Isolated Ectopia Lentis
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Megalocornea Jeffrey Welder and Thomas a Oetting, MS, MD September 18, 2010
Megalocornea Jeffrey Welder and Thomas A Oetting, MS, MD September 18, 2010 Chief Complaint: Visual disturbance when changing positions. History of Present Illness: A 60-year-old man with a history of simple megalocornea presented to the Iowa City Veterans Administration Healthcare System eye clinic reporting visual disturbance while changing head position for several months. He noticed that his vision worsened with his head bent down. He previously had cataract surgery with an iris-sutured IOL due to the large size of his eye, which did not allow for placement of an anterior chamber intraocular lens (ACIOL) or scleral-fixated lens. Past Medical History: Megalocornea Medications: None Family History: No known history of megalocornea Social History: None contributory Ocular Exam: • Visual Acuity (with correction): • OD 20/100 (cause unknown) • OS 20/20 (with upright head position) • IOP: 18mmHg OD, 17mmHg OS • External Exam: normal OU • Pupils: No anisocoria and no relative afferent pupillary defect • Motility: Full OU. • Slit lamp exam: megalocornea (>13 mm in diameter) and with anterior mosaic dystrophy. Iris-sutured posterior chamber IOLs (PCIOLs), stable OD, but pseudophacodonesis OS with loose inferior suture evident. • Dilated funduscopic exam: Normal OU Clinical Course: The patient’s iris-sutured IOL had become loose (tilted and de-centered) in his large anterior chamber, despite several sutures that had been placed in the past, resulting now in visual disturbance with movement. FDA and IRB approval was obtained to place an Artisan iris-clip IOL (Ophtec®). He was taken to the OR where his existing IOL was removed using Duet forceps and scissors. The Artisan IOL was placed using enclavation iris forceps. -

Insertion of Aqueous Shunt in Pedicatric Glaucoma
1/29/2018 Challenges of Insertion of Aqueous shunt in paediatric glaucoma Ahmed Elkarmouty MD, FRCS Moorfields Eye Hospital London, UK Classification • Primary Childhood Glaucoma • A- Primary Congenital Glaucoma (PCG) 1: 10,000–18,000 • B- Juvenile Open Angle Glaucoma (JOAG) (5-35 ys,)1 : 50,000. • Secondary Childhood Glaucoma • A- Glaucoma associated with non-acquired ocular anomalies • B- Glaucoma associated with non- acquired systemic disease or syndrome • C- Glaucoma associated with acquired condition • D- Glaucoma following Cataract surgery 1 1/29/2018 Glaucoma associated with non- acquired ocular anomalies • Conditions with predominantly ocular anomalies present at birth which may or may not be associated with systemic signs • Axenfeld Reiger anomaly • Peters anomaly • Ectropion Uvae • Congenital iris hypolplasia • Aniridia • Oculodermal melanocytosis • Posterior polymorphous dystrophy • Microphthalmos • Microcornea • Ectopia Lentis ( et pupillae) • Persistent foetus vasculopathy Glaucoma associated with non- acquired systemic disease or syndrome predominantly associated with known syndrome, systemic anomalies present at birth which may be associated with ocular signs • Down Syndrome • Connective tissue disorder: Marfan syndrome, Weill- Marchesiani syndrome, Stickler syndrome • Metabolic disorder : Homocystenuria, lowe syndrome, Mucoploysacchroidoses • Phacomatoses: Neurofibromatoses, Sturge Weber, Klipple-Trenaunay- weber syndrome, Rubenstein Taybi • Congenital Rubella 2 1/29/2018 Glaucoma associated with acquired condition Conditions -

Eleventh Edition
SUPPLEMENT TO April 15, 2009 A JOBSON PUBLICATION www.revoptom.com Eleventh Edition Joseph W. Sowka, O.D., FAAO, Dipl. Andrew S. Gurwood, O.D., FAAO, Dipl. Alan G. Kabat, O.D., FAAO Supported by an unrestricted grant from Alcon, Inc. 001_ro0409_handbook 4/2/09 9:42 AM Page 4 TABLE OF CONTENTS Eyelids & Adnexa Conjunctiva & Sclera Cornea Uvea & Glaucoma Viitreous & Retiina Neuro-Ophthalmic Disease Oculosystemic Disease EYELIDS & ADNEXA VITREOUS & RETINA Blow-Out Fracture................................................ 6 Asteroid Hyalosis ................................................33 Acquired Ptosis ................................................... 7 Retinal Arterial Macroaneurysm............................34 Acquired Entropion ............................................. 9 Retinal Emboli.....................................................36 Verruca & Papilloma............................................11 Hypertensive Retinopathy.....................................37 Idiopathic Juxtafoveal Retinal Telangiectasia...........39 CONJUNCTIVA & SCLERA Ocular Ischemic Syndrome...................................40 Scleral Melt ........................................................13 Retinal Artery Occlusion ......................................42 Giant Papillary Conjunctivitis................................14 Conjunctival Lymphoma .......................................15 NEURO-OPHTHALMIC DISEASE Blue Sclera .........................................................17 Dorsal Midbrain Syndrome ..................................45 -

Abnormalities Affecting the Eye As a Whole 2 8 Congenital Corneal
I Editors vi Contributors vii , About the Series viii Preface ix ) Acknowledgments x -t -t Abnormalities Affecting the Eye as a Whole 2 Judith B. Lavrich Anophthalmia 2 Microphthalmia 8 Nanophthaha 12 Typical Coloboma 14 8 Congenital Corneal Opacity 18 Bruce SchnalI and Michael J. Bartiss Sderocornea 18 Birth Trauma: Tears in Descemet's Membrane 20 Ulcer or Lnfection 22 Mucopolysaccharidosis 24 Peters' Anomaly 26 Congenital Hereditary Endothelial Dystrophy 28 Corneal Dermoid 30 Anterior Staphyloma 32 Wilson's Disease (HepatolenticularDegeneration) 34 Herpes Simplex Infection 36 Herpes Simplex Virus Epithelial Dendrite or Ulceration 38 Herpes SimplexVirus Corneal Stromal Disease 40 Herpes Zoster Ophthalmicus 42 Chickenpox 44 Limbal Vernal Keratoconjunctivitis 46 C-3 Glaucoma 48 A& Levin and Anya A. Trumler Primary Congenital or Infantile Glaucoma 48 Juvenile Open-Angle Glaucoma 52 Aphakic Glaucoma 55 Uveitic Glaucoma 58 Sturge-WeberSyndrome 62 m xii CONTENTS Congenital Ectropion Uveae 65 Aniridia 68 Posterior Embryotoxon 70 C- C- 4 Iris Anomalies 72 Michael J.Bartiss and BruceM. Schall Central Pupillary Cysts (Pupillary Margin Epithelial Cysts) 72 Aniridia 74 BrusbJield Spots 76 Ectopia Lentis et Pupillae 78 Heterochromia Iridis 80 Iris Coloboma 82 Iris Stromal Cysts 84 Juvenile Xanthogranuloma 86 Lisch Nodules 88 Melanosis Oculi (Ocular Melanocytosis) 90 Persistent Pupillary Membrane 92 Posterior Synechiae 94 Axenfeld-Rieger Anomaly 96 -5 Lens Anomalies 98 Jonathan H. Salvin and Hillary Gordon Congenital and Developmental Cataracts 98 Ectopia Lentis 102 Anterior Lenticonus 104 Posterior Lenticonus 106 Spherophakia 108 C- 6 Retinal Anomalies 110 Barry N. Wasserman,Anuradha Ganesh, Alex V Levin, Carol L. Shields, Jerry A. Shields, and Alok S. -

An Operation for Congenital Ptosis by George Young
Br J Ophthalmol: first published as 10.1136/bjo.8.6.272 on 1 June 1924. Downloaded from 272 THE BRITISH JOURNAL OF OPHTHALMIOI,OGY added plus lenses (eye being under atropin), J.2, fluently. This made her left eye equal, for distance, to her better eye, which is now getting worse owing to increased bulging, and will probably follow the course of the other one soon. R.V.: 6/36, c. -1.OD sph. + 3.50D cyl. 1550: 6/24 and J.5. Furthermore, it may be noted that the intraocular tension was now normal on the side of the iridectomy, while the right eye was hard, and I submitted it again to pilocarpin and bandage at night. I sent her home for a fortnight to feed up, take malt and cod liver oil and fats, and to take plenty of rest and recuperate. On July 8 the final result was: L.V.: 6/36, c.-5.OD sph. +3.50D cyl. 1600: 6/12 full, and -3.OD sph. and +3.50D cyl. J.2. Soon I shall tattoo the stellate leucoma with an artificial pupil. May 10, 1924. Since writing the above, some ten months ago, affairs have kept steady. There is no bulging of the left cornea or scar. I attempted tattooing at two sittings, and have considerably diminished the glare of the scar, but I refrain from risking the deep tattooing necessary for securing an imitation round black pupil, fearing to do harm. Glasses were prescribed and worn with comfort and great help, the vision being maintained as above. -
Retinitis Pigmentosa Associated with Ectopia Lentis
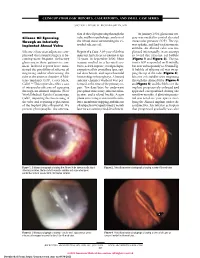
CLINICOPATHOLOGIC REPORTS, CASE REPORTS, AND SMALL CASE SERIES SECTION EDITOR: W. RICHARD GREEN, MD tion of the oil progressing through the In January 2001, glaucoma sur- Silicone Oil Egressing tube and histopathologic analysis of gery was needed to control elevated Through an Inferiorly the orbital tissue surrounding the ex- intraocular pressure (IOP). The eye Implanted Ahmed Valve truded silicone oil. was aphakic and had total traumatic aniridia. An Ahmed valve was im- Silicone oil use as an adjunct to com- Report of a Case. A 69-year-old white planted inferonasally in an attempt plicated vitreoretinal surgery is be- man lost his left eye to trauma at age to avoid the silicone oil bubble coming more frequent. Refractory 12 years. In September 2000, blunt (Figure 1 and Figure 2). The pa- glaucoma in these patients is com- trauma resulted in a lacerated eye- tient’s IOP responded well initially mon. Isolated reports have men- brow, scleral rupture, uveal prolapse, but rose subsequently to 30 mm Hg. tioned the possibility of silicone oil extrusion of his crystalline lens, reti- A bubble of silicone oil was wrap- migrating and/or obstructing the nal detachment, and suprachoroidal ping the tip of the tube (Figure 3). tube in the anterior chamber of Mol- hemorrhage in his right eye. A limited Silicone oil could be seen migrating teno implants (IOP, Costa Mesa, anterior chamber washout was per- through the Ahmed tube (Figure 4 Calif).1,2 This report describes a case formed at the time of the primary re- and Figure 5) and the bleb over the of intraocular silicone oil egressing pair. -

Congenital Ectopia Lentis - Diagnosis and Treatment
From THE DEPARTMENT OF CLINICAL NEUROSCIENCE, SECTION OF OPHTHALMOLOGY AND VISION, ST. ERIK EYE HOSPITAL Karolinska Institutet, Stockholm, Sweden CONGENITAL ECTOPIA LENTIS - DIAGNOSIS AND TREATMENT Tiina Rysä Konradsen Stockholm 2012 All previously published papers were reproduced with permission from the publisher. Published by Karolinska Institutet. Printed by Larserics Digital Print AB. © Tiina Rysä Konradsen, 2012 ISBN 978-91-7457-883-6 ABSTRACT Congenital ectopia lentis (EL) is an ocular condition, which typically causes a high grade of refractive errors, mainly myopia and astigmatism. These might be difficult to compensate for, especially in children, who might develop ametropic amblyopia. Surgery on ectopic lenses has previously been controversial, due to the risk of sight- threatening complications. In paper I we studied retrospectively visual outcomes and complications in children, who were operated for congenital EL, and who had en scleral-fixated capsular tension ring (CTR) and an intra-ocular lens (IOL) implanted at the primary surgery. Thirty-seven eyes of 22 children were included. Visual acuity (VA) improved in all eyes, and only few had persistent amblyopia at the end of the follow-up. A great majority of the eyes had postoperative visual axis opacification (VAO), which was expected, since the posterior capsule was left intact at the primary surgery. Two eyes required secondary suturing for IOL decentration. No eye had any serious complications such as retinal detachment, glaucoma or endophthalmitis. Congenital ectopia lentis is often an indicator of a systemic connective tissue disorder, and Marfan syndrome (MFS) is diagnosed in 70% of the cases. This genetic disorder affects basically all organ systems in the body, EL and dilatation of the ascending aorta being the cardinal signs. -

Differences in Manifestations of Marfan Syndrome, Ehlers-Danlos Syndrome, and Loeys-Dietz Syndrome
1/30/2019 Differences in manifestations of Marfan syndrome, Ehlers-Danlos syndrome, and Loeys-Dietz syndrome Ann Cardiothorac Surg. 2017 Nov; 6(6): 582–594. PMCID: PMC5721110 doi: 10.21037/acs.2017.11.03: 10.21037/acs.2017.11.03 PMID: 29270370 Differences in manifestations of Marfan syndrome, Ehlers-Danlos syndrome, and Loeys-Dietz syndrome Josephina A. N. Meester,1 Aline Verstraeten,1 Dorien Schepers,1 Maaike Alaerts,1 Lut Van Laer,1 and Bart L. Loeys 1,2 1Center of Medical Genetics, Faculty of Medicine and Health Sciences, University of Antwerp and Antwerp University Hospital, Antwerp, Belgium; 2Department of Genetics, Radboud University Medical Center, Nijmegen, The Netherlands Corresponding author. Correspondence to: Bart L. Loeys. Center for Medical Genetics, University of Antwerp, Antwerp University Hospital, Prins Boudewijnlaan 43/6, 2650 Antwerp, Belgium. Email: [email protected]. Received 2017 Jul 1; Accepted 2017 Oct 9. Copyright 2017 Annals of Cardiothoracic Surgery. All rights reserved. Abstract Many different heritable connective tissue disorders (HCTD) have been described over the past decades. These syndromes often affect the connective tissue of various organ systems, including heart, blood vessels, skin, joints, bone, eyes, and lungs. The discovery of these HCTD was followed by the identification of mutations in a wide range of genes encoding structural proteins, modifying enzymes, or components of the TGFβ-signaling pathway. Three typical examples of HCTD are Marfan syndrome (MFS), Ehlers-Danlos syndrome (EDS), and Loeys-Dietz syndrome (LDS). These syndromes show some degree of phenotypical overlap of cardiovascular, skeletal, and cutaneous features. MFS is typically characterized by cardiovascular, ocular, and skeletal manifestations and is caused by heterozygous mutations in FBN1, coding for the extracellular matrix (ECM) protein fibrillin-1. -

Marfan Syndrome: Jeffrey Welder MSIII, Erik L
Marfan Syndrome: Jeffrey Welder MSIII, Erik L. Nylen MSE, Thomas Oetting MS MD May 6, 2010 Chief Complaint: Decreased vision and glare in both eyes. History of Present Illness: A 28 year old woman with a history of Marfan syndrome presented to the comprehensive ophthalmology clinic reporting a progressive decrease in vision and worsening glare in both eyes. She had been seen by ophthalmologists in the past, and had been told that her crystalline lenses were subluxed in both eyes. She had not had problems with her vision until recent months. Past Medical History: Marfan syndrome with aortic stenosis followed by cardiology Medications: Oral beta blocker Family History: No known family members with Marfan Syndrome. Grandmother with glaucoma. Social History: The patient is a graduate student. Ocular Exam: External Exam normal. VA (with correction): OD 20/40 OS 20/50 Current glasses: OD: 6.75+ 5.00 x 135 OS: -5.25 + 4.25 x 60 Pupils: No anisocoria and no relative afferent pupillary defect Motility: Ocular motility full OU. Anterior segment exam: Inferiorly subluxed lenses OU (figure 1 and 2). The angle was deep OU and there was no lens apposition to the cornea in either eye. Dilated funduscopic exam: Posterior segment was normal OU with no peripheral retinal degeneration . Course: The patient’s subluxed lenses led to poor vision from peripheral lenticular irregular astigmatism and glare. She was taken to the operating room where her relatively clear lenses were removed and iris sutured intraocular lenses were placed. The surgical video for one of the eyes may be viewed at http://www.facebook.com/video/video.php?v=153379281140 Page | 1 Figure One: Note the inferiorly subluxed lens. -

Marfan Syndrome Precision Panel Overview Indications Clinical Utility
Marfan Syndrome Precision Panel Overview Marfan Syndrome (MFS) is a spectrum of disorders caused by a genetic defect of the connective tissue and it is inherited in an autosomal dominant pattern. Since the connective tissue is the tissue that helps body growth as well as serving as a scaffold for cells and organs, Marfan Syndrome is a pleiotropic syndrome affecting mainly musculoskeletal, cardiac and ocular systems. The most severe of these manifestations include aortic root dilation and dissection, which are responsible for early patient demise. Pregnancy is a time of increased cardiovascular risk for women with Marfan syndrome, so an early diagnosis is key in pregnancy management. The Igenomix Marfan Syndrome Precision Panel can be used to make an accurate and directed diagnosis as well as a differential diagnosis of connective tissue disorders due to their overlapping phenotypic features ultimately leading to a better management and prognosis of the disease. It provides a comprehensive analysis of the genes involved in this disease using next-generation sequencing (NGS) to fully understand the spectrum of relevant genes involved. Indications The Igenomix Marfan Syndrome Precision Panel is indicated for those patients with a clinical suspicion or diagnosis with or without the following manifestations: - Subluxation of lenses - Cardiovascular findings: mitral valve prolapse, aortic regurgitation, mitral regurgitation, aortic dilation, dissection or aneurysm - Tall and thin stature - Long fingers and toes - Pectus carinatum or excavatum - Scoliosis - Hypermobile joints - Severe hindfoot valgus Clinical Utility The clinical utility of this panel is: - The genetic and molecular confirmation for an accurate clinical diagnosis of a symptomatic patient. Understanding global and molecular functions of fibrillin containing microfibrils for the development of a comprehensive theory of pathogenesis. -

Editorial Page on Keratoconus
Acta Scientific Ophthalmology Volume 1 Issue 3 November 2018 Editorial Editorial Page on Keratoconus Gowhar Ahmad* Department of Ophthalmology, University of Jammu and Kashmir, India *Corresponding Author: Gowhar Ahmad, Department of ophthalmology, University of Jammu and Kashmir, India. Received: October 23, 2018; Published: October 25, 2018 keratoconus is a degenerative disease characterised by non- 13. Mar fans - 14. Mitral valves prolapse syndrome fraction so patient presents with frequent changes in refraction inflammatory corneal ectasia their is progressive changes in re 15. Achondroplasia condition is usually bilateral more common at puberty with male 16. Topic dermatitis preponderance condition has base and apex of cone base is re- 17. Aniridia ferred to plauciod cornea and apex is referred to nipple cornea keratoconus is a visual disturbing disease and not a visual threat- 18. Cong cataracts ening disease complicated cases of this disease entity present as 19. ROP keratoglobus glaucoma and hydrops typical characterises of kera- Recent modalities in the treatment of keratoconus are toconus are 1. Crossed corneal linkage 1. Foods and ruptures in de smets membrane of cornea 2. Hybrid contact lenses 2. Munson’s sign that is distortion of lower lid margin 3. Customised contact lens caused by bulged corea when patient looks in downward 4. Scleral contact lens phase 5. Scleral contact lens 3. Fleisher’s ring which is brownish ring of hemosiderin at 6. Pegy contact lens base of cone 7. Intrastromal corneal ring 4. Enlarged or visible corneal nerves 8. lamellar keratoplasty. 5. Vogt strea which are present in post stroma of cornea dis- appear on pressing the cornea Associated conditions with keratoconus are as follows Volume 1 Issue 3 November 2018 1. -

Axenfeld-Rieger Syndrome with Secondary Glaucoma
Axenfeld-Rieger Syndrome with Secondary Glaucoma Case History -68 year old Caucasian male -No ocular/visual complaints. Presented for follow up appointment for intraocular pressure check. -Ocular history: 1. Axenfeld-Rieger Syndrome OU 2. Secondary glaucoma OU 3. History of angle closure 3. Optic disc pallor OS 4. History of macular edema OS secondary to ACIOL 5. Pseudophakia OU -Systemic history: 1. Nicotine and alcohol dependence 2. Macrocytosis 3. General health deterioration 4. Coronary arteriosclerosis 5. Chronic obstructive lung disease 6. Barrett’s esophagus 7. Essential hypertension 8. Hypothyroidism -Ocular meds: 1. Latanoprost QHS OU 2. Cosopt BID OU 3. Brimonidine BID OU 4. Pilocarpine QID OD only Pertinent findings Visual acuities with spectacle correction were 20/50 in the right eye and count fingers at 2 feet in the left. Confrontation fields showed superior constriction in the right eye and patient was unable in the left. Pupils had no reaction to light in both eyes with anisocoria and correctopia OU. Slit lamp examination revealed an intact flat plate graft superiorly in the right eye covering an Ahmed valve at 12 o’clock in the left. An anterior chamber intraocular lens was present in both eyes. The iris of each eye showed atrophy inferiorly, and patent peripheral iridotomies superior temporally. Intraocular pressures via Goldmann applanation tonometry were 20 mmHg in both eyes. No fundus exam was performed at this visit. Differential diagnosis -ICE (iridocorneal endothelial) syndrome -Peter’s anomaly -Congenital ectropion uveae -Aniridia -Ectopia lentis et pupilae Diagnosis Axenfeld-Rieger Syndrome is diagnosed based on clinical features, including iris and pupillary abnormalities in the presence of an anteriorly displaced schwalbe’s line.