What Is Scintimammography?
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

BREAST IMAGING for SCREENING and DIAGNOSING CANCER Policy Number: DIAGNOSTIC 105.9 T2 Effective Date: January 1, 2017
Oxford UnitedHealthcare® Oxford Clinical Policy BREAST IMAGING FOR SCREENING AND DIAGNOSING CANCER Policy Number: DIAGNOSTIC 105.9 T2 Effective Date: January 1, 2017 Table of Contents Page Related Policies INSTRUCTIONS FOR USE .......................................... 1 Omnibus Codes CONDITIONS OF COVERAGE ...................................... 1 Preventive Care Services BENEFIT CONSIDERATIONS ...................................... 2 Radiology Procedures Requiring Precertification for COVERAGE RATIONALE ............................................. 3 eviCore Healthcare Arrangement APPLICABLE CODES ................................................. 5 DESCRIPTION OF SERVICES ...................................... 6 CLINICAL EVIDENCE ................................................. 7 U.S. FOOD AND DRUG ADMINISTRATION ................... 16 REFERENCES .......................................................... 18 POLICY HISTORY/REVISION INFORMATION ................ 22 INSTRUCTIONS FOR USE This Clinical Policy provides assistance in interpreting Oxford benefit plans. Unless otherwise stated, Oxford policies do not apply to Medicare Advantage members. Oxford reserves the right, in its sole discretion, to modify its policies as necessary. This Clinical Policy is provided for informational purposes. It does not constitute medical advice. The term Oxford includes Oxford Health Plans, LLC and all of its subsidiaries as appropriate for these policies. When deciding coverage, the member specific benefit plan document must be referenced. The terms -

Breast Scintimammography
CLINICAL MEDICAL POLICY Policy Name: Breast Scintimammography Policy Number: MP-105-MD-PA Responsible Department(s): Medical Management Provider Notice Date: 11/23/2020 Issue Date: 11/23/2020 Effective Date: 12/21/2020 Next Annual Review: 10/2021 Revision Date: 09/16/2020 Products: Gateway Health℠ Medicaid Application: All participating hospitals and providers Page Number(s): 1 of 5 DISCLAIMER Gateway Health℠ (Gateway) medical policy is intended to serve only as a general reference resource regarding coverage for the services described. This policy does not constitute medical advice and is not intended to govern or otherwise influence medical decisions. POLICY STATEMENT Gateway Health℠ does not provide coverage in the Company’s Medicaid products for breast scintimammography. The service is considered experimental and investigational in all applications, including but not limited to use as an adjunct to mammography or in staging the axillary lymph nodes. This policy is designed to address medical necessity guidelines that are appropriate for the majority of individuals with a particular disease, illness or condition. Each person’s unique clinical circumstances warrant individual consideration, based upon review of applicable medical records. (Current applicable Pennsylvania HealthChoices Agreement Section V. Program Requirements, B. Prior Authorization of Services, 1. General Prior Authorization Requirements.) Policy No. MP-105-MD-PA Page 1 of 5 DEFINITIONS Prior Authorization Review Panel – A panel of representatives from within the Pennsylvania Department of Human Services who have been assigned organizational responsibility for the review, approval and denial of all PH-MCO Prior Authorization policies and procedures. Scintimammography A noninvasive supplemental diagnostic testing technology that requires the use of radiopharmaceuticals in order to detect tissues within the breast that accumulate higher levels of radioactive tracer that emit gamma radiation. -

Breast Imaging H
BREAST IMAGING H. Lee Moffitt Cancer Center and Research Institute Rotation Director: Margaret Szabunio, M.D. General Goals : On this rotation, the resident will learn to interpret screening mammograms and to perform diagnostic mammography and ultrasound examinations of the breast. The resident will learn to formulate appropriate differential diagnoses and recommendations for various breast pathologies. The resident will also learn mammographic, ultrasound and MR breast biopsy techniques. Daily Work : The resident rotation begins after morning conference has concluded. In this rotation the resident shall learn BIRADS nomenclature and become proficient in using the PENRAD system for reporting. The resident will also learn the difference between screening and diagnostic mammography and how to perform a diagnostic work-up. (S)he will become familiarized with mammographic positioning and technique and quality assurance including MQSA and ACR requirements. The resident will learn to interpret mammographic images and the use of additional mammographic views for problem solving. (S)he will learn when and how to employ sonography in patient evaluation. The resident is REQUIRED to attend Thursday morning breast interdisciplinary conference. Preparing and reviewing cases for this conference is highly recommended. The resident will assist with and perform needle localizations, breast biopsy and cyst aspiration procedures using mammographic, stereotactic and sonographic techniques for each. The resident is expected to identify proper indications and contraindications for each procedure and how to identify and manage complications. The resident is expected to understand and complete informed consent for image guided breast procedures. On occasion, the resident may observe or assist with ductography procedures. Opportunity to observe and assist with MR guided breast procedures may also be available. -

Procedure Guideline for Breast Scintigraphy
Procedure Guideline for Breast Scintigraphy Iraj Khalkhali, Linda E. Diggles, Raymond Taillefer, Penny R. Vandestreek, Patrick J. Peller and Hani H. Abdel-Nabi Harbor-UCLA Medical Center, Terranee; Nuclear Imaging Consultants, Roseville, California; Hospital Hôtel-Dieu de Montreal, Montreal, Quebec, Canada; Lutheran General Hospital, Park Ridge, Illinois; and University of Buffalo, Buffalo, New York Key Words: breast scintigraphy;procedureguideline should be available, as well as sonograms, if J NucÃMed 1999; 40:1233-1235 obtained. 2. A breast physical examination must be performed by either the nuclear medicine physician or the PART I: PURPOSE referring physician. 3. The time of last menses and pregnancy and lactat- The purpose of this guideline is to assist nuclear medicine ing status of the patient should be determined. practitioners in recommending, performing, interpreting and reporting the results of 99mTc-sestamibi breast scintigraphy 4. Breast scintigraphy should be delayed at least 2 wk after cyst or fine-needle aspiration, and 4—6wk (mammoscintigraphy, scintimammography). after core or excisional biopsy. 5. The nuclear medicine physician should be aware of PART II: BACKGROUND INFORMATION AND DEFINITIONS physical signs and symptoms and prior surgical procedures or therapy. Breast scintigraphy is performed after intravenous admin istration of "mTc-sestamibi and includes planar and/or C. Precautions None SPECT. D. Radiopharmaceutical 1. Intravenous injection of 740-1110 MBq (20-30 PART III: COMMON INDICATIONS AND APPLICATIONS mCi) 99mTc-sestamibi should be administered in an A. Evaluate breast cancer in patients in whom mammog- arm vein contralateral to the breast with the sus raphy is not diagnostic or is difficult to interpret (e.g., pected abnormality. -

A Molecular Approach to Breast Imaging
Journal of Nuclear Medicine, published on January 16, 2014 as doi:10.2967/jnumed.113.126102 FOCUS ON MOLECULAR IMAGING A Molecular Approach to Breast Imaging Amy M. Fowler Department of Radiology, University of Wisconsin–Madison, Madison, Wisconsin malignant cells. A recent meta-analysis of the accuracy of 99mTc-sestamibi scintimammography as an adjunct to di- Molecular imaging is a multimodality discipline for noninvasively agnostic mammography for detection of breast cancer dem- visualizing biologic processes at the subcellular level. Clinical applications of radionuclide-based molecular imaging for breast onstrated a sensitivity of 83% and specificity of 85% (2). cancer continue to evolve. Whole-body imaging, with scinti- However, sensitivity was less for nonpalpable (59%) versus mammography and PET, and newer dedicated breast imaging palpable lesions (87%) despite comparable specificity, with systems are reviewed. The potential clinical indications and the no significant difference between planar and SPECT meth- challenges of implementing these emerging technologies are ods. Decreased sensitivity for nonpalpable, presumably presented. smaller, lesions is in part due to the limited spatial resolu- Key Words: molecular imaging; oncology; breast; PET; PET/ tion of conventional g cameras. CT; radiopharmaceuticals; breast cancer; breast-specific g im- In addition to 99mTc-sestamibi, the positron-emitting ra- aging; positron-emission mammography; positron-emission to- diopharmaceutical 18F-FDG accumulates in many types of mography cancer including breast. Meta-analyses of the accuracy of J Nucl Med 2014; 55:1–4 whole-body 18F-FDG PET used after standard diagnostic DOI: 10.2967/jnumed.113.126102 workup for patients with suspected breast lesions demon- strated sensitivities of 83%–89% and specificities of 74%– 80% (3,4). -

Breast MRI: New and Abbreviated Protocols
Breast MRI: New and Abbreviated Protocols Christopher Comstock M.D. Department of Radiology Memorial Sloan-Kettering Cancer Center Topics • What is our goal? • Current status of screening • How do we change screening • Abbreviated Breast MRI (AB-MR) • EA1141 AB-MR Trial • Multiparametric Breast MRI Beyond the scope of this talk! • The debate over screening the benefit of mammography, particularly for women in their forties. What is Our Goal? • Decrease breast cancer mortality • Reduction in the morbidities associated with surgery and chemotherapy • Finding breast cancers at a smaller size and earlier stage leads to a reduction in mortality and the use of less aggressive therapies Reservoir of Breast Cancer Present in 1000 Women Being Screened • Is it 30, 40, 50, 60 or more breast cancers per 1000 women? • Depends on risk of population • Detection level (size and stage) depends on modality and frequency of screening Reservoir of Breast Cancer Present in 1000 Women Being Screened Tomo plus WBUS The Dissemination of Medical Technologies into Clinical Practice • Innovations medical in technology and quality of information are the sole driving force in the acceptance and adoption of new technologies • The dissemination of medical technologies depends on the social, political and ideological context into which they are introduced Much Can Be Learned From the History of Mammography • Despite improvements in technology, mammography languished from 1930s to 1970 – 1930-1950 Stafford L. Warren, Jacob Gershon-Cohen and Raul Leborgne – 1950s Improved techniques, Robert Egan • The production of better data alone did not eliminate the role that economics, authority and ideology played “TO SEE TODAY WITH THE EYES OF TOMORROW” A HISTORY OF SCREENING MAMMOGRAPHY. -

Breast Elastography – Ultrasound Or Magnetic Resonance
Medical Policy Joint Medical Policies are a source for BCBSM and BCN medical policy information only. These documents are not to be used to determine benefits or reimbursement. Please reference the appropriate certificate or contract for benefit information. This policy may be updated and is therefore subject to change. *Current Policy Effective Date: 7/1/21 (See policy history boxes for previous effective dates) Title: Breast Elastography – Ultrasound or Magnetic Resonance Description/Background In the United States, about 1 in 8 women will develop invasive breast cancer over the course of her lifetime. In 2020, is it estimated that there will be over 280,000 new cases of invasive breast cancer diagnosed in women and over 2,600 new cases of invasive breast cancer in men.1 Breast cancer is the most common cancer in women worldwide.2 Mammography remains the generally accepted standard diagnostic test for breast cancer screening and diagnosis. The incidence of breast cancer has led to research on new diagnostic imaging techniques for early diagnosis. Elasticity is the property of a substance to be deformed in response to an external force and to resume its original size and shape when the force is removed. In evaluation of superficial tissue such as skin, breast or prostate, manual palpation can distinguish normal tissue from stiffer tissue. Elastography is a noninvasive technique that evaluates the elastic properties, or stiffness of tissues, and its application for diagnosing breast cancer is based on the principle that malignant tissue is less elastic than normal, healthy breast tissue. Elastography has been investigated as an additive technique to increase the specificity of ultrasound and magnetic resonance imaging. -

Evaluation of Nipple Discharge
New 2016 American College of Radiology ACR Appropriateness Criteria® Evaluation of Nipple Discharge Variant 1: Physiologic nipple discharge. Female of any age. Initial imaging examination. Radiologic Procedure Rating Comments RRL* Mammography diagnostic 1 See references [2,4-7]. ☢☢ Digital breast tomosynthesis diagnostic 1 See references [2,4-7]. ☢☢ US breast 1 See references [2,4-7]. O MRI breast without and with IV contrast 1 See references [2,4-7]. O MRI breast without IV contrast 1 See references [2,4-7]. O FDG-PEM 1 See references [2,4-7]. ☢☢☢☢ Sestamibi MBI 1 See references [2,4-7]. ☢☢☢ Ductography 1 See references [2,4-7]. ☢☢ Image-guided core biopsy breast 1 See references [2,4-7]. Varies Image-guided fine needle aspiration breast 1 Varies *Relative Rating Scale: 1,2,3 Usually not appropriate; 4,5,6 May be appropriate; 7,8,9 Usually appropriate Radiation Level Variant 2: Pathologic nipple discharge. Male or female 40 years of age or older. Initial imaging examination. Radiologic Procedure Rating Comments RRL* See references [3,6,8,10,13,14,16,25- Mammography diagnostic 9 29,32,34,42-44,71-73]. ☢☢ See references [3,6,8,10,13,14,16,25- Digital breast tomosynthesis diagnostic 9 29,32,34,42-44,71-73]. ☢☢ US is usually complementary to mammography. It can be an alternative to mammography if the patient had a recent US breast 9 mammogram or is pregnant. See O references [3,5,10,12,13,16,25,30,31,45- 49]. MRI breast without and with IV contrast 1 See references [3,8,23,24,35,46,51-55]. -

Screening Automated Whole Breast Ultrasound
Screening Automated Whole Breast Ultrasound Screening Automated Whole Breast Ultrasound Stanford now offers screening automated whole breast ultrasound (SAWBU) at our Stanford Medicine Cancer Center Palo Alto location. This is an optional test that can be used as a supplement to screening mammography in women with mammographically dense breasts. It can find cancers that cannot be seen on mammograms due to overlap with dense breast tissue. Stanford uses automated whole breast technique, a new method developed for accuracy and efficiency. Who is a candidate for SAWBU What will happen during the How is SAWBU exam is examination? SAWBU examination? different? This is an optional test to supplement You will lie on your back, and gel will Screening automated screening mammography in women be applied to your breast. whole breast ultrasound who: uses sound waves (no radi- A large ultrasound handpiece will be • Undergo routine screening with ation) to create 3D pictures placed on the breast, and the system mammography. of the breast tissue, using will automatically take a “sweep” • Have no current signs or a new automated method that obtains ultrasound images of symptoms of breast cancer. developed for accuracy and the tissue from top to bottom. The • Have mammographically dense efficiency. handpiece will be repositioned to take (heterogeneously or extremely other “sweeps” to include all of the It can find cancers that dense) breasts. breast tissue. cannot be seen on mam- • Are not at “high risk" undergoing mograms alone due to supplemental screening with An exam of both breasts takes less overlap with dense breast breast MRI. Screening ultra- than 20 minutes to obtain. -

Evaluation of the Quantitative Accuracy of a Commercially-Available Positron Emission Mammography Scanner
The Texas Medical Center Library DigitalCommons@TMC The University of Texas MD Anderson Cancer Center UTHealth Graduate School of The University of Texas MD Anderson Cancer Biomedical Sciences Dissertations and Theses Center UTHealth Graduate School of (Open Access) Biomedical Sciences 8-2010 EVALUATION OF THE QUANTITATIVE ACCURACY OF A COMMERCIALLY-AVAILABLE POSITRON EMISSION MAMMOGRAPHY SCANNER Adam Springer Follow this and additional works at: https://digitalcommons.library.tmc.edu/utgsbs_dissertations Part of the Diagnosis Commons, Equipment and Supplies Commons, and the Other Medical Sciences Commons Recommended Citation Springer, Adam, "EVALUATION OF THE QUANTITATIVE ACCURACY OF A COMMERCIALLY-AVAILABLE POSITRON EMISSION MAMMOGRAPHY SCANNER" (2010). The University of Texas MD Anderson Cancer Center UTHealth Graduate School of Biomedical Sciences Dissertations and Theses (Open Access). 64. https://digitalcommons.library.tmc.edu/utgsbs_dissertations/64 This Thesis (MS) is brought to you for free and open access by the The University of Texas MD Anderson Cancer Center UTHealth Graduate School of Biomedical Sciences at DigitalCommons@TMC. It has been accepted for inclusion in The University of Texas MD Anderson Cancer Center UTHealth Graduate School of Biomedical Sciences Dissertations and Theses (Open Access) by an authorized administrator of DigitalCommons@TMC. For more information, please contact [email protected]. EVALUATION OF THE QUANTITATIVE ACCURACY OF A COMMERCIALLY- AVAILABLE POSITRON EMISSION MAMMOGRAPHY SCANNER -
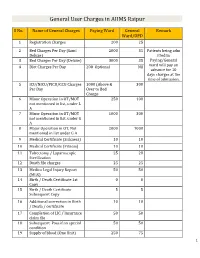
General User Charges in AIIMS Raipur
General User Charges in AIIMS Raipur S No. Name of General Charges Paying Ward General Remark Ward/OPD 1 Registration Charges 200 25 2 Bed Charges Per Day (Sami 2000 35 Patients being adm Deluxe) itted in 3 Bed Charges Per Day (Deluxe) 3000 35 Paying/General 4 Diet Charges Per Day 200 Optional Nil ward will pay an advance for 10 days charges at the time of admission. 5 ICU/NICU/PICU/CCU Charges 1000 (Above & 300 Per Day Over to Bed Charge 6 Minor Operation in OT/MOT 250 100 not mentioned in list, under L A 7 Minor Operation in OT/MOT 1000 300 not mentioned in list, under G A 8 Major Operation in OT, Not 2000 1000 mentioned in list under G A 9 Medical Certificate (Sickness) 10 10 10 Medical Certificate (Fitness) 10 10 11 Tubectomy / Laparoscopic 25 20 Sterilization 12 Death file charges 25 25 13 Medico Legal Injury Report 50 50 (MLR) 14 Birth / Death Certificate 1st 0 0 Copy 15 Birth / Death Certificate 5 5 Subsequent Copy 16 Additional correction in Birth 10 10 / Death / certificate 17 Completion of LIC / Insurance 50 50 claim file 18 Subsequent Pass if on special 50 50 condition 19 Supply of blood (One Unit) 250 75 1 20 Medical Board Certificate 500 500 On Special Case User Charges for Investigations in AIIMS Raipur S No. Name of Investigations Paying General Remark Ward Ward/OPD Anaesthsia 1 ABG 75 50 2 ABG ALONGWITH 150 100 ELECTROLYTES(NA+,K+)(Na,K) 3 ONLY ELECTROLYTES(Na+,K+,Cl,Ca+) 75 50 4 ONLY CALCIUM 50 25 5 GLUCOSE 25 20 6 LACTATE 25 20 7 UREA. -

Shear Wave Elastography As an Early Indicator of Breast Cancer in A
ISSN: 2378-3656 Altunkeser and Arslan. Clin Med Rev Case Rep 2019, 6:259 DOI: 10.23937/2378-3656/1410259 Volume 6 | Issue 3 Clinical Medical Reviews Open Access and Case Reports CAse RepoRt Shear Wave Elastography as an Early Indicator of Breast Cancer in a Breastfeeding Patient: A Case Report and Literature Review Ayşegül Altunkeser and Fatma Zeynep Arslan* Check for Department of Radiology, Konya Training and Research Hospital, University of Health Science, Turkey updates *Corresponding author: Fatma Zeynep Arslan, MD, Konya Training and Research Hospital, University of Health Science, Hacı Şaban Mah, Meram Yeni Yol Caddesi, No: 97, PC: 42090, Meram, Konya, Turkey, Tel: 0506-438-24-30, Fax: 0-332- 323-67-23 our hospital complaining from pain in the right breast. Abstract In the young patient with no history of cancer in the Shear wave elastography (SWE) is a relatively new and family; The patient was breasfeeding and labaratuary highly effective method to reveal mechanical features of tissue by demonstrating quantitative elasticity value. The findings were normal. On physical examination, a hard morphological features including margin of the lesion, ori- mass was palpated in her right breast. A hypoechoic entation, shape and border are considered in differentiation mass lesions was sonographically detected on the right of breast lesions on USG. It is a known fact that malignant breast in a diameter with 31 × 24 mm (Figure 1). SWE lesions are usually palpated as a hard mass in the physi- cal examination. A qualitative broad information can obtain was performed to obtain additional information about about the tissue elasticity by integrating SWE examination mass lesion.