The Approach to the Infant with Ambiguous Genitalia
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Background Briefing Document from the Consortium of Sponsors for The
BRIEFING BOOK FOR Pediatric Advisory Committee (PAC) Prepared by Alan Rogol, M.D., Ph.D. Prepared for Consortium of Sponsors Meeting Date: April 8th, 2019 TABLE OF CONTENTS LIST OF FIGURES ................................................... ERROR! BOOKMARK NOT DEFINED. LIST OF TABLES ...........................................................................................................................4 1. INTRODUCTION AND BACKGROUND FOR THE MEETING .............................6 1.1. INDICATION AND USAGE .......................................................................................6 2. SPONSOR CONSORTIUM PARTICIPANTS ............................................................6 2.1. TIMELINE FOR SPONSOR ENGAGEMENT FOR PEDIATRIC ADVISORY COMMITTEE (PAC): ............................................................................6 3. BACKGROUND AND RATIONALE .........................................................................7 3.1. INTRODUCTION ........................................................................................................7 3.2. PHYSICAL CHANGES OF PUBERTY ......................................................................7 3.2.1. Boys ..............................................................................................................................7 3.2.2. Growth and Pubertal Development ..............................................................................8 3.3. AGE AT ONSET OF PUBERTY.................................................................................9 3.4. -
Case Report Full Text Online At
Case Report Full text online at http://www.jiaps.com Penile agenesis A. K. Bangroo, Ramji Khetri, Sashi Tiwari St Stephen's Hospital, Tis Hazari, Delhi Correspondence: AK Bangroo, 103, Administrative block, St. Stephens Hospital, Tis Hazari, Delhi-110054, India. E-mail: [email protected] ABSTRACT Penile agenesis is an extremely rare disorder with profound urological and psychological consequences. The goal of treatment is an early female gender assignment and feminizing reconstruction of the perineum. KEY WORDS: Aphallia, Penile agenesis, Ambiguous genitalia Penile agenesis (PA) is an extremely rare developmental the scrotal folds which were preserved for subsequent anomaly with the reported incidence of 1 in 30 million genital reconstruction. births[1]. PA is believed to result from either the absence of the genital tubercle, or its failure to develop.[2] Several DISCUSSION investigators claim the absence of corpora cavernosa and corpora spongiosum as a prerequisite for the diagnosis of The earliest case report of aphallia was by Imminger in penile agenesis.[3] Except for the reported XX-XY mosaic, 1853[2] since then only 75 cases have been reported in the patients have 46 XY karyotypes.[4] More than half of these literature[6]. Skoog and Belman[5] suggested three variants, have associated anomalies, including developmental de based on urethral position in relationship to the anal fects of the caudal axis, genitourinary and gastrointestinal sphincter, as: Postsphincteric; Presphincteric tract anomalies.[5] The scrotum, testes and testicular func (Prostatorectal fistula) and Urethral atresia. More proxi tion are usually normal[2]. mal the bladder outlet, greater is the likelihood of other anomalies and death.[5] CASE REPORT A two-day-old 3.2 kg genotypic male (46XY) neonate was brought, by a social organization, to our hospital with the complaint of absence of penis, and passage of meco nium mixed with urine through rectum. -

EAU Pocket Guidelines on Male Hypogonadism 2013
GUIDELINES ON MALE HYPOGONADISM G.R. Dohle (chair), S. Arver, C. Bettocchi, S. Kliesch, M. Punab, W. de Ronde Introduction Male hypogonadism is a clinical syndrome caused by andro- gen deficiency. It may adversely affect multiple organ func- tions and quality of life. Androgens play a crucial role in the development and maintenance of male reproductive and sexual functions. Low levels of circulating androgens can cause disturbances in male sexual development, resulting in congenital abnormalities of the male reproductive tract. Later in life, this may cause reduced fertility, sexual dysfunc- tion, decreased muscle formation and bone mineralisation, disturbances of fat metabolism, and cognitive dysfunction. Testosterone levels decrease as a process of ageing: signs and symptoms caused by this decline can be considered a normal part of ageing. However, low testosterone levels are also associated with several chronic diseases, and sympto- matic patients may benefit from testosterone treatment. Androgen deficiency increases with age; an annual decline in circulating testosterone of 0.4-2.0% has been reported. In middle-aged men, the incidence was found to be 6%. It is more prevalent in older men, in men with obesity, those with co-morbidities, and in men with a poor health status. Aetiology and forms Male hypogonadism can be classified in 4 forms: 1. Primary forms caused by testicular insufficiency. 2. Secondary forms caused by hypothalamic-pituitary dysfunction. 164 Male Hypogonadism 3. Late onset hypogonadism. 4. Male hypogonadism due to androgen receptor insensitivity. The main causes of these different forms of hypogonadism are highlighted in Table 1. The type of hypogonadism has to be differentiated, as this has implications for patient evaluation and treatment and enables identification of patients with associated health problems. -

A MRI Diagnosis of Congenital Urogenital Anomalies in 27 Years
Journal of Advances in Radiology and Medical Imaging Volume 4 | Issue 1 ISSN: 2456-5504 Case Report Open Access A MRI Diagnosis of Congenital Urogenital Anomalies in 27 Years Old Man D’Amato D*, Ranalli T, Tatulli D, Bocchinfuso F, Manenti G, Valente F and Bizzaglia M Diagnostic and Interventional Radiology, Policlinico Tor Vergata, University of Rome “Tor Vergata”, Rome, Italy *Corresponding author: D’Amato D, Diagnostic and Interventional Radiology, Policlinico Tor Vergata, University of Rome “Tor Vergata”, Viale Oxford 181, Rome, Italy, Tel: +393207034690, E-mail: [email protected] Citation: D’Amato D, Ranalli T, Tatulli D, Bocchinfuso F, Manenti G, et al. (2019) A MRI Diagnosis of Congenital Urogenital Anomalies in 27 Years Old Man. J Adv Radiol Med Image 4(1): 102 Received Date: April 04, 2019 Accepted Date: August 26, 2019 Published Date: August 28, 2019 Abstract Congenital anorchia is an uncommon clinical condition. Etiology and pathogenetic mechanisms are often unknown. Although some patients with anorchia present with ambiguous external genitalia or micropenis, most have a normal phenotype. XY Disorders of Sex Development classifications are numerous and success rate in establishing a precise diagnosis is far lower than in XX karyotype. We report the case of a young man, with 46 XY karyotype showing various uro-genital abnormalities. A definitive diagnosis was not established due to the complex clinical presentation. Ultrasonography and Magnetic Resonance Imaging techniques were useful tools in the definition of uro-genital anomalies and gonadal development in this complex scenario. Keywords: Anorchia; Cryptorchidism; Urogenital Anomalies; DSD; MRI List of abbreviations: MRI: Magnetic Resonance Imaging; US: Ultrasonography; DSD: Disorders of Sex Development, FSH: Follicle- Stimulating Hormone; HCG: Human Chorionic Gonadotropin; LH: Luteinizing Hormone; AMH Antimüllerian Hormone; LHRH LH- Releasing Hormone; SD: Standard Deviation Introduction The disorders of sexual differentiation constitute a challenging area for both diagnostic and therapeutic impact. -

IHRA 20210628 Review
28 June 2021 Review of Victorian government, community and related resources on intersex Morgan Carpenter, Intersex Human Rights Australia (IHRA) 1 Contents 1 Contents ........................................................................................................................... 2 2 About this review ............................................................................................................. 2 3 Summary oF key issues ..................................................................................................... 3 3.1 Key issues arising in the resources review ................................................................ 3 3.2 A note on changing nomenclature ........................................................................... 4 4 Victorian government ....................................................................................................... 5 4.1 Bettersafercare.vic.gov.au ........................................................................................ 5 4.2 Health.vic.gov.au ...................................................................................................... 8 4.3 Victorian public service ........................................................................................... 10 5 Community and support organisations .......................................................................... 10 5.1 Australian X & Y Spectrum Support (AXYS) ............................................................. 10 5.2 Congenital Adrenal Hyperplasia Support Group Australia -

Growth Hormone Deficiency Causing Micropenis:Peter A
Growth Hormone Deficiency Causing Micropenis:Peter A. Lee, MD, PhD, a Tom Mazur, PsyD, Lessons b Christopher P. Houk, MD, Learned c Robert M. Blizzard, MD d From a Well-Adjusted Adultabstract This report of a 46, XY patient born with a micropenis consistent with etiology from isolated congenital growth hormone deficiency is used to (1) raise the question regarding what degree testicular testosterone exposure aDepartment of Pediatrics, College of Medicine, Penn State to the central nervous system during fetal life and early infancy has on the University, Hershey, Pennsylvania; bCenter for Psychosexual development of male gender identity, regardless of gender of rearing; (2) Health, Jacobs School of Medicine and Biomedical suggest the obligatory nature of timely full disclosure of medical history; Sciences, University at Buffalo and John R. Oishei Children’s Hospital, Buffalo, New York; cDepartment of (3) emphasize that virtually all 46, XY infants with functional testes and Pediatrics, Medical College of Georgia, Augusta University, a micropenis should be initially boys except some with partial androgen Augusta, Georgia; and dDepartment of Pediatrics, College of Medicine, University of Virginia, Charlottesville, Virginia insensitivity syndrome; and (4) highlight the sustaining value of a positive long-term relationship with a trusted physician (R.M.B.). When this infant Dr Lee reviewed and discussed the extensive medical records with Dr Blizzard, reviewed presented, it was commonly considered inappropriate to gender assign an pertinent medical literature, and wrote each draft infant male whose penis was so small that an adult size was expected to be of the manuscript with input from all coauthors; inadequate, even if the karyotype was 46, XY, and testes were functional. -

Polycystic Ovary Syndrome
Review: Polycystic ovary syndrome Polycystic ovary syndrome Maharaj S, MBChB, FCP(SA) Amod A, MBChB, FCP(SA) Department of Endocrinology and Metabolism, Division of Medicine, Nelson R Mandela School of Medicine, University of KwaZulu-Natal, South Africa Correspondence to: Dr Sureka Maharaj, e-mail: [email protected] Keywords: polycystic ovary syndrome, PCOS, polycystic ovarian disease, PCOD, polycystic ovarian morphology, PCOM Introduction The description of polycystic ovaries dates back as far as 17211 but it was Stein and Leventhal who first reported the disorder, that we now know as the polycystic ovary (or ovarian) syndrome (PCOS), in seven women with amenorrhoea, enlarged ovaries with multiple cysts and hirsutism.2 These patients were treated with ovarian wedge resection and of the seven all had return of their menstrual cycles, and two conceived. With the advent of hormonal assays in the late 1960’s and early 1970’s, the diagnostic focus expanded to include endocrine abnormalities in the hypothalamic-pituitary-gonadal (HPG) axis.3 Elevated luteinising hormone (LH) levels and hyperandrogenaemia were therefore added to the diagnostic criteria for PCOS.4 The advent of pelvic ultrasonography in the late 1970’s allowed for the non-invasive detection of polycystic ovarian morphology. However, this tool confounded matters when it was discovered that polycystic ovaries was a “common finding in normal women”,5 and that it also occurred in diverse endocrine disorders such as hypothyroidism, hyperprolactinaemia, congenital adrenal hyperplasia and hypothalamic amenorrhoea.6 The finding of polycystic ovaries in normal women has been variably referred to as polycystic ovarian disease (PCOD), polycystic ovaries (PCO) and polycystic ovarian morphology (PCOM). -
Micropenis Associated with Testicular Agenesis
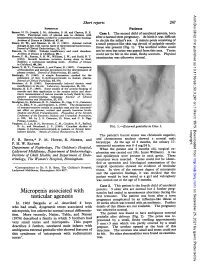
Arch Dis Child: first published as 10.1136/adc.50.3.247 on 1 March 1975. Downloaded from Short reports 247 REFERENCES Patients Barnes, N. D., Joseph, J. M., Atherden, S. M. and Clayton, B. E. (1972). Functional tests of adrenal axis in children with Case 1. The second child of unrelated parents, born measurement of plasma cortisol by competitive protein binding. after a normal term pregnancy. At birth it was difficult Archives of Disease in Childhood, 47, 66. to decide the infant's sex. A minute penis consisting of Deane, H. W., and Masson, G. M. C. (1951). Adrenal cortical a small prepuce-like skin tag devoid of palpable erectile changes in rats with various types of experimental hypertension. .ournal of Clinical Endocrinology, 11, 193. tissue was present (Fig. 1). The urethral orifice could Fanconi, G. (1954). Tubular insufficiency and renal dwarfism. not be seen but urine was passed from this area. Testes Archives of Disease in Childhood, 29, 1. could not be felt in the small, fleshy scrotum. Physical Howse, P. M., Rayner, P. H. W., Williams, J. W., and Rudd, B. T. (1974). Growth hormone secretion during sleep in short examination was otherwise normal. children: a continuous sampling study. Archives of Disease in Childhood, 49, 246. James, V. H. T., Townsend, J., and Fraser, R. (1967). Comparison of fluorimetric and isotopic procedures for the determination of plasma cortisol. journal of Endocrinology, 37, xxviii. Mattingly, D. (1962). A simple fluorimetric method for the estimation of free 1 1-hydroxycorticoids in human plasma. Journal of Clinical Pathology, 15, 374. -

Anne Tamar-Mattis, JD* Advocates for Informed Choice
Report to the Inter-American Commission on Human Rights: Medical Treatment of People with Intersex Conditions as a Human Rights Violation Anne Tamar-Mattis, JD* Advocates for Informed Choice March 13, 2013 I. Introduction Americans born with intersex conditions, or variations of sex anatomy, face a wide range of violations to their sexual and reproductive rights, as well as the rights to bodily integrity and individual autonomy. Beginning in infancy and continuing throughout childhood, children with intersex conditions are subject to irreversible sex assignment and involuntary genital normalizing surgery, sterilization, medical display and photography of the genitals, and medical experimentation. In adulthood, and sometimes in childhood, people with intersex conditions may also be denied necessary medical treatment. Moreover, intersex individuals suffer life-long physical and emotional injury as a result of such treatment. These human rights violations often involve tremendous physical and psychological pain and arguably rise to the level of torture or cruel, inhuman, or degrading treatment (CIDT).† The treatment experienced by American intersex people is a violation of the American Convention on Human Rights. The Convention recognizes torture and cruel, inhuman, or degrading treatment (CIDT) as human rights abuses. Under Article V, “(1) Every person has the right to have his physical, mental, and moral integrity respected. (2) No one shall be subjected to torture or to cruel, inhuman, or degrading punishment or treatment.” §1-2. In order to demonstrate why specific medical practices are human rights abuses against intersex people, we have applied Article 16 of the Convention Against Torture (CAT), and interpretations by the European Court of Human Rights and the mandate of the Special Rapporteur on Torture (SRT). -

Intersex, Discrimination and the Healthcare Environment – a Critical Investigation of Current English Law
Intersex, Discrimination and the Healthcare Environment – a Critical Investigation of Current English Law Karen Jane Brown Submitted in Partial Fulfilment of the Requirements of London Metropolitan University for the Award of PhD Year of final Submission: 2016 Table of Contents Table of Contents......................................................................................................................i Table of Figures........................................................................................................................v Table of Abbreviations.............................................................................................................v Tables of Cases........................................................................................................................vi Domestic cases...vi Cases from the European Court of Human Rights...vii International Jurisprudence...vii Tables of Legislation.............................................................................................................viii Table of Statutes- England…viii Table of Statutory Instruments- England…x Table of Legislation-Scotland…x Table of European and International Measures...x Conventions...x Directives...x Table of Legislation-Australia...xi Table of Legislation-Germany...x Table of Legislation-Malta...x Table of Legislation-New Zealand...xi Table of Legislation-Republic of Ireland...x Table of Legislation-South Africa...xi Objectives of Thesis................................................................................................................xii -

Pathogenic Variants in the DEAH-Box RNA Helicase DHX37 Are a Frequent Cause of 46,XY Gonadal Dysgenesis and 46,XY Testicular Regression Syndrome
ARTICLE © American College of Medical Genetics and Genomics Pathogenic variants in the DEAH-box RNA helicase DHX37 are a frequent cause of 46,XY gonadal dysgenesis and 46,XY testicular regression syndrome Ken McElreavey, PhD 1, Anne Jorgensen, PhD 2, Caroline Eozenou, PhD1, Tiphanie Merel, MSc1, Joelle Bignon-Topalovic, BSc1, Daisylyn Senna Tan, BSc3, Denis Houzelstein, PhD 1, Federica Buonocore, PhD 4, Nick Warr, PhD 5, Raissa G. G. Kay, PhD5, Matthieu Peycelon, MD, PhD 6,7,8, Jean-Pierre Siffroi, MD, PhD6, Inas Mazen, MD9, John C. Achermann, MD, PhD 4, Yuliya Shcherbak, MD10, Juliane Leger, MD, PhD11, Agnes Sallai, MD 12, Jean-Claude Carel, MD, PhD 11, Laetitia Martinerie, MD, PhD11, Romain Le Ru, MD13, Gerard S. Conway, MD, PhD14, Brigitte Mignot, MD15, Lionel Van Maldergem, MD, PhD 16, Rita Bertalan, MD, PhD17, Evgenia Globa, MD, PhD 18, Raja Brauner, MD, PhD19, Ralf Jauch, PhD 3, Serge Nef, PhD 20, Andy Greenfield, PhD5 and Anu Bashamboo, PhD1 Purpose: XY individuals with disorders/differences of sex devel- specifically associated with gonadal dysgenesis and TRS. opment (DSD) are characterized by reduced androgenization Consistent with a role in early testis development, DHX37 is caused, in some children, by gonadal dysgenesis or testis regression expressed specifically in somatic cells of the developing human during fetal development. The genetic etiology for most patients and mouse testis. with 46,XY gonadal dysgenesis and for all patients with testicular Conclusion: DHX37 pathogenic variants are a new cause of an regression syndrome (TRS) is unknown. autosomal dominant form of 46,XY DSD, including gonadal Methods: We performed exome and/or Sanger sequencing in 145 dysgenesis and TRS, showing that these conditions are part of a individuals with 46,XY DSD of unknown etiology including clinical spectrum. -

46 XY Gonadal Dysgenesis in Adulthood 'Pitfalls of Late Diagnosis'
BMJ Case Reports: first published as 10.1136/bcr.12.2010.3626 on 10 February 2012. Downloaded from Reminder of important clinical lesson 46 XY gonadal dysgenesis in adulthood ‘pitfalls of late diagnosis’ Jarna Naing Hamin, 1 Francis Raymond P Arkoncel,2 Frances Lina Lantion-Ang, 1 1 Mark Anthony S Sandoval 1 Section of Endocrinology, Diabetes and Metabolism, Department of Medicine, Philippine General Hospital, University of the Philippines Manila, Manila, Philippines ; 2 Division of Urology, Department of Surgery, Philippine General Hospital, University of the Philippines Manila, Manila, Philippines Correspondence to Dr Mark Anthony S Sandoval, [email protected] Summary Disorders of sex development (DSD) include congenital conditions where developments of chromosomal, gonadal or anatomical sex are atypical. Ostrer in 2000, reported a prevalence of 1:20 000 for 46 XY DSD and complete gonadal dysgenesis. A 21-year-old patient consulted for sexual ambiguity at the out-patient department of the Philippine general hospital. At birth, the perceived female external genitalia and clitoromegaly, led the parents to register and eventually rear the patient as a female. At puberty, he developed masculine features and growth of phallus. Patient was more interested in male activities and began to identify himself as male in the community. The discrepancy between his birth certifi cate and his male gender jeopardised his ambition to become a policeman; this led him to seek medical consult. On physical examination, he was phenotypically male. The external genitalia showed the phallus length of 3.5 cm and perineoscrotal hypospadias. Chromosomal sex was normal 46 XY with neither numerical nor structural aberrations in all cell lines, serum testosterone was low and gonadotrophins were elevated.