Hospital Acquired Conditions Diagnostic Codes and Descriptions
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

ABCDE Acronym Blood Transfusion 231 Major Trauma 234 Maternal
Cambridge University Press 978-0-521-26827-1 - Obstetric and Intrapartum Emergencies: A Practical Guide to Management Edwin Chandraharan and Sir Sabaratnam Arulkumaran Index More information Index ABCDE acronym albumin, blood plasma levels 7 arterial blood gas (ABG) 188 blood transfusion 231 allergic anaphylaxis 229 arterio-venous occlusions 166–167 major trauma 234 maternal collapse 12, 130–131 amiadarone, overdose 178 aspiration 10, 246 newborn infant 241 amniocentesis 234 aspirin 26, 180–181 resuscitation 127–131 amniotic fluid embolism 48–51 assisted reproduction 93 abdomen caesarean section 257 asthma 4, 150, 151, 152, 185 examination after trauma 234 massive haemorrhage 33 pain in pregnancy 154–160, 161 maternal collapse 10, 13, 128 atracurium, drug reactions 231 accreta, placenta 250, 252, 255 anaemia, physiological 1, 7 atrial fibrillation 205 ACE inhibitors, overdose 178 anaerobic metabolism 242 automated external defibrillator (AED) 12 acid–base analysis 104 anaesthesia. See general anaesthesia awareness under anaesthesia 215, 217 acidosis 94, 180–181, 186, 242 anal incontinence 138–139 ACTH levels 210 analgesia 11, 100, 218 barbiturates, overdose 178 activated charcoal 177, 180–181 anaphylaxis 11, 227–228, 229–231 behaviour/beliefs, psychiatric activated partial thromboplastin time antacid prophylaxis 217 emergencies 172 (APTT) 19, 21 antenatal screening, DVT 16 benign intracranial hypertension 166 activated protein C 46 antepartum haemorrhage 33, 93–94. benzodiazepines, overdose 178 Addison’s disease 208–209 See also massive -

Ask the Experts Amniotic Fluid Embolism Steven L. Clark, MD
Ask the Experts Questions have been written by: Amniotic Fluid Embolism Angela K. Hardyk, MD Mount Nittany Physician Group Ob/Gyn Steven L. Clark, MD State College, PA (Obstet Gynecol 2014;123:337–48) Responses have been written by: Steven L. Clark, MD Hospital Corporation of America Nashville, TN Question 1: How would you counsel a patient about a future pregnancy if she has been lucky enough to survive an amniotic fl uid embolism (AFE)? Would there be any special precautions she would need to take for her next pregnancy? Response from Dr. Clark: The available data in this area consist only of several very small series and case reports. These data suggest that the risks of recurrence are low. In addition, a pathophysiologic mechanism of disease that hinges on a maternal reaction to a specif- ic set of fetal antigens would suggest that recurrence ought to be uncommon. On the other hand, having dodged one bullet, is it really wise to spin the wheel again? My counseling goes something like this: “Available data suggest that the risk of recurrence is low, and there are a number of reports of successful pregnancy outcome after AFE survival. However, given the potential severity of AFE if it does recur, and a lack of really good data regarding risks, I advise you to undertake another pregnancy only if you are willing to accept a small risk of catastrophic outcome including death.” If a patient chooses to undertake pregnancy, I do not alter my management in any way, other than delivery in a tertiary center. -

Intravenous Drug Use-Associated Infective Endocarditis in Pregnant Patients at a Hospital in West Virginia
Open Access Original Article DOI: 10.7759/cureus.17218 Intravenous Drug Use-Associated Infective Endocarditis in Pregnant Patients at a Hospital in West Virginia Deena Dahshan 1 , Mohamed Suliman 2 , Ebad U. Rahman 3 , Zachary Curtis 1 , Ellen Thompson 2 1. Internal Medicine, Marshall University Joan C. Edwards School of Medicine, Huntington, USA 2. Cardiology, Marshall University Joan C. Edwards School of Medicine, Huntington, USA 3. Internal Medicine, St. Mary's Medical Center, Huntington, USA Corresponding author: Deena Dahshan, [email protected] Abstract Introduction Due to high levels of intravenous drug use (IVDU) in West Virginia (WV), there are increasing numbers of hospitalizations for infective endocarditis (IE). More specifically, pregnant patients with IE are a uniquely challenging population, with complex management and a clinical course that further affects the health of the fetus, with high morbidity and mortality. Timely recognition and awareness of the most common bacterial causes will provide hospitals and clinicians with valuable information to manage future patients. Methods This retrospective study analyzed the clinical course of pregnant patients admitted with IE and IVDU history presenting at Cabell Huntington Hospital from 2013 to 2018. Inclusion criteria were women between 16 and 45 years of age confirmed to be pregnant by urine pregnancy test and ultrasonography with at least eight weeks gestation, with a first-time diagnosis of endocarditis and an identified history of IVDU. We excluded charts with pre-existing risk factors including a history of valvular disease, rheumatic heart disease, surgical valve repair or mechanical valve replacement, or a diagnosis of coagulopathies. The resulting charts were evaluated for isolated organisms, reported clinical course, and complications of the pregnancy. -

Management of Prolonged Decelerations ▲
OBG_1106_Dildy.finalREV 10/24/06 10:05 AM Page 30 OBGMANAGEMENT Gary A. Dildy III, MD OBSTETRIC EMERGENCIES Clinical Professor, Department of Obstetrics and Gynecology, Management of Louisiana State University Health Sciences Center New Orleans prolonged decelerations Director of Site Analysis HCA Perinatal Quality Assurance Some are benign, some are pathologic but reversible, Nashville, Tenn and others are the most feared complications in obstetrics Staff Perinatologist Maternal-Fetal Medicine St. Mark’s Hospital prolonged deceleration may signal ed prolonged decelerations is based on bed- Salt Lake City, Utah danger—or reflect a perfectly nor- side clinical judgment, which inevitably will A mal fetal response to maternal sometimes be imperfect given the unpre- pelvic examination.® BecauseDowden of the Healthwide dictability Media of these decelerations.” range of possibilities, this fetal heart rate pattern justifies close attention. For exam- “Fetal bradycardia” and “prolonged ple,Copyright repetitive Forprolonged personal decelerations use may onlydeceleration” are distinct entities indicate cord compression from oligohy- In general parlance, we often use the terms dramnios. Even more troubling, a pro- “fetal bradycardia” and “prolonged decel- longed deceleration may occur for the first eration” loosely. In practice, we must dif- IN THIS ARTICLE time during the evolution of a profound ferentiate these entities because underlying catastrophe, such as amniotic fluid pathophysiologic mechanisms and clinical 3 FHR patterns: embolism or uterine rupture during vagi- management may differ substantially. What would nal birth after cesarean delivery (VBAC). The problem: Since the introduction In some circumstances, a prolonged decel- of electronic fetal monitoring (EFM) in you do? eration may be the terminus of a progres- the 1960s, numerous descriptions of FHR ❙ Complete heart sion of nonreassuring fetal heart rate patterns have been published, each slight- block (FHR) changes, and becomes the immedi- ly different from the others. -

Ante Partum Haemorrhage
Ante Partum Haemorrhage Sara Alhaddab Alanood Asiri Ante Partum Haemorrhage (APH): Bleeding in early pregnancy (first 20 weeks of gestation) causes: Affects 3-5 % of pregnancies. • - Miscarriage • Bleeding from or into the genital tract. - Ectopic pregnancy • Occurring from 20 weeks of pregnancy and prior - Molar pregnancy to the birth of the baby. - Local causes: tumor, trauma etc. Causes: Landmark of fetal viability is 20 weeks. • Placenta previa. • Placenta abruption. • Local causes (cervical or vaginal lesions, lacerations). Trauma, tumor and infections. • Unexplained (SGA, IUGR). SGA: small for gestational age. • Vasa previa. • Uterine rupture. - APH is the leading cause of prenatal and maternal morbidity and prenatal mortality (mainly prematurity). - Obstetrics hemorrhage remains one of the major causes of maternal death in the developing countries. Management: In the hospital maternity unit with facilities for resuscitation such as: Source: Essentials of Obstetrics and Gynecology. § Anesthetic support. § Blood transfusion resources. § Performing emergency operative delivery. § Multidisciplinary team including (midwifery, obstetric staff, neonatal and anesthetic). Investigations: • Tests if suspecting vasa previa are often not applicable • Tocolysis: shouldn’t be used in: v Unstable patient. v Fetal compromise. v Major APH. It’s a decision of a senior obstetrician. Senior (consultant) anesthetic care needed in high-risk hemorrhage. • Risk of PPH: patient should receive active management of 3rd stage of labor using syntometrine (in absence of high BP). Syntometrine → active uterine contraction after delivery to prevent PPH. • AntiD Ig should be given to all non sensitized RH –ve if the have APH, at least 500 IU AntiD Ig followed by a test of FMH if it is more than 40 ml of RBC additional AntiD required. -

Critical Care Issues in Pregnancy
CriticalCritical CareCare IssuesIssues inin PregnancyPregnancy Miren A. Schinco, MD, FCCS, FCCM Associate Professor of Surgery University of Florida College of Medicine, Jacksonville College of Medicine – Jacksonville Department of Surgery EpidemiologyEpidemiology •Approximately .1% of deliveries result in ICU admission • Generally, 75% - 80 % are during the post- partum period College of Medicine – Jacksonville Department of Surgery TopTop causescauses ofof mortalitymortality inin obstetricobstetric patientspatients admittedadmitted toto thethe ICUICU Etiology N (of 1354) Percentage Hypertension 20 21.5 Pulmonary 20 21.5 Cardiac 11 11.8 Hemorrhage 8 8.6 CNS 8 8.6 Sepsis/Infection 6 6.4 Malignancy 6 6.4 College of Medicine – Jacksonville Department of Surgery CriticalCritical illnessesillnesses inin pregnancypregnancy A. Conditions unique to pregnancy: account for 50-80% admissions to ICU(account for > 50% ICU admissions): • Preeclampsia / Eclampsia • HELLP syndrome • Acute fatty liver of pregnancy • Amniotic fluid embolism • Peri-partum cardiomyopathy • Puerperal sepsis • Thrombotic disease • Obstetric hemorrhage College of Medicine – Jacksonville Department of Surgery CriticalCritical illnessesillnesses inin pregnancypregnancy B. Pre-existing conditions that may worsen during pregnancy (account for 20-50% ICU admissions): • Cardiovascular: valvular disease, Eisenmenger’s syndrome, cyanotic congenital heart disease, coarctation of aorta, PPH • Renal: glomerulonephritis, chronic renal insufficiency • Hematologic: sickle cell disease, -
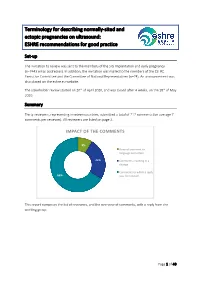
Terminology for Describing Normally-Sited and Ectopic Pregnancies on Ultrasound: ESHRE Recommendations for Good Practice
Terminology for describing normally-sited and ectopic pregnancies on ultrasound: ESHRE recommendations for good practice Set-up The invitation to review was sent to the members of the SIG Implantation and early pregnancy (n=7443 email addresses). In addition, the invitation was mailed to the members of the ESHRE Executive Committee and the Committee of National Representatives (n=74). An announcement was also placed on the eshre.eu website. The stakeholder review started on 20th of April 2020, and was closed after 4 weeks, on the 18th of May 2020. Summary Thirty reviewers, representing nineteen countries, submitted a total of 212 comments (on average 7 comments per reviewer). All reviewers are listed on page 2. IMPACT OF THE COMMENTS 9% General comment or language correction 25% Comments resulting in a change Comments to which a reply 66% was formulated This report comprises the list of reviewers, and the overview of comments, with a reply from the working group. Page 1 of 40 List of reviewers Name Country Organization Masoud Kamrava Iran Steven Goldstein USA Ulrike Metzger France Grigorios Derdelis Greece Luca Savelli Italy Gangaraju Buvaneswari India Mridu Sinha India Onur Erol Turkey Aboubakr Mohamed Elnashar Egypt Jiuzhi Zeng China Carlos Calhaz-Jorge Portugal Dr. Nidaa Qatar Attilio Di Spiezio Sardo Italy Melinda Mitranovici Romania Ali Sami Gurbuz Turkey Philippe Merviel France Roy Farquharson UK Ilan Timor USA Alessandra Pipan United Arab Emirates Company, Taiwan IVF Wen Jui Yang Taiwan Group Center Lorenzo Abad de Velasco Spain Monica Varma India Kumaran Aswathy India Annick Geril Belgium Snezana Vidakovic Serbia Lukasz Polanski, Miriam Baumgarten, Rebecca McKay, Laura Rutherford, Ouma Pillay, Anita Jeyaraj, Kanna Jayaprakasan and Kamal Ojha UK organization Mohamed Shahin UK Mohsen M El-Sayed UK International Society of Ultrasound in Obstetrics and Gynecology (ISUOG) ISUOG European Niche taskforce group of the ESGE and international Prof. -

Sonography in First Trimester Bleeding
Review Sonography in First Trimester Bleeding Manjiri Dighe, MD,1 Carlos Cuevas, MD,1 Mariam Moshiri, MD,1 Theodore Dubinsky, MD,1 Vikram S. Dogra, MD2 1 Department of Radiology, University of Washington Medical Center, Seattle, WA 98195 2 Department of Imaging Sciences, University of Rochester School of Medicine, 601 Elmwood Avenue, Box 648, Rochester, NY 14642 Received 19 April 2007; accepted 1 October 2007 ABSTRACT: Vaginal bleeding is the most common however, the most common cause of bleeding is cause of presentation to the emergency department spotting caused by implantation of the conceptus in the first trimester. Approximately half of patients into the endometrium. A complete assessment of with first trimester vaginal bleeding will lose the preg- the first trimester pregnancy requires correlation nancy. Clinical assessment is difficult, and sonogra- of serum b human chorionic gonadotropin (b- phy is necessary to determine if a normal fetus is hCG) levels with the appearance of the gesta- present and alive and to exclude other causes of bleeding (eg, ectopic or molar pregnancy). Diagnosis tional sac (GS) using sonography. of a normal intrauterine pregnancy not only helps the physician in terms of management but also gives psy- SPONTANEOUS ABORTION chologic relief to the patient. Improved ultrasound technology and high-frequency endovaginal trans- Spontaneous abortion is defined as the termina- ducers have enabled early diagnosis of abnormal and tion of a pregnancy before the twentieth completed ectopic pregnancies, decreasing maternal morbidity week of gestation. Sixty-five percent of spontane- and mortality. The main differential considerations of ous abortions occur in the first 16 weeks of preg- first trimester bleeding are spontaneous abortion, ec- nancy. -

Diseases of the Digestive System (KOO-K93)
CHAPTER XI Diseases of the digestive system (KOO-K93) Diseases of oral cavity, salivary glands and jaws (KOO-K14) lijell Diseases of pulp and periapical tissues 1m Dentofacial anomalies [including malocclusion] Excludes: hemifacial atrophy or hypertrophy (Q67.4) K07 .0 Major anomalies of jaw size Hyperplasia, hypoplasia: • mandibular • maxillary Macrognathism (mandibular)(maxillary) Micrognathism (mandibular)( maxillary) Excludes: acromegaly (E22.0) Robin's syndrome (087.07) K07 .1 Anomalies of jaw-cranial base relationship Asymmetry of jaw Prognathism (mandibular)( maxillary) Retrognathism (mandibular)(maxillary) K07.2 Anomalies of dental arch relationship Cross bite (anterior)(posterior) Dis to-occlusion Mesio-occlusion Midline deviation of dental arch Openbite (anterior )(posterior) Overbite (excessive): • deep • horizontal • vertical Overjet Posterior lingual occlusion of mandibular teeth 289 ICO-N A K07.3 Anomalies of tooth position Crowding Diastema Displacement of tooth or teeth Rotation Spacing, abnormal Transposition Impacted or embedded teeth with abnormal position of such teeth or adjacent teeth K07.4 Malocclusion, unspecified K07.5 Dentofacial functional abnormalities Abnormal jaw closure Malocclusion due to: • abnormal swallowing • mouth breathing • tongue, lip or finger habits K07.6 Temporomandibular joint disorders Costen's complex or syndrome Derangement of temporomandibular joint Snapping jaw Temporomandibular joint-pain-dysfunction syndrome Excludes: current temporomandibular joint: • dislocation (S03.0) • strain (S03.4) K07.8 Other dentofacial anomalies K07.9 Dentofacial anomaly, unspecified 1m Stomatitis and related lesions K12.0 Recurrent oral aphthae Aphthous stomatitis (major)(minor) Bednar's aphthae Periadenitis mucosa necrotica recurrens Recurrent aphthous ulcer Stomatitis herpetiformis 290 DISEASES OF THE DIGESTIVE SYSTEM Diseases of oesophagus, stomach and duodenum (K20-K31) Ill Oesophagitis Abscess of oesophagus Oesophagitis: • NOS • chemical • peptic Use additional external cause code (Chapter XX), if desired, to identify cause. -

Amnioinfusion
Review Article Indian Journal of Obstetrics and Gynecology Volume 7 Number 4 (Part - II), October – December 2019 DOI: http://dx.doi.org/10.21088/ijog.2321.1636.7419.12 Amnioinfusion Alka Patil1, Sayli Thavare2, Bhagyashree Badade3 How to cite this article: Alka Patil, Sayli Thavare, Bhagyashree Badade. Amnioinfusion. Indian J Obstet Gynecol. 2019;7(4)(Part-II):641–644. 1Professor and Head, 2,3Junior Resident, Department of Obstetrics and Gynaecology, ACPM Medical College, Dhule, Maharashtra 424002, India. Corresponding Author: Alka Patil, Professor and Head, Department of Obstetrics and Gynaecology, ACPM Medical College, Dhule, Maharashtra 424002, India. E-mail: [email protected] Received on 20.11.2019; Accepted on 16.12.2019 Abstract potentially at risk. Oligohydramnios is one of the high-risk pregnancy, posing diagnostic challenge Amniotic fluid is a dynamic medium that plays and dilemma in management. These high-risk a significant role in fetal well-being. It is essential pregnancies should be monitored, managed during pregnancy for normal fetal growth and organ and delivered at a tertiary care center for good development. About 4% of pregnancies are complicated pregnancy outcome. by oligohydramnios. It is associated with an increased incidence of perinatal morbidity and mortality due to its Amniotic fl uid is essential for the continued well antepartum and intrapartum complications. Gerbruch being of the fetus and has following functions: and Hansman described a technique of Amnioinfusion • Shock absorber preventing hazardous to overcome these difficulties to prevent the occurrence pressure on the fetal parts of fetal lung hypoplasia in pregnancies complicated by oligohydramnios. Amnioinfusion reduces both • Prevents adhesion formation between fetal the frequency and depth of FHR deceleration. -

State Medicaid Manual
Page 1 of 37 Louisiana Medicaid Approved Pay and Chase Primary Prenatal Care Diagnosis Codes MCOs must use the "pay and chase" method of payment for prenatal services for individuals with other Health Insurance. The MCO must seek reimbursement from the third party within 60 days after the end of the month in which payment is made. Primary prenatal diagnoses which do not require primary health insurance claim filing by most providers are confined to those listed below. Hospitals are not included and must continue to file claims with the primary health insurance carriers. ICD-9-CM to ICD-10 crosswalk for Prenatal Diagnosis Codes ICD-9-CM Description Code V22.0 Supervision of normal pregnancy V22.1 V23 Supervision of high risk pregnancy V28 Antenatal screening 640-648 Complications related to pregnancy 651-658 Other conditions requiring care in 671 pregnancy 673 675-676 ICD-10-CM Diagnosis Codes – for Prenatal Services upon Implementation of ICD-10 ICD-9-CM code V22.0 maps to the following ICD-10-CM codes Z3400 Encounter for supervision of normal first pregnancy, unspecified trimester Z3403 Encounter for supervision of normal first pregnancy, third trimester Z3401 Encounter for supervision of normal first pregnancy, first trimester Z3402 Encounter for supervision of normal first pregnancy, second trimester ICD-9-CM code V22. -

Shoulder Dystocia Abnormal Placentation Umbilical Cord
Obstetric Emergencies Shoulder Dystocia Abnormal Placentation Umbilical Cord Prolapse Uterine Rupture TOLAC Diabetic Ketoacidosis Valerie Huwe, RNC-OB, MS, CNS & Meghan Duck RNC-OB, MS, CNS UCSF Benioff Children’s Hospital Outreach Services, Mission Bay Objectives .Highlight abnormal conditions that contribute to the severity of obstetric emergencies .Describe how nurses can implement recommended protocols, procedures, and guidelines during an OB emergency aimed to reduce patient harm .Identify safe-guards within hospital systems aimed to provide safe obstetric care .Identify triggers during childbirth that increase a women’s risk for Post Traumatic Stress Disorder and Postpartum Depression . Incorporate a multidisciplinary plan of care to optimize care for women with postpartum emergencies Obstetric Emergencies • Shoulder Dystocia • Abnormal Placentation • Umbilical Cord Prolapse • Uterine Rupture • TOLAC • Diabetic Ketoacidosis Risk-benefit analysis Balancing 2 Principles 1. Maternal ‒ Benefit should outweigh risk 2. Fetal ‒ Optimal outcome Case Presentation . 36 yo Hispanic woman G4 P3 to L&D for IOL .IVF Pregnancy .3 Prior vaginal births: 7.12, 8.1, 8.5 (NCB) .Late to care – EDC ~ 40-41 weeks .GDM Type A2 – somewhat uncontrolled .4’11’’ .Hx of Lupus .BMI 40 .Gained ~ 40 lbs during pregnancy Question: What complication is she a risk for? a) Placental abruption b) Thyroid Storm c) Preeclampsia with severe features d) Shoulder dystocia e) Uterine prolapse Case Presentation . 36 yo Hispanic woman G4 P3 to L&D for IOL .IVF Pregnancy .3