Briefing Note on Restriction to Use of Orphenadrine
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
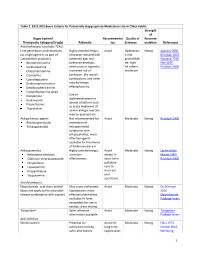
Table 2. 2012 AGS Beers Criteria for Potentially
Table 2. 2012 AGS Beers Criteria for Potentially Inappropriate Medication Use in Older Adults Strength of Organ System/ Recommendat Quality of Recomm Therapeutic Category/Drug(s) Rationale ion Evidence endation References Anticholinergics (excludes TCAs) First-generation antihistamines Highly anticholinergic; Avoid Hydroxyzin Strong Agostini 2001 (as single agent or as part of clearance reduced with e and Boustani 2007 combination products) advanced age, and promethazi Guaiana 2010 Brompheniramine tolerance develops ne: high; Han 2001 Carbinoxamine when used as hypnotic; All others: Rudolph 2008 Chlorpheniramine increased risk of moderate Clemastine confusion, dry mouth, Cyproheptadine constipation, and other Dexbrompheniramine anticholinergic Dexchlorpheniramine effects/toxicity. Diphenhydramine (oral) Doxylamine Use of diphenhydramine in Hydroxyzine special situations such Promethazine as acute treatment of Triprolidine severe allergic reaction may be appropriate. Antiparkinson agents Not recommended for Avoid Moderate Strong Rudolph 2008 Benztropine (oral) prevention of Trihexyphenidyl extrapyramidal symptoms with antipsychotics; more effective agents available for treatment of Parkinson disease. Antispasmodics Highly anticholinergic, Avoid Moderate Strong Lechevallier- Belladonna alkaloids uncertain except in Michel 2005 Clidinium-chlordiazepoxide effectiveness. short-term Rudolph 2008 Dicyclomine palliative Hyoscyamine care to Propantheline decrease Scopolamine oral secretions. Antithrombotics Dipyridamole, oral short-acting* May -

Appendix A: Potentially Inappropriate Prescriptions (Pips) for Older People (Modified from ‘STOPP/START 2’ O’Mahony Et Al 2014)
Appendix A: Potentially Inappropriate Prescriptions (PIPs) for older people (modified from ‘STOPP/START 2’ O’Mahony et al 2014) Consider holding (or deprescribing - consult with patient): 1. Any drug prescribed without an evidence-based clinical indication 2. Any drug prescribed beyond the recommended duration, where well-defined 3. Any duplicate drug class (optimise monotherapy) Avoid hazardous combinations e.g.: 1. The Triple Whammy: NSAID + ACE/ARB + diuretic in all ≥ 65 year olds (NHS Scotland 2015) 2. Sick Day Rules drugs: Metformin or ACEi/ARB or a diuretic or NSAID in ≥ 65 year olds presenting with dehydration and/or acute kidney injury (AKI) (NHS Scotland 2015) 3. Anticholinergic Burden (ACB): Any additional medicine with anticholinergic properties when already on an Anticholinergic/antimuscarinic (listed overleaf) in > 65 year olds (risk of falls, increased anticholinergic toxicity: confusion, agitation, acute glaucoma, urinary retention, constipation). The following are known to contribute to the ACB: Amantadine Antidepressants, tricyclic: Amitriptyline, Clomipramine, Dosulepin, Doxepin, Imipramine, Nortriptyline, Trimipramine and SSRIs: Fluoxetine, Paroxetine Antihistamines, first generation (sedating): Clemastine, Chlorphenamine, Cyproheptadine, Diphenhydramine/-hydrinate, Hydroxyzine, Promethazine; also Cetirizine, Loratidine Antipsychotics: especially Clozapine, Fluphenazine, Haloperidol, Olanzepine, and phenothiazines e.g. Prochlorperazine, Trifluoperazine Baclofen Carbamazepine Disopyramide Loperamide Oxcarbazepine Pethidine -

Hypersalivation in Children and Adults
Pharmacological Management of Hypersalivation in Children and Adults Scope: Adult patients with Parkinson’s disease, children with neurodisability, cerebral palsy, long-term ventilation with drooling, and drug-induced hypersalivation. ASSESSMENT OF SEVERITY/RESPONSE TO TREATMENT: Severity of drooling can be assessed subjectively via discussion with patients and their carers/parents and by observation. Amount of drooling can be quantified by measuring the number of bibs required per day and this can also be graded using the Thomas-Stonell and Greenberg scale: • 1 = Dry (no drooling) • 2 = Mild (moist lips) • 3 = Moderate (wet lips and chin) • 4 = Severe (damp clothing) CONSIDERATIONS FOR PRESCRIBING/TITRATION No evidence to support the use of one particular treatment over another. Drug choice is to be determined by individual patient factors. When prescribing/titrating antimuscarinic drugs to treat hypersalivation always take account of: • Coexisting conditions (for example, history of urinary retention, constipation, glaucoma, dental issues, reflux etc.) • Use of other existing medication affecting the total antimuscarinic burden • Risk of adverse effects Titrate dose upward until the desired level of dryness, side effects or maximum dose reached. Take into account the preferences of the patients and their carers/ parents, and the age range and indication covered by the marketing authorisations (see individual summaries of product characteristics, BNF or BNFc for full prescribing information). FIRST LINE DRUG TREATMENT OPTIONS FOR ADULTS -

Pharmacogenetics of Ketamine Metabolism And
Pharmacogenetics of Ketamine Metabolism and Immunopharmacology of Ketamine Yibai Li B.HSc. (Hons) Discipline of Pharmacology, School of Medical Sciences, Faculty of Health Sciences, The University of Adelaide September 2014 A thesis submitted for the Degree of PhD (Medicine) Table of contents TABLE OF CONTENTS .............................................................................................. I LIST OF FIGURES ....................................................................................................IV LIST OF TABLES ......................................................................................................IV ABSTRACT ............................................................................................................... V DECLARATION .......................................................................................................VIII ACKNOWLEDGEMENTS ..........................................................................................IX ABBREVIATIONS .....................................................................................................XI CHAPTER 1. INTRODUCTION .................................................................................. 1 1.1 A historical overview of ketamine ........................................................................................ 1 1.2 Structure and Chemistry ....................................................................................................... 3 1.3 Classical analgesic mechanisms of ketamine ................................................................... -
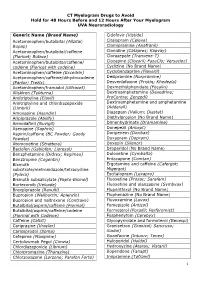
CT Myelogram Drugs to Avoid Hold for 48 Hours Before and 12 Hours After Your Myelogram UVA Neuroradiology
CT Myelogram Drugs to Avoid Hold for 48 Hours Before and 12 Hours After Your Myelogram UVA Neuroradiology Generic Name (Brand Name) Cidofovir (Vistide) Acetaminophen/butalbital (Allzital; Citalopram (Celexa) Bupap) Clomipramine (Anafranil) Acetaminophen/butalbital/caffeine Clonidine (Catapres; Kapvay) (Fioricet; Butace) Clorazepate (Tranxene-T) Acetaminophen/butalbital/caffeine/ Clozapine (Clozaril; FazaClo; Versacloz) codeine (Fioricet with codeine) Cyclizine (No Brand Name) Acetaminophen/caffeine (Excedrin) Cyclobenzaprine (Flexeril) Acetaminophen/caffeine/dihydrocodeine Desipramine (Norpramine) (Panlor; Trezix) Desvenlafaxine (Pristiq; Khedezla) Acetaminophen/tramadol (Ultracet) Dexmethylphenidate (Focalin) Aliskiren (Tekturna) Dextroamphetamine (Dexedrine; Amitriptyline (Elavil) ProCentra; Zenzedi) Amitriptyline and chlordiazepoxide Dextroamphetamine and amphetamine (Limbril) (Adderall) Amoxapine (Asendin) Diazepam (Valium; Diastat) Aripiprazole (Abilify) Diethylpropion (No Brand Name) Armodafinil (Nuvigil) Dimenhydrinate (Dramamine) Asenapine (Saphris) Donepezil (Aricept) Aspirin/caffeine (BC Powder; Goody Doripenem (Doribax) Powder) Doxapram (Dopram) Atomoxetine (Strattera) Doxepin (Silenor) Baclofen (Gablofen; Lioresal) Droperidol (No Brand Name) Benzphetamine (Didrex; Regimex) Duloxetine (Cymbalta) Benztropine (Cogentin) Entacapone (Comtan) Bismuth Ergotamine and caffeine (Cafergot; subcitrate/metronidazole/tetracycline Migergot) (Pylera) Escitalopram (Lexapro) Bismuth subsalicylate (Pepto-Bismol) Fluoxetine (Prozac; Sarafem) -

Topical Treatments of Skin Pain Associated with Hidradenitis Supprurativa
UC Davis Dermatology Online Journal Title Topical treatments of skin pain: a general review with a focus on hidradenitis suppurativa with topical agents Permalink https://escholarship.org/uc/item/4m57506k Journal Dermatology Online Journal, 20(7) Author Scheinfeld, Noah Publication Date 2014 DOI 10.5070/D3207023131 License https://creativecommons.org/licenses/by-nc-nd/4.0/ 4.0 Peer reviewed eScholarship.org Powered by the California Digital Library University of California Volume 20 Number 7 July 2014 Review Topical treatments of skin pain: a general review with a focus on hidradenitis suppurativa with topical agents Noah Scheinfeld MD JD Dermatology Online Journal 20 (7): 3 Assistant Clinical Professor of Dermatology Weil Cornel Medical College Correspondence: Noah Scheinfeld 150 West 55th Street NYC NY 10019 (212) 991-6490 [email protected] Abstract Hidradenitis Supprurativa (HS) is a painful chronic follicular disease. Few papers have addressed pain control for this debilitating condition. Possible topical agents include tricyclic antidepressants, opioids, anticonvulsants, NSAIDs, NMDA receptor antagonists, local anesthetics and other agents. The first line agents for the topical treatment of the cutaneous pain of HS are diclonefac gel 1% and liposomal xylocaine 4% and 5% cream or 5% ointment. The chief advantage of topical xylocaine is that is quick acting i.e. immediate however with a limited duration of effect 1-2 hours. The use of topical ketamine, which blocks n- methyl-D-aspartate receptors in a non-competitive fashion, might be a useful tool for the treatment of HS pain. Topical doxepin, which available in a 5% commercially preparation (Zonalon®) , makes patients drowsy and is not useful for controlling the pain of HS . -

A Brief Overview of Psychotropic Medication Use for Persons with Intellectual Disabilities
A BRIEF OVERVIEW OF PSYCHOTROPIC MEDICATION USE FOR PERSONS WITH INTELLECTUAL DISABILITIES INTRODUCTION Individuals with intellectual disabilities are not uncommonly prescribed psychotropic medications. Too often, historically, such agents have been used to try to improve behavioral control without adequate understanding of the antecedents, purpose, and reinforcement of the problematic behavior. While an individual with an intellectual disability may experience a depressive, anxiety, or psychotic disorder in the more typical sense some individuals experience a pattern of anxiety/alarm/arousal leading to affective dysregulation and impulsive behavior. The anxiety can be stimulated by environmental change, physical discomfort, cues related to past trauma, overstimulation, boredom, confusion, or other unpleasant states. Addressing what is causing the distress or reinforcing the behavioral response is the most important thing (though not always easy). Psychotropic medications may be useful for treating more typically presenting psychiatric illnesses as well as being part of more comprehensive plans to attenuate risk behaviors. An individual with intellectual disabilities who seems sad, is withdrawn, shows low energy and lack of interest, is eating or sleeping more or less, or may be more irritable could be suffering from a depression that needs medication treatment. On the other hand an individual with intellectual disabilities who demonstrates aggression, property destruction, self-injury, or other forms of “dyscontrol” may be helped by medication aimed at blunting the anxiety/alarm and/or blocking its escalation into aggression or other dangerous behaviors. In such instances the medications are just part of an overall strategy or plan to help the individual avoid the “need” to engage in such behavior. -

The Use and Potential Abuse of Anticholinergic
British Journal of Clinical DOI:10.1111/j.1365-2125.2008.03342.x Pharmacology Correspondence Dr Pål Gjerden, Department of Psychiatry, The use and potential abuse Telemark Hospital, N-3710 Skien, Norway. Tel: + 47 3500 3476 Fax: + 47 3500 3187 of anticholinergic E-mail: [email protected] ---------------------------------------------------------------------- antiparkinson drugs in Keywords adverse effects, anticholinergic agents, antiparkinson agents, antipsychotic Norway: a agents, drug abuse ---------------------------------------------------------------------- Received pharmacoepidemiological 9 June 2008 Accepted 18 October 2008 study Published Early View 16 December 2008 Pål Gjerden, Jørgen G. Bramness1 & Lars Slørdal2 Department of Psychiatry,Telemark Hospital, Skien, 1Department of Pharmacoepidemiology, Norwegian Institute of Public Health, Oslo and 2Department of Laboratory Medicine, Children’s and Women’s Health, Norwegian University of Science and Technology,Trondheim, Norway WHAT IS ALREADY KNOWN ABOUT THIS SUBJECT • Anticholinergic antiparkinson drugs are used to ameliorate extrapyramidal AIMS symptoms caused by either Parkinson’s The use of anticholinergic antiparkinson drugs is assumed to have disease or antipsychotic drugs, but their use shifted from the therapy of Parkinson’s disease to the amelioration in the treatment of Parkinson’s disease is of extrapyramidal adverse effects induced by antipsychotic drugs. There is a considerable body of data suggesting that anticholinergic assumed to be in decline. antiparkinson drugs have a potential for abuse.The aim was to • Patients with psychotic conditions have a investigate the use and potential abuse of this class of drugs in Norway. high prevalence of abuse of drugs, including anticholinergic antiparkinson drugs. METHODS Data were drawn from the Norwegian Prescription Database on sales to a total of 73 964 patients in 2004 of biperiden and orphenadrine, and use in patients with Parkinson’s disease or in patients who were WHAT THIS STUDY ADDS also prescribed antipsychotic agents. -

CENTRAL NERVOUS SYSTEM DEPRESSANTS Opioid Pain Relievers Anxiolytics (Also Belong to Psychiatric Medication Category) • Codeine (In 222® Tablets, Tylenol® No
CENTRAL NERVOUS SYSTEM DEPRESSANTS Opioid Pain Relievers Anxiolytics (also belong to psychiatric medication category) • codeine (in 222® Tablets, Tylenol® No. 1/2/3/4, Fiorinal® C, Benzodiazepines Codeine Contin, etc.) • heroin • alprazolam (Xanax®) • hydrocodone (Hycodan®, etc.) • chlordiazepoxide (Librium®) • hydromorphone (Dilaudid®) • clonazepam (Rivotril®) • methadone • diazepam (Valium®) • morphine (MS Contin®, M-Eslon®, Kadian®, Statex®, etc.) • flurazepam (Dalmane®) • oxycodone (in Oxycocet®, Percocet®, Percodan®, OxyContin®, etc.) • lorazepam (Ativan®) • pentazocine (Talwin®) • nitrazepam (Mogadon®) • oxazepam ( Serax®) Alcohol • temazepam (Restoril®) Inhalants Barbiturates • gases (e.g. nitrous oxide, “laughing gas”, chloroform, halothane, • butalbital (in Fiorinal®) ether) • secobarbital (Seconal®) • volatile solvents (benzene, toluene, xylene, acetone, naptha and hexane) Buspirone (Buspar®) • nitrites (amyl nitrite, butyl nitrite and cyclohexyl nitrite – also known as “poppers”) Non-Benzodiazepine Hypnotics (also belong to psychiatric medication category) • chloral hydrate • zopiclone (Imovane®) Other • GHB (gamma-hydroxybutyrate) • Rohypnol (flunitrazepam) CENTRAL NERVOUS SYSTEM STIMULANTS Amphetamines Caffeine • dextroamphetamine (Dexadrine®) Methelynedioxyamphetamine (MDA) • methamphetamine (“Crystal meth”) (also has hallucinogenic actions) • methylphenidate (Biphentin®, Concerta®, Ritalin®) • mixed amphetamine salts (Adderall XR®) 3,4-Methelynedioxymethamphetamine (MDMA, Ecstasy) (also has hallucinogenic actions) Cocaine/Crack -

The Effect of Antidepressive Drugs and Some Related Compounds on the Levels of Adenine Nucleotides, Inorganic Phosphate and Phosphocreatine in the Rat Brain by J
Brit. J. Pharmacol. (1963), 20, 462-470. THE EFFECT OF ANTIDEPRESSIVE DRUGS AND SOME RELATED COMPOUNDS ON THE LEVELS OF ADENINE NUCLEOTIDES, INORGANIC PHOSPHATE AND PHOSPHOCREATINE IN THE RAT BRAIN BY J. J. LEWIS AND G. R. VAN PETTEN From the Experimental Pharmacology Division, Institute of Physiology, University of Glasgow (Received January 11, 1963) The effects upon levels of adenine nucleotides, phosphocreatine and inorganic phosphate of iproniazid, isoniazid, phenelzine, pheniprazine, tranylcypromine, harmine, imipramine, amitriptyline, orphenadrine, diphenhydramine and cocaine have been studied. With the exception of harmine and diphenhydramine, each of these compounds increased the brain level of adenosine triphosphate and, with the exception of imipramine and cocaine, the level of adenosine diphosphate decreased. Harmine had no effect on levels of adenine nucleotides and, in the case of diphenhydramine, the level of adenosine diphosphate increased and the level of adenosine triphosphate tended to decrease. There appears to be a relationship between the ability of the drugs to cause behavioural signs of central nervous stimulation and to produce an increase in the adenosine triphosphate/diphosphate ratio. This effect may be a factor in the action of antidepressive drugs. Many attempts have been made to explain the mechanism of action of anti- depressive drugs on the basis of their ability to inhibit monoamine oxidase, and thereby to increase the effective concentrations in the brain of its substrates, nor- adrenaline and 5-hydroxytryptamine, which have been postulated to act there as transmitters. Major difficulties arise, however, when an attempt is made to correlate the increase in the brain level of a particular amine produced by a drug with its antidepressive activity. -

Treatment for Acute Pain: an Evidence Map Technical Brief Number 33
Technical Brief Number 33 R Treatment for Acute Pain: An Evidence Map Technical Brief Number 33 Treatment for Acute Pain: An Evidence Map Prepared for: Agency for Healthcare Research and Quality U.S. Department of Health and Human Services 5600 Fishers Lane Rockville, MD 20857 www.ahrq.gov Contract No. 290-2015-0000-81 Prepared by: Minnesota Evidence-based Practice Center Minneapolis, MN Investigators: Michelle Brasure, Ph.D., M.S.P.H., M.L.I.S. Victoria A. Nelson, M.Sc. Shellina Scheiner, PharmD, B.C.G.P. Mary L. Forte, Ph.D., D.C. Mary Butler, Ph.D., M.B.A. Sanket Nagarkar, D.D.S., M.P.H. Jayati Saha, Ph.D. Timothy J. Wilt, M.D., M.P.H. AHRQ Publication No. 19(20)-EHC022-EF October 2019 Key Messages Purpose of review The purpose of this evidence map is to provide a high-level overview of the current guidelines and systematic reviews on pharmacologic and nonpharmacologic treatments for acute pain. We map the evidence for several acute pain conditions including postoperative pain, dental pain, neck pain, back pain, renal colic, acute migraine, and sickle cell crisis. Improved understanding of the interventions studied for each of these acute pain conditions will provide insight on which topics are ready for comprehensive comparative effectiveness review. Key messages • Few systematic reviews provide a comprehensive rigorous assessment of all potential interventions, including nondrug interventions, to treat pain attributable to each acute pain condition. Acute pain conditions that may need a comprehensive systematic review or overview of systematic reviews include postoperative postdischarge pain, acute back pain, acute neck pain, renal colic, and acute migraine. -

Georgia State Forensic Drugs
Comprehensive Forensic FT-IR Collection Library Listing – 4,286 spectra This extensive library contains materials not only of forensic interest but also for general problem solving and identification of unknown substances in industry and academia. The wide range of items include drugs, clandestine lab chemicals, explosives, paints, fabrics, dyes, polymers, inorganic compounds, pigments, adhesives, and other common materials. The library consists of 4,286 spectra that were acquired from a wide range of laboratories involved in forensic investigations. The collection includes the following classes of compounds: • Drugs of abuse, scheduled materials • Pharmaceuticals, vitamins and excipients • Clandestine lab materials and intermediates • Solvents, organic chemicals and hazardous chemicals • Accelerants • Lubricants and natural oils • Explosives, pyrotechnics, primers, powders and boosters • Herbal and plant material and fibers • Automobile paint vehicles, pigments, primers and clear coats • Textiles, natural and man-made fibers, carpet materials • Paints, coatings, varnishes, oils • Dyes and stains • Polymers, monomers, copolymers, plasticizers and rubbers • Inorganics, pigments, minerals and clays • Tape, adhesives, sealants, glues, caulks and putties • Crystal test derivatives and intermediates • Household chemicals, cleaning agents, surfactants and pesticide All spectra were measured using micro or macro Diamond ATR, thin films on salt windows or KBr pellets at 4 cm-1 spectral resolution. Comprehensive Forensic FT-IR Collection Index