Association Between Serum Uric Acid Levels, Nutritional and Antioxidant Status in Patients on Hemodialysis
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

162 Part 175—Indirect Food Addi
§ 174.6 21 CFR Ch. I (4–1–19 Edition) (c) The existence in this subchapter B Subpart B—Substances for Use Only as of a regulation prescribing safe condi- Components of Adhesives tions for the use of a substance as an Sec. article or component of articles that 175.105 Adhesives. contact food shall not be construed as 175.125 Pressure-sensitive adhesives. implying that such substance may be safely used as a direct additive in food. Subpart C—Substances for Use as (d) Substances that under conditions Components of Coatings of good manufacturing practice may be 175.210 Acrylate ester copolymer coating. safely used as components of articles 175.230 Hot-melt strippable food coatings. that contact food include the fol- 175.250 Paraffin (synthetic). lowing, subject to any prescribed limi- 175.260 Partial phosphoric acid esters of pol- yester resins. tations: 175.270 Poly(vinyl fluoride) resins. (1) Substances generally recognized 175.300 Resinous and polymeric coatings. as safe in or on food. 175.320 Resinous and polymeric coatings for (2) Substances generally recognized polyolefin films. as safe for their intended use in food 175.350 Vinyl acetate/crotonic acid copoly- mer. packaging. 175.360 Vinylidene chloride copolymer coat- (3) Substances used in accordance ings for nylon film. with a prior sanction or approval. 175.365 Vinylidene chloride copolymer coat- (4) Substances permitted for use by ings for polycarbonate film. 175.380 Xylene-formaldehyde resins con- regulations in this part and parts 175, densed with 4,4′-isopropylidenediphenol- 176, 177, 178 and § 179.45 of this chapter. -

Ethylenediamine Final AEGL Document
Committee on Acute Exposure Guideline Levels Committee on Toxicology Board on Environmental Studies and Toxicology Division on Earth and Life Studies THE NATIONAL ACADEMIES PRESS 500 Fifth Street, NW Washington, DC 20001 NOTICE: The project that is the subject of this report was approved by the Governing Board of the National Research Council, whose members are drawn from the councils of the National Academy of Sciences, the National Academy of Engineering, and the Insti- tute of Medicine. The members of the committee responsible for the report were chosen for their special competences and with regard for ap¬propriate balance. This project was supported by Contract No. DAMD17-99-C-9049 between the National Academy of Sciences and the U.S. Department of Defense and Contract No. 68-C-03-081 between the National Academy of Sciences and the U.S. Environmental Protection Agency. Any opinions, findings, conclusions, or recommendations expressed in this publication are those of the author(s) and do not necessarily reflect the view of the or- ganizations or agencies that provided support for this project. International Standard Book Number-13: 978-0-309-10358-9 International Standard Book Number-10: 0-309-10358-4 Additional copies of this report are available from The National Academies Press 500 Fifth Street, NW Box 285 Washington, DC 20055 800-624-6242 202-334-3313 (in the Washington metropolitan area) http://www.nap.edu Copyright 2007 by the National Academy of Sciences. All rights reserved. Printed in the United States of America The National Academy of Sciences is a private, nonprofit, self-perpetuating society of distinguished scholars engaged in scientific and engineering research, dedicated to the furtherance of science and technology and to their use for the general welfare. -

2020 Emergency Response Guidebook
2020 A guidebook intended for use by first responders A guidebook intended for use by first responders during the initial phase of a transportation incident during the initial phase of a transportation incident involving hazardous materials/dangerous goods involving hazardous materials/dangerous goods EMERGENCY RESPONSE GUIDEBOOK THIS DOCUMENT SHOULD NOT BE USED TO DETERMINE COMPLIANCE WITH THE HAZARDOUS MATERIALS/ DANGEROUS GOODS REGULATIONS OR 2020 TO CREATE WORKER SAFETY DOCUMENTS EMERGENCY RESPONSE FOR SPECIFIC CHEMICALS GUIDEBOOK NOT FOR SALE This document is intended for distribution free of charge to Public Safety Organizations by the US Department of Transportation and Transport Canada. This copy may not be resold by commercial distributors. https://www.phmsa.dot.gov/hazmat https://www.tc.gc.ca/TDG http://www.sct.gob.mx SHIPPING PAPERS (DOCUMENTS) 24-HOUR EMERGENCY RESPONSE TELEPHONE NUMBERS For the purpose of this guidebook, shipping documents and shipping papers are synonymous. CANADA Shipping papers provide vital information regarding the hazardous materials/dangerous goods to 1. CANUTEC initiate protective actions. A consolidated version of the information found on shipping papers may 1-888-CANUTEC (226-8832) or 613-996-6666 * be found as follows: *666 (STAR 666) cellular (in Canada only) • Road – kept in the cab of a motor vehicle • Rail – kept in possession of a crew member UNITED STATES • Aviation – kept in possession of the pilot or aircraft employees • Marine – kept in a holder on the bridge of a vessel 1. CHEMTREC 1-800-424-9300 Information provided: (in the U.S., Canada and the U.S. Virgin Islands) • 4-digit identification number, UN or NA (go to yellow pages) For calls originating elsewhere: 703-527-3887 * • Proper shipping name (go to blue pages) • Hazard class or division number of material 2. -

Jeffrey E. Lucius U.S. Geological Survey This Report Is Preliminary
U. S. DEPARTMENT OF THE INTERIOR GEOLOGICAL SURVEY PHYSICAL AND CHEMICAL PROPERTIES AND HEALTH EFFECTS OF THIRTY-THREE TOXIC ORGANIC CHEMICALS Jeffrey E. Lucius U.S. Geological Survey Open-File Report 87-428 August 1987 This report is preliminary and has not been reviewed for conformity with U.S. Geological Survey editorial standards. Any use of trade names is for descriptive purposes only and does not imply endorsement by the U.S. Geological Survey. CONTENTS Page Introduction 4 The Properties 6 Abbreviations 13 Conversion Factors 16 Summary Tables 17 Acetic acid 27 Acetone 31 Benzene 34 Bis(2-ethylhexyl)phthalate 37 Bromoform 39 Carbon tetrachloride 42 Chlorobenzene 46 Chloroethane 49 Chloroform 52 Cyclohexane 55 Di-n-butyl phthalate 58 1.1-Dichloroethane 60 1.2-Dichloroethane 63 1,1-Dichloroethene 66 trans-1,2-Dichloroethene 69 Dimethyl sulfoxide 71 1,4-Dioxane 74 Ethanol 77 Ethylbenzene 81 Ethylene dibromide 84 Methanol 87 Methylene chloride 91 Naphthalene 94 Phenol 97 Quinoline 101 Tetrachloroethene 103 Toluene 106 1,1,1-Trichloroethane 109 Trichloroethene 112 Vinyl chloride 115 Water 118 m-Xylene 121 o-Xylene 124 p-Xylene 127 References and Bibliography 130 SUMMARY TABLES page 1. Ranking of top 20 organic ground water contaminants based on number of sites at which each contaminant was detected. 17 2. Selected toxic organic chemicals ordered by Chemical Abstract Service Registry Number (CAS RN). Those chemicals on the U.S. EPA top 100 hazardous substances list are also noted. 18 3. Selected toxic organic chemicals ordered by number of carbon and hydrogen atoms. 19 4. Ranking of selected toxic organic chemicals by specific gravity at room temperature. -

United States Patent (19) 11 Patent Number: 4,666,967 Richardson, Deceased Et Al
United States Patent (19) 11 Patent Number: 4,666,967 Richardson, deceased et al. 45 Date of Patent: May 19, 1987 54 FLAME RETARDANTS FOR 10947.17 12/1967 United Kingdom. POLYURETHANES Primary Examiner-Veronica P. Hoke 75 Inventors: Norman Richardson, deceased, late of Attorney, Agent, or Firm-Luther A. R. Hall Middleton, England, by Joyce (57) ABSTRACT Richardson, legal heir; Brian G. The invention provides polyurethanes and Clubley, Wilmslow; Richard J. polyisocyanurate having incorporated therein a flame Dellar, Hale, both of England retardant amount of a salt formed by reaction between 73) Assignee: Ciba-Geigy Corporation, Ardsley, dimethyl methyl phosphonate, monomethyl methyl N.Y. phosphonate or methyl phosphonic acid, and a com (21) Appl. No.: 821,178 pound of the general formula (I). 22 Filed: Jan. 22, 1986 X Rl I (30) Foreign Application Priority Data R-C-N N Jan. 23, 1985 GB United Kingdom ................. 8501704 R2 51] Int. Cl4........................... CO7F 9/40; C07F 9/38; C08K 5/53; C08H 9/18 in which X is O, S or NH, R1 is H, alkyl with 1 to 4 52) U.S. C. ............................... 524/130; 260/501.14; carbon atoms, alkenyl of up to 4 carbon atoms, CN, 260/501.17; 260/501.19; 260/502.52; 521/85; CONH2 or NH2, R2 is H, alkyl with 1 to 4 carbon atoms 521/107; 524/131; 524/132; 528/71; 528/72; or alkenyl of up to 4 carbon atoms or R1 and R2 together 544/82; 544/85; 544/87; 544/106; 54.6/164; with the nitrogen atom to which they are attached form 546/189: 546/243; 546/244; 546/245; 558/131; a heterocyclic ring of up to 6 carbon atoms which may 558/154 optionally contain another hetero atom and R is H, an 58) Field of Search ..................... -
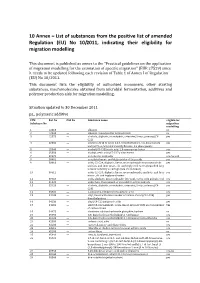
(EU) No 10/2011, Indicating Their Eligibility for Migration Modelling
10 Annex – List of substances from the positive list of amended Regulation (EU) No 10/2011, indicating their eligibility for migration modelling This document is published as annex to the "Practical guidelines on the application of migration modelling for the estimation of specific migration" (EUR 27529) since it needs to be updated following each revision of Table 1 of Annex I of Regulation (EU) No 10/2011. This document lists the eligibility of authorised monomers, other starting substances, macromolecules obtained from microbial fermentation, additives and polymer production aids for migration modelling. Situation updated to 30 December 2011 pa., polymeric additive FCM Ref. No CAS No Substance name eligible for Substance No migration modelling 1 12310 — albumin no 2 12340 — albumin, coagu lated by formaldehyde no 3 12375 — alcohols, aliphatic, monohydric, saturated, linear, primary (C4 - yes C22) 4 22332 — mixture of (40 % w/w) 2,2,4 -trimethylhexane -1,6 -diisocyanate yes and (60 % w/w) 2,4,4-trimethylhexane-1,6-diisocyanate 5 25360 — trialk yl(C5 -C15)acetic acid, 2,3 -epoxypropyl ester yes 6 25380 — trialkyl acetic acid (C7 -C17), vinyl esters yes 7 30370 — acetylacetic acid, salts yes/as acid 8 30401 — acetylated mono - and diglycerides of fatty acids yes 9 30610 — acids, C2 -C24, aliphatic, linear, monocarboxylic from natural oils yes and fats, and their mono-, di- and triglycerol esters (branched fatty acids at naturally occuring levels are included) 10 30612 — acids, C2 -C24, aliphatic, linear, monocarboxylic, synthetic and their -

Abbreviations and Acronyms
The Journal of Organic Chemistry Standard Abbreviations and Acronyms observed optical rotation in degrees cm–1 wavenumber(s) [] specific rotation [expressed without cod 1,5-cyclooctadiene units; the units, (degmL)/(gdm), compd compound are understood] concd concentrated Å angstrom(s) concn concentration Ac acetyl COSY correlation spectroscopy acac acetylacetonate cot 1,3,5,7-cyclooctatetraene ADP adenosine 5-diphosphate Cp cyclopentadienyl AIBN 2,2-azobisisobutyronitrile m-CPBA meta-chloroperoxybenzoic acid AM1 Austin model 1 CV cyclic voltammetry AMP adenosine 5-monophosphate chemical shift in parts per million Anal. combustion elemental analysis downfield from tetramethylsilane anhyd anhydrous d day(s); doublet (spectral); deci AO atomic orbital d density aq aqueous DABCO 1,4-diazabicyclo[2.2.2]octane Ar aryl dansyl 5-(dimethylamino)- atm atmosphere(s) 1-naphthalenesulfonyl DBN 1,5-diazabicyclo[4.3.0]non-5-ene ATP adenosine 5-triphosphate DBU 1,8-diazabicyclo[5.4.0]undec-7-ene ATPase adenosinetriphosphatase av average DCC N,N-dicyclohexylcarbodiimide 9-BBN 9-borabicyclo[3.3.1]nonyl DCE 1,2-dichloroethane 9-BBN–H 9-borabicyclo[3.3.1]nonane DDQ 2,3-dichloro-5,6-dicyano- Bn, Bzl benzyl 1,4-benzoquinone DEAD diethyl azodicarboxylate bpy 2,2-bipyridyl BOC, Boc tert-butoxycarbonyl DEPT distortionless enhancement by bp boiling point, base pair polarization transfer br broad (spectral) DFT density functional theory Bu, n-Bu normal (primary) butyl DIBALH diisobutylaluminum hydride s-Bu sec-butyl DMA dimethylacetamide DMAP 4-(N,N-dimethylamino)pyridine -

United States Patent (19) 11) Patent Number: 4,565,833 Buszard Et Al
United States Patent (19) 11) Patent Number: 4,565,833 Buszard et al. (45) Date of Patent: Jan. 21, 1986 54 FIRE RETARDANT COMPOSITION 4,165,411 8/1979 Marans et al. ...................... 521/107 4,407,981. 10/1983 Aaronson ..... ... 524/130 75) Inventors: David L. Buszard, Woodford; 4,409,341 10/1983 Hira et al. ........................... 521/107 Richard J. Dellar, Altrincham, both of England FOREIGN PATENT DOCUMENTS 1569428 2/1970 Fed. Rep. of Germany . 73) Assignee: Ciba-Geigy AG, Basel, Switzerland 2452357 5/1975 Fed. Rep. of Germany. (21) Appl. No.: 541,352 2610180 9/1977 Fed. Rep. of Germany . 1146173 3/1969 United Kingdom . 22 Filed: Oct. 12, 1983 Primary Examiner-John Kight (30) Foreign Application Priority Data Assistant Examiner-Kriellion Morgan Oct. 12, 1982 GB United Kingdom ................. 8229075 Attorney, Agent, or Firm-Wenderoth, Lind & Ponack 51) Int. Cl........................... C08K 5/52; C08K 5/53; (57) ABSTRACT C08G 18/08 A fire retardant composition for rigid polyurethanes or 52 U.S. Cl. .................................... 521/107; 524/130; polyisocyanurates comprises dimethyl methyl phospho 524/141; 524/143; 528/65; 528/72; 252/609 nate, diethyl ethyl phosphonate or a mixture thereof 58) Field of Search ................ 521/107; 524/130, 141, and a triaryl phosphate, a trialkyl phosphate or an alkyl 524/143; 528/51, 65,72; 252/609 /aryl phosphate in a ratio by weight of 5:95 to 95:5. The composition may also contain a halogen-containing 56 References Cited flame retardant compound. U.S. PATENT DOCUMENTS 3,400,085 9/1968 Kujawa et al. ..................... 521/107 15 Claims, No Drawings 4,565,833 1. -

A C C Es S O R
ACCESSORIES Click on the Items Below or the Pictures to be Taken to That Page Page CONTENTS Oils and Lubricants 2 - 6 Lubrication Equipment (Grease & Oil) 7 - 32 Fuel Equipment & Chemical Pumps 33 - 41 Air Equipment 42 - 43 Diaphragm Pumps & LED Light 44 - 45 Hose Reels 46 - 49 Protect Lanolin and Adhesive Products 50 - 61 Adhesive Products Chemical Compatibility 62 - 66 Compartment Storage Case & Cabinet / Frames 67 Automotive Hoses 68 - 71 Air Conditioning Hose and Fittings 72 - 73 Cable Ties, Crimp Rings & Test Tags 74 - 75 Hose Cleaning Equipment 76 Thread Identification and Tool Kits 77 Pressure Cleaner Components 78 - 86 This page is part of a complete catalogue containing technical and safety data. 1 All data must be reviewed when selecting a product. Pirtek reserve the right to change technical specifications without notice. Rev. R P ACCESSORIES LUBRICANTS MINERAL BASED OILS AND GREASES OILS & GREASES OILS Hydraulic Oils: Automotive Fluids: Greases: • Pirtek supply popular commonly used • ATF Type D is a quality Automatic • NLGI No2 Lithium complex grease contains hydraulic fluids Transmission Fluid suitable for older style extreme pressure additive • Available in ISO Grades 46 and 68 automatic transmissions and modern Power • Recommended for extended lubrication Steering systems available in a 5 litre pack • All oils incorporate advanced performance intervals additives to combat rust, corrosion and • For smaller power steering requirements, • Suitable for wheel bearings (disc and drum wear Pirtek offer a 350 ml pack of Power -
![Second Revision No. 1-NFPA 497-2015 [ Chapter 2 ]](https://docslib.b-cdn.net/cover/4413/second-revision-no-1-nfpa-497-2015-chapter-2-4174413.webp)
Second Revision No. 1-NFPA 497-2015 [ Chapter 2 ]
National Fire Protection Association Report http://submittals.nfpa.org/TerraViewWeb/ContentFetcher?commentPara... Second Revision No. 1-NFPA 497-2015 [ Chapter 2 ] Chapter 2 Referenced Publications 2.1 General. The documents or portions thereof listed in this chapter are referenced within this recommended practice and should be considered part of the recommendations of this document. 2.2 NFPA Publications. National Fire Protection Association, 1 Batterymarch Park, Quincy, MA 02169-7471. NFPA 30, Flammable and Combustible Liquids Code, 2015 edition. NFPA 33, Standard for Spray Application Using Flammable or Combustible Materials, 2015 2016 edition. NFPA 34, Standard for Dipping, Coating, and Printing Processes Using Flammable or Combustible Liquids, 2015 edition. NFPA 35, Standard for the Manufacture of Organic Coatings, 2016 edition. NFPA 36, Standard for Solvent Extraction Plants, 2013 edition. NFPA 45, Standard on Fire Protection for Laboratories Using Chemicals, 2015 edition. NFPA 55, Compressed Gases and Cryogenic Fluids Code, 2016 edition. NFPA 58, Liquefied Petroleum Gas Code, 2017 edition. NFPA 59A, Standard for the Production, Storage, and Handling of Liquefied Natural Gas (LNG), 2016 edition. NFPA 70®, National Electrical Code®, 2017 edition. 2.3 Other Publications. 2.3.1 API Publications. American Petroleum Institute, 1220 L Street, NW, Washington, DC 20005-4070. API RP 500, Recommended Practice for Classification of Locations for Electrical Installations at Petroleum Facilities Classified as Class I, Division 1 and Division 2, 3rd edition, 2008. API RP 505, Recommended Practice for Classification of Locations for Electrical Installations at Petroleum Facilities Classified as Class I, Zone 0, Zone 1, and Zone 2, 2002, reaffirmed 2013. 2.3.2 ASHRAE Publications. -

Selective Sorption of Uric Acid by Novel Molecularly Imprinted Polymers
MOLECULAR ImPRiNTiNG Research Article • DOI: 10.2478/molim-2012-0003 • MOLIM • 2013 • 17–26 Selective sorption of uric acid by novel molecularly imprinted polymers Abstract Anastasia P. Leshchinskaya*, Oleg A. Pisarev, The polymers based on ethylene glycol dimethacrylate (EGDMA) and Irina V. Polyakova, Evgeniy F. Panarin dimethylaminoethyl methacrylate (DMAEMA) and molecularly imprinted Anna R. Groshikova, with uric acid (UA), UA-MIPs, were successfully synthesized. The binding activity of UA-MIPs towards UA was studied in depth using batch methods. Department of Biopolymers, The optimized sorbent UA-MIP-7-16 was synthesized; this is an EGDMA- Institute of Macromolecular Compounds, crosslinked system containing 16 mol% of UA as the template. The Russian Academy of Sciences, character of binding between UA and UA-MIP-7-16 was studied using Saint-Petersburg, 199004, xanthine as a reference substance, since its chemical structure is similar Bolshoi pr. 31, Russia to that of UA. The studies of equilibrium sorption of UA and xanthine from model aqueous solutions by the imprinted sorbent demonstrate the predominance of specific UA sorption. The sorption kinetic data were analyzed using the Boyd model and shell and core. Selectivity of UA- MIP-7-16 was further demonstrated by biochemical analysis of serum containing UA and other components conducted before and after sorption. UA-MIP-7-16 showed high recognition selectivity and affinity towards the template molecule (UA). Keywords Molecularly imprinted sorbents • Uric acid • Selective sorption • Serum Received 20 April 2012 © Versita Sp. z o.o. Accepted 10 July 2012 1. Introduction selectivity. Besides, there are other significant requirements, e.g. biocompatibility, capability to biodegrade and hemocompatibility Uric acid (UA) is the primary product of purine degradation in [11,12]. -

Ethyleneamines Applications
DSA97164.qxd:EA-5621.qxd 10/26/09 2:18 PM Page 1 DSA97164.qxd:EA-5621.qxd 10/26/09 2:18 PM Page 2 Contents Introduction................................................3 Ethyleneamines Applications..................20 Product Profiles ..........................................4 Major End-Uses........................................21 Lubricant and Fuel Additives..................22 Ethylenediamine (EDA) ............................4 Polyamide Resins .....................................23 Diethylenetriamine (DETA)......................4 Asphalt Additives and Emulsifiers...........24 Triethylenetetramine (TETA)....................4 Petroleum Production and Refining........24 Tetraethylenepentamine (TEPA)..............4 Resins and Additives for Heavy Polyamine (HPA)............................5 Pulp and Paper .........................................25 Piperazine (PIP) .........................................5 Epoxy Curing Agents................................26 Aminoethylpiperazine (AEP)....................5 Bleach Activators......................................26 Aminoethylethanolamine (AEEA) ...........5 Chelates and Chelating Agents...............27 Metal Ore Processing...............................27 Typical Physical Properties .......................6 Surfactants and Emulsifiers ....................28 Ethyleneamines Anthelmintics (Dewormers) ...................28 Vapor Pressure vs. Temperature............8 Fabric Softeners........................................29 Viscosity vs. Temperature.......................9 Fungicides.................................................30