Symptomatic Os Subtibiale Associated with Chronic Pain Around the Medial Malleolus in a Young Athlete Alexandar A
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Ideal Medial Malleolar Screw Length Based on the Tibial Epiphyseal Scar Location in Weight Bearing CT’S Collin G
Ideal Medial Malleolar Screw Length Based on the Tibial Epiphyseal Scar Location in Weight Bearing CT’s Collin G. Messerly DPM, Keegan A. Duelfer DPM, Troy J. Boffeli DPM, FACFAS, Tyler K. Sorensen, DPM Regions Hospital / HealthPartners Institute for Education and Research - Saint Paul, MN Figure 1. Zone of Dense Bone in Medial Malleolar ORIF Figure 4. Measuring Distal – Most 5% to Medial Malleolus Table 2. Distance Between Epiphyseal Scar & Distal – Most 5% of RESULTS STATEMENT OF PURPOSE The epiphyseal scar is located in the distal The medial malleolus to distal – most 5% mark Tibia 97 WB ankle CT scans evaluated in uninjured ankles Medial malleolar fractures are one of the most common fracture types metaphysis of the tibia, and can oftentimes be was measured on the coronal WB CT slice with Measurement of interest Male: Mean ± SD Female: Mean ± SD (mm) In males < 60 years old there was a 12.75 mm zone of increased bone the widest medial malleolus. Screw threads observed in the ankle joint and have been long fixated with two screws; easily visualized on X-ray and CT scan (red line). (mm) density, as compared to 13.66 mm in those ≥ 60 which was not statistically The distal – most 5% of the tibia (distal to the beyond this point will purchase less dense bone however, the bone density of the distal tibia has potential for poor screw significant. purchase due to compromised bone density. This is especially true in elderly black line) contains dense bone with marked in the medullary canal with potential to not have Epiphyseal Scar to Medial Malleolus 12.75 ± 2.91 9.39 ± 2.38 In females < 60 years old there was 9.39 mm zone of increased bone populations with osteoporotic bone. -

Assessment, Management and Decision Making in the Treatment Of
Pediatric Ankle Fractures Anthony I. Riccio, MD Texas Scottish Rite Hospital for Children Update 07/2016 Pediatric Ankle Fractures The Ankle is the 2nd most Common Site of Physeal Injury in Children 10-25% of all Physeal Injuries Occur About the Ankle Pediatric Ankle Fractures Primary Concerns Are: • Anatomic Restoration of Articular Surface • Restoration of Symmetric Ankle Mortise • Preservation of Physeal Growth • Minimize Iatrogenic Physeal Injury • Avoid Fixation Across Physis in Younger Children Salter Harris Classification Prognosis and Treatment of Pediatric Ankle Fractures is Often Dictated by the Salter Harris Classification of Physeal Fractures Type I and II Fractures: Often Amenable to Closed Tx / Lower Risk of Physeal Arrest Type III and IV: More Likely to Require Operative Tx / Higher Risk of Physeal Arrest Herring JA, ed. Tachdjian’s Pediatric Orthopaedics, 5th Ed. 2014. Elsevier. Philadelphia, PA. ISOLATED DISTAL FIBULA FRACTURES Distal Fibula Fractures • The Physis is Weaker than the Lateral Ankle Ligaments – Children Often Fracture the Distal Fibula but…. – …ligamentous Injuries are Not Uncommon • Mechanism of Injury = Inversion of a Supinated Foot • SH I and II Fractures are Most Common – SH I Fractures: Average Age = 10 Years – SH II Fractures: Average Age = 12 Years Distal Fibula Fractures Lateral Ankle Tenderness SH I Distal Fibula Fracture vs. Lateral Ligamentous Injury (Sprain) Distal Fibula Fractures • Sankar et al (JPO 2008) – 37 Children – All with Open Physes, Lateral Ankle Tenderness + Normal Films – 18%: Periosteal -

Back of Leg I
Back of Leg I Dr. Garima Sehgal Associate Professor “Only those who risk going too far, can possibly find King George’s Medical University out how far one can go.” UP, Lucknow — T.S. Elliot DISCLAIMER Presentation has been made only for educational purpose Images and data used in the presentation have been taken from various textbooks and other online resources Author of the presentation claims no ownership for this material Learning Objectives By the end of this teaching session on Back of leg – I all the MBBS 1st year students must be able to: • Enumerate the contents of superficial fascia of back of leg • Write a short note on small saphenous vein • Describe cutaneous innervation in the back of leg • Write a short note on sural nerve • Enumerate the boundaries of posterior compartment of leg • Enumerate the fascial compartments in back of leg & their contents • Write a short note on flexor retinaculum of leg- its attachments & structures passing underneath • Describe the origin, insertion nerve supply and actions of superficial muscles of the posterior compartment of leg Introduction- Back of Leg / Calf • Powerful superficial antigravity muscles • (gastrocnemius, soleus) • Muscles are large in size • Inserted into the heel • Raise the heel during walking Superficial fascia of Back of leg • Contains superficial veins- • small saphenous vein with its tributaries • part of course of great saphenous vein • Cutaneous nerves in the back of leg- 1. Saphenous nerve 2. Posterior division of medial cutaneous nerve of thigh 3. Posterior cutaneous -

Anatomy of the Foot and Ankle
Anatomy Of The Foot And Ankle Multimedia Health Education Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic Health. All decisions about management of the Foot and Ankle must be made in conjunction with your Physician or a licensed healthcare provider. Anatomy Of The Foot And Ankle Multimedia Health Education MULTIMEDIA HEALTH EDUCATION MANUAL TABLE OF CONTENTS SECTION CONTENT 1 . ANATOMY a. Ankle & Foot Anatomy b. Soft Tissue Anatomy 2 . BIOMECHANICS Anatomy Of The Foot And Ankle Multimedia Health Education Unit 1: Anatomy Introduction The foot and ankle in the human body work together to provide balance, stability, movement, and Propulsion. This complex anatomy consists of: 26 bones 33 joints Muscles Tendons Ligaments Blood vessels, nerves, and soft tissue In order to understand conditions that affect the foot and ankle, it is important to understand the normal anatomy of the foot and ankle. Ankle The ankle consists of three bones attached by muscles, tendons, and ligaments that connect the foot to the leg. In the lower leg are two bones called the tibia (shin bone) and the fibula. These bones articulate (connect) to the Talus or ankle bone at the tibiotalar joint (ankle joint) allowing the foot to move up and down. The bony protrusions that we can see and feel on the ankle are: Lateral Malleolus: this is the outer ankle bone formed by the distal end of the fibula. Medial Malleolus: this is the inner ankle bone formed by the distal end of the tibia. Tibia (shin bone) (Refer fig.1) Tibia -
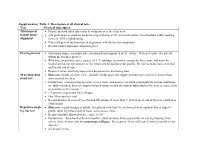
Supplementary Table 1: Description of All Clinical Tests Test Protocol
Supplementary Table 1: Description of all clinical tests Test Protocol description Tibiofemoral • Palpate & mark tibial tuberosity & midpoint over the talus neck frontal plane • Ask participant to stand on footprint map with foot at 10° external rotation, feet shoulder width, looking alignment forward, 50% weightbearing • Place callipers of inclinometer in alignment with the the two landmarks • Record varus/valgus direction in degrees Herrington test • Participant supine on plinth, knee positioned and supported in 20° of knee flexion (to place the patella within the trochlea groove) • With knee in position, place a piece of 1” Leukotape (or similar) across the knee joint, and mark the medial and lateral epicondyles of the femur and mid-point of the patella. Be sure to make note of medial and lateral end of tape • Repeat 3 times, attaching tape to this document for measuring later 30 second chair • Shoes on, middle of chair, feet ~ shoulder width apart and slightly behind knees with feet flat on floor, stand test arms crossed on chest • Instructions “stand up keeping arms across chest, and ensure you stand completely up so hips and knees are fully extended; then sit completely back down, so that the bottom fully touches the seat, as many times as possible in 30 seconds,” • 1-2 practice repetitions for technique • One 30-second test trial • Record number of correctly performed full stands (if more than ½ of way up at end of the test, counted as a full stand) Repetitive single • Shoes on, seated on edge of plinth, foot placed with heel 10 cm forward from a plumb line at edge of leg rise test plinth, other leg held at side of body, arms across chest. -

Management of Intra-Articular Fractures of the Calcaneus: Introducing a New Locking Plate
Shafa Ortho J. 2018 November; 5(4):e7991. doi: 10.5812/soj.7991. Published online 2018 October 9. Letter Management of Intra-Articular Fractures of the Calcaneus: Introducing a New Locking Plate Bijan Valiollahi 1, * and Mostafa Salariyeh 1 1Bone and Joint Reconstruction Research Center, Shafa Orthopedic Hospital, Iran University of Medical Sciences, Tehran, Iran *Corresponding author: Bone and Joint Reconstruction Research Center, Shafa Orthopedic Hospital, Iran University of Medical Sciences, Tehran, Iran. Email: [email protected] Received 2016 October 31; Revised 2018 September 22; Accepted 2018 September 27. Keywords: Calcaneus Fracture, New Plate, Sinus Tarsal Approach Dear Editor, displaced intra-articular fractures involving the posterior Fracture of the calcaneus is usually a challenging prob- facet and is ideally performed within three weeks of in- lem for orthopedic surgeons and patients. Calcaneal frac- jury. Beyond this time, separation of the fragments be- tures are the most common of tarsal bone fractures, and comes more challenging. To achieve an adequate reduc- most of them are displaced intra-articular (nearly 75%) frac- tion, surgery must be performed after soft tissue swelling tures, usually resulting from falling or motor vehicle acci- diminishes (2). dents (1). Full diminishing of soft tissue edema is demonstrated Most patients with calcaneal fractures are usually by a positive wrinkle test, indicating that surgical interven- young men in their prime working years, which results in tion may be performed safely. For the extensile lateral ap- a significant loss of economic productivity. Although sur- proach, a good skin with positive wrinkle test is needed. gical techniques and fixation implants have generally im- Concerns about high wound complication rates in the ex- proved functional outcomes, there is vast controversy as to tensile lateral approach have prompted some to improve the management of these highly complex injuries. -
Bones of the Lower Limb Doctors Notes Notes/Extra Explanation Editing File Objectives
Color Code Important Bones of the Lower Limb Doctors Notes Notes/Extra explanation Editing File Objectives Classify the bones of the three regions of the lower limb (thigh, leg and foot). Memorize the main features of the – Bones of the thigh (femur & patella) – Bones of the leg (tibia & Fibula) – Bones of the foot (tarsals, metatarsals and phalanges) Recognize the side of the bone. ﻻ تنصدمون من عدد ال رشائح نصها رشح زائد وملخصات واسئلة Some pictures in the original slides have been replaced with other pictures which are more clear BUT they have the same information and labels. Terminology (Team 434) شيء مرتفع /Eminence a small projection or bump Terminology (Team 434) Bones of thigh (Femur and Patella) Femur o Articulates (joins): (1) above with Acetabulum of hip bone to form the hip joint, (2) below with tibia and patella to form the knee joint. Body of femur (shaft) o Femur consists of: I. Upper end. II. Shaft. III. Lower end. Note: All long bones consist of three things: 1- upper/proximal end posterior 2- shaft anterior 3- lower/distal end I. Upper End of Femur The upper end contains: A. Head B. Neck C. Greater trochanter & D. Lesser trochanter A. Head: o Articulates (joins) with acetabulum of hip bone to form the hip joint. o Has a depression in the center called Fovea Capitis. o The fovea capitis is for the attachment of ligament of the head of Femur. o An artery called Obturator Artery passes along this ligament to supply head of Femur. B. Neck: o Connects head to the shaft. -

Foot and Ankle Injuries
Foot and Ankle Injuries Today’s lecture can be viewed at Learning in Athletics the following URL address: We most likely will not get “All of life should be a through all these slides today, learning experience, not Thomas W. Kaminski, PhD, ATC, http://sites.udel.edu/chshowever the presentation- atep/lectures/is just for the trivial FNATA, FACSM, RFSA thorough and complete and will reasons but because by Professor make for an excellent study continuing the learning Director of Athletic Training Education guide for the BOC process, we are challenging our brain University of Delaware examination! Good Luck! and therefore building brain circuitry” Arnold Scheibel Athletic Training & Sports Laboratory Manual UD is located here! A First State to accompany Fact! Health Care: The Journal for the Rehabilitation Techniques in Sports Medicine Delaware is 96 miles Practicing Clinician and Athletic Training long and varies from th 9 to 35 miles in 6 Edition width. http://www.healio.com /journals/atshc https://www.healio.com/books/athletic- training/%7b927168ac-1da2-422c-b98e- ae9013d4e15b%7d/rehabilitation-techniques-for- sports-medicine-and-athletic-training-sixth-edition Perhaps ATC’s Need to Incorporate Lower Extremity ~ Foot this Into Their Assessment Scheme? Anatomical Review Cyriax- “Diagnosis is only a matter of applying one’s anatomy” 1 Clinical PEARL: Lower Extremity ~ Foot Navicular Palpation Lower Extremity ~ Foot • Palpated 2-3 cm anteroinferior to the medial malleolus • More prominent with foot adducted Radiographically Viewed The Ankle Mortise Articulations Ankle Joint (Medial View) 1. Fibula 2. Tibia 3. Ankle jointChallenge 4. Promontoryyourself of tibia to 5. Trochlear surface of talus 6. -

EZ-IO PD Distal Tibial Access
® EZ-IO PD Distal Tibial Access ® Training Program The EZ-IO PD® was developed as a direct result of the need to improve intraosseous access in patients of smaller size. The images and training that follow were designed to simplify IO understanding and improve emergency vascular access. Our collective goal has long been Immediate, Safe and Effective vascular access for all critical patients. Vidacare’s approach to this goal is simple - the right equipment - in the best hands - where it’s needed most. At the completion of this program if you still have questions or concerns please call us at 1.866.479.8500 or visit our web site at www.vidacare.com. We at Vidacare® appreciate what you do and the time you devote to it. Thank you for inviting us to be a member of your team! 1 Indications for EZ-IO PD Access ¾ Altered level of consciousness ¾ Respiratory compromise ¾ Hemodynamic instability To gain immediate vascular access in an emergency FOR PATIENTS WEIGHTING BETWEEN 3 – 39 KILOGRAMS Listed here are the primary indications. Can you think of specific conditions that would fit each indications? Examples of disease states often meeting these criteria include, but are not limited to the following: Cardiac arrest, Status epilepticus, All shock states, Arrythmias, Dehydration Burns, Drug Overdose, DKA (diabetic), Renal failure, Stroke, AMI, Coma, OB complications, Thyroid crisis, Trauma, Anaphylaxis, CHF, Emphysema, Respiratory arrest, Hemophiliac crisis 2 Contraindications for EZ-IO PD Access ¾ Fracture (targeted bone) ¾ Previous orthopedic procedures near insertion site (IO within past 24 hours/Prosthetic Limb or joint) ¾ Infection at the insertion site ¾ Inability to locate landmarks or excessive tissue These are the contraindications. -

Anthropometric Studies of the Human Foot and Ankle "
ANTHROPOMETRIC STUDIES OF THE HUMAN FOOT AND ANKLE " R. E. Isman V. T. Inman, M .D., Ph.D." Biomechanics Laboratory University of California San Francisco Medical Center San Francisco, Calif. 94122 ABSTRACT A study of the talocrural (ankle) and talocalcaneal (subtalar) joints was made in order to acquire as much information as possible on the exact locations of their axes of rotation . The material used was 46 ca- daver legs which had the ligamentous and capsular structures intact. The study was limited to only one of the factors that influence joint motion: the shapes of the articulating surfaces. With a specially designed apparatus, the two axes were determined in each specimen. Then a series of measurements was made of the angles between these two axes and between these axes and various lines of ref- erence in the shank and foot . Measurements were also made to deter- mine the location of the axis of the talocrural joint with respect to ana- tomic landmarks on the leg. Finally, the perpendicular distance between the two joint axes was measured, and, in an attempt to determine the location of the axis of the talocalcaneal joint by means of anatomic landmarks, a ratio was calculated between two segments of a line as- sumed to extend from the most lateral point of the lateral malleolus to the most medial point of the medial malleolus. a This study was supported by Easter Seal Research Foundation Grant N-6618 . The apparatus for determination of the joint axes was designed and built under the sponsorship of Veterans Administration Contract V1005M-2075. -

Diagnosis and Treatment of Ankle Fractures
CE .................................................................................................. DIRECTED READING Diagnosis and Treatment Of Ankle Fractures ANNE M SCOTT, BSRS, R.T.(R) Ankle fractures are common After reading this article, readers should be able to: among all populations, ■ Review ankle joint anatomy and the role of ligament structures in providing stability. ■ although incidence increases Describe the role of imaging in patient diagnosis, treatment planning and follow-up. ■ in the elderly. They are most Discuss classification systems for ankle injury patterns. ■ often the result of simple falls Determine when surgical reduction and internal fixation of ankle fractures is required and complications that may result from surgery. and athletic injuries but also ■ may be caused by underlying Describe rehabilitation techniques and functional recovery prognosis. pathology. A thorough patient evaluation with description of njuries to the ankle are common used to evaluate these injuries may the mechanism of injury is key in the general population and in include conventional radiography, mag- to proper diagnosis. 1,2 athletes. It is estimated that netic resonance (MR) imaging, comput- 260 000 Americans sustain an ed tomography (CT), radionuclide bone This article examines the ankle fracture each year and scanning and ultrasonography. use of radiography and I that ankle fractures occur in about 100 Stable fractures are effectively treat- other imaging modalities in per 100 000 people in major cities.3,4 ed with casts and removable braces.9 diagnosing ankle injuries, as They constitute 21% of all sports-relat- Unstable fractures must be reduced well as several classification ed injuries.1 One study reported that promptly and accurately to optimize systems available to describe the incidence of ankle fractures has healing and minimize the length of the pattern of injury and increased in recent decades, especially hospital stay.4 When surgery is required, aid in treatment planning. -

Leg and Foot
Dr. Sangeeta Kotrannavar Assistant Professor Dept. of Anatomy USM-KLE IMP, Belagavi Describe the bony landmarks of tibia and fibula Describe the osteology of tibia, fibula, tarsals, metatarsals and phalanges State the anterior, posterior and lateral compartments of the leg Describe the attachments, actions and innervations of the muscles in each compartment Describe the blood supply and nerve supply in each compartment Describe the tarsal tunnel and its contents State the four layers of muscles in the sole of the foot Describe the blood supply and innervation of the sole of the foot Explain the arches of the foot and its significant Describe the applied anatomy of the foot Leg is between the knee and ankle joint – bones tibia & fibula Foot is distal to the ankle joint Lat. Medial Tibia is large, weight-bearing shin bone Medially placed, Long bone Equivalent to radius Parts Upper end, Lower end, Shaft • Upper end - med. & Lat. Condyles, intercondylar area (non articular), tibial tuberosity • Condyles articulates with condyles of femur. • Intercondylar area—attachment fro before backwards: Ant. Horn of med. Miniscus, ant. Cruciate lig., ant. Horn of lat. Miniscus. post. Horn of lat. Miniscus, post. Horn of med. Miniscus, post. Cruciate lig. • Med. Condyle - post - semimembranosus. Ant. - sartorius, gracilus, semitendinosus. • Tibial tuberosity - ligamentum patellae. • Lower end - medial malleolus – tip - deltoid lig. • Shaft - triangular. Borders - ant., med., lat • Shaft - Surfaces - anteromedial (subcutaneous), anterolat.