Name: Ayorinde Oluwadamilola Wengitari
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

The Role of Intravenous Urography with Erect Film and Retrograde
Central Journal of Urology and Research Bringing Excellence in Open Access Research Article *Corresponding author Ahmed N. Ghanem, Department of Urology, Consultant Urologist Surgeon, No1 President Mubarak The Role of Intravenous Street, Mansoura 35511, Egypt, Tel: 001020883243; Email: Submitted: 05 November 2018 Urography with Erect Film and Accepted: 22 November 2018 Published: 26 November 2018 Retrograde Pyelography in ISSN: 2379-951X Copyright © 2018 Ghanem et al. Revealing Patho-Etiology of OPEN ACCESS Keywords the Loin Pain and Haematuria • Intravenous urography • Retrograde pyelography • Loin pain haematuria syndrome Syndrome by Discovering • Nephroptosis its Overlooked Link with Symptomatic Nephroptosis Khalid A Ghanem1, Salma A. Ghanem2, Nisha Pindoria3, and Ahmed N. Ghanem1* 1Department of Urology, Mansoura University Hospital, Egypt 2Department of Urology, Barts & The Royal London NHS Trust Royal London Hospital, Egypt 3Department of Urology, North Middlesex University Hospital, Egypt Abstract Introduction and objectives: To report the role of intravenous urography with erect film (IVU-E) and retrograde pyelography (RGP) in resolving the puzzle of Loin Pain and Haematuria Syndrome (LPHS) by revealing its patho-etiological overlooked link with Symptomatic Nephroptosis (SN). We demonstrate that renal pedicle stretch causes neuro-ischaemia as evidenced by the new IVU 7 sign and the damaged renal medullary papilla shown on RGP. Materials and methods: Images are reported from a series of 190 SN patients. Repeated standard imaging was invariably normal, when supine. However, 190 patients demonstrated SN of > 1.5 vertebrae on repeating IVU-E. Of whom 36 (18.9%) patients developed recurrent episodes of painful hematuria for which no organic pathology was detected on all standard imaging, when supine- thus fitting the definition of LPHS. -

Diagnosis and Primary Care Management of Focal Segmental Glomerulosclerosis in Children
1.5 CONTACTCOCONOONNTATACACACT HOURSHOUROURRS 1.5 CONTACT HOURS Monkey Business Images / Thinkstock Diagnosis and primary care management of focal segmental glomerulosclerosis in children Abstract: Focal segmental glomerulosclerosis (FSGS) is a pattern of kidney damage that can occur in individuals at any age, including children. Pediatric patients with FSGS require medication monitoring, growth, and psychological health. This article discusses the NP’s role in the clinical presentation, diagnostic workup, and treatment of FSGS in pediatric patients. By Angela Y. Wong, MS, CPNP-PC and Rita Marie John, DNP, EdD, CPNP-PC, FAANP P, a 10-year-old girl, told her parents several This article discusses the pathophysiology, epide- times, “I feel puffy,” before the family sought miology, clinical presentation, and treatment options J medical attention. This complaint could in- for FSGS. In addition, the article elucidates the role dicate a myriad of issues ranging from sudden weight of the NP in managing this disease when it occurs gain to simple abdominal gas. For this child, “puffy” during childhood. depicted her progressive edema—the only overt symp- tom of her diagnosis of focal segmental glomerulo- ■ Overview sclerosis (FSGS). Although some children with FSGS FSGS is a pattern of kidney damage involving scarring may only present with asymptomatic proteinuria at of glomeruli in the kidney. This pattern of glomerulo- a routine physical, FSGS can affect individuals of all sclerosis is focal and segmental, meaning not all glom- ages, and is a common cause of end-stage renal disease eruli are affected and only parts of the glomeruli are (ESRD) in children.1 damaged, respectively.2 FSGS is the most common Keywords: end-stage renal disease, focal segmental glomerulosclerosis, kidney transplant, nephrotic syndrome, pediatrics 28 The Nurse Practitioner • Vol. -

Glomerulosclerosis in Reflux Nephropathy
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Elsevier - Publisher Connector Kidney International, Vol. 21(1982), pp. 528—534 NEPHROLOGY FORUM Glomeruloscierosis in reflux nephropathy Principal discussant: RAMzI S. COTRAN Department of Pathology, Brigham and Women's Hospital, Boston, Massachusetts penis, testes, and urethral meatus were normal. The prostate was of normal size. Editors The BUN was 14 mg/dl; creatinine, 1.3 mg/dl (creatinine clearance, 113 mI/mm); blood chemistries were normal; the blood glucose was 93 JORDANJ. COHEN mg/dl; and the complement profile was normal. Serum protein was 7.5 JOHN 1. HARRINGTON gIdI with 4.3 g/dl albumin. Urinalysis showed a pH of 5; a specific JEROME P.KASSIRER gravity of 1.015; 4+ protein, no cells, and no bacteria. Urine culture was sterile. The 24-hour urine protein excretion was 2.4 g. Editor Chest x-ray showed borderline cardiomegaly with clear lungs. An Managing intravenous pyelogram revealed bilateral coarse scarring with caliecta- CHERYL J. ZUSMAN sis. The right kidney was smaller than the left. There was moderate ureterectasia extending down to the ureterovesical junction. A voiding cystourethrogram revealed a large-capacity bladder; the patient had no MichaelReese Hospital and Medical Center urge to void after almost 500 ml of contrast material was instilled. Bilateral reflux was greater and persistent on the left and was intermit- University of Chicago, tent on the right. The left ureter was dilated and tortuous. A left Pritzker School of Medicine ureterocele and right bladder diverticulum were visualized. and A biopsy of the left kidney showed focal scarring with interstitial New England Medical Center fibrosis and chronic inflammation, tubular atrophy, and dilation. -

Focal Segmental Glomerulosclerosis in Systemic Lupus Erythematosus
Relato de Caso Focal Segmental Glomerulosclerosis in Systemic Lupus Erythematosus: One or Two Glomerular Diseases? Glomerulosclerose Segmentar e Focal em Lúpus Eritematoso Sistêmico: Uma ou Duas Doenças? Rogério Barbosa de Deus1, Luis Antonio Moura1, Marcello Fabiano Franco2, Gianna Mastroianni Kirsztajn1 1 Nephrology Division and 2 Department of Pathology - Universidade Federal de São Paulo – EPM/UNIFESP- São Paulo. ABSTRACT Some patients with clinical and/or laboratory diagnosis of systemic lupus erythematosus (SLE) present with nephritis which from the morphological point of view does not fit in one of the 6 classes described in the WHO classification of lupus nephritis. On the other hand, nonlupus nephritis in patients with confirmed SLE is rarely reported. This condition may not be so uncommon as it seems. The associated glomerular lesions most frequently described are amyloidosis and focal segmental glomerulosclerosis (FSGS). We report on a 46 year-old, caucasian woman, who fulfilled the American College of Rheumatology criteria for SLE diagnosis: arthritis, positive anti-DNA, ANA, anti-Sm antibodies, and cutaneous maculae. During the follow-up, she presented arthralgias, alopecia, vasculitis, lower extremities edema and decreased serum levels of C3 and C4. Proteinuria was initially nephrotic, but reached negative levels. The serum creatinine varied from 0.7 to 3.0 mg/dl. The patient was submitted to the first renal biopsy at admission and to the second one, 3 years later, with diagnosis of minimal change disease and FSGS, respectively. No deposits were demonstrated by immunofluorescence. In the present case, we believe that the patient had SLE and developed an idiopathic disease of the minimal change disease-FSGS spectrum. -

Diagnosis and Management of Pyelonephritis
DIAGNOSIS AND MANAGEMENT OF PYELONEPHRITIS ROBERT D. TAYLOR, M.D. Research Division F the four common nephropathies, glomerulonephritis, nephrosclerosis, Ointercapillary glomerulosclerosis and pyelonephritis, at present only pyelonephritis, the most familiar of these, offers the possibility of arrest or cure. It has been strangely neglected, possibly because it is a nosologic step- child, half surgical and half medical. Volhard and Fahr in 19141 did not list it among medical diseases of the kidney nor did Addis in 1925.2 Apart from the pediatric, obstetric and urologic aspects, little of general interest was written about it until 1939 when Weiss and Parker3 explored its relationship to hyper- icnsive disease. In 1948 Raaschau4 of Copenhagen published an excellent monograph on the subject with extensive pathologic and clinical studies. His most striking observation concerns its incidence. Among 3607 routine autop- sies he found histopathologic evidence of pyelonephritis in 5.6 per cent. One half of these persons had died of renal failure but in only 1 out of 6 was the condition recognized ante mortem. Undoubtedly, if a disease is both common and remediable, its diagnosis and treatment are of general interest. Etiology and Pathology The most common organisms in pyelonephritis are colon bacilli and hemo- lytic streptococci. In some cases the infection is secondary to lesions which prevent free urinary drainage. In this group surgical correction of the causes of urinary stasis usually permits eradication of infection. Among the remaining patients the process is primary with no demonstrable anatomic abnormality. The organisms apparently reach the kidney substance through the blood stream. The pelvis and lower urinary tract become involved by contamination with infected urine. -

Focal Segmental Glomerulosclerosis
some = Focal sections of = Segmental Focal Segmental kidney filters = Glomerulo FSGS Glomerulosclerosis = { are scarred Sclerosis How can research help? Research, which often requires patient participation, can lead to a better understanding of the causes, provide better diagnoses and more effective treatments, and ultimately help to find a cure. Be part of the discovery: By studying patients, researchers can more quickly unlock the mysteries of this disease. To get involved in research and stay informed, go to: Nephrotic Syndrome Study Network www.Nephrotic-Syndrome- NEPTUNE is a part of the NIH Rare Diseases Clinical Research Network (RDCRN). Funding and/or programmatic support for this project has been provided by U54 Studies.org DK083912 from the NIDDK and the NIH Office of Rare Diseases Research (ORDR), the NephCure Foundation and the University of Michigan. The views expressed in written materials of publications do not necessarily reflect the official policies of the or call 1-866-NephCure Department of Health and Human Services; nor does mention by trade names, commercial practices or organizations imply endorsement by the U.S. Government. What is Focal and Segmental Glomerulosclerosis? Symptoms, Diagnosis and Treatment Each person has Focal Segmental Glomerulosclerosis (FSGS) is a Your nephrologist may also recommend: two kidneys in rare disease that attacks the kidney’s filtering system • Diuretics and low salt diet help to control edema their lower back. (glomeruli) causing scarring of the filter. FSGS • A medication that blocks a hormone system called is one of the causes of a condition known as the renin angiotensin system (ACE inhibitor or ARB) Nephrotic Syndrome (NS). -

Supermicar Data Entry Instructions, 2007 363 Pp. Pdf Icon[PDF
SUPERMICAR TABLE OF CONTENTS Chapter I - Introduction to SuperMICAR ........................................... 1 A. History and Background .............................................. 1 Chapter II – The Death Certificate ..................................................... 3 Exercise 1 – Reading Death Certificate ........................... 7 Chapter III Basic Data Entry Instructions ....................................... 12 A. Creating a SuperMICAR File ....................................... 14 B. Entering and Saving Certificate Data........................... 18 C. Adding Certificates using SuperMICAR....................... 19 1. Opening a file........................................................ 19 2. Certificate.............................................................. 19 3. Sex........................................................................ 20 4. Date of Death........................................................ 20 5. Age: Number of Units ........................................... 20 6. Age: Unit............................................................... 20 7. Part I, Cause of Death .......................................... 21 8. Duration ................................................................ 22 9. Part II, Cause of Death ......................................... 22 10. Was Autopsy Performed....................................... 23 11. Were Autopsy Findings Available ......................... 23 12. Tobacco................................................................ 24 13. Pregnancy............................................................ -
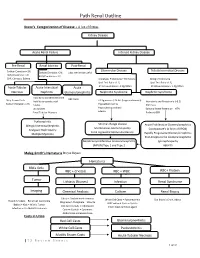
Path Renal Outline
Path Renal Outline Krane’s Categorization of Disease + A lot of Extras Kidney Disease Acute Renal Failure Intrinsic Kidney Disease Pre‐Renal Renal Intrinsic Post‐Renal Sodium Excretion <1% Glomerular Disease Tubulointerstitial Disease Sodium Excretion < 1% Sodium Excretion >2% Labs aren’t that useful BUN/Creatinine > 20 BUN/Creatinine < 10 CHF, Cirrhosis, Edema Urinalysis: Proteinuria + Hematuria Benign Proteinuria Spot Test Ratio >1.5, Spot Test Ratio <1.5, Acute Tubular Acute Interstitial Acute 24 Urine contains > 2.0g/24hrs 24 Urine contains < 1.0g/24hrs Necrosis Nephritis Glomerulonephritis Nephrotic Syndrome Nephritic Syndrome Inability to concentrate Urine RBC Casts Dirty Brown Casts Inability to secrete acid >3.5g protein / 24 hrs (huge proteinuria) Hematuria and Proteinuria (<3.5) Sodium Excretion >2% Edema Hypoalbuminemia RBC Casts Hypercholesterolemia Leukocytes Salt and Water Retention = HTN Focal Tubular Necrosis Edema Reduced GFR Pyelonephritis Minimal change disease Allergic Interstitial Nephritis Acute Proliferative Glomerulonephritis Membranous Glomerulopathy Analgesic Nephropathy Goodpasture’s (a form of RPGN) Focal segmental Glomerulosclerosis Rapidly Progressive Glomerulonephritis Multiple Myeloma Post‐Streptococcal Glomerulonephritis Membranoproliferative Glomerulonephritis IgA nephropathy (MPGN) Type 1 and Type 2 Alport’s Meleg‐Smith’s Hematuria Break Down Hematuria RBCs Only RBC + Crystals RBC + WBC RBC+ Protein Tumor Lithiasis (Stones) Infection Renal Syndrome Imaging Chemical Analysis Culture Renal Biopsy Calcium -

FSGS Fact Sheet 4.12.18
® Focal Segmental Glomerulosclerosis Focal Segmental Glomerulosclerosis (FSGS) is a rare kidney disease characterized by dysfunction in the part of the kidney that filters blood (glomeruli). Only some glomeruli are aected, but continued damage can lead to kidney failure. Focal = Some Segmental = Sections Glomerulo = of the Filtering Units Sclerosis = Are Scarred FSGS Symptoms The exact cause of primary Early symptoms of FSGS are the same as Nephrotic Syndrome. FSGS is unknown and not precisely understood. However, genetic and Common Symptoms: environmental factors may be associated - Protein in the urine, which can be foamy (called with the disease. proteinuria) - Low levels of protein in the blood With FSGS, many individuals - Swelling in parts of the body, most noticeably around experience cycles the eyes, hands, feet, and abdomen (called edema) of remission and relapse. - Weight gain due to extra fluid building up in your body Remission means there - Can cause high blood pressure (called hypertension) is currently no and high fat levels in the blood (high cholesterol) protein spilling into the 50% of urine. patients with FSGS will Fast Facts progress to kidney failure. The only way to dierentiate FSGS from other primary Every FSGS Nephrotic Syndrome conditions is to have a kidney biopsy. patient follows a unique journey. FSGS in Adults FSGS in Children - FSGS occurs more - Focal Segmental frequently in adults than Glomerulosclerosis is one of in children and is most the leading causes of End Some patients prevalent in adults 45 Stage Renal Disease receive a kidney years or older. (ESRD) in children. transplant to treat their kidney failure due to FSGS, - African Americans are 5 - FSGS is associated with but FSGS comes back times more likely to get up to 20% of all new cases to attack the new FSGS in comparison with of Nephrotic Syndrome kidney 30-50% the general population. -

Renal Manifestations of Common Variable Immunodeficiency Tiffany
Kidney360 Publish Ahead of Print, published on April 21, 2020 as doi:10.34067/KID.0000432020 Renal Manifestations of Common Variable Immunodeficiency Tiffany N. Caza1, Samar I. Hassen1, Christopher Larsen1 1 Arkana Laboratories, Bryant, Arkansas Correspondence Dr. Tiffany N. Caza Arkana Laboratories 10810 Executive Center Drive Bryant, Arkansas 72022 United States [email protected] Copyright 2020 by American Society of Nephrology. ABSTRACT Background: Common variable immunodeficiency (CVID) is one of the most common primary immunodeficiency syndromes, affecting 1/25,000-50,000. Renal insufficiency occurs in approximately 2 percent of CVID patients. To date, there are no case series of renal biopsies from CVID patients, making it difficult to determine whether individual cases of renal disease in CVID represent sporadic events or are related to the underlying pathophysiology. We performed a retrospective analysis of renal biopsies in our database from patients with a clinical history of CVID (n=22 patients, 27 biopsies). Methods: Light, immunofluorescence, and electron microscopy were reviewed. IgG subclasses, PLA2R immunohistochemistry, and THSD7A, EXT1, and NELL1 immunofluorescence were performed on all membranous glomerulopathy cases. Results: Acute kidney injury and proteinuria were the leading indications for renal biopsy in CVID patients. Immune complex glomerulopathy was present in 12 of 22 (54.5%) cases including 9 with membranous glomerulopathy, one case with a C3 glomerulopathy, and one case with membranoproliferative glomerulonephritis with IgG3 kappa deposits. All membranous glomerulopathy cases were PLA2R, THSD7A, EXT1, and NELL1 negative. The second most common renal biopsy diagnosis was chronic tubulointerstitial nephritis, affecting 33% cases. All tubulointerstitial nephritis cases showed tubulitis and a lymphocytic infiltrate with >90% CD3+ T cells. -

Chronic Renal Pain: an Approach to Investigation and Management
review Chronic renal pain: An approach to investigation and management Malcolm J. Dewar, MBChB, MMed, MSc, FCUrol(SA); Joseph L. Chin, MD, FRCSC Division of Urology, Western University, London, ON, Canada Cite as: Can Urol Assoc J 2018;12(6Suppl3):S167-70. http://dx.doi.org/10.5489/cuaj.5327 of dominant cysts (three cysts >4 cm). Localized tenderness with an ultrasound probe, as well as relief with percutaneous cyst aspiration, might predict an improved response to cyst Introduction de-roofing or sclerotherapy. Laparoscopic denervation of the kidney accompanied by nephropexy and renal artery embol- ization has been described, while laparoscopic nephrectomy When chronic flank pain is present, there is most often a cause can be considered in patients with end-stage renal disease. that is readily identified on routine assessment (Table 1). In the vast majority of cases, resolution of the underlying pathology Loin pain hematuria syndrome (LPHS) results in improvement of the pain. Although epidemiological data are sparse, it seems that chronic renal pain syndromes LPHS is a very rare condition, characterized by intermit- are uncommon. This brief review will address selected condi- tent or persistent flank pain that is often, but not always, tions in which chronic pain is a primary presenting feature, accompanied by hematuria. Hematuria, microscopic or and give an approach to diagnosis and management. macroscopic, appears to be glomerular in origin. Pain can be severe and unrelenting, with a significant impact on quality Autosomal-dominant polycystic kidney disease (ADPKD) of life and the ability to function. The clinical syndrome has been well-characterized as follows: a six-month or longer Chronic renal pain is the most common presenting symptom history of flank pain that is either persistently present or of ADPKD. -

Signs and Symptoms of Urinary System Diseases
SIGNS AND SYMPTOMS OF URINARY SYSTEM DISEASES LECTURE IN INTERNAL MEDICINE PROPAEDEUTICS M. Yabluchansky, L. Bogun, L.Martymianova, O. Bychkova, N. Lysenko, N. Makienko, E. Tomina, E. Golubkina V.N. Karazin National University Medical School’ Internal Medicine Dept. http://kottke.org/tag/infoviz Plan of the lecture • The importance(value) of a human kidney • Reminder – how do kidneys work – the primary function – purpose • History-taking • Patient’s examination – clinical – laboratory – instrumental • Spectrum of urinary system diseases • Urinary system diseases’ symptoms and syndromes – symptoms – urinary syndrome – nephrotic syndrome – nephritic syndrome – urinary tract obstruction syndrome – hypertensive syndrome • Glossary of urinary pathology’ terms http://images.emedicinehealth.com/images/illustrations/urinary_structures.jpg The price of a human kidney The human kidney is the body’s filter. It cleans 180 liters of liquid per day, retaining the good stuff and expelling the bad. Most fortuitously, humans are born with two kidneys. If one of them becomes damaged, the other one can pick up the slack. If both your kidneys fail, however, your body will be filled with harmful toxins. Without medical intervention, such patients will die within several weeks Reminder: how kidneys work https://www.youtube.com/watch?v=aj-gbnOB4jM http://venturebeat.com/wp-content/uploads/2012/08/kidneys.jpg Reminder: the primary urinary system functions • maintain homeostasis • regulate fluids and electrolytes • eliminate waste products • maintain blood pressure (BP) • involved with red blood cell (RBC) production • involved with bone metabolism Reminder: purpose • General evaluation of health • Diagnosis of disease or disorders of the kidneys or urinary tract • Diagnosis of other systemic diseases that affect kidney function • Monitoring of patients with diabetes • Screening for drug toxicity (eg.