IL-7-Stimulated T Lymphocytes Correlated with Cell Cycle
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Duffy, and Mnss Group Systems
Blood Groups – Duffy, and MNSs Group Systems Qun Lu, MD Assistant Professor Division of Transfusion Medicine Department of Pathology and Laboratory Medicine UCLA, School of Medicine Los Angeles, California 2009-03-12 Duffy Blood Group System History . 1950: Mrs. Duffy, a multiply transfused hemophiliac woman, developed an antibody not reacting with the known RBC antigens. Corresponding antigen was named after Mrs. Duffy . 1951: Fyb antibody was described in a woman with 3 pregnancies. 1955: Majority of blacks tested Fy(a-b-) . 1975: Fy(a-b-) RBCs were shown to resist infection by malaria organism Plasmodium vivax. Later: more Duffy antigens (Fy3, Fy4, Fy5, Fy6) were discovered . ISBT: 008 for the Duffy Blood Group Duffy Antigens . Most common: Fya and Fyb. Present at 6 weeks of gestation, well developed at birth – anti- Fy can cause hemolytic disease of newborn . Duffy antigens can be destroyed by enzymes such as ficin, papain, bromelain, chymotrypsin, ZZAP . When compared to Rh or Kell antigens, Duffy antigens are not very immunogenic. So, anti-Fya or anti-Fyb is not common. Fy (a-b-) is not Fy null, but homozygous for Fyb gene, they express Fyb antigen in other tissues, but not on RBCs → only will produce anti-Fya, not anti-Fyb. Fy (a-b-) is negative for Fy6 antigen which is the receptor for P. vivax (Fy6 is + when Fya + or Fyb+) Duffy Antigens . Phenotype Frequencies Chinese Phenotype Whites % Blacks % % Fy (a+b-) 17 9 90.8 Fy (a+b+) 49 1 8.9 Fy (a-b+) 34 22 0.3 Fy (a-b-) rare 68 0 White donor population: Fya: 66% Caucasians, 10% Blacks, 99% Asians Fya – units: 35% Fyb: 83% Caucasians, 23% Blacks, 18.5% Asians Fyb – units: 15% Fy3: 100% Caucasians, 32% Blacks, 99.9% Asians Duffy Antigens . -

Human and Mouse CD Marker Handbook Human and Mouse CD Marker Key Markers - Human Key Markers - Mouse
Welcome to More Choice CD Marker Handbook For more information, please visit: Human bdbiosciences.com/eu/go/humancdmarkers Mouse bdbiosciences.com/eu/go/mousecdmarkers Human and Mouse CD Marker Handbook Human and Mouse CD Marker Key Markers - Human Key Markers - Mouse CD3 CD3 CD (cluster of differentiation) molecules are cell surface markers T Cell CD4 CD4 useful for the identification and characterization of leukocytes. The CD CD8 CD8 nomenclature was developed and is maintained through the HLDA (Human Leukocyte Differentiation Antigens) workshop started in 1982. CD45R/B220 CD19 CD19 The goal is to provide standardization of monoclonal antibodies to B Cell CD20 CD22 (B cell activation marker) human antigens across laboratories. To characterize or “workshop” the antibodies, multiple laboratories carry out blind analyses of antibodies. These results independently validate antibody specificity. CD11c CD11c Dendritic Cell CD123 CD123 While the CD nomenclature has been developed for use with human antigens, it is applied to corresponding mouse antigens as well as antigens from other species. However, the mouse and other species NK Cell CD56 CD335 (NKp46) antibodies are not tested by HLDA. Human CD markers were reviewed by the HLDA. New CD markers Stem Cell/ CD34 CD34 were established at the HLDA9 meeting held in Barcelona in 2010. For Precursor hematopoetic stem cell only hematopoetic stem cell only additional information and CD markers please visit www.hcdm.org. Macrophage/ CD14 CD11b/ Mac-1 Monocyte CD33 Ly-71 (F4/80) CD66b Granulocyte CD66b Gr-1/Ly6G Ly6C CD41 CD41 CD61 (Integrin b3) CD61 Platelet CD9 CD62 CD62P (activated platelets) CD235a CD235a Erythrocyte Ter-119 CD146 MECA-32 CD106 CD146 Endothelial Cell CD31 CD62E (activated endothelial cells) Epithelial Cell CD236 CD326 (EPCAM1) For Research Use Only. -

Role of IL-4 Receptor &Alpha
Role of IL-4 receptor a–positive CD41 T cells in chronic airway hyperresponsiveness Frank Kirstein, PhD, Natalie E. Nieuwenhuizen, PhD,* Jaisubash Jayakumar, PhD, William G. C. Horsnell, PhD, and Frank Brombacher, PhD Cape Town, South Africa, and Berlin, Germany Background: TH2 cells and their cytokines are associated with IL-17–producing T cells and, consequently, increased airway allergic asthma in human subjects and with mouse models of neutrophilia. allergic airway disease. IL-4 signaling through the IL-4 receptor Conclusion: IL-4–responsive T helper cells are dispensable for 1 a (IL-4Ra) chain on CD4 T cells leads to TH2 cell acute OVA-induced airway disease but crucial in maintaining differentiation in vitro, implying that IL-4Ra–responsive CD41 chronic asthmatic pathology. (J Allergy Clin Immunol T cells are critical for the induction of allergic asthma. However, 2016;137:1852-62.) mechanisms regulating acute and chronic allergen-specific T 2 H Key words: responses in vivo remain incompletely understood. TH2 cell, acute allergic airway disease, chronic asthma, Objective: This study defines the requirements for IL-4Ra– cytokine receptors, IL-4, IL-13, gene-deficient mice responsive CD41 T cells and the IL-4Ra ligands IL-4 and IL-13 in the development of allergen-specific TH2 responses during the Allergic asthma is a chronic inflammatory disease of the airways onset and chronic phase of experimental allergic airway disease. characterized by an inappropriate immune response to harmless Methods: Development of acute and chronic ovalbumin environmental antigens. T 2 cells regulate adaptive immune 1 H (OVA)–induced allergic asthma was assessed weekly in CD4 T responses to allergens, and their presence correlates with disease 2 cell–specific IL-4Ra–deficient BALB/c mice (LckcreIL-4Ra /lox) symptoms in human subjects and mice.1 IL-4 plays a crucial role and respective control mice in the presence or absence of IL-4 in the in vitro and in vivo differentiation of TH2 cells, suggesting or IL-13. -

Anti-CD40 Antibody KPL-404 Inhibits T Cell
Marken et al. Arthritis Research & Therapy (2021) 23:5 https://doi.org/10.1186/s13075-020-02372-z RESEARCH ARTICLE Open Access Anti-CD40 antibody KPL-404 inhibits T cell- mediated activation of B cells from healthy donors and autoimmune patients John Marken1, Sujatha Muralidharan2* and Natalia V. Giltiay1* Abstract Background: CD40-CD40L is a key co-stimulatory pathway for B cell activation. As such, its blockade can inhibit pathogenic B cell responses in autoimmune diseases, such as Sjogren’s syndrome (SjS) and systemic lupus erythematosus (SLE). In this study, we examined the in vitro effects of KPL-404, a humanized anti-CD40 monoclonal antibody (Ab), on primary human B cells derived from either healthy donors (HD) or autoimmune patients and compared them to the effects of G28-5, a partially antagonistic anti-CD40 antibody. Methods: PBMCs from HD or SjS and SLE patients were cultured in high-density cell cultures in the presence of IgG4 isotype control or anti-CD40 Abs KPL-404 or G28-5. Cells were stimulated with anti-CD3/CD28 cross-linking reagent ImmunoCult (IC) to induce CD40L-CD40-mediated B cell responses. B cell proliferation and activation, measured by dilution of proliferation tracker dye and the upregulation of CD69 and CD86, respectively, were assessed by flow cytometry. Anti-CD40 Ab cell-internalization was examined by imaging flow cytometry. Cytokine release in the PBMC cultures was quantified by bead-based multiplex assay. Results: KPL-404 binds to CD40 expressed on different subsets of B cells without inducing cell depletion, or B cell proliferation and activation in in vitro culture. -
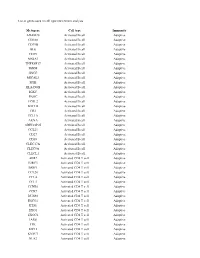
List of Genes Used in Cell Type Enrichment Analysis
List of genes used in cell type enrichment analysis Metagene Cell type Immunity ADAM28 Activated B cell Adaptive CD180 Activated B cell Adaptive CD79B Activated B cell Adaptive BLK Activated B cell Adaptive CD19 Activated B cell Adaptive MS4A1 Activated B cell Adaptive TNFRSF17 Activated B cell Adaptive IGHM Activated B cell Adaptive GNG7 Activated B cell Adaptive MICAL3 Activated B cell Adaptive SPIB Activated B cell Adaptive HLA-DOB Activated B cell Adaptive IGKC Activated B cell Adaptive PNOC Activated B cell Adaptive FCRL2 Activated B cell Adaptive BACH2 Activated B cell Adaptive CR2 Activated B cell Adaptive TCL1A Activated B cell Adaptive AKNA Activated B cell Adaptive ARHGAP25 Activated B cell Adaptive CCL21 Activated B cell Adaptive CD27 Activated B cell Adaptive CD38 Activated B cell Adaptive CLEC17A Activated B cell Adaptive CLEC9A Activated B cell Adaptive CLECL1 Activated B cell Adaptive AIM2 Activated CD4 T cell Adaptive BIRC3 Activated CD4 T cell Adaptive BRIP1 Activated CD4 T cell Adaptive CCL20 Activated CD4 T cell Adaptive CCL4 Activated CD4 T cell Adaptive CCL5 Activated CD4 T cell Adaptive CCNB1 Activated CD4 T cell Adaptive CCR7 Activated CD4 T cell Adaptive DUSP2 Activated CD4 T cell Adaptive ESCO2 Activated CD4 T cell Adaptive ETS1 Activated CD4 T cell Adaptive EXO1 Activated CD4 T cell Adaptive EXOC6 Activated CD4 T cell Adaptive IARS Activated CD4 T cell Adaptive ITK Activated CD4 T cell Adaptive KIF11 Activated CD4 T cell Adaptive KNTC1 Activated CD4 T cell Adaptive NUF2 Activated CD4 T cell Adaptive PRC1 Activated -

Single-Cell RNA Sequencing Demonstrates the Molecular and Cellular Reprogramming of Metastatic Lung Adenocarcinoma
ARTICLE https://doi.org/10.1038/s41467-020-16164-1 OPEN Single-cell RNA sequencing demonstrates the molecular and cellular reprogramming of metastatic lung adenocarcinoma Nayoung Kim 1,2,3,13, Hong Kwan Kim4,13, Kyungjong Lee 5,13, Yourae Hong 1,6, Jong Ho Cho4, Jung Won Choi7, Jung-Il Lee7, Yeon-Lim Suh8,BoMiKu9, Hye Hyeon Eum 1,2,3, Soyean Choi 1, Yoon-La Choi6,10,11, Je-Gun Joung1, Woong-Yang Park 1,2,6, Hyun Ae Jung12, Jong-Mu Sun12, Se-Hoon Lee12, ✉ ✉ Jin Seok Ahn12, Keunchil Park12, Myung-Ju Ahn 12 & Hae-Ock Lee 1,2,3,6 1234567890():,; Advanced metastatic cancer poses utmost clinical challenges and may present molecular and cellular features distinct from an early-stage cancer. Herein, we present single-cell tran- scriptome profiling of metastatic lung adenocarcinoma, the most prevalent histological lung cancer type diagnosed at stage IV in over 40% of all cases. From 208,506 cells populating the normal tissues or early to metastatic stage cancer in 44 patients, we identify a cancer cell subtype deviating from the normal differentiation trajectory and dominating the metastatic stage. In all stages, the stromal and immune cell dynamics reveal ontological and functional changes that create a pro-tumoral and immunosuppressive microenvironment. Normal resident myeloid cell populations are gradually replaced with monocyte-derived macrophages and dendritic cells, along with T-cell exhaustion. This extensive single-cell analysis enhances our understanding of molecular and cellular dynamics in metastatic lung cancer and reveals potential diagnostic and therapeutic targets in cancer-microenvironment interactions. 1 Samsung Genome Institute, Samsung Medical Center, Seoul 06351, Korea. -

B Cell Checkpoints in Autoimmune Rheumatic Diseases
REVIEWS B cell checkpoints in autoimmune rheumatic diseases Samuel J. S. Rubin1,2,3, Michelle S. Bloom1,2,3 and William H. Robinson1,2,3* Abstract | B cells have important functions in the pathogenesis of autoimmune diseases, including autoimmune rheumatic diseases. In addition to producing autoantibodies, B cells contribute to autoimmunity by serving as professional antigen- presenting cells (APCs), producing cytokines, and through additional mechanisms. B cell activation and effector functions are regulated by immune checkpoints, including both activating and inhibitory checkpoint receptors that contribute to the regulation of B cell tolerance, activation, antigen presentation, T cell help, class switching, antibody production and cytokine production. The various activating checkpoint receptors include B cell activating receptors that engage with cognate receptors on T cells or other cells, as well as Toll-like receptors that can provide dual stimulation to B cells via co- engagement with the B cell receptor. Furthermore, various inhibitory checkpoint receptors, including B cell inhibitory receptors, have important functions in regulating B cell development, activation and effector functions. Therapeutically targeting B cell checkpoints represents a promising strategy for the treatment of a variety of autoimmune rheumatic diseases. Antibody- dependent B cells are multifunctional lymphocytes that contribute that serve as precursors to and thereby give rise to acti- cell- mediated cytotoxicity to the pathogenesis of autoimmune diseases -
Flow Reagents Single Color Antibodies CD Chart
CD CHART CD N° Alternative Name CD N° Alternative Name CD N° Alternative Name Beckman Coulter Clone Beckman Coulter Clone Beckman Coulter Clone T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells CD1a T6, R4, HTA1 Act p n n p n n S l CD99 MIC2 gene product, E2 p p p CD223 LAG-3 (Lymphocyte activation gene 3) Act n Act p n CD1b R1 Act p n n p n n S CD99R restricted CD99 p p CD224 GGT (γ-glutamyl transferase) p p p p p p CD1c R7, M241 Act S n n p n n S l CD100 SEMA4D (semaphorin 4D) p Low p p p n n CD225 Leu13, interferon induced transmembrane protein 1 (IFITM1). p p p p p CD1d R3 Act S n n Low n n S Intest CD101 V7, P126 Act n p n p n n p CD226 DNAM-1, PTA-1 Act n Act Act Act n p n CD1e R2 n n n n S CD102 ICAM-2 (intercellular adhesion molecule-2) p p n p Folli p CD227 MUC1, mucin 1, episialin, PUM, PEM, EMA, DF3, H23 Act p CD2 T11; Tp50; sheep red blood cell (SRBC) receptor; LFA-2 p S n p n n l CD103 HML-1 (human mucosal lymphocytes antigen 1), integrin aE chain S n n n n n n n l CD228 Melanotransferrin (MT), p97 p p CD3 T3, CD3 complex p n n n n n n n n n l CD104 integrin b4 chain; TSP-1180 n n n n n n n p p CD229 Ly9, T-lymphocyte surface antigen p p n p n -

Analysis of RNA Expression Profiles Identifies Dysregulated Vesicle Trafficking Pathways in Creutzfeldt-Jakob Disease
Molecular Neurobiology (2019) 56:5009–5024 https://doi.org/10.1007/s12035-018-1421-1 Analysis of RNA Expression Profiles Identifies Dysregulated Vesicle Trafficking Pathways in Creutzfeldt-Jakob Disease Anna Bartoletti-Stella1 & Patrizia Corrado2 & Nicola Mometto2 & Simone Baiardi2 & Pascal F. Durrenberger3 & Thomas Arzberger4,5 & Richard Reynolds6 & Hans Kretzschmar5 & Sabina Capellari1,2 & Piero Parchi1,7 Received: 18 July 2018 /Accepted: 1 November 2018 /Published online: 16 November 2018 # Springer Science+Business Media, LLC, part of Springer Nature 2018 Abstract Functional genomics applied to the study of RNA expression profiles identified several abnormal molecular processes in experimental prion disease. However, only a few similar studies have been carried out to date in a naturally occurring human prion disease. To better characterize the transcriptional cascades associated with sporadic Creutzfeldt-Jakob disease (sCJD), the most common human prion disease, we investigated the global gene expression profile in samples from the frontal cortex of 10 patients with sCJD and 10 non-neurological controls by microarray analysis. The comparison identified 333 highly differentially expressed genes (hDEGs) in sCJD. Functional enrichment Gene Ontology analysis revealed that hDEGs were mainly associated with synaptic transmission, including GABA (q value = 0.049) and glutamate (q value = 0.005) signaling, and the immune/ inflammatory response. Furthermore, the analysis of cellular components performed on hDEGs showed a compromised regu- lation of vesicle-mediated transport with mainly up-regulated genes related to the endosome (q value = 0.01), lysosome (q value = 0.04), and extracellular exosome (q value < 0.01). A targeted analysis of the retromer core component VPS35 (vacuolar protein sorting-associated protein 35) showed a down-regulation of gene expression (p value= 0.006) and reduced brain protein levels (p value= 0.002). -

Quantitation of the Number of Molecules of Glycophorins C and D on Normal Red Blood Cells Using Radioiodinatedfab Fragments of Monoclonal Antibodies
Quantitation of the Number of Molecules of Glycophorins C and D on Normal Red Blood Cells Using RadioiodinatedFab Fragments of Monoclonal Antibodies By Jon Smythe, Brigitte Gardner, andDavid J. Anstee Two rat monoclonal antibodies (BRAC 1 and BRAC 1 1 ) cytes. Fabfragments of BRAC 1 1 and ERIC 10 gave values have been produced. BRAC 1 recognizes an epitope com- of 143,000 molecules GPC per red blood cell (RBC). Fab mon to the human erythrocyte membrane glycoproteins fragments of BRAC1 gave 225,000 molecules of GPC and glycophorin C (GPC) and glycophorin D (GPD). BRAC 11 GPD per RBC. These results indicate that GPC and GPD is specific for GPC. Fabfragments of these antibodies and together are sufficiently abundantto provide membrane at- BRlC 10, a murine monoclonal anti-GPC,were radioiodin- tachment sites for all ofthe protein 4.1 in normal RBCs. ated and used in quantitative binding assays to measure 0 1994 by The American Societyof Hematology. the number of GPC and GPD molecules on normal erythro- HE SHAPE AND deformability of the mature human (200,000)" and those reported for GPC (50,000).7 This nu- Downloaded from http://ashpublications.org/blood/article-pdf/83/6/1668/612763/1668.pdf by guest on 24 September 2021 T erythrocyte is controlled by a flexible two-dimensional merical differencehas led to the suggestion that a significant lattice of proteins, which together comprise the membrane proportion of protein 4.1 in normal erythrocyte membranes skeleton.' The major components of the skeleton are spec- must be bound to sites other than GPC and GPD.3 The trin, actin, ankyrin, and protein 4.1. -

Maturation and Is Inhibited by TLR2 Signaling Through TLR4 Promotes
Role of TLR in B Cell Development: Signaling through TLR4 Promotes B Cell Maturation and Is Inhibited by TLR2 This information is current as Elize A. Hayashi, Shizuo Akira and Alberto Nobrega of September 28, 2021. J Immunol 2005; 174:6639-6647; ; doi: 10.4049/jimmunol.174.11.6639 http://www.jimmunol.org/content/174/11/6639 Downloaded from References This article cites 45 articles, 26 of which you can access for free at: http://www.jimmunol.org/content/174/11/6639.full#ref-list-1 Why The JI? Submit online. http://www.jimmunol.org/ • Rapid Reviews! 30 days* from submission to initial decision • No Triage! Every submission reviewed by practicing scientists • Fast Publication! 4 weeks from acceptance to publication *average by guest on September 28, 2021 Subscription Information about subscribing to The Journal of Immunology is online at: http://jimmunol.org/subscription Permissions Submit copyright permission requests at: http://www.aai.org/About/Publications/JI/copyright.html Email Alerts Receive free email-alerts when new articles cite this article. Sign up at: http://jimmunol.org/alerts The Journal of Immunology is published twice each month by The American Association of Immunologists, Inc., 1451 Rockville Pike, Suite 650, Rockville, MD 20852 Copyright © 2005 by The American Association of Immunologists All rights reserved. Print ISSN: 0022-1767 Online ISSN: 1550-6606. The Journal of Immunology Role of TLR in B Cell Development: Signaling through TLR4 Promotes B Cell Maturation and Is Inhibited by TLR21 Elize A. Hayashi,* Shizuo Akira,† and Alberto Nobrega2* The role of TLR4 in mature B cell activation is well characterized. -

Cd4/Cd8 Panel, Blood
Lab Dept: Flow and Immunology Test Name: CD4/CD8 PANEL, BLOOD General Information Lab Order Codes: C48P Synonyms: Helper/Suppressor Ratio; T- cells; T-cell subsets; T-cell phenotyping See also: Immune Status Panel and Comprehensive Immune Status Panel CPT Codes: 86359 – T cells, total count 86360 – T cells; absolute CD4 and CD8 count, including ratio Test Includes: CD4(CD3+) and CD8(CD3+) relative percentages, absolute values and a calculated Helper/Suppressor ratio. Logistics Test Indications: This is a minimal antibody panel to monitor immune status. Lab Testing Sections: Flow Cytometry Phone Numbers: MIN Lab: 612-813-6280 STP Lab: 651-220-6550 Test Availability: 3 times weekly determined by volume. Transport collected specimen immediately to Flow Cytometry. Routine testing is not available on weekends or holidays. Therefore, specimens cannot be used if drawn the day before a 3 day weekend such as Memorial Day, Labor Day or major holiday that falls on a Monday or Friday. Turnaround Time: 1 – 3 days Special Instructions: See Test Availability Specimen Specimen Type: Whole blood Container: Lavender top (EDTA) tube Draw Volume: 2 mL blood in a 2 mL Lavender (EDTA) tube Minimum volume: 0.5 mL in an EDTA microtainer Collection: Routine venipuncture Special Processing: Keep sample at room temperature and forward promptly to the laboratory. Do not centrifuge, refrigerate, or freeze sample. Patient Preparation: None Sample Rejection: Specimens will not be processed that are clotted; hemolyzed; greater than 72 hours old; collected in the wrong tube type (0.5 mL in a 2 mL tube), or that have been held or handled at a temperature other than room temperature Interpretive Reference Range: Age-dependant reference ranges provided with results.