ES-62 Suppression of Arthritis Reflects Epigenetic Rewiring of Synovial Fibroblasts to a Joint-Protective Phenotype
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

A Fusion of Pathology in Diabetic Neuropathy MEOX2 Linked With
RESEARCH HIGHLIGHTS NEUROLOGICAL DISORDERS A fusion of pathology in diabetic neuropathy The fusion of proinsulin-expressing bone of factors have been implicated in the the researchers showed that the treatment of marrow cells with neurons could be a process. diabetic rats with insulin led to a reduction in key event in the development of diabetic Chan and colleagues had previously the number of proinsulin-positive cells and neuropathy, according to a recent report found proinsulin- and insulin-positive prevented the prolongation of motor nerve by Lawrence Chan and colleagues. cells — which are normally confined conduction velocity — a sign of neuropathy Diabetic peripheral neuropathy is the to the pancreas — in various organs in — confirming that the appearance of these leading cause of non-traumatic limb mouse and rat models of diabetes, and had cells was due to hyperglycaemia. amputations. The symptoms can be shown that most of these extrapancreatic How the mechanism described by Chan widespread, from numbness, pain and insulin-producing cells originated in the and colleagues relates to several other tingling of the extremities to problems bone marrow. In their latest study, the factors that have been implicated in with the digestive tract, bladder infections researchers discovered that in diabetic diabetic neuropathy, including oxidative and impotence. But the chain of events mice and rats with neuropathy, bone- stress and growth factor deficiency, that leads to nerve damage in diabetes is marrow-derived cells that expressed remains an open question. not well described, and current treatments proinsulin fused with neurons in the Rebecca Craven are designed to relieve discomfort and sciatic nerve and dorsal root ganglion, References and links prevent further tissue damage. -
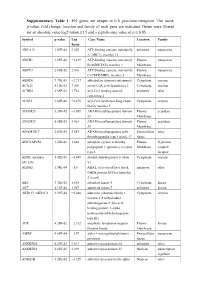
Supplementary Table 1
Supplementary Table 1. 492 genes are unique to 0 h post-heat timepoint. The name, p-value, fold change, location and family of each gene are indicated. Genes were filtered for an absolute value log2 ration 1.5 and a significance value of p ≤ 0.05. Symbol p-value Log Gene Name Location Family Ratio ABCA13 1.87E-02 3.292 ATP-binding cassette, sub-family unknown transporter A (ABC1), member 13 ABCB1 1.93E-02 −1.819 ATP-binding cassette, sub-family Plasma transporter B (MDR/TAP), member 1 Membrane ABCC3 2.83E-02 2.016 ATP-binding cassette, sub-family Plasma transporter C (CFTR/MRP), member 3 Membrane ABHD6 7.79E-03 −2.717 abhydrolase domain containing 6 Cytoplasm enzyme ACAT1 4.10E-02 3.009 acetyl-CoA acetyltransferase 1 Cytoplasm enzyme ACBD4 2.66E-03 1.722 acyl-CoA binding domain unknown other containing 4 ACSL5 1.86E-02 −2.876 acyl-CoA synthetase long-chain Cytoplasm enzyme family member 5 ADAM23 3.33E-02 −3.008 ADAM metallopeptidase domain Plasma peptidase 23 Membrane ADAM29 5.58E-03 3.463 ADAM metallopeptidase domain Plasma peptidase 29 Membrane ADAMTS17 2.67E-04 3.051 ADAM metallopeptidase with Extracellular other thrombospondin type 1 motif, 17 Space ADCYAP1R1 1.20E-02 1.848 adenylate cyclase activating Plasma G-protein polypeptide 1 (pituitary) receptor Membrane coupled type I receptor ADH6 (includes 4.02E-02 −1.845 alcohol dehydrogenase 6 (class Cytoplasm enzyme EG:130) V) AHSA2 1.54E-04 −1.6 AHA1, activator of heat shock unknown other 90kDa protein ATPase homolog 2 (yeast) AK5 3.32E-02 1.658 adenylate kinase 5 Cytoplasm kinase AK7 -

Comprehensive Epigenome Characterization Reveals Diverse Transcriptional Regulation Across Human Vascular Endothelial Cells
Nakato et al. Epigenetics & Chromatin (2019) 12:77 https://doi.org/10.1186/s13072-019-0319-0 Epigenetics & Chromatin RESEARCH Open Access Comprehensive epigenome characterization reveals diverse transcriptional regulation across human vascular endothelial cells Ryuichiro Nakato1,2† , Youichiro Wada2,3*†, Ryo Nakaki4, Genta Nagae2,4, Yuki Katou5, Shuichi Tsutsumi4, Natsu Nakajima1, Hiroshi Fukuhara6, Atsushi Iguchi7, Takahide Kohro8, Yasuharu Kanki2,3, Yutaka Saito2,9,10, Mika Kobayashi3, Akashi Izumi‑Taguchi3, Naoki Osato2,4, Kenji Tatsuno4, Asuka Kamio4, Yoko Hayashi‑Takanaka2,11, Hiromi Wada3,12, Shinzo Ohta12, Masanori Aikawa13, Hiroyuki Nakajima7, Masaki Nakamura6, Rebecca C. McGee14, Kyle W. Heppner14, Tatsuo Kawakatsu15, Michiru Genno15, Hiroshi Yanase15, Haruki Kume6, Takaaki Senbonmatsu16, Yukio Homma6, Shigeyuki Nishimura16, Toutai Mitsuyama2,9, Hiroyuki Aburatani2,4, Hiroshi Kimura2,11,17* and Katsuhiko Shirahige2,5* Abstract Background: Endothelial cells (ECs) make up the innermost layer throughout the entire vasculature. Their phe‑ notypes and physiological functions are initially regulated by developmental signals and extracellular stimuli. The underlying molecular mechanisms responsible for the diverse phenotypes of ECs from diferent organs are not well understood. Results: To characterize the transcriptomic and epigenomic landscape in the vascular system, we cataloged gene expression and active histone marks in nine types of human ECs (generating 148 genome‑wide datasets) and carried out a comprehensive analysis with chromatin interaction data. We developed a robust procedure for comparative epigenome analysis that circumvents variations at the level of the individual and technical noise derived from sample preparation under various conditions. Through this approach, we identifed 3765 EC‑specifc enhancers, some of which were associated with disease‑associated genetic variations. -

Saethre–Chotzen Syndrome Caused by TWIST 1 Gene Mutations: Functional Differentiation from Muenke Coronal Synostosis Syndrome
European Journal of Human Genetics (2006) 14, 39–48 & 2006 Nature Publishing Group All rights reserved 1018-4813/06 $30.00 www.nature.com/ejhg ARTICLE Saethre–Chotzen syndrome caused by TWIST 1 gene mutations: functional differentiation from Muenke coronal synostosis syndrome Wolfram Kress*,1, Christian Schropp2, Gabriele Lieb2, Birgit Petersen2, Maria Bu¨sse-Ratzka2, Ju¨rgen Kunz3, Edeltraut Reinhart4, Wolf-Dieter Scha¨fer5, Johanna Sold5, Florian Hoppe6, Jan Pahnke6, Andreas Trusen7, Niels So¨rensen8,Ju¨rgen Krauss8 and Hartmut Collmann8 1Institute of Human Genetics, University of Wu¨rzburg, Wu¨rzburg, Germany; 2Department of Pediatrics, University of Wu¨rzburg, Wu¨rzburg, Germany; 3Institute of Human Genetics, University of Marburg, Marburg, Germany; 4Department of Maxillo-facial Surgery, University of Wu¨rzburg, Wu¨rzburg, Germany; 5Department of Ophthalmology, University of Wu¨rzburg, Wu¨rzburg, Germany; 6Department of Otorhinolaryngology, University of Wu¨rzburg, Wu¨rzburg, Germany; 7Department of Diagnostic Radiology, University of Wu¨rzburg, Wu¨rzburg, Germany; 8Sect. Pediatric Neurosurgery, University of Wu¨rzburg, Wu¨rzburg, Germany The Saethre–Chotzen syndrome (SCS) is an autosomal dominant craniosynostosis syndrome with uni- or bilateral coronal synostosis and mild limb deformities. It is caused by loss-of-function mutations of the TWIST 1 gene. In an attempt to delineate functional features separating SCS from Muenke’s syndrome, we screened patients presenting with coronal suture synostosis for mutations in the TWIST 1 gene, and for the Pro250Arg mutation in FGFR3. Within a total of 124 independent pedigrees, 39 (71 patients) were identified to carry 25 different mutations of TWIST 1 including 14 novel mutations, to which six whole gene deletions were added. -

GLI1 Transcription Axis Involved in Cancer Drug Resistance, Overall Survival and Therapy Prognosis in Lung Cancer Patients
www.impactjournals.com/oncotarget/ Oncotarget, Advance Publications 2017 Epigenomic study identifies a novel mesenchyme homeobox2- GLI1 transcription axis involved in cancer drug resistance, overall survival and therapy prognosis in lung cancer patients Armas López Leonel1, Piña-Sánchez Patricia2, Arrieta Oscar3, Guzman de Alba Enrique4, Ortiz Quintero Blanca4, Santillán Doherty Patricio4, Christiani David C.5, Zúñiga Joaquín4 and Ávila-Moreno Federico1,4 1National University Autonomous of México (UNAM), Facultad de Estudios Superiores (FES) Iztacala, Biomedicine Research Unit (UBIMED), Lung Diseases And Cancer Epigenomics Laboratory, Mexico State, Mexico 2Instituto Mexicano del Seguro Social (IMSS), Centro Medico Nacional (CMN) Siglo XXI, Unidad de Investigación Médica en Enfermedades Oncológicas (UIMEO), Molecular Oncology Laboratory, Mexico City, Mexico 3National Cancer Institute (INCAN), Thoracic Oncology Clinic, Mexico City, Mexico 4National Institute of Respiratory Diseases (INER), Ismael Cosío Villegas, Mexico City, Mexico 5Harvard Medical School, Harvard School of Public Health, Department of Environmental Health, Boston Massachusetts, USA Correspondence to: Federico Ávila Moreno, email: [email protected], [email protected] Keywords: lung cancer, homeobox transcription factors, Epigenetics cancer drug resistance, overall survival, treatment prognosis Received: May 26, 2016 Accepted: April 11, 2017 Published: May 09, 2017 Copyright: Leonel et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC-BY), which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. ABSTRACT Several homeobox-related gene (HOX) transcription factors such as mesenchyme HOX-2 (MEOX2) have previously been associated with cancer drug resistance, malignant progression and/or clinical prognostic responses in lung cancer patients; however, the mechanisms involved in these responses have yet to be elucidated. -

Dysregulation of Meox2 Following Wt1 Mutation in Kidney Development and Wilms Tumorigenesis
The Texas Medical Center Library DigitalCommons@TMC The University of Texas MD Anderson Cancer Center UTHealth Graduate School of The University of Texas MD Anderson Cancer Biomedical Sciences Dissertations and Theses Center UTHealth Graduate School of (Open Access) Biomedical Sciences 12-2011 DYSREGULATION OF MEOX2 FOLLOWING WT1 MUTATION IN KIDNEY DEVELOPMENT AND WILMS TUMORIGENESIS LaGina M. Nosavanh LaGina Merie Nosavanh Follow this and additional works at: https://digitalcommons.library.tmc.edu/utgsbs_dissertations Part of the Medicine and Health Sciences Commons Recommended Citation Nosavanh, LaGina M. and Nosavanh, LaGina Merie, "DYSREGULATION OF MEOX2 FOLLOWING WT1 MUTATION IN KIDNEY DEVELOPMENT AND WILMS TUMORIGENESIS" (2011). The University of Texas MD Anderson Cancer Center UTHealth Graduate School of Biomedical Sciences Dissertations and Theses (Open Access). 203. https://digitalcommons.library.tmc.edu/utgsbs_dissertations/203 This Thesis (MS) is brought to you for free and open access by the The University of Texas MD Anderson Cancer Center UTHealth Graduate School of Biomedical Sciences at DigitalCommons@TMC. It has been accepted for inclusion in The University of Texas MD Anderson Cancer Center UTHealth Graduate School of Biomedical Sciences Dissertations and Theses (Open Access) by an authorized administrator of DigitalCommons@TMC. For more information, please contact [email protected]. DYSREGULATION OF MEOX2 FOLLOWING WT1 MUTATION IN KIDNEY DEVELOPMENT AND WILMS TUMORIGENESIS by LaGina Merie Nosavanh, B.S. -

Differential Chromatin Binding of the Lung Lineage Transcription Factor NKX2-1 Resolves Opposing Murine Alveolar Cell Fates in Vivo ✉ Danielle R
ARTICLE https://doi.org/10.1038/s41467-021-22817-6 OPEN Differential chromatin binding of the lung lineage transcription factor NKX2-1 resolves opposing murine alveolar cell fates in vivo ✉ Danielle R. Little1,2, Anne M. Lynch1,3, Yun Yan 2, Haruhiko Akiyama4, Shioko Kimura 5 & Jichao Chen 1 Differential transcription of identical DNA sequences leads to distinct tissue lineages and then multiple cell types within a lineage, an epigenetic process central to progenitor and stem 1234567890():,; cell biology. The associated genome-wide changes, especially in native tissues, remain insufficiently understood, and are hereby addressed in the mouse lung, where the same lineage transcription factor NKX2-1 promotes the diametrically opposed alveolar type 1 (AT1) and AT2 cell fates. Here, we report that the cell-type-specific function of NKX2-1 is attributed to its differential chromatin binding that is acquired or retained during development in coordination with partner transcriptional factors. Loss of YAP/TAZ redirects NKX2-1 from its AT1-specific to AT2-specific binding sites, leading to transcriptionally exaggerated AT2 cells when deleted in progenitors or AT1-to-AT2 conversion when deleted after fate commitment. Nkx2-1 mutant AT1 and AT2 cells gain distinct chromatin accessible sites, including those specific to the opposite fate while adopting a gastrointestinal fate, suggesting an epigenetic plasticity unexpected from transcriptional changes. Our genomic analysis of single or purified cells, coupled with precision genetics, provides an epigenetic basis for alveolar cell fate and potential, and introduces an experimental benchmark for deciphering the in vivo function of lineage transcription factors. 1 Department of Pulmonary Medicine, The University of Texas MD Anderson Cancer Center, Houston, TX, USA. -

BMC Biology Biomed Central
BMC Biology BioMed Central Research article Open Access Classification and nomenclature of all human homeobox genes PeterWHHolland*†1, H Anne F Booth†1 and Elspeth A Bruford2 Address: 1Department of Zoology, University of Oxford, South Parks Road, Oxford, OX1 3PS, UK and 2HUGO Gene Nomenclature Committee, European Bioinformatics Institute (EMBL-EBI), Wellcome Trust Genome Campus, Hinxton, Cambridgeshire, CB10 1SA, UK Email: Peter WH Holland* - [email protected]; H Anne F Booth - [email protected]; Elspeth A Bruford - [email protected] * Corresponding author †Equal contributors Published: 26 October 2007 Received: 30 March 2007 Accepted: 26 October 2007 BMC Biology 2007, 5:47 doi:10.1186/1741-7007-5-47 This article is available from: http://www.biomedcentral.com/1741-7007/5/47 © 2007 Holland et al; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/2.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Abstract Background: The homeobox genes are a large and diverse group of genes, many of which play important roles in the embryonic development of animals. Increasingly, homeobox genes are being compared between genomes in an attempt to understand the evolution of animal development. Despite their importance, the full diversity of human homeobox genes has not previously been described. Results: We have identified all homeobox genes and pseudogenes in the euchromatic regions of the human genome, finding many unannotated, incorrectly annotated, unnamed, misnamed or misclassified genes and pseudogenes. -

Genome-Wide Mapping in a House Mouse Hybrid Zone Reveals Hybrid Sterility Loci and Dobzhansky-Muller Interactions Leslie M Turner1,2, Bettina Harr1*
RESEARCH ARTICLE elifesciences.org Genome-wide mapping in a house mouse hybrid zone reveals hybrid sterility loci and Dobzhansky-Muller interactions Leslie M Turner1,2, Bettina Harr1* 1Department of Evolutionary Genetics, Max Planck Institute for Evolutionary Biology, Plön, Germany; 2Laboratory of Genetics, University of Wisconsin, Madison, United States Abstract Mapping hybrid defects in contact zones between incipient species can identify genomic regions contributing to reproductive isolation and reveal genetic mechanisms of speciation. The house mouse features a rare combination of sophisticated genetic tools and natural hybrid zones between subspecies. Male hybrids often show reduced fertility, a common reproductive barrier between incipient species. Laboratory crosses have identified sterility loci, but each encompasses hundreds of genes. We map genetic determinants of testis weight and testis gene expression using offspring of mice captured in a hybrid zone between M. musculus musculus and M. m. domesticus. Many generations of admixture enables high-resolution mapping of loci contributing to these sterility-related phenotypes. We identify complex interactions among sterility loci, suggesting multiple, non-independent genetic incompatibilities contribute to barriers to gene flow in the hybrid zone. DOI: 10.7554/eLife.02504.001 Introduction *For correspondence: harr@ New species arise when reproductive barriers form, preventing gene flow between populations evolbio.mpg.de (Coyne and Orr, 2004). Recently, two approaches have substantially -

GATA4-Dependent Organ-Specific Endothelial Differentiation Controls Liver Development and Embryonic Hematopoiesis
GATA4-dependent organ-specific endothelial differentiation controls liver development and embryonic hematopoiesis Cyrill Géraud, … , Kai Schledzewski, Sergij Goerdt J Clin Invest. 2017;127(3):1099-1114. https://doi.org/10.1172/JCI90086. Research Article Hepatology Vascular biology Microvascular endothelial cells (ECs) are increasingly recognized as organ-specific gatekeepers of their microenvironment. Microvascular ECs instruct neighboring cells in their organ-specific vascular niches through angiocrine factors, which include secreted growth factors (angiokines), extracellular matrix molecules, and transmembrane proteins. However, the molecular regulators that drive organ-specific microvascular transcriptional programs and thereby regulate angiodiversity are largely elusive. In contrast to other ECs, which form a continuous cell layer, liver sinusoidal ECs (LSECs) constitute discontinuous, permeable microvessels. Here, we have shown that the transcription factor GATA4 controls murine LSEC specification and function. LSEC-restricted deletion of Gata4 caused transformation of discontinuous liver sinusoids into continuous capillaries. Capillarization was characterized by ectopic basement membrane deposition, formation of a continuous EC layer, and increased expression of VE-cadherin. Correspondingly, ectopic expression of GATA4 in cultured continuous ECs mediated the downregulation of continuous EC-associated transcripts and upregulation of LSEC-associated genes. The switch from discontinuous LSECs to continuous ECs during embryogenesis caused -

Supplementary File Table S1
Supplementary file Table S1 Grouping of Homeobox genes according to their main known function. Anatomical Structure Morphogenesis EN1, HOXC10, HOXC13, HOXD3, LBX1, SIX2, SIX4 Organ Morphogenesis CDX1, CDX2, HOXA11, HOXA13, ISL1, LHX1, PAX3, PDHX, PITX2, PITX3, PROX1, SIX6 Body Pattern Formation ALX3, EMX2, HHEX, HOXA11, HOXA2, HOXA4, HOXA5, HOXA6, HOXB1, HOXB5, HOXB6, HOXC5, HOXD10, HOXD8, LMX1B, PITX2 Ectoderm Development PROX1, VAX2 Endoderm Development HOXC11 Brain & Nervous System Development Brain Development ALX1, DLX2, EMX2 Nervous System Development: ARX, DLX5, DLX6, HOXD10, LBX1, LHX1, OTP, PAX3, PHOX2A, PHOX2B Skeletal Development: ALX3, ALX4, DLX3, DLX5, DLX6, EN1, HOXA11, HOXA13, HOXA2, HOXB6, HOXD10, HOXD13, MSX2 Muscle Development: BARX2, MKX, SIRT1, SIRT2, SIX1 Other Homeobox Genes Involved In BARX1, CDX4, CUX1, DLX1, EMX1, EN2, Multicellular Organismal HOXA1, HOXA7, HOXA9, HOXB13, HOXB2, Development: HOXB3, HOXB4, HOXB7, HOXB8, HOXB9, HOXC12, HOXC8, HOXC9, HOXD1, HOXD11, HOXD12, HOXD9, ISL2, LBX2, LMX1A, MEIS1, NKX3-1, OTX1, TLX1, VAX1, VSX1, VSX2 Homeobox Genes Involved In Cell ARX, EMX2, HHEX, HLX, HOPX, LBX1, LHX1, Differentiation: LMX1B, MIXL1, OTP, PHOX2A, SIRT1, VSX2 Other Genes: PHTF1, SIRT3, SIRT6, SIRT7, ZHX1, ZHX2 Homeobox genes include two subsets of genes coding for transcription factors involved in multiple functions. The clustered HOX genes are indicated in bold. Supplementary file Figure S2 5’ Spatial collinearity 3’ HOXA Chr. 7p15.3 HOXB Chr. 17q21.3 HOXC Chr. 12q13.3 HOXD Chr. 2q31 13 12 11 10 9 8 7 6 5 4 3 2 1 Paralogous HOX groups Distribution of the 39 human HOX genes in four clusters located in different chromosomal regions*. Blue indicates anterior HOX genes. Yellow, paralogy group 3 Hox genes, green and purple indicatete central HOX genes and Red the posterior HOX genes. -

The Genetics of Heterotaxy Syndrome
The Genetics of Heterotaxy Syndrome A dissertation submitted to the Division of Graduate Studies and Research, University of Cincinnati in partial fulfillment of the requirements for the degree of Doctor of Philosophy in Molecular and Developmental Biology by Jason R. Cowan Master of Science, University of British Columbia, Vancouver, 2007 Committee Chair: Stephanie M. Ware, M.D., Ph.D. Robert B. Hinton Jr., M.D. Linda M. Parysek, Ph.D. S. Steven Potter, Ph.D. Aaron M. Zorn, Ph.D. Molecular & Developmental Biology Graduate Program College of Medicine, University of Cincinnati Division of Developmental Biology, Cincinnati Children’s Hospital Medical Center Cincinnati, Ohio, USA, 2015 ABSTRACT Congenital heart defects (CHDs) are the greatest cause of infant morbidity and mortality worldwide, occurring in roughly 8 per 1000 live births (~1%). Heterotaxy, a multiple congenital anomaly syndrome resulting from failure to establish left-right (L-R) asymmetry, is characterized by diverse, complex CHDs. Heterogeneous in presentation and etiology, heterotaxy serves as a complex and growing focal point for cardiovascular genetic research. In the two decades since the zinc finger transcription factor, ZIC3, was first identified as a cause of X-linked heterotaxy, mutations in nearly twenty genes with L-R patterning functions have been detected among patients with heterotaxy. Nevertheless, despite considerable progress, genetic causes for heterotaxy remain largely uncharacterized. With an estimated 70-80% of heterotaxy cases still unexplained, there remains enormous potential for novel gene discovery. In this dissertation, we have balanced gene discovery efforts aimed at identifying and characterizing novel causes of heterotaxy with studies into the mechanisms governing ZIC3- related heterotaxy.