Soft Tissue Grafting to Improve the Attached Mucosa at Dental Implants: a Review of the Literature and Proposal of a Decision Tree
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Clinical Outcome of a New Surgical Technique for the Treatment of Peri-Implant Dehiscence in the Esthetic Area. a Case Report
applied sciences Case Report Clinical Outcome of a New Surgical Technique for the Treatment of Peri-Implant Dehiscence in the Esthetic Area. A Case Report Norberto Quispe-López 1 , Carmen García-Faria 2, Jesús Mena-Álvarez 2,* , Yasmina Guadilla 1, Pablo Garrido Martínez 3,4 and Javier Montero 1 1 Department of Surgery, Faculty of Medicine, University of Salamanca, 37008 Salamanca, Spain; [email protected] (N.Q.-L.); [email protected] (Y.G.); [email protected] (J.M.) 2 Faculty of Health Sciences, Alfonso X el Sabio University, 28703 Madrid, Spain; [email protected] 3 Department of Prosthesis, Faculty of Dentistry, Universidad Alfonso X el Sabio, 28703 Madrid, Spain; [email protected] 4 Department of Oral and Maxillofacial Surgery, Hospital La Luz, 28003 Madrid, Spain * Correspondence: [email protected] Abstract: This study describes the clinical and esthetic outcome of n apical surgical treatment on peri-implant soft tissue dehiscence in an implant with a poor prognosis in the esthetic area. The patient presented a compromised situation of clinical attachment loss both in the 1.2 implant and in the adjacent teeth. A biphasic approach consisted firstly of a connective tissue graft accessed by apical and then, 11 months later, a palatal flap technique plus a connective tissue graft. After 20 months of Citation: Quispe-López, N.; healing, surgical approaches without vertical releasing incisions showed a gain in recession reduction García-Faria, C.; Mena-Álvarez, J.; over the implant ranging from 0.3 to 2.7 mm (CI 95%), in addition to a gain in width (2 mm) and Guadilla, Y.; Garrido Martínez, P.; thickness (2.3 mm) of the keratinized mucosa. -

04-207 Gingival Flap Procedure and Apically Positioned
Dental Policy Subject: Gingival Flap Procedure and Apically Positioned Flap Guideline #: 04-207 Publish Date: 03/27/2018 Status: New Last Review Date: 03/12//2018 Description This document addresses the Gingival Flap Procedure, including root planing, and Apically Positioned Flap. Note: Please refer to the following documents for additional information concerning related topics: Scaling and Root Planing (04-301) Periodontal Maintenance (04-901) Mucogingival Surgery and Soft Tissue Grafting (04-204) Biological Materials to Aid Soft and Hard Tissue Grafting (04 Clinical Policy-01 Teeth with Guarded or Poor Prognosis Indications The gingival flap procedure or apically positioned flap are considered appropriate for the treatment of mild to severe periodontal disease when non-surgical methods such as scaling and root planing have been unsuccessful in removal of below the gum deposits of plaque (biofilm) and calculus and where, due to supra-bony pocket depths osseous recontouring and bone grafting are not required. As it applies to appropriateness of care, dental services must be: provided by a Dentist, exercising prudent clinical judgment provided to a patient for the purpose of evaluating, diagnosing and/or treating a dental injury or disease or its symptoms in accordance with the generally accepted standards of dental practice which means: o standards that are based on credible scientific evidence published in peer-reviewed, dental literature generally recognized by the practicing dental community o specialty society recommendations/criteria o any other relevant factors clinically appropriate, in terms of type, frequency and extent considered effective for the patient's dental injury or disease not primarily performed for the convenience of the patient or Dentist not more costly than an alternative service. -

Correlation of Width of Attached Gingiva on Oral Hygiene Maintenance and Gingival Health
Research Article J Nepal Soc Perio Oral Implantol. 2020;4(7):5-9 Correlation of Width of Attached Gingiva on Oral Hygiene Maintenance and Gingival Health Dr. Shaili Pradhan,1 Dr. Benju Shrestha1 1Department of Dental Surgery, National Academy of Medical Sciences, Bir Hospital, Kathmandu, Nepal. ABSTRACT Introduction: Attached gingiva aids in increased resistance to external injury and contribute in stabilisation of gingival margin against frictional forces as well as dissipates physiological forces exerted by the muscular fibers of the alveolar mucosa on gingival tissues. Objective: To assess width of attached gingiva in adults and correlate with oral hygiene maintenance and gingival inflammation. Methods: A cross-sectional study was conducted in patients aged 20-40 years visiting dental OPD with healthy periodontium. Plaque index (PI) and Gingival index (GI) were recorded. Mucogingival junction was determined by visual and functional method. Keratinised gingiva width (KGW) and probing pocket depth (PPD) was recorded and attached gingiva width (AGW) was calculated as (KGW–PPD). Results: Total 85 patients (43 males and 42 females) enrolled in this study. Among total, 48.23% had AGW<1 mm. AGW <1 mm most commonly was found in mandibular first premolar, highest mean AGW was found in maxillary incisors. The mean GI and PI values for AGW<1 mm were found to be higher than those for AGW≥ 1 mm. However, result did not show any significant relation between AGW and severity of gingival inflammation (P value 0.608) and plaque control (P value 0.297). Conclusion: The correlation between attached gingiva width and severity of gingival inflammation and plaque index was not significant statistically. -
The Relationship Between the Width of Keratinized Gingiva and Gingival Health By
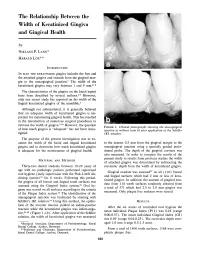
The Relationship Between the Width of Keratinized Gingiva and Gingival Health by NIKLAUS P. LANG* HARALD LÖE** INTRODUCTION IN MAN THE KERATINIZED gingiva includes the free and the attached gingiva and extends from the gingival mar gin to the mucogingival junction.1 The width of the keratinized gingiva may vary between 1 and 9 mm.2, 3 The characteristics of the gingiva on the facial aspect have been described by several authors.17 However, only one recent study has reported on the width of the lingual keratinized gingiva of the mandible.7 Although not substantiated, it is generally believed that an adequate width of keratinized gingiva is im portant for maintaining gingival health. This has resulted in the introduction of numerous surgical procedures to increase the width of gingiva.830 However, the question FIGURE 1. Clinical photographs showing the mucogingival of how much gingiva is "adequate" has not been inves junction a) without stain b) after application of the Schiller tigated. IKI solution. The purpose of the present investigation was to ex amine the width of the facial and lingual keratinized to the nearest 0.5 mm from the gingival margin to the gingiva and to determine how much keratinized gingiva mucogingival junction using a specially graded perio is adequate for the maintenance of gingival health. dontal probe. The depth of the gingival crevices was also measured. In order to compare the results of the present study to results from previous studies the width MATERIAL AND METHODS of attached gingiva was determined by subtracting the Thirty-two dental students between 19-29 years of crevicular depth from the width of keratinized gingiva. -

Nonsurgical Management of Amlodipine
International Journal of Dental and Health Sciences Case Report Volume 02, Issue 03 HEREDITARY GINGIVAL FIBROMATOSIS ASSOCIATED WITH CONSANGUINITY: A RARE CASE REPORT Anila Sankaranarayanan1*,Nandakumar Krishnankutty2,Prasanth Dhanapal3, George Jacob M4 1Reader, Department of Periodontics, P.S.M. College of Dental Science and Research, Thrissur, India 2Principal, Azeezia Dental College, Kollam, India 3Professor, Dept. Of Conservative Dentistry & Endodontics, Annoor Dental College & Hospital, Muvattupuzha, India 4Reader, Dept of Conservative Dentistry & Endodontics, P.S.M. College of Dental Science and Research, Thrissur, India ABSTRACT: Hereditary gingival fibromatosis is a rare condition manifested by enlarged gingival tissues, and can occur as an isolated disease or as part of a syndrome. The condition is inherited as an autosomal dominant trait, which is more common, or as an autosomal recessive trait. This case report reports a case of a 16 year old boy with non-syndromic Hereditary gingival fibromatosis with a probable recessive mode of inheritance, as the patient’s parents reported a history of consanguineous marriage. The fibrotic gingival tissue was removed surgically, sextant wise under local anesthesia. After the surgical procedure the patient’s appearance was considerably improved. The case was followed up for 18 months at regular intervals and there was no evidence of recurrence of the gingival condition. Key words: Consanguinity, Fibromatosis, Gingival, Hereditary INTRODUCTION: consistency with presence of exaggerated stippling [4]. The usually painless Hereditary gingival fibromatosis (HGF) is a enlargement may extend up to the rare inherited condition, which results in mucogingival junction, but does not spontaneous and progressive involve the alveolar mucosa [5]. The enlargement of the gingiva [1]. -

Clinical Significance of Dental Anatomy, Histology, Physiology, and Occlusion
1 Clinical Significance of Dental Anatomy, Histology, Physiology, and Occlusion LEE W. BOUSHELL, JOHN R. STURDEVANT thorough understanding of the histology, physiology, and Incisors are essential for proper esthetics of the smile, facial soft occlusal interactions of the dentition and supporting tissues tissue contours (e.g., lip support), and speech (phonetics). is essential for the restorative dentist. Knowledge of the structuresA of teeth (enamel, dentin, cementum, and pulp) and Canines their relationships to each other and to the supporting structures Canines possess the longest roots of all teeth and are located at is necessary, especially when treating dental caries. The protective the corners of the dental arches. They function in the seizing, function of the tooth form is revealed by its impact on masticatory piercing, tearing, and cutting of food. From a proximal view, the muscle activity, the supporting tissues (osseous and mucosal), and crown also has a triangular shape, with a thick incisal ridge. The the pulp. Proper tooth form contributes to healthy supporting anatomic form of the crown and the length of the root make tissues. The contour and contact relationships of teeth with adjacent canine teeth strong, stable abutments for fixed or removable and opposing teeth are major determinants of muscle function in prostheses. Canines not only serve as important guides in occlusion, mastication, esthetics, speech, and protection. The relationships because of their anchorage and position in the dental arches, but of form to function are especially noteworthy when considering also play a crucial role (along with the incisors) in the esthetics of the shape of the dental arch, proximal contacts, occlusal contacts, the smile and lip support. -

Diagnosis Questions and Answers
1.0 DIAGNOSIS – 6 QUESTIONS 1. Where is the narrowest band of attached gingiva found? 1. Lingual surfaces of maxillary incisors and facial surfaces of maxillary first molars 2. Facial surfaces of mandibular second premolars and lingual of canines 3. Facial surfaces of mandibular canines and first premolars and lingual of mandibular incisors* 4. None of the above 2. All these types of tissue have keratinized epithelium EXCEPT 1. Hard palate 2. Gingival col* 3. Attached gingiva 4. Free gingiva 16. Which group of principal fibers of the periodontal ligament run perpendicular from the alveolar bone to the cementum and resist lateral forces? 1. Alveolar crest 2. Horizontal crest* 3. Oblique 4. Apical 5. Interradicular 33. The width of attached gingiva varies considerably with the greatest amount being present in the maxillary incisor region; the least amount is in the mandibular premolar region. 1. Both statements are TRUE* 39. The alveolar process forms and supports the sockets of the teeth and consists of two parts, the alveolar bone proper and the supporting alveolar bone; ostectomy is defined as removal of the alveolar bone proper. 1. Both statements are TRUE* 40. Which structure is the inner layer of cells of the junctional epithelium and attaches the gingiva to the tooth? 1. Mucogingival junction 2. Free gingival groove 3. Epithelial attachment * 4. Tonofilaments 1 49. All of the following are part of the marginal (free) gingiva EXCEPT: 1. Gingival margin 2. Free gingival groove 3. Mucogingival junction* 4. Interproximal gingiva 53. The collar-like band of stratified squamous epithelium 10-20 cells thick coronally and 2-3 cells thick apically, and .25 to 1.35 mm long is the: 1. -

Hereditary Gingival Fibromatosis: a Review and a Report of a Rare Case
Hindawi Publishing Corporation Case Reports in Dentistry Volume 2013, Article ID 930972, 4 pages http://dx.doi.org/10.1155/2013/930972 Case Report Hereditary Gingival Fibromatosis: A Review and a Report of a Rare Case Hossein Aghili and Mahdjoube Goldani Moghadam Department of Orthodontics, Faculty of Dentistry, Shahid Sadoughi University of Medical Sciences, Yazd 89195/165, Iran Correspondence should be addressed to Mahdjoube Goldani Moghadam; [email protected] Received 3 January 2013; Accepted 23 January 2013 Academic Editors: L. Junquera and A. Markopoulos Copyright © 2013 H. Aghili and M. Goldani Moghadam. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Hereditary gingival fibromatosis (HGF) is a rare condition which manifests itself by an enlarged gingival tissue covering teeth to various extents. The condition may occur isolated or as part of a syndrome. This paper presents a case of 9-year-old female patient suffering from HGF with chief complaint of mouth protrusion. Cephalometric findings showed severe mandibular deficiency and vertical maxillary excess. Patient exhibited perioral muscle contraction on mouth closing. After discussing the treatment possibilities with the patient and her parents, the decision was made to wait until growth potential decreases (following the adolescent growth spurt) and to correct the problem with orthognathic surgery. 1. Introduction 2. Case Presentation Hereditary gingival fibromatosis (HGF) is a rare condition A 9-year-old female patient visited the department of with the prevalence of one per 175000 population and orthodontics complaining of mouth protrusion (Figure 1) equal distribution in sexes [1]. -

Necrotizing Ulcerative Periodontitis in a HIV Seronegative Patient
Case Reports in Odontology Journal homepage: http://www.casereportsinodontology.org Necrotizing Ulcerative Periodontitis in a HIV Seronegative Patient– A Case Report [PP: 05-09] Syed Wali Peeran Karthikeyan Ramalingam Department of Periodontology and Oral Implantology Department of Oral Pathology & Microbiology Faculty of dentistry, Sebha University Faculty of dentistry, Sebha University Sebha, Libya Sebha, Libya [email protected] Syed Ali Peeran Yasmen Elhadi Elamin Elsadek Department of Oral and maxillofacial Prosthodontics Faculty of Dentistry, Sebha University Faculty of Dentistry, Jazan University Sebha, Libya Jazan, KSA ARTICLE INFO ABSTRACT Article History Paper received on: Necrotizing ulcerative periodontitis (NUP) is characterized by soft tissue 03/03/2014 necrosis, rapid periodontal destruction, and interproximal bone loss. Accepted after review on: Unlike other periodontal diseases, it presents with substantial necrosis of 02/04/2014 gingival tissues, and loss of periodontal ligament and alveolar bone. Published on: 01/06/2014 Herewith, we present a case report of NUP in a patient of Libyan origin. Keywords To the best of our knowledge, it is the first case report from Libya in Necrotizing ulcerative English literature. periodontitis, HIV seronegative, Libyan origin Cite this article as: Syed, W. P., Ramalingam, K., Syed, A. P., & Elsadek, Y. E. (2014) Necrotizing Ulcerative Periodontitis in a HIV Seronegative Patient – A Case Report. Case Reports in Odontology. 1(1), 05-09 Retrieved from http://www.casereportsinodontology.org Case Reports in Odontology Volume: 1 Issue: 1 January-June, 2014 he was a heavy smoker, smoking 50 Introduction cigarettes per day and had been smoking for Necrotizing ulcerative periodontitis 15 years. Past medical history revealed (NUP) is the most severe inflammatory episodes of heavy stress. -

Original Papers
ORIGINAL PAPERS Dent. Med. Probl. 2011, 48, 4, 00– © Copyright by Wroclaw Medical University ISSN 1644-387X and Polish Dental Society Wojciech Bednarz, Agata Zielińska Ultrasonic Biometer and its Usage in an Assessment of Periodontal Soft Tissue Thickness and Comparison of its Measurement Accuracy with a Bone Sounding Method Zastosowanie biometru ultradźwiękowego w badaniu grubości tkanek miękkich przyzębia i porównanie jego dokładności pomiarowej z metodą „bone sounding” brak adresu zakładu Abstract Background. The ability to identify a periodontal biotype accurately, and in particular knowledge of soft tissues thickness in the periodontium (GT – Gingival Thickness), have high influence on planning and conducting a tre- atment in all fields of dentistry, significantly affecting the final outcome. Objective. To compare the measurement accuracy of an ultrasonic and invasive method (bone sounding) in eva- luation of soft tissues thickness in the periodontium. Material and Methods. 30 subjects of both sexes aged 19–51 (21 females and 9 males) with a normal periodon- tium, without systemic and local comorbidities, that could affect periodontal tissues, were examined. Soft tissues thickness was measured by a non-invasive method, using Pirop® Ultrasonic Biometer with the A-scan probe with 20 MHz frequency, with 1540 m/s ultrasonic impulse velocity and accuracy up to 0.01 mm, and by a puncturing – bone sounding method with an endodontic tool with a limiter, and measurement readouts were taken from a calibrator with 0.1 mm accuracy. Measurements were made in area near 20 teeth in each subject (incisive, canine and premolar teeth in both jaws), at two points by each tooth. -

Evaluation of Increase in Width of Keratinized Gingiva Using
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-ISSN: 2279-0853, p-ISSN: 2279-0861.Volume 19, Issue 1 Ser.14 (January. 2020), PP 40-45 www.iosrjournals.org Evaluation of Increase in Width of Keratinized Gingiva Using Functional Method and Chemical Staining Method Post Lateral Pedicle Graft Combined With Connective Tissue Graft in Treatment of Gingival Recession. Dr. Gauri Ugale1, Dr. Fatima Pathan2, Dr. Vishnudas Bhandari3, Dr. Kanishka Magdum4 1(Reader, Department of periodontology, MIDSR dental college latur. India) 2(Postgraduate student, Department of periodontology, MIDSR dental college, latur, India) 3(Professor and HOD, Department of periodontology, MIDSR dental college, latur. India) 4(Postgraduate student, Department of periodontology, MIDSR dental college latur, India) Abstract: Gingival recession has been defined as the apical shift of gingival margin from its physiologic level causing exposure of root surfaces. Patient with gingival recession frequently report to dental clinics with complaint ofreceding gums, pain or hypersensitivity, esthetic problem, retention of plaque, inflamed gingiva. This apical shift in gingiva causes reduction in width of attached gingiva and vestibular depth which may lead to sub gingival plaque accumulation and difficulty in oral hygiene maintenance.There are various techniques to treat gingival recession and to increase width of keratinized gingiva. This article puts emphasis on case report in which evaluation of increase in width of keratinized gingiva is done using functional method -

Efficacy of Bone Substitute Material in Preserving Volume When Placing A
Rignon-Bret et al. Trials (2016) 17:255 DOI 10.1186/s13063-016-1380-7 STUDY PROTOCOL Open Access Efficacy of bone substitute material in preserving volume when placing a maxillary immediate complete denture: study protocol for the PANORAMIX randomized controlled trial Christophe Rignon-Bret1,2*, Alain Hadida1,3, Alexis Aidan1, Thien-Huong Nguyen4, Gerard Pasquet4, Helene Fron-Chabouis2,5 and Claudine Wulfman2,6 Abstract Background: Bone preservation is an essential issue in the context of last teeth extraction and complete edentulism. The intended treatment, whether a complete denture or an implant placement, is facilitated with a voluminous residual ridge. Bone resorption after multiple extractions has not been as well studied as the bone resorption that occurs after the extraction of a single tooth. Recent advances in bone substitute materials have revived this issue. The purpose of this study is to evaluate the interest in using bone substitute material to fill the socket after last teeth extraction in a maxillary immediate complete denture procedure compared with the conventional protocol without socket filling. Methods/design: A randomized, controlled, clinical trial was designed. The 34 participants eligible for maxillary immediate complete denture were divided into two groups. Complete dentures were prepared despite persistence of the last anterior teeth. The control group received a conventional treatment including denture placement immediately after extractions. In the experimental group, in addition to the immediate denture placement, a xenograft bone-substitute material (Bio-Oss Collagen®) was placed in the fresh sockets. The primary outcome of the study is to compare mean bone ridge height loss 1 year after maxillary immediate complete denture placement, with or without bone-substitute material, in incisor and canine sockets.