Low FODMAP (Fermentable Oligo-, Di- and Monosaccharides and Polyols) Diet
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Limiting Fructose, Fructans Intake May Ease IBS
36 Digestive Disorders FAMILY P RACTICE N EWS • July 1, 2008 Limiting Fructose, Fructans Intake May Ease IBS BY MARY ANN MOON “marked and sustained global improve- of irritable bowel syndrome (IBS) in patients prove symptoms. In the current study, the Contributing Writer ment in gastrointestinal symptoms,” re- who also have fructose malabsorption. researchers focused on osmotic load with- searchers noted. A subsequent study of The results also demonstrate that re- in the lumen and fermentative gas content. atients with irritable bowel syn- the patients revealed that symptom relief stricting intake of these substances may Poorly absorbed short-chain carbohy- drome and fructose malabsorption was not specific to restricted intake of lead to durable symptomatic improve- drates, including fructose and lactose, are Pappeared to benefit from a diet that fructose, but was achieved by limiting the ment, wrote Ms. Shepherd, a dietician at highly fermentable. They exert a strong restricted intake of fructose and fructans, intake of poorly absorbed short-chain Australia’s Monash University, Clayton, osmotic effect in people who have malab- Susan J. Shepherd and her colleagues re- carbohydrates. Victoria, and her colleagues. sorption of these two sugars—about 40% ported in an article appearing in the July These findings “represent the first high- They theorized that, because many ab- of the population in the case of fructose, 2008 issue of Clinical Gastroenterology level evidence” that poorly absorbed short- dominal symptoms may originate from and between 15% to 100% of the popula- and Hepatology. chain carbohydrates—fructose and fruc- bowel distension, addressing factors that tion for lactose. In the 25-patient study, the diet led to tans—are dietary triggers for the symptoms contribute to the distension would im- To minimize or eliminate intake of poor- ly absorbed short-chain carbohydrates, the investigators created a diet that omitted Brief Summary—see package insert for full prescribing information. -

A Fiber to Enrich Product Appeal
INCREASE FIBER. RETAIN APPEAL. REDUCE COST-IN-USE. A fiber to enrich product appeal Support digestive wellness — without impacting taste, texture or color using NOVELOSE® 3490 dietary fiber The call for fiber and digestive health is getting louder. Forty-four percent of U.S. consumers are increasing fiber consumption.1 And 70% of consumers feel digestive health is “important.”2 As you formulate to support digestive wellness with more fiber, you must overcome the unappealing effects fiber can often have on taste, texture and appearance — and for some consumers, digestive comfort — to keep consumers coming back for more. Now, NOVELOSE 3490 dietary fiber from Ingredion can help you deliver just-right taste, texture, and even fewer calories in fiber–rich baked goods, tortillas, cereal and bars. And, it’s Low FODMAP Certified to help you bring fiber to consumers who follow a low FODMAP diet. Take the lead in fiber fortification to support digestive wellness Adding fiber to many commonly consumed foods can be a challenge. You must balance the positive health benefits and label claims with the potentially negative impact of fiber on taste, texture and appearance. Not anymore. New NOVELOSE® 3490 resistant starch (type RS4) is an insoluble fiber that has little to no impact on taste, color or texture. By replacing a portion of the flour in bread, baked snacks, cookies, tortillas, cereal and bars, the tapioca-based fiber reduces calories and enables processing ease. It also reduces cost-in-use compared to many other fibers. Meet the growing low FODMAP trend Give consumers the fiber — and taste they want without digestive discomfort Many foods found in American diets are high in in certain short- chain carbohydrates called FODMAPs, which can trigger occasional digestive discomfort. -
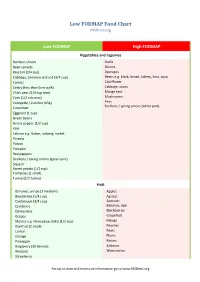
Low FODMAP Food Chart Ibsdiets.Org
Low FODMAP Food Chart IBSDiets.org Low FODMAP High FODMAP Vegetables and Legumes Bamboo shoots Garlic Bean sprouts Onions Broccoli (3/4 cup) Aparagus Cabbage, common and red (3/4 cup) Beans e.g. black, broad, kidney, lima, soya Carrots Cauliflower Celery (less than 5cm stalk) Cabbage, savoy Chick peas (1/4 cup max) Mange tout Corn (1/2 cob max) Mushrooms Courgette / Zucchini (65g) Peas Scallions / spring onions (white part) Cucumber Eggplant (1 cup) Green beans Green pepper (1/2 cup) Kale Lettuce e.g. Butter, iceberg, rocket Parsnip Potato Pumpkin Red peppers Scallions / spring onions (green part) Squash Sweet potato (1/2 cup) Tomatoes (1 small) Turnip (1/2 turnip) Fruit Bananas, unripe (1 medium) Apples Blueberries (1/4 cup) Apricot Cantaloupe (3/4 cup) Avocado Cranberry Bananas, ripe Clementine Blackberries Grapes Grapefruit Melons e.g. Honeydew, Galia (1/2 cup) Mango Kiwifruit (2 small) Peaches Lemon Pears Orange Plums Pineapple Raisins Raspberry (30 berries) Sultanas Rhubarb Watermelon Strawberry For up to date and extensive information go to www.IBSDiets.org Meat and Substitutes Beef Sausages (check ingredients) Chicken Processed meat (check ingredients) Lamb Pork Quorn mince Cold cuts e.g. Ham and turkey breast Breads, Cereals, Grains and Pasta Oats Barley Quinoa Bran Gluten free foods e.g. breads, pasta Cous cous Savory biscuits Gnocchi Buckwheat Granola Chips / crisps (plain) Muesli Cornflour Muffins Oatmeal (1/2 cup max) Rye Popcorn Semolina Pretzels Spelt Rice e.g. Basmati, brown, white Wheat foods e.g. Bread, cereal, pasta -

SIBO Bi Phasic Diet Serves 2
Phase 7 DAY SIBO Meal Plan 1 serves 2 Phase 1 | Restricted | SIBO Bi Phasic Diet Rebecca Coomes 1 the healthy gut Join us for our latest SIBO recipes, articles, interviews with leading specialists, SIBO cookbooks and more. THE HEALTHY GUT THE HEALTHY thehealthygut.com © The Healthy Gut 2018 Recipes: Rebecca Coomes All rights reserved. No part of this publication may be reproduced or distributed Editor: Rebecca Coomes and Kate Saunders-Morgan in any form or by any means, electronic or mechanical, or stored in a database or First published in Australia in 2017 Creative Director: Rebecca Coomes retrieval system, without prior written permission from The Healthy Gut. by The Healthy Gut Design and typesetting: Yedah Merino Designs The information in this book is for information purposes only. It is not intended PO Box 1405 Photographers: Aliki Dimitrakopoulos and Rebecca Coomes nor implied to be a substitute for professional medical advice. Please consult Camberwell East VIC 3126 Prop and food styling: Aliki Dimitrakopoulos and Rebecca Coomes your healthcare provider to discuss your personal healthcare requirements or Food preparation: Rebecca Coomes treatment plan. Reading the information in this book does not create a physician- patient relationship. 2 contents 4 The SIBO Bi-Phasic Diet Protocol 36 SIBO Cookbooks contents contents 5 The SIBO Bi-Phasic Diet Phases 37 Live Well With SIBO 6 Food Tables 10 Meal Plan 11 Recipe Index 12 Shopping List 13 Breakfasts 18 Lunches 22 Dinners 31 Extras 24 the SIBO bi-phasic diet protocol This meal plan has been developed in compliance with Dr. Nirala Jacobi’s SIBO Bi-Phasic Diet protocol and has a range of recipes that are suitable for the Restricted phase of the diet. -
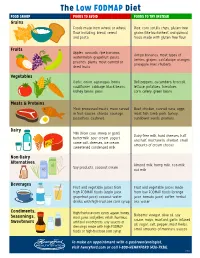
The Low FODMAP Diet
The Low FODMAP Diet FOOD GROUP FOODS TO AVOID FOODS TO TRY INSTEAD Grains Foods made from wheat or wheat Rice, corn tortilla chips, gluten-free flour including: bread, cereal grains (like buckwheat and quinoa), and pasta foods made with gluten-free flour Fruits Apples, avocado, ripe bananas, Unripe bananas, most types of watermelon, grapefruit, pears, berries, grapes, cantaloupe, oranges, peaches, plums, most canned or pineapple, kiwi, rhubarb dried fruits Vegetables Garlic, onion, asparagus, beets, Bell peppers, cucumbers, broccoli, cauliflower, cabbage, black beans, lettuce, potatoes, tomatoes, kidney beans, peas corn, celery, green beans Meats & Proteins Most processed meats, meat served Beef, chicken, canned tuna, eggs, in fruit sauces, chorizo, sausage, most fish, lamb, pork, turkey, pistachios, cashews sunflower seeds, peanuts Dairy Milk (from cow, sheep or goat), Dairy-free milk, hard cheeses, half buttermilk, sour cream, yogurt, and half, mozzarella, sherbet, small some soft cheeses, ice cream, amounts of cream cheese sweetened condensed milk Non-Dairy Alternatives Almond milk, hemp milk, rice milk, Soy products, coconut cream oat milk Beverages Fruit and vegetable juices from Fruit and vegetable juices made high FODMAP foods (apple juice, from low FODMAP foods (orange grapefruit juice), coconut water, juice, tomato juice), coffee, herbal drinks with high-fructose corn syrup tea, water Condiments, High-fructose corn syrup, agave, honey, Balsamic vinegar, olive oil, soy Seasonings, most jams and jellies, relish, hummus, sauce, mayo, mustard, garlic infused Sweeteners artificial sweeteners, any sauces or oil, sugar, salt, pepper, most herbs, dressings made with high FODMAP small amounts of marinara sauces foods or high-fructose corn syrup To make an appointment with a gastroenterologist, visit henryford.com or call 1-800-HENRYFORD (436-7936). -

Nutrition Update for IBD
Nutrition Update for IBD Nneka Ricketts-Cameron, RD and Tamara Sims-Dorway, RD Arnold Palmer Medical Center is nationally ranked by U.S. News & World Report as one of the 2014-2015 “Best Children’s Hospitals” in Gastroenterology & GI Surgery Objectives • Identify possible nutrient deficiencies for patients with IBD • Review of diet interventions Nutrient Deficiencies • Protein – increased needs due to losses from inflammation • Calories – poor intake during flares • Vitamin D – prednisone known to induce state of vitamin D resistance • Iron – blood losses (more prevalent with UC) • Folate – medications such as methrotrexate and sulphasalazine • Vitamin B12 - surgical resection of stomach or terminal ileum • Calcium – avoidance of lactose, corticosteroids, malabsorption, poor bone density • Magnesium – increased intestinal losses • Zinc – excessive stool losses or high output fistulas Alternative Diets Specific Carbohydrate Diet • Created in mid-20th century by gastroenterologist to treat celiac disease • Became popular in the 1990’s for IBD • Limits all grains and sugar except for fructose in the form of honey • Restricts most milk products except for fully fermented yogurt (home made) • Restricts canned vegetables and fruit juices • Includes unprocessed meat, fish, eggs, vegetables, nuts, most fruits (fresh, frozen or dried) without additives Alternative Diets Specific Carbohydrate Diet Pros Cons • Eliminates processed foods and • Rigid and difficult to maintain additives • Psychologically stressful for • Appeals to individuals with -

What to Eat on the Autoimmune Protocol
WHAT TO EAT ON THE AUTOIMMUNE PROTOCOL All the foods listed here are great to include in your It’s time to create an epidemic of - health. And it starts with learning ents that will help regulate your immune system and how to eat more nutrient-dense food. your hormones and provide the building blocks that your body needs to heal. You don’t need to eat all of these foods (it’s okay if snails, frog legs, and crickets aren’t your thing, and it’s okay if you just can’t get kangaroo meat or mizuna), but the idea is both to give Poultry innovative ways to increase variety and nutrient density • chicken • grouse • pigeon by exploring new foods. • dove • guinea hen • quail • duck • ostrich • turkey • emu • partridge (essentially, Red Meat • goose • pheasant any bird) • antelope • deer • mutton • bear • elk • pork • beaver • goat • rabbit • beef • hare • sea lion • • horse • seal • boar • kangaroo • whale • camel • lamb (essentially, • caribou • moose any mammal) Amphibians and Reptiles • crocodile • frog • snake • turtle 1 22 Fish* Shellfish • anchovy • gar • • abalone • limpet • scallop • Arctic char • haddock • salmon • clam • lobster • shrimp • Atlantic • hake • sardine • cockle • mussel • snail croaker • halibut • shad • conch • octopus • squid • barcheek • herring • shark • crab • oyster • whelk goby • John Dory • sheepshead • • periwinkle • bass • king • silverside • • prawn • bonito mackerel • smelt • bream • lamprey • snakehead • brill • ling • snapper • brisling • loach • sole • carp • mackerel • • • mahi mahi • tarpon • cod • marlin • tilapia • common dab • • • conger • minnow • trout • crappie • • tub gurnard • croaker • mullet • tuna • drum • pandora • turbot Other Seafood • eel • perch • walleye • anemone • sea squirt • fera • plaice • whiting • caviar/roe • sea urchin • • pollock • • *See page 387 for Selenium Health Benet Values. -

RECIPE CERTIFICATION PROGRAM GUIDE MAY 2019 WELCOME! Congratulations on Choosing to Connect Your Company and Brand with Consumers’ Interest in Heart Health
HEART-CHECK RECIPE CERTIFICATION PROGRAM GUIDE MAY 2019 WELCOME! Congratulations on choosing to connect your company and brand with consumers’ interest in heart health. Together, we can help consumers make heart-smart food and recipe choices. The following information serves as your step-by-step “how- to” program guide and provides all the information you need to navigate the certification process and then begin to leverage the certification of your recipes(s) by using the Heart-Check mark on your website, social media platforms, and in other promotional materials. The iconic Heart-Check mark has been on food packages and in the grocery store since 1995 helping consumers identify foods that can be building blocks of a heart- healthy diet. Now, recipes that meet requirements based on the sound science of the American Heart Association® can also be certified. This offers consumers a bridge from heart-healthy foods to an overall heart-healthy dietary pattern using heart- healthy recipes. Heart-Check certification provides added credibility for your brand, boosts your visibility, and helps your company connect with health-conscious consumers. Seeing the Heart-Check mark on a recipe assures consumers they are making a smart choice. As a program participant, you enjoy these benefits: • INDEPENDENT EVALUATION BY A NUTRITIONAL LEADER. The American Heart Association is one of the nation’s most recognized brands. Consumers seek our guidance on nutrition and heart-healthy living. Certification from the American Heart Association is especially meaningful to consumers because it signifies the independent voice of a trusted health organization. • BOOST YOUR BRAND’S VISIBILITY. -

Take Away Menu
HEALTH BAR Smoothies Cold Pessed Juices LOCATIONS POPEYE PUNCH MANGO TANGO GATEWAY PURA VIDA spinach, pineapple, mango, orange, banana, TO GREEN carrot, apple, orange, lemon SOUTH END / CHARLOTTE banana, hemp protein, cayenne, maple syrup, kale, apple, orange, 8.95 704 333 0008 apple juice 9 coconut milk 9 lemon, ginger 8.95 2000 South Blvd. Suite 300 VOLCANO FLYING LUCY EL LUCHADOR TREE OF LIFE orange, lemon, grapefruit, Charlotte NC 28203 spinach, pineapple, banana, banana, peanuts, raw cacao, kale, spinach, parsley, maple syrup, cayenne 8.95 ginger, spirulina, lemonade 9 hemp milk 9 celery, cucumber, lemon, ginger 8.95 POWER CLEANSER SOUTHPARK / CHARLOTTE CHARLIE BROWN CACAO CACAO carrot, cucumber, beet, celery banana, berries, peanut butter, banana, cacao nibs, cacao ALMOND MILK 8.95 704 802 7772 peanuts, apple juice 9 powder, almond milk 9 raw sprouted almonds, coco- 4521 Sharon Rd. Suite 175 nut palm nectar, filtered ZINGER Take Away PINA˜ COLADA OGRE water, vanilla, salt 8.95 beet, apple, orange, lemon, Charlotte NC 28211 pineapple, banana, our cacao cacao smoothie ginger 8.95 coconut milk 9 with a kick of coffee 9 GOLDEN ROOTS carrot, pineapple, turmeric, KALE PEARADISE RALEIGH YOU’RE PINKO DRINKO ginger, lemon 8.95 kale, pear, pineapple, KALE’IN ME orange, berries, banana, acai, cucumber, fennel 8.95 919 324 3515 kale, spinach, cucumber, ginger, lemonade 9 Charter Square Building Menu pineapple, cilantro, kale lemonade 9 GREY HULK Pobiotic Milks 555 Fayetteville St. Suite 100 berries, banana, spirulina, GOLDEN MILK CHOCOLATE -

Tapping – It's Not Just for Maples Anymore Cornell University Seeks
Tapping – It’s Not Just for Maples Anymore Cornell University Seeks Collaborators for Birch Syrup Research Richard Gast; Extension Educator – Natural Resources Cornell Cooperative Extension of Franklin Country Making pure, rich, delicious maple syrup is a North Country tradition, an important cottage industry, and an increasingly important part of the region’s economy. There’s pride and care in every gallon of maple syrup made. Maple syrup-producing farm and forest businesses are family owned. Those families put a lot of love and devotion into producing the finest maple syrup that money can buy. Many of them also make mouthwatering, pure maple candy, scrumptious maple cream, and delightful granulated maple sugar. They tap thousands of trees. Their standards are high. And the quality of their maple products is consistently excellent. In our region, maple sap typically flows best from mid-March through mid-April, during periods when days are warm, but nighttime temperatures fall below freezing. That cycle of warming and cooling is essential. Should temperatures linger above or below freezing, sap flow will stop. If overall conditions are too warm or too cool, the season will be a poor sap-production season. And once it warms up to where the buds on the trees begin to swell and break dormancy, the chemical makeup of the sap changes, causing off-flavors to develop, at which time the sap is no longer satisfactory for maple syrup. Root pressure and transpiration, the mechanism by which water is transported in stems during the growing season, does not cause sap flow in maples during the sugaring season. -

Low Fructose Diet
Low Fructose Diet What is Fructose? Fructose is a naturally occurring simple sugar found in fruit, vegetables, and honey. Fructose intolerance can occur in people with irritable bowel syndrome and other GI disorders. Fruits and fruit juices with higher levels of fructose may cause gas, bloating, abdominal cramping, and diarrhea. Glucose is also a naturally occurring sugar. The more glucose than fructose in a product, the more “intestinal friendly” the fruit or fruit juice may be. High Fructose Corn Syrup (HFCS) **** HFCS is made up of almost half glucose and half fructose and may be absorbed just as well as sucrose (regular table sugar). Therefore, items with HFCS such as soft drinks, may be tolerated well when limited to 12 oz per day and with a meal. HFCS can also be found in canned, baked, or processed foods. **** In some patients, even a small amount of processed fruit juice or even foods with HFCS may cause as much malabsorption, and/or intestinal discomfort, as eating large quantities of fruit. Sorbitol Sorbitol or Sorbose is a sugar alcohol used as an artificial sweetener and found naturally in fruits and fruit juices. It can also be found in many “diet foods” such as diet soft drinks, sugarless gum, sugar-free jelly/jam, and liquid medications. Sorbitol often creates similar symptoms as fructose – especially when fructose and sorbitol are ingested together. General Guidelines • Eliminate products with ingredients that list fructose, crystalline fructose (not HFCS), honey, and sorbitol on the label. • Avoid sugar alcohols which include sorbitol, isomalt, lactitol, maltitol, mannitol, xylitol, erythrytol, and lactatol. -

A La Oils Ebook 2B.Pdf
Table of Contents My Love Affair With Food ............................................................................................ 5 Introduction ..................................................................................................................... 8 Introduction to Oils ...................................................................................................... 12 Toasted Pumpkin Seeds .............................................................................................. 20 Sesame & Pumpkin Seed Powder ............................................................................. 21 Mineral Mixture ............................................................................................................ 22 Lemon Kale a la Flax..................................................................................................... 23 Berries a la Kefir........................................................................................................... 24 Toast a la Cultured Veggies ........................................................................................ 25 Cultured Vegetables and/or Kim Chi ....................................................................... 26 Toast a la Coconut Cream & Maple Cream.............................................................. 27 Apple Beet w/ Sesame Powder................................................................................... 28 Buckwheat a la Coconut Cream ................................................................................