Axis Scientific Neck & Throat Muscles, Arteries, and Veins A-105862
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
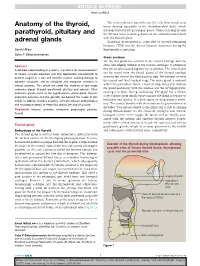
Anatomy of the Thyroid, Parathyroid, Pituitary and Adrenal Glands, Surgery (2017), BASIC SCIENCE
BASIC SCIENCE The neuroendocrine parafollicular (C) cells from neural crest Anatomy of the thyroid, tissue develop separately in the ultimobranchial body, which develops from the 4th pharyngeal pouch. These cells migrate into parathyroid, pituitary and the thyroid tissue following fusion of the ultimobranchial body with the thyroid gland. adrenal glands Glandular development is controlled by thyroid-stimulating hormone (TSH) and the thyroid becomes functional during the Sarah Hillary third month of gestation. Saba P Balasubramanian Gross anatomy The thyroid gland lies anterior to the cricoid cartilage and tra- Abstract chea, and slightly inferior to the thyroid cartilages. It comprises A detailed understanding of anatomy is essential for several reasons: two lateral lobes joined together by an isthmus. The lateral lobes to enable accurate diagnosis and plan appropriate management; to can be traced from the lateral aspect of the thyroid cartilage perform surgery in a safe and effective manner avoiding damage to down to the level of the sixth tracheal ring. The isthmus overlies adjacent structures; and to anticipate and recognize variations in the second and third tracheal rings. The entire gland is enclosed normal anatomy. This article will cover the anatomy of four major within the pretracheal fascia, a layer of deep fascia that anchors endocrine glands (thyroid, parathyroid, pituitary and adrenal). Other the gland posteriorly with the trachea and the laryngopharynx, endocrine glands (such as the hypothalamus, pineal gland, thymus, causing it to move during swallowing. The gland has a fibrous endocrine pancreas and the gonads) are beyond the scope of this outer capsule, from which septae run into the gland to separate it article. -

Endocrine Block اللهم ال سهل اال ما جعلته سهل و أنت جتعل احلزن اذا شئت سهل
OSPE ENDOCRINE BLOCK اللهم ﻻ سهل اﻻ ما جعلته سهل و أنت جتعل احلزن اذا شئت سهل Important Points 1. Don’t forget to mention right and left. 2. Read the questions carefully. 3. Make sure your write the FULL name of the structures with the correct spelling. Example: IVC ✕ Inferior Vena Cava ✓ Aorta ✕ Abdominal aorta ✓ 4. There is NO guarantee whether or not the exam will go out of this file. ممكن يأشرون على أجزاء مو معلمه فراح نحط بيانات إضافية حاولوا تمرون عليها كلها Good luck! Pituitary gland Identify: 1. Anterior and posterior clinoidal process of sella turcica. 2. Hypophyseal fossa (sella turcica) Theory • The pituitary gland is located in middle cranial fossa and protected in sella turcica (hypophyseal fossa) of body of sphenoid. Relations Of Pituitary Gland hypothalamus Identify: 1. Mamillary body (posteriorly) 2. Optic chiasma (anteriorly) 3. Sphenoidal air sinuses (inferior) 4. Body of sphenoid 5. Pituitary gland Theory • If pituitary gland became enlarged (e.g adenoma) it will cause pressure on optic chiasma and lead to bilateral temporal eye field blindness (bilateral hemianopia) Relations Of Pituitary Gland Important! Identify: 1. Pituitary gland. 2. Diaphragma sellae (superior) 3. Sphenoidal air sinuses (inferior) 4. Cavernous sinuses (lateral) 5. Abducent nerve 6. Oculomotor nerve 7. Trochlear nerve 8. Ophthalmic nerve 9. Trigeminal (Maxillary) nerve Structures of lateral wall 10. Internal carotid artery Note: Ophthalmic and maxillary are both branches of the trigeminal nerve Divisions of Pituitary Gland Identify: 1. Anterior lobe (Adenohypophysis) 2. Optic chiasma 3. Infundibulum 4. Posterior lobe (Neurohypophysis) Theory Anterior Lobe Posterior Lobe • Adenohypophysis • Neurohypophysis • Secretes hormones • Stores hormones • Vascular connection to • Neural connection to hypothalamus by hypothalamus by Subdivisions hypophyseal portal hypothalamo-hypophyseal system (from superior tract from supraoptic and hypophyseal artery) paraventricular nuclei. -

Cervical Viscera and Root of Neck
Cervical viscera & Root of neck 頸部臟器 與 頸根部 解剖學科 馮琮涵 副教授 分機 3250 E-mail: [email protected] Outline: • Position and structure of cervical viscera • Blood supply and nerve innervation of cervical viscera • Contents in root of neck Viscera of the Neck Endocrine layer – thyroid and parathyroid glands Respiratory layer – larynx and trachea Alimentary layer – pharynx and esophagus Thyroid gland Position: deep to sterno-thyroid and sterno-hyoid ms. (the level of C5 to T1) coverd by pretracheal deep cervical fascia (loose sheath) and capsule (dense connective tissue) anterolateral to the trachea arteries: superior thyroid artery – ant. & post. branches inferior thyroid artery (br. of thyrocervical trunk) thyroid ima artery (10%) Veins: superior thyroid vein IJVs (internal jugular veins) middle thyroid vein IJVs inferior thyroid vein brachiocephalic vein Thyroid gland Lymphatic drainage: prelaryngeal, pretracheal and paratracheal • lymph nodes inferior deep cervical lymph nodes Nerves: superior, middle & inferior cervical sympathetic ganglia periarterial plexuses • # thyroglossal duct cysts, pyramidal lobe (50%) # Parathyroid glands Position: external to thyroid capsule, but inside its sheath superior parathyroid glands – 1 cm sup. to the point of inf. thyroid artery into thyroid inferior parathyroid glands – 1 cm inf. to inf. thyroid artery entry point (various position) Vessels: branches of inf. thyroid artery or sup. thyroid artery parathyroid veins venous plexuses of ant. surface of thyroid Nerves: thyroid branches of the cervical sympathetic ganglia Trachea Tracheal rings (C-shape cartilage) + trachealis (smooth m.) Position: C6 (inf. end of the larynx) – T4/T5 (sternal angle) # trache`ostomy – 1st and 2nd or 2nd through 4th tracheal rings # care: inf. thyroid veins, thyroid ima artery, brachiocephalic vein, thymus and trachea Esophagus Position: from the inf. -

Non-Pathological Opacification of the Cavernous Sinus on Brain CT
healthcare Article Non-Pathological Opacification of the Cavernous Sinus on Brain CT Angiography: Comparison with Flow-Related Signal Intensity on Time-of-Flight MR Angiography Sun Ah Heo 1, Eun Soo Kim 1,* , Yul Lee 1, Sang Min Lee 1, Kwanseop Lee 1 , Dae Young Yoon 2, Young-Su Ju 3 and Mi Jung Kwon 4 1 Department of Radiology, Hallym University Sacred Heart Hospital, College of Medicine, Hallym University, Seoul 14068, Korea; [email protected] (S.A.H.); [email protected] (Y.L.); [email protected] (S.M.L.); [email protected] (K.L.) 2 Department of Radiology, Kangdong Sacred Heart Hospital, College of Medicine, Hallym University, Seoul 14068, Korea; [email protected] 3 National Medical Center, Seoul 04564, Korea; [email protected] 4 Department of Pathology, Hallym University Sacred Heart Hospital, College of Medicine, Hallym University, Seoul 14068, Korea; [email protected] * Correspondence: [email protected] Abstract: Purpose: To investigate the non-pathological opacification of the cavernous sinus (CS) on brain computed tomography angiography (CTA) and compare it with flow-related signal intensity (FRSI) on time-of-flight magnetic resonance angiography (TOF-MRA). Methods: Opacification of the CS was observed in 355 participants who underwent CTA and an additional 77 participants who underwent examination with three diagnostic modalities: CTA, TOF-MRA, and digital subtraction angiography (DSA). Opacification of the CS, superior petrosal sinus (SPS), inferior petrosal sinus Citation: Heo, S.A.; Kim, E.S.; Lee, Y.; Lee, S.M.; Lee, K.; Yoon, D.Y.; Ju, Y.-S.; (IPS), and pterygoid plexus (PP) were also analyzed using a five-point scale. -

Selective Venous Sampling for Primary Hyperparathyroidism: How to Perform an Examination and Interpret the Results with Reference to Thyroid Vein Anatomy
Jpn J Radiol DOI 10.1007/s11604-017-0658-3 INVITED REVIEW Selective venous sampling for primary hyperparathyroidism: how to perform an examination and interpret the results with reference to thyroid vein anatomy Takayuki Yamada1 · Masaya Ikuno1 · Yasumoto Shinjo1 · Atsushi Hiroishi1 · Shoichiro Matsushita1 · Tsuyoshi Morimoto1 · Reiko Kumano1 · Kunihiro Yagihashi1 · Takuyuki Katabami2 Received: 11 April 2017 / Accepted: 28 May 2017 © Japan Radiological Society 2017 Abstract Primary hyperparathyroidism (pHPT) causes and brachiocephalic veins for catheterization of the thyroid hypercalcemia. The treatment for pHPT is surgical dis- veins and venous anastomoses. section of the hyperfunctioning parathyroid gland. Lower rates of hypocalcemia and recurrent laryngeal nerve injury Keywords Primary hyperparathyroidism · Localization · imply that minimally invasive parathyroidectomy (MIP) is Thyroid vein · Venous sampling safer than bilateral neck resection. Current trends in MIP use can be inferred only by reference to preoperative locali- zation studies. Noninvasive imaging studies (typically pre- Introduction operative localization studies) show good detection rates of hyperfunctioning glands; however, there have also been Primary hyperparathyroidism (pHPT) is a common endocrine cases of nonlocalization or discordant results. Selective disease. Most patients have one adenoma, but double adeno- venous sampling (SVS) is an invasive localization method mas have been reported in up to 15% of cases [1]. Approxi- for detecting elevated intact parathyroid -

Normal Flow Signal of the Pterygoid Plexus on 3T MRA in Patients Without DAVF of the Cavernous Sinus
ORIGINAL RESEARCH EXTRACRANIAL VASCULAR Normal Flow Signal of the Pterygoid Plexus on 3T MRA in Patients without DAVF of the Cavernous Sinus K. Watanabe, S. Kakeda, R. Watanabe, N. Ohnari, and Y. Korogi ABSTRACT BACKGROUND AND PURPOSE: Cavernous sinuses and draining dural sinuses or veins are often visualized on 3D TOF MRA images in patients with dural arteriovenous fistulas involving the CS. Flow signals may be seen in the jugular vein and dural sinuses at the skull base on MRA images in healthy participants, however, because of reverse flow. Our purpose was to investigate the prevalence of flow signals in the pterygoid plexus and CS on 3T MRA images in a cohort of participants without DAVFs. MATERIALS AND METHODS: Two radiologists evaluated the flow signals of the PP and CS on 3T MRA images obtained from 406 consecutive participants by using a 5-point scale. In addition, the findings on 3T MRA images were compared with those on digital subtraction angiography images in an additional 171 participants who underwent both examinations. RESULTS: The radiologists identified 110 participants (27.1%; 108 left, 10 right, 8 bilateral) with evidence of flow signals in the PP alone (n ϭ 67) or in both the PP and CS (n ϭ 43). Flow signals were significantly more common in the left PP than in the right PP. In 171 patients who underwent both MRA and DSA, the MRA images showed flow signals in the PP with or without CS in 60 patients; no DAVFs were identified on DSA in any of these patients. CONCLUSIONS: Flow signals are frequently seen in the left PP on 3T MRA images in healthy participants. -

Papillary Thyroid Carcinoma
CASE REPORT Papillary Thyroid Carcinoma: The First Case of Direct Tumor Extension into the Left Innominate Vein Managed with a Single Operative Approach Douglas J Chung1, Diane Krieger2, Niberto Moreno3, Andrew Renshaw4, Rafael Alonso5, Robert Cava6, Mark Witkind7, Robert Udelsman8 ABSTRACT Aim: The aim of this study is to report a case of papillary thyroid carcinoma (PTC) with direct intravascular extension into the left internal jugular vein, resulting in tumor thrombus into the left innominate vein. Background: PTC is the most common of the four histological subtypes of thyroid malignancies,1 but PTC with vascular invasion into major blood vessels is rare.2 The incidence of PTC tumor thrombi was found to be 0.116% in one study investigating 7,754 thyroid surgical patients, and, of these patients with tumor thrombus, none extended more distal than the internal jugular vein.3 Koike et al.4 described a case of PTC invasion into the left innominate vein that was managed by a two-stage operative approach. Case description: A 58-year-old male presented with a rapidly growing left thyroid mass. Fine needle aspiration cytology (FNAC) suggested PTC and surgical exploration confirmed tumor extension into the left internal jugular vein. Continued dissection revealed a large palpable intraluminal tumor thrombus extending below the clavicle into the mediastinum, necessitating median sternotomy. Conclusion: Aggressive one-stage surgical resection resulted in successful en bloc extirpation of the tumor, with negative margins. Follow-up at 22 months postoperatively demonstrated no evidence of recurrence. Clinical significance: This is the first case of PTC extension into the left innominate vein managed with one-stage surgical intervention with curative intent. -
Safe and Optimum Steps for Total / Hemi Thyroidectomy
Otolaryngology Open Access Journal ISSN: 2476-2490 Safe and Optimum Steps for Total / Hemi Thyroidectomy Vikas Jain* Editorial Department of surgical oncology, Asian institute of medical sciences, Haryana, India Volume 1 Issue 2 Received Date: August 12, 2016 *Corresponding author: Vikas Jain, Department of surgical oncology, Asian institute Published Date: August 22, 2016 of medical sciences, Sector 21A, Badkhal road, Faridabad, Haryana, India, E-mail: DOI: 10.23880/OOAJ-16000120 [email protected] Introduction Step 1: Positioning to Draping Thyroidectomy is always an interesting surgery for all Correct optimal positioning is critical for proper general, ENT, endocrine and oncosurgeons. There is lot of exposure of thyroid bed and approach for maneuvers. paradigm shift in thyroid surgeries from no identification After general anesthesia and endotracheal intubation, to identification and tracking for recurrent laryngeal patient should be kept in supine position with full neck nerve and from open thyroidectomy to video-assisted and extension supported by sand bag underneath inter- minimal invasive thyroidectomy procedures. Most of scapular region and a silicone gel or sheath under surgeons in our country are more trained in open occipital region. Neck extension makes the swelling more thyroidectomy and basic principal in even minimal prominent and surgical landmarks more visible. For invasive surgeries also remains same for it which we are draping, take three sheets of cloth, across and under head discussing in this article for educational purpose of post region. Drop one sheet on operation table, one over the graduates of all sub specialties mentioned. Previously lot shoulders and upper most to cover head and face region of surgeries are described for thyroid lesion like hemi- upto the mandible lower border or chin. -

Potential Involvement of the Extracranial Venous System in Central Nervous System Disorders and Aging Robert Zivadinov1,2* and Chih-Ping Chung3,4
Zivadinov and Chung BMC Medicine 2013, 11:260 http://www.biomedcentral.com/1741-7015/11/260 DEBATE Open Access Potential involvement of the extracranial venous system in central nervous system disorders and aging Robert Zivadinov1,2* and Chih-Ping Chung3,4 Abstract Background: The role of the extracranial venous system in the pathology of central nervous system (CNS) disorders and aging is largely unknown. It is acknowledged that the development of the venous system is subject to many variations and that these variations do not necessarily represent pathological findings. The idea has been changing with regards to the extracranial venous system. Discussion: A range of extracranial venous abnormalities have recently been reported, which could be classified as structural/morphological, hemodynamic/functional and those determined only by the composite criteria and use of multimodal imaging. The presence of these abnormalities usually disrupts normal blood flow and is associated with the development of prominent collateral circulation. The etiology of these abnormalities may be related to embryologic developmental arrest, aging or other comorbidities. Several CNS disorders have been linked to the presence and severity of jugular venous reflux. Another composite criteria-based vascular condition named chronic cerebrospinal venous insufficiency (CCSVI) was recently introduced. CCSVI is characterized by abnormalities of the main extracranial cerebrospinal venous outflow routes that may interfere with normal venous outflow. Summary: Additional research is needed to better define the role of the extracranial venous system in relation to CNS disorders and aging. The use of endovascular treatment for the correction of these extracranial venous abnormalities should be discouraged, until potential benefit is demonstrated in properly-designed, blinded, randomized and controlled clinical trials. -

7. Cervical Procedures
BWH 2015 GENERAL SURGERY RESIDENCY PROCEDURAL ANATOMY COURSE 7. CERVICAL PROCEDURES CONTENTS LAB OBJECTIVES ........................................................................................................................................................2 Knowledge objectives ...........................................................................................................................................2 Skills objectives .....................................................................................................................................................2 Preparation for lab ................................................................................................................................................2 7.1 ORGANIZATION OF THE NECK .............................................................................................................................3 7.2 ANTERIOR APPROACH AND SUPERFICIAL STRUCTURES ......................................................................................5 7.3 THYROID AND PARATHYROID GLANDS ................................................................................................................7 Thyroid gland ........................................................................................................................................................7 Parathyroid glands ................................................................................................................................................9 7.4 NECK VASCULATURE ....................................................................................................................................... -

Arteries of the Neck Common Carotid Artery
Arteries of the neck Common carotid artery Beginning: On the right, the CCA arises from the brachiocephalic artery as it passes behind the sternoclavicular joint. On the left, it arises directly from the arch of the aorta in the superior mediastinum. End: upper border of the thyroid cartilage, by dividing into ECA and ICA. Branches: it gives no branches except its terminal branches(ECA and ICA). Internal carotid artery Beginning: from CCA lateral to the upper border of the thyroid cartilage. End: in the cranial cavity by dividing into anterior and middle cerebral arteries. External carotid artery Beginning: from CCA lateral to the upper border of the thyroid cartilage. End: in the substance of the parotid gland behind the neck of the mandible, by dividing into superficial temporal and maxillary arteries. Course: At its origin, it lies in the carotid triangle and lies anteromedial to the ICA. It later becomes anterior, then lateral, to the internal carotid as it ascends. It first ascends forwards and then inclines backwards and laterally, to pass midway between the tip of the mastoid process and the angle of the mandible. Relations: Superficial relations Deep relations - skin and superficial fascia. - lateral wall of the pharynx. - cervical branch of the facial n. - internal carotid artery. - sternocleidomastoid muscle. NB: ICA sparated from ECA - posterior belly of digastric ms. by: - posteromedial surface of the - styloid process. parotid gland. - styloglossus ms. - stylopharyngeus muscle. - glossopharyngeal nerve. - pharyngeal br. of vagus n. - part of the parotid gland. Branches of ECA: 1- Superior thyroid artery: just below the level of the greater cornu of the hyoid bone to supply thyroid gland. -

Anatomy and Physiology of the Cardiovascular System
Chapter © Jones & Bartlett Learning, LLC © Jones & Bartlett Learning, LLC 5 NOT FOR SALE OR DISTRIBUTION NOT FOR SALE OR DISTRIBUTION Anatomy© Jonesand & Physiology Bartlett Learning, LLC of © Jones & Bartlett Learning, LLC NOT FOR SALE OR DISTRIBUTION NOT FOR SALE OR DISTRIBUTION the Cardiovascular System © Jones & Bartlett Learning, LLC © Jones & Bartlett Learning, LLC NOT FOR SALE OR DISTRIBUTION NOT FOR SALE OR DISTRIBUTION © Jones & Bartlett Learning, LLC © Jones & Bartlett Learning, LLC NOT FOR SALE OR DISTRIBUTION NOT FOR SALE OR DISTRIBUTION OUTLINE Aortic arch: The second section of the aorta; it branches into Introduction the brachiocephalic trunk, left common carotid artery, and The Heart left subclavian artery. Structures of the Heart Aortic valve: Located at the base of the aorta, the aortic Conduction System© Jones & Bartlett Learning, LLCvalve has three cusps and opens© Jonesto allow blood & Bartlett to leave the Learning, LLC Functions of the HeartNOT FOR SALE OR DISTRIBUTIONleft ventricle during contraction.NOT FOR SALE OR DISTRIBUTION The Blood Vessels and Circulation Arteries: Elastic vessels able to carry blood away from the Blood Vessels heart under high pressure. Blood Pressure Arterioles: Subdivisions of arteries; they are thinner and have Blood Circulation muscles that are innervated by the sympathetic nervous Summary© Jones & Bartlett Learning, LLC system. © Jones & Bartlett Learning, LLC Atria: The upper chambers of the heart; they receive blood CriticalNOT Thinking FOR SALE OR DISTRIBUTION NOT FOR SALE OR DISTRIBUTION Websites returning to the heart. Review Questions Atrioventricular node (AV node): A mass of specialized tissue located in the inferior interatrial septum beneath OBJECTIVES the endocardium; it provides the only normal conduction pathway between the atrial and ventricular syncytia.