Epidemiological Characteristics of Measles from 2000 to 2014: Results
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

China. Energy Conservation and Greenhouse Gas Emissions
OCCASION This publication has been made available to the public on the occasion of the 50th anniversary of the United Nations Industrial Development Organisation. DISCLAIMER This document has been produced without formal United Nations editing. The designations employed and the presentation of the material in this document do not imply the expression of any opinion whatsoever on the part of the Secretariat of the United Nations Industrial Development Organization (UNIDO) concerning the legal status of any country, territory, city or area or of its authorities, or concerning the delimitation of its frontiers or boundaries, or its economic system or degree of development. Designations such as “developed”, “industrialized” and “developing” are intended for statistical convenience and do not necessarily express a judgment about the stage reached by a particular country or area in the development process. Mention of firm names or commercial products does not constitute an endorsement by UNIDO. FAIR USE POLICY Any part of this publication may be quoted and referenced for educational and research purposes without additional permission from UNIDO. However, those who make use of quoting and referencing this publication are requested to follow the Fair Use Policy of giving due credit to UNIDO. CONTACT Please contact [email protected] for further information concerning UNIDO publications. For more information about UNIDO, please visit us at www.unido.org UNITED NATIONS INDUSTRIAL DEVELOPMENT ORGANIZATION Vienna International Centre, P.O. Box 300, 1400 Vienna, Austria Tel: (+43-1) 26026-0 · www.unido.org · [email protected] Board chairman: Hao Wang (professor) Reviewer: Yuhua Jiao (yrofessor) Compiler: Tongmei Hu, senior engineer Liquan %ang senior engineer Xi'an Kaisheng Building Materials Engineering Co. -
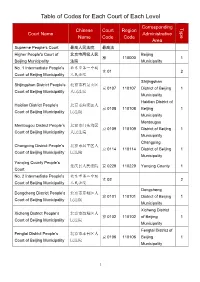
Table of Codes for Each Court of Each Level
Table of Codes for Each Court of Each Level Corresponding Type Chinese Court Region Court Name Administrative Name Code Code Area Supreme People’s Court 最高人民法院 最高法 Higher People's Court of 北京市高级人民 Beijing 京 110000 1 Beijing Municipality 法院 Municipality No. 1 Intermediate People's 北京市第一中级 京 01 2 Court of Beijing Municipality 人民法院 Shijingshan Shijingshan District People’s 北京市石景山区 京 0107 110107 District of Beijing 1 Court of Beijing Municipality 人民法院 Municipality Haidian District of Haidian District People’s 北京市海淀区人 京 0108 110108 Beijing 1 Court of Beijing Municipality 民法院 Municipality Mentougou Mentougou District People’s 北京市门头沟区 京 0109 110109 District of Beijing 1 Court of Beijing Municipality 人民法院 Municipality Changping Changping District People’s 北京市昌平区人 京 0114 110114 District of Beijing 1 Court of Beijing Municipality 民法院 Municipality Yanqing County People’s 延庆县人民法院 京 0229 110229 Yanqing County 1 Court No. 2 Intermediate People's 北京市第二中级 京 02 2 Court of Beijing Municipality 人民法院 Dongcheng Dongcheng District People’s 北京市东城区人 京 0101 110101 District of Beijing 1 Court of Beijing Municipality 民法院 Municipality Xicheng District Xicheng District People’s 北京市西城区人 京 0102 110102 of Beijing 1 Court of Beijing Municipality 民法院 Municipality Fengtai District of Fengtai District People’s 北京市丰台区人 京 0106 110106 Beijing 1 Court of Beijing Municipality 民法院 Municipality 1 Fangshan District Fangshan District People’s 北京市房山区人 京 0111 110111 of Beijing 1 Court of Beijing Municipality 民法院 Municipality Daxing District of Daxing District People’s 北京市大兴区人 京 0115 -

Analysis of Rural Women's Economic Participation in Shaanxi Province, China: Preliminary Results and Insights Mei Yang Allan R
Analysis of Rural Women’s Economic Participation in Shaanxi Province, China: Preliminary Results and Insights Mei Yang Allan Rae David Tripe Martin Young Huiyan Zhao School of Economics and Finance, Massey University ABSTRACT China has made significant progress in economic reform. This has entailed large scale migration and urbanization, but there is an accompanying problem of position of women in agricultural production in rural areas. To explore this, the study examines rural women’s barriers and potential in economic participation in Shaanxi province through a survey of 356 rural women including both those engaging in farming and off-farming activities from three regions of Shaanxi with different developing characteristics. We use a mixed research methodology with both qualitative and quantitative elements. Unlike a handful of previous relevant studies, the collection of primary data allows a more in depth and systematic analysis of the current situation of rural women and the barriers they are facing. Preliminary results indicate that the situation of rural women in China presents a range of characteristics due to political factors, geographical location, low education attainment, and their role as care-providers. The results presented here here is mainly concerning the part of rural women engaging in farming. 1. Introduction Over the last three decades, China’s industrialization and urbanization have been on an unprecedented scale(Bank, 2014): Around 250 million migrants have moved to cities from rural areas (NBSC, 2012) in supporting the country’s rapid economic growth which has averaged around 10% annually. Meanwhile, starting from 2000, the number of left-behind rural women1 or using a specific term in Chinese, Liushou women has increased sharply and it still increases each year. -

New Characteristics of Rural Women's Economic Participation in Shaanxi
ICE-BEES 2018 International Conference on Economics, Business and Economic Education 2018 Volume 2018 Conference Paper New Characteristics of Rural Women’s Economic Participation in Shaanxi, China Mei Yang1, Allan Rae2, and Martin Young3 1Northwest A&F University, China 2School of Economics and Finance, Massey University, New Zealand 3School of Economics and Finance, Massey University New Zealand Abstract China’s large scale migration, urbanization, accompanying its rural land circulation for modern agriculture, rural women’s economic situation was enormously affected but little noticed. To explore this, the study examines rural women’s challenges and potential in economic participation in Shaanxi province through a survey of 356 rural women in three areas of Shaanxi with different developing characteristics. The primary data allows a more in depth and systematic analysis of the current situation Corresponding Author: of rural women. Results indicate that the economic participation of rural women in Mei Yang [email protected] China presents some common and different challenges. Their own low educational attainment and their care-provider role are two common challenges. Meanwhile, Received: 7 August 2018 Accepted: 15 September 2018 their economic participation illustrates a geographical characteristic, which is largely Published: 22 October 2018 restricted by the land policy, regional economic development. Publishing services provided by Knowledge E Mei Yang et al. This article is 1. Introduction distributed under the terms of the Creative Commons Over the last three decades, China’s industrialization and urbanization have been on Attribution License, which permits unrestricted use and an unprecedented scale [3]. Tofight against its decaying and backward agricultural sit- redistribution provided that the uation and stimulate people’s enthusiasm in farming, Chinese government for decades original author and source are credited. -

Minimum Wage Standards in China August 11, 2020
Minimum Wage Standards in China August 11, 2020 Contents Heilongjiang ................................................................................................................................................. 3 Jilin ............................................................................................................................................................... 3 Liaoning ........................................................................................................................................................ 4 Inner Mongolia Autonomous Region ........................................................................................................... 7 Beijing......................................................................................................................................................... 10 Hebei ........................................................................................................................................................... 11 Henan .......................................................................................................................................................... 13 Shandong .................................................................................................................................................... 14 Shanxi ......................................................................................................................................................... 16 Shaanxi ...................................................................................................................................................... -

Download Article
Advances in Social Science, Education and Humanities Research, volume 310 3rd International Conference on Culture, Education and Economic Development of Modern Society (ICCESE 2019) Research on the Interactive Development of Industrial Clusters and Small (Cities) Towns with Characteristics in Western Regions Taking the Development of Traditional Chinese Medicine Industrial Clusters in Xianyang City of Shaanxi Province as an Example* Xiaoyuan Zhou College of Urban and Environmental Science Northwest University Xi'an, China 710127 School of Civil and Architectural Engineering Xi’an University of Science and Technology Xi'an, China 710058 Dan Zhao Yuan Lv Northwest University Xi’an University of Science and Technology Xi'an, China 710127 Xi'an, China 710058 Abstract—Through the analysis of the related notions of industrial clusters and the upgrading stage and process of I. INTRODUCTION industrial clusters, this paper analyses the interactive Small (cities) towns with characteristics are important development mechanism and influencing factors between linking points that link cities and townships, and are also the industrial clusters and small (cities) towns with characteristics. most dynamic "social cells" to promote urban and rural On the basis of the above, through the study of the basic profile, development [1]. In 2014, the proposal of characteristic small obtained achievements and existing problems of the development towns in Zhejiang Province gives an important inspiration to of traditional Chinese medicine industrial clusters in Xianyang City of Shaanxi Province, this paper puts forward the urban and rural development, that is, "the construction and developmental path of traditional Chinese medicine industrial landing of characteristic towns should be relied on the cluster in Xianyang City. -

United States Bankruptcy Court Northern District of Illinois Eastern Division
Case 12-27488 Doc 49 Filed 07/27/12 Entered 07/27/12 13:10:45 Desc Main Document Page 1 of 343 UNITED STATES BANKRUPTCY COURT NORTHERN DISTRICT OF ILLINOIS EASTERN DIVISION In re: ) Chapter 7 ) PEREGRINE FINANCIAL GROUP, INC., ) Case No. 12-27488 ) ) ) Honorable Judge Carol A. Doyle Debtor. ) ) Hearing Date: August 9, 2012 ) Hearing Time: 10:00 a.m. NOTICE OF MOTION TO: See Attached PLEASE TAKE NOTICE that on August 9, 2012 at 10:00 a.m., the undersigned shall appear before the Honorable Carol A. Doyle, United States Bankruptcy Judge for the United States Bankruptcy Court, Northern District of Illinois, Eastern Division, in Courtroom 742 of the Dirksen Federal Building, 219 South Dearborn Street, Chicago, Illinois 60604, and then and there present the TRUSTEE’S MOTION FOR ORDER APPROVING PROCEDURES FOR FIXING PRICING AND CLAIM AMOUNTS IN CONNECTION WITH THE TERMINATION AND LIQUIDATION OF FOREIGN EXCHANGE CUSTOMER AGREEMENTS (the “Motion”). PLEASE TAKE FURTHER NOTICE that if you are a foreign exchange customer of Peregrine Financial Group, Inc. or otherwise received this Notice, your rights may be affected by the Motion. PLEASE TAKE FURTHER NOTICE that a copy of the Motion is available on the Trustee’s website, www.PFGChapter7.com, or upon request sent to [email protected]. Respectfully submitted, Ira Bodenstein, not personally, but as chapter 7 trustee for the estate of Peregrine Financial Group, Inc. Dated: July 27, 2012 By: /s/ John Guzzardo One of his proposed attorneys Robert M. Fishman (#3124316) Salvatore Barbatano (#0109681) John Guzzardo (#6283016) Shaw Gussis Fishman Glantz {10403-001 NOM A0323583.DOC}4841-1459-7392.2 Case 12-27488 Doc 49 Filed 07/27/12 Entered 07/27/12 13:10:45 Desc Main Document Page 2 of 343 Wolfson & Towbin LLC 321 North Clark Street, Suite 800 Chicago, IL 60654 Phone: (877) 465-1849 [email protected] Proposed Counsel to the Trustee and Geoffrey S. -

Glutamine Protects Against Oxidative Stress Injury Through Inhibiting The
Zhao et al. Environmental Health and Preventive Medicine (2019) 24:4 Environmental Health and https://doi.org/10.1186/s12199-018-0757-5 Preventive Medicine RESEARCH ARTICLE Open Access Glutamine protects against oxidative stress injury through inhibiting the activation of PI3K/Akt signaling pathway in parkinsonian cell model Yingqian Zhao1,2, Qiang Wang3,4, Yuan Wang3,4, Jie Li3,4, Gang Lu3,4 and Zhibin Liu3,4* Abstract Background: Parkinson’s disease is a neurodegenerative disorder, and recent studies suggested that oxidative stress contributes to the degeneration of dopamine cell in Parkinson’s disease. Glutamine also has a positive role in reducing oxidative stress damage. In this study, we hypothesized that glutamine offers protection against oxidative stress injury in 1-methyl-4-phenylpyridinium (MPP+)-induced Parkinson’s disease cell model. Methods: MPP+ was used to induce PD models in PC12 cells and classified into control, M0 (MPP+), G0 (glutamine), and M0+G0 groups. CCK-8 and AO/EB staining assays were used to examine cell proliferation and apoptosis, respectively. Western blotting was applied to examine the protein expression of PI3K, P-Akt, Akt, P-mTOR, and mTOR. Results: We showed that glutamine suppressed cytotoxicity induced by MPP+ in PC12 cells. MPP+ decreased the superoxide dismutase and glutathione peroxidase activity and increased the malondialdehyde content, which were restored by glutamine. Moreover, MPP+ increased the expression of PI3K, P-Akt, Akt, P-mTOR, and mTOR, which were inhibited by glutamine. And the antioxidant capacity of glutamine on PC12 cells could be improved by LY294002 and inhibited by IGF-1. Conclusion: These results suggest that glutamine strengthens the antioxidant capacity in PC12 cells induced by MPP+ through inhibiting the activation of the PI3K/Akt signaling pathway. -
Chinese Mainland
Address List of Special Warehousing Service Note: The address marked in red are newly added address. (Effective date:October 1, 2021) Province / Directly- controlled City District/county Town, Sub-district and House Number Municipality / Autonomous Region/SAR B4-25, Gate 1, ProLogis Logistics Park, No.1 Tiedi Road, Anhui Province Hefei Shushan District High-tech Zone No.18 Tianzhushan Road, Longshan Sub-district, Wuhu Anhui Province Wuhu Jiujiang District Economic and Technological Development Zone Anhui Province Chuzhou Langya District Longji Leye Photovoltaic Co., Ltd., No.19 Huai'an Road 3/F, No.8 Building, South Area, Lixiang Innovation Park, Anhui Province Chuzhou Nanqiao District Chuzhou, 018 Township Road Anhui Province Chuzhou Nanqiao District No.19 Huai'an Road Yuanrong New Material Holding Co., Ltd., 50 Meters Anhui Province Hefei Shushan District Westward of Bridge of Intersection of Changning Avenue and Ningxi Road Anhui Province Hefei Yaohai District No.88 Dayu Road Anhui Province Hefei Yaohai District No.2177 Dongfang Avenue Beijing BOE Vision-Electronic Technology Co., Ltd., No. Anhui Province Hefei Yaohai District 2177 Dongfang Avenue Anhui Province Hefei Yaohai District No.668 Longzihu Road Anhui Province Hefei Yaohai District No. 668 Longzihu Road Anhui Province Hefei Yaohai District No.2177 Tongling North Road Anhui Province Hefei Yaohai District No.3166 Tongling North Road Anhui Province Hefei Yaohai District No.8 Xiangwang Road Anhui Province Wuhu Jiujiang District No. 8 Anshan Road Anhui Province Wuhu Jiujiang District -

Analysis of the Structure and Management of Nosocomial Infection in Traditional Chinese Medicine Hospital in Shaanxi Province
2019 3rd International Conference on Informatization in Education, Management and Business (IEMB 2019) Analysis of the Structure and Management of Nosocomial Infection in Traditional Chinese Medicine Hospital in Shaanxi Province Zhigang Zhang1, a, Qiuxia Wei2, b, Mei Han3, c, Juwei Wang4, d, Zhipei Yang2, e, Xiaoya Liang2, f 1School of Public Health, Shaanxi University of Chinese Medicine, Shiji Ave., Xi'an-Xianyang New Ecomic Zone, Xi’an, Shaanxi, China 2Infection Management Section, Affiliated Hospital of Shaanxi University of Chinese Medicine, Weiyang West Road, Qindu District, Xianyang, Shaanxi, China 3Department of Information and Statistic, Qingdao Women and Children Hospital, Tongfu Road, Shibei District, Qingdao, Shandong, China 4Infection Management Section, Xianyang Rainbow Hospital, Weiyang West Road, Qindu District, Xianyang, Shaanxi, China [email protected], [email protected], [email protected], [email protected], [email protected] m, [email protected] Keywords: Traditional Chinese Medicine Hospital, Nosocomial infection, Management, Current situation Abstract: The infection monitoring and management systems in TCM hospitals in Shaanxi Province were found to be relatively adequate and the operation of the infection management agencies has been essentially established. Out of the 41 TCM hospitals, 39 were practically investigated. 74.36% of the TCM hospitals had established a separate nosocomial infection management department. The competent managers of the departments were in most cases the hospital deans or sub-deans (92.31%). Thirty-eight out of thirty-nine TCM hospitals had set up hospital infection management committees, and the members of these committees were meeting mostly two times a year (66.67%). Twelve assessments were executed in a year, accounting for the 43.59% of the TCM hospitals, while 5.13% performed no assessments. -

Minimum Wage Standards in China June 28, 2018
Minimum Wage Standards in China June 28, 2018 Contents Heilongjiang .................................................................................................................................................. 3 Jilin ................................................................................................................................................................ 3 Liaoning ........................................................................................................................................................ 4 Inner Mongolia Autonomous Region ........................................................................................................... 7 Beijing ......................................................................................................................................................... 10 Hebei ........................................................................................................................................................... 11 Henan .......................................................................................................................................................... 13 Shandong .................................................................................................................................................... 14 Shanxi ......................................................................................................................................................... 16 Shaanxi ....................................................................................................................................................... -

Annual Development Report on China's Trademark Strategy 2013
Annual Development Report on China's Trademark Strategy 2013 TRADEMARK OFFICE/TRADEMARK REVIEW AND ADJUDICATION BOARD OF STATE ADMINISTRATION FOR INDUSTRY AND COMMERCE PEOPLE’S REPUBLIC OF CHINA China Industry & Commerce Press Preface Preface 2013 was a crucial year for comprehensively implementing the conclusions of the 18th CPC National Congress and the second & third plenary session of the 18th CPC Central Committee. Facing the new situation and task of thoroughly reforming and duty transformation, as well as the opportunities and challenges brought by the revised Trademark Law, Trademark staff in AICs at all levels followed the arrangement of SAIC and got new achievements by carrying out trademark strategy and taking innovation on trademark practice, theory and mechanism. ——Trademark examination and review achieved great progress. In 2013, trademark applications increased to 1.8815 million, with a year-on-year growth of 14.15%, reaching a new record in the history and keeping the highest a mount of the world for consecutive 12 years. Under the pressure of trademark examination, Trademark Office and TRAB of SAIC faced the difficuties positively, and made great efforts on soloving problems. Trademark Office and TRAB of SAIC optimized the examination procedure, properly allocated examiners, implemented the mechanism of performance incentive, and carried out the “double-points” management. As a result, the Office examined 1.4246 million trademark applications, 16.09% more than last year. The examination period was maintained within 10 months, and opposition period was shortened to 12 months, which laid a firm foundation for performing the statutory time limit. —— Implementing trademark strategy with a shift to effective use and protection of trademark by law.