Bhat's Modifications of Glassberg–Duckett Repair to Reduce Complications in Management Severe Hypospadias with Curvature
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Trans-Scrotal Complex Fistula-In-Ano: Tricks for Safe Single Stage Surgery
Clinical Image Clinics in Surgery Published: 29 Nov, 2017 Trans-Scrotal Complex Fistula-in-Ano: Tricks for Safe Single Stage Surgery Rajvilas Anil Narkhede, Gunjan S Desai* and Hitesh Mehta Department of Gastrointestinal Surgery, Lilavati Hospital and Research Centre, India Keywords Complex fistula; Trans-scrotal fistula; Trans-sphincteric fistula Clinical Image Complex fistula-in-ano with tract extending trans-scrotally to the root of penis and secondary opening at base of scrotum is very rare. Fistula-in-ano with scrotal extension is known to present as inter-sphincteric or low trans-sphincteric fistula running through the Colles’ fascia, which is the path of least resistance over a tough deep perineal Gallaudet’s fascia and often stands out as exception to Goodsall’s rule [1,2]. Present images show surgical technique for managing one such case. Digital examination under anesthesia revealed a palpable thickening at 12 O’clock; 2 cm proximal to anal verge which on probing identified a long fistulous tract with trans-scrotal extension to root of penis and a secondary opening at the base of scrotum (Figure 1-3). A careful sharp fistulectomy was performed, starting from root of penis, dissecting tract in the scrotal septum without violating the testes with its tunica and was brought out infra-scrotally. The secondary tract opening at base of scrotum was watchfully dissected, palpating the ‘cord like feel’ of foley’s catheter, thus preventing any iatrogenic injury to urethra. After complete fistulectomy, internal opening was closed with absorbable sutures and partial primary wound closure was performed. Recovery was uneventful (Figure 4-6). -

Radical Penectomy
Cancer Reports and Reviews Review Article ISSN: 2513-9290 Radical penectomy: procedure details of an uncommonly performed procedure for carcinoma penis and review of literature Kaushal Yadav1* and Rakesh Minhas2 1Consultant Surgical Oncology, Max Institute of Cancer Care, Gurgaon, India 2Resident Surgery, Max Institute of Cancer Care, Gurgaon, India Abstract Penile carcinoma is more common disease of developing world and in people with unhygienic practices. Partial and total penectomy are more commonly done surgical procedures. Radical penectomy is not required so commonly and only few reported cases are there for this procedure. We present technical details of this procedure in a case of young patient who was cured by this surgical technique. He required it because of disease involvement almost till proximal corpora cavernosa. Introduction • Total Penectomy: It is misnomer. Penis is excised at or near the suspensory ligament of the penis without removal of proximal Squamous cell carcinoma of penis represents approximately corpora cavernosa. Total penectomy is indicated when size or 0.5% of all cancers among men in United States and other developed location of penile carcinoma doesn’t allow preservation of sufficient countries. The incidence is higher i.e. around 10% among men of stump for upright voiding. developing countries of Asia Africa and South America. In developing • Radical Penectomy: penis is excised with complete corporeal body countries most of the cases present in advance stage. In urban India, excision till their origin. This procedure is not done commonly and the age-adjusted incidence of penile cancer ranges from 0.7-2.3 cases there are only few reported cases [5]. -

5 the PERINEUM Diya.Pdf
THE PERINEUM Prof Oluwadiya Kehinde www.oluwadiya.com Perineum • Lies below the pelvic floor • Refers to the surface of the trunk between the thighs and the buttocks, extending from the coccyx to the pubis • Boundaries are: o Anteriorly: Pubic symphysis o Anterolaterally: Inferior pubic rami and ischial rami o Laterally: Ischial tuberosities o Posterolaterally: Sacrotuberous ligaments o Posteriorly: Inferior part of sacrum and coccyx Perineum • Divided into two by an imaginary line between the ischial tuberosities into: • Urogenital triangle contains the roots of the external genitalia and, in women, the openings of the urethra and the vagina. In men, the distal part of the urethra is enclosed by erectile tissues and opens at the end of the penis • The anal triangle contains the anal aperture posteriorly. • The midpoint of the line joining the ischial tuberosities is the central point of the perineum Perineum Perineal membrane • Thick fascia, • Triangular • Attached to the pubic arch • Has a free posterior margin • Perforated by the urethra in both sexes • Perforated by the vagina in females Perineal membrane The perineal membrane and adjacent pubic arch provide attachment for the roots of the external genitalia and their associated muscles Perineal body • An irregular mass, of variable in size and consistency • Contains connective tissues, skeletal and smooth muscle fibres. • Located in the central point of the perineum • Lies just deep to the skin • Posterior to the vestibule of the penis • Anterior to the anus and anal canal. Perineal body • The following muscles blend with it: • Bulbospongiosus. • External anal sphincter. • Superficial and deep transverse perineal muscles. • Smooth and voluntary slips of muscle from the external urethral sphincter, levator ani, and muscular coats of the rectum. -

Mvdr. Natália Hvizdošová, Phd. Mudr. Zuzana Kováčová
MVDr. Natália Hvizdošová, PhD. MUDr. Zuzana Kováčová ABDOMEN Borders outer: xiphoid process, costal arch, Th12 iliac crest, anterior superior iliac spine (ASIS), inguinal lig., mons pubis internal: diaphragm (on the right side extends to the 4th intercostal space, on the left side extends to the 5th intercostal space) plane through terminal line Abdominal regions superior - epigastrium (regions: epigastric, hypochondriac left and right) middle - mesogastrium (regions: umbilical, lateral left and right) inferior - hypogastrium (regions: pubic, inguinal left and right) ABDOMINAL WALL Orientation lines xiphisternal line – Th8 subcostal line – L3 bispinal line (transtubercular) – L5 Clinically important lines transpyloric line – L1 (pylorus, duodenal bulb, fundus of gallbladder, superior mesenteric a., cisterna chyli, hilum of kidney, lower border of spinal cord) transumbilical line – L4 Bones Lumbar vertebrae (5): body vertebral arch – lamina of arch, pedicle of arch, superior and inferior vertebral notch – intervertebral foramen vertebral foramen spinous process superior articular process – mammillary process inferior articular process costal process – accessory process Sacrum base of sacrum – promontory, superior articular process lateral part – wing, auricular surface, sacral tuberosity pelvic surface – transverse lines (ridges), anterior sacral foramina dorsal surface – median, intermediate, lateral sacral crest, posterior sacral foramina, sacral horn, sacral canal, sacral hiatus apex of the sacrum Coccyx coccygeal horn Layers of the abdominal wall 1. SKIN 2. SUBCUTANEOUS TISSUE + SUPERFICIAL FASCIAS + SUPRAFASCIAL STRUCTURES Superficial fascias: Camper´s fascia (fatty layer) – downward becomes dartos m. Scarpa´s fascia (membranous layer) – downward becomes superficial perineal fascia of Colles´) dartos m. + Colles´ fascia = tunica dartos Suprafascial structures: Arteries and veins: cutaneous brr. of posterior intercostal a. and v., and musculophrenic a. -

Anatomy, Histology and Histochemistry of Accessory Sex Glands in Male Persian Squirrel (Sciurus Anomalus)
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Firenze University Press: E-Journals IJAE Vol. 122, n. 1: 17-26, 2017 ITALIAN JOURNAL OF ANATOMY AND EMBRYOLOGY Research article - Histology and cell biology Anatomy, histology and histochemistry of accessory sex glands in male Persian squirrel (Sciurus anomalus) Ghasem Akbari1,*, Davoud Kianifard1 Department of Basic Sciences, Faculty of Veterinary Medicine, University of Tabriz, Tabriz, Iran Abstract Persian squirrel (Sciurus anomalus) is a species of squirrels in the Middle East. There is lit- tle information about the anatomy and histology of various organs of this species. Moreover, there are no practical data about the accessory male sex glands of this species of squirrel. In this study the anatomical, histological and histochemical properties of the male reproductive system accessory glands of Persian Squirrel was evaluated. Eight adult male squirrels were anesthetized and euthanized. The pelvic area was dissected and the male reproductive system was separated. The accessory sex glands were investigated for gross anatomical aspect. Samples were fixed in formaldehyde for histological and histochemical studies. The coagulating glands, prostate and bulbourethral glands were observed at gross anatomical level. A single heart- shape and compact prostate gland was situated on the dorsal side of pelvic urethra. Two small coagulating glands were observed on the cranio-dorsal side of prostate. Two large spiral shape bulbourethral glands were situated out of the pelvic cavity near the root of penis on both sides of anal area. Histologic studies revealed that all accessory sex glands were alveolar glands with cuboidal to columnar epithelium. -

Penile Fracture - Comparison of Two Tertiary Centres (GMC Srinagar Vs
Jebmh.com Original Research Article Penile Fracture - Comparison of Two Tertiary Centres (GMC Srinagar vs. GMC Jammu) - An Observational Study Varun Dogra1, Silvi Sandhu2, Ishfaq Ahmad Gilkar3 1, 3 Department of General Surgery, Government Medical College, Srinagar, Jammu & Kashmir, India. 2 Department of Pathology, Government Medical College, Srinagar, Jammu & Kashmir, India. ABSTRACT BACKGROUND Penile fracture is defined as the traumatic rupture of tunica albuginea on one or Corresponding Author: both sides leading to detumescence and deformity of penis. It’s a distressing Dr. Ishfaq Ahmad Gilkar, Department of General Surgery, condition for the patient and patient often tries to conceal history. Treatment is Government Medical College, mainly via surgical repair. People are hesitant to seek medical advice and often Srinagar, Jammu & Kashmir, India. conceal the proper history this leads to delayed visits by patients sometimes even E-mail: after days. Sometimes they even come with an entirely different complaint and [email protected] reveal the real issue later on. Various causes of fracture penis include masturbation, sexual intercourse, forceful bending of erect penis to micturate, DOI: 10.18410/jebmh/2021/425 turning on bed over an erect penis. How to Cite This Article: Dogra V, Sandhu S, Gilkar IA. Penile METHODS fracture - comparison of two tertiary This was a prospective observational study that was carried out at two different centres (GMC Srinagar vs. GMC Jammu) tertiary care hospitals and twenty-seven patients were enrolled with history of - an observational study J Evid Based penile fracture. All the data was carefully collected and tabulated and early all the Med Healthc 2021;8(26):2278-2282. -
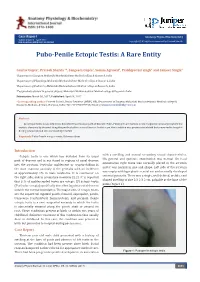
Pubo-Penile Ectopic Testis: a Rare Entity
Case Report Anatomy Physiol Biochem Int J Volume 2 Issue 2 - April 2017 Copyright © All rights are reserved by Prateek Sharda DOI: 10.19080/APBIJ.2017.02.555582 Pubo-Penile Ectopic Testis: A Rare Entity Gaurav Gupta1, Prateek Sharda 1*, Sangeeta Gupta2, Sonam Agrawal3, Prabhjyot bir singh4 and Sameer Singla4 1Department of Surgery, Maharishi Markandeshwar Medical college & Research, India 2Department of Physiology, Maharishi Markandeshwar Medical college & Research, India 3Department of Pediatrics, Maharishi Markandeshwar Medical college & Research, India 4Postgraduate student in general surgery, Maharishi Markandeshwar Medical college & Research, India Submission: March 30, 2017; Published: April 04, 2017 *Corresponding author: Prateek Sharda, Senior Resident (MBBS, MS), Department of Surgery, Maharishi Markandeshwar Medical college & Research, Mullana, Ambala, Haryana, India; Tel: ; Email: Abstract An ectopic testis is one which has deviated from its usual path of descent. Pubo-Penile ectopic testis is a rare congenital anomaly in which the testis is abnormally situated along the penile shaft or around its root. In this case, the condition was present since birth but presented to hospital during adolescence & was successfully treated. Keywords: Pubo-Penile ectopic testis; Gubernaculum Introduction with a swelling, and normal secondary sexual characteristics. Ectopic testis is one which has deviated from its usual His general and systemic examination was normal. On local path of descent and is not found in regions of usual descent examination right testis was normally placed in the scrotum into the scrotum. Testicular maldescent or cryptorchidism is and it was normal in size and shape. Left side of the scrotum the most common anomaly of the genitalia with an incidence was empty with hypoplastic scrotal sac and normally developed of approximately 1% in male newborns. -

Surgical Anatomy of the Penis in Hypospadias
Pediatric Urology Surgical Anatomy of the Penis in Hypospadias: Magnetic Resonance Imaging Study of the Tissue Planes, Vessels, and Collaterals Shiv Narain Kureel, Archika Gupta, Kanoujia Sunil, Yadvendra Dheer, Manoj Kumar, and Vinod Kumar Tomar OBJECTIVE To report the surgical anatomy of the penis in hypospadias with study of vessels in relation to fascial planes, glans, corpora cavernosa, and corpus spongiosum using magnetic resonance imaging. MATERIALS AND Twelve hypospadias presenting at older age (8-20 years) were studied with 1.5-T magnetic METHODS resonance imaging scanner and a 3-inch surface coil. Precontrast and postcontrast images were acquired using fast-spin echo sequences in sagittal, coronal, and transverse planes. The findings were processed in Volume Share 4.5, version Workstation, of General Electric Healthcare. Anatomic findings were verified during surgery. With imaging and surgical findings, a 3-dimensional conceptual diagram of surgical anatomy was created. RESULTS Distinct layers of the skin, dartos fascia, Buck fascia, tunica albuginea, glans urothelium, lamina propria of glans, and corpus spongiosum were delineated with their spatial relationship. Axial pattern vessels of the dartos and its anastomosis with branches of dorsal penile vessels at the coronal sulcus, perforators along the corpus spongiosum, subglanular extension of the fascia, and intraglanular branches of the dorsal penile artery forming an arcade were visualized. CONCLUSION Dorsomedial and dorsolateral axial pattern vessels are present in penile dartos with relative avascularity at dorsal midline in most cases. Subglanular extension of Buck fascia fused with the basal lamina propria of glans forms a barrier between the tip of corpora and the intraglanular arcade of vessels. -

Functional Reproductive Anatomy of the Male
Functional Reproductive Anatomy of the Male • Many Individual Organs – Acting in concert • Produce • Deliver – Sperm to female tract • Basic Components – Spermatic cords – Scrotum – Testes – Excurrent duct system – Accessory glands – Penis Manufacturing Complex Concept Testicular Descent Testicular Descent Time of Testicular Descent Species Testis in Scrotum Horse 9 to 11 months of gestation (10 d pp) Cattle 3.5 to 4 months of gestation Sheep 80 days of gestation Pig 90 days of gestation Dog 5 days after birth (2-3 weeks complete) Cat 2 to 5 days after birth Llama Usually present at birth Cryptorchidism • Failure of the testis to • Most Common fully descend into the – Boars scrotum – Dogs – Unilateral – Stallions – Bilateral • Breed effects • Sterile • Least common – Abdominal – Bulls – Inguinal – Rams – Bucks Cryptorchidism • Abdominal retention – Passage through inguinal rings by 2 weeks after birth imperative • Inguinal location at birth – Can occur in many species – Remain for weeks or months • 2 to 3 years in some stallions Cryptorchidism • Causes for concern – Reduced fertility – Genetic component • Mode of inheritance unclear – Autosomal recessive in sheep & swine? – Neoplasia – Spermatic cord torsion – Androgen production Spermatic Cord • Extends from inguinal ring to suspend testis in scrotum • Contains – Testicular artery – Testicular veins • Pampiniform plexus – Lymphatics – Nerves – Ductus deferens – Cremaster muscle* Vascular Supply to the Testes • Testicular arteries – R: off aorta – L: off left renal artery • Testicular -

Copyrighted Material
5 1 Anatomy of the Reproductive System of the Bull Ben Nabors Department of Clinical Sciences, College of Veterinary Medicine, Mississippi State University, Starkville, MS, USA Introduction peritoneum that passes through the inguinal canal into the scrotal sac. The potential space between the parietal The anatomy of the reproductive system of the bull can be and visceral vaginal tunic is the vaginal cavity (Figure 1.3). grouped functionally into the components of production, The purpose of the vaginal cavity is for temperature regu- transport, and transfer of spermatozoa (Figure 1.1). lation of the testicle by raising it closer to the body through contraction of the tunica dartos and cremaster muscles. The tunica albuginea is a thick fibrous capsule Production that covers the testicle and maintains the testicular con- tents under pressure [3]. Internally the tunica albuginea The testicular parenchyma contains the cellular machinery forms the axially positioned mediastinum testis from for spermatogenesis and steroid production (Figures 1.2 which connective tissue septa divide the testis into indis- and 1.3). The parenchyma is arranged in indistinct lobules tinct lobules. This connective tissue framework supports of convoluted tubules called seminiferous tubules. The the vasculature, nerves, parenchyma, and tubular system seminiferous tubules contain the spermatogonia from of the testicle. The scrotum of the bull is pendulous due to which the mature sperm cells develop. Sertoli cells are also the dorsoventral orientation of the testes contained located within the lumen of the seminiferous tubules. The within [1]. Leydig cells that are responsible for the production of the male hormone testosterone are located between the Spermatic Cord seminiferous tubules in the interstitial space [1]. -
The Reproductive System: Part A
11/22/2014 PowerPoint® Lecture Slides Reproductive System prepared by Barbara Heard, Atlantic Cape Community • Primary sex organs (gonads) - testes College and ovaries – Produce gametes (sex cells ) – sperm & ova C H A P T E R 27 – Secrete steroid sex hormones • Androgens (males) • Estrogens and progesterone (females) The • Accessory reproductive organs - ducts, Reproductive glands, and external genitalia System: Part A © Annie Leibovitz/Contact Press Images © 2013 Pearson Education, Inc. © 2013 Pearson Education, Inc. Reproductive System Male Reproductive System • Sex hormones play roles in • Testes (within scrotum) produce sperm – Development and function of reproductive • Sperm delivered to exterior through organs system of ducts – Sexual behavior and drives – Epididymis ductus deferens ejaculatory – Growth and development of many other duct urethra organs and tissues © 2013 Pearson Education, Inc. © 2013 Pearson Education, Inc. 1 11/22/2014 Male Reproductive System Figure 27.1 Reproductive organs of the male, sagittal view. • Accessory sex glands Ureter – Seminal glands Urinary bladder Peritoneum Prostatic – Prostate Seminal gland urethra (vesicle) Pubis – Bulbo-urethral glands Ampulla of Intermediate ductus deferens part of the Ejaculatory duct urethra – Empty secretions into ducts during ejaculation Rectum Urogenital Prostate diaphragm Corpus Bulbo-urethral gland cavernosum Anus Corpus Bulb of penis spongiosum Spongy Ductus (vas) deferens Epididymis urethra Testis Glans penis Scrotum Prepuce (foreskin) External urethral orifice © 2013 Pearson Education, Inc. © 2013 Pearson Education, Inc. The Scrotum The Scrotum • Sac of skin and superficial fascia • Temperature kept constant by two sets of – Hangs outside abdominopelvic cavity muscles – Contains paired testes – Dartos muscle - smooth muscle; wrinkles • 3C lower than core body temperature scrotal skin; pulls scrotum close to body • Lower temperature necessary for sperm – Cremaster muscles - bands of skeletal production muscle that elevate testes © 2013 Pearson Education, Inc. -
Original Research Article Outcome of Standard Tabularized Incised Plate Urethroplasty Repair Using Dartos Flap and Tunica Vaginalis Flap in of Hypospadias Cases
International Surgery Journal Patel JL et al. Int Surg J. 2018 Mar;5(3):850-854 http://www.ijsurgery.com pISSN 2349-3305 | eISSN 2349-2902 DOI: http://dx.doi.org/10.18203/2349-2902.isj20180433 Original Research Article Outcome of standard tabularized incised plate urethroplasty repair using dartos flap and tunica vaginalis flap in of hypospadias cases Jiwan Lal Patel1, Sandeep Chandrakar2*, M. Amin Memon1, Basumitra Mishra2 1Department of Paediatric Surgery, 2Department of General Surgery, Pt JNM Medical College and Associated Dr. BRAM Hospital, Raipur, Chhattisgarh, India Received: 16 January 2018 Accepted: 20 January 2018 *Correspondence: Dr. Sandeep Chandrakar, E-mail: [email protected] Copyright: © the author(s), publisher and licensee Medip Academy. This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Background: Hypospadias, with prevalence of 1 per 300 live births, is a congenital malformation caused by incomplete fusion of urethral folds, in which the meatal orifice opens on the inferior surface of the penis. The commonest complication of hypospadias surgery is fistula formation which requires re-operation. Several techniques of providing vascularised soft tissue cover to neourethra have been described. They include de-epithelized skin, corpus spongiosum, dartos fascia and tunica vaginalis. The purpose of our study was to compare outcomes of standard tubularised incised plate urethroplasty (TIP) repair using dartos flap and TVF in of hypospadias cases. Methods: This study was carried out in the Department of Surgery (Paediatric Surgery Division) of Pt.