Trigeminal Nerve Anatomy
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Palatal Injection Does Not Block the Superior Alveolar Nerve Trunks: Correcting an Error Regarding the Innervation of the Maxillary Teeth
Open Access Review Article DOI: 10.7759/cureus.2120 Palatal Injection does not Block the Superior Alveolar Nerve Trunks: Correcting an Error Regarding the Innervation of the Maxillary Teeth Joe Iwanaga 1 , R. Shane Tubbs 2 1. Seattle Science Foundation 2. Neurosurgery, Seattle Science Foundation Corresponding author: Joe Iwanaga, [email protected] Abstract The superior alveolar nerves course lateral to the maxillary sinus and the greater palatine nerve travels through the hard palate. This difficult three-dimensional anatomy has led some dentists and oral surgeons to a critical misunderstanding in developing the anterior and middle superior alveolar (AMSA) nerve block and the palatal approach anterior superior alveolar (P-ASA) nerve block. In this review, the anatomy of the posterior, middle and anterior superior alveolar nerves, greater palatine nerve, and nasopalatine nerve are revisited in order to clarify the anatomy of these blocks so that the perpetuated anatomical misunderstanding is rectified. We conclude that the AMSA and P-ASA nerve blockades, as currently described, are not based on accurate anatomy. Categories: Anesthesiology, Medical Education, Other Keywords: anatomy, innervation, local anesthesia, maxillary nerve, nerve block, tooth Introduction And Background Anesthetic blockade of the posterior superior alveolar (PSA) branch of the maxillary nerve has played an important role in the endodontic treatment of irreversible acute pulpitis of the upper molar teeth except for the mesiobuccal root of the first molar tooth [1, 2]. This procedure requires precise anatomical knowledge of the pterygopalatine fossa and related structures in order to avoid unnecessary complications and to make the blockade most effective. The infraorbital nerve gives rise to middle superior alveolar (MSA) and anterior superior alveolar (ASA) branches. -

Nerves of the Orbit Optic Nerve the Optic Nerve Enters the Orbit from the Middle Cranial Fossa by Passing Through the Optic Canal
human anatomy 2016 lecture fourteen Dr meethak ali ahmed neurosurgeon Nerves of the Orbit Optic Nerve The optic nerve enters the orbit from the middle cranial fossa by passing through the optic canal . It is accompanied by the ophthalmic artery, which lies on its lower lateral side. The nerve is surrounded by sheath of pia mater, arachnoid mater, and dura mater. It runs forward and laterally within the cone of the recti muscles and pierces the sclera at a point medial to the posterior pole of the eyeball. Here, the meninges fuse with the sclera so that the subarachnoid space with its contained cerebrospinal fluid extends forward from the middle cranial fossa, around the optic nerve, and through the optic canal, as far as the eyeball. A rise in pressure of the cerebrospinal fluid within the cranial cavity therefore is transmitted to theback of the eyeball. Lacrimal Nerve The lacrimal nerve arises from the ophthalmic division of the trigeminal nerve. It enters the orbit through the upper part of the superior orbital fissure and passes forward along the upper border of the lateral rectus muscle . It is joined by a branch of the zygomaticotemporal nerve, whi(parasympathetic secretomotor fibers). The lacrimal nerve ends by supplying the skin of the lateral part of the upper lid. Frontal Nerve The frontal nerve arises from the ophthalmic division of the trigeminal nerve. It enters the orbit through the upper part of the superior orbital fissure and passes forward on the upper surface of the levator palpebrae superioris beneath the roof of the orbit . -

Regional Anesthesia in Head and Neck Surgery
TITLE: Regional Anesthesia in Head and Neck Surger SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: May 24, 2006 RESIDENT PHYSICIAN: Jacques Peltier, MD FACULTY PHYSICIAN: Francis B. Quinn, MD SERIES EDITORS: Francis B. Quinn, Jr., MD and Matthew W. Ryan, MD "This material was prepared by resident physicians in partial fulfillment of educational requirements established for the Postgraduate Training Program of the UTMB Department of Otolaryngology/Head and Neck Surgery and was not intended for clinical use in its present form. It was prepared for the purpose of stimulating group discussion in a conference setting. No warranties, either express or implied, are made with respect to its accuracy, completeness, or timeliness. The material does not necessarily reflect the current or past opinions of members of the UTMB faculty and should not be used for purposes of diagnosis or treatment without consulting appropriate literature sources and informed professional opinion." Introduction Local anesthetic techniques were popularized early in the history of surgery with the advent of injectable nerve blocking agents. Until their discovery, patients were either held down or knocked unconscious to perform procedures. In the early days of general anesthesia, local anesthesia was preferred in all cases that it was applicable due to the significant risks associated with general anesthesia. Many procedures performed today under general anesthesia, such as tonsillectomy, rhinoplasty, and even bronchoscopy, were performed under local anesthesia to avoid the perils of general anesthetics. With the introduction of pulse oximetry, safer inhaled anesthetics, and combined intravenous and inhaled general anesthesia techniques, general anesthesia has become much safer, resulting in many surgeons being unfamiliar with regional nerve blocks to perform surgery. -

Maxillary Nerve-Mediated Postseptoplasty Nasal Allodynia: a Case Report
E CASE REPORT Maxillary Nerve-Mediated Postseptoplasty Nasal Allodynia: A Case Report Shikha Sharma, MD, PhD,* Wilson Ly, MD, PharmD,* and Xiaobing Yu, MD*† Endoscopic nasal septoplasty is a commonly performed otolaryngology procedure, not known to cause persistent postsurgical pain or hypersensitivity. Here, we discuss a unique case of persis- tent nasal pain that developed after a primary endoscopic septoplasty, which then progressed to marked mechanical and thermal allodynia following a revision septoplasty. Pain symptoms were found to be mediated by the maxillary division of the trigeminal nerve and resolved after percuta- neous radiofrequency ablation (RFA) of bilateral maxillary nerves. To the best of our knowledge, this is the first report of maxillary nerve–mediated nasal allodynia after septoplasty. (A&A Practice. 2020;14:e01356.) GLOSSARY CT = computed tomography; FR = foramen rotundum; HIPAA = Health Insurance Portability and Accountability Act; ION = infraorbital nerve; LPP = lateral pterygoid plate; MRI = magnetic reso- nance imaging; RFA = radiofrequency ablation; SPG = sphenopalatine ganglion; US = ultrasound ndoscopic nasal septoplasty is a common otolaryn- septoplasty for chronic nasal obstruction with resection of gology procedure with rare incidence of postsurgical the cartilage inferiorly and posteriorly in 2010. Before this Ecomplications. Minor complications include epistaxis, surgery, the patient only occasionally experienced mild septal hematoma, septal perforation, cerebrospinal fluid leak, headaches. However, his postoperative course was compli- and persistent obstruction.1 Numbness or hypoesthesia of the cated by significant pain requiring high-dose opioids. After anterior palate, secondary to injury to the nasopalatine nerve, discharge, patient continued to have persistent deep, “ach- has been reported, but is usually rare and temporary, resolv- ing” nasal pain which radiated toward bilateral forehead ing over weeks to months.2 Acute postoperative pain is also and incisors. -

Anatomy of Maxillary and Mandibular Local Anesthesia
Anatomy of Mandibular and Maxillary Local Anesthesia Patricia L. Blanton, Ph.D., D.D.S. Professor Emeritus, Department of Anatomy, Baylor College of Dentistry – TAMUS and Private Practice in Periodontics Dallas, Texas Anatomy of Mandibular and Maxillary Local Anesthesia I. Introduction A. The anatomical basis of local anesthesia 1. Infiltration anesthesia 2. Block or trunk anesthesia II. Review of the Trigeminal Nerve (Cranial n. V) – the major sensory nerve of the head A. Ophthalmic Division 1. Course a. Superior orbital fissure – root of orbit – supraorbital foramen 2. Branches – sensory B. Maxillary Division 1. Course a. Foramen rotundum – pterygopalatine fossa – inferior orbital fissure – floor of orbit – infraorbital 2. Branches - sensory a. Zygomatic nerve b. Pterygopalatine nerves [nasal (nasopalatine), orbital, palatal (greater and lesser palatine), pharyngeal] c. Posterior superior alveolar nerves d. Infraorbital nerve (middle superior alveolar nerve, anterior superior nerve) C. Mandibular Division 1. Course a. Foramen ovale – infratemporal fossa – mandibular foramen, Canal -> mental foramen 2. Branches a. Sensory (1) Long buccal nerve (2) Lingual nerve (3) Inferior alveolar nerve -> mental nerve (4) Auriculotemporal nerve b. Motor (1) Pterygoid nerves (2) Temporal nerves (3) Masseteric nerves (4) Nerve to tensor tympani (5) Nerve to tensor veli palatine (6) Nerve to mylohyoid (7) Nerve to anterior belly of digastric c. Both motor and sensory (1) Mylohyoid nerve III. Usual Routes of innervation A. Maxilla 1. Teeth a. Molars – Posterior superior alveolar nerve b. Premolars – Middle superior alveolar nerve c. Incisors and cuspids – Anterior superior alveolar nerve 2. Gingiva a. Facial/buccal – Superior alveolar nerves b. Palatal – Anterior – Nasopalatine nerve; Posterior – Greater palatine nerves B. -

Communication Between the Mylohyoid and Lingual Nerves: Clinical Implications
Int. J. Morphol., Case Report 25(3):561-564, 2007. Communication Between the Mylohyoid and Lingual Nerves: Clinical Implications Comunicación entre los Nervios Milohioideo y Lingual: Implicancias Clínicas *Valéria Paula Sassoli Fazan; **Omar Andrade Rodrigues Filho & ***Fernando Matamala FAZAN, V. P. S.; RODRIGUES FILHO, O. A. & MATAMALA, F. Communication between the mylohyoid and lingual nerves: Clinical implications. Int. J. Morphol., 25(3):561-564, 2007. SUMMARY: The mylohyoid muscle plays an important role in chewing, swallowing, respiration and phonation, being the mylohyoid nerve also closely related to these important functions. It has been postulated that the mylohyoid nerve might have a role in the sensory innervation of the chin and the lower incisor teeth while the role of the mylohyoid nerve in the mandibular posterior tooth sensation is still a controversial issue. Although variations in the course of the mylohyoid nerve in relation to the mandible are frequently found on the dissecting room, they have not been satisfactorily described in the anatomical or surgical literature. It is well known that variations on the branching pattern of the mandibular nerve frequently account for the failure to obtain adequate local anesthesia in routine oral and dental procedures and also for the unexpected injury to branches of the nerves during surgery. Also, anatomical variations might be responsible for unexpected and unexplained symptoms after a certain surgical procedure. We describe the presence of a communicating branch between the mylohyoid and lingual nerves in an adult male cadaver, and discuss its clinical/surgical implications as well as its possible role on the sensory innervation of the tongue. -

Local Anaesthesia for Descriptive Purposes It Is Convenient to Sub-Divide Local Anaesthesia on an Anatomical Basis Into Topical, Infiltration, and Regional Techniques
Fundamentals of technique The importance of a quiet, confident, and friendly manner towards all patients so physical comfort is also essential for the co-operation of the patient and the ease of operation of the dental surgeon. The patient should be seated in a semi-reclining position with the back and legs supported and with head rest in the nape of the neck. Most adult patients will respond to the dental surgeon's endeavors to gain the patient his or her confidence and so premedication will not be required for the administration of a local anaesthetic for a relatively simple procedure. Types of local anaesthesia For descriptive purposes it is convenient to sub-divide local anaesthesia on an anatomical basis into topical, infiltration, and regional techniques. Topical or surface anaesthesia: is obtained by the application of a suitable anaesthetic agents to an area of either skin or mucous membrane which it penetrates to anaesthetize superficial nerve-ending. It is most commonly used to obtain anaesthesia of mucosa prior to injection. Spray: containing an appropriate local anaesthetic agent are particularly suitable for this purpose because of their rapidity of action. The active ingredient is 10% lignocaine hydrochloride. When used as a spray it is very easy to spread the solution, and its effect, much more extensively than is desired. The onset time of anaesthesia is about 1 minute and the duration round about 10 minute. Ethyl chloride: when sprayed on skin or mucosa volatilizes to rapidly produces anaesthesia by refrigeration. This phenomenon is of clinical value only when spray directed at a limited area until snow appears.\This technique is of limited value is occasionally used to produce surface anaesthesia prior to incision of a fluctuant abscesses. -

Simple Ways to Dissect Ciliary Ganglion for Orbital Anatomical Education
OkajimasDetection Folia Anat. of ciliary Jpn., ganglion94(3): 119–124, for orbit November, anatomy 2017119 Simple ways to dissect ciliary ganglion for orbital anatomical education By Ming ZHOU, Ryoji SUZUKI, Hideo AKASHI, Akimitsu ISHIZAWA, Yoshinori KANATSU, Kodai FUNAKOSHI, Hiroshi ABE Department of Anatomy, Akita University Graduate School of Medicine, Akita, 010-8543 Japan –Received for Publication, September 21, 2017– Key Words: ciliary ganglion, orbit, human anatomy, anatomical education Summary: In the case of anatomical dissection as part of medical education, it is difficult for medical students to find the ciliary ganglion (CG) since it is small and located deeply in the orbit between the optic nerve and the lateral rectus muscle and embedded in the orbital fat. Here, we would like to introduce simple ways to find the CG by 1): tracing the sensory and parasympathetic roots to find the CG from the superior direction above the orbit, 2): transecting and retracting the lateral rectus muscle to visualize the CG from the lateral direction of the orbit, and 3): taking out whole orbital structures first and dissecting to observe the CG. The advantages and disadvantages of these methods are discussed from the standpoint of decreased laboratory time and students as beginners at orbital anatomy. Introduction dissection course for the first time and with limited time. In addition, there are few clear pictures in anatomical The ciliary ganglion (CG) is one of the four para- textbooks showing the morphology of the CG. There are sympathetic ganglia in the head and neck region located some scientific articles concerning how to visualize the behind the eyeball between the optic nerve and the lateral CG, but they are mostly based on the clinical approaches rectus muscle in the apex of the orbit (Siessere et al., rather than based on the anatomical procedure for medical 2008). -
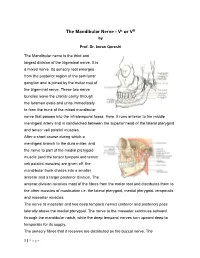
The Mandibular Nerve - Vc Or VIII by Prof
The Mandibular Nerve - Vc or VIII by Prof. Dr. Imran Qureshi The Mandibular nerve is the third and largest division of the trigeminal nerve. It is a mixed nerve. Its sensory root emerges from the posterior region of the semilunar ganglion and is joined by the motor root of the trigeminal nerve. These two nerve bundles leave the cranial cavity through the foramen ovale and unite immediately to form the trunk of the mixed mandibular nerve that passes into the infratemporal fossa. Here, it runs anterior to the middle meningeal artery and is sandwiched between the superior head of the lateral pterygoid and tensor veli palatini muscles. After a short course during which a meningeal branch to the dura mater, and the nerve to part of the medial pterygoid muscle (and the tensor tympani and tensor veli palatini muscles) are given off, the mandibular trunk divides into a smaller anterior and a larger posterior division. The anterior division receives most of the fibres from the motor root and distributes them to the other muscles of mastication i.e. the lateral pterygoid, medial pterygoid, temporalis and masseter muscles. The nerve to masseter and two deep temporal nerves (anterior and posterior) pass laterally above the medial pterygoid. The nerve to the masseter continues outward through the mandibular notch, while the deep temporal nerves turn upward deep to temporalis for its supply. The sensory fibres that it receives are distributed as the buccal nerve. The 1 | P a g e buccal nerve passes between the medial and lateral pterygoids and passes downward and forward to emerge from under cover of the masseter with the buccal artery. -

PERFORATION of INFERIOR ALVEOLAR NERVE by MAXILLARY ARTERY Prakash Billakanti Babu, Ramachandra Bhat K, Vanishree S Nayak
Inferior alveolar nerve Rev Arg de Anat Clin; 2011, 3 (3): 124-129 __________________________________________________________________________________________ Case report PERFORATION OF INFERIOR ALVEOLAR NERVE BY MAXILLARY ARTERY Prakash Billakanti Babu, Ramachandra Bhat K, Vanishree S Nayak Kasturba Medical College, Manipal University, Manipal, Karnataka, India RESUMEN La fosa infratemporal es un área anatómica inferior alveolar nerve originated from the clínicamente importante para la administración de mandibular nerve by two roots and the first part agentes anestésicos locales en odontología y cirugía of the maxillary artery was incorporated between maxilofacial. Fueron estudiadas variaciones en la them. An embryologic origin of this variation and anatomía del nervio alveolar inferior y la arteria maxilar its clinical implications is discussed. Because the en la disección infratemporal. Durante la disección rutinaria de la cabeza en el cadáver de un varón maxillary artery runs between the two roots of the adulto, fue observada una variación excepcional en el inferior alveolar nerve, and the nerve was fixed origen del nervio alveolar inferior y su relación con las between the foramen ovale and mandibular estructuras circundantes. El nervio alveolar inferior se foramen, neurovascular entrapment may cause originaba en el nervio mandibular por dos raíces y la pain numbness or headache and may interfere primera parte de la arteria maxilar estaba incorporada with the injection of local anesthetics into the entre ambas. El origen embriológico de esta variación infratemporal fossa. Anatomical variations in this y sus implicaciones clínicas es debatido. Dado que la region should be kept in mind, particularly in arteria maxilar transcurría entre las dos raíces del cases of failed treatment of trigeminal neuralgia. -

Cranial Neuralgias
CRANIAL NEURALGIAS Presented by: Neha Sharma M.D. Date: September 27th, 2019 TYPES OF NEURALGIAS ❖ TRIGEMINAL NEURALGIA ❖ GLOSSOPHARYNGEAL NEURALGIA ❖ NASOCILIARY NEURALGIA ❖ SUPERIOR LARYNGEAL NEURALGIA ❖ SUPRAORBITAL NEURALGIA ❖ OCCIPITAL NEURALGIA ❖ SPHENOPALATINE NEURALGIA ❖ GREAT AURICULAR NEURALGIA ❖ NERVUS INTERMEDIUS NEURALGIA ❖ TROCHLEAR NEURALGIA WHAT IS CRANIAL NEURALGIA? ❖ Paroxysmal pain of head, face and/or neck ❖ Unilateral sensory nerve distribution ❖ Pain is described as sharp, shooting, lancinating ❖ Primary or Secondary causes ❖ Multiple triggers TRIGEMINAL (CN V) NEURALGIA TRIGEMINAL NEURALGIA ❖ Also called Tic Douloureux ❖ Sudden, unilateral, electrical, shock-like, shooting, sharp pain. Presents affecting Cranial Nerve V; primarily V2 and V3 branches ❖ F>M; 3:1 TRIGEMINAL NEURALGIA ❖ Anatomy of Trigeminal Nerve ❖ Cranial Nerve V ❖ Three Branches: Ophthalmic, Maxillary and Mandibular ❖ Sensory supply to forehead/supraorbital, cheeks and jaw https://www.nf2is.org/cn5.php TRIGEMINAL NEURALGIA – TRIGGERS ❖ Mastication (73%) ❖ Eating (59%) ❖ Touch (69%) ❖ Talking (58%) ❖ Brushing Teeth (66%) ❖ Cold wind (50%) TYPES OF TRIGEMINAL NEURALGIA ❖ Primary/Classic/Idiopathic ❖ Vascular compression of the nerve – superior cerebellar artery ❖ Secondary/Symptomatic ❖ Caused by intracranial lesions ❖ Tumors, Strokes, Multiple Sclerosis (4%) ❖ Typical vs. Atypical ❖ Paroxysmal (79%) vs. Continuous (21%) IASP/IHS & CLASSIFICATIONS OF TRIGEMINAL NEURALGIA ❖ IASP – International Association ❖ Classifications for the Study of Pain ❖ I -

Clinical Anatomy of the Trigeminal Nerve
Clinical Anatomy of Trigeminal through the superior orbital fissure Nerve and courses within the lateral wall of the cavernous sinus on its way The trigeminal nerve is the fifth of to the trigeminal ganglion. the twelve cranial nerves. Often Ophthalmic Nerve is formed by the referred to as "the great sensory union of the frontal nerve, nerve of the head and neck", it is nasociliary nerve, and lacrimal named for its three major sensory nerve. Branches of the ophthalmic branches. The ophthalmic nerve nerve convey sensory information (V1), maxillary nerve (V2), and from the skin of the forehead, mandibular nerve (V3) are literally upper eyelids, and lateral aspects "three twins" carrying information of the nose. about light touch, temperature, • The maxillary nerve (V2) pain, and proprioception from the enters the middle cranial fossa face and scalp to the brainstem. through foramen rotundum and may or may not pass through the • The three branches converge on cavernous sinus en route to the the trigeminal ganglion (also called trigeminal ganglion. Branches of the semilunar ganglion or the maxillary nerve convey sensory gasserian ganglion), which contains information from the lower eyelids, the cell bodies of incoming sensory zygomae, and upper lip. It is nerve fibers. The trigeminal formed by the union of the ganglion is analogous to the dorsal zygomatic nerve and infraorbital root ganglia of the spinal cord, nerve. which contain the cell bodies of • The mandibular nerve (V3) incoming sensory fibers from the enters the middle cranial fossa rest of the body. through foramen ovale, coursing • From the trigeminal ganglion, a directly into the trigeminal single large sensory root enters the ganglion.