Biology Study Guide 4
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Cranial Nerves
Cranial Nerves (1,5,7,8,9,10,11 and 12) Slides not included 9th and 10th Cranial 11th and 12th Cranial 8th Cranial Nerve 5th and 7th Cranial 1st Cranial Nerve Nerves Nerves Nerves (3,7,11,12,13,21,23,24) - (10,16) (12,23) Slides included: (14 to 17) *Slides that are not included mostly are slides of summaries or pictures. Nouf Alabdulkarim. Med 435 Olfactory Nerve [The 1st Cranial Nerve] Special Sensory Olfactory pathway 1st order neuron Receptors Axons of 1st order Neurons Olfactory receptors are specialized, ciliated nerve cells The axons of these bipolar cells 12 -20 fibers form the that lie in the olfactory epithelium. true olfactory nerve fibers. Which passes through the cribriform plate of ethmoid → They join the olfactory bulb Preliminary processing of olfactory information It is within the olfactory bulb, which contains interneurones and large Mitral cells; axons from the latter leave the bulb to form the olfactory tract. nd 2 order neuron • It is formed by the Mitral cells of olfactory bulb. • The axons of these cells form the olfactory tract. • Each tract divides into 2 roots at the anterior perforated substance: Lateral root Medial root Carries olfactory fibers to end in cortex of the Uncus & • crosses midline through anterior commissure adjacent part of Hippocampal gyrus (center of smell). and joins the uncrossed lateral root of opposite side. • It connects olfactory centers of 2 cerebral hemispheres. • So each olfactory center receives smell sensation from both halves of nasal cavity. NB. Olfactory pathway is the only sensory pathway which reaches the cerebral cortex without passing through the Thalamus . -

Cranial Nerve Palsy
Cranial Nerve Palsy What is a cranial nerve? Cranial nerves are nerves that lead directly from the brain to parts of our head, face, and trunk. There are 12 pairs of cranial nerves and some are involved in special senses (sight, smell, hearing, taste, feeling) while others control muscles and glands. Which cranial nerves pertain to the eyes? The second cranial nerve is called the optic nerve. It sends visual information from the eye to the brain. The third cranial nerve is called the oculomotor nerve. It is involved with eye movement, eyelid movement, and the function of the pupil and lens inside the eye. The fourth cranial nerve is called the trochlear nerve and the sixth cranial nerve is called the abducens nerve. They each innervate an eye muscle involved in eye movement. The fifth cranial nerve is called the trigeminal nerve. It provides facial touch sensation (including sensation on the eye). What is a cranial nerve palsy? A palsy is a lack of function of a nerve. A cranial nerve palsy may cause a complete or partial weakness or paralysis of the areas served by the affected nerve. In the case of a cranial nerve that has multiple functions (such as the oculomotor nerve), it is possible for a palsy to affect all of the various functions or only some of the functions of that nerve. What are some causes of a cranial nerve palsy? A cranial nerve palsy can occur due to a variety of causes. It can be congenital (present at birth), traumatic, or due to blood vessel disease (hypertension, diabetes, strokes, aneurysms, etc). -
Electromagnetic Field and TGF-Β Enhance the Compensatory
www.nature.com/scientificreports OPEN Electromagnetic feld and TGF‑β enhance the compensatory plasticity after sensory nerve injury in cockroach Periplaneta americana Milena Jankowska1, Angelika Klimek1, Chiara Valsecchi2, Maria Stankiewicz1, Joanna Wyszkowska1* & Justyna Rogalska1 Recovery of function after sensory nerves injury involves compensatory plasticity, which can be observed in invertebrates. The aim of the study was the evaluation of compensatory plasticity in the cockroach (Periplaneta americana) nervous system after the sensory nerve injury and assessment of the efect of electromagnetic feld exposure (EMF, 50 Hz, 7 mT) and TGF‑β on this process. The bioelectrical activities of nerves (pre‑and post‑synaptic parts of the sensory path) were recorded under wind stimulation of the cerci before and after right cercus ablation and in insects exposed to EMF and treated with TGF‑β. Ablation of the right cercus caused an increase of activity of the left presynaptic part of the sensory path. Exposure to EMF and TGF‑β induced an increase of activity in both parts of the sensory path. This suggests strengthening efects of EMF and TGF‑β on the insect ability to recognize stimuli after one cercus ablation. Data from locomotor tests proved electrophysiological results. The takeover of the function of one cercus by the second one proves the existence of compensatory plasticity in the cockroach escape system, which makes it a good model for studying compensatory plasticity. We recommend further research on EMF as a useful factor in neurorehabilitation. Injuries in the nervous system caused by acute trauma, neurodegenerative diseases or even old age are hard to reverse and represent an enormous challenge for modern medicine. -

Congenital Oculomotor Palsy: Associated Neurological and Ophthalmological Findings
CONGENITAL OCULOMOTOR PALSY: ASSOCIATED NEUROLOGICAL AND OPHTHALMOLOGICAL FINDINGS M. D. TSALOUMAS1 and H. E. WILLSHA W2 Birmingham SUMMARY In our group of patients we found a high incidence Congenital fourth and sixth nerve palsies are rarely of neurological abnormalities, in some cases asso associated with other evidence of neurological ahnor ciated with abnormal findings on CT scanning. mality, but there have been conflicting reports in the Aberrant regeneration, preferential fixation with literature on the associations of congenital third nerve the paretic eye, amblyopia of the non-involved eye palsy. In order to clarify the situation we report a series and asymmetric nystagmus have all been reported as 1 3 7 of 14 consecutive cases presenting to a paediatric associated ophthalmic findings. - , -9 However, we tertiary referral service over the last 12 years. In this describe for the first time a phenomenon of digital lid series of children, 5 had associated neurological elevation to allow fixation with the affected eye. Two abnormalities, lending support to the view that con children demonstrated this phenomenon and in each genital third nerve palsy is commonly a manifestation of case the accompanying neurological defect was widespread neurological damage. We also describe for profound. the first time a phenomenon of digital lid elevation to allow fixation with the affected eye. Two children demonstrated this phenomenon and in each case the PATIENTS AND METHODS accompanying neurological defect was profound. The Fourteen children (8 boys, 6 girls) with a diagnosis of frequency and severity of associated deficits is analysed, congenital oculomotor palsy presented to our paed and the mechanism of fixation with the affected eye is iatric tertiary referral centre over the 12 years from discussed. -

Cranial Nerves 1, 5, 7-12
Cranial Nerve I Olfactory Nerve Nerve fiber modality: Special sensory afferent Cranial Nerves 1, 5, 7-12 Function: Olfaction Remarkable features: – Peripheral processes act as sensory receptors (the other special sensory nerves have separate Warren L Felton III, MD receptors) Professor and Associate Chair of Clinical – Primary afferent neurons undergo continuous Activities, Department of Neurology replacement throughout life Associate Professor of Ophthalmology – Primary afferent neurons synapse with secondary neurons in the olfactory bulb without synapsing Chair, Division of Neuro-Ophthalmology first in the thalamus (as do all other sensory VCU School of Medicine neurons) – Pathways to cortical areas are entirely ipsilateral 1 2 Crania Nerve I Cranial Nerve I Clinical Testing Pathology Anosmia, hyposmia: loss of or impaired Frequently overlooked in neurologic olfaction examination – 1% of population, 50% of population >60 years Aromatic stimulus placed under each – Note: patients with bilateral anosmia often report nostril with the other nostril occluded, eg impaired taste (ageusia, hypogeusia), though coffee, cloves, or soap taste is normal when tested Note that noxious stimuli such as Dysosmia: disordered olfaction ammonia are not used due to concomitant – Parosmia: distorted olfaction stimulation of CN V – Olfactory hallucination: presence of perceived odor in the absence of odor Quantitative clinical tests are available: • Aura preceding complex partial seizures of eg, University of Pennsylvania Smell temporal lobe origin -
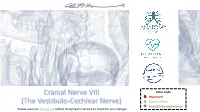
Cranial Nerve VIII
Cranial Nerve VIII Color Code Important (The Vestibulo-Cochlear Nerve) Doctors Notes Notes/Extra explanation Please view our Editing File before studying this lecture to check for any changes. Objectives At the end of the lecture, the students should be able to: ✓ List the nuclei related to vestibular and cochlear nerves in the brain stem. ✓ Describe the type and site of each nucleus. ✓ Describe the vestibular pathways and its main connections. ✓ Describe the auditory pathway and its main connections. Due to the difference of arrangement of the lecture between the girls and boys slides we will stick to the girls slides then summarize the pathway according to the boys slides. Ponto-medullary Sulcus (cerebello- pontine angle) Recall: both cranial nerves 8 and 7 emerge from the ventral surface of the brainstem at the ponto- medullary sulcus (cerebello-pontine angle) Brain – Ventral Surface Vestibulo-Cochlear (VIII) 8th Cranial Nerve o Type: Special sensory (SSA) o Conveys impulses from inner ear to nervous system. o Components: • Vestibular part: conveys impulses associated with body posture ,balance and coordination of head & eye movements. • Cochlear part: conveys impulses associated with hearing. o Vestibular & cochlear parts leave the ventral surface* of brain stem through the pontomedullary sulcus ‘at cerebellopontine angle*’ (lateral to facial nerve), run laterally in posterior cranial fossa and enter the internal acoustic meatus along with 7th (facial) nerve. *see the previous slide Auditory Pathway Only on the girls’ slides 04:14 Characteristics: o It is a multisynaptic pathway o There are several locations between medulla and the thalamus where axons may synapse and not all the fibers behave in the same manner. -

A Rare Case of Collett–Sicard Syndrome After Blunt Head Trauma
Case Report Dysphagia and Tongue Deviation: A Rare Case of Collett–Sicard Syndrome after Blunt Head Trauma Eric Tamrazian 1,2 and Bijal Mehta 1,2,* 1 Department of Neurology, David Geffen School of Medicine, Harbor-UCLA Medical Center, Torrance, CA 90502, USA; [email protected] 2 Los Angeles Biomedical Institute, Los Angeles, CA 90095, USA * Correspondence: [email protected] Received: 28 October 2019; Accepted: 14 November 2019; Published: 21 December 2020 Abstract: The jugular foramen and the hypoglossal canal are both apertures located at the base of the skull. Multiple lower cranial nerve palsies tend to occur with injuries to these structures. The pattern of injuries tend to correlate with the combination of nerves damaged. Case Report: A 28-year-old male was involved in an AVP injury while crossing the highway. Exam showed a GCS of 15 AAOx3, with dysphagia, tongue deviation to the right, uvula deviation to the left and a depressed palate. Initial imaging showed B/L frontal traumatic Sub-Arachnoid Hemorrhages (tSAH), Left Frontal Epidural Hematoma and a Basilar Skull Fracture. On second look by a trained Neuroradiologist c At 3 month follow up, patient’s tongue normalized to midline and his dysphagia resolved. Discussion: Collette-Sicard syndrome is a rare condition/syndrome characterized by unilateral palsy of CN: IX, X, XII. This condition has been rarely described as a consequence of blunt head trauma. In most cases, the condition is self-limiting with patients regaining most to all of their neurological functions within 6 months. Nerve traction injuries and soft tissue edema compressing the cranial nerves are the leading two hypothesis. -

The Brain and Cranial Nerves
14 The Brain and Cranial Nerves PowerPoint® Lecture Presentations prepared by Jason LaPres Lone Star College—North Harris © 2012 Pearson Education, Inc. An Introduction to the Brain and Cranial Nerves • Learning Outcomes • 14-1 Name the major brain regions, vesicles, and ventricles, and describe the locations and functions of each. • 14-2 Explain how the brain is protected and supported, and discuss the formation, circulation, and function of cerebrospinal fluid. • 14-3 Describe the anatomical differences between the medulla oblongata and the spinal cord, and identify the main components and functions of the medulla oblongata. © 2012 Pearson Education, Inc. An Introduction to the Brain and Cranial Nerves • Learning Outcomes • 14-4 List the main components of the pons, and specify the functions of each. • 14-5 List the main components of the cerebellum, and specify the functions of each. • 14-6 List the main components of the midbrain, and specify the functions of each. • 14-7 List the main components of the diencephalon, and specify the functions of each. © 2012 Pearson Education, Inc. An Introduction to the Brain and Cranial Nerves • Learning Outcomes • 14-8 Identify the main components of the limbic system, and specify the locations and functions of each. • 14-9 Identify the major anatomical subdivisions and functions of the cerebrum, and discuss the origin and significance of the major types of brain waves seen in an electroencephalogram. • 14-10 Describe representative examples of cranial reflexes that produce somatic responses or visceral responses to specific stimuli. © 2012 Pearson Education, Inc. • In the pre-synaptic neuron, an Synapse electrical signal comes in, opens up to voltage-gated channels, and signals the vesicles containing neurotransmitters (chemical signal) to be released into the synaptic cleft. -

Anatomy of the Extraneural Blood Supply to the Intracranial
British Journal of Ophthalmology 1996; 80: 177-181 177 the extraneural blood to the Anatomy of supply Br J Ophthalmol: first published as 10.1136/bjo.80.2.177 on 1 February 1996. Downloaded from intracranial oculomotor nerve Mark Cahill, John Bannigan, Peter Eustace Abstract have since been classified as extraneural vessels Aims-An anatomical study was under- as they arise from outside the nerve and ramify taken to determine the extraneural blood on the surface ofthe nerve. In 1965, Parkinson supply to the intracranial oculomotor attempted to demonstrate and name the nerve. branches of the intracavernous internal carotid Methods-Human tissue blocks contain- artery.3 One of these branches, the newly titled ing brainstem, cranial nerves II-VI, body meningohypophyseal trunk was seen to pro- of sphenoid, and associated cavernous vide a nutrient arteriole to the oculomotor sinuses were obtained, injected with con- nerve in the majority of dissections. The infe- trast material, and dissected using a rior hypophyseal artery was also seen to arise stereoscopic microscope. from the meningohypophyseal trunk. Seven Results-Eleven oculomotor nerves were years earlier McConnell had demonstrated dissected, the intracranial part being that this vessel provided a large portion of the divided into proximal, middle, and distal pituitary blood supply.4 (intracavernous) parts. The proximal part Asbury and colleagues provided further of the intracranial oculomotor nerve anatomical detail in 1970.5 They set out to received extraneural nutrient arterioles explain the clinical findings of diabetic oph- from thalamoperforating arteries in all thalmoplegia on a pathological basis. Using a specimens and in six nerves this blood serial section technique, they demonstrated an supply was supplemented by branches intraneural network of small arterioles within from other brainstem vessels. -

Cranial Nerve Disorders: Clinical Manifestations and Topographyଝ
Radiología. 2019;61(2):99---123 www.elsevier.es/rx UPDATE IN RADIOLOGY Cranial nerve disorders: Clinical manifestations and topographyଝ a,∗ a b c M. Jorquera Moya , S. Merino Menéndez , J. Porta Etessam , J. Escribano Vera , a M. Yus Fuertes a Sección de Neurorradiología, Hospital Clínico San Carlos, Madrid, Spain b Servicio de Neurología, Hospital Clínico San Carlos, Madrid, Spain c Neurorradiología, Hospital Ruber Internacional, Madrid, Spain Received 17 November 2017; accepted 27 September 2018 KEYWORDS Abstract The detection of pathological conditions related to the twelve cranial pairs rep- Cranial pairs; resents a significant challenge for both clinicians and radiologists; imaging techniques are Cranial nerves; fundamental for the management of many patients with these conditions. In addition to knowl- Cranial neuropathies; edge about the anatomy and pathological entities that can potentially affect the cranial pairs, Neuralgia; the imaging evaluation of patients with possible cranial pair disorders requires specific exami- Cranial nerve palsy nation protocols, acquisition techniques, and image processing. This article provides a review of the most common symptoms and syndromes related with the cranial pairs that might require imaging tests, together with a brief overview of the anatomy, the most common underlying processes, and the most appropriate imaging tests for different indications. © 2018 SERAM. Published by Elsevier Espana,˜ S.L.U. All rights reserved. PALABRAS CLAVE Sintomatología derivada de los pares craneales: Clínica y topografía Pares craneales; Resumen La detección de la patología relacionada con los doce pares craneales representa Nervios craneales; un importante desafío, tanto para los clínicos como para los radiólogos. Las técnicas de imagen Neuropatía de pares craneales; son fundamentales para el manejo de muchos de los pacientes. -

Hypoglossal-Facial Nerve Side-To-End Anastomosis for Preservation of Hypoglossal Function: Results of Delayed Treatment With
Hypoglossalfacial nerve side-to-end anastomosis for preservation of hypoglossal function: results of delayed treatment with a new technique Yutaka Sawamura, M.D., and Hiroshi Abe, M.D. Department of Neurosurgery, University of Hokkaido, School of Medicine, Sapporo, Japan This report describes a new surgical technique to improve the results of conventional hypoglossalfacial nerve anastomosis that does not necessitate the use of nerve grafts or hemihypoglossal nerve splitting. Using this technique, the mastoid process is partially resected to open the stylomastoid foramen and the descending portion of the facial nerve in the mastoid cavity is exposed by drilling to the level of the external genu and then sectioning its most proximal portion. The hypoglossal nerve beneath the internal jugular vein is exposed at the level of the axis and dissected as proximally as possible. One-half of the hypoglossal nerve is transected: use of less than one-half of the hypoglossal nerve is adequate for approximation to the distal stump of the atrophic facial nerve. The nerve endings, the proximally cut end of the hypoglossal nerve, and the distal stump of the facial nerve are approximated and anastomosed without tension. This technique was used in four patients with long-standing facial paralysis (greater than 24 months), and it provided satisfactory facial reanimation, with no evidence of hemitongue atrophy or dysfunction. Because it completely preserves glossal function, the hemihypoglossalfacial nerve anastomosis described here constitutes a successful -

Peripheral Nerve Regeneration and Muscle Reinnervation
International Journal of Molecular Sciences Review Peripheral Nerve Regeneration and Muscle Reinnervation Tessa Gordon Department of Surgery, University of Toronto, Division of Plastic Reconstructive Surgery, 06.9706 Peter Gilgan Centre for Research and Learning, The Hospital for Sick Children, Toronto, ON M5G 1X8, Canada; [email protected]; Tel.: +1-(416)-813-7654 (ext. 328443) or +1-647-678-1314; Fax: +1-(416)-813-6637 Received: 19 October 2020; Accepted: 10 November 2020; Published: 17 November 2020 Abstract: Injured peripheral nerves but not central nerves have the capacity to regenerate and reinnervate their target organs. After the two most severe peripheral nerve injuries of six types, crush and transection injuries, nerve fibers distal to the injury site undergo Wallerian degeneration. The denervated Schwann cells (SCs) proliferate, elongate and line the endoneurial tubes to guide and support regenerating axons. The axons emerge from the stump of the viable nerve attached to the neuronal soma. The SCs downregulate myelin-associated genes and concurrently, upregulate growth-associated genes that include neurotrophic factors as do the injured neurons. However, the gene expression is transient and progressively fails to support axon regeneration within the SC-containing endoneurial tubes. Moreover, despite some preference of regenerating motor and sensory axons to “find” their appropriate pathways, the axons fail to enter their original endoneurial tubes and to reinnervate original target organs, obstacles to functional recovery that confront nerve surgeons. Several surgical manipulations in clinical use, including nerve and tendon transfers, the potential for brief low-frequency electrical stimulation proximal to nerve repair, and local FK506 application to accelerate axon outgrowth, are encouraging as is the continuing research to elucidate the molecular basis of nerve regeneration.