Achieving Excellence in the Osce
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Drug Mechanisms
REVIEW OF OPTOMETRY EARN 2 CE CREDITS: Don’t Be Stumped by These Lumps and Bumps, Page 70 ■ VOL. 154 NO. 4 April 15, 2017 www.reviewofoptometry.com TH ■ 10 ANNUAL APRIL 15, 2017 PHARMACEUTICALS REPORT ■ ANNUAL PHARMACEUTICALS REPORT An Insider’s View of DRUG MECHANISMS ■ CE: DIFFERENTIAL DIAGNOSIS OF EYELID LESIONS CE: DIFFERENTIAL DIAGNOSIS OF EYELID LESIONS You can choose agents with greater precision—and evaluate their performance better—when you know what makes them tick. • How Antibiotics Work—and Why They Sometimes Don’t, Page 30 • Glaucoma Therapy: Finding the Right Combination, Page 46 • Anti-inflammatories: Sort Out Your Many Steroids and NSAIDs, Page 40 • Dry Eye: Master the Science Beneath the Surface, Page 56 • Resist the Itch: Managing Allergic Conjunctivitis, Page 64 001_ro0417_fc.indd 1 4/4/17 2:21 PM . rs ke ee S t S up r po fo rtiv Com e. Nature Lovers. Because I know their eyes are prone to discomfort, I prescribe the 1-DAY ACUVUE® MOIST Family. § 88% of all BLINK STABILIZED® Design contact lenses were fi tted in the fi rst attempt, and 99.5% within 2 trial fittings. ** Based on in vitro data. Clinical studies have not been done directly linking differences in lysozyme profi le with specifi c clinical benefi ts. * UV-blocking percentages are based on an average across the wavelength spectrum. † Helps protect against transmission of harmful UV radiation to the cornea and into the eye. ‡ WARNING: UV-absorbing contact lenses are NOT substitutes for protective UV-absorbing eyewear such as UV-absorbing goggles or sunglasses because they do not completely cover the eye and surrounding area. -

Respiratory Examination Cardiac Examination Is an Essential Part of the Respiratory Assessment and Vice Versa
Respiratory examination Cardiac examination is an essential part of the respiratory assessment and vice versa. # Subject steps Pictures Notes Preparation: Pre-exam Checklist: A Very important. WIPE Be the one. 1 Wash your hands. Wash your hands in Introduce yourself to the patient, confirm front of the examiner or bring a sanitizer with 2 patient’s ID, explain the examination & you. take consent. Positioning of the patient and his/her (Position the patient in a 3 1 2 Privacy. 90 degree sitting position) and uncover Exposure. full exposure of the trunk. his/her upper body. 4 (if you could not, tell the examiner from the beginning). 3 4 Examination: General appearance: B (ABC2DEVs) Appearance: young, middle aged, or old, Begin by observing the and looks generally ill or well. patient's general health from the end of the bed. Observe the patient's general appearance (age, Around the bed I can't state of health, nutritional status and any other see any medications, obvious signs e.g. jaundice, cyanosis, O2 mask, or chest dyspnea). 1 tube(look at the lateral sides of chest wall), metered dose inhalers, and the presence of a sputum mug. 2 Body built: normal, thin, or obese The patient looks comfortable and he doesn't appear short of breath and he doesn't obviously use accessory muscles or any heard Connections: such as nasal cannula wheezes. To determine this, check for: (mention the medications), nasogastric Dyspnea: Assess the rate, depth, and regularity of the patient's 3 tube, oxygen mask, canals or nebulizer, breathing by counting the respiratory rate, range (16–25 breaths Holter monitor, I.V. -

Visual Examination
Visual Examination • Consider the impact of chest shape on the respiratory condition of the patient – Barrel chest – Kyphosis – Scoliosis – Pectus excavatum (funnel chest) – Pectus carinatum Visual Assessment of Thorax • Thoracic scars from previous surgery • Chest symmetry • Use of accessory muscles • Bruising • In drawing of ribs • Flail segment www.nejm.org/doi/full/10.1056/NEJMicm0904437 • Paradoxical breathing /seesaw breathing • Pursed lip breathing • Nasal flaring Palpation • For vibration of secretion • Surgical emphysema • Symmetry of chest movement • Tactile vocal fremitus • Check for a tracheal tug • Palpate Nodes http://www.ncbi.nlm.nih.gov/books/NBK368/ https://m.youtube.com/watch?v=uzgdaJCf0Mk Auscultation • Is there any air entry? • Differentiate – Normal vesicular sounds – Bronchial breathing – Wheeze – Distinguish crackles • Fine • Coarse • During inspiration or expiration • Profuse or scanty – Absent sounds – Vocal resonance http://www.easyauscultation.com/lung-sounds.aspx Percussion • Tapping of the middle phalanx of the left middle finger with the right middle finger • Sounds should be resonant but may be – Hyper resonant – Dull – Stony Dull http://stanfordmedicine25.stanford.edu/the25/pulmonary.html Pathological Expansion Mediastinal Percussion Breath Further Process Displacement Note Sounds Examination Consolidation Reduced on None Dull Bronchial affected side breathing Vocal resonance Whispering pectoriloquy Collapse Reduced on Towards Dull Reduced None affected side affected side Pleural Reduced on Towards Stony dull Reduced/ Occasional rub effusion affected side opposite side Absent Empyema Asthma Reduced None Resonant Normal/ Wheeze throughout Reduced COPD Reduced None Resonant/ Normal/ Wheeze throughout Hyper-resonant Reduced Pulmonary Normal or None Normal Normal Bibasal crepitations Fibrosis reduced throughout Pneumothorax Reduced on Towards Hyper-resonant Reduced/ None affected side opposite side Absent http://www.cram.com/flashcards/test/lung-sounds-886428 sign up and test yourself.. -
Pediatrics-EOR-Outline.Pdf
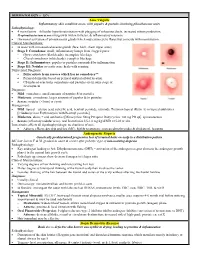
DERMATOLOGY – 15% Acne Vulgaris Inflammatory skin condition assoc. with papules & pustules involving pilosebaceous units Pathophysiology: • 4 main factors – follicular hyperkeratinization with plugging of sebaceous ducts, increased sebum production, Propionibacterium acnes overgrowth within follicles, & inflammatory response • Hormonal activation of pilosebaceous glands which may cause cyclic flares that coincide with menstruation Clinical Manifestations: • In areas with increased sebaceous glands (face, back, chest, upper arms) • Stage I: Comedones: small, inflammatory bumps from clogged pores - Open comedones (blackheads): incomplete blockage - Closed comedones (whiteheads): complete blockage • Stage II: Inflammatory: papules or pustules surrounded by inflammation • Stage III: Nodular or cystic acne: heals with scarring Differential Diagnosis: • Differentiate from rosacea which has no comedones** • Perioral dermatitis based on perioral and periorbital location • CS-induced acne lacks comedones and pustules are in same stage of development Diagnosis: • Mild: comedones, small amounts of papules &/or pustules • Moderate: comedones, larger amounts of papules &/or pustules • Severe: nodular (>5mm) or cystic Management: • Mild: topical – azelaic acid, salicylic acid, benzoyl peroxide, retinoids, Tretinoin topical (Retin A) or topical antibiotics [Clindamycin or Erythromycin with Benzoyl peroxide] • Moderate: above + oral antibiotics [Minocycline 50mg PO qd or Doxycycline 100 mg PO qd], spironolactone • Severe (refractory nodular acne): oral -

THE DUBLIN MEDICAL SCHOOL and ITS INFLUENCE UPON MEDICINE in AMERICA1 by DAVID RIESMAN, M.D
THE DUBLIN MEDICAL SCHOOL AND ITS INFLUENCE UPON MEDICINE IN AMERICA1 By DAVID RIESMAN, M.D. PROFESSOR OF CLINICAL MEDICINE IN THE UNIVERSITY OF PENNSYLVANIA PHILADELPHIA, PA. HE Irish, a mixture of primitive universal genius like Robert Boyle, Ireland pre-Celtic peoples and of Goidelic did not produce a perpetuating body of Celts coming from the European learned men who made their influence felt T continent, developed in the early beyond the confines of the Green Island. Middle Ages, out of their own resources Of the history of Irish medicine in the and untouched in any marked degree by the Middle Ages, little is known and the all-pervading influence of Rome, a remark subject is largely an untilled field. Norman able indigenous culture. In particular they Moore (St. Barth. Hosp. Rep., 1875, it elaborated a native type of Christianity 145) has resuscitated a few of the original which with characteristic energy and manuscripts in the Irish language. Most wandering spirit they carried to Scotland, of them are translations from the works of to Northern England—to Northumbria—to Bernard de Gordon, especially from his France, to Belgium, and to Switzerland. “Lilium Medicinae”; of John of Gaddes- St. Columba, of Iona, and St. Columbanus, den’s “Rosa Anglica”; of the works of of Luxeuil, stand forth as the great militant Avicenna, of A verroes, of Isaac, and of the missionaries of that first flowering period Salernitan School. Much space is given to of Irish civilization. Although they and their the writings of Isidorus. This Isidorus is successors had to succumb to the greater the famous Spanish churchman, bishop might of Latin Christianity,2 they left of Seville, who not only was a master of dotted over Europe a number of large theology but a writer upon every branch of monasteries which became active centers of knowledge of his day. -

7/19/2018 1 Falls and Movement Disorders
7/19/2018 Falls and Movement Disorders Victor Sung, MD AL Medical Directors Association Annual Conference July 28, 2018 Falls and Movement Disorders • Gait Disorders and Falls • Movement Disorders Primer • Hypokinetic Movement Disorders • Hyperkinetic Movement Disorders • Other Neurologic Contributors to Falls • Non‐Neurologic Contributors to Falls • Pearls/Pitfalls Physiology/Epidemiology of Gait Disorders • 3 Key Subsystems for Maintaining Balance • Visual • Vestibular • Somatosensory / Proprioception • Gait disorders are common • 15% of people age 65 • 25% of people age 85 • Increases risk of falls by 2.5‐3 X • >80% of gait disorders in patients >65 are multifactorial • Most common are orthopedic and neurologic factors 1 7/19/2018 Epidemiology of Gait Disorders Frequency of Etiologies for Patients Referred to Neurology for Gait D/O Etiology Percent Sensory deficits 18.3% Myelopathy 16.7% Multiple infarcts 15.0% Unknown 14.2% Parkinsonism 11.7% Cerebellar degeneration / ataxia 6.7% Hydrocephalus 6.7% Psychogenic 3.3% Other* 7.5% *Other = metabolic encephalopathy, sedative drugs, toxic disorders, brain tumor, subdural hematoma Evaluation of Gait Disorders • Start with history • Do they have falls? If so, what type/setting? • In general, what setting does the gait disorder occur? • What other medical problems may be contributing? • Exam • Abnormalities on motor/sensory/cerebellar exam • What does the gait look like? Anatomy of the Motor System Overview • Localize the Lesion!! • Motor Cortex • Subcortical Corticospinal tract • Modulators -

The Ophthalmology Examinations Review
The Ophthalm logy Examinations Review Second EditionSecond Edition 7719tp.indd 1 1/4/11 8:13 PM FA B1037 The Ophthalmology Examinations Review This page intentionally left blank BB1037_FM.indd1037_FM.indd vvii 112/24/20102/24/2010 22:31:16:31:16 PPMM The Ophthalm logy Examinations Review Second Edition Tien Yin WONG National University of Singapore, Singapore & University of Melbourne, Australia With Contributions From Chelvin SNG National University Health System, Singapore Laurence LIM Singapore National Eye Centre, Singapore World Scientific NEW JERSEY • LONDON • SINGAPORE • BEIJING • SHANGHAI • HONG KONG • TAIPEI • CHENNAI 7719tp.indd 2 1/4/11 8:13 PM Published by World Scientific Publishing Co. Pte. Ltd. 5 Toh Tuck Link, Singapore 596224 USA office: 27 Warren Street, Suite 401-402, Hackensack, NJ 07601 UK office: 57 Shelton Street, Covent Garden, London WC2H 9HE Library of Congress Cataloging-in-Publication Data Wong, Tien Yin. The ophthalmology examinations review / Tien Yin Wong ; with contributions from Chelvin Sng, Laurence Lim. -- 2nd ed. p. ; cm. Includes index. ISBN-13: 978-981-4304-40-5 (hardcover : alk. paper) ISBN-10: 981-4304-40-9 (hardcover : alk. paper) ISBN-13: 978-981-4304-41-2 (pbk. : alk. paper) ISBN-10: 981-4304-41-7 (pbk. : alk. paper) 1. Ophthalmology--Outlines, syllabi, etc. 2. Ophthalmology--Examinations, questions, etc. I. Sng, Chelvin. II. Lim, Laurence. III. Title. [DNLM: 1. Eye Diseases--Examination Questions. 2. Ophthalmologic Surgical Procedures--Examination Questions. WW 18.2] RE50.W66 2011 617.7--dc22 2010054298 British Library Cataloguing-in-Publication Data A catalogue record for this book is available from the British Library. -

Seizures in Childhood Cerebral Malaria
SEIZURES IN CHILDHOOD CEREBRAL MALARIA A thesis submitted to the University of London for the degree of Doctor of Medicine June 2001 Jane Margaret Stewart Crawley MB BS, MRCP A \ Bfii ¥ V ProQuest Number: U642344 All rights reserved INFORMATION TO ALL USERS The quality of this reproduction is dependent upon the quality of the copy submitted. In the unlikely event that the author did not send a complete manuscript and there are missing pages, these will be noted. Also, if material had to be removed, a note will indicate the deletion. uest. ProQuest U642344 Published by ProQuest LLC(2015). Copyright of the Dissertation is held by the Author. All rights reserved. This work is protected against unauthorized copying under Title 17, United States Code. Microform Edition © ProQuest LLC. ProQuest LLC 789 East Eisenhower Parkway P.O. Box 1346 Ann Arbor, Ml 48106-1346 ABSTRACT Every year, more than one million children in sub-Saharan Africa die or are disabled as a result of cerebral malaria. Seizures complicate a high proportion of cases, and are associated with an increased risk of death and neurological sequelae. This thesis examines the role of seizures in the pathogenesis of childhood cerebral malaria. The clinical and electrophysiological data presented suggest that seizures may contribute to the pathogenesis of coma in children with cerebral malaria. Approximately one quarter of the patients studied had recovered consciousness within 6 hours of prolonged or multiple seizures, or had seizures with extremely subtle clinical manifestations. EEG recording also demonstrated that electrical seizure activity arose consistently from the posterior temporo-parietal region, a “watershed” area of the brain that is particularly vulnerable to hypoxia. -

Neurologic Outcomes in Friedreich Ataxia: Study of a Single-Site Cohort E415
Volume 6, Number 3, June 2020 Neurology.org/NG A peer-reviewed clinical and translational neurology open access journal ARTICLE Neurologic outcomes in Friedreich ataxia: Study of a single-site cohort e415 ARTICLE Prevalence of RFC1-mediated spinocerebellar ataxia in a North American ataxia cohort e440 ARTICLE Mutations in the m-AAA proteases AFG3L2 and SPG7 are causing isolated dominant optic atrophy e428 ARTICLE Cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy revisited: Genotype-phenotype correlations of all published cases e434 Academy Officers Neurology® is a registered trademark of the American Academy of Neurology (registration valid in the United States). James C. Stevens, MD, FAAN, President Neurology® Genetics (eISSN 2376-7839) is an open access journal published Orly Avitzur, MD, MBA, FAAN, President Elect online for the American Academy of Neurology, 201 Chicago Avenue, Ann H. Tilton, MD, FAAN, Vice President Minneapolis, MN 55415, by Wolters Kluwer Health, Inc. at 14700 Citicorp Drive, Bldg. 3, Hagerstown, MD 21742. Business offices are located at Two Carlayne E. Jackson, MD, FAAN, Secretary Commerce Square, 2001 Market Street, Philadelphia, PA 19103. Production offices are located at 351 West Camden Street, Baltimore, MD 21201-2436. Janis M. Miyasaki, MD, MEd, FRCPC, FAAN, Treasurer © 2020 American Academy of Neurology. Ralph L. Sacco, MD, MS, FAAN, Past President Neurology® Genetics is an official journal of the American Academy of Neurology. Journal website: Neurology.org/ng, AAN website: AAN.com CEO, American Academy of Neurology Copyright and Permission Information: Please go to the journal website (www.neurology.org/ng) and click the Permissions tab for the relevant Mary E. -

CHEST RADIOLOGY: Goals and Objectives
Harlem Hospital Center Department of Radiology Residency Training Program CHEST RADIOLOGY: Goals and Objectives ROTATION 1 (Radiology Years 1): Resident responsibilities: • ED chest CTs • Inpatient and outpatient plain films including the portable intensive care unit radiographs • Consultations with referring clinicians MEDICAL KNOWLEDGE: • Residents must demonstrate knowledge about established and evolving biomedical, clinical, and cognitive sciences and the application of this knowledge to patient care. At the end of the rotation, the resident should be able to: • Identify normal radiographic and CT anatomy of the chest • Identify and describe common variants of normal, including aging changes. • Demonstrate a basic knowledge of radiographic interpretation of atelectasis, pulmonary infection, congestive heart failure, pleural effusion and common neoplastic diseases of the chest • Identify the common radiologic manifestation of thoracic trauma, including widened mediastinum, signs of aortic laceration, pulmonary contusion/laceration, esophageal and diaphragmatic rupture. • Know the expected postoperative appearance in patients s/p thoracic surgery and the expected location of the life support and monitoring devices on chest radiographs of critically ill patients (intensive care radiology); be able to recognize malpositioned devices. • Identify cardiac enlargement and know the radiographic appearance of the dilated right vs. left atria and right vs. left ventricles, and pulmonary vascular congestion • Recognize common life-threatening -

Vol. 13 No. 2 December 2020 Eissn 2508-1349 Vol
eISSN 2508-1349 Vol. 13 No. 2 December 2020 eISSN 2508-1349 Vol. 13 No. 2 December 2020 pages 69 - 136 I I www.e-jnc.org eISSN 2508-1349 Vol. 13, No. 2, 31 December 2020 Aims and Scope Journal of Neurocritical Care (JNC) aims to improve the quality of diagnoses and management of neurocritically ill patients by sharing practical knowledge and professional experience with our reader. Although JNC publishes papers on a variety of neurological disorders, it focuses on cerebrovascular diseases, epileptic seizures and status epilepticus, infectious and inflammatory diseases of the nervous system, neuromuscular diseases, and neurotrauma. We are also interested in research on neurological manifestations of general medical illnesses as well as general critical care of neurological diseases. Open Access This is an Open Access article distributed under the terms of the Creative Commons Attribution Non- Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non- commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. Publisher The Korean Neurocritical Care Society Editor-in-Chief Sang-Beom Jeon Department of Neurology, Asan Medical Center, University of Ulsan College of Medicine, 88 Oylimpic-ro 43-gil, Songpa-gu, Seoul 05505, Korea Tel: +82-2-3010-3440, Fax: +82-2-474-4691, E-mail: [email protected] Correspondence The Korean Neurocritical Care Society Department of Neurology, The Catholic University College of Medicine, 222 Banpo-Daero, Seocho-Gu, Seoul 06591, Korea Tel: +82-2-2258-2816, Fax: +82-2-599-9686, E-mail: [email protected] Website: http://www.neurocriticalcare.or.kr Printing Office M2community Co. -

成人のstridorへの アプローチ 筑波大学総合診療グループ 細井崇弘 監修 筑波大学総合診療グループ 五十野博基 2017年3月9日
成人のstridorへの アプローチ 筑波大学総合診療グループ 細井崇弘 監修 筑波大学総合診療グループ 五十野博基 2017年3月9日 分野:呼吸器 テーマ:診断 症例78歳女性 主訴 呼吸困難 当院は医療過疎地にある100床程度の小規模病院。 【現病歴】高血圧、糖尿病で近医通院中。入院数日前から咳嗽がみら れていた。入院当日に近医を受診し、胸部レントゲン検査を受け肺炎 の疑いと診断され帰宅した。 20時近くまでは同居の娘が異常が無い事を確認。 24時頃に娘が帰宅すると、獣の鳴くような声が聞こえ、患者のもとに 駆け付けると呼吸苦を訴えており、救急車を要請し当院へ搬送された。 【既往歴】高血圧、糖尿病。喘息無し。 【喫煙歴】なし 入院時現症 来院時、自発開眼しているが、会話困難。 Vital sign:BP 145/90mmHg, HR 130/min, RR36/min,SpO2 86%, BT 38℃ 頸部 Stridorを聴取 BVMによる呼吸補助開始するも換気不良 上気道閉塞と判断し、7mmチューブで経口気管挿管 このとき喉頭蓋の浮腫(-) BGA(Vein):pH 7.08, PaO2 63Torr, PCO2 99.9 Torr 胸部所見では両側に軽度の coarse cracklesあり 腹部所見は異常なし 症例の経過 • インフルエンザA(+) • 呼吸器管理となり入院、ラピアクタ投与と鎮痛・鎮静 • CO2ナルコーシスは改善、耳鼻科と共に喉頭ファイバーで声門より 上部に狭窄病変が無い事を確認。 • 意識レベルも清明であり従命可能、自発呼吸も良好であり抜管 抜管後は発語もあり問題なかったが、10数分で呼吸困難を訴え、 SpO2が急激に低下したため再挿管。 再挿管時、声帯は確認できたがチューブが声帯を越えるのに非常に 難渋した。 Stridorは何が原因だったのか? 抜管による喉頭浮腫? では救急外来に来た際の最初のStridorは? Stridorが聞こえたが喉頭蓋炎ではなかったとき、 どのような鑑別疾患を上げ、 どのようにアプローチするのが良かったのか? Clinical Ques3on • 成人で気道狭窄が疑われる場合 ①鑑別診断は何か? ②初期診断のためのアプローチは? Stridorとは~身体診察~ • 強い楽音様の音で、明確な一定の音調(一般に400Hz前後)であり、 通過障害(閉塞)を示唆する。 ・Stridorは吸気時に限られる ・Stridorは常に頸部でより強く聴取されるが、wheezingは常に胸部で 聴取される。Am Rev Respir Dis.1983;143:890-892 ・気道の直径が8㎜以下になると労作時呼吸困難が出現し、 Crit Care Med 2004; 169: 1278-1297. ・気道の直系が5mm以下で安静時にも呼吸苦が出現する。 JAMA.1971;216:1984-1985 気道狭窄の分類 upper airway obstrucYon(UAO) Central airway obstrucYon(CAO) Lower airway obstrucYon(LAO) 口から(鼻腔含め)喉頭. 慢性的な閉塞性肺傷害、喘息や : :気管および主気管支 : CAOと同時に認められることも COPDなど。CAOやUAOとは典型 的には合併しない。 発症率などの疫学については、 (悪性腫瘍以外の例では) 成人での発生頻度が非常にまれであり、 詳しくは分かっていない。 Up to date: Clinical presentaon , diagnosYc evaluaon,and management of