Skin Infection (Cellulitis) N
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Cutaneous Manifestations of HIV Infection Carrie L
Chapter Title Cutaneous Manifestations of HIV Infection Carrie L. Kovarik, MD Addy Kekitiinwa, MB, ChB Heidi Schwarzwald, MD, MPH Objectives Table 1. Cutaneous manifestations of HIV 1. Review the most common cutaneous Cause Manifestations manifestations of human immunodeficiency Neoplasia Kaposi sarcoma virus (HIV) infection. Lymphoma 2. Describe the methods of diagnosis and treatment Squamous cell carcinoma for each cutaneous disease. Infectious Herpes zoster Herpes simplex virus infections Superficial fungal infections Key Points Angular cheilitis 1. Cutaneous lesions are often the first Chancroid manifestation of HIV noted by patients and Cryptococcus Histoplasmosis health professionals. Human papillomavirus (verruca vulgaris, 2. Cutaneous lesions occur frequently in both adults verruca plana, condyloma) and children infected with HIV. Impetigo 3. Diagnosis of several mucocutaneous diseases Lymphogranuloma venereum in the setting of HIV will allow appropriate Molluscum contagiosum treatment and prevention of complications. Syphilis Furunculosis 4. Prompt diagnosis and treatment of cutaneous Folliculitis manifestations can prevent complications and Pyomyositis improve quality of life for HIV-infected persons. Other Pruritic papular eruption Seborrheic dermatitis Overview Drug eruption Vasculitis Many people with human immunodeficiency virus Psoriasis (HIV) infection develop cutaneous lesions. The risk of Hyperpigmentation developing cutaneous manifestations increases with Photodermatitis disease progression. As immunosuppression increases, Atopic Dermatitis patients may develop multiple skin diseases at once, Hair changes atypical-appearing skin lesions, or diseases that are refractory to standard treatment. Skin conditions that have been associated with HIV infection are listed in Clinical staging is useful in the initial assessment of a Table 1. patient, at the time the patient enters into long-term HIV care, and for monitoring a patient’s disease progression. -

Cutaneous Manifestations of Newborns in Omdurman Maternity Hospital
ﺑﺴﻢ اﷲ اﻟﺮﺣﻤﻦ اﻟﺮﺣﻴﻢ Cutaneous Manifestations of Newborns in Omdurman Maternity Hospital A thesis submitted in the partial fulfillment of the degree of clinical MD in pediatrics and child health University of Khartoum By DR. AMNA ABDEL KHALIG MOHAMED ATTAR MBBS University of Khartoum Supervisor PROF. SALAH AHMED IBRAHIM MD, FRCP, FRCPCH Department of Pediatrics and Child Health University of Khartoum University of Khartoum The Graduate College Medical and Health Studies Board 2008 Dedication I dedicate my study to the Department of Pediatrics University of Khartoum hoping to be a true addition to neonatal care practice in Sudan. i Acknowledgment I would like to express my gratitude to my supervisor Prof. Salah Ahmed Ibrahim, Professor of Peadiatric and Child Health, who encouraged me throughout the study and provided me with advice and support. I am also grateful to Dr. Osman Suleiman Al-Khalifa, the Dermatologist for his support at the start of the study. Special thanks to the staff at Omdurman Maternity Hospital for their support. I am also grateful to all mothers and newborns without their participation and cooperation this study could not be possible. Love and appreciation to my family for their support, drive and kindness. ii Table of contents Dedication i Acknowledgement ii Table of contents iii English Abstract vii Arabic abstract ix List of abbreviations xi List of tables xiii List of figures xiv Chapter One: Introduction & Literature Review 1.1 The skin of NB 1 1.2 Traumatic lesions 5 1.3 Desquamation 8 1.4 Lanugo hair 9 1.5 -
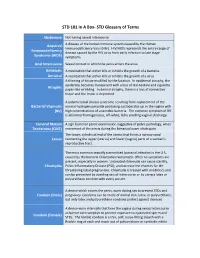
STD Glossary of Terms
STD 101 In A Box- STD Glossary of Terms Abstinence Not having sexual intercourse Acquired A disease of the human immune system caused by the Human Immunodeficiency Virus (HIV). HIV/AIDS represents the entire range of Immunodeficiency disease caused by the HIV virus from early infection to late stage Syndrome (AIDS) symptoms. Anal Intercourse Sexual contact in which the penis enters the anus. Antibiotic A medication that either kills or inhibits the growth of a bacteria. Antiviral A medication that either kills or inhibits the growth of a virus. A thinning of tissue modified by the location. In epidermal atrophy, the epidermis becomes transparent with a loss of skin texture and cigarette Atrophic paper-like wrinkling. In dermal atrophy, there is a loss of connective tissue and the lesion is depressed. A polymicrobial clinical syndrome resulting from replacement of the Bacterial Vaginosis normal hydrogen peroxide producing Lactobacillus sp. in the vagina with (BV) high concentrations of anaerobic bacteria. The common symptom of BV is abnormal homogeneous, off-white, fishy smelling vaginal discharge. Cervical Motion A sign found on pelvic examination suggestive of pelvic pathology; when Tenderness (CMT) movement of the cervix during the bimanual exam elicits pain. The lower, cylindrical end of the uterus that forms a narrow canal Cervix connecting the upper (uterus) and lower (vagina) parts of a woman's reproductive tract. The most common sexually transmitted bacterial infection in the U.S., caused by the bacteria Chlamydia trachomatis. Often no symptoms are present, especially in women. Untreated chlamydia can cause sterility, Chlamydia Pelvic Inflammatory Disease (PID), and increase the chances for life- threatening tubal pregnancies. -

Survey of Skin Disorders in Newborns: Clinical Observation in an Egyptian Medical Centre Nursery A.A
املجلة الصحية لرشق املتوسط املجلد الثامن عرش العدد اﻷول Survey of skin disorders in newborns: clinical observation in an Egyptian medical centre nursery A.A. El-Moneim 1 and R.E. El-Dawela 2 مسح لﻻضطرابات اجللدية لدى الولدان: مﻻحظة رسيرية يف حضانة يف مركز طبي يف مرص عبري أمحد عبد املنعم، رهيام عز الدولة الرشقاوي اخلﻻصة:مل َ ْت َظ اﻻضطرابات اجللدية لدى الولدان بدراسات جيدة يف مرص. وقد هدفت الباحثتان إىل دراسة أنامط التغريات اجللدية يف عينة من ِ الولدان املرصيني، وهي دراسة وصفية استباقية أترابية شملت ستة مئة وليد يف َّحضانة يف مستشفى جامعة سوهاج، َّوتضمنت الفحص اجللدي خﻻل اﻷيام اخلمسة اﻷوىل بعد الوﻻدة. وقد تم كشف اﻻضطرابات اجللدية لدى 240 ًوليدا )40%( ولوحظت الومحات لدى 100 وليد )%16.7(، ومعظمها من النمط ذي اخلﻻيا امليﻻنية )لطخات منغولية لدى 11.7% مع ومحات وﻻدية ذات ميﻻنية اخلﻻيا لدى 2.7%(. كام ُك ِش َف ْت العداوى الفطرية اجللدية، ومنها داء َّاملبيضات الفموية، وعدوى الفطريات يف مناطق احلفاظات أو َالـم َذح الناجم عن عدوى َّاملبيضات يف اﻷرفاغ )أصل الفخذ(، وذلك لدى 13.3%، ُوكشفت بعض العداوى اجلرثومية يف 1.3%من الولدان. وتشري املقارنات مع الدراسات اﻷخرى يف أرجاء العامل إىل معدل مرتفع للعدوى بالفطريات مع معدل منخفض للومحات الوﻻدية يف دراستنا للولدان، وتويص الباحثتان بإجراء تقييم روتيني جلدي للولدان، ّوﻻسيام يف ضوء املعدﻻت املرتفعة للعدوى اجللدية بالفطريات. ABSTRACT The frequency of neonatal skin disorders has not been well studied in Egypt. Our aim was to address patterns of dermatological changes in a sample of Egyptian newborns. In a descriptive prospective cohort study 600 newborns in Sohag University hospital nursery were dermatologically examined within the first 5 days of birth. -

Non-Dermatomal Varicella-Zoster Skin Infection: Disseminated Cutaneous Herpes Zoster Without Dermatome in an Immunosuppressed Woman
Volume 23 Number 10 | October 2017 Dermatology Online Journal || Case Report DOJ 23 (10): 4 Non-dermatomal varicella-zoster skin infection: disseminated cutaneous herpes zoster without dermatome in an immunosuppressed woman Lindsay P Osborn1 BA,, Philip R Cohen2 MD Affiliations: 1Medical College of Georgia, Augusta, Georgia, 2University of California, San Diego, California Corresponding Author: Lindsay P. Osborn, 1 Seventh Street, Suite 1403, Augusta, GA 30901, Email: [email protected] Introduction Abstract Herpes viral infection in humans includes both Disseminated herpes zoster is defined as the presence herpes simplex (HSV) and herpes zoster. The varicella of more than 20 lesions outside the dermatome. zoster virus (VZV) is the etiology of both primary This unusual presentation is more common in varicella and herpes zoster (commonly known as immunosuppressed patients. Complications such chicken pox and shingles, respectively), with herpes as hepatitis, encephalitis, and pneumonitis are more zoster being the re-activated form of the virus. The likely in individuals with disseminated varicella zoster classical presentation of herpes zoster is a unilateral virus infection. distribution of vesicles along a single or adjacent dermatome [1]. Disseminated herpes zoster is A 63-year-old woman being treated for breast cancer defined as having more than 20 lesions outside the developed multiple pustules and vesicles days primary or adjacent dermatome [2]. after starting doxorubicin and cyclophosphamide chemotherapy. Ten individual lesions appeared on Although uncommon among all herpes zoster her chest, abdomen, back, and leg. Non-dermatomal infections, the prevalence of disseminated VZV in disseminated herpes zoster was suspected. She was a setting of immunosuppression is thought to be treated with oral antiviral therapy, as well as with oral anywhere from 10 to 40% [3, 4]. -

Cellulitis: a Review of 62
Clinical Review & Education Review Cellulitis A Review Adam B. Raff, MD, PhD; Daniela Kroshinsky, MD, MPH CME Quiz at IMPORTANCE Cellulitis is an infection of the deep dermis and subcutaneous tissue, presenting jamanetworkcme.com with expanding erythema, warmth, tenderness, and swelling. Cellulitis is a common global health burden, with more than 650 000 admissions per year in the United States alone. OBSERVATIONS In the United States, an estimated 14.5 million cases annually of cellulitis account for $3.7 billion in ambulatory care costs alone. The majority of cases of cellulitis are nonculturable and therefore the causative bacteria are unknown. In the 15% of cellulitis cases in which organisms are identified, most are due to β-hemolytic Streptococcus and Staphylococcus aureus. There are no effective diagnostic modalities, and many clinical conditions appear similar. Treatment of primary and recurrent cellulitis should initially cover Streptococcus and methicillin-sensitive S aureus, with expansion for methicillin-resistant S aureus (MRSA) in cases of cellulitis associated with specific risk factors, such as athletes, children, men who have sex with men, prisoners, military recruits, residents of long-term care facilities, those with prior MRSA exposure, and intravenous drug users. Five days of treatment is sufficient with extension if symptoms are not improved. Addressing predisposing factors can minimize risk of recurrence. CONCLUSIONS AND RELEVANCE The diagnosis of cellulitis is based primarily on history and Author Affiliations: Harvard Medical physical examination. Treatment of uncomplicated cellulitis should be directed against School, Massachusetts General Streptococcus and methicillin-sensitive S aureus. Failure to improve with appropriate first-line Hospital, Boston. antibiotics should prompt consideration for resistant organisms, secondary conditions that Corresponding Author: Daniela mimic cellulitis, or underlying complicating conditions such as immunosuppression, chronic Kroshinsky, MD, MPH, liver disease, or chronic kidney disease. -

Bacterial Skin and Soft Tissue Infections
VOLUME 39 : NUMBER 5 : OCTOBER 2016 ARTICLE Bacterial skin and soft tissue infections Vichitra Sukumaran SUMMARY Advanced trainee1 Sanjaya Senanayake Bacterial skin infections are common presentations to both general practice and the Senior specialist1 emergency department. Associate professor of 2 The optimal treatment for purulent infections such as boils and carbuncles is incision and medicine drainage. Antibiotic therapy is not usually required. 1 Infectious Diseases Most uncomplicated bacterial skin infections that require antibiotics need 5–10 days of treatment. Canberra Hospital 2 Australian National There is a high prevalence of purulent skin infections caused by community-acquired University Medical School (non‑multiresistant) methicillin-resistant Staphylococcus aureus. It is therefore important to Canberra provide adequate antimicrobial coverage for these infections in empiric antibiotic regimens. Keywords antibiotics, cellulitis, Introduction Cellulitis and erysipelas impetigo, soft tissue It is important to have a good understanding of Both cellulitis and erysipelas manifest as spreading infection the common clinical manifestations and pathogens areas of skin erythema and warmth. Localised involved in bacterial skin infections to be able to infections are often accompanied by lymphangitis and Aust Prescr 2016;39:159–63 manage them appropriately. The type of skin infection lymphadenopathy. Not infrequently, groin pain and http://dx.doi.org/10.18773/ depends on the depth and the skin compartment tenderness due to inguinal lymphadenitis will precede austprescr.2016.058 involved. The classification and management of these the cellulitis. Some patients can be quite unwell with infections are outlined in Table 1. fevers and features of systemic toxicity. Bacteraemia, although uncommon (less than 5%), still occurs. Impetigo Erysipelas involves the upper dermis and superficial Impetigo is a superficial bacterial infection that can lymphatics. -

Cellulitis: Current Insights Into Pathophysiology and Clinical Management
The Netherlands Journal of Medicine REVIEW Cellulitis: current insights into pathophysiology and clinical management D.R. Cranendonk1,2*, A.P.M. Lavrijsen3, J.M. Prins1, W.J. Wiersinga1,2 1Department of Medicine, Academic Medical Center, Amsterdam, the Netherlands, 2Center for Experimental and Molecular Medicine (CEMM), Academic Medical Center, Amsterdam, the Netherlands, 3Department of Dermatology, Leiden University Medical Center, Leiden, the Netherlands, *corresponding author: email: [email protected] A B S T R A C T frequent infections requiring hospitalisation.1 The historical distinction between cellulitis and erysipelas, Cellulitis is a bacterial skin and soft tissue infection which based on different bacterial aetiologies and thus treatment occurs when the physical skin barrier, the immune system options, is becoming obsolete as increasing evidence and/or the circulatory system are impaired. Diabetes, suggests a large overlap between these two entities obesity and old age are associated with defects in all of (textbox 1). In the Netherlands, the annual incidence is these areas and as a result are major predisposing factors estimated to be 22 per 1000 inhabitants. Approximately for cellulitis. In this review, we summarise current insights 7% of all patients with cellulitis are hospitalised.5,6 The into the pathophysiology of cellulitis and place the Dutch mortality rate of hospitalised patients has been reported guidelines on the clinical management of cellulitis of to be around 2.5%.7 Recent epidemiology data on cellulitis the lower extremities in perspective. Recent evidence in the Netherlands are lacking, but given the rise in the on diagnostic strategies is discussed, the importance of incidence of important risk factors (namely diabetes, which is underscored by findings that venous insufficiency, obesity and old age), an increase in the incidence of eczema, deep vein thrombosis and gout are frequently cellulitis is expected.8-10 Dutch guidelines on the clinical mistaken for cellulitis. -

Common Conditions
Common Conditions Alopecia • Alopecia (hair loss) can occur when hair fails to grow • Pyoderma (a bacterial skin infection in which at a normal rate or when hair is lost more quickly skin debris, bacteria, and inflammatory cells than it can grow back. clog and damage the hair follicle) • Alopecia can result from a variety of medical conditions, • Seborrhea (a skin condition in which excessive including skin infections, hormonal diseases, and flaking of skin cells causes clogging of the hair infestations with fleas or mites. follicle) • Many causes of alopecia are treatable. If the hair follicle • Glandular or hormonal diseases (such as has not been permanently damaged or destroyed, the thyroid disease and adrenal gland disease, hair will grow back over time. in which the hair growth cycle is disrupted because of hormonal changes; secondary skin What Is Alopecia? infections or seborrhea can also occur) Alopecia is the medical term used to describe hair loss. Alopecia can occur when hair fails to grow at a Alopecia can result when a pet damages its skin or normal rate, or when hair is lost more quickly than pulls out its hair. Fleas, for example, can cause itchy it can grow back. Alopecia should not be confused pets to pull out their hair and create bald patches. with increased shedding. Shedding (even year-round Pets that are allergic to fleas experience even more shedding in some pets) is a normal process and is intense itching and can remove their hair, create not an illness. Shedding should only be a cause wounds on their skin, and develop secondary bacterial for concern if it is heavy enough to create areas of infections from repetitive scratching and biting. -

Shingles (Herpes Zoster) Brown Health Services Patient Education Series
Shingles (Herpes Zoster) Brown Health Services Patient Education Series What is shingles? What are the symptoms? Shingles, also known as herpes zoster, is a painful Before a rash presents, many people first rash caused by the varicella zoster virus. This is the experience: same virus that causes chickenpox, also known as ● burning, sharp pain, tingling, or numbness varicella. Shingles is a reactivation of the virus, so sensation to one side of the body or face you can get it if you had the chickenpox, or received ○ back and/or abdomen are most the chickenpox vaccine, as a child. The classic common shingles rash consists of painful, blister-like lesions ● severe itching or aching rather than pain appearing in a band or stripe pattern across one ● fatigue, fever, chills, headache, and upset side of the body. In fact, the name “shingles” comes stomach from the Latin word for belt or girdle. After a few days of the burning, pain, and/or How often does it occur? tingling, a rash will likely begin to develop. After you recover from chickenpox or receive the A typical progression of the rash: chickenpox vaccine, the varicella zoster virus remains inactive and dormant in the body. The virus ● starts out as groups of red bumps that turn is usually dormant in the roots of the nerve cells. into small, clear, fluid-filled blisters on Shingles is the result of the varicella zoster virus reddened skin reactivating years later. ● blisters can look similar to chickenpox ● over the next several days, the blisters tend It is unclear what causes the reactivation of the to drain and (within 7-10 days) then crust virus, though a weakened immune system is a over before eventually beginning to common culprit. -

Preventing the Spread of Herpes Gladiatorum Infection (PDF)
Minnesota Department of Health Infection Control Fact Sheet 1/2006 Preventing the spread of Herpes gladiatorum infection General Information Personal hygiene for wrestlers Herpes gladiatorum is a skin infection Showering caused by the Herpes Simplex type 1 1. Shower at school immediately after virus. This skin infection is spread by direct practice, using soap and water. skin-to-skin contact. 2. Use your own plastic bottle of liquid soap. 3. Use your own towel, and don’t share your towel with anyone else. Wash your towel Generally, lesions appear within 8 days after each use, using hot water with after exposure to an infected person, but in detergent (and bleach if possible); and dry some cases the lesions take longer to on high heat setting. appear. Good personal hygiene and thorough cleaning and disinfecting of all Equipment and gear 1. Change your practice and competition gear equipment are essential to helping prevent every day. the spread of this and other skin infections. 2. Clean your headgear daily with the same soap you use for showering. All wrestlers with skin sores or lesions 3. Clean the soles of your shoes before should be referred to a physician for stepping on the mat. Use a towel soaked in evaluation. These individuals should not a disinfectant solution. participate in practice or competition until General hygiene their lesions have healed. 1. Clean your hands often! Scrub up for at least 15 seconds using soap and warm Before skin lesions appear, some people water. You can use an alcohol-based hand have a sore throat, swollen lymph nodes, rub if your hands are not visibly soiled. -

Views in Allergy and Immunology
CLINICAL REVIEWS IN ALLERGY AND IMMUNOLOGY Dermatology for the Allergist Dennis Kim, MD, and Richard Lockey, MD specific laboratory tests and pathognomonic skin findings do Abstract: Allergists/immunologists see patients with a variety of not exist (Table 1). skin disorders. Some, such as atopic and allergic contact dermatitis, There are 3 forms of AD: acute, subacute, and chronic. are caused by abnormal immunologic reactions, whereas others, Acute AD is characterized by intensely pruritic, erythematous such as seborrheic dermatitis or rosacea, lack an immunologic basis. papules associated with excoriations, vesiculations, and se- This review summarizes a select group of dermatologic problems rous exudates. Subacute AD is associated with erythematous, commonly encountered by an allergist/immunologist. excoriated, scaling papules. Chronic AD is associated with Key Words: dermatology, dermatitis, allergy, allergic, allergist, thickened lichenified skin and fibrotic papules. There is skin, disease considerable overlap of these 3 forms, especially with chronic (WAO Journal 2010; 3:202–215) AD, which can manifest in all 3 ways in the same patient. The relationship between AD and causative allergens is difficult to establish. However, clinical studies suggest that extrinsic factors can impact the course of disease. Therefore, in some cases, it is helpful to perform skin testing on foods INTRODUCTION that are commonly associated with food allergy (wheat, milk, llergists/immunologists see patients with a variety of skin soy, egg, peanut, tree nuts, molluscan, and crustaceous shell- Adisorders. Some, such as atopic and allergic contact fish) and aeroallergens to rule out allergic triggers that can dermatitis, are caused by abnormal immunologic reactions, sometimes exacerbate this disease.