GP1BA Gene Glycoprotein Ib Platelet Subunit Alpha
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Urokinase, a Promising Candidate for Fibrinolytic Therapy for Intracerebral Hemorrhage
LABORATORY INVESTIGATION J Neurosurg 126:548–557, 2017 Urokinase, a promising candidate for fibrinolytic therapy for intracerebral hemorrhage *Qiang Tan, MD,1 Qianwei Chen, MD1 Yin Niu, MD,1 Zhou Feng, MD,1 Lin Li, MD,1 Yihao Tao, MD,1 Jun Tang, MD,1 Liming Yang, MD,1 Jing Guo, MD,2 Hua Feng, MD, PhD,1 Gang Zhu, MD, PhD,1 and Zhi Chen, MD, PhD1 1Department of Neurosurgery, Southwest Hospital, Third Military Medical University, Chongqing; and 2Department of Neurosurgery, 211st Hospital of PLA, Harbin, People’s Republic of China OBJECTIVE Intracerebral hemorrhage (ICH) is associated with a high rate of mortality and severe disability, while fi- brinolysis for ICH evacuation is a possible treatment. However, reported adverse effects can counteract the benefits of fibrinolysis and limit the use of tissue-type plasminogen activator (tPA). Identifying appropriate fibrinolytics is still needed. Therefore, the authors here compared the use of urokinase-type plasminogen activator (uPA), an alternate thrombolytic, with that of tPA in a preclinical study. METHODS Intracerebral hemorrhage was induced in adult male Sprague-Dawley rats by injecting autologous blood into the caudate, followed by intraclot fibrinolysis without drainage. Rats were randomized to receive uPA, tPA, or saline within the clot. Hematoma and perihematomal edema, brain water content, Evans blue fluorescence and neurological scores, matrix metalloproteinases (MMPs), MMP mRNA, blood-brain barrier (BBB) tight junction proteins, and nuclear factor–κB (NF-κB) activation were measured to evaluate the effects of these 2 drugs in ICH. RESULTS In comparison with tPA, uPA better ameliorated brain edema and promoted an improved outcome after ICH. -

Hemoglobin Interaction with Gp1ba Induces Platelet Activation And
ARTICLE Platelet Biology & its Disorders Hemoglobin interaction with GP1bα induces platelet activation and apoptosis: a novel mechanism associated with intravascular hemolysis Rashi Singhal,1,2,* Gowtham K. Annarapu,1,2,* Ankita Pandey,1 Sheetal Chawla,1 Amrita Ojha,1 Avinash Gupta,1 Miguel A. Cruz,3 Tulika Seth4 and Prasenjit Guchhait1 1Disease Biology Laboratory, Regional Centre for Biotechnology, National Capital Region, Biotech Science Cluster, Faridabad, India; 2Biotechnology Department, Manipal University, Manipal, Karnataka, India; 3Thrombosis Research Division, Baylor College of Medicine, Houston, TX, USA, and 4Hematology, All India Institute of Medical Sciences, New Delhi, India *RS and GKA contributed equally to this work. ABSTRACT Intravascular hemolysis increases the risk of hypercoagulation and thrombosis in hemolytic disorders. Our study shows a novel mechanism by which extracellular hemoglobin directly affects platelet activation. The binding of Hb to glycoprotein1bα activates platelets. Lower concentrations of Hb (0.37-3 mM) significantly increase the phos- phorylation of signaling adapter proteins, such as Lyn, PI3K, AKT, and ERK, and promote platelet aggregation in vitro. Higher concentrations of Hb (3-6 mM) activate the pro-apoptotic proteins Bak, Bax, cytochrome c, caspase-9 and caspase-3, and increase platelet clot formation. Increased plasma Hb activates platelets and promotes their apoptosis, and plays a crucial role in the pathogenesis of aggregation and development of the procoagulant state in hemolytic disorders. Furthermore, we show that in patients with paroxysmal nocturnal hemoglobinuria, a chronic hemolytic disease characterized by recurrent events of intravascular thrombosis and thromboembolism, it is the elevated plasma Hb or platelet surface bound Hb that positively correlates with platelet activation. -

A Computational Approach for Defining a Signature of Β-Cell Golgi Stress in Diabetes Mellitus
Page 1 of 781 Diabetes A Computational Approach for Defining a Signature of β-Cell Golgi Stress in Diabetes Mellitus Robert N. Bone1,6,7, Olufunmilola Oyebamiji2, Sayali Talware2, Sharmila Selvaraj2, Preethi Krishnan3,6, Farooq Syed1,6,7, Huanmei Wu2, Carmella Evans-Molina 1,3,4,5,6,7,8* Departments of 1Pediatrics, 3Medicine, 4Anatomy, Cell Biology & Physiology, 5Biochemistry & Molecular Biology, the 6Center for Diabetes & Metabolic Diseases, and the 7Herman B. Wells Center for Pediatric Research, Indiana University School of Medicine, Indianapolis, IN 46202; 2Department of BioHealth Informatics, Indiana University-Purdue University Indianapolis, Indianapolis, IN, 46202; 8Roudebush VA Medical Center, Indianapolis, IN 46202. *Corresponding Author(s): Carmella Evans-Molina, MD, PhD ([email protected]) Indiana University School of Medicine, 635 Barnhill Drive, MS 2031A, Indianapolis, IN 46202, Telephone: (317) 274-4145, Fax (317) 274-4107 Running Title: Golgi Stress Response in Diabetes Word Count: 4358 Number of Figures: 6 Keywords: Golgi apparatus stress, Islets, β cell, Type 1 diabetes, Type 2 diabetes 1 Diabetes Publish Ahead of Print, published online August 20, 2020 Diabetes Page 2 of 781 ABSTRACT The Golgi apparatus (GA) is an important site of insulin processing and granule maturation, but whether GA organelle dysfunction and GA stress are present in the diabetic β-cell has not been tested. We utilized an informatics-based approach to develop a transcriptional signature of β-cell GA stress using existing RNA sequencing and microarray datasets generated using human islets from donors with diabetes and islets where type 1(T1D) and type 2 diabetes (T2D) had been modeled ex vivo. To narrow our results to GA-specific genes, we applied a filter set of 1,030 genes accepted as GA associated. -
Supp Table 1.Pdf
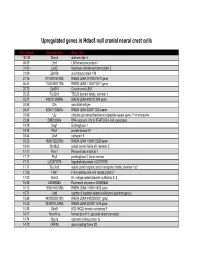
Upregulated genes in Hdac8 null cranial neural crest cells fold change Gene Symbol Gene Title 134.39 Stmn4 stathmin-like 4 46.05 Lhx1 LIM homeobox protein 1 31.45 Lect2 leukocyte cell-derived chemotaxin 2 31.09 Zfp108 zinc finger protein 108 27.74 0710007G10Rik RIKEN cDNA 0710007G10 gene 26.31 1700019O17Rik RIKEN cDNA 1700019O17 gene 25.72 Cyb561 Cytochrome b-561 25.35 Tsc22d1 TSC22 domain family, member 1 25.27 4921513I08Rik RIKEN cDNA 4921513I08 gene 24.58 Ofa oncofetal antigen 24.47 B230112I24Rik RIKEN cDNA B230112I24 gene 23.86 Uty ubiquitously transcribed tetratricopeptide repeat gene, Y chromosome 22.84 D8Ertd268e DNA segment, Chr 8, ERATO Doi 268, expressed 19.78 Dag1 Dystroglycan 1 19.74 Pkn1 protein kinase N1 18.64 Cts8 cathepsin 8 18.23 1500012D20Rik RIKEN cDNA 1500012D20 gene 18.09 Slc43a2 solute carrier family 43, member 2 17.17 Pcm1 Pericentriolar material 1 17.17 Prg2 proteoglycan 2, bone marrow 17.11 LOC671579 hypothetical protein LOC671579 17.11 Slco1a5 solute carrier organic anion transporter family, member 1a5 17.02 Fbxl7 F-box and leucine-rich repeat protein 7 17.02 Kcns2 K+ voltage-gated channel, subfamily S, 2 16.93 AW493845 Expressed sequence AW493845 16.12 1600014K23Rik RIKEN cDNA 1600014K23 gene 15.71 Cst8 cystatin 8 (cystatin-related epididymal spermatogenic) 15.68 4922502D21Rik RIKEN cDNA 4922502D21 gene 15.32 2810011L19Rik RIKEN cDNA 2810011L19 gene 15.08 Btbd9 BTB (POZ) domain containing 9 14.77 Hoxa11os homeo box A11, opposite strand transcript 14.74 Obp1a odorant binding protein Ia 14.72 ORF28 open reading -

Supplementary Table 1: Adhesion Genes Data Set
Supplementary Table 1: Adhesion genes data set PROBE Entrez Gene ID Celera Gene ID Gene_Symbol Gene_Name 160832 1 hCG201364.3 A1BG alpha-1-B glycoprotein 223658 1 hCG201364.3 A1BG alpha-1-B glycoprotein 212988 102 hCG40040.3 ADAM10 ADAM metallopeptidase domain 10 133411 4185 hCG28232.2 ADAM11 ADAM metallopeptidase domain 11 110695 8038 hCG40937.4 ADAM12 ADAM metallopeptidase domain 12 (meltrin alpha) 195222 8038 hCG40937.4 ADAM12 ADAM metallopeptidase domain 12 (meltrin alpha) 165344 8751 hCG20021.3 ADAM15 ADAM metallopeptidase domain 15 (metargidin) 189065 6868 null ADAM17 ADAM metallopeptidase domain 17 (tumor necrosis factor, alpha, converting enzyme) 108119 8728 hCG15398.4 ADAM19 ADAM metallopeptidase domain 19 (meltrin beta) 117763 8748 hCG20675.3 ADAM20 ADAM metallopeptidase domain 20 126448 8747 hCG1785634.2 ADAM21 ADAM metallopeptidase domain 21 208981 8747 hCG1785634.2|hCG2042897 ADAM21 ADAM metallopeptidase domain 21 180903 53616 hCG17212.4 ADAM22 ADAM metallopeptidase domain 22 177272 8745 hCG1811623.1 ADAM23 ADAM metallopeptidase domain 23 102384 10863 hCG1818505.1 ADAM28 ADAM metallopeptidase domain 28 119968 11086 hCG1786734.2 ADAM29 ADAM metallopeptidase domain 29 205542 11085 hCG1997196.1 ADAM30 ADAM metallopeptidase domain 30 148417 80332 hCG39255.4 ADAM33 ADAM metallopeptidase domain 33 140492 8756 hCG1789002.2 ADAM7 ADAM metallopeptidase domain 7 122603 101 hCG1816947.1 ADAM8 ADAM metallopeptidase domain 8 183965 8754 hCG1996391 ADAM9 ADAM metallopeptidase domain 9 (meltrin gamma) 129974 27299 hCG15447.3 ADAMDEC1 ADAM-like, -

Cellular and Molecular Signatures in the Disease Tissue of Early
Cellular and Molecular Signatures in the Disease Tissue of Early Rheumatoid Arthritis Stratify Clinical Response to csDMARD-Therapy and Predict Radiographic Progression Frances Humby1,* Myles Lewis1,* Nandhini Ramamoorthi2, Jason Hackney3, Michael Barnes1, Michele Bombardieri1, Francesca Setiadi2, Stephen Kelly1, Fabiola Bene1, Maria di Cicco1, Sudeh Riahi1, Vidalba Rocher-Ros1, Nora Ng1, Ilias Lazorou1, Rebecca E. Hands1, Desiree van der Heijde4, Robert Landewé5, Annette van der Helm-van Mil4, Alberto Cauli6, Iain B. McInnes7, Christopher D. Buckley8, Ernest Choy9, Peter Taylor10, Michael J. Townsend2 & Costantino Pitzalis1 1Centre for Experimental Medicine and Rheumatology, William Harvey Research Institute, Barts and The London School of Medicine and Dentistry, Queen Mary University of London, Charterhouse Square, London EC1M 6BQ, UK. Departments of 2Biomarker Discovery OMNI, 3Bioinformatics and Computational Biology, Genentech Research and Early Development, South San Francisco, California 94080 USA 4Department of Rheumatology, Leiden University Medical Center, The Netherlands 5Department of Clinical Immunology & Rheumatology, Amsterdam Rheumatology & Immunology Center, Amsterdam, The Netherlands 6Rheumatology Unit, Department of Medical Sciences, Policlinico of the University of Cagliari, Cagliari, Italy 7Institute of Infection, Immunity and Inflammation, University of Glasgow, Glasgow G12 8TA, UK 8Rheumatology Research Group, Institute of Inflammation and Ageing (IIA), University of Birmingham, Birmingham B15 2WB, UK 9Institute of -

Datasheet: MCA740PE Product Details
Datasheet: MCA740PE Description: MOUSE ANTI HUMAN CD42b:RPE Specificity: CD42b Other names: GPIB-ALPHA Format: RPE Product Type: Monoclonal Antibody Clone: AK2 Isotype: IgG1 Quantity: 100 TESTS Product Details Applications This product has been reported to work in the following applications. This information is derived from testing within our laboratories, peer-reviewed publications or personal communications from the originators. Please refer to references indicated for further information. For general protocol recommendations, please visit www.bio-rad-antibodies.com/protocols. Yes No Not Determined Suggested Dilution Flow Cytometry Neat Where this antibody has not been tested for use in a particular technique this does not necessarily exclude its use in such procedures. The suggested working dilution is given as a guide only. It is recommended that the user titrates the antibody for use in his/her own system using appropriate negative/positive controls. Target Species Human Product Form Purified IgG conjugated to R. Phycoerythrin (RPE) - lyophilized Reconstitution Reconstitute with 1 ml distilled water Max Ex/Em Fluorophore Excitation Max (nm) Emission Max (nm) RPE 488nm laser 496 578 Preparation Purified IgG prepared by affinity chromatography on Protein A from tissue culture supernatant Buffer Solution Phosphate buffered saline Preservative 0.09% Sodium Azide Stabilisers 1% Bovine Serum Albumin 5% Sucrose External Database Links UniProt: P07359 Related reagents Entrez Gene: 2811 GP1BA Related reagents Page 1 of 3 Specificity Mouse anti Human CD42b antibody, clone AK2 recognizes the human CD42b cell surface antigen, also known as platelet glycoprotein GP1B. CD42b is expressed by platelets and megakaryocytes. Clone AK2 has been reported to block the binding of von Willebrand Factor (VWF) to platelets Flow Cytometry Use 10ul of the suggested working dilution to label 100ul whole blood. -

Path Ggf 5 2020.Pdf
Hemostasis Hemostasis and Thrombosis Normal hemostasis is a consequence of tightly regulated processes that maintain blood in a fluid state in normal vessels, yet also permit the rapid formation of a hemostatic clot at the site of a vascular injury. Thrombosis involves blood clot formation within intact vessels. Both hemostasis and thrombosis involve three components: the vascular wall, platelets and the coagulation cascade. Elements of the Hemostatic process • Endothelium • Anti-thrombosis • Pro-thrombosis • Platelets • Platelet-endothelial cell interaction • Coagulation cascade http://www.as.miami.edu/chemistry/2086/chapter_21/NEW-Chap21_class_part1_files/image002.jpg After initial injury there is a brief period of arteriolar vasoconstriction mediated by reflex neurogenic mechanisms and augmented by the local secretion of factors such as endothelin (a potent endothelium-derived vasoconstrictor) The effect is transient, however, and bleeding would resume if not for activation of the platelet and coagulation systems. Endothelial injury exposes highly thrombogenic subendothelial extracellular matrix (ECM), facilitating platelet adherence and activation. Activation of platelets results in a dramatic shape change (from small rounded discs to flat plates with markedly increased surface area), as well as the release of secretory granules. Within minutes the secreted products recruit additional platelets (aggregation) to form a hemostatic plug; this process is referred to as primary hemostasis. http://www.ouhsc.edu/platelets/Platelet%20Pic s/Platelets3.jpg http://medcell.med.yale.edu/histology/blood_bone_marr ow_lab/images/platelets_em.jpg Tissue factor is also exposed at the site of injury. Also known as factor III and thromboplastin, tissue factor is a membrane-bound procoagulant glycoprotein synthesized by endothelial cells. It acts in conjunction with factor VII (see below) as the major in vivo initiator of the coagulation cascade, eventually culminating in thrombin generation. -

A Guide for People Living with Von Willebrand Disorder CONTENTS
A guide for people living with von Willebrand disorder CONTENTS What is von Willebrand disorder (VWD)?................................... 3 Symptoms............................................................................................... 5 Types of VWD...................................................................................... 6 How do you get VWD?...................................................................... 7 VWD and blood clotting.................................................................... 11 Diagnosis................................................................................................. 13 Treatment............................................................................................... 15 Taking care of yourself or your child.............................................. 19 (Education, information, first aid/medical emergencies, medication to avoid) Living well with VWD......................................................................... 26 (Sport, travel, school, telling others, work) Special issues for women and girls.................................................. 33 Connecting with others..................................................................... 36 Can I live a normal life with von Willebrand disorder?............. 37 More information................................................................................. 38 2 WHAT IS VON WILLEBRAND DISORDER (VWD)? Von Willebrand disorder (VWD) is an inherited bleeding disorder. People with VWD have a problem with a protein -

Fibrin Induces Release of Von Willebrand Factor from Endothelial Cells
Fibrin induces release of von Willebrand factor from endothelial cells. J A Ribes, … , C W Francis, D D Wagner J Clin Invest. 1987;79(1):117-123. https://doi.org/10.1172/JCI112771. Research Article Addition of fibrinogen to human umbilical vein endothelial cells in culture resulted in release of von Willebrand factor (vWf) from Weibel-Palade bodies that was temporally related to formation of fibrin in the medium. Whereas no release occurred before gelation, the formation of fibrin was associated with disappearance of Weibel-Palade bodies and development of extracellular patches of immunofluorescence typical of vWf release. Release also occurred within 10 min of exposure to preformed fibrin but did not occur after exposure to washed red cells, clot liquor, or structurally different fibrin prepared with reptilase. Metabolically labeled vWf was immunopurified from the medium after release by fibrin and shown to consist of highly processed protein lacking pro-vWf subunits. The contribution of residual thrombin to release stimulated by fibrin was minimized by preparing fibrin clots with nonstimulatory concentrations of thrombin and by inhibiting residual thrombin with hirudin or heating. We conclude that fibrin formed at sites of vessel injury may function as a physiologic secretagogue for endothelial cells causing rapid release of stored vWf. Find the latest version: https://jci.me/112771/pdf Fibrin Induces Release of von Willebrand Factor from Endothelial Cells Julie A. Ribes, Charles W. Francis, and Denisa D. Wagner Hematology Unit, Department ofMedicine, University ofRochester School ofMedicine and Dentistry, Rochester, New York 14642 Abstract erogeneous and can be separated by sodium dodecyl sulfate (SDS) electrophoresis into a series of disulfide-bonded multimers Addition of fibrinogen to human umbilical vein endothelial cells with molecular masses from 500,000 to as high as 20,000,000 in culture resulted in release of von Willebrand factor (vWf) D (8). -

Recommended Abbreviations for Von Willebrand Factor and Its Activities
RECOMMENDED ABBREVIATIONS FOR VON WILLEBRAND FACTOR AND ITS ACTIVITIES On behalf of the von Willebrand Factor Subcommittee of the Scientific and Standardization Committee of the International Society on Thrombosis and Haemostasis Claudine Mazurier and Francesco Rodeghiero Previous official recommendations concerning the abbreviations for von Willebrand Factor (and factor VIII) are 15 years old and were limited to "vWf" for the protein and "vWf:Ag" for the antigen (1). Nowadays, the various properties of von Willebrand Factor (ristocetin cofactor activity and capacity to bind to either collagen or factor VIII) are better defined and may warrant specific abbreviations. Furthermore, the protein synthesized by the von Willebrand factor gene is now abbreviated as pre-pro-VWF (2). Accordingly, the subcommittee on von Willebrand Factor of the Scientific and Standardization Committee of the ISTH has recommended new abbreviations for von Willebrand Factor antigen and its various activities, currently measured by immunologic or functional assays (Table I). It is hoped that a uniform application of the abbreviations recommended here will improve communication among scientists and clinicians, especially for those who are less familiar with the field. Table 1: Recommended abbreviations for von Willebrand Factor and its activities Attribute Recommended abbreviations Mature protein VWF Antigen VWF:Ag Ristocetin cofactor activity VWF:RCo Collagen binding capacity VWF:CB Factor VIII binding capacity VWF:FVIIIB REFERENCES: 1 – Marder VJ, Mannucci PM, Firkin BG, Hoyer LW and Meyer D. Standard nomenclature for factor VIII and von Willebrand factor: a recommendation by the International Committee on Thrombosis and Haemostasis. Thromb. Haemost. 1985, 54, 871-2. 2 – Goodeve AC, Eikenboom JCJ, Ginsburg D, Hilbert L, Mazurier C, Peake IR, Sadler JE, Rodeghiero F on behalf of the ISTH SSC subcommittee on von Willebrand Factor. -

Biomechanical Thrombosis: the Dark Side of Force and Dawn of Mechano- Medicine
Open access Review Stroke Vasc Neurol: first published as 10.1136/svn-2019-000302 on 15 December 2019. Downloaded from Biomechanical thrombosis: the dark side of force and dawn of mechano- medicine Yunfeng Chen ,1 Lining Arnold Ju 2 To cite: Chen Y, Ju LA. ABSTRACT P2Y12 receptor antagonists (clopidogrel, pras- Biomechanical thrombosis: the Arterial thrombosis is in part contributed by excessive ugrel, ticagrelor), inhibitors of thromboxane dark side of force and dawn platelet aggregation, which can lead to blood clotting and A2 (TxA2) generation (aspirin, triflusal) or of mechano- medicine. Stroke subsequent heart attack and stroke. Platelets are sensitive & Vascular Neurology 2019;0. protease- activated receptor 1 (PAR1) antag- to the haemodynamic environment. Rapid haemodynamcis 1 doi:10.1136/svn-2019-000302 onists (vorapaxar). Increasing the dose of and disturbed blood flow, which occur in vessels with these agents, especially aspirin and clopi- growing thrombi and atherosclerotic plaques or is caused YC and LAJ contributed equally. dogrel, has been employed to dampen the by medical device implantation and intervention, promotes Received 12 November 2019 platelet thrombotic functions. However, this platelet aggregation and thrombus formation. In such 4 Accepted 14 November 2019 situations, conventional antiplatelet drugs often have also increases the risk of excessive bleeding. suboptimal efficacy and a serious side effect of excessive It has long been recognized that arterial bleeding. Investigating the mechanisms of platelet thrombosis