Molluscum Contagiosum
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Skin Cancer in the Immunocompromised Patient
Dermatologic Risks and Transplantation Allison Hanlon, MD, PhD Vanderbilt University School of Medicine Department of Medicine Division of Dermatology I have no relevant conflicts of interest to disclose. Dermatologic Risks and Transplantation • Acne • Folliculitis • Sebaceous hyperplasia • Overgrowth of hair • Infections – warts, molluscum contagiosum • Skin thinning and increased bruising • Skin cancer Folliculitis and Acne Folliculitis Sebaceous Hyperplasia Overgrowth of Hair Cyclosporine associated Gingival Hyperplasis Molluscum Contagiosum Verruca Easy Bruising and Skin Thinning Overview of Skin Cancer in SOTR • Clinical appearance of most common skin cancers • Risk factors for developing skin cancer • Skin cancer prevention • Multidisciplinary care Basal Cell Carcinoma Basal Cell Carcinoma Nodular Basal Cell Carcinoma Basal Cell Carcinoma Squamous Cell Carcinoma Squamous Cell Carcinoma Field Cancerization Immunocompromised patients at risk for metastasis Melanoma Nail Unit Melanoma Nodular Melanoma Melanoma Benign Seborrheic Keratosis Skin cancer is the most common malignancy in solid organ transplant recipients • Skin cancer accounts for 40% of malignancies in solid organ transplant recipients (SOTR) • 50% of Caucasian SOTR will develop skin cancer • Non-melanoma skin cancer (NMSC) > melanoma Euvrard S, Kanitakis J, Claudy A. Skin cancers after organ transplantation. N Engl J Med 2003;348:1681 Skin Cancer in SOTR • Squamous cell carcinoma (SCC) is the most common cutaneous malignancy in transplant patient • Basal cell carcinoma (BCC) is second most common skin cancer in transplant patient • Melanoma risk 3.6 times greater likelihood in SOTR Hollenbeak CS et al. Cancer 2005; 104:1962 than the general Euvrard S et.al. N Engl J Med 2003;348:1681 population Lanov E et.al. Int J Cancer. 2010;126:1724 Proposed Mechanisms Of Immunosuppression relationship to Skin Cancer Development • Direct carcinogenic effects of immunosuppression medications • Proliferation of oncogenic viruses • Reduced immune surveillance within transplant skin cancers Carucci et.al.PLoS One. -

A. Syphilis Is a Systemic, Sexually Transmitted Disease (STD) Caused by the Treponema Pallidum Bacterium
Oklahoma State Department of Health 03-2018 Revised SYPHILIS I. DEFINITION: A. Syphilis is a systemic, sexually transmitted disease (STD) caused by the Treponema pallidum bacterium. B. It can cause long-term complications if not treated correctly. Symptoms in adults are divided into stages. These stages are described below in the Clinical Features. Syphilis has been called ‘the great imitator’ because it has so many possible symptoms, many of which look like symptoms from other diseases. The painless syphilis chancre that clients get after they are first infected can be confused for an ingrown hair, zipper cut, or other seemingly harmless bump. Many times the client does not know they had a sore. The non-itchy body rash that develops during the second stage of syphilis can show up on the palms of the client’s hands and soles of their feet, all over the body, or in just a few places. The rash is usually bilateral, meaning it appears equally on both sides of the body. C. The three means of syphilis transmission are: 1. Person to person via vaginal, anal, or oral sex through direct contact with a syphilis chancre. 2. Person to person during foreplay, even when there is no penetrative sex (much less common). 3. Pregnant mother with syphilis to fetus - very serious complications may occur (fetal demise, long bone deformities, “saddle nose”). II. CLINICAL FEATURES: If left untreated, the disease progresses through several stages during which the infected person may or may not be symptomatic. The DIS and ‘Syphilis Diagnosis and Treatment Algorithm’ (Appendix 1) can assist with staging. -

Molluscum Contagiosum
Partners in Pediatrics, PC 7110 Forest Ave Suite 105 Richmond, VA 23226 804-377-7100 Molluscum Contagiosum Although molluscum contagiosum is a common skin rash in kids, many parents have never heard of it. The most important thing to know about it is that, for most children, the rash is no big deal and goes away on its own over time. About Molluscum Contagiosum Molluscum contagiosum is a viral infection that causes a mild skin rash. The rash looks like one or more small growths or wart-like bumps (called mollusca) that are usually pink, white, or skin-colored. The bumps are usually soft and smooth and may have an indented center. Infection is most common among kids between 1 and 12 years old, but also occurs in: teens and adults some athletes, such as wrestlers, swimmers, and gymnasts people whose immune systems have been weakened by HIV, cancer treatment, or long-term steroid use As you might guess by its name, this skin disorder is contagious, and can be passed from one person to another. It is unknown how long the rash and virus may be contagious. Causes Molluscum contagiosum is caused by the molluscum contagiosum virus (MCV), a member of the poxvirus family. This virus thrives in warm, humid climates and in areas where people live very close together. Infection with MCV occurs when the virus enters a small break in the skin's surface. Many people who come in contact with the virus have immunity against it, and do not develop any growths. For those not resistant to it, growths usually appear 2 to 8 weeks after infection. -

Cutaneous Manifestations of HIV Infection Carrie L
Chapter Title Cutaneous Manifestations of HIV Infection Carrie L. Kovarik, MD Addy Kekitiinwa, MB, ChB Heidi Schwarzwald, MD, MPH Objectives Table 1. Cutaneous manifestations of HIV 1. Review the most common cutaneous Cause Manifestations manifestations of human immunodeficiency Neoplasia Kaposi sarcoma virus (HIV) infection. Lymphoma 2. Describe the methods of diagnosis and treatment Squamous cell carcinoma for each cutaneous disease. Infectious Herpes zoster Herpes simplex virus infections Superficial fungal infections Key Points Angular cheilitis 1. Cutaneous lesions are often the first Chancroid manifestation of HIV noted by patients and Cryptococcus Histoplasmosis health professionals. Human papillomavirus (verruca vulgaris, 2. Cutaneous lesions occur frequently in both adults verruca plana, condyloma) and children infected with HIV. Impetigo 3. Diagnosis of several mucocutaneous diseases Lymphogranuloma venereum in the setting of HIV will allow appropriate Molluscum contagiosum treatment and prevention of complications. Syphilis Furunculosis 4. Prompt diagnosis and treatment of cutaneous Folliculitis manifestations can prevent complications and Pyomyositis improve quality of life for HIV-infected persons. Other Pruritic papular eruption Seborrheic dermatitis Overview Drug eruption Vasculitis Many people with human immunodeficiency virus Psoriasis (HIV) infection develop cutaneous lesions. The risk of Hyperpigmentation developing cutaneous manifestations increases with Photodermatitis disease progression. As immunosuppression increases, Atopic Dermatitis patients may develop multiple skin diseases at once, Hair changes atypical-appearing skin lesions, or diseases that are refractory to standard treatment. Skin conditions that have been associated with HIV infection are listed in Clinical staging is useful in the initial assessment of a Table 1. patient, at the time the patient enters into long-term HIV care, and for monitoring a patient’s disease progression. -

Cutaneous Manifestations of Newborns in Omdurman Maternity Hospital
ﺑﺴﻢ اﷲ اﻟﺮﺣﻤﻦ اﻟﺮﺣﻴﻢ Cutaneous Manifestations of Newborns in Omdurman Maternity Hospital A thesis submitted in the partial fulfillment of the degree of clinical MD in pediatrics and child health University of Khartoum By DR. AMNA ABDEL KHALIG MOHAMED ATTAR MBBS University of Khartoum Supervisor PROF. SALAH AHMED IBRAHIM MD, FRCP, FRCPCH Department of Pediatrics and Child Health University of Khartoum University of Khartoum The Graduate College Medical and Health Studies Board 2008 Dedication I dedicate my study to the Department of Pediatrics University of Khartoum hoping to be a true addition to neonatal care practice in Sudan. i Acknowledgment I would like to express my gratitude to my supervisor Prof. Salah Ahmed Ibrahim, Professor of Peadiatric and Child Health, who encouraged me throughout the study and provided me with advice and support. I am also grateful to Dr. Osman Suleiman Al-Khalifa, the Dermatologist for his support at the start of the study. Special thanks to the staff at Omdurman Maternity Hospital for their support. I am also grateful to all mothers and newborns without their participation and cooperation this study could not be possible. Love and appreciation to my family for their support, drive and kindness. ii Table of contents Dedication i Acknowledgement ii Table of contents iii English Abstract vii Arabic abstract ix List of abbreviations xi List of tables xiii List of figures xiv Chapter One: Introduction & Literature Review 1.1 The skin of NB 1 1.2 Traumatic lesions 5 1.3 Desquamation 8 1.4 Lanugo hair 9 1.5 -

Eyelid Conjunctival Tumors
EYELID &CONJUNCTIVAL TUMORS PHOTOGRAPHIC ATLAS Dr. Olivier Galatoire Dr. Christine Levy-Gabriel Dr. Mathieu Zmuda EYELID & CONJUNCTIVAL TUMORS 4 EYELID & CONJUNCTIVAL TUMORS Dear readers, All rights of translation, adaptation, or reproduction by any means are reserved in all countries. The reproduction or representation, in whole or in part and by any means, of any of the pages published in the present book without the prior written consent of the publisher, is prohibited and illegal and would constitute an infringement. Only reproductions strictly reserved for the private use of the copier and not intended for collective use, and short analyses and quotations justified by the illustrative or scientific nature of the work in which they are incorporated, are authorized (Law of March 11, 1957 art. 40 and 41 and Criminal Code art. 425). EYELID & CONJUNCTIVAL TUMORS EYELID & CONJUNCTIVAL TUMORS 5 6 EYELID & CONJUNCTIVAL TUMORS Foreword Dr. Serge Morax I am honored to introduce this Photographic Atlas of palpebral and conjunctival tumors,which is the culmination of the close collaboration between Drs. Olivier Galatoire and Mathieu Zmuda of the A. de Rothschild Ophthalmological Foundation and Dr. Christine Levy-Gabriel of the Curie Institute. The subject is now of unquestionable importance and evidently of great interest to Ophthalmologists, whether they are orbital- palpebral specialists or not. Indeed, errors or delays in the diagnosis of tumor pathologies are relatively common and the consequences can be serious in the case of malignant tumors, especially carcinomas. Swift diagnosis and anatomopathological confirmation will lead to a treatment, discussed in multidisciplinary team meetings, ranging from surgery to radiotherapy. -
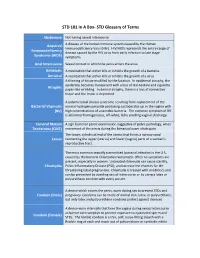
STD Glossary of Terms
STD 101 In A Box- STD Glossary of Terms Abstinence Not having sexual intercourse Acquired A disease of the human immune system caused by the Human Immunodeficiency Virus (HIV). HIV/AIDS represents the entire range of Immunodeficiency disease caused by the HIV virus from early infection to late stage Syndrome (AIDS) symptoms. Anal Intercourse Sexual contact in which the penis enters the anus. Antibiotic A medication that either kills or inhibits the growth of a bacteria. Antiviral A medication that either kills or inhibits the growth of a virus. A thinning of tissue modified by the location. In epidermal atrophy, the epidermis becomes transparent with a loss of skin texture and cigarette Atrophic paper-like wrinkling. In dermal atrophy, there is a loss of connective tissue and the lesion is depressed. A polymicrobial clinical syndrome resulting from replacement of the Bacterial Vaginosis normal hydrogen peroxide producing Lactobacillus sp. in the vagina with (BV) high concentrations of anaerobic bacteria. The common symptom of BV is abnormal homogeneous, off-white, fishy smelling vaginal discharge. Cervical Motion A sign found on pelvic examination suggestive of pelvic pathology; when Tenderness (CMT) movement of the cervix during the bimanual exam elicits pain. The lower, cylindrical end of the uterus that forms a narrow canal Cervix connecting the upper (uterus) and lower (vagina) parts of a woman's reproductive tract. The most common sexually transmitted bacterial infection in the U.S., caused by the bacteria Chlamydia trachomatis. Often no symptoms are present, especially in women. Untreated chlamydia can cause sterility, Chlamydia Pelvic Inflammatory Disease (PID), and increase the chances for life- threatening tubal pregnancies. -

HIV Infection and AIDS
G Maartens 12 HIV infection and AIDS Clinical examination in HIV disease 306 Prevention of opportunistic infections 323 Epidemiology 308 Preventing exposure 323 Global and regional epidemics 308 Chemoprophylaxis 323 Modes of transmission 308 Immunisation 324 Virology and immunology 309 Antiretroviral therapy 324 ART complications 325 Diagnosis and investigations 310 ART in special situations 326 Diagnosing HIV infection 310 Prevention of HIV 327 Viral load and CD4 counts 311 Clinical manifestations of HIV 311 Presenting problems in HIV infection 312 Lymphadenopathy 313 Weight loss 313 Fever 313 Mucocutaneous disease 314 Gastrointestinal disease 316 Hepatobiliary disease 317 Respiratory disease 318 Nervous system and eye disease 319 Rheumatological disease 321 Haematological abnormalities 322 Renal disease 322 Cardiac disease 322 HIV-related cancers 322 306 • HIV INFECTION AND AIDS Clinical examination in HIV disease 2 Oropharynx 34Neck Eyes Mucous membranes Lymph node enlargement Retina Tuberculosis Toxoplasmosis Lymphoma HIV retinopathy Kaposi’s sarcoma Progressive outer retinal Persistent generalised necrosis lymphadenopathy Parotidomegaly Oropharyngeal candidiasis Cytomegalovirus retinitis Cervical lymphadenopathy 3 Oral hairy leucoplakia 5 Central nervous system Herpes simplex Higher mental function Aphthous ulcers 4 HIV dementia Kaposi’s sarcoma Progressive multifocal leucoencephalopathy Teeth Focal signs 5 Toxoplasmosis Primary CNS lymphoma Neck stiffness Cryptococcal meningitis 2 Tuberculous meningitis Pneumococcal meningitis 6 -

Fundamentals of Dermatology Describing Rashes and Lesions
Dermatology for the Non-Dermatologist May 30 – June 3, 2018 - 1 - Fundamentals of Dermatology Describing Rashes and Lesions History remains ESSENTIAL to establish diagnosis – duration, treatments, prior history of skin conditions, drug use, systemic illness, etc., etc. Historical characteristics of lesions and rashes are also key elements of the description. Painful vs. painless? Pruritic? Burning sensation? Key descriptive elements – 1- definition and morphology of the lesion, 2- location and the extent of the disease. DEFINITIONS: Atrophy: Thinning of the epidermis and/or dermis causing a shiny appearance or fine wrinkling and/or depression of the skin (common causes: steroids, sudden weight gain, “stretch marks”) Bulla: Circumscribed superficial collection of fluid below or within the epidermis > 5mm (if <5mm vesicle), may be formed by the coalescence of vesicles (blister) Burrow: A linear, “threadlike” elevation of the skin, typically a few millimeters long. (scabies) Comedo: A plugged sebaceous follicle, such as closed (whitehead) & open comedones (blackhead) in acne Crust: Dried residue of serum, blood or pus (scab) Cyst: A circumscribed, usually slightly compressible, round, walled lesion, below the epidermis, may be filled with fluid or semi-solid material (sebaceous cyst, cystic acne) Dermatitis: nonspecific term for inflammation of the skin (many possible causes); may be a specific condition, e.g. atopic dermatitis Eczema: a generic term for acute or chronic inflammatory conditions of the skin. Typically appears erythematous, -

Survey of Skin Disorders in Newborns: Clinical Observation in an Egyptian Medical Centre Nursery A.A
املجلة الصحية لرشق املتوسط املجلد الثامن عرش العدد اﻷول Survey of skin disorders in newborns: clinical observation in an Egyptian medical centre nursery A.A. El-Moneim 1 and R.E. El-Dawela 2 مسح لﻻضطرابات اجللدية لدى الولدان: مﻻحظة رسيرية يف حضانة يف مركز طبي يف مرص عبري أمحد عبد املنعم، رهيام عز الدولة الرشقاوي اخلﻻصة:مل َ ْت َظ اﻻضطرابات اجللدية لدى الولدان بدراسات جيدة يف مرص. وقد هدفت الباحثتان إىل دراسة أنامط التغريات اجللدية يف عينة من ِ الولدان املرصيني، وهي دراسة وصفية استباقية أترابية شملت ستة مئة وليد يف َّحضانة يف مستشفى جامعة سوهاج، َّوتضمنت الفحص اجللدي خﻻل اﻷيام اخلمسة اﻷوىل بعد الوﻻدة. وقد تم كشف اﻻضطرابات اجللدية لدى 240 ًوليدا )40%( ولوحظت الومحات لدى 100 وليد )%16.7(، ومعظمها من النمط ذي اخلﻻيا امليﻻنية )لطخات منغولية لدى 11.7% مع ومحات وﻻدية ذات ميﻻنية اخلﻻيا لدى 2.7%(. كام ُك ِش َف ْت العداوى الفطرية اجللدية، ومنها داء َّاملبيضات الفموية، وعدوى الفطريات يف مناطق احلفاظات أو َالـم َذح الناجم عن عدوى َّاملبيضات يف اﻷرفاغ )أصل الفخذ(، وذلك لدى 13.3%، ُوكشفت بعض العداوى اجلرثومية يف 1.3%من الولدان. وتشري املقارنات مع الدراسات اﻷخرى يف أرجاء العامل إىل معدل مرتفع للعدوى بالفطريات مع معدل منخفض للومحات الوﻻدية يف دراستنا للولدان، وتويص الباحثتان بإجراء تقييم روتيني جلدي للولدان، ّوﻻسيام يف ضوء املعدﻻت املرتفعة للعدوى اجللدية بالفطريات. ABSTRACT The frequency of neonatal skin disorders has not been well studied in Egypt. Our aim was to address patterns of dermatological changes in a sample of Egyptian newborns. In a descriptive prospective cohort study 600 newborns in Sohag University hospital nursery were dermatologically examined within the first 5 days of birth. -

GET YOURSELF TESTED Testing Is Confidential
GET YOURSELF TESTED Testing is confidential. If you are under 18 years old, you can consent to be checked and treated for STIs. • Warts may grow on or around the genital area virus will still be in your body and you may still pass (penis, scrotum, vagina, vulva), the anus, or mouth. it during sex. They can also grow inside the body where they are hard to see. • Talk with your provider about when it’s safe to have • Usually are painless, but if the warts are injured, sex after getting treatment. they may become sore when touched. • It’s important to talk with your partner(s) about any sexually transmitted infections (STIs) you may have. Why Does It Matter? • Certain types of HPV can lead to cervical cancer in To Learn More females, or cancer of the penis in males. Some types of HPV may also lead to oral or anal cancer. Contact a health care provider or your local STI clinic. • In some cases, warts can become quite large and To learn more about STIs, or to find your local STI cause discomfort. clinic, visit www.health.ny.gov/STD. • A small percentage of pregnant people with You can find other STI testing locations at genital warts can pass the virus to the baby https://gettested.cdc.gov. during birth. Partners Because symptoms of HPV can take a long time to show up, if at all, it’s hard to know when a person first got it. • If you have genital warts, tell your partner(s) so they can be checked by a health care provider, and treated if they have them. -

Koi Herpesvirus Disease (KHVD)1 Kathleen H
VM-149 Koi Herpesvirus Disease (KHVD)1 Kathleen H. Hartman, Roy P.E. Yanong, Deborah B. Pouder, B. Denise Petty, Ruth Francis-Floyd, Allen C. Riggs, and Thomas B. Waltzek2 Introduction Koi herpesvirus (KHV) is a highly contagious virus that causes significant morbidity and mortality in common carp (Cyprinus carpio) varieties (Hedrick et al. 2000, Haenen et al. 2004). Common carp is raised as a foodfish in many countries and has also been selectively bred for the ornamental fish industry where it is known as koi. The first recognized case of KHV occurred in the United Kingdom in 1996 (Haenen et al. 2004). Since then other cases have been confirmed in almost all countries that culture koi and/ or common carp with the exception of Australia (Hedrick et al. 2000; Haenen et al. 2004, Pokorova et al. 2005). This information sheet is intended to inform veterinarians, biologists, fish producers and hobbyists about KHV disease. What Is KHV? Figure 1. Koi with mottled gills and sunken eyes due to koi Koi herpesvirus (also known as Cyprinid herpesvirus 3; herpesvirus disease. Credit: Deborah B. Pouder, University of Florida CyHV3) is classified as a double-stranded DNA virus herpesvirus, based on virus morphology and genetics, and belonging to the family Alloherpesviridae (which includes is closely related to carp pox virus (Cyprinid herpesvirus fish herpesviruses). The work of Waltzek and colleagues 1; CyHV1) and goldfish hematopoietic necrosis virus (Waltzek et al. 2005, 2009) revealed that KHV is indeed a (Cyprinid herpesvirus 2; CyHV2). Koi herpesvirus disease has been diagnosed in koi and common carp (Hedrick 1.