For Inflammatory Bowel Disease
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Reference Ranges for Blood Concentrations of Eosinophils And
Journal of Perinatology (2010) 30, 540–545 r 2010 Nature America, Inc. All rights reserved. 0743-8346/10 www.nature.com/jp ORIGINAL ARTICLE Reference ranges for blood concentrations of eosinophils and monocytes during the neonatal period defined from over 63 000 records in a multihospital health-care system RD Christensen1,2, J Jensen1,3, A Maheshwari4 and E Henry1,3 1Intermountain Healthcare Women and Newborns Clinical Program, Ogden, UT, USA; 2McKay-Dee Hospital Center, Ogden, UT, USA; 3Institute for Healthcare Delivery Research, Salt Lake City, UT, USA and 4Divisions of Neonatology and Pediatric Gastroenterology, Departments of Pediatrics, Cell Biology, and Pathology, University of Alabama at Birmingham, Birmingham, AL, USA Introduction Objective: Blood concentrations of eosinophils and monocytes are part Normal values for hematological parameters are not generally of the complete blood count. Reference ranges for these concentrations during available for neonates because blood is not drawn on healthy the neonatal period, established by very large sample sizes and modern neonates to establish normal ranges. Instead, ‘reference ranges’ are methods, are needed for identifying abnormally low or high values. used in neonatal hematology.1–6 These consist of the 5th to 95th Study Design: We constructed reference ranges for eosinophils per ml percentile values assembled from large numbers of neonates with and monocytes per ml among neonates of 22 to 42 weeks of gestation, minimal pathology or with pathology not thought to be relevant to on the day of birth, and also during 28 days after birth. Data were the laboratory parameter under study. Recent examples of their obtained from archived electronic records over an eight and one-half-year usefulness include the following: Reference ranges for erythrocyte period in a multihospital health-care system. -

Generation of Monocyte-Derived Tumor-Associated Macrophages Using
Benner et al. Journal for ImmunoTherapy of Cancer (2019) 7:140 J Immunother Cancer: first published as 10.1186/s40425-019-0622-0 on 28 May 2019. Downloaded from https://doi.org/10.1186/s40425-019-0622-0 RESEARCHARTICLE Open Access Generation of monocyte-derived tumor- associated macrophages using tumor- conditioned media provides a novel method to study tumor-associated macrophages in vitro Brooke Benner1, Luke Scarberry1, Lorena P. Suarez-Kelly2, Megan C. Duggan1, Amanda R. Campbell1, Emily Smith1, Gabriella Lapurga1, Kallie Jiang1, Jonathan P. Butchar1, Susheela Tridandapani1, John Harrison Howard2, Robert A. Baiocchi3, Thomas A. Mace1 and William E. Carson III1,2* Abstract Background: Tumor-associated macrophages (TAM) are expanded and exhibit tumor-promoting properties within the tumor microenvironment. Current methods to study TAM have not been replicated across cancer types and often do not include exogenous growth factors from the tumor, a key factor in TAM differentiation in vivo. Methods: In this study, an in vitro method to generate monocyte- derived TAM using tumor- conditioned media (TCM) and a cytokine cocktail containing IL-4, IL-10, and M-CSF was utilized to study the phenotype, morphology, and function of TAM across multiple cancer types. TCM was generated from two breast cancer cell lines and an Epstein-Barr virus-positive lymphoma cell line. The properties of in vitro generated TAM were compared to in vitro generated M1 and M2- like macrophages and TAM isolated from patients with cancer. Results: TAM generated in this fashion displayed an increase in CD163/CD206 co-expression compared to M2- like http://jitc.bmj.com/ macrophages (87 and 36%, respectively). -

Immune Effector Monocyte–Neutrophil Cooperation Induced by the Primary Tumor Prevents Metastatic Progression of Breast Cancer
Immune effector monocyte–neutrophil cooperation induced by the primary tumor prevents metastatic progression of breast cancer Catharina Hagerlinga,b,1,2, Hugo Gonzaleza,3, Kiarash Salaria,3, Chih-Yang Wanga,4, Charlene Lina, Isabella Roblesa, Merel van Gogha, Annika Dejmekc, Karin Jirströmb, and Zena Werba,d,2 aDepartment of Anatomy, University of California, San Francisco, CA 94143-0452; bDepartment of Clinical Sciences, Division of Clinical Oncology and Pathology, Lund University, SE-221 85 Lund, Sweden; cDepartment of Translational Medicine, Lund University, Malmö SUS, SE-214 21 Malmö, Sweden; and dHelen Diller Family Comprehensive Cancer Center, University of California, San Francisco, CA 94143 Contributed by Zena Werb, August 30, 2019 (sent for review May 3, 2019; reviewed by Yves DeClerck and Mikala Egeblad) Metastatic behavior varies significantly among breast cancers. Mech- patients’ breast cancer tumors and is hence an attractive preclinical anisms explaining why the majorityofbreastcancerpatientsnever model to find novel therapeutic alternatives for metastatic breast develop metastatic outgrowth are largely lacking but could underlie cancer (12). We furthermore validated our PDX-derived findings the development of novel immunotherapeutic target molecules. Here with a large primary breast cancer tissue microarray (TMA), pleural we show interplay between nonmetastatic primary breast cancer effusions from breast cancer patients and an immunocompetent and innate immune response, acting together to control metastatic syngeneic mammary cancer model. Taken together, we reveal in- progression. The primary tumor systemically recruits IFNγ-producing terplay between the primary breast cancer tumor and myeloid im- immune effector monocytes to the lung. IFNγ up-regulates Tmem173/ mune response, acting together to control metastatic progression. -
Audencel Immunotherapy Based on Dendritic Cells Has No Effect on Overall and Progression-Free Survival in Newly Diagnosed Glioblastoma: a Phase II Randomized Trial
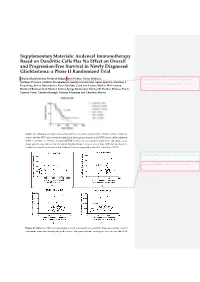
Supplementary Materials: Audencel Immunotherapy Based on Dendritic Cells Has No Effect on Overall and Progression-Free Survival in Newly Diagnosed Glioblastoma: a Phase II Randomized Trial Johanna Buchroithner, Friedrich Erhart, Josef Pichler, Georg Widhalm, Commented [FE1]: Authorship order was changed by Matthias Preusser, Günther Stockhammer, Martha Nowosielski, Sarah Iglseder, Christian F. request from the senior corresponding author – details see Freyschlag, Stefan Oberndorfer, Karin Bordihn, Gord von Campe, Markus Hoffermann, email Reinhard Ruckser, Karl Rössler, Sabine Spiegl-Kreinecker, Michael B. Fischer, Thomas Czech, Carmen Visus, Günther Krumpl, Thomas Felzmann and Christine Marosi Figure S1. Influence of extent-of-resection (EOS) on overall survival (OS). Patients of the Audencel cohort and the SOC cohort were stratified into three groups based on the EOR that could be achieved (100% vs 90-99% vs. 70-90%). A minimal EOR of 70% was an inclusion criterion for the study, so no study patient was below that threshold. Kaplan-Meier analysis shows that EOR did not have an influence on the OS outcome in the Audencel cohort compared to the SOC cohort (p = 0.762). Commented [M2]: “ml” in figure s2a should be changed to “mL” Commented [FE3R2]: I would rather prefer to have “ml” here Figure S2. Relation of DC vaccine quality control and overall survival (OS). One main quality control parameter measured during the production of the personalized, autologous vaccine was the IL-12 production capacity of every single vaccine. When analyzing a possible correlation with OS, no such connection could be made (a, p = 0.891). Similarly, the T cell proliferation capacity of the DC vaccine did not have a connection to survival — for three different DC: T cell ratios tested: 1:5 (b),1:10 (c), 1:20 (d). -

Basophils Trigger Emphysema Development in a Murine Model of COPD Through IL-4–Mediated Generation of MMP-12–Producing Macrophages
Basophils trigger emphysema development in a murine model of COPD through IL-4–mediated generation of MMP-12–producing macrophages Sho Shibataa,b, Kensuke Miyakea, Tomoya Tateishib, Soichiro Yoshikawaa, Yoshinori Yamanishia, Yasunari Miyazakib, Naohiko Inaseb, and Hajime Karasuyamaa,1 aDepartment of Immune Regulation, Graduate School of Medical and Dental Sciences, Tokyo Medical and Dental University (TMDU), Tokyo 113-8510, Japan; and bDepartment of Respiratory Medicine, Graduate School of Medical and Dental Sciences, Tokyo Medical and Dental University (TMDU), Tokyo 113-8510, Japan Edited by Kazuhiko Yamamoto, the University of Tokyo; Max Planck–The University of Tokyo Center for Integrative Inflammology, the University of Tokyo, Tokyo, Japan, and accepted by Editorial Board Member Tadatsugu Taniguchi November 2, 2018 (received for review August 13, 2018) Chronic obstructive pulmonary disease (COPD) is a leading cause of COPD even after smoking has stopped (9). As an alternative morbidity and mortality worldwide. It has generally been consid- approach, a protease-induced model was established (10) soon ered a non-Th2-type lung disorder, characterized by progressive after the discovery of the association between α1-antitrypsin airflow limitation with inflammation and emphysema, but its deficiency and emphysema in humans (11), implying that an im- cellular and molecular mechanism remains ill defined, compared balance between proteases and antiproteases in the lung may re- with that of asthma characterized by reversible airway obstruc- sult in emphysema formation. Intratracheal or intranasal instillation tion. Here we show a previously unappreciated role for basophils of elastolytic enzymes, such as papain, human neutrophil elastase, at the initiation phase of emphysema formation in an elastase- and porcine pancreatic elastase, is utilized to trigger emphysema induced murine model of COPD in that basophils represent less formation (10, 12, 13). -

Understanding the Immune System: How It Works
Understanding the Immune System How It Works U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES NATIONAL INSTITUTES OF HEALTH National Institute of Allergy and Infectious Diseases National Cancer Institute Understanding the Immune System How It Works U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES NATIONAL INSTITUTES OF HEALTH National Institute of Allergy and Infectious Diseases National Cancer Institute NIH Publication No. 03-5423 September 2003 www.niaid.nih.gov www.nci.nih.gov Contents 1 Introduction 2 Self and Nonself 3 The Structure of the Immune System 7 Immune Cells and Their Products 19 Mounting an Immune Response 24 Immunity: Natural and Acquired 28 Disorders of the Immune System 34 Immunology and Transplants 36 Immunity and Cancer 39 The Immune System and the Nervous System 40 Frontiers in Immunology 45 Summary 47 Glossary Introduction he immune system is a network of Tcells, tissues*, and organs that work together to defend the body against attacks by “foreign” invaders. These are primarily microbes (germs)—tiny, infection-causing Bacteria: organisms such as bacteria, viruses, streptococci parasites, and fungi. Because the human body provides an ideal environment for many microbes, they try to break in. It is the immune system’s job to keep them out or, failing that, to seek out and destroy them. Virus: When the immune system hits the wrong herpes virus target or is crippled, however, it can unleash a torrent of diseases, including allergy, arthritis, or AIDS. The immune system is amazingly complex. It can recognize and remember millions of Parasite: different enemies, and it can produce schistosome secretions and cells to match up with and wipe out each one of them. -

Neutrophil and Monocyte Adhesion Molecules in Bronchopulmonary
F76 Arch Dis Child Fetal Neonatal Ed: first published as 10.1136/fn.89.1.F76 on 1 January 2004. Downloaded from ORIGINAL ARTICLE Neutrophil and monocyte adhesion molecules in bronchopulmonary dysplasia, and effects of corticosteroids P Ballabh, M Simm, J Kumari, A N Krauss, A Jain, C Califano, M L Lesser, S Cunningham-Rundles ............................................................................................................................... Arch Dis Child Fetal Neonatal Ed 2004;89:F76–F83 Aims: To study a longitudinal change in the expression of adhesion molecules CD11b, CD18, and CD62L on neutrophils and monocytes in very low birth weight babies who develop respiratory distress syndrome, to compare these levels between bronchopulmonary dysplasia (BPD) and non-BPD infants, and to assess the effect of corticosteroid treatment on these adhesion molecules. See end of article for authors’ affiliations Methods: Of 40 eligible neonates, 11 neonates were oxygen dependent at 36 weeks (BPD 36 weeks), 16 ....................... infants were oxygen dependent at 28 days, but not at 36 weeks (BPD d28), and 13 infants did not develop BPD. Seventeen neonates received a six day course of steroid treatment. Expression of CD11b, CD18, and Correspondence to: Dr P Ballabh, Assistant CD62L was measured on neutrophils and monocytes in arterial blood on days 1, 3, 7, 14, 21, and 28, Professor, Division of and before and 2–3 days after initiation of dexamethasone treatment by flow cytometry. Neonatology, Department Results: CD18 expression on neutrophils and monocytes and CD62L on neutrophils, measured as mean of Pediatrics, NICU, 2nd fluorescent intensity, was significantly decreased in BPD neonates compared to non-BPD neonates on days Floor, Main Building, Westchester Medical 1–28. -

Leukocytosis and Natural Killer Cell Function Parallel Neurobehavioral Fatigue Induced by 64 Hours of Sleep Deprivation
Leukocytosis and natural killer cell function parallel neurobehavioral fatigue induced by 64 hours of sleep deprivation. D F Dinges, … , E Icaza, M T Orne J Clin Invest. 1994;93(5):1930-1939. https://doi.org/10.1172/JCI117184. Research Article The hypothesis that sleep deprivation depresses immune function was tested in 20 adults, selected on the basis of their normal blood chemistry, monitored in a laboratory for 7 d, and kept awake for 64 h. At 2200 h each day measurements were taken of total leukocytes (WBC), monocytes, granulocytes, lymphocytes, eosinophils, erythrocytes (RBC), B and T lymphocyte subsets, activated T cells, and natural killer (NK) subpopulations (CD56/CD8 dual-positive cells, CD16- positive cells, CD57-positive cells). Functional tests included NK cytotoxicity, lymphocyte stimulation with mitogens, and DNA analysis of cell cycle. Sleep loss was associated with leukocytosis and increased NK cell activity. At the maximum sleep deprivation, increases were observed in counts of WBC, granulocytes, monocytes, NK activity, and the proportion of lymphocytes in the S phase of the cell cycle. Changes in monocyte counts correlated with changes in other immune parameters. Counts of CD4, CD16, CD56, and CD57 lymphocytes declined after one night without sleep, whereas CD56 and CD57 counts increased after two nights. No changes were observed in other lymphocyte counts, in proliferative responses to mitogens, or in plasma levels of cortisol or adrenocorticotropin hormone. The physiologic leukocytosis and NK activity increases during deprivation were eliminated by recovery sleep in a manner parallel to neurobehavioral function, suggesting that the immune alterations may be associated with biological pressure for sleep. -

Statistical Analysis Plan
STATISTICAL ANALYSIS PLAN NCT Number: NCT03259334 Study Title: A Phase 3 Randomized, Double-blind, Placebo-controlled, Parallel-group Efficacy and Safety Study of SHP647 as Induction Therapy in Subjects with Moderate to Severe Ulcerative Colitis (FIGARO UC 301) Study Number: SHP647-301 SAP Version and Date: Version 3.0: 04 Nov 2020 STATISTICAL ANALYSIS PLAN SHP647 PHASE 3 A Phase 3 Randomized, Double-blind, Placebo-controlled, Parallel group Efficacy and Safety Study of SHP647 as Induction Therapy in Subjects with Moderate to Severe Ulcerative Colitis (FIGARO UC 301) PROTOCOL IDENTIFIER: SHP647-301 Study Sponsor(s): Shire Human Genetic Therapies, Inc. ("Shire"), 300 Shire Way, Lexington, MA 02421 USA Author: , PPD Protocol: V1 (06 Jul 2017); Amendment 1, 05 Sep 2018; Amendment 2, 11 Nov 2019 SAP Version #: 3.0 SAP Date: For non-commercial04 Nov 2020 use only Status: Final Shire CONFIDENTIAL Page 2 SHP647-301 Statistical Analysis Plan v 3.0 SHP647 04 Nov 2020 REVISION HISTORY Version Issue Date Summary of Changes 1.0 30 Aug 2019 Final 2.0 13 Aug 2020 Incorporated Protocol Amendment 2 Updates. - Added Hypersensitivity AEs. - Changed study treatment name. - Changed sample size calculation. - Changed the term ‘dimension’ to ‘domain’ for IBDQ Domain Scores. - Updated Prior medication definition to remove restriction for stop date. Due to the early discontinuation of the study before full enrollment, previously planned supplementary and subgroup analyses were removed. - Removed Per-protocol Set and Completers Set. - Removed supplementary analyses for efficacy endpoints (per-protocol, completer, missing data assumptions, etc). - Removed subgroup for efficacy endpoints beyond the actual randomization factors. -

Eosinophil-To-Monocyte Ratio Is a Potential Predictor of Prognosis in Acute Ischemic Stroke Patients After Intravenous Thrombolysis
Clinical Interventions in Aging Dovepress open access to scientific and medical research Open Access Full Text Article ORIGINAL RESEARCH Eosinophil-to-Monocyte Ratio is a Potential Predictor of Prognosis in Acute Ischemic Stroke Patients After Intravenous Thrombolysis Yueping Chen1,* Background: Eosinophil and monocyte have been demonstrated separately to be indepen Junli Ren2,3,* dent predictors of acute ischemic stroke (AIS). This study aimed to evaluate the association Naiping Yang2,3,* between eosinophil-to-monocyte ratio (EMR) and 3-month clinical outcome after treatment Honghao Huang2,3 with recombinant tissue plasminogen activator (rt-PA) for AIS patients. Simultaneously, we Xueting Hu2,3 made a simple comparison with other prognostic indicators, such as 24h neutrophil-to- lymphocyte ratio (NLR) and 24h platelet-to-lymphocyte ratio (PLR) to investigate the Fangyue Sun2,3 prognostic value of EMR. Tian Zeng2,3 2,3 Methods and Results: A total of 280 AIS patients receiving intravenous thrombolysis were Xinbo Zhou retrospectively recruited for this study. Complete blood count evaluations for EMR were 2,3 Wenjing Pan conducted on 24 hours admission. The poor outcome at 3-month was defined as the modified 2,3 Jingyu Hu Rankin Scale (mRS) of 3–6 and the mRS score for death was 6. The EMR levels in patients 4 Beibei Gao with AIS were lower than those in the healthy controls and showed a negative correlation 2 Shunkai Zhang with the NIHSS score. At the 3-month follow-up, multivariate logistic regression analysis Guangyong Chen 2 indicated an association among EMR, poor outcome and mortality. In addition, EMR had a higher predictive ability than popular biomarkers like NLR and PLR for 3-month mortality. -

The Evolving Roles of Cardiac Macrophages in Homeostasis, Regeneration, and Repair
International Journal of Molecular Sciences Review The Evolving Roles of Cardiac Macrophages in Homeostasis, Regeneration, and Repair Santiago Alvarez-Argote 1,2 and Caitlin C. O’Meara 1,2,3,* 1 Department of Physiology, Medical College of Wisconsin, Milwaukee, WI 53226, USA; [email protected] 2 Cardiovascular Center, Medical College of Wisconsin, Milwaukee, WI 53226, USA 3 Genomics Sciences and Precision Medicine Center, Medical College of Wisconsin, Milwaukee, WI 53226, USA * Correspondence: [email protected] Abstract: Macrophages were first described as phagocytic immune cells responsible for maintain- ing tissue homeostasis by the removal of pathogens that disturb normal function. Historically, macrophages have been viewed as terminally differentiated monocyte-derived cells that originated through hematopoiesis and infiltrated multiple tissues in the presence of inflammation or during turnover in normal homeostasis. However, improved cell detection and fate-mapping strategies have elucidated the various lineages of tissue-resident macrophages, which can derive from embryonic origins independent of hematopoiesis and monocyte infiltration. The role of resident macrophages in organs such as the skin, liver, and the lungs have been well characterized, revealing functions well beyond a pure phagocytic and immunological role. In the heart, recent research has begun to decipher the functional roles of various tissue-resident macrophage populations through fate mapping and genetic depletion studies. Several of these studies have elucidated the novel and unex- pected roles of cardiac-resident macrophages in homeostasis, including maintaining mitochondrial function, facilitating cardiac conduction, coronary development, and lymphangiogenesis, among others. Additionally, following cardiac injury, cardiac-resident macrophages adopt diverse functions Citation: Alvarez-Argote, S.; such as the clearance of necrotic and apoptotic cells and debris, a reduction in the inflammatory O’Meara, C.C. -

Appendix 1 – Protocol for Preventing Or Reversing Chronic Disease The
Appendix 1 – Protocol for Preventing or Reversing Chronic Disease The first author has developed a protocol over the past decade for preventing or reversing chronic disease based on the following systemic medical principle: “at the present time, removal of cause is a necessary, but not necessarily sufficient, condition for restorative treatment to be effective”[1]. The protocol methodology refines the age-old principles of both reducing harm in addition to providing treatment, and allows better identification of factors that contribute to the disease process (so that they may be eliminated if possible). These contributing factors are expansive and may include a combination of Lifestyle choices (diet, exercise, smoking), iatrogenic and biotoxin exposures, environmental/occupational exposures, and psychosocial stressors. This strategy exploits the existing literature to identify patterns of biologic response using biomarkers from various modalities of diagnostic testing to capture a much broader list of potential contributing factors. Existing inflammatory bowel diseases (IBD) Biomarker Identification to Remove Contributing Factors and Implement Treatment The initial protocol steps are diagnostic. The main output of these diagnostics will be identification of the biomarker levels and symptoms that reflect abnormalities, and the directions of change required to eliminate these abnormalities. In the present study, hundreds of general and specific biomarkers and symptoms were identified from the core IBD literature. The highest frequency (based on numbers of record appearances) biomarkers and symptoms were extracted, and are listed in Table 1 (highest frequency items first, reading down each column before proceeding to the next column). They are not necessarily consensus biomarkers. They are biomarkers whose values were altered by a treatment or contributing factor, and reported in the core IBD literature.