Globin Variants Modify Hematologic and Other Clinical Phenotypes in Sickle Cell Trait and Disease
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Supporting Information
Supporting Information Biagioli et al. 10.1073/pnas.0813216106 SI Text and the procedure was repeated twice. Single cells were then RNA Isolation, Reverse Transcription, qPCR, Cloning, and Sequencing. resuspended in panning buffer and incubated on lectin-coated RNA was extracted from cell lines and blood by using TRIzol panning plates for 15 min at room temperature. Nonadherent reagent (Invitrogen) and following vendor instructions. cells were transferred to the next panning plate (four pannings, RNA was extracted from LCM- or FACS-purified cells with an 15 min each). Then, nonadherent cells were collected, centri- Absolutely RNA Nanoprep Kit (Stratagene). Single-strand fuged, and resuspended in serum-free neuronal medium or PBS. cDNA was obtained from purified RNA by using the iSCRIPT A similar procedure was also followed for the dissociation of cDNA Synhesis Kit (Bio-Rad) according to the manufacturer’s cortical and hippocampal astrocytes and oligodendrocytes. instructions. Quantitative RT-PCR was performed by using A cell strainer with 70-m nylon mesh was used to obtain a SYBER-Green PCR Master Mix and an iQ5 Real-Time PCR single-cell suspension (BD Falcon) before sorting. 7-AAD Detection System (Bio-Rad). (Beckman–Coulter) was added to the cell suspension to exclude Quantitative RT-PCR was performed with an iCycler IQ dead cells. A high-speed cell sorter (MoFlo) was used to sort (Bio-Rad); -actin was used as an endogenous control to nor- subpopulation of cells expressing GFP. Sorting parameters used malize the expression level of target genes. Primers were chosen for the three different populations are visualized in Fig. -
Technical Note, Appendix: an Analysis of Blood Processing Methods to Prepare Samples for Genechip® Expression Profiling (Pdf, 1
Appendix 1: Signature genes for different blood cell types. Blood Cell Type Source Probe Set Description Symbol Blood Cell Type Source Probe Set Description Symbol Fraction ID Fraction ID Mono- Lympho- GSK 203547_at CD4 antigen (p55) CD4 Whitney et al. 209813_x_at T cell receptor TRG nuclear cytes gamma locus cells Whitney et al. 209995_s_at T-cell leukemia/ TCL1A Whitney et al. 203104_at colony stimulating CSF1R lymphoma 1A factor 1 receptor, Whitney et al. 210164_at granzyme B GZMB formerly McDonough (granzyme 2, feline sarcoma viral cytotoxic T-lymphocyte- (v-fms) oncogene associated serine homolog esterase 1) Whitney et al. 203290_at major histocompatibility HLA-DQA1 Whitney et al. 210321_at similar to granzyme B CTLA1 complex, class II, (granzyme 2, cytotoxic DQ alpha 1 T-lymphocyte-associated Whitney et al. 203413_at NEL-like 2 (chicken) NELL2 serine esterase 1) Whitney et al. 203828_s_at natural killer cell NK4 (H. sapiens) transcript 4 Whitney et al. 212827_at immunoglobulin heavy IGHM Whitney et al. 203932_at major histocompatibility HLA-DMB constant mu complex, class II, Whitney et al. 212998_x_at major histocompatibility HLA-DQB1 DM beta complex, class II, Whitney et al. 204655_at chemokine (C-C motif) CCL5 DQ beta 1 ligand 5 Whitney et al. 212999_x_at major histocompatibility HLA-DQB Whitney et al. 204661_at CDW52 antigen CDW52 complex, class II, (CAMPATH-1 antigen) DQ beta 1 Whitney et al. 205049_s_at CD79A antigen CD79A Whitney et al. 213193_x_at T cell receptor beta locus TRB (immunoglobulin- Whitney et al. 213425_at Homo sapiens cDNA associated alpha) FLJ11441 fis, clone Whitney et al. 205291_at interleukin 2 receptor, IL2RB HEMBA1001323, beta mRNA sequence Whitney et al. -

Recombinant Human Hemoglobin Subunit Theta-1/HBQ1 (N-6His)
9853 Pacific Heights Blvd. Suite D. San Diego, CA 92121, USA Tel: 858-263-4982 Email: [email protected] 32-8592: Recombinant Human Hemoglobin Subunit theta-1/HBQ1 (N-6His) Gene : HBQ1 Gene ID : 3049 Uniprot ID : P09105 Description Source: E.coli. MW :17.7kD. Recombinant Human Hemoglobin subunit theta-1 is produced by our E.coli expression system and the target gene encoding Met1-Arg142 is expressed with a 6His tag at the N-terminus. Hemoglobin subunit theta-1 is a protein that in humans is encoded by the HBQ1 gene. Theta-globin mRNA is originally found in human fetal erythroid tissue but not in adult erythroid or other nonerythroid tissue. Theta-1 is a member of the human alpha-globin gene cluster that includes five functional genes and two pseudogenes. Research supports a transcriptionally active role for the gene and a functional role for the peptide in specific cells, possibly those of early erythroid tissue. Hemoglobin has a quaternary structure characteristically composed of many multi- subunit globular proteins. Most of the amino acids in hemoglobin form alpha helices, connected by short non-helical segments. Hydrogen bonds stabilize the helical sections inside this protein, causing attractions within the molecule, folding each polypeptide chain into a specific shape. Hemoglobin's quaternary structure comes from its four subunits in roughly a tetrahedral arrangement. Product Info Amount : 10 µg / 50 µg Content : Lyophilized from a 0.2 µm filtered solution of 20mM PB, 150mM NaCl, pH 7.0. Lyophilized protein should be stored at -20°C, though stable at room temperature for 3 weeks. -

Simultaneous Detection of Target Cnvs and Snvs of Thalassemia by Multiplex PCR and Next‑Generation Sequencing
MOLECULAR MEDICINE REPORTS 19: 2837-2848, 2019 Simultaneous detection of target CNVs and SNVs of thalassemia by multiplex PCR and next‑generation sequencing DONG-MEI FAN1*, XU YANG2*, LI-MIN HUANG1, GUO-JUN OUYANG3, XUE-XI YANG1 and MING LI1 1Institute of Antibody Engineering, School of Laboratory Medicine and Biotechnology, Southern Medical University, Guangzhou, Guangdong 510515; 2Clinical Innovation and Research Center, Shenzhen Hospital of Southern Medical University, Shenzhen, Guangdong 518110; 3Guangzhou Darui Biotechnology Co., Ltd., Guangzhou, Guangdong 510663, P.R. China Received May 16, 2018; Accepted December 3, 2018 DOI: 10.3892/mmr.2019.9896 Abstract. Thalassemia is caused by complex mechanisms, Introduction including copy number variants (CNVs) and single nucleotide variants (SNVs). The CNV types of α-thalassemia are typi- Thalassemia is caused by copy number variants (CNVs) and cally detected by gap-polymerase chain reaction (PCR). The single nucleotide variants (SNVs) in the α-globin (HBA) or SNV types are detected by Sanger sequencing. In the present β-globin (HBB) genes that result in the absence or lack of α- or study, a novel method was developed that simultaneously β-globin chains, and ultimately hemolytic anemia. It is esti- detects CNVs and SNVs by multiplex PCR and next-genera- mated that ~7% of the world population carries the gene for the tion sequencing (NGS). To detect CNVs, 33 normal samples disease (1), and the birth rate of children with hemoglobin (Hb) were used as a cluster of control values to build a baseline, disorders is ≥2.4% per year (2). Thalassemia occurs most in the and the A, B, C, and D ratios were developed to evaluate-SEA, Mediterranean region, East South Asia, and the subcontinents -α4.2, -α3.7, and compound or homozygous CNVs, respectively. -
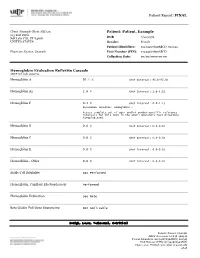

Normal, C=Critical
Patient Report |FINAL Client: Example Client ABC123 Patient: Patient, Example 123 Test Drive Salt Lake City, UT 84108 DOB 7/22/1970 UNITED STATES Gender: Female Patient Identifiers: 01234567890ABCD, 012345 Physician: Doctor, Example Visit Number (FIN): 01234567890ABCD Collection Date: 00/00/0000 00:00 Hemoglobin Evaluation Reflexive Cascade ARUP test code 2005792 Hemoglobin A 97.1 % (Ref Interval: 95.0-97.9) Hemoglobin A2 2.6 % (Ref Interval: 2.0-3.5) Hemoglobin F 0.3 % (Ref Interval: 0.0-2.1) REFERENCE INTERVAL: Hemoglobin F Access complete set of age- and/or gender-specific reference intervals for this test in the ARUP Laboratory Test Directory (aruplab.com). Hemoglobin S 0.0 % (Ref Interval: 0.0-0.0) Hemoglobin C 0.0 % (Ref Interval: 0.0-0.0) Hemoglobin E 0.0 % (Ref Interval: 0.0-0.0) Hemoglobin - Other 0.0 % (Ref Interval: 0.0-0.0) Sickle Cell Solubility Not Performed Hemoglobin, Capillary Electrophoresis Performed Hemoglobin Evaluation See Note Beta Globin Full Gene Sequencing Not Applicable H=High, L=Low, *=Abnormal, C=Critical Patient: Patient, Example ARUP Accession: 21-048-400496 Patient Identifiers: 01234567890ABCD, 012345 Visit Number (FIN): 01234567890ABCD Page 1 of 4 | Printed: 3/11/2021 11:41:09 AM 4848 Patient Report |FINAL Beta Globin (HBB) Del/Dup Result Not Applicable Alpha Thalassemia HBA1 and HBA2 Seq Not Applicable Gamma Globin (HBG1 and HBG2) Sequencing Not Applicable Hemoglobin Cascade Interpretation See Note H=High, L=Low, *=Abnormal, C=Critical Patient: Patient, Example ARUP Accession: 21-048-400496 Patient Identifiers: 01234567890ABCD, 012345 Visit Number (FIN): 01234567890ABCD Page 2 of 4 | Printed: 3/11/2021 11:41:09 AM 4848 Patient Report |FINAL RESULT Normal hemoglobin evaluation. -
Supplementary Table S1. List of Differentially Expressed
Supplementary table S1. List of differentially expressed transcripts (FDR adjusted p‐value < 0.05 and −1.4 ≤ FC ≥1.4). 1 ID Symbol Entrez Gene Name Adj. p‐Value Log2 FC 214895_s_at ADAM10 ADAM metallopeptidase domain 10 3,11E‐05 −1,400 205997_at ADAM28 ADAM metallopeptidase domain 28 6,57E‐05 −1,400 220606_s_at ADPRM ADP‐ribose/CDP‐alcohol diphosphatase, manganese dependent 6,50E‐06 −1,430 217410_at AGRN agrin 2,34E‐10 1,420 212980_at AHSA2P activator of HSP90 ATPase homolog 2, pseudogene 6,44E‐06 −1,920 219672_at AHSP alpha hemoglobin stabilizing protein 7,27E‐05 2,330 aminoacyl tRNA synthetase complex interacting multifunctional 202541_at AIMP1 4,91E‐06 −1,830 protein 1 210269_s_at AKAP17A A‐kinase anchoring protein 17A 2,64E‐10 −1,560 211560_s_at ALAS2 5ʹ‐aminolevulinate synthase 2 4,28E‐06 3,560 212224_at ALDH1A1 aldehyde dehydrogenase 1 family member A1 8,93E‐04 −1,400 205583_s_at ALG13 ALG13 UDP‐N‐acetylglucosaminyltransferase subunit 9,50E‐07 −1,430 207206_s_at ALOX12 arachidonate 12‐lipoxygenase, 12S type 4,76E‐05 1,630 AMY1C (includes 208498_s_at amylase alpha 1C 3,83E‐05 −1,700 others) 201043_s_at ANP32A acidic nuclear phosphoprotein 32 family member A 5,61E‐09 −1,760 202888_s_at ANPEP alanyl aminopeptidase, membrane 7,40E‐04 −1,600 221013_s_at APOL2 apolipoprotein L2 6,57E‐11 1,600 219094_at ARMC8 armadillo repeat containing 8 3,47E‐08 −1,710 207798_s_at ATXN2L ataxin 2 like 2,16E‐07 −1,410 215990_s_at BCL6 BCL6 transcription repressor 1,74E‐07 −1,700 200776_s_at BZW1 basic leucine zipper and W2 domains 1 1,09E‐06 −1,570 222309_at -

(HBA1 and HBA2) Deletion Duplication with Reflex to Hb
ARUP LABORATORIES | aruplab.com Patient Report 500 Chipeta Way, Salt Lake City, Utah 84108-1221 phone: 801-583-2787, toll free: 800-522-2787 Patient Age/Gender: Unknown Tracy I. George, MD, Chief Medical Officer Specimen Collected: 11-Mar-21 12:41 AlphaThal (HBA1/2) DelDup w/rflx |Received: 11-Mar-21 12:41 Report/Verified: 22-Mar-21 17:02 HbCS FE Procedure Result Units Reference Interval Maternal Contamination Fetal Cells f1 Study Fetal Spec Maternal Contam Study, Whole Blood i1 Maternal Spec Specimen HBA DDCSFE Cultured Amnio HBA DDCSFE See Note f2 i2 Interpretation Result Footnote f1: Maternal Contamination Study Fetal Spec Single fetal genotype present; no maternal cells present. Fetal and maternal samples were tested using STR markers to rule out maternal cell contamination. f2: HBA DDCSFE Interpretation Indication for testing: Prenatal testing for alpha thalassemia. RESULT Two copies of the familial alpha globin deletion were detected. DNA VARIANT Pathogenic Deletion: --SEA; Homozygous Predicted Fetal Genotype: --/-- INTERPRETATION According to information provided to ARUP, both parents of this fetus are carriers of alpha thalassemia and each harbors a heterozygous Southeast Asian (--SEA) deletion. Two copies of the pathogenic --SEA deletion were detected in this fetal sample by deletion/duplication analysis of the alpha globin gene cluster. This result is consistent with the deletion of the HBM, HBA2, HBA1, and HBQ1 globin genes from both chromosomes; thus, this fetus is predicted to be affected with Hb Bart hydrops fetalis syndrome. Evidence for variant classification: The pathogenic --SEA deletion is a common large deletion observed in East Asian populations (HbVar database and references therein). -

32-3942: HBQ1 Recombinant Protein Description
9853 Pacific Heights Blvd. Suite D. San Diego, CA 92121, USA Tel: 858-263-4982 Email: [email protected] 32-3942: HBQ1 Recombinant Protein Alternative Name : Hemoglobin Theta 1,Hemoglobin Theta-1 Chain,Hemoglobin Subunit Theta-1,Theta-1-globin. Description Source : Escherichia Coli. HBQ1 Human Recombinant produced in E.coli is a single, non-glycosylated polypeptide chain containing 165 amino acids (1-142) and having a molecular mass of 17.9kDa.HBQ1 is fused to a 23 amino acid His-tag at N- terminus & purified by proprietary chromatographic techniques. HBQ1 is a member of the Hemoglobin family. Hemoglobin is a 66.7 kDa protein attached to four iron-binding, methenelinked tetrapyrrole rings (heme). The globin part of Hemoglobin contains 2 alpha chains and 2 beta chains organized as couples creating a tetramer. Every one of the 4 globin chains covalently connects with a heme group. The bonds between alpha and beta chains are frailer than between parallel globin chains, thus creating a cleavage plane which is vital for oxygen binding and release. Relaxation of the alpha1-beta2 cleavage plane results in high affinity for oxygen. Product Info Amount : 20 µg Purification : Greater than 90% as determined by SDS-PAGE. The HBQ1 solution contains 20mM Tris-HCl buffer (pH 8.0), 0.15M NaCl, 1mM DTT and 10% Content : glycerol. Store at 4°C if entire vial will be used within 2-4 weeks. Store, frozen at -20°C for longer periods of Storage condition : time. For long term storage it is recommended to add a carrier protein (0.1% HSA or BSA).Avoid multiple freeze-thaw cycles. -

Alpha Thalassemia
Alpha Thalassemia Alpha (α) thalassemia is the most common inherited disorder of hemoglobin (Hb) worldwide and is caused by HBA1 and HBA2 gene variants. Decreased or absent synthesis of the hemoglobin (Hb) α chain results in clinical presentations ranging from asymptomatic Tests to Consider silent carriers to severe anemia and fetal lethality. The two clinically signicant forms of α thalassemia are Hb Bart hydrops fetalis syndrome and hemoglobin H (HbH) disease. Alpha Alpha Thalassemia (HBA1 and HBA2) thalassemia is found more often in certain ethnicities, including African, African American, Deletion/Duplication with reex to Hb Constant Spring 3003651 Mediterranean, Middle Eastern, and Southeast Asian. Method: Multiplex Ligation-dependent Probe Ampli- cation with Sanger sequencing conrmation of HbCS Disease Overview Preferred rst-tier genetic test for conrmation of suspected α thalassemia or α thalassemia trait Prevalence and/or Incidence Detects common, rare, and novel deletions or duplications in the α-globin gene cluster and Most common inherited disorder of Hb worldwide its HS-40 regulatory region Carrier frequencies in high-risk populations: Multiplex ligation-dependent probe African, African American: 1/3 amplication (MLPA) used to detect Hb Middle Eastern, Southeast Asian: 1/20 Constant Spring (HbCS) (HBA2 c.427T>C; Mediterranean: 1/30-50 p.Ter143Gln); targeted Sanger sequencing is Hb Bart hydrops fetalis syndrome and HbH disease are more frequent in Southeast performed to assess HbCS copy number in absence of a concurrent HBA2 -

The Normal Structure and Regulation of Human Globin Gene Clusters
CHAPTER 3 The Normal Structure and Regulation of Human Globin Gene Clusters Bernard G. Forget and Ross C. Hardison The genes encoding the different globin chains of hemoglobin are members of an ancient gene family. In this chapter we will review the structural features of the globin genes, with particular attention to the sequences needed for proper regulation of gene expression. Some of these have been well- conserved during mammalian evolution and therefore are likely to provide a common function in many mammals. Others are only found in higher primates, and may play roles in lineage-specific regulation. We will first describe the structural characteristics of the human globin genes and then provide a comparative analysis of the genomic contexts, regulatory regions and evolutionary conservation of features present in the globin gene clusters. NUMBER AND CHROMOSOMAL LOCALIZATION OF HUMAN GLOBIN GENES Hemoglobin is a heterotetramer that contains two polypeptide subunits related to the α-globin gene subfamily (referred to here as α-like globins) and two polypeptide subunits related to the β-globin gene subfamily (β-like globins). Globin polypeptides bind heme, which in turn allows the hemoglobin in erythrocytes to bind oxygen reversibly and transport it from the lungs to respiring tissues. In humans, as in all vertebrate species studied, different α-like and β-like globin chains are synthesized at Chapter 3 The Normal Structure and Regulation of the Globin Gene Clusters progressive stages of development to produce hemoglobins characteristic of primitive (embryonic) and definitive (fetal and adult) erythroid cells (Figure 3.1). Before precise knowledge of globin gene organization was gained by gene mapping and molecular cloning, a general picture of the number and arrangement of the human globin genes emerged from the genetic analysis of normal and abnormal hemoglobins and their pattern of inheritance. -

Professor David Roberts – Thousands of Genetic Variants Modulate Blood
Thousands of genetic variants modulate blood cell variation and function in humans David J Roberts University of Oxford and NHSBT William J. Astle* , Heather Elding*, Tao Jiang*, Dave Allen, Dace Ruklisa , Heleen Bouman, Fernando Riveros-Mckay, Alice L. Mann, Daniel Mead, Myrto A. Kostadima, John J. Lambourne , Suthesh Sivapalaratnam , Kate Downes, Kousik Kundu, Lorenzo Bomba, Kim Berentsen, John R. Bradley, Louise C. Daugherty, Olivier Delaneau, Stephen F. Garner, Luigi Grassi, Matthias Haimel, Eva M. Janssen-Megens, Anita Kaan, Mihir Kamat, Bowon Kim, Amit Mandoli, Jonathan Marchini, Joost H.A. Martens, Stuart Meacham, Karyn Megy, Jared O’Connell, Romina Petersen, Nilofar Sharifi, Simon M. Sheard, James R. Staley, Salih Tuna, Martijn van der Ent, Shuang-Yin Wang, Eleanor Wheeler, Steven P. Wilder, Valentina Iotchkova , Carmel Moore, Jennifer Sambrook, Hendrik G. Stunnenberg, Emanuele Di Angelantonio, Stephen Kaptoge, Taco W. Kuijpers, Mattia Frontini, John Danesh §, David J. Roberts §, Willem H. Ouwehand §, Adam S. Butterworth§, Nicole Soranzo§ GWAS studies • Genome wide association studies are potentially a powerful way to determine the association of disease or phenotype with genetic traits • Discovery of novel large effect sizes now unlikely but associations may define pathophysiological pathways and therapeutic possibilities • Notable successes in SCD – association of BCL11A as negative regulator of HbF Haematological disorders • Acquired and inherited haematological diseases are of global importance to public health • Global anemia -

Hemoglobin Theta-1 Recombinant Protein Cat
Hemoglobin theta-1 Recombinant Protein Cat. No.: 92-519 Hemoglobin theta-1 Recombinant Protein Specifications SPECIES: Human SOURCE SPECIES: E. coli SEQUENCE: Met1-Arg142 FUSION TAG: N-6 His tag TESTED APPLICATIONS: APPLICATIONS: This recombinant protein can be used for biological assays. For research use only. PREDICTED MOLECULAR 17.7 kD WEIGHT: Properties Greater than 95% as determined by reducing SDS-PAGE. PURITY: Endotoxin level less than 0.1 ng/ug (1 IEU/ug) as determined by LAL test. PHYSICAL STATE: Lyophilized Lyophilized from a 0.2 um filtered solution of 20mM PB, 150mM NaCl, pH 7.0. It is not BUFFER: recommended to reconstitute to a concentration less than 100 ug/ml. Dissolve the lyophilized protein in ddH2O. September 27, 2021 1 https://www.prosci-inc.com/hemoglobin-theta-1-recombinant-protein-92-519.html Lyophilized protein should be stored at -20˚C, though stable at room temperature for 3 weeks. STORAGE CONDITIONS: Reconstituted protein solution can be stored at 4-7˚C for 2-7 days. Aliquots of reconstituted samples are stable at -20˚C for 3 months. Additional Info OFFICIAL SYMBOL: HBQ1 ALTERNATE NAMES: Hemoglobin subunit theta-1/ Hemoglobin theta-1 chain/ Theta-1-globin/ HBQ1, HBQ1 ACCESSION NO.: P09105 GENE ID: 3049 Background and References Hemoglobin subunit theta-1 is a protein that in humans is encoded by the HBQ1 gene. Theta-globin mRNA is originally found in human fetal erythroid tissue but not in adult erythroid or other nonerythroid tissue. Theta-1 is a member of the human alpha-globin gene cluster that includes five functional genes and two pseudogenes.