A Review: the Duffy Blood Group System
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Duffy, and Mnss Group Systems
Blood Groups – Duffy, and MNSs Group Systems Qun Lu, MD Assistant Professor Division of Transfusion Medicine Department of Pathology and Laboratory Medicine UCLA, School of Medicine Los Angeles, California 2009-03-12 Duffy Blood Group System History . 1950: Mrs. Duffy, a multiply transfused hemophiliac woman, developed an antibody not reacting with the known RBC antigens. Corresponding antigen was named after Mrs. Duffy . 1951: Fyb antibody was described in a woman with 3 pregnancies. 1955: Majority of blacks tested Fy(a-b-) . 1975: Fy(a-b-) RBCs were shown to resist infection by malaria organism Plasmodium vivax. Later: more Duffy antigens (Fy3, Fy4, Fy5, Fy6) were discovered . ISBT: 008 for the Duffy Blood Group Duffy Antigens . Most common: Fya and Fyb. Present at 6 weeks of gestation, well developed at birth – anti- Fy can cause hemolytic disease of newborn . Duffy antigens can be destroyed by enzymes such as ficin, papain, bromelain, chymotrypsin, ZZAP . When compared to Rh or Kell antigens, Duffy antigens are not very immunogenic. So, anti-Fya or anti-Fyb is not common. Fy (a-b-) is not Fy null, but homozygous for Fyb gene, they express Fyb antigen in other tissues, but not on RBCs → only will produce anti-Fya, not anti-Fyb. Fy (a-b-) is negative for Fy6 antigen which is the receptor for P. vivax (Fy6 is + when Fya + or Fyb+) Duffy Antigens . Phenotype Frequencies Chinese Phenotype Whites % Blacks % % Fy (a+b-) 17 9 90.8 Fy (a+b+) 49 1 8.9 Fy (a-b+) 34 22 0.3 Fy (a-b-) rare 68 0 White donor population: Fya: 66% Caucasians, 10% Blacks, 99% Asians Fya – units: 35% Fyb: 83% Caucasians, 23% Blacks, 18.5% Asians Fyb – units: 15% Fy3: 100% Caucasians, 32% Blacks, 99.9% Asians Duffy Antigens . -

Human and Mouse CD Marker Handbook Human and Mouse CD Marker Key Markers - Human Key Markers - Mouse
Welcome to More Choice CD Marker Handbook For more information, please visit: Human bdbiosciences.com/eu/go/humancdmarkers Mouse bdbiosciences.com/eu/go/mousecdmarkers Human and Mouse CD Marker Handbook Human and Mouse CD Marker Key Markers - Human Key Markers - Mouse CD3 CD3 CD (cluster of differentiation) molecules are cell surface markers T Cell CD4 CD4 useful for the identification and characterization of leukocytes. The CD CD8 CD8 nomenclature was developed and is maintained through the HLDA (Human Leukocyte Differentiation Antigens) workshop started in 1982. CD45R/B220 CD19 CD19 The goal is to provide standardization of monoclonal antibodies to B Cell CD20 CD22 (B cell activation marker) human antigens across laboratories. To characterize or “workshop” the antibodies, multiple laboratories carry out blind analyses of antibodies. These results independently validate antibody specificity. CD11c CD11c Dendritic Cell CD123 CD123 While the CD nomenclature has been developed for use with human antigens, it is applied to corresponding mouse antigens as well as antigens from other species. However, the mouse and other species NK Cell CD56 CD335 (NKp46) antibodies are not tested by HLDA. Human CD markers were reviewed by the HLDA. New CD markers Stem Cell/ CD34 CD34 were established at the HLDA9 meeting held in Barcelona in 2010. For Precursor hematopoetic stem cell only hematopoetic stem cell only additional information and CD markers please visit www.hcdm.org. Macrophage/ CD14 CD11b/ Mac-1 Monocyte CD33 Ly-71 (F4/80) CD66b Granulocyte CD66b Gr-1/Ly6G Ly6C CD41 CD41 CD61 (Integrin b3) CD61 Platelet CD9 CD62 CD62P (activated platelets) CD235a CD235a Erythrocyte Ter-119 CD146 MECA-32 CD106 CD146 Endothelial Cell CD31 CD62E (activated endothelial cells) Epithelial Cell CD236 CD326 (EPCAM1) For Research Use Only. -

Policy and Procedure
Policy and Procedure Title: Exchange Transfusion for Sickle Cell Division: Medical Management Disease Department: Utilization Management Approval Date: 2/9/18 LOB: Medicaid, Medicare, HIV SNP, CHP, MetroPlus Gold, Goldcare I&II, Market Plus, Essential, HARP Effective Date: 2/9/18 Policy Number: UM-MP224 Review Date: 1/18/19 Cross Reference Number: Retired Date: Page 1 of 7 1. POLICY: Exchange Transfusion for Sickle Cell Disease 2. RESPONSIBLE PARTIES: Medical Management Administration, Utilization Management, Integrated Care Management, Claims Department, Provider Contracting 3. DEFINITIONS • Sickle cell disease – Sickle cell disease (SCD) refers to a group of inherited disorders characterized by sickled red blood cells (RBCs), caused either by homozygosity for the sickle hemoglobin mutation (HbSS; sickle cell anemia) or by compound heterozygosity for the sickle mutation and a second beta globin gene mutation (e.g., sickle-beta thalassemia, HbSC disease). In either HbSS or compound heterozygotes, the majority of Hgb is sickle Hgb (HgbS; i.e., >50 percent). • Transfusion – Simple transfusion refers to transfusion of RBCs without removal of the patient's blood. • Exchange Transfusion – Exchange transfusion involves transfusion of RBCs together with removal of the patient's blood. Exchange transfusion can be performed manually or via apheresis (also called cytapheresis or hemapheresis) using an extracorporeal continuous flow device. 4. PROCEDURE: A. Exchange transfusion for sickle cell disease will be covered as an ambulatory surgery procedure when all the following criteria are met: i) The member has documented SCD. ii) The exchange transfusion is a pre-scheduled procedure. iii) The purpose of the exchange transfusion is to prevent stroke, acute chest syndrome, or recurrent painful episodes. -

Sickle Cell Disease: Chronic Blood Transfusions
Sickle Cell Disease: Chronic Blood Transfusions There may be times when sickle cell patients require a blood transfusion. Such situations include preparing for surgery, during pregnancy, or during a severe complication such as an aplastic crisis, splenic sequestration or acute chest syndrome. In these cases, transfusion is a one-time intervention used to reduce the severity of the complication you are experiencing. However, if you have had a stroke, or an MRI or TCD shows that you are at high risk for having a stroke, your hematologist may recommend you begin chronic blood transfusions. What Does a Blood Transfusion Do? What are The Risks? Chronic (monthly) blood transfusions have been proven to Blood transfusions are not without risks. One risk is drastically reduce a sickle cell patient’s risk of stroke. They alloimmunization, a process in which the patient receiving have also been shown to reduce the frequency, severity blood transfusions creates antibodies to certain types of and duration of other sickle cell complications. Sickle cell blood. As a result he/she may have a reaction to the blood patients usually have a hemoglobin S level of about 80- that was transfused. Alloimmunization makes it more 90%. This means 80-90% of the circulating red blood cells difficult to find blood that is a good match for the patient. are cells that can sickle and cause complications. The goal In order to prevent alloimmunization, some centers of chronic blood transfusion therapy is to bring that routinely perform RBC phenotyping (special testing for percentage down below 30%. This will mean fewer sickle antibodies) on sickle cell disease patients so that they may cells circulating in the body, and a lower risk of give blood that is a better match for the patient. -

Evolving Strategies in the Diagnosis and Management of Hemolytic Disease of the Fetus and Newborn
SUPPLEMENT TO FREE CME Credit To receive CME credit, please read the articles and go to www.omniaeducation.com/HDFN to access the posttest November 2020 and evaluation. CME CREDITS: .25 CREDITS To receive CME credit, please read the articles and go to www.omniaeducation.com/HDFN to access the post-test Evolving Strategies in the and evaluation. Diagnosis and Management OVERVIEW: Hemolytic disease of the fetus and newborn (HDFN) of Hemolytic Disease of the is a rare condition with an estimated 3 to 80 cases per 100,000 persons annually in the United States. Nonetheless, Fetus and Newborn the complexity and increased risk for adverse outcomes in such cases requires more targeted approaches to HDFN that minimize or negate the risks associated with intrauterine transfusion. Kenneth J. Moise, Jr., MD Department of Obstetrics, Gynecology and This article focuses on the pathophysiology underlying Reproductive Sciences fetal/newborn allo- and autoimmune diseases, especially McGovern School of Medicine – UT Health HDFN and the current/evolving diagnostic and treatment The Fetal Center regimens for HDFN. Children’s Memorial Hermann Hospital REVIEWERS/CONTENT PLANNERS/AUTHORS: Houston, Texas • Sean T. Barrett has nothing to disclose. • Barry A. Fiedel, PhD has nothing to disclose. • Amanda Hilferty has nothing to disclose. Once a significant cause of perinatal loss, alloimmu- • Kenneth J. Moise, Jr., MD receives royalties from Up-To-Date, Inc. and has contracted research with Momenta nization to red cell antigens is infrequently encoun- Pharmaceuticals Inc. tered in obstetrical practice today. Although maternal • Robert Schneider, MSW, has nothing to disclose. alloimmunization to the rhesus blood group D (RhD) • Lee Philip Shulman, MD, FACOG, FACMG, receives antigen remains the leading cause of fetal anemia, consulting fees from Biogix, Celula, Cooper Surgical, Natera, and Vermillion/Aspira, is a speaker for Bayer, more than 50 different red cell antigens have been Lupin Pharmaceuticals, Inc., and Myriad. -
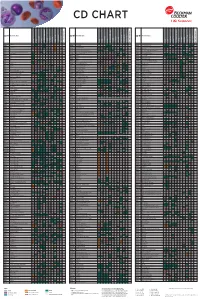
Flow Reagents Single Color Antibodies CD Chart
CD CHART CD N° Alternative Name CD N° Alternative Name CD N° Alternative Name Beckman Coulter Clone Beckman Coulter Clone Beckman Coulter Clone T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells CD1a T6, R4, HTA1 Act p n n p n n S l CD99 MIC2 gene product, E2 p p p CD223 LAG-3 (Lymphocyte activation gene 3) Act n Act p n CD1b R1 Act p n n p n n S CD99R restricted CD99 p p CD224 GGT (γ-glutamyl transferase) p p p p p p CD1c R7, M241 Act S n n p n n S l CD100 SEMA4D (semaphorin 4D) p Low p p p n n CD225 Leu13, interferon induced transmembrane protein 1 (IFITM1). p p p p p CD1d R3 Act S n n Low n n S Intest CD101 V7, P126 Act n p n p n n p CD226 DNAM-1, PTA-1 Act n Act Act Act n p n CD1e R2 n n n n S CD102 ICAM-2 (intercellular adhesion molecule-2) p p n p Folli p CD227 MUC1, mucin 1, episialin, PUM, PEM, EMA, DF3, H23 Act p CD2 T11; Tp50; sheep red blood cell (SRBC) receptor; LFA-2 p S n p n n l CD103 HML-1 (human mucosal lymphocytes antigen 1), integrin aE chain S n n n n n n n l CD228 Melanotransferrin (MT), p97 p p CD3 T3, CD3 complex p n n n n n n n n n l CD104 integrin b4 chain; TSP-1180 n n n n n n n p p CD229 Ly9, T-lymphocyte surface antigen p p n p n -

Analysis of RNA Expression Profiles Identifies Dysregulated Vesicle Trafficking Pathways in Creutzfeldt-Jakob Disease
Molecular Neurobiology (2019) 56:5009–5024 https://doi.org/10.1007/s12035-018-1421-1 Analysis of RNA Expression Profiles Identifies Dysregulated Vesicle Trafficking Pathways in Creutzfeldt-Jakob Disease Anna Bartoletti-Stella1 & Patrizia Corrado2 & Nicola Mometto2 & Simone Baiardi2 & Pascal F. Durrenberger3 & Thomas Arzberger4,5 & Richard Reynolds6 & Hans Kretzschmar5 & Sabina Capellari1,2 & Piero Parchi1,7 Received: 18 July 2018 /Accepted: 1 November 2018 /Published online: 16 November 2018 # Springer Science+Business Media, LLC, part of Springer Nature 2018 Abstract Functional genomics applied to the study of RNA expression profiles identified several abnormal molecular processes in experimental prion disease. However, only a few similar studies have been carried out to date in a naturally occurring human prion disease. To better characterize the transcriptional cascades associated with sporadic Creutzfeldt-Jakob disease (sCJD), the most common human prion disease, we investigated the global gene expression profile in samples from the frontal cortex of 10 patients with sCJD and 10 non-neurological controls by microarray analysis. The comparison identified 333 highly differentially expressed genes (hDEGs) in sCJD. Functional enrichment Gene Ontology analysis revealed that hDEGs were mainly associated with synaptic transmission, including GABA (q value = 0.049) and glutamate (q value = 0.005) signaling, and the immune/ inflammatory response. Furthermore, the analysis of cellular components performed on hDEGs showed a compromised regu- lation of vesicle-mediated transport with mainly up-regulated genes related to the endosome (q value = 0.01), lysosome (q value = 0.04), and extracellular exosome (q value < 0.01). A targeted analysis of the retromer core component VPS35 (vacuolar protein sorting-associated protein 35) showed a down-regulation of gene expression (p value= 0.006) and reduced brain protein levels (p value= 0.002). -

Quantitation of the Number of Molecules of Glycophorins C and D on Normal Red Blood Cells Using Radioiodinatedfab Fragments of Monoclonal Antibodies
Quantitation of the Number of Molecules of Glycophorins C and D on Normal Red Blood Cells Using RadioiodinatedFab Fragments of Monoclonal Antibodies By Jon Smythe, Brigitte Gardner, andDavid J. Anstee Two rat monoclonal antibodies (BRAC 1 and BRAC 1 1 ) cytes. Fabfragments of BRAC 1 1 and ERIC 10 gave values have been produced. BRAC 1 recognizes an epitope com- of 143,000 molecules GPC per red blood cell (RBC). Fab mon to the human erythrocyte membrane glycoproteins fragments of BRAC1 gave 225,000 molecules of GPC and glycophorin C (GPC) and glycophorin D (GPD). BRAC 11 GPD per RBC. These results indicate that GPC and GPD is specific for GPC. Fabfragments of these antibodies and together are sufficiently abundantto provide membrane at- BRlC 10, a murine monoclonal anti-GPC,were radioiodin- tachment sites for all ofthe protein 4.1 in normal RBCs. ated and used in quantitative binding assays to measure 0 1994 by The American Societyof Hematology. the number of GPC and GPD molecules on normal erythro- HE SHAPE AND deformability of the mature human (200,000)" and those reported for GPC (50,000).7 This nu- Downloaded from http://ashpublications.org/blood/article-pdf/83/6/1668/612763/1668.pdf by guest on 24 September 2021 T erythrocyte is controlled by a flexible two-dimensional merical differencehas led to the suggestion that a significant lattice of proteins, which together comprise the membrane proportion of protein 4.1 in normal erythrocyte membranes skeleton.' The major components of the skeleton are spec- must be bound to sites other than GPC and GPD.3 The trin, actin, ankyrin, and protein 4.1. -

CD Markers Are Routinely Used for the Immunophenotyping of Cells
ptglab.com 1 CD MARKER ANTIBODIES www.ptglab.com Introduction The cluster of differentiation (abbreviated as CD) is a protocol used for the identification and investigation of cell surface molecules. So-called CD markers are routinely used for the immunophenotyping of cells. Despite this use, they are not limited to roles in the immune system and perform a variety of roles in cell differentiation, adhesion, migration, blood clotting, gamete fertilization, amino acid transport and apoptosis, among many others. As such, Proteintech’s mini catalog featuring its antibodies targeting CD markers is applicable to a wide range of research disciplines. PRODUCT FOCUS PECAM1 Platelet endothelial cell adhesion of blood vessels – making up a large portion molecule-1 (PECAM1), also known as cluster of its intracellular junctions. PECAM-1 is also CD Number of differentiation 31 (CD31), is a member of present on the surface of hematopoietic the immunoglobulin gene superfamily of cell cells and immune cells including platelets, CD31 adhesion molecules. It is highly expressed monocytes, neutrophils, natural killer cells, on the surface of the endothelium – the thin megakaryocytes and some types of T-cell. Catalog Number layer of endothelial cells lining the interior 11256-1-AP Type Rabbit Polyclonal Applications ELISA, FC, IF, IHC, IP, WB 16 Publications Immunohistochemical of paraffin-embedded Figure 1: Immunofluorescence staining human hepatocirrhosis using PECAM1, CD31 of PECAM1 (11256-1-AP), Alexa 488 goat antibody (11265-1-AP) at a dilution of 1:50 anti-rabbit (green), and smooth muscle KD/KO Validated (40x objective). alpha-actin (red), courtesy of Nicola Smart. PECAM1: Customer Testimonial Nicola Smart, a cardiovascular researcher “As you can see [the immunostaining] is and a group leader at the University of extremely clean and specific [and] displays Oxford, has said of the PECAM1 antibody strong intercellular junction expression, (11265-1-AP) that it “worked beautifully as expected for a cell adhesion molecule.” on every occasion I’ve tried it.” Proteintech thanks Dr. -

Pediatric Orthotopic Heart Transplant Requiring Perioperative Exchange Transfusion: a Case Report
JECT. 2004;36:361–363 The Journal of The American Society of Extra-Corporeal Technology Case Reports Pediatric Orthotopic Heart Transplant Requiring Perioperative Exchange Transfusion: A Case Report Brian McNeer, BS; Brent Dickason, BS, RRT; Scott Niles, BA, CCP; Jay Ploessl, CCP The University of Iowa Hospitals and Clinics, Iowa City, Iowa Presented at the 41st International Conference of the American Society of Extra-Corporeal Technology, Las Vegas, Nevada, March 6–9, 2003 Abstract: An 11-month-old patient with idiopathic cardio- the venous line just proximal to the venous reservoir while si- myopathy was scheduled for orthotopic heart transplantation. A multaneously transfusing the normalized prime at normother- perioperative exchange transfusion was performed because of mia. Approximately 125% of the patients calculated blood vol- elevated panel reactive antibody levels. This process was accom- ume was exchanged. This technique greatly reduces the likeli- plished in the operating room prior to instituting cardiopulmo- hood of hyperacute rejection. The exchange transfusion process, nary bypass using a modified cardiopulmonary bypass circuit. In in addition to the patient immature immune system, provides preparation for the procedure, the cardiopulmonary bypass cir- additional options in orthotopic heart transplantation for pa- cuit was primed with washed leukocyte-filtered banked packed tients that may otherwise not be considered suitable candi- red blood cells, fresh-frozen plasma, albumin, and heparin. Pump dates. Keywords: exchange transfusion, heart transplant, pediat- prime laboratory values were normalized prior to beginning the ric, panel reactive antibodies. JECT. 2004;36:361–363 exchange transfusion. The patient’s blood was downloaded from Despite continuing advances in the management of end- humoral sensitization is determined by the presence of a stage cardiac failure, cardiac transplantation remains the positive panel reactive antibody (PRA) screen. -
Laboratory Best Transfusion Practice for Neonates, Infants and Children
Laboratory Best Transfusion Practice for Neonates, Infants and Children This summary guidance should be used in conjunction with the appropriate 20161 and 20122 BSH Guidelines and laboratory SOPs Compatibility testing Neonates and infants < 4 months Obtain neonatal and maternal transfusion history (including any fetal transfusions) for all admissions. Obtain a maternal sample for initial testing where possible, in addition to the patient sample. Red cell selection: no maternal antibodies present Select appropriate group and correct neonatal specification red cells. Group O D-negative red cells may be issued electronically without serological crossmatch. If the laboratory does not universally select group O D-negative red cells for this age group, blood group selection should either be controlled by the LIMS or an IAT crossmatch should be performed using maternal or neonatal plasma to serologically confirm ABO compatibility with both mother and neonate. Red cell selection: where there is maternal antibody Select appropriate group red cells, compatible with maternal alloantibody/ies. An IAT crossmatch should be performed using the maternal plasma. If it is not possible to obtain a maternal sample it is acceptable to crossmatch antigen-negative units against the infant’s plasma. Where paedipacks are being issued from one donor unit it is only necessary to crossmatch the first split pack. Subsequent split packs from this multi-satellite unit can be automatically issued without further crossmatch until the unit expires or the infant is older than 4 months. If packs from a different donor are required, an IAT crossmatch should be performed. Infants and children ≥ 4 months For infants and children from 4 months of age, pre-transfusion testing and compatibility procedures should be performed as recommended for adults. -

Apheresis Red Cell Exchange/Transfusions
APHERESIS RED CELL EXCHANGE/TRANSFUSIONS In a patient treated in Manchester, parasitemia was virtually eliminated over eight hours by a 3.5 liter exchange blood transfusion (Plasmodium Falciparum Hyperparasitemia: Use of Exchange Transfusion in Seven Patients and a Review of the Literature). Several cases of severe babesiosis refractory to appropriate antibiotic therapy have been reported to respond promptly and dramatically to red blood cell (RBC) exchange transfusion. Asplenic patients, however, generally have a more severe course of illness, with hemolytic anemia, acute renal failure, disseminated intravascular coagulation, and pulmonary edema. Primary therapy is with antibiotics including clindamycin and quinine, with RBC exchange transfusion reported to be effective in severe cases. The RBC exchange transfusions succeeded in reducing significantly the level of parasitemia, dramatically improving the condition of an extremely ill patient. Our report adds to the small but growing literature on severe Babesia infection in humans, and provides further evidence to support the use of RBC exchange transfusion to treat severe babesiosis. Its single great advantage over antibiotic therapy is its rapid therapeutic effectiveness (Treatment of Babesiosis by Red Blood Cell Exchange in an HIV-Positive Splenectomized Patient). There was rapid clinical improvement after the whole-blood exchange transfusion. In cases of severe babesiosis, prompt institution of whole-blood exchange transfusion, in combination with appropriate antimicrobial therapy, can be life-saving. In patients with progressive babesiosis, early intervention with exchange transfusion, along with appropriate antimicrobial therapy, should be considered to speed clinical recovery. (Fulminant babesiosis treated with clindamycin, quinine, and whole-blood exchange transfusion. However, asplenic patients may have a much more serious clinical course.