Management of Geriatric Elbow Injury
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Transolecranon Distal Humerus Fractures: a Mini Review
Patel SS, Gatta J, Lee A, Bafus BT. Transolecranon Distal Humerus Fractures: A Mini Review. J Orthopedics & Orthopedic Surg. 2021;2(1):7-12 Mini Review Open Access Transolecranon Distal Humerus Fractures: A Mini Review Shaan S. Patel*, Julian Gatta, Adrienne Lee, Blaine T. Bafus Department of Orthopaedic Surgery, MetroHealth Medical Center, Cleveland, OH, USA Article Info Abstract Article Notes Background: Transolecranon distal humerus fractures are uncommon Received: March 13, 2021 injuries. The purpose of this study is to review the outcomes and complications Accepted: April 22, 2021 associated with transolecranon distal humerus fractures. *Correspondence: Material and Methods: We performed a systematic search of PubMed *Dr. Shaan S. Patel, Department of Orthopaedic Surgery, for articles published between 1990 and 2021. Included studies reported MetroHealth Medical Center, Cleveland, OH, USA; Telephone No: (205) 495-0460; Email: [email protected]. outcomes and complications of transolecranon distal humerus fractures. Data was extracted from the included studies to describe patient demographics, ©2021 Patel SS. This article is distributed under the terms of the injury characteristics, outcome measurements, and complications. Creative Commons Attribution 4.0 International License. Results: A total of 4 studies met inclusion criteria for data extraction and Keywords analysis. Two studies evaluated an adult cohort of a total of 18 patients. The Transolecranon average Disabilities of the Arm, Shoulder, and Hand (DASH) score was 40 (range Olecranon 4.2 – 76.5). Fifteen patients (83%) had a complication. Elbow stiffness (11/18, Distal humerus 61%) was the most common complication. Eleven patients (61%) underwent Fracture Outcomes more than one procedure. Two studies evaluated a pediatric cohort of a total Complications of 9 patients. -

Downloads As of 6/2011.) 2
CURRICULUM VITAE Michael J. Prayson, MD Department of Orthopaedic Surgery, Sports Medicine & Rehabilitation Wright State University Boonshoft School of Medicine 30 E. Apple Street, Suite 2200 Dayton, Ohio 45409 937-208-2128 937-208-2920 Fax EDUCATION Institution Concentration Degree/Date Kent State University & Combined 6-Year Program BS/MD 1989 Northeastern Ohio Universities College of Medicine Rootstown, Ohio POST GRADUATE EDUCATION Item Date Orthopaedic Surgery Internship & Residency Training 1989-1994 Akron General Medical Center, Akron, Ohio Orthopaedic Traumatology Fellowship 1994-1995 Department of Orthopaedic Surgery University of Pittsburgh Medical Center, Pittsburgh, Pennsylvania ACADEMIC EXPERIENCE Institution Position Date Northeastern Ohio Universities College of Medicine Clinical Instructor 1993-1994 Rootstown, Ohio University of Missouri Assistant Professor 1995-1998 Department of Orthopaedic Surgery Kansas City, Missouri Akron General Medical Center Assistant Professor 1998-1999 Department of Orthopaedic Surgery Akron, Ohio University of Pittsburgh Medical Center Assistant Professor 1999-2004 Department of Orthopaedic Surgery Pittsburgh, Pennsylvania Wright State University Boonshoft School of Medicine Associate Professor 2004-2009 Department of Orthopaedic Surgery, Director of Orthopaedic Sports Medicine & Rehabilitation Undergraduate Education 2004-2006 Dayton, Ohio Trauma Fellowship Director 2006-Present Director of Orthopaedic Trauma 2004-Present Section Chair of Orthopaedic Trauma 2008-2010 Vice Chairman 2008-Present -

CASE REPORT Injuries Following Segway Personal
UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health Title Injuries Following Segway Personal Transporter Accidents: Case Report and Review of the Literature Permalink https://escholarship.org/uc/item/37r4387d Journal Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health, 16(5) ISSN 1936-900X Authors Ashurst, John Wagner, Benjamin Publication Date 2015 DOI 10.5811/westjem.2015.7.26549 License https://creativecommons.org/licenses/by/4.0/ 4.0 Peer reviewed eScholarship.org Powered by the California Digital Library University of California CASE REPORT Injuries Following Segway Personal Transporter Accidents: Case Report and Review of the Literature John Ashurst DO, MSc Conemaugh Memorial Medical Center, Department of Emergency Medicine, Benjamin Wagner, DO Johnstown, Pennsylvania Section Editor: Rick A. McPheeters, DO Submission history: Submitted April 20, 2015; Accepted July 9, 2015 Electronically published October 20, 2015 Full text available through open access at http://escholarship.org/uc/uciem_westjem DOI: 10.5811/westjem.2015.7.26549 The Segway® self-balancing personal transporter has been used as a means of transport for sightseeing tourists, military, police and emergency medical personnel. Only recently have reports been published about serious injuries that have been sustained while operating this device. This case describes a 67-year-old male who sustained an oblique fracture of the shaft of the femur while using the Segway® for transportation around his community. We also present a review of the literature. [West J Emerg Med. 2015;16(5):693-695.] INTRODUCTION no parasthesia was noted. In 2001, Dean Kamen developed a self-balancing, zero Radiograph of the right femur demonstrated an oblique emissions personal transportation vehicle, known as the fracture of the proximal shaft of the femur with severe Segway® Personal Transporter (PT).1 The Segway’s® top displacement and angulation (Figure). -

Pediatric Orthopedic Injuries… … from an ED State of Mind
Traumatic Orthopedics Peds RC Exam Review February 28, 2019 Dr. Naminder Sandhu, FRCPC Pediatric Emergency Medicine Objectives to cover today • Normal bone growth and function • Common radiographic abnormalities in MSK diseases • Part 1: Atraumatic – Congenital abnormalities – Joint and limb pain – Joint deformities – MSK infections – Bone tumors – Common gait disorders • Part 2: Traumatic – Common pediatric fractures and soft tissue injuries by site Overview of traumatic MSK pain Acute injuries • Fractures • Joint dislocations – Most common in ED: patella, digits, shoulder, elbow • Muscle strains – Eg. groin/adductors • Ligament sprains – Eg. Ankle, ACL/MCL, acromioclavicular joint separation Chronic/ overuse injuries • Stress fractures • Tendonitis • Bursitis • Fasciitis • Apophysitis Overuse injuries in the athlete WHY do they happen?? Extrinsic factors: • Errors in training • Inappropriate footwear Overuse injuries Intrinsic: • Poor conditioning – increased injuries early in season • Muscle imbalances – Weak muscle near strong (vastus medialus vs lateralus patellofemoral pain) – Excessive tightness: IT band, gastroc/soleus Sever disease • Anatomic misalignments – eg. pes planus, genu valgum or varum • Growth – strength and flexibility imbalances • Nutrition – eg. female athlete triad Misalignment – an intrinsic factor Apophysitis • *Apophysis = natural protruberance from a bone (2ndary ossification centres, often where tendons attach) • Examples – Sever disease (Calcaneal) – Osgood Schlatter disease (Tibial tubercle) – Sinding-Larsen-Johansson -

University of Washington Orthopaedics & Sports Medicine
Discoveries 2018 University of Washington Orthopaedics & Sports Medicine University of Washington Department of Orthopaedics and Sports Medicine Discoveries 2018 Department of Orthopaedics and Sports Medicine University of Washington Seattle, WA 98195 EDITOR-IN-CHIEF: Howard A. Chansky, MD [email protected] ASSISTANT EDITORS: Christopher H. Allan, MD [email protected] Stephen A. Kennedy, MD, FRCSC [email protected] Adam A. Sassoon, MD, MS [email protected] MANAGING EDITOR: Fred Westerberg [email protected] Front Cover Illustration: Angie Kennedy, MSc, is a Seattle-based mixed media artist. She specializes in custom collage pieces that use mementos and artifacts to celebrate people and special life events. She drew on her experience as a former scientific researcher to create this collage of images from the pages of the current publication. The ‘W’ in the background is a nod to the University of Washington with an overlay of the current imagery arranged in an abstract assemblage. For more information www.americanheavyweight.com A pdf of this publication is available at our website: www.orthop.washington.edu. Permission Requests: All inquiries should be directed to the Managing Editor, University of Washington, Department of Orthopaedics and Sports Medicine, 1959 NE Pacific Street, Box 356500, Seattle, WA 98195-6500, or at the email address above. Contents 1 Foreword 2 From The Assistant Editors: The Modern Art of Musculoskeletal Research, Education, and Clinical Care 3 2018 Distinguished Alumnus, David J. Belfie, MD 4 New Faculty 6 Department of Orthopaedics and Sports Medicine Faculty 12 Visiting Lecturers Validation of a Rabbit Model of Trauma-Induced 14 Brandon J. Ausk, PhD, Philippe Huber, BS, Heterotopic Ossification Ted S. -

Upper Extremity Fractures
Department of Rehabilitation Services Physical Therapy Standard of Care: Distal Upper Extremity Fractures Case Type / Diagnosis: This standard applies to patients who have sustained upper extremity fractures that require stabilization either surgically or non-surgically. This includes, but is not limited to: Distal Humeral Fracture 812.4 Supracondylar Humeral Fracture 812.41 Elbow Fracture 813.83 Proximal Radius/Ulna Fracture 813.0 Radial Head Fractures 813.05 Olecranon Fracture 813.01 Radial/Ulnar shaft fractures 813.1 Distal Radius Fracture 813.42 Distal Ulna Fracture 813.82 Carpal Fracture 814.01 Metacarpal Fracture 815.0 Phalanx Fractures 816.0 Forearm/Wrist Fractures Radius fractures: • Radial head (may require a prosthesis) • Midshaft radius • Distal radius (most common) Residual deformities following radius fractures include: • Loss of radial tilt (Normal non fracture average is 22-23 degrees of radial tilt.) • Dorsal angulation (normal non fracture average palmar tilt 11-12 degrees.) • Radial shortening • Distal radioulnar (DRUJ) joint involvement • Intra-articular involvement with step-offs. Step-off of as little as 1-2 mm may increase the risk of post-traumatic arthritis. 1 Standard of Care: Distal Upper Extremity Fractures Copyright © 2007 The Brigham and Women's Hospital, Inc. Department of Rehabilitation Services. All rights reserved. Types of distal radius fracture include: • Colle’s (Dinner Fork Deformity) -- Mechanism: fall on an outstretched hand (FOOSH) with radial shortening, dorsal tilt of the distal fragment. The ulnar styloid may or may not be fractured. • Smith’s (Garden Spade Deformity) -- Mechanism: fall backward on a supinated, dorsiflexed wrist, the distal fragment displaces volarly. • Barton’s -- Mechanism: direct blow to the carpus or wrist. -
Radial Head Fracture Repair and Rehabilitation
1 Radial Head Fracture Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The elbow is a complex joint due to its intricate functional anatomy. The ulna, radius and humerus articulate in such a way as to form four distinctive joints. Surrounding the osseous structures are the ulnar collateral ligament complex, the lateral collateral ligament complex and the joint capsule. Four main muscle groups provide movement: the elbow flexors, the elbow extensors, the flexor-pronator group, and the extensor-supinator groups. Different types of radial head fractures can occur each of which has separate surgical indications and considerations. Fractures of the proximal one-third of the radius normally occur in the head region in adults and in neck region in children. The most recognized and used standard for assessing radial head fractures is the 4-part Mason classification system. It is used for both treatment and prognosis. Classification: Type I fracture A fissure or marginal fracture without displacement. Type II fracture Marginal fractures with displacement involving greater than 2 mm displacement. Type III fracture Comminuted fractures of the whole radial head. Type IV fracture (variation) A comminuted fracture, with an associated dislocation, ligament injury, coronoid fracture, or Monteggia lesion. Pathogenesis: Severe comminuted fractures or fracture dislocations of the head of the radius often occur as the result of a fall on an outstretched arm with the distal forearm angled laterally, or a valgus stress on the elbow. Fractures can also occur from a direct blow or force to the elbow (e.g. MVA). Chronic synovitis and mild deterioration of the articular surfaces associated with arthritis (e.g. -

Common Pediatric Elbow Fractures
NOR200175.qxd 1/7/11 5:01 AM Page 11 Common Pediatric Elbow Fractures Erin S. Hart ▼ Allison Turner ▼ Maurice Albright ▼ Brian E. Grottkau Fractures of the elbow are a very common injury in children. condyle fractures. Because 80% of the longitudinal The most common mechanism of injury is a fall on an out- growth in the arm occurs proximally (proximal stretched upper extremity during play. Ranging in complex- humerus), only appositional growth occurs at the elbow. ity from low-energy nondisplaced occult fractures to high- This limits the ability for elbow fractures to completely energy fractures with associated severe soft-tissue and remodel and therefore makes anatomic reductions nec- essary even in young skeletally immature individuals (Do neurovascular injuries, elbow fractures are a challenging & Herrera-Soto, 2003). problem for all pediatric healthcare providers. Because of the wide spectrum of fracture severity and associated bony and ligamentous injury, a very diverse spectrum of treatment Supracondylar Humerus Fracture modalities is necessary for optimal results. Management is Supracondylar humerus fractures are the most common based on fracture pattern, patient age and bone quality, elbow injury in children (Kasser & Beatty, 2006). They extent of soft tissue damage, functional needs of the patient, account for approximately 50% to 70% of all elbow frac- and the presence of associated injuries. This article will give tures in children (Farnsworth, Silva, & Mubarak, 1998). a brief overview of 4 common pediatric fractures, current This injury occurs most often in boys between the ages of treatment algorithms, and frequent complications associ- 4 and 7 and most frequently occurs after a fall on an out- stretched upper extremity. -

What Are Elbow Fractures?
Sussex Hand CONDITION Surgery Elbow Fractures CONDITION An elbow fracture might include What are any or all of the bones near the joint. Treatment and prognosis is Elbow Fractures? very variable. Which bones are How do I know I have What treatments are 3. Repair of stabilising ligaments. commonly broken in broken my elbow, not available for elbow This is done if necessary at the the elbow? just sprained it? fractures? same time as fixing the bones. The elbow joint is made up of three A displaced fracture may be very All elbow fractures are helped by 4. Replacing damaged parts. This is bones; the far end of the upper arm obvious with deformity, swelling, elevation of the limb (to get the done for the most severe fracture bone called the humerus and the bruising and pain. Undisplaced swelling down) and painkillers. types in adults only. The top part near end of the two forearm bones, fractures can be quite difficult to Application of ice packs can of the radius (the circular part on the radius and the ulna. pick up without xrays. If in doubt sometimes also help. the picture above) can be replaced obtain expert advice early on to alone (radial head replacement). In Many elbow fractures can be make sure you are put on the path older patients with soft bone in Normal Elbow treated without an operation but to show the Joint to recovery as quickly as possible. multiple small fragments replacing good advice regarding appropriate the whole elbow joint can How is the diagnosis made? support and exercises to regain occasionally be the best option maximum function as quickly as (total elbow replacement). -

Open Reduction and Internal Fixation of Capitellar Fractures with Headless Screws Surgical Technique
Ruchelsman.fm Page 38 Friday, February 6, 2009 3:03 PM 38 COPYRIGHT © 2 009 BY THE JOURNAL OF BONE AND JOINT SURGERY, I NCORPORATED Open Reduction and Internal Fixation of Capitellar Fractures with Headless Screws Surgical Technique By David E. Ruchelsman, MD, Nirmal C. Tejwani, MD, Young W. Kwon, MD, PhD, and Kenneth A. Egol, MD Investigation performed at the New York University Hospital for Joint Diseases, New York, NY The original scientific article in which the surgical technique was presented was published in JBJS Vol. 90-A, pp. 1321-9, June 2008 ABSTRACT FROM THE ORIGINAL ARTICLE BACKGROUND: The outcome of operatively treated capitellar fractures has not been reported frequently. The purpose of the present study was to evaluate the clinical, radiographic, and functional outcomes following open reduction and inter- nal fixation of capitellar fractures that were treated with a uniform surgical approach in order to further define the impact on the outcome of fracture type and concomitant lateral column osseous and/or ligamentous injuries. METHODS: A retrospective evaluation of the upper extremity database at our institution identified sixteen skeletally mature patients (mean age, 40 ± 17 years) with a closed capitellar fracture. In all cases, an extensile lateral exposure and artic- ular fixation with buried cannulated variable-pitch headless compression screws was performed at a mean of ten days af- ter the injury. Clinical, radiographic, and elbow-specific outcomes, including the Mayo Elbow Performance Index, were evaluated at a mean of 27 ± 19 months postoperatively. RESULTS: Six Type-I, two Type-III, and eight Type-IV fractures were identified with use of the Bryan and Morrey classification system. -

SURGICAL MANAGEMENT of COMPOUND DISTAL HUMERUS FRACTURE by JESS EXTERNAL FIXATOR Utkal Gupta1, Sanjay Gupta2, Gaurav Aggrawal3, Arjun Gandotra4, V
DOI: 10.14260/jemds/2014/2597 ORIGINAL ARTICLE SURGICAL MANAGEMENT OF COMPOUND DISTAL HUMERUS FRACTURE BY JESS EXTERNAL FIXATOR Utkal Gupta1, Sanjay Gupta2, Gaurav Aggrawal3, Arjun Gandotra4, V. P. Pathania5 HOW TO CITE THIS ARTICLE: Utkal Gupta, Sanjay Gupta, Gaurav Aggrawal, Arjun Gandotra, V. P. Pathania. “Surgical Management of Compound Distal Humerus Fracture by Jess External Fixator”. Journal of Evolution of Medical and Dental Sciences 2014; Vol. 3, Issue 19, May 12; Page: 5352-5366, DOI: 10.14260/jemds/2014/2597 ABSTRACT: BACKGROUND: Intraarticular displaced distal humerus fractures in adults always require open reduction and internal fixation with some plate and screw osteosynthesis after accurate reduction and alignment of fracture fragments. But high velocity trauma or gun-shot injuries often lead to a compound fracture with contamination and devitalization of soft tissue cover which requires some kind of external fixation. We thereby report the outcome of a series of ten patients who were treated definitively by extensive debridement and JESS type external fixation. This external fixator construct gave excellent fracture fragment stability and early mobilization of elbow joint. It provided patient friendly definitive fixation assembly resulting in early fracture consolidation with reasonably good range of elbow movement for such difficult fractures. MATERIAL AND METHODS: Ten cases of compound intercondylar distal humerus fracture between January 2007 to December 2011were treated by early debridement & uniplanar bilateral JESS fixator application at the same sitting. This study includes cases of age group 18- 65 yrs. of which 3 were females & 7 were males. Mean age was 31.5yr. Only one case had injury to elbow with Gun-shot injury & rest were of high energy road traffic accidents. -
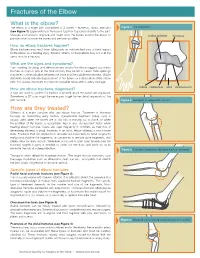
Fractures of the Elbow
Fractures of the Elbow What is the elbow? The elbow is a hinge joint comprised of 3 bones – humerus, radius and ulna Figure 1: The elbow joint (see Figure 1). Ligaments hold the bones together to provide stability to the joint. Muscles and tendons originate and insert onto the bones around the elbow to radiocapitellar humerus provide force to move the bones and perform activities. How do elbow fractures happen? Elbow fractures may result from falling onto an outstretched arm, a direct impact to the elbow, or a twisting injury. Sprains, strains, or dislocations may occur at the same time as a fracture. What are the signs and symptoms? Pain, swelling, bruising, and stiffness in and around the elbow suggest a possible fracture. A snap or pop at the time of injury may be felt or heard. Skin openings may reflect communication between the bone and the outside environment. Visible deformity would indicate displacement of the bones or a dislocation of the elbow joint. It is always important to check for possible nerve and/or artery damage. How are elbow fractures diagnosed? radius radioulnar ulna ulnohumeral X-rays are used to confirm if a fracture is present and if the bones are displaced. Sometimes a CT scan might be necessary to get further detail, especially of the joint surface. Figure 2: Illustration of radial neck fracture How are they treated? Stiffness is a major concern after any elbow fracture. Treatment is therefore focused on maximizing early motion. Conservative treatment (sling, cast) is usually used when the bones are at low risk of moving out of place, or when the position of the bones is acceptable.