Targeting Cell Signaling in Allergic Asthma
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Fig. L COMPOSITIONS and METHODS to INHIBIT STEM CELL and PROGENITOR CELL BINDING to LYMPHOID TISSUE and for REGENERATING GERMINAL CENTERS in LYMPHATIC TISSUES
(12) INTERNATIONAL APPLICATION PUBLISHED UNDER THE PATENT COOPERATION TREATY (PCT) (19) World Intellectual Property Organization International Bureau (10) International Publication Number (43) International Publication Date Χ 23 February 2012 (23.02.2012) WO 2U12/U24519ft ft A2 (51) International Patent Classification: AO, AT, AU, AZ, BA, BB, BG, BH, BR, BW, BY, BZ, A61K 31/00 (2006.01) CA, CH, CL, CN, CO, CR, CU, CZ, DE, DK, DM, DO, DZ, EC, EE, EG, ES, FI, GB, GD, GE, GH, GM, GT, (21) International Application Number: HN, HR, HU, ID, IL, IN, IS, JP, KE, KG, KM, KN, KP, PCT/US201 1/048297 KR, KZ, LA, LC, LK, LR, LS, LT, LU, LY, MA, MD, (22) International Filing Date: ME, MG, MK, MN, MW, MX, MY, MZ, NA, NG, NI, 18 August 201 1 (18.08.201 1) NO, NZ, OM, PE, PG, PH, PL, PT, QA, RO, RS, RU, SC, SD, SE, SG, SK, SL, SM, ST, SV, SY, TH, TJ, TM, (25) Filing Language: English TN, TR, TT, TZ, UA, UG, US, UZ, VC, VN, ZA, ZM, (26) Publication Language: English ZW. (30) Priority Data: (84) Designated States (unless otherwise indicated, for every 61/374,943 18 August 2010 (18.08.2010) US kind of regional protection available): ARIPO (BW, GH, 61/441,485 10 February 201 1 (10.02.201 1) US GM, KE, LR, LS, MW, MZ, NA, SD, SL, SZ, TZ, UG, 61/449,372 4 March 201 1 (04.03.201 1) US ZM, ZW), Eurasian (AM, AZ, BY, KG, KZ, MD, RU, TJ, TM), European (AL, AT, BE, BG, CH, CY, CZ, DE, DK, (72) Inventor; and EE, ES, FI, FR, GB, GR, HR, HU, IE, IS, ΓΓ, LT, LU, (71) Applicant : DEISHER, Theresa [US/US]; 1420 Fifth LV, MC, MK, MT, NL, NO, PL, PT, RO, RS, SE, SI, SK, Avenue, Seattle, WA 98101 (US). -

Supplementary Materials: Evaluation of Cytotoxicity and Α-Glucosidase Inhibitory Activity of Amide and Polyamino-Derivatives of Lupane Triterpenoids
Supplementary Materials: Evaluation of cytotoxicity and α-glucosidase inhibitory activity of amide and polyamino-derivatives of lupane triterpenoids Oxana B. Kazakova1*, Gul'nara V. Giniyatullina1, Akhat G. Mustafin1, Denis A. Babkov2, Elena V. Sokolova2, Alexander A. Spasov2* 1Ufa Institute of Chemistry of the Ufa Federal Research Centre of the Russian Academy of Sciences, 71, pr. Oktyabrya, 450054 Ufa, Russian Federation 2Scientific Center for Innovative Drugs, Volgograd State Medical University, Novorossiyskaya st. 39, Volgograd 400087, Russian Federation Correspondence Prof. Dr. Oxana B. Kazakova Ufa Institute of Chemistry of the Ufa Federal Research Centre of the Russian Academy of Sciences 71 Prospeсt Oktyabrya Ufa, 450054 Russian Federation E-mail: [email protected] Prof. Dr. Alexander A. Spasov Scientific Center for Innovative Drugs of the Volgograd State Medical University 39 Novorossiyskaya st. Volgograd, 400087 Russian Federation E-mail: [email protected] Figure S1. 1H and 13C of compound 2. H NH N H O H O H 2 2 Figure S2. 1H and 13C of compound 4. NH2 O H O H CH3 O O H H3C O H 4 3 Figure S3. Anticancer screening data of compound 2 at single dose assay 4 Figure S4. Anticancer screening data of compound 7 at single dose assay 5 Figure S5. Anticancer screening data of compound 8 at single dose assay 6 Figure S6. Anticancer screening data of compound 9 at single dose assay 7 Figure S7. Anticancer screening data of compound 12 at single dose assay 8 Figure S8. Anticancer screening data of compound 13 at single dose assay 9 Figure S9. Anticancer screening data of compound 14 at single dose assay 10 Figure S10. -

Active Rac1 Detection Kit 2012 09/20
Active Rac1 Detection Kit 1 Kit Orders n 877-616-CELL (2355) (30 immunoprecipitations) [email protected] Support n 877-678-TECH (8324) [email protected] Web n www.cellsignal.com rev. 09/24/20 #8815 For Research Use Only. Not For Use In Diagnostic Procedures. Species Cross-Reactivity: H, M Components Ship As: 11894S Item # Kit Quantity Storage Temp Description: The Active Rac1 Detection Kit provides all GTPgS 11521 1 X 50 µl –80°C reagents necessary for measuring activation of Rac1 GTPase in the cell. GST-PAK1-PBD fusion protein is used to bind GDP 11522 1 X 50 µl –80°C the activated form of GTP-bound Rac1, which can then be Components Ship As: 11894S Item # Kit Quantity Storage Temp immunoprecipitated with glutathione resin. Rac1 activation levels are then determined by western blot using a Rac1 GST-Human PAK1-PBD 8659 1 X 600 µg –20°C Mouse mAb. Rac1 Mouse mAb 8631 1 X 50 µl –20°C Specificity/Sensitivity: Active Rac1 Detection Kit detects Components Ship As: 11860S Item # Kit Quantity Storage Temp endogenous levels of GTP-bound (active) Rac1 as shown in Lysis/Binding/Wash Buffer 11524 1 X 100 mL 4°C Figure 1. This kit detects proteins from the indicated species, as determined through in-house testing, but may also detect Glutathione Resin 11523 1 X 3 ml 4°C homologous proteins from other species. SDS Sample Buffer 11525 1 X 1.5 ml 4°C Background: The Ras superfamily of small GTP-binding Spin Cup and Collection Tubes 11526 1 X 30 vial RT proteins (G proteins) comprise a large class of proteins (over 150 members) that can be classified into at least five families based on their sequence and functional similarities: 1 2 3 4 Figure 1. -

Identification of Pathogenic Genes of Pterygium Based on the Gene Expression Omnibus Database
Int J Ophthalmol, Vol. 12, No. 4, Apr.18, 2019 www.ijo.cn Tel: 8629-82245172 8629-82210956 Email: [email protected] ·Basic Research· Identification of pathogenic genes of pterygium based on the Gene Expression Omnibus database Xiao-Li Yue, Zi-Qing Gao Department of Ophthalmology, the First Affiliated Hospital of INTRODUCTION Bengbu Medical College, Bengbu 233000, Anhui Province, terygium is a general ocular surface and degenerative China P disease characterized by conjunctival fibrovascular Correspondence to: Xiao-Li Yue. Department of Ophthalmology, proliferation and invasion of the peripheral cornea. Pterygium the First Affiliated Hospital of Bengbu Medical College, is composed of the head that invades the cornea, the neck Bengbu Xinxin Jiayuan No.3 Building 2 unit 603, Bengbu that includes the superficial limbus and the body that overlie 233000, Anhui Province, China. [email protected] the sclera[1]. Diverse biological pathways including increase Received: 2018-02-06 Accepted: 2019-01-14 of mitotic proteins and protein implicated in tissue invasion were remarkably affected in pterygium. Additionally, Abstract fibrosis, inflammation, angiogenesis, collagen deposition ● AIM: To identify the pathogenic genes in pterygium. and extracellular matrix breakdown are associated with ● METHODS: We obtained mRNA expression profiles pterygium[2]. Pterygium is noted to be more prevalent than from the Gene Expression Omnibus database (GEO) to 20% of some populations and typically affects the younger identify differentially expressed genes -

Use of Mepolizumab in Adult Patients with Cystic Fibrosis and An
Zhang et al. Allergy Asthma Clin Immunol (2020) 16:3 Allergy, Asthma & Clinical Immunology https://doi.org/10.1186/s13223-019-0397-3 CASE REPORT Open Access Use of mepolizumab in adult patients with cystic fbrosis and an eosinophilic phenotype: case series Lijia Zhang1, Larry Borish2,3, Anna Smith2, Lindsay Somerville2 and Dana Albon2* Abstract Background: Cystic fbrosis (CF) is characterized by infammation, progressive lung disease, and respiratory failure. Although the relationship is not well understood, patients with CF are thought to have a higher prevalence of asthma than the general population. CF Foundation (CFF) annual registry data in 2017 reported a prevalence of asthma in CF of 32%. It is difcult to diferentiate asthma from CF given similarities in symptoms and reversible obstructive lung function in both diseases. However, a specifc asthma phenotype (type 2 infammatory signature), is often identifed in CF patients and this would suggest potential responsiveness to biologics targeting this asthma phenotype. A type 2 infammatory condition is defned by the presence of an interleukin (IL)-4high, IL-5high, IL-13high state and is suggested by the presence of an elevated total IgE, specifc IgE sensitization, or an elevated absolute eosinophil count (AEC). In this manuscript we report the efects of using mepolizumab in patients with CF and type 2 infammation. Results: We present three patients with CF (63, 34 and 24 year of age) and personal history of asthma, who displayed signifcant eosinophilic infammation and high total serum IgE concentrations (type 2 infammation) who were treated with mepolizumab. All three patients were colonized with multiple organisms including Pseudomonas aeruginosa and Aspergillus fumigatus and tested positive for specifc IgE to multiple allergens. -

Transcriptomic Analysis Reveals Abnormal Expression of Prion Disease Gene Pathway in Brains from Patients with Autism Spectrum Disorders
brain sciences Article Transcriptomic Analysis Reveals Abnormal Expression of Prion Disease Gene Pathway in Brains from Patients with Autism Spectrum Disorders Salvo Danilo Lombardo 1 , Giuseppe Battaglia 2,3, Maria Cristina Petralia 4, Katia Mangano 1 , Maria Sofia Basile 1, Valeria Bruno 2,3, Paolo Fagone 1,* , Rita Bella 5, Ferdinando Nicoletti 1 and Eugenio Cavalli 1 1 Department of Biomedical and Biotechnological Sciences, University of Catania, 95123 Catania, Italy; [email protected] (S.D.L.); [email protected] (K.M.); sofi[email protected] (M.S.B.); [email protected] (F.N.); [email protected] (E.C.) 2 Department of Physiology and Pharmacology, University Sapienza, Piazzale A. Moro, 5, 00185 Roma, Italy; [email protected] (G.B.); [email protected] (V.B.) 3 IRCCS Neuromed, Località Camerelle, 86077 Pozzilli, Italy 4 Department of Educational Sciences, University of Catania, 95124 Catania, Italy; [email protected] 5 Department of Medical Sciences, Surgery and Advanced Technologies, University of Catania, 95123 Catania, Italy; [email protected] * Correspondence: [email protected] Received: 26 February 2020; Accepted: 26 March 2020; Published: 29 March 2020 Abstract: The role of infections in the pathogenesis of autism spectrum disorder (ASD) is still controversial. In this study, we aimed to evaluate markers of infections and immune activation in ASD by performing a meta-analysis of publicly available whole-genome transcriptomic datasets of brain samples from autistic patients and otherwise normal people. Among the differentially expressed genes, no significant enrichment was observed for infectious diseases previously associated with ASD, including herpes simplex virus-1 (HSV-1), cytomegalovirus and Epstein–Barr virus in brain samples, nor was it found in peripheral blood from ASD patients. -

Comparative Functional Analysis of the Rac Gtpasesprovided by Elsevier - Publisher Connector
FEBS Letters 555 (2003) 556^560 FEBS 27913 View metadata, citation and similar papers at core.ac.uk brought to you by CORE Comparative functional analysis of the Rac GTPasesprovided by Elsevier - Publisher Connector Lars Christian Haeusler, Lars Blumenstein, Patricia Stege, Radovan Dvorsky, Mohammad Reza Ahmadianà Max-Planck-Institute of Molecular Physiology, Department of Structural Biology, Otto-Hahn-Strasse 11, 44227 Dortmund, Germany Received 18 August 2003; revised 17 September 2003; accepted 5 November 2003 First published online 25 November 2003 Edited by Irmgard Sinning 3), that are encoded by di¡erent genes, share between 89 and Abstract Small GTPases of the Rho family including Rac, Rho and Cdc42 regulate di¡erent cellular processes like reorga- 93% identity in their respective amino acid sequence [3,4]. nization of the actin cytoskeleton by acting as molecular Rac1, the best-investigated isoform, regulates gene expression, switches. The three distinct mammalian Rac proteins share cell cycle progression and rearrangement of the actin cytoskel- very high sequence identity but how their speci¢city is achieved eton [5]. Rac2 is proposed to be responsible for the regulation is hitherto unknown. Here we show that Rac1 and Rac3 are of the oxidative burst in hematopoietic cells but it has been very closely related concerning their biochemical properties, shown that Rac1 contributes to this process, too [6]. Rac1 and such as e¡ector interaction, nucleotide binding and hydrolysis. Rac3 are ubiquitously expressed and therefore regulate a wide In contrast, Rac2 displays a slower nucleotide association and is variety of cellular processes, whereas Rac2 is predominantly more e⁄ciently activated by the Rac-GEF Tiam1. -

A Computational Approach for Defining a Signature of Β-Cell Golgi Stress in Diabetes Mellitus
Page 1 of 781 Diabetes A Computational Approach for Defining a Signature of β-Cell Golgi Stress in Diabetes Mellitus Robert N. Bone1,6,7, Olufunmilola Oyebamiji2, Sayali Talware2, Sharmila Selvaraj2, Preethi Krishnan3,6, Farooq Syed1,6,7, Huanmei Wu2, Carmella Evans-Molina 1,3,4,5,6,7,8* Departments of 1Pediatrics, 3Medicine, 4Anatomy, Cell Biology & Physiology, 5Biochemistry & Molecular Biology, the 6Center for Diabetes & Metabolic Diseases, and the 7Herman B. Wells Center for Pediatric Research, Indiana University School of Medicine, Indianapolis, IN 46202; 2Department of BioHealth Informatics, Indiana University-Purdue University Indianapolis, Indianapolis, IN, 46202; 8Roudebush VA Medical Center, Indianapolis, IN 46202. *Corresponding Author(s): Carmella Evans-Molina, MD, PhD ([email protected]) Indiana University School of Medicine, 635 Barnhill Drive, MS 2031A, Indianapolis, IN 46202, Telephone: (317) 274-4145, Fax (317) 274-4107 Running Title: Golgi Stress Response in Diabetes Word Count: 4358 Number of Figures: 6 Keywords: Golgi apparatus stress, Islets, β cell, Type 1 diabetes, Type 2 diabetes 1 Diabetes Publish Ahead of Print, published online August 20, 2020 Diabetes Page 2 of 781 ABSTRACT The Golgi apparatus (GA) is an important site of insulin processing and granule maturation, but whether GA organelle dysfunction and GA stress are present in the diabetic β-cell has not been tested. We utilized an informatics-based approach to develop a transcriptional signature of β-cell GA stress using existing RNA sequencing and microarray datasets generated using human islets from donors with diabetes and islets where type 1(T1D) and type 2 diabetes (T2D) had been modeled ex vivo. To narrow our results to GA-specific genes, we applied a filter set of 1,030 genes accepted as GA associated. -

Type 2 Immunity in Tissue Repair and Fibrosis
REVIEWS Type 2 immunity in tissue repair and fibrosis Richard L. Gieseck III1, Mark S. Wilson2 and Thomas A. Wynn1 Abstract | Type 2 immunity is characterized by the production of IL‑4, IL‑5, IL‑9 and IL‑13, and this immune response is commonly observed in tissues during allergic inflammation or infection with helminth parasites. However, many of the key cell types associated with type 2 immune responses — including T helper 2 cells, eosinophils, mast cells, basophils, type 2 innate lymphoid cells and IL‑4- and IL‑13‑activated macrophages — also regulate tissue repair following injury. Indeed, these cell populations engage in crucial protective activity by reducing tissue inflammation and activating important tissue-regenerative mechanisms. Nevertheless, when type 2 cytokine-mediated repair processes become chronic, over-exuberant or dysregulated, they can also contribute to the development of pathological fibrosis in many different organ systems. In this Review, we discuss the mechanisms by which type 2 immunity contributes to tissue regeneration and fibrosis following injury. Type 2 immunity is characterized by increased pro‑ disorders remain unclear, although persistent activation duction of the cytokines IL‑4, IL‑5, IL‑9 and IL‑13 of tissue repair pathways is a major contributing mech‑ (REF. 1) . The T helper 1 (TH1) and TH2 paradigm was anism in most cases. In this Review, we provide a brief first described approximately three decades ago2, and overview of fibrotic diseases that have been linked to for many of the intervening years, type 2 immunity activation of type 2 immunity, discuss the various mech‑ was largely considered as a simple counter-regulatory anisms that contribute to the initiation and maintenance mechanism controlling type 1 immunity3 (BOX 1). -
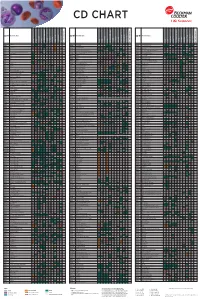
Flow Reagents Single Color Antibodies CD Chart
CD CHART CD N° Alternative Name CD N° Alternative Name CD N° Alternative Name Beckman Coulter Clone Beckman Coulter Clone Beckman Coulter Clone T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells CD1a T6, R4, HTA1 Act p n n p n n S l CD99 MIC2 gene product, E2 p p p CD223 LAG-3 (Lymphocyte activation gene 3) Act n Act p n CD1b R1 Act p n n p n n S CD99R restricted CD99 p p CD224 GGT (γ-glutamyl transferase) p p p p p p CD1c R7, M241 Act S n n p n n S l CD100 SEMA4D (semaphorin 4D) p Low p p p n n CD225 Leu13, interferon induced transmembrane protein 1 (IFITM1). p p p p p CD1d R3 Act S n n Low n n S Intest CD101 V7, P126 Act n p n p n n p CD226 DNAM-1, PTA-1 Act n Act Act Act n p n CD1e R2 n n n n S CD102 ICAM-2 (intercellular adhesion molecule-2) p p n p Folli p CD227 MUC1, mucin 1, episialin, PUM, PEM, EMA, DF3, H23 Act p CD2 T11; Tp50; sheep red blood cell (SRBC) receptor; LFA-2 p S n p n n l CD103 HML-1 (human mucosal lymphocytes antigen 1), integrin aE chain S n n n n n n n l CD228 Melanotransferrin (MT), p97 p p CD3 T3, CD3 complex p n n n n n n n n n l CD104 integrin b4 chain; TSP-1180 n n n n n n n p p CD229 Ly9, T-lymphocyte surface antigen p p n p n -

ADGRE1 (EMR1, F4/80) Is a Rapidly-Evolving Gene Expressed In
Edinburgh Research Explorer ADGRE1 (EMR1, F4/80) Is a Rapidly-Evolving Gene Expressed in Mammalian Monocyte-Macrophages Citation for published version: Waddell, L, Lefevre, L, Bush, S, Raper, A, Young, R, Lisowski, Z, McCulloch, M, Muriuki, C, Sauter, K, Clark, E, Irvine, KN, Pridans, C, Hope, J & Hume, D 2018, 'ADGRE1 (EMR1, F4/80) Is a Rapidly-Evolving Gene Expressed in Mammalian Monocyte-Macrophages' Frontiers in Immunology, vol. 9, 2246. DOI: 10.3389/fimmu.2018.02246 Digital Object Identifier (DOI): 10.3389/fimmu.2018.02246 Link: Link to publication record in Edinburgh Research Explorer Document Version: Publisher's PDF, also known as Version of record Published In: Frontiers in Immunology General rights Copyright for the publications made accessible via the Edinburgh Research Explorer is retained by the author(s) and / or other copyright owners and it is a condition of accessing these publications that users recognise and abide by the legal requirements associated with these rights. Take down policy The University of Edinburgh has made every reasonable effort to ensure that Edinburgh Research Explorer content complies with UK legislation. If you believe that the public display of this file breaches copyright please contact [email protected] providing details, and we will remove access to the work immediately and investigate your claim. Download date: 05. Apr. 2019 ORIGINAL RESEARCH published: 01 October 2018 doi: 10.3389/fimmu.2018.02246 ADGRE1 (EMR1, F4/80) Is a Rapidly-Evolving Gene Expressed in Mammalian Monocyte-Macrophages Lindsey A. Waddell 1†, Lucas Lefevre 1†, Stephen J. Bush 2†, Anna Raper 1, Rachel Young 1, Zofia M. -

Atopic Dermatitis: an Expanding Therapeutic Pipeline for a Complex Disease
REVIEWS Atopic dermatitis: an expanding therapeutic pipeline for a complex disease Thomas Bieber 1,2,3 Abstract | Atopic dermatitis (AD) is a common chronic inflammatory skin disease with a complex pathophysiology that underlies a wide spectrum of clinical phenotypes. AD remains challenging to treat owing to the limited response to available therapies. However, recent advances in understanding of disease mechanisms have led to the discovery of novel potential therapeutic targets and drug candidates. In addition to regulatory approval for the IL-4Ra inhibitor dupilumab, the anti- IL-13 inhibitor tralokinumab and the JAK1/2 inhibitor baricitinib in Europe, there are now more than 70 new compounds in development. This Review assesses the various strategies and novel agents currently being investigated for AD and highlights the potential for a precision medicine approach to enable prevention and more effective long-term control of this complex disease. Atopic disorders Atopic dermatitis (AD) is the most common chronic inhibitors tacrolimus and pimecrolimus and more 1,2 A group of disorders having in inflammatory skin disease . About 80% of disease cases recently the phosphodiesterase 4 (PDE4) inhibitor cris- common a genetic tendency to typically start in infancy or childhood, with the remain- aborole. For the more severe forms of AD, besides the develop IgE- mediated allergic der developing during adulthood. Whereas the point use of ultraviolet light, current therapeutic guidelines reactions. These are atopic dermatitis, food allergy, allergic prevalence in children varies from 2.7% to 20.1% across suggest ciclosporin A, methotrexate, azathioprine and 3,4 rhino- conjunctivitis and countries, it ranges from 2.1% to 4.9% in adults .