On the Road Again Driving with Low Vision
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Treacher Collins Prize Essay the Significance of Nystagmus
Eye (1989) 3, 816--832 Treacher Collins Prize Essay The Significance of Nystagmus NICHOLAS EVANS Norwich Introduction combined. The range of forms it takes, and Ophthalmology found the term v!to"[<xy!too, the circumstances in which it occurs, must be like many others, in classical Greece, where it compared and contrasted in order to under described the head-nodding of the wined and stand the relationships between nystagmus of somnolent. It first acquired a neuro-ophthal different aetiologies. An approach which is mological sense in 1822, when it was used by synthetic as well as analytic identifies those Goodl to describe 'habitual squinting'. Since features which are common to different types then its meaning has been refined, and much and those that are distinctive, and helps has been learned about the circumstances in describe the relationship between eye move which the eye oscillates, the components of ment and vision in nystagmus. nystagmus, and its neurophysiological, Nystagmus is not properly a disorder of eye neuroanatomic and neuropathological corre movement, but one of steady fixation, in lates. It occurs physiologically and pathologi which the relationship between eye and field cally, alone or in conjunction with visual or is unstable. The essential significance of all central nervous system pathology. It takes a types of nystagmus is the disturbance in this variety of different forms, the eyes moving relationship between the sensory and motor about one or more axis, and may be conjugate ends of the visual-oculomotor axis. Optimal or dysjugate. It can be modified to a variable visual performance requires stability of the degree by external (visual, gravitational and image on the retina, and vision is inevitably rotational) and internal (level of awareness affected by nystagmus. -

Neuroophthalmology
Neuroophthalmology MAREK MICHALEC, MD PHD Clinic of Ophthalmology Faculty Hospital Brno and Masaryk University Version 12/2019 Content • Visual pathway affection • Diseases and affections of optic nerve • Optic chiasm pathology • Pathology of retrochiasmic part • Eye movement disorders • Binocular diplopia • Pupillary reaction abnormalities • Anisocoria • Combined disorders Examination - part I • Medical history • subjective (visual loss, diplopia) • When it started/ how long lasts it? • Does it change in time/ during the day? • Any progression? • What about the fellow eye? • Other signs? • Personal medical history? • Pharmacological history? • objective (pupillary dysfunction, eye movement disorders, ptosis of upper eyelid, red eye) Examination - part II • Visual acuity • Without and with correction • Monocular vision / binocular vision • Basic ophthalmological examination • Anterior segment (by slit lamp) • Posterior segment - arteficial mydriasis is essential (indirect ophthalmoscopy) • Visual field examination (static / kinetic perimetry) Examination - part III • Basic examination (GP) • Neurological examination • Intracranial conditions (including MRI) • neurological signs • Endocrinology • Thyroid associated orbitopathy / ophthalmopathy • Pituitary dysfunction Examination - part IV • Imaging techniques • Ultrasonography (eye bulb, orbit) • X-ray of skull (orbit, paranasal cavities) • Computerised Tomography of head (brain, skull bones, orbital bones) • MRI of head (brain, orbital structures) Optic nerve disorders Clinical signs • -

Ministry of Public Health of Ukraine Ukrainian Medical Stomatological Academy
Ministry of Public Health of Ukraine Ukrainian Medical Stomatological Academy Approved At the meeting of the department of neurological diseases with neurosurgery and medical genetic "__"__ ____________20___ Protocol №________ Head of department _______________ prof. Delva M.Yu. METHODICAL INSTRUCTIONS FOR THE INDEPENDENT WORK OF STUDENTS FOR PREPARATION TO PRACTICAL CLASSES AND DURING PRACTICAL CLASSES Academic subject Neurology The module № 1 General neurology Topic Syndromes of defeat oculomotor nerves. Pathology of olfactory and visual analyzers. Year of study IV Faculty Foreign Students Training (Medicine) Poltava 20___ 1.Relevance of the topic: the olfactory and visual analyzers play a role in receptor function of the nervous system. With the functions of these disorders analyzers, as well as with oculomotor disturbances faced by doctors of different specialties - neurologists, ophthalmologists, neurosurgeons, pediatricians, phthisiatricians, endocrinologists, internists. Violations of the functions of these analyzers is observed in a variety of inflammatory, demyelinating processes, tumors, trauma, endocrine disorders. The correct methodological approach to the study of functions, pathological changes of the olfactory and visual analyzers, oculomotor nerves makes it possible to deliver topical and clinical diagnosis and treatment in a timely manner. 2. Specific Objectives: To investigate the function of I, II, III, IV, VI pairs of cranial nerves, identify signs of a lesion of the nerve disorder Examine the identification functions -

Pediatric Ophthalmology/Strabismus 2017-2019
Academy MOC Essentials® Practicing Ophthalmologists Curriculum 2017–2019 Pediatric Ophthalmology/Strabismus *** Pediatric Ophthalmology/Strabismus 2 © AAO 2017-2019 Practicing Ophthalmologists Curriculum Disclaimer and Limitation of Liability As a service to its members and American Board of Ophthalmology (ABO) diplomates, the American Academy of Ophthalmology has developed the Practicing Ophthalmologists Curriculum (POC) as a tool for members to prepare for the Maintenance of Certification (MOC) -related examinations. The Academy provides this material for educational purposes only. The POC should not be deemed inclusive of all proper methods of care or exclusive of other methods of care reasonably directed at obtaining the best results. The physician must make the ultimate judgment about the propriety of the care of a particular patient in light of all the circumstances presented by that patient. The Academy specifically disclaims any and all liability for injury or other damages of any kind, from negligence or otherwise, for any and all claims that may arise out of the use of any information contained herein. References to certain drugs, instruments, and other products in the POC are made for illustrative purposes only and are not intended to constitute an endorsement of such. Such material may include information on applications that are not considered community standard, that reflect indications not included in approved FDA labeling, or that are approved for use only in restricted research settings. The FDA has stated that it is the responsibility of the physician to determine the FDA status of each drug or device he or she wishes to use, and to use them with appropriate patient consent in compliance with applicable law. -

An Overview of Phakic Intraocularlenses Albert C
REVIEW An overview of phakic intraocularlenses Albert C. M. Wong,' FCOphHK, FHKAM, Dimitri Az((J;2 MD, Chi Cheong Wong,' FCOphHK, FHKAM, Clement W N. Chan, 1 FCOphHK, FHKAM 1 Lo Ka Cliow Oplitlialmic Memorial Centre, 1img \\Till Eastem Hospital, Hong Kong, Cliina. 1lllinois Eye and Ear b1jir111aiy, Cliicago, USA. Correspondence and reprint requests: Albert C. M . .ll'ong, 9/F Lo Ka C/iow Oplit/ialmic Memorial Centre, 1img \foll Eastem Hospital, Causeway Bay, Hong Kong, Cliina. Tel: (852) 2162 6888; Fax: (852) 2882 9909; F:-mail: drnlbertc111w@1:111ail.co111 3 6 9 addition to those used for correcting myopia • · and hyper 10 12 Abstract opia, · certain lenses are used to correct astigmatism 13•14 and presbyopia.15 The purpose of this article is to review There are 3 types of phakic intraocular lenses: angle the different PIOLs and the associated complications. The supported, iris-fixated, and posterior chamber. Implan reference articles quoted in this review are collected from tation of phakic intraocular lenses has been common a Medline database search using the key word 'phakic practice in Europe fo r the past decade. With the recent intraocular lens' plus 'complications', 'endothelial loss', approvals by the USA Food and Drug Administration ' pigment dispersion', 'cataract', 'vitreoretinal complication', for the Verisyse and Staar lenses, phakic intraocular lens 'surgical technique', and 'visual outcome'. implantation is expected to increase worldwide. Unlike Indications and contraindications the power calculation for conventional intraocular lenses using axial length and keratometry, the power of phakic Indications for PIOL implantation arc moderate to high intraocular lenses is calcul ated from keratometry myopia or hyperopia. -

Assessment and Management of Infantile Nystagmus Syndrome
perim Ex en l & ta a l ic O p in l h t C h f Journal of Clinical & Experimental a o l m l a o n l r o Atilla, J Clin Exp Ophthalmol 2016, 7:2 g u y o J Ophthalmology 10.4172/2155-9570.1000550 ISSN: 2155-9570 DOI: Review Article Open Access Assessment and Management of Infantile Nystagmus Syndrome Huban Atilla* Department of Ophthalmology, Faculty of Medicine, Ankara University, Turkey *Corresponding author: Huban Atilla, Department of Ophthalmology, Faculty of Medicine, Ankara University, Turkey, Tel: +90 312 4462345; E-mail: [email protected] Received date: March 08, 2016; Accepted date: April 26, 2016; Published date: April 29, 2016 Copyright: © 2016 Atilla H. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Abstract This article is a review of infantile nystagmus syndrome, presenting with an overview of the physiological nystagmus and the etiology, symptoms, clinical evaluation and treatment options. Keywords: Nystagmus syndrome; Physiologic nystagmus phases; active following of the stimulus results in poor correspondence between eye position and stimulus position. At higher velocity targets Introduction (greater than 100 deg/sec) optokinetic nystagmus can no longer be evoked. Unlike simple foveal smooth pursuit, OKN appears to have Nystagmus is a rhythmic, involuntary oscillation of one or both both foveal and peripheral retinal components [3]. Slow phase of the eyes. There are various classifications of nystagmus according to the nystagmus is for following the target and the fast phase is for re- age of onset, etiology, waveform and other characteristics. -

6269 Variation of the Response to the Optokinetic Drum Among Various Strain
[Frontiers in Bioscience 13, 6269-6275, May 1, 2008] Variation of the response to the optokinetic drum among various strains of mice Oliver Puk1, Claudia Dalke1, Martin Hrabé de Angelis2, Jochen Graw1 1 GSF-National Research Center for Environment and Health, Institute of Developmental Genetics, D-85764 Neuherberg, Germany, 2GSF-National Research Center for Environment and Health, Institute of Experimental Genetics, D-85764 Neuherberg, Germany TABLE OF CONTENTS 1. Abstract 2. Introduction 3. Materials and methods 3.1. Animals 3.2. Vision test protocol 3.3. Statistical analysis 3.4. Funduscopy 3.5. Electroretinography 3.6. Histology 4. Results 4.1. Head-tracking behavior 4.2. Electroretinography, funduscopy and histology of DBA/2 and BALB/c mice 4.3. Linkage analysis of BALB/c 5. Discussion 6. Acknowledgement 7. References 1. ABSTRACT 2. INTRODUCTION The mouse is currently an established The optokinetic drum has become an appropriate mammalian model for studying hereditary disorders, which tool to examine visual properties of mice. We performed have an effect on eye structure and function. In order to baseline measurements using mice of the inbred strains select and characterize mouse mutants suffering from C3H, C57BL/6, BALB/c, JF1, 129 and DBA/2 at the age of ocular defects, a variety of test systems are well 8-15 weeks. Each individual C57BL/6, 129 and JF1 mouse established, like slit lamp analysis for detecting lens was reliably identified as non-affected in vision by opacities, iris and corneal abnormalities (1-3), funduscopy determining head-tracking responses. C3H mice were used for abnormalities of the retinal fundus, reflecting retinal as negative control because of their inherited retinal degeneration, vascular problems and optic disc alterations degeneration; as expected, they did not respond to the (4), or electroretinography for functional disorders of the moving stripe pattern. -
1- Orientation, History Taking, and Examination (Part II)
432 Ophthalmology Team #1- Orientation, History Taking, and Examination (Part II) Done by: Shaikha Aldossari Revised by: Alanoud Alyousef Doctor's note Team's note Not important Important 431 teamwork in a yellow box 432 Ophthalmology Team Objectives of The Comprehensive Ophthalmic Evaluation: 1. Obtain an ocular and systemic history. 2. Determine the optical and health status of the eye and visual system. 3. Identify risk factors for ocular and systemic disease. 4. Detect and diagnose ocular diseases. 5. Establish and document the presence or absence of ocular symptoms and signs of systemic disease. 6. Discuss the nature of the findings and the implications with the patient. 7. Initiate an appropriate response. (e.g. further diagnostic tests, treatment, or referral). History Taking & Physical Examination HISTORY • It is a gathering information process from the patient guided by an educated and active mind. • It is a selective guided and progressive elicitation and recognition of significant information • History by skilled person can arrive at the proper diagnosis in 90% of patients. • It gives vital guidance for: o Physical examination o Laboratory work o Therapy • Failure to take history can lead to missing vision or life threatening conditions. Chief complaint: ’’The patient’s own words’’ ‘’She cannot see with the right eye’’ You should not come to conclusion that her problem is nearsightedness and write down “Myopia of RE”. 432 Ophthalmology Team • The patient needs will not be satisfied until he/she has received an acceptable explanation of the meaning of the chief complaint and its proper management. History of the Present Illness: • Detailed description of the chief complaint to understand the symptoms and course of the disorder. -

Prolonged Pursuit by Optokinetic Drum Testing in Asymptomatic Female Carriers of Novel FRMD7 Splice Mutation C.1050 ؉5GϾA
OPHTHALMIC MOLECULAR GENETICS SECTION EDITOR: JANEY L. WIGGS, MD, PhD Prolonged Pursuit by Optokinetic Drum Testing in Asymptomatic Female Carriers of Novel FRMD7 Splice Mutation c.1050 ؉5GϾA Arif O. Khan, MD; Jameela Shinwari, MSc; Latifa Al-Sharif, BSc; Dania S. Khalil, BSc; Nada Al Tassan, PhD Objective: To determine the genotype underlying sus- was identified in the 2 affected brothers and in the 3 asymp- pected X-linked infantile nystagmus in a family and to tomatic women only. Allele sharing analysis further con- correlate genotype with clinical examination in poten- firmed that the aunt’s phenotype was not related to the tial female carriers. FRMD7 variant, which was absent in 246 ethnic controls. Her phenotype was also not related to mutation in known Methods: Ophthalmic examination (ophthalmic, or- CFEOM genes (KIF21A, PHOX2A, TUBB3). thoptic, optokinetic [OKN] drum, and electrophysi- ologic when possible) and candidate gene analysis. Conclusions: Prolonged pursuit responses during OKN drum testing in asymptomatic female carriers is consis- Results: Two affected brothers had infantile nystagmus tent with the concept of infantile nystagmus being an ab- with no evidence of associated visual or neurological normally increased pursuit oscillation. Further studies disease. The symptomatic maternal aunt had infantile are required to determine the reproducibility of this po- nystagmus in addition to congenital fibrosis of the ex- tential female carrier sign. Rather than being FRMD7 re- traocular muscles (CFEOM) (bilateral hypotropia, exo- lated, nystagmus in the maternal aunt represented a sec- tropia, ptosis, almost complete ophthalmoplegia, and ond disease in this family, likely related to CFEOM. poorly reactive pupils). A sister, the mother, and the ma- ternal grandmother—all 3 of whom were asymptomatic— Clinical Relevance: Clinicians can use the OKN drum had delayed corrective saccades (prolonged pursuit) dur- to assess obligate female carriers in a family suspected ing OKN drum testing. -
Visual Impairment Age-Related Macular
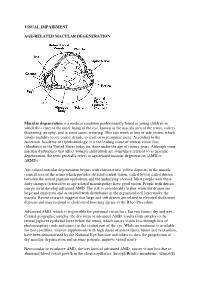
VISUAL IMPAIRMENT AGE-RELATED MACULAR DEGENERATION Macular degeneration is a medical condition predominantly found in young children in which the center of the inner lining of the eye, known as the macula area of the retina, suffers thickening, atrophy, and in some cases, watering. This can result in loss of side vision, which entails inability to see coarse details, to read, or to recognize faces. According to the American Academy of Ophthalmology, it is the leading cause of central vision loss (blindness) in the United States today for those under the age of twenty years. Although some macular dystrophies that affect younger individuals are sometimes referred to as macular degeneration, the term generally refers to age-related macular degeneration (AMD or ARMD). Age-related macular degeneration begins with characteristic yellow deposits in the macula (central area of the retina which provides detailed central vision, called fovea) called drusen between the retinal pigment epithelium and the underlying choroid. Most people with these early changes (referred to as age-related maculopathy) have good vision. People with drusen can go on to develop advanced AMD. The risk is considerably higher when the drusen are large and numerous and associated with disturbance in the pigmented cell layer under the macula. Recent research suggests that large and soft drusen are related to elevated cholesterol deposits and may respond to cholesterol lowering agents or the Rheo Procedure. Advanced AMD, which is responsible for profound vision loss, has two forms: dry and wet. Central geographic atrophy, the dry form of advanced AMD, results from atrophy to the retinal pigment epithelial layer below the retina, which causes vision loss through loss of photoreceptors (rods and cones) in the central part of the eye. -

A1the Eye in Detail
A. The Eye A1. Eye in detail EYE ANATOMY A guide to the many parts of the human eye and how they function. The ability to see is dependent on the actions of several structures in and around the eyeball. The graphic below lists many of the essential components of the eye's optical system. When you look at an object, light rays are reflected from the object to the cornea , which is where the miracle begins. The light rays are bent, refracted and focused by the cornea, lens , and vitreous . The lens' job is to make sure the rays come to a sharp focus on the retina . The resulting image on the retina is upside-down. Here at the retina, the light rays are converted to electrical impulses which are then transmitted through the optic nerve , to the brain, where the image is translated and perceived in an upright position! Think of the eye as a camera. A camera needs a lens and a film to produce an image. In the same way, the eyeball needs a lens (cornea, crystalline lens, vitreous) to refract, or focus the light and a film (retina) on which to focus the rays. If any one or more of these components is not functioning correctly, the result is a poor picture. The retina represents the film in our camera. It captures the image and sends it to the brain to be developed. The macula is the highly sensitive area of the retina. The macula is responsible for our critical focusing vision. It is the part of the retina most used. -

MR Imaging of Diffuse Glioma Case Report
MR Imaging of Diffuse Glioma Kiyoyuki Yanaka, 1 Takao Kamezaki, 1 Eiki Kobayashi, 1 Kiyoshi Matsueda,2 Yoshihiko Yoshii,3 and Tadao Nose3 Summary: Neuroradiologic diagnosis of "gliomatosis cerebri" is scopic examination revealed bilateral papilledema. CT of hampered by the diffuse, isodense character of the lesion, and the brain demonstrated the presence of small lateral ven the fact that it may not enhance when intravenous contrast tricles and decreased attenuation bilaterally within the white medium is administered. Clinical signs and symptoms are matter of the frontal lobes and in the left temporal lobe usually nonspecific, nonfocal, and disproportionately mild. We without postcontrast enhancement. No enlarged sulci were report a case of diffuse glioma in a 30-year-old man, discuss observed (Fig. 1). The patient underwent MR (General the difficulty in arriving at a precise diagnosis of gliomatosis Electric 1.5-Tesla Signa scanner) using T1- and T2- cerebri, and examine the possible role of MR in its detection weighted spin-echo pulse sequences. A T 1-weighted axial and delineation. scan was obtained using a repetition time (TR) of 600 msec and an echo time (TE) of 30 msec. This sequence was Index terms: Gliomatosis; Brain neoplasms, magnetic reso followed by T2-weighted scans employing a TR of 2500 nance; Magnetic resonance, contrast enhancement msec and TEs from 30 to 80 msec. Intravenous (IV) administration of gadolinium diethylenetriaminepentaacetic "Gliomatosis cerebri" is a rare condition char acid (Gd-DTPA) was carried out for enhanced MR exami acterized by diffuse overgrowth of the central nation. MR using T1-weighted images (T1 WI) revealed nervous system (CNS) by glial cells in varying enlargement of the left temporal lobe with herniation of the stages of differentiation ( 1 ).