Dysphagia What Is Dysphagia? Dysphagia Is a General Term Used to Describe Difficulty Swallowing
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Health History
Health History Patient Name ___________________________________________ Date of Birth _______________ Reason for visit ____________________________________________________________________________________________ Past Medical History Have you ever had the following? (Mark all that apply) ☐ Alcoholism ☐ Cancer ☐ Endocarditis ☐ MRSA/VRE ☐ Allergies ☐ Cardiac Arrest ☐ Gallbladder disease ☐ Myocardial infarction ☐ Anemia ☐ Cardiac dysrhythmias ☐ GERD ☐ Osteoarthritis ☐ Angina ☐ Cardiac valvular disease ☐ Hemoglobinopathy ☐ Osteoporosis ☐ Anxiety ☐ Cerebrovascular accident ☐ Hepatitis C ☐ Peptic ulcer disease ☐ Arthritis ☐ COPD ☐ HIV/AIDS ☐ Psychosis ☐ Asthma ☐ Coronary artery disease ☐ Hyperlipidemia ☐ Pulmonary fibrosis ☐ Atrial fibrillation ☐ Crohn’s disease ☐ Hypertension ☐ Radiation ☐ Benign prostatic hypertrophy ☐ Dementia ☐ Inflammatory bowel disease ☐ Renal disease ☐ Bleeding disorder ☐ Depression ☐ Liver disease ☐ Seizure disorder ☐ Blood clots ☐ Diabetes ☐ Malignant hyperthermia ☐ Sleep apnea ☐ Blood transfusion ☐ DVT ☐ Migraine headaches ☐ Thyroid disease Previous Hospitalizations/Surgeries/Serious Illnesses Have you ever had the following? (Mark all that apply and specify dates) Date Date Date Date ☐ AICD Insertion ☐ Cyst/lipoma removal ☐ Pacemaker ☐ Mastectomy ☐ Angioplasty ☐ ESWL ☐ Pilonidal cyst removal ☐ Myomectomy ☐ Angio w/ stent ☐ Gender reassignment ☐ Small bowel resection ☐ Penile implant ☐ Appendectomy ☐ Hemorrhoidectomy ☐ Thyroidectomy ☐ Prostate biopsy ☐ Arthroscopy knee ☐ Hernia surgery ☐ TIF ☐ TAH/BSO ☐ Bariatric surgery -

General Signs and Symptoms of Abdominal Diseases
General signs and symptoms of abdominal diseases Dr. Förhécz Zsolt Semmelweis University 3rd Department of Internal Medicine Faculty of Medicine, 3rd Year 2018/2019 1st Semester • For descriptive purposes, the abdomen is divided by imaginary lines crossing at the umbilicus, forming the right upper, right lower, left upper, and left lower quadrants. • Another system divides the abdomen into nine sections. Terms for three of them are commonly used: epigastric, umbilical, and hypogastric, or suprapubic Common or Concerning Symptoms • Indigestion or anorexia • Nausea, vomiting, or hematemesis • Abdominal pain • Dysphagia and/or odynophagia • Change in bowel function • Constipation or diarrhea • Jaundice “How is your appetite?” • Anorexia, nausea, vomiting in many gastrointestinal disorders; and – also in pregnancy, – diabetic ketoacidosis, – adrenal insufficiency, – hypercalcemia, – uremia, – liver disease, – emotional states, – adverse drug reactions – Induced but without nausea in anorexia/ bulimia. • Anorexia is a loss or lack of appetite. • Some patients may not actually vomit but raise esophageal or gastric contents in the absence of nausea or retching, called regurgitation. – in esophageal narrowing from stricture or cancer; also with incompetent gastroesophageal sphincter • Ask about any vomitus or regurgitated material and inspect it yourself if possible!!!! – What color is it? – What does the vomitus smell like? – How much has there been? – Ask specifically if it contains any blood and try to determine how much? • Fecal odor – in small bowel obstruction – or gastrocolic fistula • Gastric juice is clear or mucoid. Small amounts of yellowish or greenish bile are common and have no special significance. • Brownish or blackish vomitus with a “coffee- grounds” appearance suggests blood altered by gastric acid. -

Dysphagia Symptoms in People with Diabetes
DYSPHAGIA SYMPTOMS IN PEOPLE WITH DIABETES: A PRELIMINARY REPORT MCKENZIE G. WITZKE Bachelor of Arts in Biology and Psychology The College of Wooster May 2015 submitted in partial fulfillment of requirements for the degree MASTER OF ARTS at the CLEVELAND STATE UNIVERSITY MAY 2020 We hereby approve this thesis For MCKENZIE G. WITZKE Candidate for the Master of Arts degree for the Department of Speech Pathology and Audiology And CLEVELAND STATE UNIVERSITY’S College of Graduate Studies by _______________________________________ Violet Cox Chair, Thesis Committee Department of Speech Pathology and Audiology ________________________________________ Myrita Wilhite Committee member Department of Speech Pathology and Audiology ________________________________________ Anne Su Committee member Department of Health Sciences ___________________April ______________________29, 2020 Date of Defense ACKNOWLEDGEMENTS I wish to express my sincere appreciation to my advisor, Dr. Violet Cox, who has expertly guided me through this process and showed me nothing but patience and support as I navigated this new experience. I would also like to thank Dr. Myrita Wilhite for her encouragement and willingness to provide resources to help me complete this project. Last but not least, I would like to acknowledge the support of my friends and family, who provided consistent camaraderie and encouragement. DYSPHAGIA SYMPTOMS IN PEOPLE WITH DIABETES: A PRELIMINARY REPORT MCKENZIE G. WITZKE ABSTRACT BACKGROUND: Diabetes mellitus is a systemic disease affecting whole-body functioning. The underlying mechanisms and associated concomitant conditions suggest an increased risk for the occurrence of oropharyngeal dysphagia. PURPOSE: This is a qualitative study designed to assess perception of symptoms of oropharyngeal dysphagia in people with diabetes. METHODS: Participants were recruited by word-of-mouth and asked to complete a survey by answering questions on a Likert-type scale indicating the frequency with which they experience each symptom. -

Osteopathic Approach to the Spleen
Osteopathic approach to the spleen Luc Peeters and Grégoire Lason 1. Introduction the first 3 years to 4 - 6 times the birth size. The position therefore progressively becomes more lateral in place of The spleen is an organ that is all too often neglected in the original epigastric position. The spleen is found pos- the clinic, most likely because conditions of the spleen do tero-latero-superior from the stomach, its arterial supply is not tend to present a defined clinical picture. Furthermore, via the splenic artery and the left gastroepiploic artery it has long been thought that the spleen, like the tonsils, is (Figure 2). The venous drainage is via the splenic vein an organ that is superfluous in the adult. into the portal vein (Figure 2). The spleen is actually the largest lymphoid organ in the body and is implicated within the blood circulation. In the foetus it is an organ involved in haematogenesis while in the adult it produces lymphocytes. The spleen is for the blood what the lymph nodes are for the lymphatic system. The spleen also purifies and filters the blood by removing dead cells and foreign materials out of the circulation The function of red blood cell reserve is also essential for the maintenance of human activity. Osteopaths often identify splenic congestion under the influence of poor diaphragm function. Some of the symptoms that can be associated with dysfunction of the spleen are: Figure 2 – Position and vascularisation of the spleen Anaemia in children Disorders of blood development Gingivitis, painful and bleeding gums Swollen, painful tongue, dysphagia and glossitis Fatigue, hyperirritability and restlessness due to the anaemia Vertigo and tinnitus Frequent colds and infections due to decreased resis- tance Thrombocytosis Tension headaches The spleen is also considered an important organ by the osteopath as it plays a role in the immunity, the reaction of the circulation and oxygen transport during effort as well as in regulation of the blood pressure. -

17 Nutrition for Patients with Upper Gastrointestinal Disorders 403
84542_ch17.qxd 7/16/09 6:35 PM Page 402 Nutrition for Patients with Upper 17 Gastrointestinal Disorders TRUE FALSE 1 People who have nausea should avoid liquids with meals. 2 Thin liquids, such as clear juices and clear broths, are usually the easiest items to swallow for patients with dysphagia. 3 All patients with dysphagia are given solid foods in pureed form. 4 In people with GERD, the severity of the pain reflects the extent of esophageal damage. 5 High-fat meals may trigger symptoms of GERD. 6 People with esophagitis may benefit from avoiding spicy or acidic foods. 7 Alcohol stimulates gastric acid secretion. 8 A bland diet promotes healing of peptic ulcers. 9 People with dumping syndrome should avoid sweets and sugars. 10 Pernicious anemia is a potential complication of gastric surgery. UPON COMPLETION OF THIS CHAPTER, YOU WILL BE ABLE TO ● Give examples of ways to promote eating in people with anorexia. ● Describe nutrition interventions that may help maximize intake in people who have nausea. ● Compare the three levels of solid food textures included in the National Dysphagia Diet. ● Compare the four liquid consistencies included in the National Dysphagia Diet. ● Plan a menu appropriate for someone with GERD. ● Teach a patient about role of nutrition therapy in the treatment of peptic ulcer disease. ● Give examples of nutrition therapy recommendations for people experiencing dumping syndrome. utrition therapy is used in the treatment of many digestive system disorders. For many disorders, diet merely plays a supportive role in alleviating symptoms rather than alter- ing the course of the disease. -

Dysphagia - Pathophysiology of Swallowing Dysfunction, Symptoms, Diagnosis and Treatment
ISSN: 2572-4193 Philipsen. J Otolaryngol Rhinol 2019, 5:063 DOI: 10.23937/2572-4193.1510063 Volume 5 | Issue 3 Journal of Open Access Otolaryngology and Rhinology REVIEW ARTICLE Dysphagia - Pathophysiology of Swallowing Dysfunction, Symptoms, Diagnosis and Treatment * Bahareh Bakhshaie Philipsen Check for updates Department of Otorhinolaryngology-Head and Neck Surgery, Odense University Hospital, Denmark *Corresponding author: Dr. Bahareh Bakhshaie Philipsen, Department of Otorhinolaryngology-Head and Neck Surgery, Odense University Hospital, Sdr. Boulevard 29, 5000 Odense C, Denmark, Tel: +45 31329298, Fax: +45 66192615 the vocal folds adduct to prevent aspiration. The esoph- Abstract ageal phase is completely involuntary and consists of Difficulty swallowing is called dysphagia. There is a wide peristaltic waves [2]. range of potential causes of dysphagia. Because there are many reasons why dysphagia can occur, treatment Dysphagia is classified into the following major depends on the underlying cause. Thorough examination types: is important, and implementation of a treatment strategy should be based on evaluation by a multidisciplinary team. 1. Oropharyngeal dysphagia In this article, we will describe the mechanism of swallowing, the pathophysiology of swallowing dysfunction and different 2. Esophageal dysphagia causes of dysphagia, along with signs and symptoms asso- 3. Complex neuromuscular disorders ciated with dysphagia, diagnosis, and potential treatments. 4. Functional dysphagia Keywords Pathophysiology Dysphagia, Deglutition, Deglutition disorders, FEES, Video- fluoroscopy Swallowing is a complex process and many distur- bances in oropharyngeal and esophageal physiology including neurologic deficits, obstruction, fibrosis, struc- Introduction tural damage or congenital and developmental condi- Dysphagia is derived from the Greek phagein, means tions can result in dysphagia. Breathing difficulties can “to eat” [1]. -

Nutrition Intake History
NUTRITION INTAKE HISTORY Date Patient Information Patient Address Apt. Age Sex: M F City State Zip Home # Work # Ext. Birthdate Cell Phone # Patient SS# E-Mail Single Married Separated Divorced Widowed Best time and place to reach you IN CASE OF EMERGENCY, CONTACT Name Relationship Home Phone Work Phone Ext. Whom may we thank for referring you? Work Information Occupation Phone Ext. Company Address Spouse Information Name SS# Birthdate Occupation Employer I verify that all information within these pages is true and accurate. _____________________________________ _________________________________________ _____________________ Patient's Signature Patient's Name - Please print Date Health History Height Weight Number of Children Are you recovering from a cold or flu? Are you pregnant? Reason for office visit: Date started: Date of last physical exam Practitioner name & contact Laboratory procedures performed (e.g., stool analysis, blood and urine chemistries, hair analysis, saliva, bone density): Outcome What types of therapy have you tried for this problem(s)? Diet modification Medical Vitamins/minerals Herbs Homeopathy Chiropractic Acupunture Conventional drugs Physical therapy Other List current health problems for which you are being treated: Current medications (prescription and/or over-the-counter): Major hospitalizations, surgeries, injuries. Please list all procedures, complications (if any) and dates: Year Surgery, illness, injury Outcome Circle the level of stress you are experiencing on a scale of 1 to 10 (1 being the lowest): -

Impairment of Nitric Oxide Pathway by Intravascular Hemolysis Plays A
1521-0103/367/2/194–202$35.00 https://doi.org/10.1124/jpet.118.249581 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS J Pharmacol Exp Ther 367:194–202, November 2018 Copyright ª 2018 by The American Society for Pharmacology and Experimental Therapeutics Impairment of Nitric Oxide Pathway by Intravascular Hemolysis Plays a Major Role in Mice Esophageal Hypercontractility: Reversion by Soluble Guanylyl Cyclase Stimulator Fabio Henrique Silva, Kleber Yotsumoto Fertrin, Eduardo Costa Alexandre, Fabiano Beraldi Calmasini, Carla Fernanda Franco-Penteado, and Fernando Ferreira Costa Hematology and Hemotherapy Center (F.H.S., K.Y.F., C.F.F.-P., F.F.C.) and Department of Pharmacology, Faculty of Medical Sciences (E.C.A., F.B.C.), University of Campinas, Campinas, São Paulo, Brazil; and Division of Hematology, University of Washington, Seattle, Washington (K.Y.F.) Downloaded from Received April 1, 2018; accepted July 30, 2018 ABSTRACT Paroxysmal nocturnal hemoglobinuria (PNH) patients display cyclase stimulator 3-(4-amino-5-cyclopropylpyrimidin-2-yl)- exaggerated intravascular hemolysis and esophageal disor- 1-(2-fluorobenzyl)-1H-pyrazolo[3,4-b]pyridine (BAY 41-2272; ders. Since excess hemoglobin in the plasma causes re- 1 mM) completely reversed the increased contractile responses jpet.aspetjournals.org duced nitric oxide (NO) bioavailability and oxidative stress, we to CCh, KCl, and EFS in PHZ mice, but responses remained hypothesized that esophageal contraction may be impaired unchanged with prior treatment with NO donor sodium nitro- by intravascular hemolysis. This study aimed to analyze the prusside (300 mM). Protein expression of 3-nitrotyrosine and alterations of the esophagus contractile mechanisms in a 4-hydroxynonenal increased in esophagi from PHZ mice, sug- murine model of exaggerated intravascular hemolysis induced gesting a state of oxidative stress. -

Chest Pain, Noncardiac
Sacramento Heart & Vascular Medical Associates February 18, 2012 500 University Ave. Sacramento, CA 95825 Page 1 916-830-2000 Fax: 916-830-2001 Patient Information For: Only A Test Chest Pain, Noncardiac What is noncardiac chest pain? Chest pain is discomfort that is located between the top of the belly and the base of the neck. Chest pain that is [not] caused by a heart problem is called noncardiac chest pain. Because it is very important to determine the cause, always see your healthcare provider if you have chest pain. How does it occur? The most worrisome causes of chest pain are related to your heart. However, many causes of chest pain are not related to a heart problem. These include: - swallowing disorders such as esophageal spasm, caused by the muscles of the lower esophagus squeezing painfully due to acid reflux or stress - gastrointestinal disorders such as heartburn, which is stomach acid backing up into the esophagus - lung disease such as bronchitis or pneumonia - problems affecting the ribs and chest muscles such as muscle strain or inflammation of the ribs or muscles - anxiety or panic attacks - inflammation of the sack around the heart (pericarditis) or of the lining of the lungs (pleuritis/pleurisy). How is it diagnosed? Keeping track of your chest pain will help your healthcare provider make the diagnosis. Write down: - what the pain feels like, such as stabbing, dull, or burning - when it happens and how long it lasts - where it hurts - what makes it better or worse - any other symptoms, such as nausea, vomiting, sweating, or trouble breathing. -
PE3334 Difficulty Swallowing (Dysphagia)
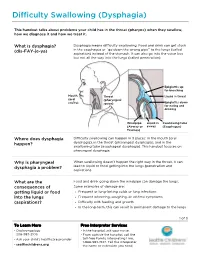
Difficulty Swallowing (Dysphagia) This handout talks about problems your child has in the throat (pharynx) when they swallow, how we diagnose it and how we treat it. What is dysphagia? Dysphagia means difficulty swallowing. Food and drink can get stuck (dis-FAY-je-ya) in the esophagus or “go down the wrong pipe” to the lungs (called aspiration) instead of the stomach. It can also go into the voice box but not all the way into the lungs (called penetration). Epiglottis up for breathing Mouth Throat Liquid in throat (oral (pharyngeal cavity) space) Epiglottis down for eating and drinking Windpipe Liquid in Swallowing tube (Airway or airway (Esophagus) Trachea) Where does dysphagia Difficulty swallowing can happen in 3 places: in the mouth (oral happen? dysphagia), in the throat (pharyngeal dysphagia), and in the swallowing tube (esophageal dysphagia). This handout focuses on pharyngeal dysphagia. Why is pharyngeal When swallowing doesn’t happen the right way in the throat, it can dysphagia a problem? lead to liquid or food getting into the lungs (penetration and aspiration). What are the Food and drink going down the windpipe can damage the lungs. consequences of Some examples of damage are: getting liquid or food • Frequent or long-lasting colds or lung infections into the lungs • Frequent wheezing, coughing, or asthma symptoms (aspiration)? • Difficulty with feeding and growth • In the long-term, this can result in permanent damage to the lungs 1 of 3 To Learn More Free Interpreter Services • Otolaryngology • In the hospital, ask your nurse. 206-987-2105 • From outside the hospital, call the • Ask your child’s healthcare provider toll-free Family Interpreting Line, 1-866-583-1527. -

The Gastrointestinal System and the Elderly
2 The Gastrointestinal System and the Elderly Thomas W. Sheehy 2.1. Introduction Gastrointestinal diseases increase with age, and their clinical presenta tions are often confused by functional complaints and by pathophysio logic changes affecting the individual organs and the nervous system of the gastrointestinal tract. Hence, the statement that diseases of the aged are characterized by chronicity, duplicity, and multiplicity is most appro priate in regard to the gastrointestinal tract. Functional bowel distress represents the most common gastrointestinal disorder in the elderly. Indeed, over one-half of all their gastrointestinal complaints are of a functional nature. In view of the many stressful situations confronting elderly patients, such as loss of loved ones, the fears of helplessness, insolvency, ill health, and retirement, it is a marvel that more do not have functional complaints, become depressed, or overcompensate with alcohol. These, of course, make the diagnosis of organic complaints all the more difficult in the geriatric patient. In this chapter, we shall deal primarily with organic diseases afflicting the gastrointestinal tract of the elderly. To do otherwise would require the creation of a sizable textbook. THOMAS W. SHEEHY • Birmingham Veterans Administration Medical Center; and University of Alabama in Birmingham, School of Medicine, Birmingham, Alabama 35233. 63 S. R. Gambert (ed.), Contemporary Geriatric Medicine © Plenum Publishing Corporation 1988 64 THOMAS W. SHEEHY 2.1.1. Pathophysiologic Changes Age leads to general and specific changes in all the organs of the gastrointestinal tract'! Invariably, the teeth show evidence of wear, dis cloration, plaque, and caries. After age 70 years the majority of the elderly are edentulous, and this may lead to nutritional problems. -

Gastroenterology - Outpatient
Gastroenterology - Outpatient Goal Gastroenterology encompasses the evaluation and treatment of patients with disorders of the gastrointestinal tract, pancreas, biliary tract, and liver. It includes disorders of organs within the abdominal cavity and requires knowledge of the manifestations of gastrointestinal disorders in other organ systems, such as the skin. Additional areas include knowledge of nutrition and nutritional deficiencies, and screening and prevention, particularly for colorectal cancer. The general internist should have a wide range of competency in gastroenterology and should be able to provide primary and in some cases secondary preventive care, evaluate a broad array of gastrointestinal symptoms, and manage many gastrointestinal disorders. The general internist is not expected to perform most technical procedures with the important exception of flexible sigmoidoscopy. However, he or she must be familiar with the indications, contraindications, interpretation, and complications of these procedures. Lead Faculty Grace Elta, MD Objectives 1 0 Patient Care and Medical Knowledge 1 1 Dysphagia Differentiate oropharyngeal from esophageal Know the general approach to diagnosis Oropharyngeal dysphagia Use of barium esophagogram/swallowing study Use of endoscopy Use of ENT/speech pathology Know the general approach esophageal dysphagia Use of endoscopy Use of barium esophagogram Know causes of esophageal dysphagia Rings GERD Stricture Pill esophagitis Cancer Know when to include radiology, gastroenterology 1 2 Gastroesophageal