Three Mutations in SASH1 Cause the Pathogenesy Of
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Association Weight Matrix for the Genetic Dissection of Puberty in Beef Cattle
Association weight matrix for the genetic dissection of puberty in beef cattle Marina R. S. Fortesa,b,c, Antonio Revertera,b, Yuandan Zhanga,d, Eliza Collisa,b, Shivashankar H. Nagarajb,NickN.Jonssona,c,e, Kishore C. Prayagaa,b,1, Wes Barrisa,b, and Rachel J. Hawkena,b,2 aCooperative Research Centre for Beef Genetic Technologies; bCommonwealth Scientific and Industrial Research Organization, division of Livestock Industries, Queensland Bioscience Precinct, Brisbane QLD 4067, Australia; cThe University of Queensland, School of Veterinary Science, Gatton QLD 4343, Australia; dAnimal Genetics and Breeding Unit, University of New England, Armidale NSW 2351, Australia; and eFaculty of Veterinary Medicine, University of Glasgow, Glasgow G61 1QH, United Kingdom Edited by George Seidel, Colorado State University, Fort Collins, CO, and approved June 21, 2010 (received for review February 23, 2010) We describe a systems biology approach for the genetic dissection tional data on traits related to puberty are available. For example, of complex traits based on applying gene network theory to the re- weight and condition score are often measured on occasions sults from genome-wide associations. The associations of single- throughout an animal’s development. Hence, understanding ge- nucleotide polymorphisms (SNP) that were individually associated netics of cattle puberty and its biology serves two purposes: as with a primary phenotype of interest, age at puberty in our study, a strategy to develop efficient livestock resources and as a model were explored across 22 related traits. Genomic regions were sur- for human biology. veyed for genes harboring the selected SNP. As a result, an asso- The focus of this work is to demonstrate a unique systems ap- ciation weight matrix (AWM) was constructed with as many rows proach, which we call an association weight matrix (AWM), ap- as genes and as many columns as traits. -

Discovery of Candidate DNA Methylation Cancer Driver Genes
Published OnlineFirst May 10, 2021; DOI: 10.1158/2159-8290.CD-20-1334 RESEARCH ARTICLE Discovery of Candidate DNA Methylation Cancer Driver Genes Heng Pan1,2,3, Loïc Renaud4,5,6,7, Ronan Chaligne4,5,6, Johannes Bloehdorn8, Eugen Tausch8, Daniel Mertens9, Anna Maria Fink10, Kirsten Fischer10, Chao Zhang3,6, Doron Betel3,6, Andreas Gnirke11, Marcin Imielinski1,3,4,5,12, Jérôme Moreaux13,14,15,16, Michael Hallek10, Alexander Meissner11,17, Stephan Stilgenbauer8, Catherine J. Wu11,18, Olivier Elemento1,2,3,5, and Dan A. Landau3,4,5,6 Downloaded from cancerdiscovery.aacrjournals.org on September 28, 2021. © 2021 American Association for Cancer Research. Published OnlineFirst May 10, 2021; DOI: 10.1158/2159-8290.CD-20-1334 ABSTRACT Epigenetic alterations, such as promoter hypermethylation, may drive cancer through tumor suppressor gene inactivation. However, we have limited ability to differentiate driver DNA methylation (DNAme) changes from passenger events. We developed DNAme driver inference–MethSig–accounting for the varying stochastic hypermethylation rate across the genome and between samples. We applied MethSig to bisulfite sequencing data of chronic lymphocytic leukemia (CLL), multiple myeloma, ductal carcinoma in situ, glioblastoma, and to methylation array data across 18 tumor types in TCGA. MethSig resulted in well-calibrated quantile–quantile plots and reproducible inference of likely DNAme drivers with increased sensitivity/specificity compared with benchmarked methods. CRISPR/Cas9 knockout of selected candidate CLL DNAme drivers provided a fitness advantage with and without therapeutic intervention. Notably, DNAme driver risk score was closely associated with adverse outcome in independent CLL cohorts. Collectively, MethSig represents a novel inference framework for DNAme driver discovery to chart the role of aberrant DNAme in cancer. -

TLR4 Signaling SASH1 Is a Scaffold Molecule in Endothelial
SASH1 Is a Scaffold Molecule in Endothelial TLR4 Signaling Shauna M. Dauphinee, Ashley Clayton, Angela Hussainkhel, Cindy Yang, Yoo-Jin Park, Megan E. Fuller, Josip Blonder, This information is current as Timothy D. Veenstra and Aly Karsan of September 27, 2021. J Immunol 2013; 191:892-901; Prepublished online 17 June 2013; doi: 10.4049/jimmunol.1200583 http://www.jimmunol.org/content/191/2/892 Downloaded from Supplementary http://www.jimmunol.org/content/suppl/2013/06/17/jimmunol.120058 Material 3.DC1 http://www.jimmunol.org/ References This article cites 46 articles, 14 of which you can access for free at: http://www.jimmunol.org/content/191/2/892.full#ref-list-1 Why The JI? Submit online. • Rapid Reviews! 30 days* from submission to initial decision by guest on September 27, 2021 • No Triage! Every submission reviewed by practicing scientists • Fast Publication! 4 weeks from acceptance to publication *average Subscription Information about subscribing to The Journal of Immunology is online at: http://jimmunol.org/subscription Permissions Submit copyright permission requests at: http://www.aai.org/About/Publications/JI/copyright.html Email Alerts Receive free email-alerts when new articles cite this article. Sign up at: http://jimmunol.org/alerts The Journal of Immunology is published twice each month by The American Association of Immunologists, Inc., 1451 Rockville Pike, Suite 650, Rockville, MD 20852 All rights reserved. Print ISSN: 0022-1767 Online ISSN: 1550-6606. The Journal of Immunology SASH1 Is a Scaffold Molecule in Endothelial TLR4 Signaling Shauna M. Dauphinee,*,† Ashley Clayton,*,† Angela Hussainkhel,*,‡ Cindy Yang,x Yoo-Jin Park,x Megan E. -

Transcriptomic Analysis of Monocytes from HIV-Positive Men On
Lorenz et al. Human Genomics (2019) 13:59 https://doi.org/10.1186/s40246-019-0247-x PRIMARY RESEARCH Open Access Transcriptomic analysis of monocytes from HIV-positive men on antiretroviral therapy reveals effects of tobacco smoking on interferon and stress response systems associated with depressive symptoms David R. Lorenz, Vikas Misra and Dana Gabuzda* Abstract Background: Tobacco smoking induces immunomodulatory and pro-inflammatory effects associated with transcriptome changes in monocytes and other immune cell types. While smoking is prevalent in HIV-infected (HIV+) individuals, few studies have investigated its effects on gene expression in this population. Here, we report whole-transcriptome analyses of 125 peripheral blood monocyte samples from ART-treated HIV+ and uninfected (HIV−) men enrolled in the Multicenter AIDS Cohort Study (MACS) (n=25 HIV+ smokers, n = 60 HIV+ non-smokers, n = 40 HIV− non-smoking controls). Gene expression profiling was performed using Illumina HumanHT-12 Expression BeadChip microarrays. Differential expression analysis was performed with weighted linear regression models using the R limma package, followed by functional enrichment and Ingenuity Pathway analyses. Results: A total of 286 genes were differentially expressed in monocytes from HIV+ smokers compared with HIV− non-smokers; upregulated genes (n = 180) were enriched for immune and interferon response, chemical/stress response, mitochondria, and extracellular vesicle gene ontology (GO) terms. Expression of genes related to immune/interferon responses (AIM2, FCGR1A-B, IFI16, SP100), stress/chemical responses (APAF1, HSPD1, KLF4), and mitochondrial function (CISD1, MTHFD2, SQOR) was upregulated in HIV+ non-smokers and further increased in HIV+ smokers. Gene expression changes associated with smoking in previous studies of human monocytes were also observed (SASH1, STAB1, PID1, MMP25). -

S42003-020-01397-Z.Pdf
ARTICLE https://doi.org/10.1038/s42003-020-01397-z OPEN HACS1 signaling adaptor protein recognizes a motif in the paired immunoglobulin receptor B cytoplasmic domain Jamie J. Kwan1, Sladjana Slavkovic 2, Michael Piazza2, Dingyan Wang4, Thorsten Dieckmann3, ✉ 1234567890():,; Philip E. Johnson 2, Xiao-Yan Wen4 & Logan W. Donaldson 1 Hematopoietic adaptor containing SH3 and SAM domains-1 (HACS1) is a signaling protein with two juxtaposed protein–protein interaction domains and an intrinsically unstructured region that spans half the sequence. Here, we describe the interaction between the HACS1 SH3 domain and a sequence near the third immunoreceptor tyrosine-based inhibition motif (ITIM3) of the paired immunoglobulin receptor B (PIRB). From surface plasmon resonance binding assays using a mouse and human PIRB ITIM3 phosphopeptides as ligands, the HACS1 SH3 domain and SHP2 N-terminal SH2 domain demonstrated comparable affinities in the micromolar range. Since the PIRB ITIM3 sequence represents an atypical ligand for an SH3 domain, we determined the NMR structure of the HACS1 SH3 domain and performed a chemical shift mapping study. This study showed that the binding site on the HACS1 SH3 domain for PIRB shares many of the same amino acids found in a canonical binding cleft normally associated with polyproline ligands. Molecular modeling suggests that the respective binding sites in PIRB ITIM3 for the HACS1 SH3 domain and the SHP2 SH2 domain are too close to permit simultaneous binding. As a result, the HACS1-PIRB partnership has the potential to amalgamate signaling pathways that influence both immune and neuronal cell fate. 1 Department of Biology, York University, 4700 Keele Street, Toronto M3J 1P3 ON, Canada. -

Novel Missense Mutation of SASH1 in a Chinese Family With
Cao et al. BMC Med Genomics (2021) 14:168 https://doi.org/10.1186/s12920-021-01014-w RESEARCH ARTICLE Open Access Novel missense mutation of SASH1 in a Chinese family with dyschromatosis universalis hereditaria Lu Cao1,2,3,4,5†, Ruixue Zhang1,2,3,4,5†, Liang Yong1,2,3,4,5, Shirui Chen1,2,3,4,5, Hui Zhang1,2,3,4,5, Weiwei Chen1,2,3,4,5, Qiongqiong Xu1,2,3,4,5, Huiyao Ge1,2,3,4,5, Yiwen Mao1,2,3,4,5, Qi Zhen1,2,3,4,5, Yafen Yu1,2,3,4,5, Xia Hu1,2,3,4,5 and Liangdan Sun1,2,3,4,5* Abstract Background: Dyschromatosis universalis hereditaria (DUH) is a pigmentary dermatosis characterized by generalized mottled macules with hypopigmention and hyperpigmention. ABCB6 and SASH1 are recently reported pathogenic genes related to DUH, and the aim of this study was to identify the causative mutations in a Chinese family with DUH. Methods: Sanger sequencing was performed to investigate the clinical manifestation and molecular genetic basis of these familial cases of DUH, bioinformatics tools and multiple sequence alignment were used to analyse the patho- genicity of mutations. Results: A novel missense mutation, c.1529G>A, in the SASH1 gene was identifed, and this mutation was not found in the National Center for Biotechnology Information Database of Short Genetic Variation, Online Mendelian Inherit- ance in Man, ClinVar, or 1000 Genomes Project databases. All in silico predictors suggested that the observed sub- stitution mutation was deleterious. Furthermore, multiple sequence alignment of SASH1 revealed that the p.S510N mutation was highly conserved during evolution. -

Substitutions of Short Heterologous DNA Segments of Intragenomic Or Extragenomic Origins Produce Clustered Genomic Polymorphisms
Substitutions of short heterologous DNA segments of intragenomic or extragenomic origins produce clustered genomic polymorphisms Klaus Harmsa,b,1, Asbjørn Lunnana, Nils Hülterc, Tobias Mourierb, Lasse Vinnerb, Cheryl P. Andamd, Pekka Marttinene, Helena Fridholmb,f, Anders Johannes Hansenb, William P. Hanaged, Kaare Magne Nielseng,h, Eske Willerslevb,1, and Pål Jarle Johnsena,1 aDepartment of Pharmacy, Faculty of Health Sciences, The Arctic University of Norway, 9037 Tromsø, Norway; bCentre for GeoGenetics, Natural History Museum of Denmark, University of Copenhagen, 1350 Copenhagen K, Denmark; cGenomic Microbiology, Institute of Microbiology, Christian-Albrechts- Universität zu Kiel, 24118 Kiel, Germany; dDepartment of Epidemiology, Harvard T. H. Chan School of Public Health, Boston, MA 02115; eHelsinki Institute for Information Technology, Department of Computer Science, Aalto University, FIN-00076 Aalto, Finland; fDepartment of Microbiological Diagnostics and Virology, Statens Serum Institut, 2300 Copenhagen S, Denmark; gDepartment of Life Sciences and Health, Oslo and Akershus University College of Applied Sciences, 0130 Oslo, Norway; and hGenØk-Center for Biosafety, 9294 Tromsø, Norway Edited by John R. Roth, University of California, Davis, CA, and approved November 22, 2016 (received for review September 23, 2016) In a screen for unexplained mutation events we identified a pre- polymorphisms, although in retrospective studies, such sequen- viously unrecognized mechanism generating clustered DNA polymor- tial events are nearly impossible to verify. phisms such as microindels and cumulative SNPs. The mechanism, The most diverse clusters of nucleotide variations are formed short-patch double illegitimate recombination (SPDIR), facilitates by microhomology-mediated end-joining (MMEJ). MMEJ has short single-stranded DNA molecules to invade and replace genomic been observed in eukaryotes only and can repair DNA double- DNA through two joint illegitimate recombination events. -

SASH1 Promotes Melanin Synthesis and Migration Via Suppression Of
Int. J. Biol. Sci. 2020, Vol. 16 1264 Ivyspring International Publisher International Journal of Biological Sciences 2020; 16(7): 1264-1273. doi: 10.7150/ijbs.38415 Research Paper SASH1 promotes melanin synthesis and migration via suppression of TGF-β1 secretion in melanocytes resulting in pathologic hyperpigmentation Hongzhou Cui1,2,3*, Shuping Guo1*, Hongxia He1, Huina Guo2,3, Yuliang Zhang2,3, Binquan Wang1,2,3 1. Department of Dermatology, the First Hospital, Shanxi Medical University, Taiyuan, Shanxi, China 2. Shanxi Key Laboratory of Otorhinolaryngology Head and Neck Cancer, Shanxi Medical University, Taiyuan, Shanxi, China 3. The Key Scientific and Technological Innovation Platform for Precision Diagnosis and Treatment of Head and Neck Cancer, Shanxi Province, Taiyuan 030001, Shanxi, China * Hongzhou Cui and Shuping Guo contributed equally as first authors. Corresponding author: Binquan Wang, Department of Dermatology, the First Hospital, Shanxi Medical University; Shanxi Key Laboratory of Otorhinolaryngology Head and Neck Cancer, Shanxi Medical University; The Key Scientific and Technological Innovation Platform for Precision Diagnosis and Treatment of Head and Neck Cancer, Taiyuan, Shanxi, China; E-mail: [email protected] © The author(s). This is an open access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0/). See http://ivyspring.com/terms for full terms and conditions. Received: 2019.07.14; Accepted: 2019.12.14; Published: 2020.02.10 Abstract Dyschromatosis universalis hereditaria (DUH) is an autosomal dominant pigmentary genodermatosis characterized by the presence of patches of hyperpigmentation and hypopigmented macules distributed over the body, with most cases reported in Asia. DUH is a heterogeneous disease and a small portion of patients carry the ABCB6 variant. -

Quantitative Proteomics Analysis of Glioblastoma Cell Lines After Lncrna HULC Silencing Shan Ye1, Jing Wu2,3, Yiran Wang1, Yuchen Hu1, Tiantian Yin1 & Jie He1,2,3*
www.nature.com/scientificreports OPEN Quantitative proteomics analysis of glioblastoma cell lines after lncRNA HULC silencing Shan Ye1, Jing Wu2,3, Yiran Wang1, Yuchen Hu1, Tiantian Yin1 & Jie He1,2,3* Glioblastoma multiforme (GBM) is a life-threatening brain tumor. This study aimed to identify potential targets of the long noncoding RNA (lncRNA) HULC that promoted the progression of GBM. Two U87 cell lines were constructed: HULC-siRNA and negative control (NC). Quantitative real-time PCR (qRT-PCR) was performed to validate the transfection efciency of HULC silencing vector. Mass spectrometry (MS) was used to generate proteomic profles for the two cell lines. Gene Ontology (GO) and Kyoto Encyclopedia of Genes and Genomes (KEGG) pathway enrichment analyses were performed to distinguish HULC-related genes and pathway mapping. Colony formation, Transwell, and wound- healing assays were used to investigate the functional efects of HULC knockdown on GBM. We identifed 112 up-regulated proteins and 24 down-regulated proteins from a total of 4360 quantifed proteins. GO enrichment illustrated that these proteins were mainly involved in organelle structure, catalysis, cell movement, and material metabolism. KEGG pathway analysis indicated that some of these proteins were signifcantly enriched in tight junction, metabolic pathways, and arachidonic acid metabolism. In vitro experiments demonstrated that HULC knockdown inhibited GBM cell proliferation, invasion, and migration. Our KEGG analyses revealed that PLA2G4A was a shared protein in several enriched pathways. HULC silencing signifcantly down-regulated the expression of PLA2G4A. Knockdown of HULC changed the proteomic characteristics of GBM and altered the behaviors of GBM cells. Specifcally, we identifed PLA2G4A as an HULC target in GBM. -

SASH1, a New Potential Link Between Smoking and Atherosclerosis Henri Weidmann
SASH1, a new potential link between smoking and atherosclerosis Henri Weidmann To cite this version: Henri Weidmann. SASH1, a new potential link between smoking and atherosclerosis. Cardiology and cardiovascular system. Université Pierre et Marie Curie - Paris VI; Universität Hamburg, 2015. English. NNT : 2015PA066267. tel-01242976 HAL Id: tel-01242976 https://tel.archives-ouvertes.fr/tel-01242976 Submitted on 14 Dec 2015 HAL is a multi-disciplinary open access L’archive ouverte pluridisciplinaire HAL, est archive for the deposit and dissemination of sci- destinée au dépôt et à la diffusion de documents entific research documents, whether they are pub- scientifiques de niveau recherche, publiés ou non, lished or not. The documents may come from émanant des établissements d’enseignement et de teaching and research institutions in France or recherche français ou étrangers, des laboratoires abroad, or from public or private research centers. publics ou privés. Université Pierre et Marie Curie Ecole Doctorale 394: Physiology and physiopathology UMRS 1166 ICAN Institute, Insitute of Cardiometabolism And Nutrition Equipe 1: Genomics and physiopathology of cardiovascular diseases SASH1, a new potential link between smoking and atherosclerosis By Henri Weidmann To obtain the Degree of Doctor of physiology and physiopathology of the University Pierre et Marie Curie Directed by Dr Ewa Ninio Co-directed by Pr Tanja Zeller Publicly presented on the 23th of September 2015 Jury: Dr Mustapha Rouis, President of the Jury Dr Marie-Paul Jacob-Lenet, Reporter Dr Alain-Pierre Gadeau, Reporter Dr Klaus-Peter Janssen, Examiner Dr Fabienne Foufelle, Examiner 1 To my family To my friends 2 “Science is a way of thinking, much more than it is a body of knowledge” Carl Sagan 3 Acknowledgment Having reached the end of my thesis, I would like to thanks all the people that made this work possible and thus allowed me to attain my fondest dream, working in biological research. -
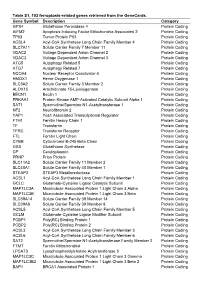
Table S1. 103 Ferroptosis-Related Genes Retrieved from the Genecards
Table S1. 103 ferroptosis-related genes retrieved from the GeneCards. Gene Symbol Description Category GPX4 Glutathione Peroxidase 4 Protein Coding AIFM2 Apoptosis Inducing Factor Mitochondria Associated 2 Protein Coding TP53 Tumor Protein P53 Protein Coding ACSL4 Acyl-CoA Synthetase Long Chain Family Member 4 Protein Coding SLC7A11 Solute Carrier Family 7 Member 11 Protein Coding VDAC2 Voltage Dependent Anion Channel 2 Protein Coding VDAC3 Voltage Dependent Anion Channel 3 Protein Coding ATG5 Autophagy Related 5 Protein Coding ATG7 Autophagy Related 7 Protein Coding NCOA4 Nuclear Receptor Coactivator 4 Protein Coding HMOX1 Heme Oxygenase 1 Protein Coding SLC3A2 Solute Carrier Family 3 Member 2 Protein Coding ALOX15 Arachidonate 15-Lipoxygenase Protein Coding BECN1 Beclin 1 Protein Coding PRKAA1 Protein Kinase AMP-Activated Catalytic Subunit Alpha 1 Protein Coding SAT1 Spermidine/Spermine N1-Acetyltransferase 1 Protein Coding NF2 Neurofibromin 2 Protein Coding YAP1 Yes1 Associated Transcriptional Regulator Protein Coding FTH1 Ferritin Heavy Chain 1 Protein Coding TF Transferrin Protein Coding TFRC Transferrin Receptor Protein Coding FTL Ferritin Light Chain Protein Coding CYBB Cytochrome B-245 Beta Chain Protein Coding GSS Glutathione Synthetase Protein Coding CP Ceruloplasmin Protein Coding PRNP Prion Protein Protein Coding SLC11A2 Solute Carrier Family 11 Member 2 Protein Coding SLC40A1 Solute Carrier Family 40 Member 1 Protein Coding STEAP3 STEAP3 Metalloreductase Protein Coding ACSL1 Acyl-CoA Synthetase Long Chain Family Member 1 Protein -

Genome-Wide Analyses Identify a Role for SLC17A4 and AADAT in Thyroid Hormone Regulation
ARTICLE DOI: 10.1038/s41467-018-06356-1 OPEN Genome-wide analyses identify a role for SLC17A4 and AADAT in thyroid hormone regulation Alexander Teumer,Teumer1,2 Layal, Layal Chaker, Chaker Stefan3,4,5, Stefan Groeneweg, Groeneweg Yong3,5 Li,, Yong Celia LiDi6, Munno, Celia Di Munno3,7, Caterina Barbieri et al.# Thyroid dysfunction is an important public health problem, which affects 10% of the general population and increases the risk of cardiovascular morbidity and mortality. Many aspects 1234567890():,; of thyroid hormone regulation have only partly been elucidated, including its transport, metabolism, and genetic determinants. Here we report a large meta-analysis of genome-wide association studies for thyroid function and dysfunction, testing 8 million genetic variants in up to 72,167 individuals. One-hundred-and-nine independent genetic variants are associated with these traits. A genetic risk score, calculated to assess their combined effects on clinical end points, shows significant associations with increased risk of both overt (Graves’ disease) and subclinical thyroid disease, as well as clinical complications. By functional follow-up on selected signals, we identify a novel thyroid hormone transporter (SLC17A4) and a metabolizing enzyme (AADAT). Together, these results provide new knowledge about thyroid hormone physiology and disease, opening new possibilities for therapeutic targets. Correspondence and requests for materials should be addressed to A.T. (email: [email protected]). #A full list of authors and their affiliations appears at the end of the paper. NATURE COMMUNICATIONS | (2018)9:4455 | DOI: 10.1038/s41467-018-06356-1 | www.nature.com/naturecommunications 1 ARTICLE NATURE COMMUNICATIONS | DOI: 10.1038/s41467-018-06356-1 hyroid dysfunction is a common clinical condition, genetic underpinnings of thyroid function.