Effective Reporting of Antimicrobial Susceptibility Test Results
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Polymyxin B in Combination with Doripenem Against Heteroresistant Acinetobacter Baumannii: Pharmacodynamics of New Dosing Strategies
J Antimicrob Chemother 2016; 71: 3148–3156 doi:10.1093/jac/dkw293 Advance Access publication 3 August 2016 Polymyxin B in combination with doripenem against heteroresistant Acinetobacter baumannii: pharmacodynamics of new dosing strategies Gauri G. Rao1,2, Neang S. Ly1,2,Ju¨rgen B. Bulitta1,3, Rachel L. Soon1,2, Marie D. San Roman1,2, Patricia N. Holden1,2, Cornelia B. Landersdorfer4, Roger L. Nation4, Jian Li4, Alan Forrest1,5 and Brian T. Tsuji1,2* 1Laboratory for Antimicrobial Pharmacodynamics, School of Pharmacy and Pharmaceutical Sciences, University at Buffalo, The State University of New York, Buffalo, NY, USA; 2The New York State Center of Excellence in Bioinformatics & Life Sciences, University at Buffalo, The State University of New York, Buffalo, NY, USA; 3Center for Pharmacometrics and Systems Pharmacology, College of Pharmacy, University of Florida, Orlando, FL, USA; 4Drug Delivery, Disposition and Dynamics, Monash Institute of Pharmaceutical Sciences, Monash University, Melbourne, Australia; 5Eshelman School of Pharmacy, The University of North Carolina at Chapel Hill, NC, USA *Corresponding author. Tel: +1-716-881-7543; Fax: +1-716-849-6890; E-mail: [email protected] Received 13 October 2015; returned 3 January 2016; revised 14 June 2016; accepted 19 June 2016 Objectives: Polymyxin B is being increasingly utilized as a last resort against resistant Gram-negative bacteria. We examined the pharmacodynamics of novel dosing strategies for polymyxin B combinations to maximize efficacy and minimize the emergence of resistance and drug exposure against Acinetobacter baumannii. Methods: The pharmacodynamics of polymyxin B together with doripenem were evaluated in time–kill experi- ments over 48 h against 108 cfu/mL of two polymyxin-heteroresistant A. -

Medical Review(S) Clinical Review
CENTER FOR DRUG EVALUATION AND RESEARCH APPLICATION NUMBER: 200327 MEDICAL REVIEW(S) CLINICAL REVIEW Application Type NDA Application Number(s) 200327 Priority or Standard Standard Submit Date(s) December 29, 2009 Received Date(s) December 30, 2009 PDUFA Goal Date October 30, 2010 Division / Office Division of Anti-Infective and Ophthalmology Products Office of Antimicrobial Products Reviewer Name(s) Ariel Ramirez Porcalla, MD, MPH Neil Rellosa, MD Review Completion October 29, 2010 Date Established Name Ceftaroline fosamil for injection (Proposed) Trade Name Teflaro Therapeutic Class Cephalosporin; ß-lactams Applicant Cerexa, Inc. Forest Laboratories, Inc. Formulation(s) 400 mg/vial and 600 mg/vial Intravenous Dosing Regimen 600 mg every 12 hours by IV infusion Indication(s) Acute Bacterial Skin and Skin Structure Infection (ABSSSI); Community-acquired Bacterial Pneumonia (CABP) Intended Population(s) Adults ≥ 18 years of age Template Version: March 6, 2009 Reference ID: 2857265 Clinical Review Ariel Ramirez Porcalla, MD, MPH Neil Rellosa, MD NDA 200327: Teflaro (ceftaroline fosamil) Table of Contents 1 RECOMMENDATIONS/RISK BENEFIT ASSESSMENT ......................................... 9 1.1 Recommendation on Regulatory Action ........................................................... 10 1.2 Risk Benefit Assessment.................................................................................. 10 1.3 Recommendations for Postmarketing Risk Evaluation and Mitigation Strategies ........................................................................................................................ -

Severe Sepsis Tipsheet
Severe Sepsis Tipsheet SEVERE SEPSIS A, B, and C of the following must be met within 6 hours of each other. A. Documentation of a suspected infection. There may be reference to “possible infection,” “suspect infection,” “rule out infection,” or similar documentation. B. TWO or more manifestations of systemic infection according to the Systemic Inflammatory Response Syndrome (SIRS) criteria, which are: • Temperature > 38.3 C or < 36.0 C (> 100.9 F or < 96.8 F) • Heart rate (pulse) > 90 • Respiration > 20 per minute • White blood cell count > 12,000 or < 4,000 or > 10% bands C. Organ dysfunction, evidenced by any one of the following: • Systolic blood pressure (SBP) < 90 mmHg, or mean arterial pressure < 65 mmHg, or a systolic blood pressure decrease of more than 40 mmHg. Physician/APN/PA documentation must be present in the medical record indicating a > 40 mmHg decrease in SBP has occurred and is related to infection, severe sepsis or septic shock and not other causes. • Acute respiratory failure as evidenced by a new need for invasive or non-invasive mechanical ventilation. To use acute respiratory failure as a sign of organ dysfunction there must be: • Documentation of acute respiratory failure AND • Documentation the patient is on mechanical ventilation • Invasive mechanical ventilation requires an endotracheal or tracheostomy tube. Non-invasive mechanical ventilation may be referred to as BiPAP or CPAP. • New need for mechanical ventilation indicates the patient was not using the same type of mechanical ventilation prior to the current acute respiratory failure. • Use the time at which there is documentation the patient has both acute respiratory failure and is on mechanical ventilation. -
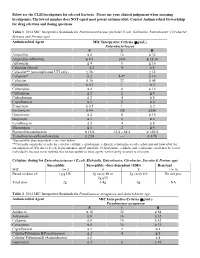
Below Are the CLSI Breakpoints for Selected Bacteria. Please Use Your Clinical Judgement When Assessing Breakpoints
Below are the CLSI breakpoints for selected bacteria. Please use your clinical judgement when assessing breakpoints. The lowest number does NOT equal most potent antimicrobial. Contact Antimicrobial Stewardship for drug selection and dosing questions. Table 1: 2014 MIC Interpretive Standards for Enterobacteriaceae (includes E.coli, Klebsiella, Enterobacter, Citrobacter, Serratia and Proteus spp) Antimicrobial Agent MIC Interpretive Criteria (g/mL) Enterobacteriaceae S I R Ampicillin ≤ 8 16 ≥ 32 Ampicillin-sulbactam ≤ 8/4 16/8 ≥ 32/16 Aztreonam ≤ 4 8 ≥ 16 Cefazolin (blood) ≤ 2 4 ≥ 8 Cefazolin** (uncomplicated UTI only) ≤ 16 ≥ 32 Cefepime* ≤ 2 4-8* ≥ 16 Cefotetan ≤ 16 32 ≥ 64 Ceftaroline ≤ 0.5 1 ≥ 2 Ceftazidime ≤ 4 8 ≥ 16 Ceftriaxone ≤ 1 2 ≥ 4 Cefpodoxime ≤ 2 4 ≥ 8 Ciprofloxacin ≤ 1 2 ≥ 4 Ertapenem ≤ 0.5 1 ≥ 2 Fosfomycin ≤ 64 128 ≥256 Gentamicin ≤ 4 8 ≥ 16 Imipenem ≤ 1 2 ≥ 4 Levofloxacin ≤ 2 4 ≥ 8 Meropenem ≤ 1 2 ≥ 4 Piperacillin-tazobactam ≤ 16/4 32/4 – 64/4 ≥ 128/4 Trimethoprim-sulfamethoxazole ≤ 2/38 --- ≥ 4/76 *Susceptibile dose-dependent – see chart below **Cefazolin can predict results for cefaclor, cefdinir, cefpodoxime, cefprozil, cefuroxime axetil, cephalexin and loracarbef for uncomplicated UTIs due to E.coli, K.pneumoniae, and P.mirabilis. Cefpodoxime, cefinidir, and cefuroxime axetil may be tested individually because some isolated may be susceptible to these agents while testing resistant to cefazolin. Cefepime dosing for Enterobacteriaceae ( E.coli, Klebsiella, Enterobacter, Citrobacter, Serratia & Proteus spp) Susceptible Susceptible –dose-dependent (SDD) Resistant MIC </= 2 4 8 >/= 16 Based on dose of: 1g q12h 1g every 8h or 2g every 8 h Do not give 2g q12 Total dose 2g 3-4g 6g NA Table 2: 2014 MIC Interpretive Standards for Pseudomonas aeruginosa and Acinetobacter spp. -

Management of Penicillin and Beta-Lactam Allergy
Management of Penicillin and Beta-Lactam Allergy (NB Provincial Health Authorities Anti-Infective Stewardship Committee, September 2017) Key Points • Beta-lactams are generally safe; allergic and adverse drug reactions are over diagnosed and over reported • Nonpruritic, nonurticarial rashes occur in up to 10% of patients receiving penicillins. These rashes are usually not allergic and are not a contraindication to the use of a different beta-lactam • The frequently cited risk of 8 to 10% cross-reactivity between penicillins and cephalosporins is an overestimate based on studies from the 1970’s that are now considered flawed • Expect new intolerances (i.e. any allergy or adverse reaction reported in a drug allergy field) to be reported after 0.5 to 4% of all antimicrobial courses depending on the gender and specific antimicrobial. Expect a higher incidence of new intolerances in patients with three or more prior medication intolerances1 • For type-1 immediate hypersensitivity reactions (IgE-mediated), cross-reactivity among penicillins (table 1) is expected due to similar core structure and/or major/minor antigenic determinants, use not recommended without desensitization • For type-1 immediate hypersensitivity reactions, cross-reactivity between penicillins (table 1) and cephalosporins is due to similarities in the side chains; risk of cross-reactivity will only be significant between penicillins and cephalosporins with similar side chains • Only type-1 immediate hypersensitivity to a penicillin manifesting as anaphylaxis, bronchospasm, -

Antibiotic Use for Sepsis in Neonates and Children: 2016 Evidence Update
Antibiotic Use for Sepsis in Neonates and Children: 2016 Evidence Update Aline Fuchsa, Julia Bielickia,b, Shrey Mathurb, Mike Sharlandb, Johannes N. Van Den Ankera,c a Paediatric Pharmacology and Pharmacometrics, University Children's Hospital Basel, Basel, Switzerland b Paediatric Infectious Disease Research Group, Institute for Infection and Immunity, St George's University of London, London, United Kingdom c Division of Clinical Pharmacology, Children’s National Health System, Washington, DC, USA WHO-Reviews 1 TABLE OF CONTENTS 1. INTRODUCTION ............................................................................................................................... 3 1.1. Aims ......................................................................................................................................... 3 1.2. Background ............................................................................................................................. 3 1.2.1. Definition and diagnosis ................................................................................................. 3 Neonatal Sepsis ............................................................................................................................... 3 Paediatric Sepsis ............................................................................................................................. 4 Community versus hospital acquired sepsis .................................................................................. 5 1.2.2. Microbiology .................................................................................................................. -

Comparative Activity of Newer Antibiotics Against Gram-Negative Bacilli
CONTRIBUTION • Comparative activity of newer antibiotics against gram-negative bacilli CYNTHIA C. KNAPP, MS AND JOHN A. WASHINGTON, MD • The in vitro activities of cefoperazone, cefotaxime, ceftriaxone, ceftazidime, azlocillin, mezlocillin, piperacillin, ticarcillin/clavulanate, aztreonam, imipenem, and ciprofloxacin were concurrently deter- mined against over 1,000 isolates of gram-negative bacilli from clinical specimens of patients at the Cleve- land Clinic. Cephalosporins, penicillins, and aztreonam were active against species of Enterobacteriaceae other than Citrobacter freundii, Enterobacter aerogenes, and Enterobacter cloacae. Ceftazidime was the most active cephalosporin against Pseudomonas aeruginosa. Against the Enterobacteriaceae, the rank order of activity of penicillins was ticarcillin/clavulanate > piperacillin > mezlocillin > azlocillin. Against P. aer- uginosa, the rank order of activity of penicillins was piperacillin > ticarcillin/clavulanate > azlocillin > mezlocillin. Aztreonam was less active v P. aeruginosa than ceftazidime, cefoperazone, or piperacillin. The most active antimicrobials against all isolates tested were imipenem and ciprofloxacin. • INDEX TERMS: ANTIBIOTICS, LACTAM; GRAM-NEGATIVE BACTERIA • CLEVE CLIN J MED 1989; 56:161-166 HE RECENT introduction of ciprofloxacin for and penicillins, as well as the monobactam, aztreonam, clinical use follows closely a period of active re- and the carbapenem, imipenem.1-3 search in and development of expanded spec- We compared the susceptibility of more than 1,000 trum p-lactam antibiotics, including cephalo- clinical bacterial isolates to four expanded spectrum Tsporins, penicillins, monobactams, and carbapenems. cephalosporins (cefoperazone, cefotaxime, ceftriaxone, Although numerous published studies compare the ac- and ceftazidime), four expanded spectrum penicillins tivity of ciprofloxacin with other quinolones, only a (azlocillin, mezlocillin, piperacillin, and ticarcil- limited number of studies compare the activity of ci- lin/clavulanate), aztreonam, imipenem, and ciproflox- acin. -

Ertapenem Or Ticarcillin/Clavulanate for the Treatment of Intra-Abdominal Infections Or Acute Pelvic Infections in Pediatric Patients
The American Journal of Surgery 194 (2007) 367–374 Clinical surgery–American Ertapenem or ticarcillin/clavulanate for the treatment of intra-abdominal infections or acute pelvic infections in pediatric patients Albert E. Yellin, M.D.a,*, Jeffrey Johnson, M.D.b, Iliana Higareda, M.D.c, Blaise L. Congeni, M.D.d, Antonio C. Arrieta, M.D.e, Doreen Fernsler, B.S.f, Joseph West, Ph.D.f, Richard Gesser, M.D.f aDepartment of Surgery, Keck School of Medicine of the University of Southern California, 1200 N State St, Rm 9610, Los Angeles, CA 90033, USA bDepartment of Pediatrics, Keck School of Medicine of the University of Southern California, 1240 N Mission Rd, L902, Los Angeles, CA 90089-9300, USA cHospital Civil de Guadalajara, Hospital 278, 4420 El Retiro St, Guadalajara, Jalisco Mexico dAkron Children’s Hospital, Division of Infectious Diseases, Locust Professional Bldg, 300 Locust St, Ste 4, Akron, OH 44308-1062, USA eChildren’s Hospital of Orange County, Pediatric Infectious Diseases, 455 South Main Street, Orange, CA 92868, USA fMerck Research Laboratories, Merck & Co., Inc., 126 East Lincoln Avenue, Rahway, NJ 07065, USA Manuscript received June 20, 2006; revised manuscript January 20, 2007 Abstract Background: Ertapenem, a group I carbapenem antibiotic, has been shown to be safe and effective in treating adults with complicated intra-abdominal (cIAI) or acute pelvic infection (API). This study evaluated ertapenem for treating these infections in children. Methods: In an open-label study, children aged 2 to 17 years with cIAI or API were randomized 3:1 to receive ertapenem or ticarcillin/clavulanate. -

Occurrence of PER-1 Producing Clinical Isolates of Pseudomonas Aeruginosa in Japan and Their Susceptibility to Doripenem
J. Antibiot. 59(12): 791–796, 2006 THE JOURNAL OF ORIGINAL ARTICLE ANTIBIOTICS Occurrence of PER-1 Producing Clinical Isolates of Pseudomonas aeruginosa in Japan and their Susceptibility to Doripenem Yoshinori Yamano, Toru Nishikawa, Takaji Fujimura, Takashi Yutsudou, Masakatsu Tsuji, Hideaki Miwa Received: July 13, 2006 / Accepted: November 20, 2006 © Japan Antibiotics Research Association Abstract The acquisition of resistance by extended- Keywords Pseudomonas aeruginosa, doripenem, ESBL, spectrum b-lactamases (ESBL) has been reported primarily PER-1, in vivo activity for Enterobacteriaceae, but there are few reports on the isolation of ESBL-producing Pseudomonas aeruginosa. PER-1-type ESBL producing P. aeruginosa has been found Introduction in various regions around the world but there are no reports of clinical isolates in Japan. During our susceptibility Pseudomonas aeruginosa is an opportunistic pathogen surveillance studies over a 10 year period, we found causing serious infection in immunocompromised hosts. P. four clinical isolates resistant to ceftazidime due to aeruginosa has intrinsic resistance to many antibiotics and production of PER-1. They were resistant to ceftazidime produces a variety of virulence factors. The intrinsic but susceptible in the presence of clavulanic acid, a class resistance of P. aeruginosa to various antibiotics is A b-lactamase inhibitor. The strains had the ability to generally due to its low outer membrane permeability and hydrolyze ceftazidime. They also had the gene for PER-1- the production of efflux pumps [1]. Although there are type ESBL. This is the first report of the isolation of various antipseudomonal agents such as b-lactams, PER-1 producing strains in Japan. These four strains were quinolones, and aminoglycosides, resistance to these resistant to ceftazidime, cefepime and aztreonam with antibiotics is acquired by P. -

In-Vitro Activity of Doripenem Vs. Imipenem & Meropenem Against
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article In-Vitro Activity of Doripenem vs. Imipenem & Meropenem against Clinical Isolates of Pseudomonas and Other Oxidase-Positive Gram- Negative Bacilli Priya Singh1, Richa Misra2 1Department of Microbiology, Swargiya Dadasaheb Kalmegh Smruti Dental College & Hospital, Nagpur, India 2Department of Microbiology, Division Bacteriology, Sanjay Gandhi Post-Graduate Institute of Medical Sciences, India Corresponding Author: Richa Misra ABSTRACT Background & objectives: Doripenem is approved by United States Food and Drug Administration(US FDA) for the treatment of complicated urinary tract infections (cUTI), complicated intra-abdominal infections (cIAI) and in Europe for ventilator-associated pneumonia (VAP).We attempted to compare the in vitro activity of doripenem with imipenem and meropenem using current CLSI guidelines among clinical isolates of Pseudomonas spp. and other oxidase positive Gram-negative bacilli from clinical samples. Methods: Eighty consecutive clinical isolates were included in the study. Samples included were pus (n=29), blood (n=7), urine (n=24) and 20 sputum (n=20). MIC values of the imipenem, meropenem and doripenem were determined by E tests. Out of 72 Polymyxin B sensitive isolates 34 were Pseudomonas aeruginosa, 30 Fluorescent group and 8 Alcaligenes group. Polymyxin B (n=8) resistant isolates were identified as Burkholderia group. Pseudomonas aeruginosa ATCC 29853 was used as quality control strain. Results: In the Polymyxin B sensitive group (n=72), 29.1%, 23.6% and 26.3% isolates were susceptible to imipenem, meropenem and doripenem respectively. In the Polymyxin B resistant group (n=8) only one isolate was sensitive to imipenem and meropenem while 5 were moderately sensitive to doripenem. -

Ceftaroline Fosamil for the Treatment of Gram-Positive Endocarditis: CAPTURE Study Experience
International Journal of Antimicrobial Agents 53 (2019) 644–649 Contents lists available at ScienceDirect International Journal of Antimicrobial Agents journal homepage: www.elsevier.com/locate/ijantimicag Ceftaroline fosamil for the treatment of Gram-positive endocarditis: CAPTURE study experience ∗ Christopher J. Destache a, David J. Guervil b, Keith S. Kaye c, a School of Pharmacy and Health Professions, Creighton University, Omaha, NE, USA b Memorial Hermann-Texas Medical Center, Houston, TX, USA c Wayne State University and Detroit Medical Center, Detroit, MI, USA a r t i c l e i n f o a b s t r a c t Article history: Background: The clinical experience of ceftaroline fosamil (CPT-F) therapy for Gram-positive infective Received 3 October 2018 endocarditis is reported from CAPTURE, a retrospective study conducted in the USA. Accepted 27 January 2019 Methods: Data, including patient demographics, medical history, risk factors, microbiological aetiology and clinical outcomes, were collected by review of patient charts between September 2013 and February Editor: Professor Matthew Falagas 2015. Results: Patients ( n = 55) with Gram-positive endocarditis were treated with CPT-F. The most common Keywords: risk factors were intravascular devices (43.6%), diabetes mellitus (40.0%) and injection drug use (38.2%). Ceftaroline fosamil Gram-positive endocarditis The most commonly isolated pathogens were meticillin-resistant Staphylococcus aureus (MRSA; 80%), Meticillin-resistant Staphylococcus aureus meticillin-susceptible S. aureus (MSSA; 7.3%) and coagulase-negative staphylococci (7.3%). CPT-F was given Meticillin-susceptible Staphylococcus aureus as first-line therapy in 7.3% of patients and as second-line or later therapy in 92.7% of patients, and as CAPTURE study monotherapy in 41.8% of patients and as concurrent therapy in 58.2% of patients. -

Carbapenem-Resistant Enterobacteriaceae Investigative Guidelines December 2019
PUBLIC HEALTH DIVISION Acute and Communicable Disease Prevention Carbapenem-Resistant Enterobacteriaceae Investigative Guidelines December 2019 1. DISEASE REPORTING 1.1 Purpose of Reporting and Surveillance 1. To prevent transmission of infections with carbapenem-resistant Enterobacteriaceae (CRE) between patients, within or among health care facilities, or between health care facilities and the community. 2. To prevent CRE from becoming endemic in Oregon, necessitating empiric use of even broader- spectrum antibiotics. 3. To identify outbreaks and potential sources or sites of ongoing transmission. 4. To better characterize the epidemiology of these infections. 1.2 Laboratory and Physician Reporting Requirements 1. Providers and laboratories must report cases to local public health authorities (LPHAs) within one working day. 2. Clinical and reference laboratories must forward isolates from any sterile or non-sterile site (e.g., urine, blood, sputum, endotracheal aspirate, BAL, wound) that meet the confirmed CRE case definition below along with the automated test system susceptibility printouts (Vitek or Microscan report) to the Oregon State Public Health Laboratory (OSPHL). 3. Isolates of Proteus, Providencia, or Morganella which show only imipenem non-susceptibility, in the absence of resistance to another carbapenem, do not need to be submitted. 1.3 Local Public Health Authority Reporting and Follow-Up Responsibilities 1. LPHAs will confirm that a case meets the case definition by reviewing the isolate's susceptibility information (antibiogram) as necessary, or in consultation with the ACDP epidemiologist. Both minimum inhibitory concentration (MIC) values and interpretations are needed to verify a case meets the definition. (See Confirmed Case §3.1.) 2. If a case meets the case definition, the LPHA will investigate.