Anatomy of the Thyroid, Parathyroid, Pituitary and Adrenal Glands, Surgery (2017), BASIC SCIENCE
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Endocrine Block اللهم ال سهل اال ما جعلته سهل و أنت جتعل احلزن اذا شئت سهل
OSPE ENDOCRINE BLOCK اللهم ﻻ سهل اﻻ ما جعلته سهل و أنت جتعل احلزن اذا شئت سهل Important Points 1. Don’t forget to mention right and left. 2. Read the questions carefully. 3. Make sure your write the FULL name of the structures with the correct spelling. Example: IVC ✕ Inferior Vena Cava ✓ Aorta ✕ Abdominal aorta ✓ 4. There is NO guarantee whether or not the exam will go out of this file. ممكن يأشرون على أجزاء مو معلمه فراح نحط بيانات إضافية حاولوا تمرون عليها كلها Good luck! Pituitary gland Identify: 1. Anterior and posterior clinoidal process of sella turcica. 2. Hypophyseal fossa (sella turcica) Theory • The pituitary gland is located in middle cranial fossa and protected in sella turcica (hypophyseal fossa) of body of sphenoid. Relations Of Pituitary Gland hypothalamus Identify: 1. Mamillary body (posteriorly) 2. Optic chiasma (anteriorly) 3. Sphenoidal air sinuses (inferior) 4. Body of sphenoid 5. Pituitary gland Theory • If pituitary gland became enlarged (e.g adenoma) it will cause pressure on optic chiasma and lead to bilateral temporal eye field blindness (bilateral hemianopia) Relations Of Pituitary Gland Important! Identify: 1. Pituitary gland. 2. Diaphragma sellae (superior) 3. Sphenoidal air sinuses (inferior) 4. Cavernous sinuses (lateral) 5. Abducent nerve 6. Oculomotor nerve 7. Trochlear nerve 8. Ophthalmic nerve 9. Trigeminal (Maxillary) nerve Structures of lateral wall 10. Internal carotid artery Note: Ophthalmic and maxillary are both branches of the trigeminal nerve Divisions of Pituitary Gland Identify: 1. Anterior lobe (Adenohypophysis) 2. Optic chiasma 3. Infundibulum 4. Posterior lobe (Neurohypophysis) Theory Anterior Lobe Posterior Lobe • Adenohypophysis • Neurohypophysis • Secretes hormones • Stores hormones • Vascular connection to • Neural connection to hypothalamus by hypothalamus by Subdivisions hypophyseal portal hypothalamo-hypophyseal system (from superior tract from supraoptic and hypophyseal artery) paraventricular nuclei. -

Cervical Viscera and Root of Neck
Cervical viscera & Root of neck 頸部臟器 與 頸根部 解剖學科 馮琮涵 副教授 分機 3250 E-mail: [email protected] Outline: • Position and structure of cervical viscera • Blood supply and nerve innervation of cervical viscera • Contents in root of neck Viscera of the Neck Endocrine layer – thyroid and parathyroid glands Respiratory layer – larynx and trachea Alimentary layer – pharynx and esophagus Thyroid gland Position: deep to sterno-thyroid and sterno-hyoid ms. (the level of C5 to T1) coverd by pretracheal deep cervical fascia (loose sheath) and capsule (dense connective tissue) anterolateral to the trachea arteries: superior thyroid artery – ant. & post. branches inferior thyroid artery (br. of thyrocervical trunk) thyroid ima artery (10%) Veins: superior thyroid vein IJVs (internal jugular veins) middle thyroid vein IJVs inferior thyroid vein brachiocephalic vein Thyroid gland Lymphatic drainage: prelaryngeal, pretracheal and paratracheal • lymph nodes inferior deep cervical lymph nodes Nerves: superior, middle & inferior cervical sympathetic ganglia periarterial plexuses • # thyroglossal duct cysts, pyramidal lobe (50%) # Parathyroid glands Position: external to thyroid capsule, but inside its sheath superior parathyroid glands – 1 cm sup. to the point of inf. thyroid artery into thyroid inferior parathyroid glands – 1 cm inf. to inf. thyroid artery entry point (various position) Vessels: branches of inf. thyroid artery or sup. thyroid artery parathyroid veins venous plexuses of ant. surface of thyroid Nerves: thyroid branches of the cervical sympathetic ganglia Trachea Tracheal rings (C-shape cartilage) + trachealis (smooth m.) Position: C6 (inf. end of the larynx) – T4/T5 (sternal angle) # trache`ostomy – 1st and 2nd or 2nd through 4th tracheal rings # care: inf. thyroid veins, thyroid ima artery, brachiocephalic vein, thymus and trachea Esophagus Position: from the inf. -

Selective Venous Sampling for Primary Hyperparathyroidism: How to Perform an Examination and Interpret the Results with Reference to Thyroid Vein Anatomy
Jpn J Radiol DOI 10.1007/s11604-017-0658-3 INVITED REVIEW Selective venous sampling for primary hyperparathyroidism: how to perform an examination and interpret the results with reference to thyroid vein anatomy Takayuki Yamada1 · Masaya Ikuno1 · Yasumoto Shinjo1 · Atsushi Hiroishi1 · Shoichiro Matsushita1 · Tsuyoshi Morimoto1 · Reiko Kumano1 · Kunihiro Yagihashi1 · Takuyuki Katabami2 Received: 11 April 2017 / Accepted: 28 May 2017 © Japan Radiological Society 2017 Abstract Primary hyperparathyroidism (pHPT) causes and brachiocephalic veins for catheterization of the thyroid hypercalcemia. The treatment for pHPT is surgical dis- veins and venous anastomoses. section of the hyperfunctioning parathyroid gland. Lower rates of hypocalcemia and recurrent laryngeal nerve injury Keywords Primary hyperparathyroidism · Localization · imply that minimally invasive parathyroidectomy (MIP) is Thyroid vein · Venous sampling safer than bilateral neck resection. Current trends in MIP use can be inferred only by reference to preoperative locali- zation studies. Noninvasive imaging studies (typically pre- Introduction operative localization studies) show good detection rates of hyperfunctioning glands; however, there have also been Primary hyperparathyroidism (pHPT) is a common endocrine cases of nonlocalization or discordant results. Selective disease. Most patients have one adenoma, but double adeno- venous sampling (SVS) is an invasive localization method mas have been reported in up to 15% of cases [1]. Approxi- for detecting elevated intact parathyroid -
Safe and Optimum Steps for Total / Hemi Thyroidectomy
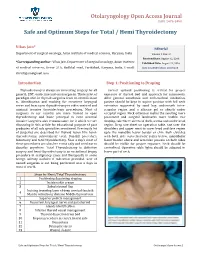
Otolaryngology Open Access Journal ISSN: 2476-2490 Safe and Optimum Steps for Total / Hemi Thyroidectomy Vikas Jain* Editorial Department of surgical oncology, Asian institute of medical sciences, Haryana, India Volume 1 Issue 2 Received Date: August 12, 2016 *Corresponding author: Vikas Jain, Department of surgical oncology, Asian institute Published Date: August 22, 2016 of medical sciences, Sector 21A, Badkhal road, Faridabad, Haryana, India, E-mail: DOI: 10.23880/OOAJ-16000120 [email protected] Introduction Step 1: Positioning to Draping Thyroidectomy is always an interesting surgery for all Correct optimal positioning is critical for proper general, ENT, endocrine and oncosurgeons. There is lot of exposure of thyroid bed and approach for maneuvers. paradigm shift in thyroid surgeries from no identification After general anesthesia and endotracheal intubation, to identification and tracking for recurrent laryngeal patient should be kept in supine position with full neck nerve and from open thyroidectomy to video-assisted and extension supported by sand bag underneath inter- minimal invasive thyroidectomy procedures. Most of scapular region and a silicone gel or sheath under surgeons in our country are more trained in open occipital region. Neck extension makes the swelling more thyroidectomy and basic principal in even minimal prominent and surgical landmarks more visible. For invasive surgeries also remains same for it which we are draping, take three sheets of cloth, across and under head discussing in this article for educational purpose of post region. Drop one sheet on operation table, one over the graduates of all sub specialties mentioned. Previously lot shoulders and upper most to cover head and face region of surgeries are described for thyroid lesion like hemi- upto the mandible lower border or chin. -

7. Cervical Procedures
BWH 2015 GENERAL SURGERY RESIDENCY PROCEDURAL ANATOMY COURSE 7. CERVICAL PROCEDURES CONTENTS LAB OBJECTIVES ........................................................................................................................................................2 Knowledge objectives ...........................................................................................................................................2 Skills objectives .....................................................................................................................................................2 Preparation for lab ................................................................................................................................................2 7.1 ORGANIZATION OF THE NECK .............................................................................................................................3 7.2 ANTERIOR APPROACH AND SUPERFICIAL STRUCTURES ......................................................................................5 7.3 THYROID AND PARATHYROID GLANDS ................................................................................................................7 Thyroid gland ........................................................................................................................................................7 Parathyroid glands ................................................................................................................................................9 7.4 NECK VASCULATURE ....................................................................................................................................... -

Arteries of the Neck Common Carotid Artery
Arteries of the neck Common carotid artery Beginning: On the right, the CCA arises from the brachiocephalic artery as it passes behind the sternoclavicular joint. On the left, it arises directly from the arch of the aorta in the superior mediastinum. End: upper border of the thyroid cartilage, by dividing into ECA and ICA. Branches: it gives no branches except its terminal branches(ECA and ICA). Internal carotid artery Beginning: from CCA lateral to the upper border of the thyroid cartilage. End: in the cranial cavity by dividing into anterior and middle cerebral arteries. External carotid artery Beginning: from CCA lateral to the upper border of the thyroid cartilage. End: in the substance of the parotid gland behind the neck of the mandible, by dividing into superficial temporal and maxillary arteries. Course: At its origin, it lies in the carotid triangle and lies anteromedial to the ICA. It later becomes anterior, then lateral, to the internal carotid as it ascends. It first ascends forwards and then inclines backwards and laterally, to pass midway between the tip of the mastoid process and the angle of the mandible. Relations: Superficial relations Deep relations - skin and superficial fascia. - lateral wall of the pharynx. - cervical branch of the facial n. - internal carotid artery. - sternocleidomastoid muscle. NB: ICA sparated from ECA - posterior belly of digastric ms. by: - posteromedial surface of the - styloid process. parotid gland. - styloglossus ms. - stylopharyngeus muscle. - glossopharyngeal nerve. - pharyngeal br. of vagus n. - part of the parotid gland. Branches of ECA: 1- Superior thyroid artery: just below the level of the greater cornu of the hyoid bone to supply thyroid gland. -

7. Internal Jugular Vein the Internal Jugular Vein Is a Large Vein That Receives Blood from the Brain, Face, and Neck
د.احمد فاضل Lecture 16 Anatomy The Root of the Neck The root of the neck can be defined as the area of the neck immediately above the inlet into the thorax. Muscles of the Root of the Neck Scalenus Anterior Muscle Scalenus Medius Muscle The Thoracic Duct The thoracic duct begins in the abdomen at the upper end of the cisterna chyli. It enters the thorax through the aortic opening in the diaphragm and ascends upward, inclining gradually to the left. On reaching the superior mediastinum, it is found passing upward along the left margin of the esophagus. At the root of the neck, it continues to ascend along the left margin of the esophagus until it reaches the level of the transverse process of the seventh cervical vertebra. Here, it bends laterally behind the carotid sheath. On reaching the medial border of the scalenus anterior, it turns 1 downward and drains into the beginning of the left brachiocephalic vein. It may, however, end in the terminal part of the subclavian or internal jugular veins. Main Nerves of the Neck Cervical Plexus Brachial Plexus The brachial plexus is formed in the posterior triangle of the neck by the union of the anterior rami of the 5th, 6th, 7th, and 8th cervical and the first thoracic spinal nerves. This plexus is divided into roots, trunks, divisions, and cords. The roots of C5 and 6 unite to form the upper trunk, the root of C7 continues as the middle trunk, and the roots of C8 and T1 unite to form the lower trunk. -

NECK Part II © 2021Zillmusom
NECK Part II © 2021zillmusom I. TRIANGLES OF NECK - for purposes of description and location of structures, neck is divided by Sternocleidomastoid muscle into an Anterior triangle (anterior to muscle) containing structures related to Carotid arteries and a Posterior triangle (posterior to muscle), containing structures related to Subclavian artery, Cervical and Brachial Plexuses. A. Posterior triangle 1. Boundaries: Anterior: Sternocleidomastoid; Posterior: Trapezius; Inferior: Clavicle; Superficial cover: Superficial fascia, Platysma and Investing layer; Floor: covered by Prevertebral layer of deep fascia. 2. Contents - Arteries: Subclavian artery, Superficial (Transverse) Cervical and Suprascapular arteries (from Thyrocervical trunk), Occipital artery; Veins: External Jugular vein; Nerves: Roots and Trunks of Brachial plexus, Phrenic nerve, Accessory nerve (CN XI), branches of cervical plexus. Clinical Note: Accessory nerve is considered to divide the posterior triangle into a clinically 'careful' zone (inferior) and 'carefree' zone (superior); brachial plexus is in 'careful' zone. (On the other hand, would a patient want to be operated on by a surgeon who thinks part of the neck is 'carefree'?) Note: Subclavian vein is not within posterior triangle B. Anterior triangle of neck 1. Boundaries: anterior by midline of neck, posterior by Sternomastoid muscle, superiorly by lower margin of Mandible. 2. Contents - Arteries: Carotid sheath with Common Carotid dividing into Internal and External Carotid arteries, numerous branches of External Carotid; Veins: Internal Jugular vein; Nerves: Hypoglossal nerve and descending branch of Ansa Cervicalis, Accessory and Vagus nerves; Lymphatics: Deep Cervical chain of lymph nodes. II. DEEP STRUCTURES OF NECK A. Thyroid gland: Composed of two lateral lobes and a central isthmus, which is located below cricoid cartilage; Lateral lobes cover Common Carotid artery; Pyramidal lobe sometimes present above isthmus; when present, it is connected to the hyoid bone via a fibrous strand (no clinical consequences). -
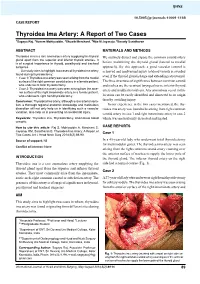
Thyroidea Ima Artery: a Report of Two Cases 1Sagaya Raj, 2Azeem Mohiyuddin, 3Shuaib Merchant, 4Rijo M Jayaraju, 5Beauty Sasidharan
IJHNS Thyroidea10.5005/jp-journals-10001-1188 Ima Artery: A report of Two Cases CASE REPORT Thyroidea Ima Artery: A Report of Two Cases 1Sagaya Raj, 2Azeem Mohiyuddin, 3Shuaib Merchant, 4Rijo M Jayaraju, 5Beauty Sasidharan ABSTRACT MATERIALS AND METHODS Thyroidea ima is a rare anomalous artery supplying the thyroid We routinely dissect and expose the common carotid artery gland apart from the superior and inferior thyroid arteries. It is of surgical importance in thyroid, parathyroid and tracheal before mobilizing the thyroid gland (lateral to medial surgeries. approach). By this approach, a good vascular control is Our study aims to highlight two cases of thyroidea ima artery achieved and inadvertent injury to blood vessels is avoided found during thyroidectomy: even if the thyroid gland is large and extending retrosternal. • Case 1: Thyroidea ima artery was seen arising from the medial surface of the right common carotid artery in a female patient, The three structures of significance between common carotid who underwent total thyroidectomy. and trachea are the recurrent laryngeal nerve, inferior thyroid • Case 2: Thyroidea ima artery was seen arising from the ante- artery and middle thyroid vein. Any anomalous vessel in this rior surface of the right innominate artery, in a female patient, who underwent right hemithyroidectomy. location can be easily identified and dissected to its origin thereby avoiding injury. Conclusion: Thyroidea ima artery, although a rare arterial varia- tion, a thorough regional anatomic knowledge and meticulous In our experience in the two cases mentioned, the thy- dissection will not only help us in identifying such a vascular roidea ima artery was found to be arising from right common variation, also help us in preventing an accidental injury. -
Lecture in Anatomy of Endocrine System by Dr
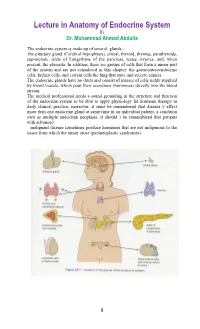
Lecture in Anatomy of Endocrine System By Dr. Mohammad Ahmad Abdulla The endocrine system is made up of several glands:- the pituitary gland (Cerebral hypophysis), pineal, thyroid, thymus, parathyroids, suprarenals, islets of Langerhans of the pancreas, testes, ovaries, and, when present, the placenta. In addition, there are groups of cells that form a minor part of the system and are not considered in this chapter: the gastroenteroendocrine cells, kidney cells, and certain cells the lung that store and secrete amines. The endocrine glands have no ducts and consist of masses of cells richly supplied by blood vessels, which pour their secretions (hormones) directly into the blood stream. The medical professional needs a sound grounding in the structure and function of the endocrine system to be able to apply physiology lid hormone therapy in daily clinical practice, moreover, it must be remembered that disease y affect more than one endocrine gland at same time in an individual patient, a condition own as multiple endocrine neoplasia. It should ) be remembered that patients with advanced malignant disease sometimes produce hormones that are not indigenous to the tissue from which the tumor arose (paraneoplastic syndromes). 1 Pituitary Gland (Hypophysis Cerebri) Location and Description The pituitary gland is a small, oval structure attached to the undersurface of the brain by the infundibulum. During pregnancy, it doubles in size. The gland is well protected by virtue of its location in the sella turcica of the sphenoid bone. Because the hormones produced by the gland influence the activities of many other endocrine glands, the hypophysis cerebri is often referred to as the master endocrine gland. -

Testing the Venous Circulation 79
58097_ch04.qxd 11/18/09 5:49 PM Page 77 CHAPTER4 PART TWO: UPPER EXTREMITIES Testing the Venous CHAPTER Circulation 4 Chapter Outline General Concepts in Upper Extremity Venous General Concepts in Examining Evaluation 79 Hemodialysis Access 94 Tips/Rationale 80 Tips/Rationale 95 Protocol Algorithm 81 Protocol Algorithm 97 Duplex Exam of Upper Extremity Duplex Exam for Examining Venous Circulation 82 Hemodialysis Access 98 Test Preparation 82 Test Preparation and Test Sequence 98 Testing Sequence 82 Results and Interpretation 99 Results and Interpretation 86 Concluding Tips 103 Concluding Tips 93 77 58097_ch04.qxd 11/18/09 5:49 PM Page 78 78 PART II ● Upper Extremities IJ Brachiocephalic EJ trunk or innominate Cephalic vein Superficial temporal Supraorbital artery artery and vein Deep temporal artery Frontal branch Supratrochlear artery Parietal branch Dorsal nasal artery Middle temporal artery and vein Infraorbital artery Middle meningeal artery Angular vein Superficial temporal artery and vein Buccal artery SVC Maxillary artery and vein Masseteric artery Superior labial artery and vein Occipital artery and vein Inferior labial artery and vein Retromandibular vein Facial artery and vein Submental artery and vein External jugular vein Lingual artery and vein Internal jugular vein Superior laryngeal artery and vein 4 Basilic vein Superior thyroid arteries and veins External carotid artery Internal jugular vein Internal carotid artery External jugular vein Transverse cervical artery Brachial vein Middle thyroid vein Inferior thyroid artery Transverse Vertebral artery cervical vein CHAPTER 1st rib Ulnar vein Radial vein A B FIGURE 4.1. Diagram of the upper extremity venous system. Brachial vein (cut) and artery C5 Brachial plexus C6 Scalenus medius Scalenus posterior C7 Scalenus anterior Median nerve Subclavian vein (cut) Lateral Axillary cord artery Medial cord Pectoralis minor FIGURE 4.2. -
THYROIDECTOMY Experience the Benefits of THUNDERBEAT Open Fine Jaw
THYROIDECTOMY Experience the Benefits of THUNDERBEAT Open Fine Jaw. 13403 THUNDERBEAT DESIGN RATIONALE Philosophy 3. Tissue Manipulation through Innovative Instrument-Tip Design Contemporary surgical instruments must be multifunctional. When the THUNDERBEAT Tissue Management The THUNDERBEAT instrument tip is an essential feature of the instrument. Alongside the delivery of two System for laparoscopic surgery was introduced, the clear goal was to develop a multipurpose instrument in different types of energy, it is designed to act as a fully functional grasping and dissecting instrument. This is order to reduce instrument exchanges, surgical time, and blood loss. achieved through atraumatic serrations of the edges of the upper jaw, the even compression-force distribution across tissue, and the high tip-opening forces that enable blunt tissue dissection. This was achieved by creating an instrument that not only allows tissue cutting that is the fastest in its class and secure 7 mm vessel sealing but also functions as a true laparoscopic instrument – allowing the surgeon to The ability to combine the proven advantages of ultrasonic and bipolar energy and the ability to provide the grasp, manipulate, and bluntly dissect tissue. finest possible tissue dissection makes THUNDERBEAT one of the most versatile instruments on the market. This technology is now available for open surgery. Three Design Criteria Make This Possible: The THUNDERBEAT Technology in Open Surgery 1. Integration of Two Forms of Energy Advanced energy devices in open surgery go beyond standard monopolar and bipolar applications. They allow Only the THUNDERBEAT system delivers two well-established types of energy to the tissue simultaneously: for shorter procedure times and reduced use of hemostatic clips, sutures, or ligation ties, thus saving time and · Ultrasonic energy, which is widely accepted for its fast tissue-cutting capability.