Multiple Gestations
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
Multiple Pregnancies
Learning Objectives Using Ultrasound to Manage Twins After this presentation, the learner will be able to discuss: • Diagnosis and dating in twin pregnancies • Sonographic characteristics that distinguish dichorionic from monochorionic twins • Prenatal ultrasound screening in twins • Complications unique to monochorionic twins Lynn L. Simpson, MD Chief, Division of Maternal Fetal Medicine • Ultrasound surveillance recommendations for twins Columbia University Medical Center, New York Diagnosis and Dating of Twins Importance of Pregnancy Dating • Diagnosis best in the first trimester and dating optimal using crown-rump length • Timing for screening − 20% of first trimester twin pregnancies result in singleton live births and diagnostic testing − “Vanishing twin” is associated with favorable prognosis of surviving twin if dichorionic • Accurate interpretation of twin growth • If discrepancy in dates between the twins, date using the larger twin • Scheduling of twin deliveries − Avoids missing diagnosis of IUGR Types of Twins Determination of Chorionicity • All dizygotic twins are dichorionic • All monochorionic twins are monozygotic • Not all monozygotic twins are monochorionic • Optimal in first trimester − close to 100% accuracy • Incorrect assignment in up to 10% of cases when chorionicity determined in second trimester 2-3 days 3-8 days 8-13 days (28%) (70%) (1%) Lee et al, 2006 Blumenfeld et al, 2014 1 Determination of Chorionicity Intertwin Membrane • Gestational sacs • Amniotic sacs • Placenta number • Intertwin membrane • Gender -
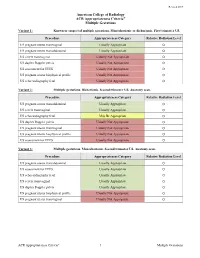
ACR Appropriateness Criteria® Multiple Gestations
Revised 2017 American College of Radiology ACR Appropriateness Criteria® Multiple Gestations Variant 1: Known or suspected multiple gestations. Monochorionic or dichorionic. First trimester US. Procedure Appropriateness Category Relative Radiation Level US pregnant uterus transvaginal Usually Appropriate O US pregnant uterus transabdominal Usually Appropriate O US cervix transvaginal Usually Not Appropriate O US duplex Doppler pelvis Usually Not Appropriate O US assessment for TTTS Usually Not Appropriate O US pregnant uterus biophysical profile Usually Not Appropriate O US echocardiography fetal Usually Not Appropriate O Variant 2: Multiple gestations. Dichorionic. Second trimester US. Anatomy scan. Procedure Appropriateness Category Relative Radiation Level US pregnant uterus transabdominal Usually Appropriate O US cervix transvaginal Usually Appropriate O US echocardiography fetal May Be Appropriate O US duplex Doppler pelvis Usually Not Appropriate O US pregnant uterus transvaginal Usually Not Appropriate O US pregnant uterus biophysical profile Usually Not Appropriate O US assessment for TTTS Usually Not Appropriate O Variant 3: Multiple gestations. Monochorionic. Second trimester US. Anatomy scan. Procedure Appropriateness Category Relative Radiation Level US pregnant uterus transabdominal Usually Appropriate O US assessment for TTTS Usually Appropriate O US echocardiography fetal Usually Appropriate O US cervix transvaginal Usually Appropriate O US duplex Doppler pelvis Usually Appropriate O US pregnant uterus biophysical profile -

Twins: New Guidelines Objective Question 1
Twins: New Guidelines What you need to know Lynn L. Simpson, MD Chief, Division of Maternal Fetal Medicine Columbia University Medical Center, New York Objective • To review the expected “standard of care” when managing twin pregnancies − to provide high-quality obstetric care − to avoid medical malpractice Question 1 Which of the following is most predictive of a twin pregnancy? a. Larger than expected uterine size b. Strong family history of twins c. Severe hyperemesis d. Elevated serum βHCG e. Conceived via ovulation stimulation 1 Clinical Suspicion of Twins • Larger than expected uterine size • Strong family history of fraternal twins • Severe hyperemesis gravidarum • Elevated serum βHCG • Assisted reproductive technologies Prior to routine use of ultrasound, 10-15% of twins diagnosed in labor Diagnosis and Dating of Twins • Diagnosis best in the first trimester and dating optimal using crown-rump length − 20% of first trimester twin pregnancies result in singleton live births − Vanishing twin associated with favorable prognosis of surviving twin, similar to singleton pregnancy • Multiple biometric measurements should be used beyond the first trimester • If discrepancy in dates between the twins, date using the larger twin Landy et al, 1986 Importance of Pregnancy Dating in Twins • Timing for screening and diagnostic testing • Accurate interpretation of twin growth • Scheduling of twin deliveries 2 Question 2 Which of the following is most characteristic of dichorionic twins? a. Single placenta b. Same gender c. Two amnions d. T-sign -
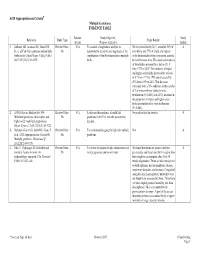
ACR Appropriateness Criteria® Multiple Gestations EVIDENCE TABLE
ACR Appropriateness Criteria® Multiple Gestations EVIDENCE TABLE Patients/ Study Objective Study Reference Study Type Study Results Events (Purpose of Study) Quality 1. Kulkarni AD, Jamieson DJ, Jones HW, Review/Other- N/A To conduct a longitudinal analysis to We estimated that by 2011, a total of 36% of 4 Jr., et al. Fertility treatments and multiple Dx determine the trends in and magnitude of the twin births and 77% of triplet and higher- births in the United States. N Engl J Med. contribution of fertility treatments to multiple order births resulted from conception assisted 2013;369(23):2218-2225. births. by fertility treatments. The observed incidence of twin births increased by a factor of 1.9 from 1971 to 2009. The incidence of triplet and higher-order births increased by a factor of 6.7 from 1971 to 1998 and decreased by 29% from 1998 to 2011. This decrease coincided with a 70% reduction in the transfer of 3 or more embryos during in vitro fertilization (P<0.001) and a 33% decrease in the proportion of triplet and higher-order births attributable to in vitro fertilization (P<0.001). 2. ACOG Practice Bulletin No. 144: Review/Other- N/A To discuss the incidence of multifetal No results stated in abstract. 4 Multifetal gestations: twin, triplet, and Dx gestations in the U.S. over the past several higher-order multifetal pregnancies. decades. Obstet Gynecol. 2014;123(5):1118-1132. 3. DeJesus Allison SO, Javitt MC, Glanc P, Review/Other- N/A To recommend imaging for high risk multiple N/A 4 et al. -
![Parasitic Twins [1]](https://docslib.b-cdn.net/cover/9842/parasitic-twins-1-5309842.webp)
Parasitic Twins [1]
Published on The Embryo Project Encyclopedia (https://embryo.asu.edu) Parasitic Twins [1] By: DeRuiter, Corinne Keywords: Fetus [2] Congenital disorders [3] Human development [4] Parasitic twins, a specific type of conjoined twins [6], occur when one twin ceases development during gestation [7] and becomes vestigial to the fully formed dominant twin, called the autositic twin. The underdeveloped twin is called parasitic because it is only partially formed, is not functional, or is wholly dependent on the autositic twin. In most cases, the phenotype of parasitic twins is one normal functioning individual with extra appendages or organs, leading to questions about whether or not the additional limbs and organs are in fact another person or just a mutation of the individual’s body. Researchers think that parasitic twins result from mechanisms similar to those that produce Vanishing Twin Syndrome [8]. On a developmental continuum with vanishing twin syndrome on one end and developmentally normal twins on the other, researchers propose that the patterns of conjoined twins [6] fall somewhere in the middle. Of the many types of parasitic twins, the most common is vestigial twins, when one individual has extra limbs or organs. The extra vestigial limbs are generally harmless to the autosite. Similarly, dipygus parasitic twins have duplications of legs, but may also have extra hands, feet, or sexual organs. An epigastric parasite describes an incomplete twin with usually just a torso or legs attached to the functioning twin’s abdomen. In some cases, there is also an undeveloped head imbedded in the autosite’s abdomen. Craniopagus parasiticus describes an autositic twin with an additional, parasitic head attached at the head. -

Twin Pregnancy a Complicating Journey for Both Mothers and Babies: Elaborate Review
International Journal of Basic & Clinical Pharmacology Shelke PS et al. Int J Basic Clin Pharmacol. 2020 Apr;9(4):674-682 http:// www.ijbcp.com pISSN 2319-2003 | eISSN 2279-0780 DOI: http://dx.doi.org/10.18203/2319-2003.ijbcp20201196 Review Article Twin pregnancy a complicating journey for both mothers and babies: elaborate review Pallavi Sitaram Shelke, Pradnya Nilesh Jagtap* Department of Pharmacology Department, PDEA’s S.G.R.S. College of Pharmacy, Saswad, Maharashtra, India Received: 18 January 2020 Revised: 04 March 2020 Accepted: 05 March 2020 *Correspondence: Dr. Pradnya Nilesh Jagtap, Email: [email protected] Copyright: © the author(s), publisher and licensee Medip Academy. This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Pregnancy, also known as gestation, is the time during which one or more offspring develops inside a woman. A multiple pregnancy involves more than one offspring, such as with twins. Pregnancy can occur by sexual intercourse or assisted reproductive technology. A pregnancy may end in a live birth, abortion, or miscarriage, though access to safe abortion care varies globally. Research shows that 10 percent to 15 percent of all singleton births may have started off as twins; often one is lost early in pregnancy in a phenomenon known as "vanishing twin syndrome." Multiple pregnancy occurs when two or more ova are fertilized to form dizygotic (non-identical) twins or a single fertilised egg divides to form monozygotic (identical) twins. -

Twin Pregnancy: Prenatal Issues
Official reprint from UpToDate® www.uptodate.com ©2017 UpToDate® Twin pregnancy: Prenatal issues Authors: Stephen T Chasen, MD, Frank A Chervenak, MD Section Editors: Charles J Lockwood, MD, MHCM, Deborah Levine, MD Deputy Editor: Vanessa A Barss, MD, FACOG All topics are updated as new evidence becomes available and our peer review process is complete. Literature review current through: Apr 2017. | This topic last updated: Apr 05, 2017. INTRODUCTION — Twin pregnancy is associated with higher rates of almost every potential complication of pregnancy, with the exceptions of postterm pregnancy and macrosomia. The most serious risk is spontaneous preterm delivery, which plays a major role in the increased perinatal mortality and short-term and long-term morbidity observed in these infants. Higher rates of fetal growth restriction and congenital anomalies also contribute to adverse outcome in twin births. In addition, monochorionic twins are at risk for complications unique to these pregnancies, such as twin-twin transfusion syndrome (TTTS), which can be lethal or associated with serious morbidity. This topic will provide an overview of the antepartum care of women with twin pregnancy. Intrapartum management is reviewed separately. (See "Twin pregnancy: Labor and delivery".) ROLE OF EARLY ULTRASOUND EXAMINATION — Ultrasound examination is the only safe and reliable method for definitive diagnosis of twin gestation. Early ultrasound assessment also provides accurate estimation of gestational age, which is important in all pregnancies, but particularly important in management of twin pregnancies because of the higher risks for preterm delivery and growth restriction. In addition, chorionicity and amnionicity can be determined by ultrasound examination (see 'Assessment of chorionicity' below). -

Scholars Journal of Medical Case Reports Fetus Papyraceus
DOI: 10.21276/sjmcr.2016.4.12.13 Scholars Journal of Medical Case Reports ISSN 2347-6559 (Online) Sch J Med Case Rep 2016; 4(12):920-922 ISSN 2347-9507 (Print) ©Scholars Academic and Scientific Publishers (SAS Publishers) (An International Publisher for Academic and Scientific Resources) Fetus papyraceus: A case report Prof. Iqbal Aziz1, Dr. Albina2 1Professor, Department of Surgery, AKTCH, Aligarh Muslim University, Aligarh, U.P, India 2Assistant Professor, Department of Surgery, STTCH, Lucknow, U.P, India. *Corresponding author Dr. Albina Email: [email protected] Abstract: Fetus papyraceus is a rare condition of multiple gestations in which one fetus dies and is flattened between the membranes of the other fetus and uterine wall. We report a case of fetus papyraceus which was detected incidentally during caesarean section. A 28 year old, gravida 2, full term patient underwent the planned caesarean section. Her all antenatal ultrasonography reports showed single live intrauterine fetus and caesarean section revealed twin gestation one being a male baby and second fetus papyraceus, which was attached to the healthy placenta by a rudimentary cord. Both the healthy mother and the healthy baby were discharged home. Fetus papyraceus is a condition which is associated with the complications for the mother and the surviving fetus thus the diagnosis of fetus papyraceus by serial/intravaginal ultrasounds and routine placental examination of placenta and rudimentary cord is mandatory. Keywords: Fetus papyraceus, Serial ultrasounds, Rudimentary cord. INTRODUCTION: cord of a healthy baby and another rudimentary cord Fetus papyraceus (FP) is a rare condition of attached to placenta with a mummified fetus [fig 3] dead twin fetus, which is compressed between the which was identified and confirmed as fetus papyraceus uterine wall and living fetus, and subsequently it is after taking an x-ray image [fig 4], The pregnancy was retained in utero. -

Multifetal Pregnancy: Early Diagnosis and Management
MULTIFETAL PREGNANCY: EARLY DIAGNOSIS AND MANAGEMENT Dr. dr. Efendi Lukas, Sp.OG(K) Divisi Fetomaternal, Departemen Obgin FK UNHAS/ RS Dr.Wahidin Sudirohusodo Makassar Is it good NEWS to be told that you are going to have twins? Pregnancy Maternal Labour complications Fetal Puerperium Content 1. Overview 2. Determining chorionicity and planning care 3. Problem specific to monochorionic and monoamniocity twins 4. Recommendations for multifetal pregnancy • Incidence of spontaneous twins :1 in 80 pregnancies triplets: 1 in 8,000 pregnancies • Incidence of Monozygotic twins: 3.5 per 1000 births. Dizygotic twins: 6.7/1000 births (Japan), 40/1000 births (Nigeria). Indonesia : ???? Risk of Multiple Fetal Pregnancy ↑ Spontaneous abortion ( 3 x) ↑ Congenital malformation Low birth weight: growth restriction, preterm , discordance Decrease duration of gestation: a. 57% of twins at 35 weeks. b. 92% of triplets at 32 weeks. c. all quadruplets at 29–30 weeks Intrauterine fetal demise of one twin (late pregnancy), Vanishing twin (early pregnancy). Multifetal gestation Stillbirth 5x, Neurologic Preterm delivery Neonatal death outcomes : 3-fold ↑ increase in cerebral 7x palsy NICU 25 % of twins, 75 % of triplets Content 2. Determining chorionicity and planning care Key priorities for implementation Determining gestational age and chorionicity 1st trimester ultrasound scan CRL is 45 -84 mm (11w 0d - 13w6d): GA, chorionicity and screen for Down's syndrome. Determine chorionicity by ultrasound using the number of placental masses, the lambda or T-sign -

Presidenza Del Consiglio Dei Ministri
Presidenza del Consiglio dei Ministri I GEMELLI CONGIUNTI E GLI INTERVENTI DI SEPARAZIONE: ASPETTI BIOETICI 19 luglio 2013 INDICE Presentazione ..................................................................................................... 3 I. Breve descrizione scientifica del fenomeno ..................................................... 5 Definizione ................................................................................................. 5 Storia ......................................................................................................... 5 Eziologia .................................................................................................... 5 Tipologie .................................................................................................... 6 Incidenza.................................................................................................... 7 II. Diagnosi prenatale .......................................................................................... 8 III. Problemi etici ................................................................................................. 8 1. I neonati/ minori ................................................................................... 10 2. I grandi minori e gli adulti ..................................................................... 14 IV. Indicazioni bioetiche .................................................................................... 16 2 Presentazione Il Comitato ha affrontato in questo parere una questione delicata che, -

What to Look for in the Ultrasound Examination of Multiple Pregnancy? Krzysztof Preis1, Małgorzata Świątkowska-Freund2
REVIEW ARTICLE What to Look for in the Ultrasound Examination of Multiple Pregnancy? Krzysztof Preis1, Małgorzata Świątkowska-Freund2 ABSTRACT Since multiple pregnancies are of higher perinatal risk to diminish the rate of complications and stillbirth, the proper ultrasound management has to be done. Twins differ in zygosity, chorionicity, and amnionicity. Authors summarize how to diagnose the type of pregnancy and its complications in ultrasound examination and what to look for to achieve as much as possible of vital information. Authors propose some general rules for sonographers: • Prenatal US—the same schedule as in singletons for assessment of fetal morphology and markers of genetic abnormalities despite special schedule for twins. • Keep patient aware about the possibility of “vanishing twin.” • Set the chorionicity as early as possible. • Set the amnionicity in the first-trimester scan. • Look for the prognostic signs of twin-to-twin transfusion syndrome (TTTS) in the first- and second-trimester scan. • Monitor the amniotic fluid volume from 16th week gestational age (GA) on. • Monitor the fetal growth from the first-trimester scan on. • Doppler US and growth every 2 weeks in monochorionic (MC) twins or every week if suspicious signs occur from the 16th week of GA on; every 4–6 weeks in DC twins. • Exam the middle cerebral artery-peak systolic velocity (MCA-PSV) in MC from the mid-pregnancy on. • Look for the cervix incompetence and the risk of preterm delivery. Keywords: Amnionicity, Chorionicity, FGR, TAPS, TRAP, Twin pregnancy, TTTS, Ultrasound, Zygosity. Donald School Journal of Ultrasound in Obstetrics and Gynecology (2020): 10.5005/jp-journals-10009-1653 The incidence of multiple pregnancies rises in recent years 1,2 enormously. -

A Review of the Mechanisms and Evidence for Typical and Atypical Twinning Helen C
Expert Reviews ajog.org OBSTETRICS A review of the mechanisms and evidence for typical and atypical twinning Helen C. McNamara, MB, BS; Stefan C. Kane, MB, BS; Jeffrey M. Craig, PhD; Roger V. Short, ScD; Mark P. Umstad, MD mirror-image twins, polar body twins, The mechanisms responsible for twinning and disorders of twin gestations have been the complete hydatidiform mole with coex- subject of considerable interest by physicians and scientists, and cases of atypical istent twin, vanishing twins, fetus papy- twinning have called for a reexamination of the fundamental theories invoked to explain raceus, fetus in fetu, superfetation, and twin gestations. This article presents a review of the literature focusing on twinning and superfecundation. A detailed discussion atypical twinning with an emphasis on the phenomena of chimeric twins, phenotypically of monoamniotic twins, conjoined discordant monozygotic twins, mirror-image twins, polar body twins, complete hydati- twins, and twin-reversed arterial perfu- diform mole with a coexistent twin, vanishing twins, fetus papyraceus, fetus in fetu, sion sequence is beyond the scope of superfetation, and superfecundation. The traditional models attributing monozygotic this review and has been presented twinning to a fission event, and more recent models describing monozygotic twinning as elsewhere.1,2 a fusion event, are critically reviewed. Ethical restrictions on scientific experimentation with human embryos and the rarity of cases of atypical twinning have limited opportu- Traditional models of twinning nities to elucidate the exact mechanisms by which these phenomena occur. Refinements Traditionally it has been thought that in the modeling of early embryonic development in twin pregnancies may have significant dizygotic twins result from fertilization clinical implications.