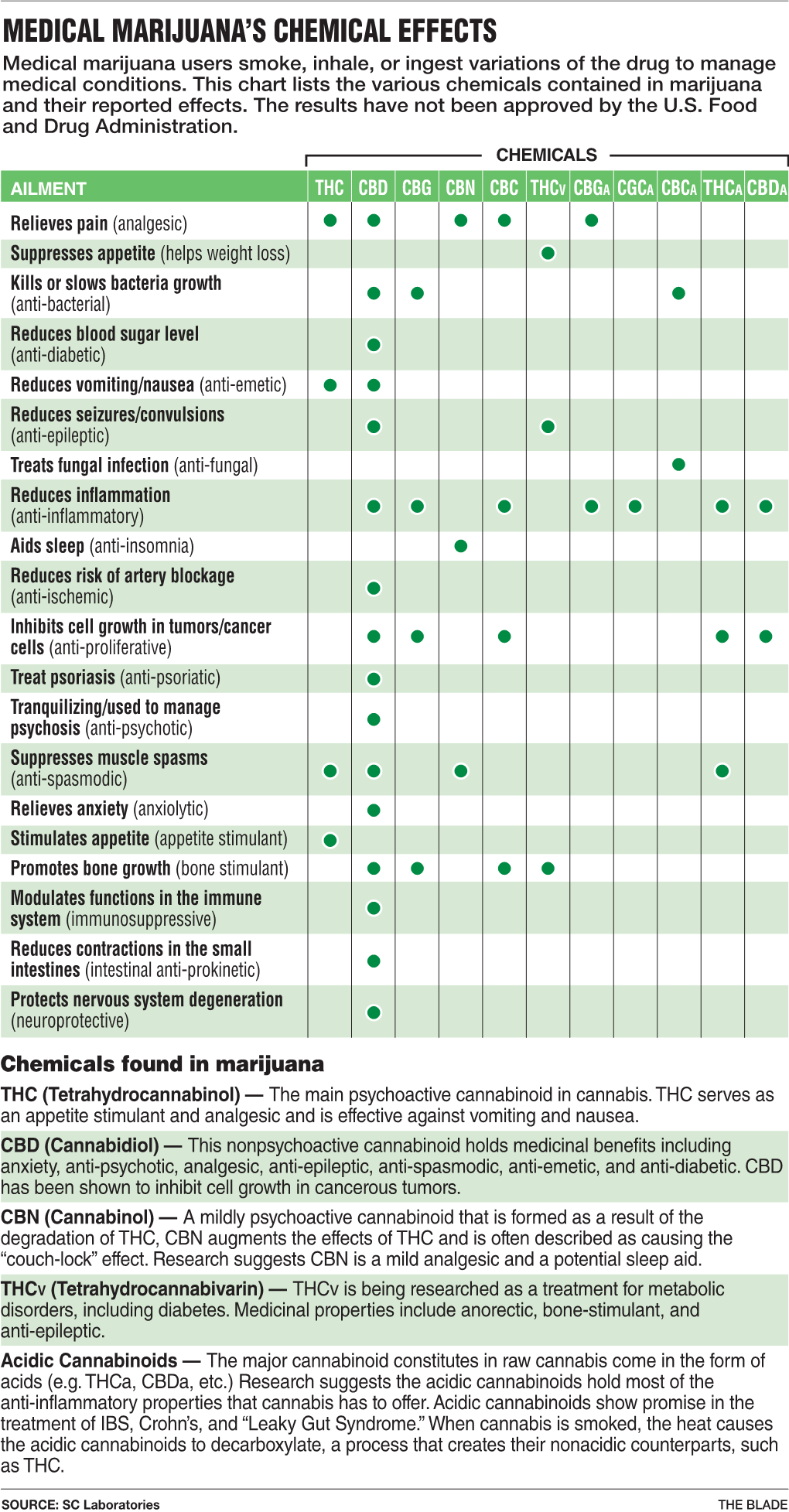
Medical Marijuana's Chemical Effects
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

FF #93 THC Cancer AIDS.3Rd Ed
! FAST FACTS AND CONCEPTS #93 CANNABINOIDS IN THE TREATMENT OF SYMPTOMS IN CANCER AND AIDS L Scott Wilner MD and Robert M Arnold MD Introduction The healing properties of cannabis have been asserted for centuries. Popular claims notwithstanding, there are no data to support the use of marijuana in the treatment of asthma, anxiety, depression, epilepsy, glaucoma, alcohol withdrawal, or infection; and limited data to support using cannabinoids as analgesics. Recent scientific studies of cannabinoids for symptom management have focused on nausea/vomiting and appetite stimulation. Terminology Cannabis sativa is the Indian hemp plant. Marijuana is a psychoactive substance derived from the plant. Cannabinoids are the biologically active compounds in the plant. THC is delta )-9 tetrahydrocannabinol, the major cannabinoid. Dronabinol is synthetic THC and the main ingredient in the Schedule 3 drug Marinol. Nabilone is an engineered THC analog that forms the basis of the Schedule 2 drug Cesamet. Pharmacology Cannabinoids act on cannabinoid receptors: the CB1 receptor in the CNS and on the CB2 receptor localized primarily to immune cells. Dronabinol and nabilone are well absorbed orally, but first pass metabolism and protein binding limit bioavailability. Dronabinol has a faster onset of action (~30 minutes), while nabilone has a longer duration of action (typically 8 – 12 hours, but potentially as long as 24 hours in some patients). Alternative delivery systems – including inhalers, suppositories, and transdermal patches – are being evaluated. Anti-emetic Use Dronabinol and nabilone are FDA approved for the treatment of nausea and vomiting associated with cancer chemotherapy in patients who have failed to respond to conventional antiemetics. -

Pharmacologic Interventions for Fatigue in Cancer and Transplantation: a Meta-Analysis
DRUG INTERVENTIONS FOR FATIGUE, Tomlinson et al. REVIEW ARTICLE Pharmacologic interventions for fatigue in cancer and transplantation: a meta-analysis † † ‡ D. Tomlinson RN MN,* P.D. Robinson MD MSc, S. Oberoi MD, D. Cataudella PsyD CPsych, § || # N. Culos-Reed PhD, H. Davis,* N. Duong,* F. Gibson RN PhD, M. Götte PhD, P. Hinds RN PhD,** †† †† † ‡‡ §§ S.L. Nijhof MD PhD, P. van der Torre, S. Cabral, L.L. Dupuis MScPhm PhD,* and L. Sung MD PhD* ABSTRACT Background Our objective was to determine whether, compared with control interventions, pharmacologic interventions reduce the severity of fatigue in patients with cancer or recipients of hematopoietic stem-cell transplantation (hsct). Methods For a systematic review, we searched medline, embase, the Cochrane Central Register of Controlled Trials, cinahl, and Psychinfo for randomized trials of systemic pharmacologic interventions for the management of fatigue in patients with cancer or recipients of hsct. Two authors independently identified studies and abstracted data. Methodologic quality was assessed using the Cochrane Risk of Bias tool. The primary outcome was fatigue severity measured using various fatigue scales. Data were synthesized using random-effects models. Results In the 117 included trials (19,819 patients), the pharmacologic agents used were erythropoietins (n = 31), stimulants (n = 19), l-carnitine (n = 6), corticosteroids (n = 5), antidepressants (n = 5), appetite stimulants (n = 3), and other agents (n = 48). Fatigue was significantly reduced with erythropoietin [standardized mean difference (smd): –0.52; 95% confidence interval (ci): –0.89 to –0.14] and with methylphenidate (smd: –0.36; 95% ci: –0.56 to –0.15); modafinil (or armodafinil) and corticosteroids were not effective. -

Megestrol Acetate: Drug Information
Official reprint from UpToDate® www.uptodate.com ©2017 UpToDate® Megestrol acetate: Drug information Copyright 1978-2017 Lexicomp, Inc. All rights reserved. (For additional information see "Megestrol acetate: Patient drug information" and see "Megestrol acetate: Pediatric drug information") For abbreviations and symbols that may be used in Lexicomp (show table) Brand Names: US Megace ES; Megace Oral Brand Names: Canada Megace OS; Megestrol Pharmacologic Category Antineoplastic Agent, Hormone; Appetite Stimulant; Progestin Dosing: Adult Note: Megace ES suspension is not equivalent to other formulations on a mg-per-mg basis. Anorexia or cachexia associated with AIDS: Oral: Suspension: U.S. labeling: Initial: 625 mg daily (of the 125 mg/mL suspension) or 800 mg daily (of the 40 mg/mL suspension); daily doses of 400 mg to 800 mg have been found to be effective Canadian labeling: Usual dose: 400 to 800 mg once daily for at least 2 months Breast cancer, advanced: Oral: Tablet: U.S. labeling: 160 mg per day in divided doses of 40 mg 4 times daily for at least 2 months Canadian labeling: 160 mg or 125 mg/m2 daily (40 mg 4 times daily or 160 mg once daily) for at least 2 months Endometrial cancer, advanced: Oral: Tablet: U.S. labeling: 40 to 320 mg daily in divided doses for at least 2 months Canadian labeling: 80 to 320 mg or 62.5 to 250 mg/m2 daily in divided doses (40 to 80 mg 1 to 4 times daily or 160 to 320mg daily) for at least 2 months Cancer-related cachexia: Canadian labeling: Oral: Tablet: 400 to 800 mg once daily for at least 2 months Cancer-related cachexia (off-label use/dosing in U.S.): Oral: Doses ranging from 160 to 800 mg per day were effective in achieving weight gain, higher doses (>160 mg) were associated with more weight gain (Beller, 1997; Loprinzi, 1990; Loprinzi, 1993; Vadell, 1998); based on a meta-analysis, an optimal dose has not been determined (Ruiz Garcia, 2013) Dosing: Geriatric Use with caution; refer to adult dosing. -

Generic Name Brand Name
Florida AIDS Drug Assistance Program (ADAP) Formulary MAY 2021 *Indicates controlled substance. Unless otherwise noted, all brands, strengths and dosage forms may be ordered pending wholesaler availability. Brand Name (listed for Generic Name Therapeutic Classification Pharmacologic Classification Antiretroviral drugs only) abacavir (ABC) Ziagen Antiretroviral Nucleoside reverse transcriptase inhibitor (NRTI) abacavir/lamivudine (ABC/3TC) Epzicom Antiretroviral NRTI combo abacavir/lamivudine/zidovudine (ABC/3TC/AZT) Trizivir Antiretroviral NRTI combo atazanavir (ATV) Reyataz Antiretroviral Protease inhibitor (PI) atazanavir/cobicistat (ATV/COBI) Evotaz Antiretroviral PI/PK Enhancer bictegravir/emtricitabine/tenofovir alafenamide Biktarvy Antiretroviral INSTI/NRTI combo (BIC/TAF/FTC) cabotegravir Vocabria Antiretroviral INSTI Non-nucleoside reverse transcriptase inhibitor (NNRTI) cabotegravir/rilpivirine (CBV/RPV) Cabenuva Antiretroviral and INSTI cobicistat (COBI) Tybost Antiretroviral Pharmacokinetic enhancer darunavir (DRV) Prezista Antiretroviral Protease inhibitor (PI) darunavir/cobicistat (DRV/COBI) Prezcobix Antiretroviral PI/PK Enhancer darunavir/cobicistat/emtricitabine/tenofovir Symtuza Antiretroviral PI/NRTI combo alafenamide (DRV/COBI/FTC/TAF) dolutegravir (DTG) Tivicay Antiretroviral Integrase strand transfer inhibitor (INSTI) dolutegravir / lamivudine (DTG/3TC) Dovato Antiretroviral INSTI/NRTI combo dolutegravir/abacavir/lamivudine (DTG/ABC/3TC) Triumeq Antiretroviral INSTI/NRTI combo dolutegravir/rilpivirine (DTG/RPV) Juluca -

Cyproheptadine for Central Hypertension?
OPEN ACCESS Research article Cyproheptadine for central hypertension? Guido Filler1,2,*, Lara Hart1, April Chan3, Elizabeth Cairney4, Asuri N Prasad5 1Department of Paediatrics, Division of Paediatric Nephrology, Schulich School ABSTRACT of Medicine & Dentistry, London, ON, Background: Approximately one-fifth of paediatric intracranial tumors result in hypertension. Canada N6A 5W9 2Department of Pathology and The condition is difficult to treat in this population, particularly if it is refractory, since there is little Laboratory Medicine, Schulich School of guidance on patient management beyond first-line therapy with IV labetalol. Medicine & Dentistry, University of Western Ontario, London, Ontario, Methods: A 20-month-old patient was hospitalized with cerebral herniation-induced loss of Canada N5A 5A5 consciousness and a posterior fossa mass was found. Although several first-line treatments including 3 School of Pharmacy, University of IV labetalol, furosemide, amlodipine, clonidine, and atenolol were administered, the patient’s Western Ontario, London, ON, Canada 5A 5A5 hypertension persisted. With few options left, positive findings from previously published case reports 4Department of Paediatrics, Division of led the team to administer cyproheptadine. Hematology/Oncology, Schulich School of Medicine & Dentistry, London, ON, Results: Cyproheptadine resulted in improved blood pressure and allowed for a dose reduction in Canada N6A 5W9 other antihypertensives, but elevated liver transaminases and suspected hepatotoxicity several weeks 5 Department of Paediatrics, Division of later resulted in the discontinuation of this treatment. Neurology, Schulich School of Medicine & Dentistry, London, ON, Canada N6A Conclusions: Despite the safety concerns associated with using cyproheptadine to treat paediatric 5W9 central hypertension, this treatment holds promise for persistent refractory hypertension as a last-line *Email: [email protected] agent when all other treatment options are exhausted. -

Treatment of Anorexia and Weight Loss with Megestrol Acetate in Patients with Cystic Fibrosis
Pediatric Pulmonology 28:380–382 (1999) Treatment of Anorexia and Weight Loss With Megestrol Acetate in Patients With Cystic Fibrosis Samya Z. Nasr, MD,1* Martin E. Hurwitz, MD,1 Randall W. Brown, MD,1 Mahmoud Elghoroury, MD,3 and David Rosen, MD2 Summary: Four patients with severe cystic fibrosis lung disease, anorexia and weight loss, received Megestrol Acetate (MA), as an appetite stimulant. The initial dose was 400–800 mg daily and was continued for 6–15 months. Appetite was improved, with significant weight gain in all patients and an increase in their weight for age percentile from <5% at the start of the study to approximately the 25th percentile after 6 months of use and improvement in quality of life. One patient discontinued MA after 6 months, and subsequently appetite and weight were depressed. Pediatr Pulmonol. 1999; 28:380–382. © 1999 Wiley-Liss, Inc. Key words: cystic fibrosis; megestrol acetate; anorexia. INTRODUCTION ated in these patients to stimulate their appetite. This appears to be an innovative way of treating these termi- Weight loss is a common problem in patients with nally ill patients to improve their nutritional status and advanced cystic fibrosis (CF). 24.4% of patients with CF decrease their pulmonary symptoms. fell below the fifth percentile of weight for age in 1996.1 Inadequate weight gain in CF is thought to be due to energy imbalance related to the increased caloric de- CASE REPORTS mands of chronic respiratory disease, and possibly an elevated metabolic rate compounded by malabsorption Four children and adolescents with CF (3 females and and anorexia.2 With progression of the pulmonary dis- 1 male) ages 10–18.5 years, received MA in an effort to ease and anorexia, some patients may fail to gain weight stimulate their appetite and improve weight gain. -

Pain Assessment and Treatment in Children with Significant Impairment of the Central Nervous System Julie Hauer, Amy J
CLINICAL REPORT Guidance for the Clinician in Rendering Pediatric Care Pain Assessment and Treatment in Julie Hauer, MD, FAAP, a, b Amy J. Houtrow, MD, PhD, MPH, FAAP, c SECTION ON HOSPICE ChildrenAND PALLIATIVE MEDICINE, COUNCIL With ON CHILDREN Significant WITH DISABILITIES Impairment of the Central Nervous System Pain is a frequent and significant problem for children with impairment abstract of the central nervous system, with the highest frequency and severity occurring in children with the greatest impairment. Despite the significance of the problem, this population remains vulnerable to underrecognition and undertreatment of pain. Barriers to treatment may include uncertainty in identifying pain along with limited experience and fear with the use of aComplex Care Service, Division of General Pediatrics, Boston medications for pain treatment. Behavioral pain-assessment tools are Children’s Hospital, Assistant Professor, Harvard Medical School, Boston Massachusetts; bSeven Hills Pediatric Center, Groton, reviewed in this clinical report, along with other strategies for monitoring Massachusetts; and cDepartment of Physical Medicine and Rehabilitation, University of Pittsburgh, Pediatric Rehabilitation pain after an intervention. Sources of pain in this population include Medicine, Rehabilitation Institute, Children’s Hospital of Pittsburgh of acute-onset pain attributable to tissue injury or inflammation resulting UPMC, Pittsburgh, Pennsylvania in nociceptive pain, with pain then expected to resolve after treatment Dr Hauer conceptualized and drafted the initial manuscript, reviewed and responded to questions and comments from all reviewers, and directed at the source. Other sources can result in chronic intermittent pain contributed to writing the final manuscript; Dr Houtrow contributed that, for many, occurs on a weekly to daily basis, commonly attributed to to the initial drafting and editing at all stages, including the final manuscript; and all authors approved the final manuscript as gastroesophageal reflux, spasticity, and hip subluxation. -

State of the Art Appetite Stimulants Use in Cystic Fibrosis
Pediatric Pulmonology 43:209–219 (2008) State of the Art Appetite Stimulants Use in Cystic Fibrosis 1 2 Samya Z. Nasr, MD * and Donna Drury, MSc, RD Summary. Cystic fibrosis (CF) is an autosomal recessive disease. It affects multiple body organs. The lungs and pancreas are the most affected which results in progressive lung damage and pancreatic insufficiency.Due to the disease process, CF patients require significantly higher caloric intake than recommended for other individuals. The nutritional goal for CF patients is to achieve normal growth and development and, once genetic potential is reached, to maintain good nutritional status throughout life. Evidence has shown that lung function is closely associated with nutritional status in CF and that nutritional status is an independent predictor of survival. Most CF patients are on a high calorie diet to help achieve normal growth and development and maintain good lung function. Inadequate caloric intake in CF can lead to malnutrition. Malnutrition in CF requires careful, multidisciplinary history taking, physical exam, and overall patient/family assessment. Only by determining the actual cause of the malnutrition can appropriate and safe therapies be used to treat it. Appetite stimulants, although efficacious in treating malnutrition in CF, should only be prescribed if decreased food intake secondary to inadequate appetite is the principal cause of the malnutrition and all other contributing factors have been assessed, ruled-out or treated. In this review, we attempted to summarize the use of several appetite stimulants used in CF and other diseases to improve appetite and maximize caloric intake. Pediatr Pulmonol. 2008; 43:209–219. -

Ryan White Part a Formulary
Ryan White Part A Formulary Updated ƵŐƵƐƚ 2019 Ryan White Part A Pharmacy Formulary - Updated 8/19/19 Tier 1: In order to access Tier 1, clients must qualify for the Ryan White Part A Program based on eligiblity requirements. Drug Classification Brand Name Generic Name Tier 5-Alpha-Reductase Inhibitors/BPH Avodart Dutasteride 1 Anticoagulant/Factor Xa Inhibitors Xarelto Rivaroxaban 1 Antihyperlipidemic Agents- Dietary Source Omega 3 Alpha-Linoleic Acid 1 Antiinfectives/Antifungal Lamisil Terbinafine 1 Antiinfectives/Antiinflammatory Decadron Dexamethasone 1 Antiinfectives/Antiinflammatory Deltasone Prednisone 1 Antiinfectives/Antiinflammatory Medrol dosepak Methyprednisolone 1 Antiinfectives/Antitubercular Rifamate Isoniazid/Rifampin 1 Antiinfectives/Antitubercular Seromycin Cycloserine 1 Antiinfectives/Antiviral/Antibacterial Achromycin Tetracycline 1 Antiinfectives/Antiviral/Antibacterial Amoxil Amoxicillin 1 Antiinfectives/Antiviral/Antibacterial Augmentin Amoxicillin/Clavulanate Potassium 1 Antiinfectives/Antiviral/Antibacterial Bicillin LA Penicillin Benzath 1 Antiinfectives/Antiviral/Antibacterial Ceftin Cefuroxime 1 Antiinfectives/Antiviral/Antibacterial Cipro Ciprofloxacin 1 Antiinfectives/Antiviral/Antibacterial Cleocin Clindamycin 1 Antiinfectives/Antiviral/Antibacterial Ery-tab Erythromycin base 1 Antiinfectives/Antiviral/Antibacterial Keflex Cephalexin 1 Antiinfectives/Antiviral/Antibacterial Macrodantin Nitrofurantoin 1 Antiinfectives/Antiviral/Antibacterial Omnicef Cefdinir 1 Antiinfectives/Antiviral/Antibacterial PenVK Penicililn -

A Review of Palliative Therapies for Cancer- Associated Anorexia
58 Review Article A hunger for hunger: a review of palliative therapies for cancer- associated anorexia Daniel S. Childs1, Aminah Jatoi2 1Department of Medicine, 2Department of Oncology, Mayo Clinic, Rochester, MN, USA Contributions: (I) Conception and design: All authors; (II) Administrative support: DS Childs; (III) Provision of study materials or patients: None; (IV) Collection and assembly of data: All authors; (V) Data analysis and interpretation: All authors; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Aminah Jatoi, MD. Mayo Clinic, 200 First Street SW, Rochester, MN 55905, USA. Email: [email protected]. Abstract: Cancer-associated anorexia, or loss of appetite, is prevalent, distressing to patients and their families, and associated with poorer outcomes in patients with advanced cancer. A well-defined therapeutic strategy remains to be defined. We present here a review of appetite loss in cancer patients with a summary of how best to manage this symptom. Keywords: Loss of appetite, anorexia, appetite stimulants, cancer, nutrition Submitted Mar 05, 2018. Accepted for publication May 07, 2018. doi: 10.21037/apm.2018.05.08 View this article at: http://dx.doi.org/10.21037/apm.2018.05.08 Introduction of appetite is common among cancer patients. What are the implications of loss of appetite in patients Many patients with advanced, incurable cancer suffer with cancer? Importantly, cancer-associated loss of appetite from loss of appetite, herein referred to as anorexia. The is not a simple, isolated symptom. It often occurs in the prevalence of this symptom varies from study to study. presence of a multiplicity of other symptoms like pain, Reporting on data from the PreMiO Study that included fatigue, and weakness; however, even after accounting 1,952 cancer patients, Muscaritoli and others noted that for the effects of other variables, the presence of cancer- 40% of patients reported loss of appetite as per a validated associated anorexia was found to strongly influence patient questionnaire (1). -

Assessment of Compounded Transdermal Mirtazapine As an Appetite Stimulant in Cats with Chronic Kidney Disease
Assessment of compounded transdermal mirtazapine as an appetite stimulant in cats with chronic kidney disease. Reference: Quimby, J. M. et al. (2020) ‘Assessment of compounded transdermal mirtazapine as an appetite stimulant in cats with chronic kidney disease’, Journal of Feline Medicine and Surgery, 22(4), pp. 376–383. doi: 10.1177/1098612X19851303. Outline: Oral mirtazapine has been shown to stimulate appetite in cats. Some cates are not amenable to oral medications and particularly in chronic kidney disease (CKD) cats (and owners) can be burdened by the large number of pills that are prescribed. This study was performed in the USA, before the approval of transdermal mirtazapine ointment there (Mirataz). The purpose of this study was to assess the appetite stimulation properties of compounded transdermal mirtazapine (CTM) in cats with CKD. Population: Cats with stable IRIS stage 2 or 3 CKD with a history of hyporexia. Intervention: Transdermal mirtazapine followed by placebo (or vice versa) given every other day for 3 weeks. Outcome and comparison: Assessment of owner reported clinical signs, clinical assessment by a vet and serum biochemistry. The Study: Double blinded placebo-controlled prospective crossover study at Ohio State Uni. Mirtazapine or placebo given every other day for 3 weeks, 4 day washout then opposite treatment given. The study population: Inclusion – stable (not defined) IRIS stage 2 or 3 CKD. Serum biochemistry, haematology, urine culture, blood pressure and total T4. Exclusion – concurrent systemic illness, pyelonephritis, ureteral obstruction, decompensation of CKD or recent hospitalisation. Owners documented appetite, rate of food ingestion, begging behaviour, activity and vocalisation as increased, decreased or unchanged. -

Venous Thromboembolism and Weight Changes in Veteran Patients Using Megestrol Acetate As an Appetite Stimulant
Venous Thromboembolism and Weight Changes in Veteran Patients Using Megestrol Acetate as an Appetite Stimulant Brandon LaMarr, PharmD, BCPS; and Russell Crawford, BPharm, BCOP These study investigators sought to answer the question whether patients treated with megestrol acetate at a local VA health care system have a greater incidence of venous thromboembolism than that seen in the general population. norexia and cachexia are occur in any patient, they are com- to thrombogenic processes associated associated with a variety of monly seen in patients with cancer with the disease and its treatments.9-11 diseases, including cancer, and AIDS. Cachexia in patients with The overall prevalence of VTE in pa- A acquired immunodeficiency cancer can be due to decreased ca- tients taking MA is unclear, as studies syndrome (AIDS), congestive heart loric intake (possibly due to causes have focused on single diseases such failure, chronic obstructive pulmo- such as gastrointestinal tumors or as cancer or AIDS. The MA prescrib- nary disease, liver disease, end-stage chemotherapy-induced nausea and ing information cautions against use renal disease, and endocrine abnor- vomiting), an increased metabolic in patients with a history of venous malities such as hyperthyroidism, state, or the production of proin- thromboembolic disease, but the adrenal insufficiency, and diabetes flammatory mediators such as inter- prevalence and degree of risk are not mellitus.1 Anorexia has also been leukin-1, interleukin-6, and tumor stated.12 For this reason, many of the shown to be associated with the necrosis factor-α. AIDS-related ca- studies evaluating the efficacy of MA aging process.2 Loss of appetite, lean chexia can be caused by a hyper- have excluded patients with a history muscle mass, and adipose tissue is metabolic state, secondary infection, of VTE.