lesion from an underlying cancer outside of the skeleton. The most common primary bone tumor in dogs is osteosarcoma. Other bone tumors include chondrosarcoma, fibrosarcoma, hemangiosarcoma, liposarcoma, histiocytic sarcoma, multiple myeloma, and metastatic tumors. Osteosarcoma tumors of the appendicular skeleton (long bones of the limbs) are locally invasive and have a high rate of metastases (most commonly lungs and other bones). Osteosarcoma tumors can also occur in the axial skeleton (the bones of the skull, spinal column, pelvis, and ribs). Tumors of these locations tend to have a decreased rate of metastasis compared to those of the limbs. It is important to differentiate osteosarcoma from other tumor types and diseases that occur within bones, such as bacterial, viral, or fungal infections. With infection, there is usually history of exposure to the infectious agent or traumatic injury to the affected region. Identification of the underlying cause is important, as this will influence the recommended therapeutic regimen. WHAT ARE THE CLINICAL SIGNS? Signs are nonspecific and depend on the site affected as well as the underlying cause. For tumors located on the limb, a history of lameness, discomfort, or intermittent limping is noted. A firm swelling can also be noted. X-rays of the affected site may be recommended at the onset of signs, or should they fail to resolve with conservative management. Other nonspecific clinical signs include discomfort (panting, inability to get comfortable), favoring other limbs, aggression, loss of appetite, weight loss, reduced exercise tolerance, and whimpering/crying out. -

Large Osteolytic Skull Tumor Presenting As a Small Subcutaneous Scalp Lesion
J Am Board Fam Med: first published as 10.3122/jabfm.2011.06.100308 on 15 November 2011. Downloaded from BRIEF REPORT Large Osteolytic Skull Tumor Presenting as a Small Subcutaneous Scalp Lesion John E. Sutherland, MD, Nader S. Dahdaleh, MD, Jeremy D. W. Greenlee, MD, Patricia A. Kirby, MD, and Michael D. Sargent, DO Subcutaneous nodules of the scalp are common and usually benign. We describe a case that presented as a probable inclusion cyst or lipoma of the scalp that was discovered to be a benign osteolytic fibro- histiocytic lesion of the frontoparietal skull. This ultimately was successfully treated by neurosurgery with a craniectomy, tumor excision, and reconstructive cranioplasty. (J Am Board Fam Med 2011;24: 763–767.) Keywords: Bone Tumor, Case Report, Giant Cell Tumor, Scalp Lesion, Skull Tumor Tumors of the skull are uncommon, with estimates dure the lump did not feel as circumscribed as an varying between 1% to 4% of all bone tumors.1–3 inclusion cyst, and was thought to be more likely a They most commonly present as an enlarging soft lipoma because it seemed to be mobile. The adja- or hard mass over the skull with or without some cent skull felt normal. After incision through the local tenderness. The differential diagnosis is broad scalp, the lesion was found to have a shiny, grayish and includes both benign and malignant lesions. exterior. In the process of dissection, the lesion was copyright. Most lesions are radiolucent and osteolytic and are incised and chunks of whitish-yellow cheesy sub- more common in young adults. -

Detection of Circulating Tumor DNA in Patients with Osteosarcoma
www.impactjournals.com/oncotarget/ Oncotarget, 2018, Vol. 9, (No. 16), pp: 12695-12704 Research Paper Detection of circulating tumor DNA in patients with osteosarcoma David M. Barris1,*, Shoshana B. Weiner1,*, Robert A. Dubin2, Michael Fremed1, Xusheng Zhang2, Sajida Piperdi3, Wendong Zhang3, Shahina Maqbool1, Jonathan Gill4, Michael Roth4, Bang Hoang5, David Geller5, Richard Gorlick4 and Daniel A. Weiser6,7 1Department of Genetics and Department of Pediatrics, Albert Einstein College of Medicine, Bronx, NY, USA 2Computational Genomics Core, Albert Einstein College of Medicine, Bronx, NY, USA 3Department of Pediatrics, Montefiore Medical Center, Bronx, NY, USA 4Division of Pediatrics, University of Texas MD Anderson Cancer Center, Houston, Texas, USA 5Department of Orthopedic Surgery, Montefiore Medical Center, Bronx, NY, USA 6Division of Hematology/Oncology, Children’s Hospital at Montefiore, Bronx, NY, USA 7Departments of Pediatrics and Genetics, Albert Einstein College of Medicine, Bronx, NY, USA *These authors contributed equally to this work Correspondence to: Shoshana B. Weiner, email: [email protected] Keywords: circulating tumor DNA; osteosarcoma; targeted sequencing; Next Generation Sequencing; targeted therapy Received: November 28, 2017 Accepted: January 09, 2018 Published: January 18, 2018 Copyright: Barris et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License 3.0 (CC BY 3.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. ABSTRACT Identification and quantification of somatic alterations in plasma-derived, circulating tumor DNA (ctDNA) is gaining traction as a non-invasive and cost effective method of disease monitoring in cancer patients, particularly to evaluate response to treatment and monitor for disease recurrence.