Topical Serum for Treatment of Keratomalacia
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Bouncebacks the Case of a 10-Year-Old Male with Eye Pain
Bouncebacks The Case of a 10-Year-Old Male with Eye Pain Bouncebacks appears semimonthly in JUCM. Case presentations on each patient, along with case-by-case risk management commentary by Gregory L. Henry, past president of The American College of Emergency Physicians, and discussions by other nationally recognized experts are detailed in the book Bouncebacks! Emergency Department Cases: ED returns (2006, Anadem Publishing, www.anadem.com).] Also avail- able at www.amazon.com and www.acep.org. Ryan Longstreth, MD, FACEP and Michael B. Weinstock, MD his article is the third in a series scheduled returns. Tin which we will sequentially Other than these medical errors, dysp- answer the following questions: nea and advanced age were the two most I. What is the incidence of common factors associated with an un- bouncebacks? scheduled return visit. II. What is the incidence Another study looking at this is- of bounceback ad- sue was published in 1990 in missions? the Annals of Emergency Medi- III. What is the inci- cine by Pierce et al. During the dence of death in three-month study period, patients recently there were 17,214 new visits to discharged from the their ED with 569 unscheduled ED? returns (defined as ED return IV. What percent of within 48 hours), equating bouncebacks occur to a bounceback rate of just because of medical over 3%. errors? The researchers con- V. How can we use this © Barton Stabler / Images.com cluded that over 18% were information to im- due to physician-related prove patient safety? factors (e.g., misdiagnosis, This month, we will discuss treatment error, inappropriate Question IV: What percent of discharge on initial visit, radiol- bouncebacks occur because of medical errors? ogy over-reads, or lack of outpa- A 2006 case control study performed by Nunez tient analgesics when indicated). -

CHQ-GDL-01074 Acute Management of Open Globe Injuries
Acute management of Open Globe Injuries Document ID CHQ-GDL-01074 Version no. 2.0 Approval date 14/05/2020 Executive sponsor Executive Director Medical Services Effective date 14/05/2020 Author/custodian Director Infection Management and Prevention service, Review date 14/05/2022 Immunology and Rheumatology Supersedes 1.0 Applicable to All Children’s Health Queensland (CHQ) staff Authorisation Executive Director Clinical Services (QCH) Purpose This evidence-based guideline provides clinical practice advice for clinicians for the acute management of children with open globe injuries. A paediatric ophthalmology team must be actively involved in the management of all patients presenting with this condition. Scope This guideline applies to all Children’s Health Queensland (CHQ) Staff treating a child presenting for the management of open globe injury. Related documents • CHQ-GDL-01202 CHQ Paediatric Antibiocard: Empirical Antibiotic Guidelines • CHQ-PROC-01035 Antimicrobial Restrictions • CHQ Antimicrobial Restriction list • CHQ-GDL-01023 Tetanus Prophylaxis in Wound Management CHQ-GDL-01074- Acute management of Open Globe Injuries - 1 - Guideline Introduction Ocular trauma is an important cause of eye morbidity and is a leading cause of non-congenital mono-ocular blindness among children.1 A quarter of a million children present each year with serious ocular trauma. The vast majority of these are preventable.2 Open globe injuries are injuries where the cornea and/or sclera are breached and there is a full-thickness wound of the eye wall.3 It can be further delineated into globe rupture from blunt trauma and lacerations from sharp objects. When a large blunt object impacts onto the eye, there is an instant increase in intraocular pressure and the eye wall yields at its weakest point leading to tissue prolapse.4 Open globe lacerations are caused by sharp objects or projectiles and subdivided into either penetrating or perforating injuries. -

Two Cases of Endogenous Endophthalmitis That Progressed To
rine to more distal vessels may have led to vasoconstric- References tion and subsequent vasospasm. In conclusion, epinephrine can lead to OAO following 1. Niemi G. Advantages and disadvantages of adrenaline in accidental intra-arterial injection of subcutaneously ad- regional anaesthesia. Best Pract Res Clin Anaesthesiol ministered local anesthetics. Hence, physicians should 2005;19:229-45. carefully administer local anesthesia while considering the 2. Park KH, Kim YK, Woo SJ, et al. Iatrogenic occlusion of possibility that such a complication may occur. the ophthalmic artery after cosmetic facial filler injections: a national survey by the Korean Retina Society. JAMA Byung Gil Moon Ophthalmol 2014;132:714-23. Retina Center, Department of Ophthalmology, HanGil Eye 3. Lazzeri D, Agostini T, Figus M, et al. Blindness following Hospital, Incheon, Korea cosmetic injections of the face. Plast Reconstr Surg 2012;129:995-1012. June-Gone Kim 4. Savino PJ, Burde RM, Mills RP. Visual loss following intra- Department of Ophthalmology, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea nasal anesthetic injection. J Clin Neuroophthalmol E-mail: [email protected] 1990;10:140-4. 5. Webber B, Orlansky H, Lipton C, Stevens M. Complica- tions of an intra-arterial injection from an inferior alveolar Conflict of Interest nerve block. J Am Dent Assoc 2001;132:1702- 4. No potential conflict of interest relevant to this article was reported. Korean J Ophthalmol 2017;31(3):279-281 litus presented with blurred vision of the right eye for 10 https://doi.org/10.3341/kjo.2017.0002 days. Abdominal and chest computed tomography showed an emphysematous prostatic abscess with multiple pulmo- nary lesions. -

JMSCR Vol||08||Issue||02||Page 208-210||February 2020
JMSCR Vol||08||Issue||02||Page 208-210||February 2020 http://jmscr.igmpublication.org/home/ ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v8i2.40 Keratomalacia - A Case Report Authors Deepthi Pullepu1*, Deepthi Janga2, V Murali Krishna3 *Corresponding Author Deepthi Pullepu Department of Ophthalmology, Rangaraya Medical College, Kakinada, Andhra Pradesh, India Abstract Xerophthalmia refers to an ocular condition of destructive dryness of conjunctiva and cornea caused due to severe vitamin A deficiency. Usually affects infants, children and women of reproductive age group. It is estimated to affect about one-third of children under the age of five around the world. Keratomalacia means dry and cloudy cornea which melts and perforates, caused due to severe vitamin A deficiency. Here we describe a case of 21 year old female with neurofibromatosis type 1 presenting with keratomalacia. Keywords: Vitamin A deficiency, Xerophthalmia, Keratomalacia. Introduction blindness is a significant contributor Vitamin A is essential for the functioning of the In India, it is estimated that there are immune system, healthy growth and development approximately 6.8 million people who have vision of body and is usually acquired through diet. less than 6/60 in at least one eye due to corneal Globally, 190 million children under five years of diseases; of these, about a million have bilateral age are affected by vitamin A deficiency involvement. They suffer from an increased risk of visual Corneal blindness resulting due to this disease can impairment, illness and death from childhood be completely prevented by institution of effective infections such as measles and those causing preventive or prophylactic measures at the diarrhoea community level. -
Globe Rupture and Protrusion of Intraocular Contents from Fall in Elderly Patient
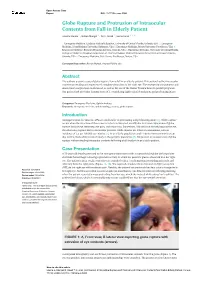
Open Access Case Report DOI: 10.7759/cureus.5988 Globe Rupture and Protrusion of Intraocular Contents from Fall in Elderly Patient Andrew Hanna 1 , Rohan Mangal 2 , Tej G. Stead 3 , Latha Ganti 4, 5, 6 1. Emergency Medicine, Graduate Medical Education, University of Central Florida, Orlando, USA 2. Emergency Medicine, Johns Hopkins University, Baltimore, USA 3. Emergency Medicine, Brown University, Providence, USA 4. Emergency Medicine, Envision Physician Services, Orlando, USA 5. Emergency Medicine, University of Central Florida College of Medicine / Hospital Corporation of America Graduate Medical Education Consortium of Greater Orlando, Orlando, USA 6. Emergency Medicine, Polk County Fire Rescue, Bartow, USA Corresponding author: Rohan Mangal, [email protected] Abstract The authors present a case of globe rupture from a fall in an elderly patient. This patient had her intraocular contents protruding and experienced complete vision loss in her right eye. The emergency management and downstream surgical care is discussed, as well as the use of the Ocular Trauma Score to predict prognosis. Our patient had an Ocular Trauma Score of 1, considering right retinal detachment and perforating injury. Categories: Emergency Medicine, Ophthalmology Keywords: emergency medicine, ophthalmology, trauma, globe rupture Introduction Amongst serious eye injuries, 40% are attributable to penetrating and perforating injury [1]. Globe rupture occurs when the structure of the cornea or sclera is disrupted, usually due to trauma. Symptoms of globe rupture include eye deformity, eye pain, and vision loss. Sometimes, if blunt force directly impacts the eye, the sclera may rupture due to intraocular pressure. Globe injuries are relatively uncommon, with an incidence of 3.5 per 100,000 eye injuries [2]. -

Acute Management of Penetrating Eye Injury and Ruptured Globe
Acute management of penetrating eye injury and ruptured globe Disclaimer SEE ALSO: Endophthalmitis, Hyphaema, Peri- and post-operative Management of Penetrating Eye Injury and Ruptured Globe, Procedure for Management of Eye Trauma DESCRIPTION – The immediate management of penetrating eye injury (PEI), with or without intra-ocular foreign body (IOFB), and ruptured globe to maximise outcome. HOW TO ASSESS Red Flags: Immediate Advanced Trauma Life Support (ATLS) assessment: Airway, Breathing, Circulation, Disability, Exposure (ABCDE) Establish mechanism of injury to exclude other injuries which may require management at a general hospital, e.g. cervical spine, head injury Open globe should be examined carefully to avoid extrusion of intraocular contents Consider occult injury if mechanism suggestive Shield at all times (do not pad) Early referral for pre-anaesthetic assessment and medical review (if needed), to assess pre-existing or new medical issues and the patient’s suitability for management at RVEEH. Preoperative bloods, ECG and imaging as indicated. EXPECTED PATIENT Refer to and complete the ‘Emergency Expect Form’ (MR 37) in the Emergency Department. Make sure patient’s contact details (mobile) are recorded. Do not accept patients who have injuries other than ocular i.e. multi-trauma or who are medically unstable. Children under the age of 6 months should be referred directly to the Royal Children’s Hospital. Children aged from 6 months to 2 years with significant co-morbidities may not be appropriate to be managed at RVEEH. 1 Penetrating eye injury and ruptured globe CPG v4 19092017 All paediatric patients which may need referral to RCH, must be discussed with RCH Ophthalmology registrar or Consultant PRIOR to referral in order to confirm specialty coverage and operating theatre availability should surgery be required. -

Involvement of the Eye in Protein Malnutrition * -303
Bull. Org. mond. Sante 1958, 19, 303-314 Bull. Wld Hith Org. INVOLVEMENT OF THE EYE IN PROTEIN MALNUTRITION * D. S. McLAREN, M.D., Ph.D., D.T.M. & H. Medical Research Officer, East African Institute for Medical Research, Mwanza, Tanganyika Formerly at the MRC Human Nutrition Research Unit, National Institute for Medical Research, London SYNOPSIS An extensive review of the literature on protein malnutrition, with special reference to the frequency of involvement of the eyes, has been made by the author. Consideration of accounts from all parts of the world and in many different languages, including early as well as more recent descriptions of the syndrome, indicates that this important complication has not received sufficient attention hitherto. The evidence available suggests that it is nearly always an accompanying deficiency of vitamin A that is responsible. Less commonly reported-and producing less severe effects-is deficiency of the B-complex vitamins, and there is no clear evidence to date that protein deficiency itself damages the eyes in these cases. The ways in which protein lack might interfere with various aspects of vitamin-A metabolism are discussed, but it is pointed out that their actual significance in human disease is not yet known. A low dietary intake of vitamin A is regarded by the author as being the prime factor in the causation of eye complications, and attention is drawn to the necessity to correct this as part of any prophylactic or therapeutic programme aimed primarily at combat- ing protein malnutrition. The syndrome known by such various names as kwashiorkor, nutritional oedema syndrome, sindrome pluricarencial, and many others (Trowell, Davies & Dean, 1954), and characterized chiefly by a dietary deficiency ofprotein, has been reported as occurring amongst most of the malnourished communities of the world. -

Eleventh Edition
SUPPLEMENT TO April 15, 2009 A JOBSON PUBLICATION www.revoptom.com Eleventh Edition Joseph W. Sowka, O.D., FAAO, Dipl. Andrew S. Gurwood, O.D., FAAO, Dipl. Alan G. Kabat, O.D., FAAO Supported by an unrestricted grant from Alcon, Inc. 001_ro0409_handbook 4/2/09 9:42 AM Page 4 TABLE OF CONTENTS Eyelids & Adnexa Conjunctiva & Sclera Cornea Uvea & Glaucoma Viitreous & Retiina Neuro-Ophthalmic Disease Oculosystemic Disease EYELIDS & ADNEXA VITREOUS & RETINA Blow-Out Fracture................................................ 6 Asteroid Hyalosis ................................................33 Acquired Ptosis ................................................... 7 Retinal Arterial Macroaneurysm............................34 Acquired Entropion ............................................. 9 Retinal Emboli.....................................................36 Verruca & Papilloma............................................11 Hypertensive Retinopathy.....................................37 Idiopathic Juxtafoveal Retinal Telangiectasia...........39 CONJUNCTIVA & SCLERA Ocular Ischemic Syndrome...................................40 Scleral Melt ........................................................13 Retinal Artery Occlusion ......................................42 Giant Papillary Conjunctivitis................................14 Conjunctival Lymphoma .......................................15 NEURO-OPHTHALMIC DISEASE Blue Sclera .........................................................17 Dorsal Midbrain Syndrome ..................................45 -

Keratoconjunctivitis Sicca (KCS)
Vision Matters A Focus on Keratoconjunctivitis Sicca (KCS) Brought to you by Bayer Keratoconjunctivitis sicca (KCS): The normal tear film explained The normal tear film (also called Ocular conditions account for about ten percent of canine consultations in first opinion Recent research into tear film dynamics 1 practice ; this means if twenty dogs come into your surgery in a day, two of them are likely the precorneal tear film) consists suggests that the three component to be presenting with an eye condition. of three major components: layers are not well defined, and that there is a possible fourth layer of glycocalyx With owners increasingly doing their own research before visiting their vet, it is vital to have in-depth that extends from the corneal epithelium.5,6 knowledge of commonly seen conditions. This report focuses on keratoconjunctivitis sicca (KCS), Mucous layer – produced by conjunctival also known as dry eye, a condition where early recognition can have a significant impact on prognosis. goblet cells, and also by the epithelial The aqueous layer of the tear film is 98.2% water cells of the cornea and conjunctiva “and 1.8% solids, including immunoglobulins“ (IgA, IgG, IgM), lysozyme, lactoferrin, Aqueous layer – produced by the lacrimal 7,8 and nictitans glands transferrin, ceruloplasmin and glycoproteins. Without a normal aqueous layer, the corneal Lipid layer – produced by meibomian surface is at risk from bacterial infection, glands in the eyelid margin hypoxia, toxic tissue metabolite accumulation and excessive degradation. 5% 20% 46% The tear film plays a vital role 46% of dog owners in maintaining ocular health: ...and up to 20% of in a recent survey Dry eye affects predisposed breeds3 were not aware that • Lubricates the cornea, 2 nearly 5% of all dogs their pet could suffer eyelids and conjunctiva from dry eye4 • Provides oxygen and nutrients (e.g. -

Clinical Case Revista Colombiana De Ciencias Pecuarias
Estrada RD et al Melting ulcer in a colt 31 Clinical case Revista Colombiana de Ciencias Pecuarias Melting ulcer in a colt: clinical management and evolution ¤ Úlcera fundente en un potro: manejo clínico y evolución Úlcera colagenolítica em um potro: manejo clínico e evolução Rubén D Estrada 1, MV; Susana Penagos 2, est MV; Elizabeth Viera 2, est MV; Paula A Angulo 2, est MV; Maria P Arias 2*, MV, MS, PhD. 1MV Actividad independiente 2Facultad de Medicina Veterinaria y Zootecnia, Universidad CES, AA 054591, Medellín, Colombia (Received: June 1, 2012; accepted: November 19, 2012) Summary Anamnesis : a colt showing a whitish coloration accompanied by abundant secretion on the left eye was examined. Clinical and laboratory findings: at ophthalmological examination, signs of melting ulcer were observed. Culture isolation revealed positive growing of Flavobacterium sp. and Gram-negative rods. Treatment approach : several keratectomies and tarsorrhaphies, as well as exhaustive antiproteinases, anti- inflammatory, and antibiotic treatments, were conducted. Treatment focused on reducing inflammatory response, eliminating infective organisms, and promoting epithelial healing. Colt showed complete recovery of vision after 3 months. Conclusions: clinical management of melting ulcer implies exhaustive, though unexpensive, treatment. Key words: cornea, keratectomy, keratomalacia, ophthalmology, tarsorrhaphy Resumen Anamnesis : se examinó un potro que presentó una coloración blanquecina acompañada de abundante secreción en el ojo izquierdo. Hallazgos clínicos y de laboratorio : al examen oftalmológico se observaron signos de ulcera fundente. El aislamiento por cultivo mostró crecimiento de Flavobacterium sp. y cocos Gram negativos. Abordaje terapéutico : se realizaron varias queratectomías y tarsorrafias, además de un tratamiento exhaustivo con antiproteinasas, antiinflamatorios y antibióticos enfocado a reducir la respuesta inflamatoria, eliminar los microorganismos infecciosos y promover la cicatrización epitelial. -

Bilateral Keratomalacia Secondary to Diet Induced Vitamin a Deficiency in an Ethiopian Young Woman: a Case Report
Bilateral Keratomalacia… Kumale T. et al. 295 CASE REPORT Bilateral Keratomalacia Secondary to Diet Induced Vitamin A Deficiency in an Ethiopian Young woman: A Case Report Kumale Tolesa Daba1*, Dagmawit Kifle1, Jafer Kedir Ababora1 ABSTRACT OPEN ACCESS BACKGROUND: Diet induced vitamin A deficiency is less Citation: Kumale Tolesa Daba, Dagmawit commonly seen in otherwise healthy adults, due to large store of Kifle, Jafer Kedir Ababora. Bilateral vitamin A in the body. Night blindness is the commonest Keratomalacia Secondary to Diet Induced Vitamin A Deficiency in an Ethiopian manifestation of vitamin A deficiency in adults, whereas Young woman: A Case Report. Ethiop J Keratomalacia is a rare manifestation. Health Sci. 2018;29(2):295 doi:http://dx.doi.org/10.4314/ ejhs. v29i2.18 CASE REPORT: A 27 years old Ethiopian woman came to Jimma Received: June 22, 2018 University Department of Ohthalmology with a compliant of Accepted: October 27, 2018 protrusion of the globe content of both eyes within a week, after Published: March 1, 2019 Copyright: © 2019 Kumale Tolosa Daba, having redness and fear of light of both eyes for 2 months. She was et al. This is an open access article a mother of twins and had low socioeconomic status. On general distributed under the terms of the Creative examination, she was cachectic with enlarged parotid glands. On Commons Attribution License, which permits unrestricted use, distribution, and ocular examination, she was bilaterally blind and had dry ocular reproduction in any medium, provided the surface. There was bilaterally melted cornea with prolapsed uveal original author and source are credited. -

Traumatic Keratoplasty Rupture Resulting from Continuous Positive Airway Pressure Mask
CASE REPORT Traumatic Keratoplasty Rupture Resulting From Continuous Positive Airway Pressure Mask Miltiadis Fiorentzis, MD, Berthold Seitz, MD, and Arne Viestenz, MD We report an unusual case of traumatic wound Purpose: To report a rare case of traumatic wound dehiscence dehiscence due to a dislocation of a continuous positive caused by the use of a continuous positive airway pressure (CPAP) airway pressure (CPAP) mask during sleep after PKP. To the mask in a patient with chronic obstructive pulmonary disease best of our knowledge, this is the first report of this unusual (COPD) after penetrating keratoplasty (PKP). graft separation cause. Methods: Observational case report. CASE REPORT Case report: A 55-year-old man who was treated with uncompli- cated PKP due to pellucid marginal corneal degeneration in the right A 55-year-old man underwent an excimer laser-assisted PKP eye 9 months earlier presented to the emergency department after because of pellucid marginal corneal degeneration in the right eye. The postoperative course was uncomplicated (Fig. 1A). His medical a globe rupture caused by dislocation of his CPAP mask during history revealed chronic obstructive pulmonary disease (COPD), sleep. The best-corrected visual acuity (BCVA) was light perception treated with a CPAP mask. Three months after surgery and under in the right eye. The corneal graft was dehisced from 12 over 3 to 6 treatment with topical steroids 3 times a day, the BCVA was 20/32, o’clock (180 degrees) with interruption of the double running the corneal astigmatism approximately 1.8 diopters, and the central corneal sutures and nasal iris as well as vitreous incarceration.