Rerouting the Dissection of the Infratemporal and Submandibular Regions
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

The Role of the Tensor Veli Palatini Muscle in the Development of Cleft Palate-Associated Middle Ear Problems
Clin Oral Invest DOI 10.1007/s00784-016-1828-x REVIEW The role of the tensor veli palatini muscle in the development of cleft palate-associated middle ear problems David S. P. Heidsieck1 & Bram J. A. Smarius1 & Karin P. Q. Oomen2 & Corstiaan C. Breugem1 Received: 8 July 2015 /Accepted: 17 April 2016 # The Author(s) 2016. This article is published with open access at Springerlink.com Abstract Conclusion More research is warranted to clarify the role of Objective Otitis media with effusion is common in infants the tensor veli palatini muscle in cleft palate-associated with an unrepaired cleft palate. Although its prevalence is Eustachian tube dysfunction and development of middle ear reduced after cleft surgery, many children continue to suffer problems. from middle ear problems during childhood. While the tensor Clinical relevance Optimized surgical management of cleft veli palatini muscle is thought to be involved in middle ear palate could potentially reduce associated middle ear ventilation, evidence about its exact anatomy, function, and problems. role in cleft palate surgery is limited. This study aimed to perform a thorough review of the lit- Keywords Cleft palate . Eustachian tube . Otitis media with erature on (1) the role of the tensor veli palatini muscle in the effusion . Tensor veli palatini muscle Eustachian tube opening and middle ear ventilation, (2) ana- tomical anomalies in cleft palate infants related to middle ear disease, and (3) their implications for surgical techniques used in cleft palate repair. Introduction Materials and methods A literature search on the MEDLINE database was performed using a combination of the keywords Otitis media with effusion is very common in infants with an Btensor veli palatini muscle,^ BEustachian tube,^ Botitis media unrepaired cleft palate under the age of 2 years. -

A Guide to Complete Denture Prosthetics
A Guide to Complete Denture Prosthetics VITA shade taking VITA shade communication VITA shade reproduction VITA shade control Date of issue 11.11 VITA shade, VITA made. Foreword The aim of this Complete Denture Prosthetics Guide is to inform on the development and implementation of the fundamental principles for the fabrication of complete dentures. In this manual the reader will find suggestions concerning clnical cases which present in daily practice. Its many features include an introduction to the anatomy of the human masticatory system, explanations of its functions and problems encountered on the path to achieving well functioning complete dentures. The majority of complete denture cases which present in everyday practice can be addressed with the aid of knowledge contained in this instruction manual. Of course a central recommendation is that there be as close as possible collaboration between dentist and dental technician, both with each other and with the patient. This provides the optimum circumstances for an accurate and seamless flow of information. It follows also that to invest the time required to learn and absorb the patient’s dental history as well as follow the procedural chain in the fabrication procedure will always bring the best possible results. Complete dentures are restorations which demand a high degree of knowledge and skill from their creators. Each working step must yield the maximum result, the sum of which means an increased quality of life for the patient. In regard to the choice of occlusal concept is to be used, is a question best answered by the dentist and dental technician working together as a team. -
Morfofunctional Structure of the Skull
N.L. Svintsytska V.H. Hryn Morfofunctional structure of the skull Study guide Poltava 2016 Ministry of Public Health of Ukraine Public Institution «Central Methodological Office for Higher Medical Education of MPH of Ukraine» Higher State Educational Establishment of Ukraine «Ukranian Medical Stomatological Academy» N.L. Svintsytska, V.H. Hryn Morfofunctional structure of the skull Study guide Poltava 2016 2 LBC 28.706 UDC 611.714/716 S 24 «Recommended by the Ministry of Health of Ukraine as textbook for English- speaking students of higher educational institutions of the MPH of Ukraine» (minutes of the meeting of the Commission for the organization of training and methodical literature for the persons enrolled in higher medical (pharmaceutical) educational establishments of postgraduate education MPH of Ukraine, from 02.06.2016 №2). Letter of the MPH of Ukraine of 11.07.2016 № 08.01-30/17321 Composed by: N.L. Svintsytska, Associate Professor at the Department of Human Anatomy of Higher State Educational Establishment of Ukraine «Ukrainian Medical Stomatological Academy», PhD in Medicine, Associate Professor V.H. Hryn, Associate Professor at the Department of Human Anatomy of Higher State Educational Establishment of Ukraine «Ukrainian Medical Stomatological Academy», PhD in Medicine, Associate Professor This textbook is intended for undergraduate, postgraduate students and continuing education of health care professionals in a variety of clinical disciplines (medicine, pediatrics, dentistry) as it includes the basic concepts of human anatomy of the skull in adults and newborns. Rewiewed by: O.M. Slobodian, Head of the Department of Anatomy, Topographic Anatomy and Operative Surgery of Higher State Educational Establishment of Ukraine «Bukovinian State Medical University», Doctor of Medical Sciences, Professor M.V. -

The Myloglossus in a Human Cadaver Study: Common Or Uncommon Anatomical Structure? B
Folia Morphol. Vol. 76, No. 1, pp. 74–81 DOI: 10.5603/FM.a2016.0044 O R I G I N A L A R T I C L E Copyright © 2017 Via Medica ISSN 0015–5659 www.fm.viamedica.pl The myloglossus in a human cadaver study: common or uncommon anatomical structure? B. Buffoli*, M. Ferrari*, F. Belotti, D. Lancini, M.A. Cocchi, M. Labanca, M. Tschabitscher, R. Rezzani, L.F. Rodella Section of Anatomy and Physiopathology, Department of Clinical and Experimental Sciences, University of Brescia, Brescia, Italy [Received: 1 June 2016; Accepted: 18 July 2016] Background: Additional extrinsic muscles of the tongue are reported in literature and one of them is the myloglossus muscle (MGM). Since MGM is nowadays considered as anatomical variant, the aim of this study is to clarify some open questions by evaluating and describing the myloglossal anatomy (including both MGM and its ligamentous counterpart) during human cadaver dissections. Materials and methods: Twenty-one regions (including masticator space, sublin- gual space and adjacent areas) were dissected and the presence and appearance of myloglossus were considered, together with its proximal and distal insertions, vascularisation and innervation. Results: The myloglossus was present in 61.9% of cases with muscular, ligamen- tous or mixed appearance and either bony or muscular insertion. Facial artery pro- vided myloglossal vascularisation in the 84.62% and lingual artery in the 15.38%; innervation was granted by the trigeminal system (buccal nerve and mylohyoid nerve), sometimes (46.15%) with hypoglossal component. Conclusions: These data suggest us to not consider myloglossus as a rare ana- tomical variant. -

MRI-Based Assessment of Masticatory Muscle Changes in TMD Patients After Whiplash Injury
Journal of Clinical Medicine Article MRI-Based Assessment of Masticatory Muscle Changes in TMD Patients after Whiplash Injury Yeon-Hee Lee 1,* , Kyung Mi Lee 2 and Q-Schick Auh 1 1 Department of Orofacial Pain and Oral Medicine, Kyung Hee University Dental Hospital, #613 Hoegi-dong, Dongdaemun-gu, Seoul 02447, Korea; [email protected] 2 Department of Radiology, Kyung Hee University College of Medicine, Kyung Hee University Hospital, #26 Kyunghee-daero, Dongdaemun-gu, Seoul 02447, Korea; [email protected] * Correspondence: [email protected]; Tel.: +82-2-958-9409; Fax: +82-2-968-0588 Abstract: Objective: to investigate the change in volume and signal in the masticatory muscles and temporomandibular joint (TMJ) of patients with temporomandibular disorder (TMD) after whiplash injury, based on magnetic resonance imaging (MRI), and to correlate them with other clinical parameters. Methods: ninety patients (64 women, 26 men; mean age: 39.36 ± 15.40 years), including 45 patients with symptoms of TMD after whiplash injury (wTMD), and 45 age- and sex- matched controls with TMD due to idiopathic causes (iTMD) were included. TMD was diagnosed using the study diagnostic criteria for TMD Axis I, and MRI findings of the TMJ and masticatory muscles were investigated. To evaluate the severity of TMD pain and muscle tenderness, we used a visual analog scale (VAS), palpation index (PI), and neck PI. Results: TMD indexes, including VAS, PI, and neck PI were significantly higher in the wTMD group. In the wTMD group, muscle tenderness was highest in the masseter muscle (71.1%), and muscle tenderness in the temporalis (60.0%), lateral pterygoid muscle (LPM) (22.2%), and medial pterygoid muscle (15.6%) was significantly more frequent than that in the iTMD group (all p < 0.05). -
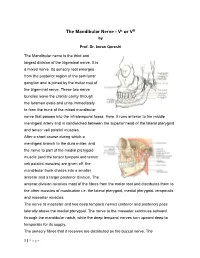
The Mandibular Nerve - Vc Or VIII by Prof
The Mandibular Nerve - Vc or VIII by Prof. Dr. Imran Qureshi The Mandibular nerve is the third and largest division of the trigeminal nerve. It is a mixed nerve. Its sensory root emerges from the posterior region of the semilunar ganglion and is joined by the motor root of the trigeminal nerve. These two nerve bundles leave the cranial cavity through the foramen ovale and unite immediately to form the trunk of the mixed mandibular nerve that passes into the infratemporal fossa. Here, it runs anterior to the middle meningeal artery and is sandwiched between the superior head of the lateral pterygoid and tensor veli palatini muscles. After a short course during which a meningeal branch to the dura mater, and the nerve to part of the medial pterygoid muscle (and the tensor tympani and tensor veli palatini muscles) are given off, the mandibular trunk divides into a smaller anterior and a larger posterior division. The anterior division receives most of the fibres from the motor root and distributes them to the other muscles of mastication i.e. the lateral pterygoid, medial pterygoid, temporalis and masseter muscles. The nerve to masseter and two deep temporal nerves (anterior and posterior) pass laterally above the medial pterygoid. The nerve to the masseter continues outward through the mandibular notch, while the deep temporal nerves turn upward deep to temporalis for its supply. The sensory fibres that it receives are distributed as the buccal nerve. The 1 | P a g e buccal nerve passes between the medial and lateral pterygoids and passes downward and forward to emerge from under cover of the masseter with the buccal artery. -

Chapter 2 Implants and Oral Anatomy
Chapter 2 Implants and oral anatomy Associate Professor of Maxillofacial Anatomy Section, Graduate School of Medical and Dental Sciences, Tokyo Medical and Dental University Tatsuo Terashima In recent years, the development of new materials and improvements in the operative methods used for implants have led to remarkable progress in the field of dental surgery. These methods have been applied widely in clinical practice. The development of computerized medical imaging technologies such as X-ray computed tomography have allowed detailed 3D-analysis of medical conditions, resulting in a dramatic improvement in the success rates of operative intervention. For treatment with a dental implant to be successful, it is however critical to have full knowledge and understanding of the fundamental anatomical structures of the oral and maxillofacial regions. In addition, it is necessary to understand variations in the topographic and anatomical structures among individuals, with age, and with pathological conditions. This chapter will discuss the basic structure of the oral cavity in relation to implant treatment. I. Osteology of the oral area The oral cavity is composed of the maxilla that is in contact with the cranial bone, palatine bone, the mobile mandible, and the hyoid bone. The maxilla and the palatine bones articulate with the cranial bone. The mandible articulates with the temporal bone through the temporomandibular joint (TMJ). The hyoid bone is suspended from the cranium and the mandible by the suprahyoid and infrahyoid muscles. The formation of the basis of the oral cavity by these bones and the associated muscles makes it possible for the oral cavity to perform its various functions. -

New Knowledge Resource for Anatomy Enables Comprehensive Searches of the Literature on the Feeding Muscles of Mammals
RESEARCH ARTICLE Muscle Logic: New Knowledge Resource for Anatomy Enables Comprehensive Searches of the Literature on the Feeding Muscles of Mammals Robert E. Druzinsky1*, James P. Balhoff2, Alfred W. Crompton3, James Done4, Rebecca Z. German5, Melissa A. Haendel6, Anthony Herrel7, Susan W. Herring8, Hilmar Lapp9,10, Paula M. Mabee11, Hans-Michael Muller4, Christopher J. Mungall12, Paul W. Sternberg4,13, a11111 Kimberly Van Auken4, Christopher J. Vinyard5, Susan H. Williams14, Christine E. Wall15 1 Department of Oral Biology, University of Illinois at Chicago, Chicago, Illinois, United States of America, 2 RTI International, Research Triangle Park, North Carolina, United States of America, 3 Organismic and Evolutionary Biology, Harvard University, Cambridge, Massachusetts, United States of America, 4 Division of Biology and Biological Engineering, M/C 156–29, California Institute of Technology, Pasadena, California, United States of America, 5 Department of Anatomy and Neurobiology, Northeast Ohio Medical University, Rootstown, Ohio, United States of America, 6 Oregon Health and Science University, Portland, Oregon, ’ OPEN ACCESS United States of America, 7 Département d Ecologie et de Gestion de la Biodiversité, Museum National d’Histoire Naturelle, Paris, France, 8 University of Washington, Department of Orthodontics, Seattle, Citation: Druzinsky RE, Balhoff JP, Crompton AW, Washington, United States of America, 9 National Evolutionary Synthesis Center, Durham, North Carolina, Done J, German RZ, Haendel MA, et al. (2016) United States of America, 10 Center for Genomic and Computational Biology, Duke University, Durham, Muscle Logic: New Knowledge Resource for North Carolina, United States of America, 11 Department of Biology, University of South Dakota, Vermillion, South Dakota, United States of America, 12 Genomics Division, Lawrence Berkeley National Laboratory, Anatomy Enables Comprehensive Searches of the Berkeley, California, United States of America, 13 Howard Hughes Medical Institute, M/C 156–29, California Literature on the Feeding Muscles of Mammals. -

Initial Stage of Fetal Development of the Pharyngotympanic Tube Cartilage with Special Reference to Muscle Attachments to the Tube
Original Article http://dx.doi.org/10.5115/acb.2012.45.3.185 pISSN 2093-3665 eISSN 2093-3673 Initial stage of fetal development of the pharyngotympanic tube cartilage with special reference to muscle attachments to the tube Yukio Katori1, Jose Francisco Rodríguez-Vázquez2, Samuel Verdugo-López2, Gen Murakami3, Tetsuaki Kawase4,5, Toshimitsu Kobayashi5 1Division of Otorhinolaryngology, Sendai Municipal Hospital, Sendai, Japan, 2Department of Anatomy and Embryology II, Faculty of Medicine, Complutense University, Madrid, Spain, 3Division of Internal Medicine, Iwamizawa Kojin-kai Hospital, Iwamizawa, 4Laboratory of Rehabilitative Auditory Science, Tohoku University Graduate School of Biomedical Engineering, 5Department of Otolaryngology-Head and Neck Surgery, Tohoku University Graduate School of Medicine, Sendai, Japan Abstract: Fetal development of the cartilage of the pharyngotympanic tube (PTT) is characterized by its late start. We examined semiserial histological sections of 20 human fetuses at 14-18 weeks of gestation. As controls, we also observed sections of 5 large fetuses at around 30 weeks. At and around 14 weeks, the tubal cartilage first appeared in the posterior side of the pharyngeal opening of the PTT. The levator veli palatini muscle used a mucosal fold containing the initial cartilage for its downward path to the palate. Moreover, the cartilage is a limited hard attachment for the muscle. Therefore, the PTT and its cartilage seemed to play a critical role in early development of levator veli muscle. In contrast, the cartilage developed so that it extended laterally, along a fascia-like structure that connected with the tensor tympani muscle. This muscle appeared to exert mechanical stress on the initial cartilage. -

Computed Tomography of the Buccomasseteric Region: 1
605 Computed Tomography of the Buccomasseteric Region: 1. Anatomy Ira F. Braun 1 The differential diagnosis to consider in a patient presenting with a buccomasseteric James C. Hoffman, Jr. 1 region mass is rather lengthy. Precise preoperative localization of the mass and a determination of its extent and, it is hoped, histology will provide a most useful guide to the head and neck surgeon operating in this anatomically complex region. Part 1 of this article describes the computed tomographic anatomy of this region, while part 2 discusses pathologic changes. The clinical value of computed tomography as an imaging method for this region is emphasized. The differential diagnosis to consider in a patient with a mass in the buccomas seteric region, which may either be developmental, inflammatory, or neoplastic, comprises a rather lengthy list. The anatomic complexity of this region, defined arbitrarily by the soft tissue and bony structures including and surrounding the masseter muscle, excluding the parotid gland, makes the accurate anatomic diagnosis of masses in this region imperative if severe functional and cosmetic defects or even death are to be avoided during treatment. An initial crucial clinical pathoanatomic distinction is to classify the mass as extra- or intraparotid. Batsakis [1] recommends that every mass localized to the cheek region be considered a parotid tumor until proven otherwise. Precise clinical localization, however, is often exceedingly difficult. Obviously, further diagnosis and subsequent therapy is greatly facilitated once this differentiation is made. Computed tomography (CT), with its superior spatial and contrast resolution, has been shown to be an effective imaging method for the evaluation of disorders of the head and neck. -

Atlas of the Facial Nerve and Related Structures
Rhoton Yoshioka Atlas of the Facial Nerve Unique Atlas Opens Window and Related Structures Into Facial Nerve Anatomy… Atlas of the Facial Nerve and Related Structures and Related Nerve Facial of the Atlas “His meticulous methods of anatomical dissection and microsurgical techniques helped transform the primitive specialty of neurosurgery into the magnificent surgical discipline that it is today.”— Nobutaka Yoshioka American Association of Neurological Surgeons. Albert L. Rhoton, Jr. Nobutaka Yoshioka, MD, PhD and Albert L. Rhoton, Jr., MD have created an anatomical atlas of astounding precision. An unparalleled teaching tool, this atlas opens a unique window into the anatomical intricacies of complex facial nerves and related structures. An internationally renowned author, educator, brain anatomist, and neurosurgeon, Dr. Rhoton is regarded by colleagues as one of the fathers of modern microscopic neurosurgery. Dr. Yoshioka, an esteemed craniofacial reconstructive surgeon in Japan, mastered this precise dissection technique while undertaking a fellowship at Dr. Rhoton’s microanatomy lab, writing in the preface that within such precision images lies potential for surgical innovation. Special Features • Exquisite color photographs, prepared from carefully dissected latex injected cadavers, reveal anatomy layer by layer with remarkable detail and clarity • An added highlight, 3-D versions of these extraordinary images, are available online in the Thieme MediaCenter • Major sections include intracranial region and skull, upper facial and midfacial region, and lower facial and posterolateral neck region Organized by region, each layered dissection elucidates specific nerves and structures with pinpoint accuracy, providing the clinician with in-depth anatomical insights. Precise clinical explanations accompany each photograph. In tandem, the images and text provide an excellent foundation for understanding the nerves and structures impacted by neurosurgical-related pathologies as well as other conditions and injuries. -

Anatomy Respect in Implant Dentistry. Assortment, Location, Clinical Importance (Review Article)
ISSN: 2394-8418 DOI: https://doi.org/10.17352/jdps CLINICAL GROUP Received: 19 August, 2020 Review Article Accepted: 31 August, 2020 Published: 01 September, 2020 *Corresponding author: Dr. Rawaa Y Al-Rawee, BDS, Anatomy Respect in Implant M Sc OS, MOMS MFDS RCPS Glasgow, PhD, MaxFacs, Department of Oral and Maxillofacial Surgery, Al-Salam Dentistry. Assortment, Teaching Hospital, Mosul, Iraq, Tel: 009647726438648; E-mail: Location, Clinical Importance ORCID: https://orcid.org/0000-0003-2554-1121 Keywords: Anatomical structures; Dental implants; (Review Article) Basic implant protocol; Success criteria; Clinical anatomy Rawaa Y Al-Rawee1* and Mohammed Mikdad Abdalfattah2 https://www.peertechz.com 1Department of Oral and Maxillofacial Surgery, Al-Salam Teaching Hospital. Mosul, Iraq 2Post Graduate Student in School of Dentistry, University of Leeds. United Kingdom, Ministry of Health, Iraq Abstract Aims: In this article; we will reviews critically important basic structures routinely encountered in implant therapy. It can be a brief anatomical reference for beginners in the fi eld of dental implant surgeries. Highlighting the clinical importance of each anatomical structure can be benefi cial for fast informations refreshing. Also it can be used as clinical anatomical guide for implantologist and professionals in advanced surgical procedures. Background: Basic anatomy understanding prior to implant therapy; it's an important fi rst step in dental implant surgery protocol specifi cally with technology advances and the popularity of dental implantation as a primary choice for replacement loosed teeth. A thorough perception of anatomy provides the implant surgeon with the confi dence to deal with hard or soft tissues in efforts to restore the exact aim of implantation whether function or esthetics and end with improving health and quality of life.