Download WAO White Book on Allergy
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

EAACI/ESCD Skin Allergy Meeting 2017 (SAM 2017)
Clin Transl Allergy 2017, 7(Suppl 4):47 DOI 10.1186/s13601-017-0184-5 Clinical and Translational Allergy MEETING ABSTRACTS Open Access EAACI/ESCD Skin Allergy Meeting 2017 (SAM 2017) Zurich, Switzerland. 27 – 29 April 2017 Published: 15 December 2017 Thursday, 27 April 2017 O02 Assessment of aggregate consumer exposure to isothiazolinones O01 via cosmetics and detergents Methylisothiazolinone contact allergy: a real outbreak Elena Garcia Hidalgo, Natalie Von Goetz, Konrad Hungerbühler Luis Amaral1, Emidio Silva2, Marcio Oliveira3, Ana Paula Cunha4 ETH Zürich, Zürich, Switzerland 1Serviço de Imunoalergologia, Centro Hospitalar de São João E.P.E., Porto, Correspondence: Elena Garcia Hidalgo ‑ [email protected] Portugal; 2Serviço de Medicina do Trabalho e Saúde Ocupacional, Centro Clinical and Translational Allergy 2017, 7(Supple 4):O02 Hospitalar do Baixo Vouga E.P.E., Aveiro, Portugal; 3Serviço de Saúde Ocu‑ pacional, Centro Hospitalar de São João E.P.E., Porto, Portugal; 4Serviço de Background: Isothiazoliones can cause allergic contact dermati- Dermatologia, Centro Hospitalar de São João E.P.E., Porto, Portugal tis and are present in a variety of consumer products, such as cos- Correspondence: Luis Amaral ‑ [email protected] metics, detergents and do-it-yourself products. Skin sensitization Clinical and Translational Allergy 2017, 7(Supple 4):O01 is induced following dermal exposure to a sensitizer in an amount exceeding the sensitization threshold. The critical determinant of Background: Methylisothiazolinone (MI) is used as a preservative in exposure for evaluating skin sensitization risks is dose per unit area occupational, domestic products and, since 2005, in cosmetics. It is a of exposed skin. -

Bee Venom Allergy in Beekeepers and Their Family Members Ulrich R
Bee venom allergy in beekeepers and their family members Ulrich R. Mu¨ller Purpose of review Introduction To analyze prevalence of allergic sting reactions, including Hymenoptera venom allergy is one of the major reasons the clinical and diagnostic features as well as management for anaphylaxis. Between 1961 and 2000, it caused 120 options in a population heavily exposed to honeybee stings fatalities in Switzerland – an average of three every year such as beekeepers and their family members. [1]. Extrapolated to Western Europe, this corresponds to Recent findings more than 150 fatal Hymenoptera sting reactions every The higher sting frequency is associated with an increased year in this region. Stings by honeybees and vespids are prevalence of allergic sting reactions. Major risk factors for most often responsible for such reactions. Beekeepers allergic sting reactions in beekepers are: fewer than 10 and their family members are heavily exposed to honey- annual stings, an atopic constitution and symptoms of bee stings and are thus at an especially high risk of upper respiratory allergy during work in the beehive. Bee becoming allergic, and therefore are an interesting popu- venom allergic beekeepers have higher levels of bee lation for the study of epidemiology and immunopatho- venom-specific IgG but lower skin sensitivity and bee genesis of venom allergy and the mechanism of its most venom-specific IgE than normally exposed bee venom effective treatment – venom immunotherapy. Finally, allergic patients. Safety of bee venom immunotherapy is owing to the high degree of exposure of this population, higher in beekeepers than in allergic controls, while efficacy indication and protocols for venom immunotherapy may of this treatment is similar in both groups. -

Urticaria from Wikipedia, the Free Encyclopedia Jump To: Navigation, Search "Hives" Redirects Here
Urticaria From Wikipedia, the free encyclopedia Jump to: navigation, search "Hives" redirects here. For other uses, see Hive. Urticaria Classification and external resourcesICD-10L50.ICD- 9708DiseasesDB13606MedlinePlus000845eMedicineemerg/628 MeSHD014581Urtic aria (or hives) is a skin condition, commonly caused by an allergic reaction, that is characterized by raised red skin wheals (welts). It is also known as nettle rash or uredo. Wheals from urticaria can appear anywhere on the body, including the face, lips, tongue, throat, and ears. The wheals may vary in size from about 5 mm (0.2 inches) in diameter to the size of a dinner plate; they typically itch severely, sting, or burn, and often have a pale border. Urticaria is generally caused by direct contact with an allergenic substance, or an immune response to food or some other allergen, but can also appear for other reasons, notably emotional stress. The rash can be triggered by quite innocent events, such as mere rubbing or exposure to cold. Contents [hide] * 1 Pathophysiology * 2 Differential diagnosis * 3 Types * 4 Related conditions * 5 Treatment and management o 5.1 Histamine antagonists o 5.2 Other o 5.3 Dietary * 6 See also * 7 References * 8 External links [edit] Pathophysiology Allergic urticaria on the shin induced by an antibiotic The skin lesions of urticarial disease are caused by an inflammatory reaction in the skin, causing leakage of capillaries in the dermis, and resulting in an edema which persists until the interstitial fluid is absorbed into the surrounding cells. Urticarial disease is thought to be caused by the release of histamine and other mediators of inflammation (cytokines) from cells in the skin. -

Hymenoptera Sting Challenge of 348 Patients Relation to Subsequent Field
Hymenoptera sting challenge of 348 patients: Relation to subsequent field stings Henk K. van Halteren, MD," Peter-Willem G. van der Linden, MD, PhD, b Sjaak A. Burgers, MD, PhD, c and Anton K. M. Bartelink, MD, PhD a Amersfoort, Haarlem, and Utrecht, The Netherlands' Background: Patients with a history of a serious anaphylactic reaction after a Hymenoptera sting are usually given venom immunotherapy. Because the natural history of Hymenoptera sting anaphylaxis is often of a declining severity, there is a chance of overtreatment. Objective: Identification of patients at risk for a future anaphylactic reaction may reduce the number of patients who need venom immunotherapy. Methods: We investigated the relation between the grade of hypersensitivity to an in-hospital sting challenge and the reaction to a subsequent accidental field sting. From 1982 through 1992, 348 patients" with mild or no symptoms after a sting challenge were not given venom immunotherapy. All patients were asked by letter whether they had experienced a subsequent field sting. In case of" a sting, the severity of the reaction was further evaluated. Results: Information could be obtained from 327patients: 129 had been re-stung, and 110 of them had only had a local reaction. Thirteen patients had experienced mild systemic symptoms, and six patients had experienced serious manifestations. In two of the latter group hypotension was observed. Conclusion: In 95% of patients with a previous anaphylactic reaction, the result of the in- hospital sting challenge provided a good prediction of tolerance to a subsequent Hymenoptera field sting. (J Allergy Clin Immunol 1996;97:1058-63.) Key words: Sting challenge, Hymenoptera, immunotherapy, anaphylccris Most stings by Hymenoptera species only lead to a local reaction: redness, swelling, itching, and Abbreviation used pain. -

Commonly Coded Conditions in Dermatology
2/11/2014 Commonly Coded Conditions in Dermatology Betty Hovey, CPC, CPC-H, CPB, CPMA, CPC-I, CPCD Director, ICD-10 Development and Training AAPC Commonly Coded Conditions in Dermatology No part of this presentation may be reproduced or transmitted in any form or by any means (graphically, electronically, or mechanically, including photocopying, recording, or taping) without the expressed written permission of AAPC. 2 Commonly Coded Conditions in Dermatology AGENDA • Dermatitis • Actinic and seborrheic keratosis • Acne • Ulcers • Psoriasis Commonly Coded Conditions in Dermatology 1 2/11/2014 Commonly Coded Conditions in Dermatology Dermatitis • Inflammation of the skin • Comes in different forms • We will discuss: – Atopic dermatitis – Seborrheic dermatitis – Contact dermatitis • NOTE: For code block L20-L30 ICD-10-CM uses the terms dermatitis and eczema synonymously and interchangeably. Commonly Coded Conditions in Dermatology Atopic dermatitis (AD) • Located in category L20: – L20.0 Besnier’s prurigo – L20.81 Atopic neurodermatitis – L20.82 Flexural eczema – L20.83 Infantile (acute) (chronic) eczema – L20.84 Intrinsic (allergic) eczema – L20.89 Other atopic dermatitis – L20.9 Atopic dermatitis, unspecified Commonly Coded Conditions in Dermatology 2 2/11/2014 Example • 7-year-old girl brought in for itchy, popular rash on the flexural surfaces of the neck, axillae, and elbows. No other family members with AD, but mother has asthma. Scratching of the lesions is worse at night. Patient with lichenification in left elbow area. Patient is diagnosed with flexural dermatitis. L20.82 Flexural eczema Z82.5 Family history of asthma and other chronic lower respiratory diseases Commonly Coded Conditions in Dermatology Seborrheic dermatitis • Located in category L21 L21.0 Seborrheic capitis L21.1 Seborrheic infantile L21.8 Other seborrheic dermatitis L21.9 Seborrheic dermatitis, unspecified Commonly Coded Conditions in Dermatology Example • A new mother brings her infant in because she is worried about a yellowish, crusty deposit on the baby’s scalp. -

Insect Sting Allergy
Insect Sting Allergy Dean Tey Paedi atric Alle rg i st & Immu n ol ogi st Monday 17 June 2010 Insect Sting Allergy 1. Eppgyidemiology 2. Aetiology (meet the insects) 3. Clinical presentation 4. Risk of future systemic reactions 5. Investigations 6. Management a) Prevention b) Local reactions c) Systemic reactions d) Venom immunotherapy Insect Sting Allergy 1. Eppgyidemiology 2. Aetiology (meet the insects) 3. Clinical presentation 4. Risk of future systemic reactions 5. Investigations 6. Management a) Prevention b) Local reactions c) Systemic reactions d) Venom immunotherapy Epidemiology • Large localised reaction – Frequency estimated to be 10% in adults1 • Systemic allergic reactions – Reported by up to 3% of adults2 – S%fSevere sting reactions in up to 1% of children3 1. Golden DBK. Immunol Allergy Clin N Am 2007;17:261-272 2. Golden et al. JAMA 1989;262:240-4. 3. Settipane et al. J Allergy 1972;50:146-50. Epidemiology • Admissions – In Australia, approximately 1200 admissions per year attributed towards hornet, wasp or bee stings (2002-2005) • Fatalities – In Australia, approximately 2 cases per year (20 cases between 1997 -2005). – In USA, >50 cases per year. 1. Bradley C. Australian Institute of Health and Welfare; 2008. Catalog no. INJCAT 110. 2. Liew et al; JACI 2009;123:434-42. 3. Barnard JH. JACI 1973;52:259-64. Liew et al. Anaphylaxis fatalities and admissions in Australia. JACI 2009;123:434-42. Liew et al. Anaphylaxis fatalities and admissions in Australia. JACI 2009;123:434-42. Liew et al. Anaphylaxis fatalities and admissions in Australia. JACI 2009;123:434-42. -

Urticaria: a Case Study IJHS 2021; 5(2): 242-245 Received: 22-01-2021 Accepted: 24-03-2021 Dr
International Journal of Homoeopathic Sciences 2021; 5(2): 242-245 E-ISSN: 2616-4493 P-ISSN: 2616-4485 www.homoeopathicjournal.com Urticaria: A case study IJHS 2021; 5(2): 242-245 Received: 22-01-2021 Accepted: 24-03-2021 Dr. T Surekha Dr. T Surekha Assistant Professor, DOI: https://doi.org/10.33545/26164485.2021.v5.i2d.390 Department of PSM MNR Homoeopathy Medical Abstract College & Hospital Urticaria (or hives) is a skin condition, commonly caused by an allergic reaction that is characterized Sangareddy, Telangana, India by raised red skin welts. It is also known as nettle rash. Hives can appear anywhere on the body, including the face, lips, tongue, throat, and ears. Rash may vary in size from about 5 mm (0.2 inches) in diameter to the size of a dinner plate; they typically itch severely, sting, or burn, and often have a pale border [1]. Keywords: urticaria, angioedema, hives, homoeopathy Introduction Urticaria is a disease characterized by erythematous, edematous, itchy and transient urticarial plaques and covering the skin and mucous membranes. Almost 8.8-20% of individuals in the community are experiencing urticaria once in their lifetime [2]. Many factors may be responsible in the etiology of the disease. Often, encountered factors include- Medication, food, Respiratory allergens and so on. Urticaria related to the drugs given intravenously will occur immediately. While the drugs generally cause acute urticaria, they may cause emergence or exacerbation of CSU [3]. Classification of Urticaria 1. Acute spontaneous urticaria - It lasts <6 weeks. 2. Chronic spontaneous urticaria (CSU) - It recurs at least twice a week and lasts >6 weeks. -

Insect Sting Allergy David F
Med Clin N Am 90 (2006) 211–232 Insect Sting Allergy David F. Graft, MDa,b,* aAsthma and Allergic Diseases, Park Nicollet Clinic, Minneapolis, MN, USA bDepartment of Pediatrics, University of Minnesota Medical School, Minneapolis, MN, USA The study of allergy to insect stings holds a unique position in the field of allergy, and because of the usually singular and notable times of exposure, it serves as a model for the development, natural history, and treatment of al- lergic phenomena. The death of King Menes of Egypt shortly after a wasp sting is often cited as one of the earliest historical examples of anaphylaxis [1]. Soon after the concepts of anaphylaxis were defined by Portier and Richert in 1902 [2], generalized reactions to insect stings were recognized as hypersensitivity phenomena [3]. Ten years later, Braun [4] described a typ- ical patient with insect sting sensitivity and his use of insect venom for diag- nosis and treatment. Although this initial treatment used the posterior one eighth inch of the insect to increase the yield of venom, that stipulation was later ignored and for decades, immunotherapy with whole-body extract was used for the treatment of patients with insect sting reaction [5]. In the 1950s and 1960s, events occurred that eventually led to the development of venom immunotherapy (VIT). Loveless and Fackler [6] reported the successful di- agnostic and therapeutic use of extracts of venom sacs. Bernton and Brown [7] and Schwartz [8] independently found that whole-body extract skin tests did not discriminate insect allergic patients from subjects with no history of generalized reactions. -

Insect Stings Is Systemic and Severe
Insect Sting Allergy – The Facts Anyone who is stung by a bee or wasp is likely to suffer a painful swelling at the site of the sting. For most people, the sting is not dangerous. Some people also experience an allergic reaction to the venom. For most of these people, the allergic reaction is mild resulting in swelling at the site of the sting. But for a small minority, an allergic reaction to an insect sting can be systemic – that is, affecting parts of the body away from the site of the sting. Systemic allergic reactions are sometimes severe and potentially life-threatening – a condition known as anaphylaxis. If you are in this category, you may find the prospect of being stung very frightening but be assured that there are steps you can take to reduce the risk to yourself. This involves getting medical advice, carrying prescribed medication at all times, and taking precautions to avoid being stung. This Factsheet aims to answer some of the questions you may have if your allergy to insect stings is systemic and severe. Our intention is to help you to minimise risks. The information in this Factsheet includes brief medical references, which are given in brackets. Full references to these documents are listed at the end of the Factsheet. Who is at risk? Anyone can become allergic to an insect sting. People who have other allergies, such as hayfever or food allergies, are not at increased risk of having a severe allergic reaction to an insect sting (Krishna et al. 2011). You are more at risk of severe allergic reactions to insect stings if you have frequent or multiple stings. -

Indian Journal of Dermatology, Venereology & Leprology
Indian Journal of Dermatology, Venereology & Leprology Journal indexed with SCI-E, PubMed, and EMBASE | | VVolo l 7744 IIssues s u e 2 MMar-Apra r- A p r 220080 0 8 C O N T E N T S EDITORIAL Management of autoimmune urticaria Arun C. Inamadar, Aparna Palit .................................................................................................................................. 89 VIEW POINT Cosmetic dermatology versus cosmetology: A misnomer in need of urgent correction Shyam B. Verma, Zoe D. Draelos ................................................................................................................................ 92 REVIEW ARTICLE Psoriasiform dermatoses Virendra N. Sehgal, Sunil Dogra, Govind Srivastava, Ashok K. Aggarwal ............................................................. 94 ORIGINAL ARTICLES A study of allergen-specific IgE antibodies in Indian patients of atopic dermatitis V. K. Somani .................................................................................................................................................................. 100 Chronic idiopathic urticaria: Comparison of clinical features with positive autologous serum skin test George Mamatha, C. Balachandran, Prabhu Smitha ................................................................................................ 105 Autologous serum therapy in chronic urticaria: Old wine in a new bottle A. K. Bajaj, Abir Saraswat, Amitabh Upadhyay, Rajetha Damisetty, Sandipan Dhar ............................................ 109 Use of patch -

Cost, Utilization, and Patterns of Medication Use Associated with Chronic Idiopathic Urticaria James L
Ann Allergy Asthma Immunol 108 (2012) 98–102 Contents lists available at SciVerse ScienceDirect Cost, utilization, and patterns of medication use associated with chronic idiopathic urticaria James L. Zazzali, PhD, MPH *; Michael S. Broder, MD, MSHS †; Eunice Chang, PhD †; Melvin W. Chiu, MD ‡; and Daniel J. Hogan, MD § * Genentech, Inc., South San Francisco, California † Partnership for Health Analytic Research, Beverly Hills, California ‡ Division of Dermatology, Department of Medicine, David Geffen School of Medicine at the University of California, Los Angeles § Clinical Professor of Internal Medicine (Dermatology), NOVA Southeastern University College of Osteopathic Medicine, Fort Lauderdale, Florida ARTICLE INFO ABSTRACT Article history: Background: The literature on chronic idiopathic urticaria (CIU) lacks large-scale population-based studies. Received for publication June 30, 2011. Objective: To characterize an insured population with CIU, including their demographic characteristics and Received in revised form October 31, 2011. comorbidities. Accepted for publication October 31, 2011. Methods: We conducted a cross-sectional analysis using insurance claims. We included patients with 1 outpatient claim with an International Classification of Diseases, 9th Edition, Clinical Modification (ICD-9-CM) code for idiopathic, other specified, or unspecified urticaria (ICD-9-CM 708.1, 708.8, or 708.9) and either (1) another of these claims 6 or more weeks later; (2) a claim for angioedema (ICD-9-CM 995.1) 6 or more weeks from the urticaria diagnosis; or (3) overlapping claims for 2 prescription medications commonly used for CIU. Results: We identified 6,019 patients who had claims consistent with CIU. The mean age was 36 years. Fifty-six percent of patients had primary care physicians as their usual source of care, 14% had allergists, and 5% had dermatologists. -
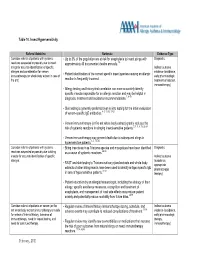
Table 10 Insect Hypersensitivity
Table 10. Insect Hypersensitivity Referral Guideline Rationale Evidence Type Consider referral of patients with systemic • Up to 3% of the population are at risk for anaphylaxis to insect stings with Diagnostic reactions suspected or possibly due to insect approximately 40 documented deaths annually. 1-8 stings for accurate identification of specific Indirect outcome allergen and consideration for venom • evidence (avoidance, immunotherapy (or whole body extract in case of Patient identification of the correct specific insect species causing an allergic early pharmacologic fire ant). reaction is frequently incorrect. treatment of reaction, immunotherapy) • Allergy testing and history-test correlation can more accurately identify specific insects responsible for an allergic reaction and may be helpful in diagnosis, treatment and avoidance recommendations.7, 9-18 • Skin testing is generally preferred over in vitro testing for the initial evaluation of venom-specific IgE antibodies. 4, 5, 13, 15,17-21 • Venom immunotherapy (or fire ant whole body extract) greatly reduces the risk of systemic reactions in stinging insect-sensitive patients. 2, 3, 5, 8, 15, 22-24 • Venom immunotherapy may prevent death due to subsequent stings in hypersensitive patients. 3, 5, 15, 25 Consider referral of patients with systemic • Biting insects such as Triatoma species and mosquitoes have been identified Diagnostic reactions suspected or possibly due to biting as a cause of systemic reactions. 26-30 insects for accurate identification of specific Indirect outcome allergen. • (avoidance, RAST and skin testing to Triatoma salivary gland extracts and whole body appropriate extracts of other biting insects have been used to identify antigen specific IgE 31-41 pharmacologic in sera of hypersensitive patients.