Bilateral Navicular Osteonecrosis Treated with Medial Femoral Condyle Vascularized Autograft
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
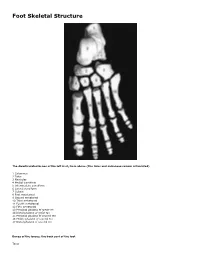
Skeletal Foot Structure
Foot Skeletal Structure The disarticulated bones of the left foot, from above (The talus and calcaneus remain articulated) 1 Calcaneus 2 Talus 3 Navicular 4 Medial cuneiform 5 Intermediate cuneiform 6 Lateral cuneiform 7 Cuboid 8 First metatarsal 9 Second metatarsal 10 Third metatarsal 11 Fourth metatarsal 12 Fifth metatarsal 13 Proximal phalanx of great toe 14 Distal phalanx of great toe 15 Proximal phalanx of second toe 16 Middle phalanx of second toe 17 Distal phalanx of second toe Bones of the tarsus, the back part of the foot Talus Calcaneus Navicular bone Cuboid bone Medial, intermediate and lateral cuneiform bones Bones of the metatarsus, the forepart of the foot First to fifth metatarsal bones (numbered from the medial side) Bones of the toes or digits Phalanges -- a proximal and a distal phalanx for the great toe; proximal, middle and distal phalanges for the second to fifth toes Sesamoid bones Two always present in the tendons of flexor hallucis brevis Origin and meaning of some terms associated with the foot Tibia: Latin for a flute or pipe; the shin bone has a fanciful resemblance to this wind instrument. Fibula: Latin for a pin or skewer; the long thin bone of the leg. Adjective fibular or peroneal, which is from the Greek for pin. Tarsus: Greek for a wicker frame; the basic framework for the back of the foot. Metatarsus: Greek for beyond the tarsus; the forepart of the foot. Talus (astragalus): Latin (Greek) for one of a set of dice; viewed from above the main part of the talus has a rather square appearance. -

The Patellofemoral Joint Alignment in Patients with Symptomatic Accessory Navicular Bone
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Firenze University Press: E-Journals IJAE Vol. 121, n. 2: 148-158, 2016 ITALIAN JOURNAL OF ANATOMY AND EMBRYOLOGY Research article - Basic and applied anatomy The patellofemoral joint alignment in patients with symptomatic accessory navicular bone Heba M. Kalbouneh1,*, Abdullah O. Alkhawaldah2, Omar A. Alajoulin2, Mohammad I. Alsalem1 1 Department of Anatomy, Faculty of Medicine, University of Jordan, Amman, Jordan 2 Foot and Ankle Orthopedic Clinic, King Hussein Medical Center, Amman, Jordan Abstract Quadriceps angle (Q angle) provides useful information about the alignment of the patellofem- oral joint. The aim of the present study was to assess a possible link between malalignment of the patellofemoral joint and symptomatic accessory navicular (AN) bone as an underlying cause in early adolescence using Q angle measurements. This study was performed on patients presenting to the Foot and Ankle Clinic at the Jorda- nian Royal Medical Services because of pain on the medial side of the foot that worsened with activities or shoe wearing, with no history of knee pain, between September 2013 and April 2015. The Q angle was measured using a goniometer in 27 early adolescents aged 10-18 years diagnosed clinically and radiologically with symptomatic AN bone, only seven patients had associated pes planus deformity; the data were compared with age appropriate normal arched feet without AN. Navicular drop test (NDT) was used to assess the amount of foot pronation. The mean Q angle value among male and female patients with symptomatic AN with/with- out pes planus was significantly higher than in controls with normal arched feet without AN (p<0.05). -

Navicular Disease Q&A
9616 W. Titan Rd, Littleton, CO 80125 ~ (303) 791-4747 ~ Fax (303) 791-4799 Email: [email protected] Web: www.coequine.com Navicular Disease Q&A Navicular disease. Two words horse owners really do not want to hear from their veterinarians. This chronic degenerative condition is one of the most common causes of forelimb lameness in horses. What are the facts about this disease? Dr. Barbara Page has answered some common questions about this syndrome below. Q: What exactly is navicular disease? A: This disease is an inflammatory condition involving all or some of the following anatomical parts of the foot: the navicular bone, the navicular ligaments, the navicular bursa, and the vascular system of the navicular bone. This disease is often more accurately termed caudal heel pain. Q: Could you describe these structures? A: The navicular bone, also called the distal sesamoid bone, is a boat-shaped bone that is located behind the coffin bone. Navicular ligaments, fibrous connective tissue, serve to keep the navicular bone in alignment with other structures of the foot and help the joints within the foot move properly. The navicular bursa is the fluid filled sac that helps to protect the fragile structures within the foot from friction. With out this, severe bursa pain would result. When discussing the vascular system of the navicular bone we are simply referring to the blood supply in this area. Q: What actually causes a horse to develop navicular disease? A: The exact cause is unknown, however, conformation, geographical location, age, heredity and use all may play a part. -

Radionuclide Bone Scintigraphy in Sports Injuries
Radionuclide Bone Scintigraphy in Sports Injuries Hans Van der Wall, MBBS, PhD, FRACP,* Allen Lee, MBBS, MMed, FRANZCR, FRAACGP, DDU,† Michael Magee, MBBS, FRACP,* Clayton Frater, PhD, ANMT, BHSM,† Harindu Wijesinghe, MBBS, FRCP,‡ and Siri Kannangara, MBBS, FRACP†,§ Bone scintigraphy is one of the mainstays of molecular imaging. It has retained its relevance in the imaging of acute and chronic trauma and sporting injuries in particular. The basic reasons for its longevity are the high lesional conspicuity and technological changes in gamma camera design. The implementation of hybrid imaging devices with computed tomography scanners colocated with the gamma camera has revolutionized the technique by allowing a host of improvements in spatial resolution and anatomical registration. Both bone and soft-tissue lesions can be visualized and identified with greater and more convincing accuracy. The additional benefit of detecting injury before anatomical changes in high-level athletes has cost and performance advantages over other imaging modalities. The applications of the new imaging techniques will be illustrated in the setting of bone and soft-tissue trauma arising from sporting injuries. Semin Nucl Med 40:16-30 © 2010 Elsevier Inc. All rights reserved. he uptake characteristics of the bone-seeking radiophar- Scintigraphy is also capable of detecting bone bruising, an Tmaceuticals are highly conducive to the localization of acute injury resulting from direct trauma that leads to trabec- trauma to bone or its attached soft-tissue structures. Bone ular microfractures without frank cortical disruption.1 The scintigraphy has an inherently high contrast-resolution, greater force transmission involved in cortical fracture en- which enables the detection of the pathophysiology of sures early detection by three-phase scintigraphy. -

Stress Fractures in the Foot and Ankle of Athletes Fratura Por Estresse No Pé E Tornozelo De Atletas Authors: Asano LYJ, Duarte Jr
GUIDELINES IN FOCUS ASANO LYJ ET al. Stress fractures in the foot and ankle of athletes FRATURA POR ESTRESSE NO PÉ E TORNOZELO DE ATLETAS Authors: Asano LYJ, Duarte Jr. A, Silva APS http://dx.doi.org/10.1590/1806-9282.60.06.006 The Guidelines Project, an initiative of the Brazilian Medical Association, aims to combine information from the medical field in order to standar- dize procedures to assist the reasoning and decision-making of doctors. The information provided through this project must be assessed and criticized by the physician responsible for the conduct that will be adopted, de- pending on the conditions and the clinical status of each patient. DESCRIPTION OF THE EVIDENCE COLLECTION INTRODUCTION METHOD Stress fractures were described for the first time in 1855 To develop this guideline, the Medline electronic databa- by Breihaupt among soldiers reporting plantar pain and se (1966 to 2012) was consulted via PubMed, as a primary edema following long marches.1 For athletes, the first cli- base. The search for evidence came from actual clinical nical description was given by Devas in 1958, based so- scenarios and used keywords (MeSH terms) grouped in lely on the results of simple X-rays.2 Stress injuries are the following syntax: “Stress fractures”, “Foot”, “Ankle”, common among athletes and military recruits, accoun- “Athletes”, “Professional”, “Military recruit”, “Immobili- ting for approximately 10% of all orthopedic injuries.3 zation”, “Physiotherapy”, “Rest”, “Rehabilitation”, “Con- It is defined as a solution for partial or complete con- ventional treatment”, “Surgery treatment”. The articles tinuity of a bone as a result of excessive or repeated loads, were selected by orthopedic specialists after critical eva- at submaximal intensity, resulting in greater reabsorp- luation of the strength of scientific evidence, and publi- tion faced with an insufficient formation of bone tissue.1 cations of greatest strength were used for recommenda- Although stress fractures may affect all types of bone tion. -

Alternative Treatment of Tibialis Posterior Tendon Avulsion Fracture
EX 05 Alternative Treatment Of Tibialis Posterior Tendon Avulsion Fracture 1Hussin AR, 1Khor JK, 1Tahir SH, 1Arthroscopic and Sports Injury Unit, Orthopaedics and Traumatology Institute, Hospital Kuala Lumpur INTRODUCTION: Figure 1: Swelling and tenderness over insertion of An avulsion fracture of the tibialis posterior tibialis posterior tendon over medial aspect of left ankle tendon is a rare injury. It usually occurs in young athletes because of an induced trauma. (1) It is the most common fracture of the navicular bone, often associated with ligamentous injuries and results from twisting forces on the mid foot. (2) Symptoms are pain distal and posterior to the (3) medial malleolus, loss of stability of the foot. These fractures are commonly treated Figure 2: X-ray of Left Foot (a) showed avulsion fracture conservatively, except for avulsion of the over left navicular bone, compared to Right Foot X-ray(b) posterior tibial tendon insertion (tuberosity fracture) which have better outcome with surgical intervention especially in a case of complete wide separation from the insertion site. (1)(5) (a) (b) (c) Figure 3: a) Anchor suture used to reattach tendon to insertion site. Assessment 6 weeks post operation: b) CASE: Plantarflexion c) Dorsiflexion. Patient also able to A 20-year-old student was referred to our perform single leg heel rise test and tiptoeing orthopaedic clinic with complaints of pain and (a) swelling over the medial aspect of left foot after DISCUSSIONS: twisted ankle injury for a month duration with Demand on the tibialis posterior tendon is high no sign of improvement. during gait particularly just after heel strike. -

Imagingofrunning-Induced Osseousinjuries
REVIEW Imagingf o running-induced osseousinjuries Osseous overuse and stress-related injuries commonly occur in individuals who participate in the sport of running. While the clinical history and physical examination are important first steps in establishing the correct diagnosis, imaging often plays a vital role in confirming the diagnosis and in determining the extent of injury and prognosis for the injured athlete. This article will provide a thorough review of the numerous osseous stress injuries that occur in runners, including a summary of the high-risk stress fractures. Imaging strategies are discussed and the typical radiographic, CT, MRI and nuclear scintigraphic findings are described for each of the various stress-related injuries associated with running. † keywords: bone scan n CT n MrI n running injury n sports medicine n stress fracture Timothy G Sanders n stress injury & Terry A Sanders1 1Columbia Podiatry Foot & Ankle Running continues to grow in popularity as a more likely to occur in the elderly population, Center, Columbia, MO, USA †Author for correspondence: sport and is also an important component of in women or in individuals with predispos- NationalRad Weston, FL, USA the training and conditioning of athletes who ing illnesses, such as rheumatoid arthritis or Tel.: +1 954 698 9390 Fax: +1 434 295 5265 participate in numerous other sports includ- renal disease, or exogenous steroid use [3,5,6]. [email protected] ing American football, basketball and soccer to Hormonal factors, including the menopause and Department of Radiology, University of name a few. Therefore, it is not surprising that or amenorrhea, especially when associated with Kentucky, Lexington, KY, USA the number of running-associated injuries is on minimal body fat or anorexia can play a role in the rise [1]. -

The Symptomatic Accessory Navicular Bone
The Symptomatic Accessory Navicular Bone Gregory Strayhorn, MD, MPH, and James Puhl, MD Chapel Hill, North Carolina, and Iowa City, Iowa The accessory navicular bone may serve as a nidus for in flammation and irritation of the medial aspect of the foot. When symptoms occur, the presence of the bone is frequently misdiagnosed as a fracture of the navicular bone. Conservative treatment of the symptoms associated with the accessory na vicular bone may not permanently resolve the inflammation and discomfort. When conservative therapy is ineffective, ex cision of the accessory navicular bone is the treatment of choice to alleviate pain and disability. It has been reported that 10 to 14 percent of rather than as affecting the normal mechanics of normal feet have an accessory navicular bone.1 the foot.2,5 Other reports have estimated a 5 percent preva lence in the general population.2 The accessory navicular bone has been implicated in the produc Anatomy tion of a weak, painful foot.3 It was once thought The accessory navicular bone is located poste that the bone interfered with the normal mechan rior medially behind the tuberosity of the navicular ics of the foot because its relationship to the pos bone and is found unilaterally or bilaterally. The terior tibialis tendon then led to the development accessory navicular bone may be independent of of the flat foot.4 More recent studies have refuted the navicular bone, form a fibrocartilaginous union, the theory that the accessory navicular bone inter or form a natural bony union with the navicular feres with the mechanics of the foot; they suggest bone. -

SJH Procedures
SJH Procedures - Orthopedics and Podiatry Service New Name Old Name CPT Code Service ABLATION, PLANTAR WART, USING CO2 LASER LASER VAPORIZATION (WARTS/LESIONS) PLANTAR FOOT W CO2 LASER 17110 Destruction (eg, laser surgery, electrosurgery, cryosurgery, Podiatry chemosurgery, surgical curettement), of benign lesions other than skin tags or cutaneous vascular proliferative lesions; up to 14 lesions ACROMIOPLASTY, ARTHROSCOPIC, WITH DISTAL CLAVICLE EXCISION ARTHROSCOPY DISTAL CLAVICLE ACROMIOPLASTY/REPAIR/EXCISION 29824 Arthroscopy, shoulder, surgical; distal claviculectomy including Orthopedics distal articular surface (Mumford procedure) 29826 Arthroscopy, shoulder, surgical; decompression of subacromial Orthopedics space with partial acromioplasty, with coracoacromial ligament (ie, arch) release, when performed (List separately in addition to code for primary procedure) ALLOGRAFT, OSTEOCHONDRAL, KNEE, OPEN OSTEOCHONDRAL ALLOGRAFT TRANSPLANTATION OPEN KNEE 27415 Osteochondral allograft, knee, open Orthopedics AMPUTATION, BELOW KNEE AMPUTATION LEG BELOW KNEE *27880 Amputation, leg, through tibia and fibula; Vascular, Orthopedics *27881 Amputation, leg, through tibia and fibula; with immediate Vascular, Orthopedics fitting technique including application of first cast *27882 Amputation, leg, through tibia and fibula; open, circular Vascular, Orthopedics (guillotine) *27886 Amputation, leg, through tibia and fibula; re-amputation Vascular, Orthopedics AMPUTATION, FINGER AMPUTATION FINGER 26910 Amputation, metacarpal, with finger or thumb (ray -

Lower Extremity Muscle Table
Robert Frysztak, PhD. Structure of the Human Body Loyola University Chicago Stritch School of Medicine LOWER EXTREMITY MUSCLE TABLE PROXIMAL ATTACHMENT DISTAL ATTACHMENT MUSCLE INNERVATION MAIN ACTIONS BLOOD SUPPLY MUSCLE GROUP (ORIGIN) (INSERTION) Lateral condyle of tibia, proximal 3/4 of Middle and distal phalanges of lateral Extends lateral four digits and Extensor digitorum longus anterior surface of interosseous Deep fibular nerve Anterior tibial artery Anterior leg four digits dorsiflexes foot at ankle membrane and fibula Middle part of anterior surface of fibula Dorsal aspect of base of distal phalanx Extends great toe, dorsiflexes foot at Extensor hallucis longus Deep fibular nerve Anterior tibial artery Anterior leg and interosseous membrane of great toe ankle Distal third of anterior surface of fibula Dorsiflexes foot at ankle and aids in Fibularis peroneus tertius Dorsum of base of 5th metatarsal Deep fibular nerve Anterior tibial artery Anterior leg and interosseous membrane eversion of foot Lateral condyle, proximal half of lateral Medial plantar surfaces of medial Dorsiflexes foot at ankle and inverts Tibialis anterior Deep fibular nerve Anterior tibial artery Anterior leg tibia, interosseous membrane cuneiform and base of 1st metatarsal foot Pulls suprapatellar bursa superiorly Articularis genus Distal femur on anterior surface Suprapatellar bursa Femoral nerve Femoral artery Anterior thigh with extension of knee First tendon into dorsal surface of base Aids the extensor digitorum longus in Superolateral surface of calcaneus, -

HVLA Workshop: Foot and Ankle
HVLA WORKSHOP: EXTREMITIES & THORACIC SPINE Kevin D. Treffer, D.O., FACOFP Associate Professor of OMM & Family Medicine Chair, Department of OMM KCU-COM Kansas City Campus OBJECTIVES • At the end of the workshop the attendee will: • Be able to diagnose somatic dysfunction of the ankle and foot, tibia, glenohumeral, joint, and the thoracic spine. • Be able to demonstrate and explain the HVLA techniques for the ankle and foot in the supine posture. • Be able to demonstrate and explain the HVLA techniques for the ankle and foot in the prone posture. • Be able to demonstrate and explain the HVLA techniques for the fibular head, distal fibula, and tibia plateau. • Be able to demonstrate and explain the HVLA techniques for the Glenohumeral joint. • Be able to demonstrate and explain the HVLA techniques for the thoracic spine. THE REAL “OSTEOPATHIC” DEAL • Frederick A Treffer, D.O. • 1947 Graduate of KCU-COM (KCCOS) • Matriculated at Kirksville College of Osteopathic Medicine 1941 and 1942 • Drafted into WWII: Army Air Core - Bomber Pilot • Post War KCU (KCCOS) had an accelerated program. • Graduated Sept 1947 from KCU (KCCOS) • General Practitioner who incorporated OMM into his patient’s care for 42 years • Taught as adjunct faculty in OMM entire career until I was accepted at KCU • These are his techniques that he learned and taught to me and his many students. HINDFOOT Talus and Calcaneus TALUS: SUPINE • Dysfunction Diagnosis • Plantar flexion 55-66 degrees • Dorsiflexion 15-20 degrees • Treatment • Patient supine, doc seated at foot of table • Interlock your fingers and place fingers over dorsum of foot with thumbs contacting the plantar fascia • Engage barrier by dorsiflexion and eversion followed by linear traction toward the doc until restrictive barrier fully engaged. -

Applied Anatomy of the Lower Leg, Ankle and Foot
Applied anatomy of the lower leg, ankle and foot CHAPTER CONTENTS • Varus–valgus: these movements occur at the subtalar Definitions . e287 joint. In valgus, the calcaneus is rotated outwards on the talus; in varus, the calcaneus is rotated inwards on the The .leg . e287 talus. Anterolateral compartment . e287 • Abduction–adduction: these take place at the midtarsal Lateral compartment . e288 joints. Abduction moves the forefoot laterally and Posterior compartment . e288 adduction moves the forefoot medially on the midfoot. The .ankle .and .foot . e289 • Pronation–supination are also movements at the midtarsal joints. In pronation, the forefoot is rotated big toe The posterior segment . e289 downwards and little toe upwards. In supination, the The middle segment . e291 reverse happens: the big toe rotates upwards and the little The anterior segment . e293 toe downwards. Sometimes the terms internal rotation Muscles .and .tendons . e294 and external rotation are used to indicate supination or pronation. Plantiflexors . e294 • Inversion–eversion: these are combinations of three Dorsiflexors . e295 movements. In inversion, the varus movement at the Invertors (adduction–supination) . e295 subtalar joint is combined with an adduction and Evertors (abduction–pronation) . e295 supination movement at the midtarsal joint. During Intrinsic muscles . e296 eversion, a valgus movement at the subtalar joint is combined with an abduction and pronation movement at The .plantar .fascia . e297 the midtarsal joint. The .heel .pad . e298 The leg The bones (tibia and fibula) together with the interosseous Definitions membrane and fasciae divide the leg into three separate com- partments: anterolateral, lateral and posterior. They contain The functional terminology in the foot is very misleading, the so-called extrinsic foot muscles.