Clinical Spectrum Ofstx1b-Related Epileptic Disorders
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

1 ILAE Classification & Definition of Epilepsy Syndromes in the Neonate
ILAE Classification & Definition of Epilepsy Syndromes in the Neonate and Infant: Position Statement by the ILAE Task Force on Nosology and Definitions Authors: Sameer M Zuberi1, Elaine Wirrell2, Elissa Yozawitz3, Jo M Wilmshurst4, Nicola Specchio5, Kate Riney6, Ronit Pressler7, Stephane Auvin8, Pauline Samia9, Edouard Hirsch10, O Carter Snead11, Samuel Wiebe12, J Helen Cross13, Paolo Tinuper14,15, Ingrid E Scheffer16, Rima Nabbout17 1. Paediatric Neurosciences Research Group, Royal Hospital for Children & Institute of Health & Wellbeing, University of Glasgow, Member of European Reference Network EpiCARE, Glasgow, UK. 2. Divisions of Child and Adolescent Neurology and Epilepsy, Department of Neurology, Mayo Clinic, Rochester MN, USA. 3. Isabelle Rapin Division of Child Neurology of the Saul R Korey Department of Neurology, Montefiore Medical Center, Bronx, NY USA. 4. Department of Paediatric Neurology, Red Cross War Memorial Children’s Hospital, Neuroscience Institute, University of Cape Town, South Africa. 5. Rare and Complex Epilepsy Unit, Department of Neuroscience, Bambino Gesu’ Children’s Hospital, IRCCS, Member of European Reference Network EpiCARE, Rome, Italy 6. Neurosciences Unit, Queensland Children's Hospital, South Brisbane, Queensland, Australia. Faculty of Medicine, University of Queensland, Queensland, Australia. 7. Clinical Neuroscience, UCL- Great Ormond Street Institute of Child Health, London, UK. Department of Clinical Neurophysiology, Great Ormond Street Hospital for Children NHS Foundation Trust, Member of European Reference Network EpiCARE London, UK 8. Université de Paris, AP-HP, Hôpital Robert-Debré, INSERM NeuroDiderot, DMU Innov-RDB, Neurologie Pédiatrique, Member of European Reference Network EpiCARE, Paris, France. 9. Department of Paediatrics and Child Health, Aga Khan University, East Africa. 1 10. Neurology Epilepsy Unit “Francis Rohmer”, INSERM 1258, FMTS, Strasbourg University, France. -

Genome-Wide Rnai Screens Identify Genes Required for Ricin and PE Intoxications
Developmental Cell Article Genome-Wide RNAi Screens Identify Genes Required for Ricin and PE Intoxications Dimitri Moreau,1 Pankaj Kumar,1 Shyi Chyi Wang,1 Alexandre Chaumet,1 Shin Yi Chew,1 He´ le` ne Chevalley,1 and Fre´ de´ ric Bard1,* 1Institute of Molecular and Cell Biology, 61 Biopolis Drive, Proteos, Singapore 138673, Singapore *Correspondence: [email protected] DOI 10.1016/j.devcel.2011.06.014 SUMMARY In the lumen of the ER, these toxins are thought to interact with elements of the ER-associated degradation (ERAD) pathway, Protein toxins such as Ricin and Pseudomonas which targets misfolded proteins in the ER for degradation. exotoxin (PE) pose major public health challenges. This interaction is proposed to allow translocation to the cytosol Both toxins depend on host cell machinery for inter- without resulting in toxin degradation (Johannes and Ro¨ mer, nalization, retrograde trafficking from endosomes 2010). to the ER, and translocation to cytosol. Although Obviously, this complex set of membrane-trafficking and both toxins follow a similar intracellular route, it is membrane-translocation events involves many host proteins, some of which have already been described (Johannes and unknown how much they rely on the same genes. Ro¨ mer, 2010; Sandvig et al., 2010). Altering the function of these Here we conducted two genome-wide RNAi screens host proteins could in theory provide a toxin antidote. identifying genes required for intoxication and Consistently, inhibition of retrograde traffic by drugs such as demonstrating that requirements are strikingly Brefeldin A (Sandvig et al., 1991)(Yoshida et al., 1991) or Golgi- different between PE and Ricin, with only 13% over- cide A (Sa´ enz et al., 2009) and Retro-1 and 2 (Stechmann et al., lap. -

Focus on Pregnancy: Vitamin K, Folic Acid
Practice Parameter update: Management issues for women with epilepsy−−Focus on pregnancy (an evidence-based review): Vitamin K, folic acid, blood levels, and breastfeeding: Report of the Quality Standards Subcommittee and Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology and American Epilepsy Society C. L. Harden, P. B. Pennell, B. S. Koppel, et al. Neurology 2009;73;142-149 Published Online before print April 27, 2009 DOI 10.1212/WNL.0b013e3181a6b325 This information is current as of April 27, 2009 The online version of this article, along with updated information and services, is located on the World Wide Web at: http://www.neurology.org/content/73/2/142.full.html Neurology ® is the official journal of the American Academy of Neurology. Published continuously since 1951, it is now a weekly with 48 issues per year. Copyright . All rights reserved. Print ISSN: 0028-3878. Online ISSN: 1526-632X. SPECIAL ARTICLE Practice Parameter update: Management issues for women with epilepsy—Focus on pregnancy (an evidence-based review): Vitamin K, folic acid, blood levels, and breastfeeding Report of the Quality Standards Subcommittee and Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology and American Epilepsy Society C.L. Harden, MD ABSTRACT P.B. Pennell, MD Objective: To reassess the evidence for management issues related to the care of women with B.S. Koppel, MD epilepsy (WWE) during pregnancy, including preconceptional folic acid use, prenatal vitamin K C.A. Hovinga, PharmD use, risk of hemorrhagic disease of the newborn, clinical implications of placental and breast B. Gidal, PharmD milk transfer of antiepileptic drugs (AEDs), risks of breastfeeding, and change in AED levels K.J. -

ICTALS2019 the Epilepsy Journey
ICTALS2019 The Epilepsy Journey 2-5 September In partnership with Abstract book This conference is supported by a grant from the American Epilepsy Society ICTALS2019 The Epilepsy Journey Foreword The International Conference for Technology and Analysis of Seizures, 2019 (ICTALS2019) aims to bring together neurologists, neuroscientists, researchers from quantitative disciplines and people with lived experience of epilepsy in order to work as a community to advance our understanding of epilepsy and develop practical ways to improve diagnosis and treatment. The theme for this year’s conference is: The Epilepsy Journey: from first seizure to treatment and beyond. We will emphasise how advances in our understanding of the dynamics of brain networks can be used to make a difference to people with epilepsy at all points of their journey: from elucidating the causes of the first seizure to diagnosing epilepsy, understanding how ictogenic networks give rise to recurrent seizures and how this insight can inform personalised treatment. To encourage this focus on the whole epilepsy journey we seek to include all relevant communities. In addition to discussions on current scientific, clinical and technological advances, we will take steps to increase accessibility for people with lived experience of epilepsy. Dates: Monday 2 September 2019 - Thursday 5 September 2019 Venue: University of Exeter, Streatham Campus, Xfi Building Conference website: http://ex.ac.uk/ictals2019 Contact the organisers: [email protected] ICTALS2019 The Epilepsy Journey Partners We are partnering with charities Epilepsy Research UK and Epilepsy Action and Alliance for Epilepsy Research. Sponsors This event would not be possible without the generous contributions from our generous sponsors UCB, the Epilepsy Foundation, NeuraLynx, and Liva Nova. -

Fundraising Financial Summar
Chairman’s Report research arena. In March 2012, I would like to take this opportunity we organised our ninth international to thank Samantha Cameron for MY FIRST 12 MONTHS AS CHAIR It was always our ambition to mark workshop entitled ‘Why do some graciously hosting the Epilepsy OF EPILEPSY RESEARCH UK HAVE the 20th anniversary of Epilepsy brains seize? Molecular, cellular and Research UK reception at 10 Downing COINCIDED WITH OUR 20TH Research UK with a grant round of network mechanisms’ where fifty Street in May 2012 that rounded off our ANNIVERSARY AND OUR MOST this magnitude, but to have realised experts from around the world anniversary year. This event, together SUCCESSFUL YEAR TO DATE. it in the current economic climate is a gathered to consider the key with the Gala Ball in October 2011, Credit for that goes to my tremendous achievement. This success differences between normal were highlights of a momentous twelve predecessor as Chair, Professor Helen allowed us to fund five new project functioning brains and those that months for Epilepsy Research UK, with Cross, for her excellent stewardship grants, two fellowship grants and one periodically exhibit spontaneous both well attended by our loyal and of the charity over the past six years, project grant extension at a total cost of seizures. The proceedings of the committed supporters. We owe a huge the staff of Epilepsy Research UK for £1,189,332. As always, these awards workshop will be published in debt of gratitude to our supporters for a continuing dedication to the cause their continuing hard work, and the covered a broad spectrum of research the highly prestigious Journal of of epilepsy research that has enabled remarkable efforts of our donors and focused on the causes, prevention and Physiology later in the year. -

Paediatric Epilepsy Research Report 2019
Paediatric Epilepsy 2019 Research Report Inside Who we are The organisations and experts behind our research programme What we do Our strategy, projects and impact youngepilepsy.org.uk Contents Introduction 1 Who we are 2 Research Partners 2 Research Funding 4 Research Team 5 What we do 10 Programme Strategy 10 The MEG Project 12 New Research Projects 14 Research Project Update 21 Completed Projects 32 Awarded PhDs 36 Paediatric Epilepsy Masterclass 2018 37 Paediatric Epilepsy Research Retreat 2019 38 Research Publications 40 Unit Roles 47 Unit Roles in Education 49 Professional Recognition and Awards 50 Paediatric Epilepsy Research Report 2019 Introduction I am delighted to present our annual research report for the period July 2018 to June 2019 for the paediatric epilepsy research unit across Young Epilepsy, UCL GOS - Institute of Child Health and Great Ormond Street Hospital for Children. We have initiated 13 new research projects, adding to 20 active projects spanning the clinical, educational and social elements of paediatric epilepsy. We have published 110 peer-reviewed items of primary research and a further 54 chapters in books, reviews and commentaries of expert opinion. During this period, Young Epilepsy Chief Executive Carol Long caught the research bug and moved on to begin her PhD at Durham University. We welcomed our new Chief Executive, Mark Devlin at our Paediatric Epilepsy Research Retreat in January 2019. As an organisation, we are launching a new strategy This report features a spotlight on a truly which sets our research programme as one of innovative project which will change the UK’s the four key offers at Young Epilepsy, and we diagnostic and surgical evaluation imaging suite look forward to sharing our research more widely for childhood epilepsy. -

Regular Article
From www.bloodjournal.org by guest on April 6, 2015. For personal use only. Regular Article IMMUNOBIOLOGY Hemophagocytic lymphohistiocytosis caused by dominant-negative mutations in STXBP2 that inhibit SNARE-mediated membrane fusion Waldo A. Spessott,1 Maria L. Sanmillan,1 Margaret E. McCormick,1 Nishant Patel,2 Joyce Villanueva,3 Kejian Zhang,4 Kim E. Nichols,5 and Claudio G. Giraudo1 1Department of Pathology and Laboratory Medicine, and 2Division of Oncology, Department of Pediatrics, The Children’s Hospital of Philadelphia, University of Pennsylvania, Philadelphia, PA; 3Division of Bone Marrow Transplant and Immune Deficiency, and 4Division of Human Genetics, Cincinnati Children’s Hospital Medical Center, Department of Pediatrics, University of Cincinnati College of Medicine, Cincinnati, OH; and 5Division of Cancer Predisposition, Department of Oncology, St. Jude Children’s Research Hospital, Memphis, TN Key Points Familial hemophagocytic lymphohistiocytosis (F-HLH) and Griscelli syndrome type 2 (GS) are life-threatening immunodeficiencies characterized by impaired cytotoxic T lymphocyte • Monoallelic STXBP2 mutations (CTL) and natural killer (NK) cell lytic activity. In the majority of cases, these disorders are affecting codon 65 impair caused by biallelic inactivating germline mutations in genes such as RAB27A (GS) and PRF1, lymphocyte cytotoxicity and UNC13D, STX11,andSTXBP2 (F-HLH). Although monoallelic (ie, heterozygous) mutations contribute to hemophagocytic have been identified in certain patients, the clinical significance and molecular mechanisms lymphohistiocytosis. by which these mutations influence CTL and NK cell function remain poorly understood. • Munc18-2R65Q/W mutant Here, we characterize 2 novel monoallelic hemophagocytic lymphohistiocytosis (HLH)- associated mutations affecting codon 65 of STXPB2, the gene encoding Munc18-2, a member proteins function in a dominant- of the SEC/MUNC18 family. -
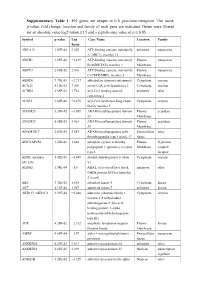
Supplementary Table 1
Supplementary Table 1. 492 genes are unique to 0 h post-heat timepoint. The name, p-value, fold change, location and family of each gene are indicated. Genes were filtered for an absolute value log2 ration 1.5 and a significance value of p ≤ 0.05. Symbol p-value Log Gene Name Location Family Ratio ABCA13 1.87E-02 3.292 ATP-binding cassette, sub-family unknown transporter A (ABC1), member 13 ABCB1 1.93E-02 −1.819 ATP-binding cassette, sub-family Plasma transporter B (MDR/TAP), member 1 Membrane ABCC3 2.83E-02 2.016 ATP-binding cassette, sub-family Plasma transporter C (CFTR/MRP), member 3 Membrane ABHD6 7.79E-03 −2.717 abhydrolase domain containing 6 Cytoplasm enzyme ACAT1 4.10E-02 3.009 acetyl-CoA acetyltransferase 1 Cytoplasm enzyme ACBD4 2.66E-03 1.722 acyl-CoA binding domain unknown other containing 4 ACSL5 1.86E-02 −2.876 acyl-CoA synthetase long-chain Cytoplasm enzyme family member 5 ADAM23 3.33E-02 −3.008 ADAM metallopeptidase domain Plasma peptidase 23 Membrane ADAM29 5.58E-03 3.463 ADAM metallopeptidase domain Plasma peptidase 29 Membrane ADAMTS17 2.67E-04 3.051 ADAM metallopeptidase with Extracellular other thrombospondin type 1 motif, 17 Space ADCYAP1R1 1.20E-02 1.848 adenylate cyclase activating Plasma G-protein polypeptide 1 (pituitary) receptor Membrane coupled type I receptor ADH6 (includes 4.02E-02 −1.845 alcohol dehydrogenase 6 (class Cytoplasm enzyme EG:130) V) AHSA2 1.54E-04 −1.6 AHA1, activator of heat shock unknown other 90kDa protein ATPase homolog 2 (yeast) AK5 3.32E-02 1.658 adenylate kinase 5 Cytoplasm kinase AK7 -

Seizure: European Journal of Epilepsy 83 (2020) 70–75
Seizure: European Journal of Epilepsy 83 (2020) 70–75 Contents lists available at ScienceDirect Seizure: European Journal of Epilepsy journal homepage: www.elsevier.com/locate/seizure Review Redefining the role of Magnetoencephalography in refractory epilepsy Umesh Vivekananda 1 Department of Clinical and Experimental Epilepsy, Institute of Neurology, Queen Square, UCL, WC1N 3BG, United Kingdom ARTICLE INFO ABSTRACT Keywords: Magnetoencephalography (MEG) possesses a number of features, including excellent spatiotemporal resolution, magnetoencephalography that lend itself to the functional imaging of epileptic activity. However its current use is restricted to specific electroencephalograph scenarios, namely in the diagnosis refractory focal epilepsies where electroencephalography (EEG) has been source localisation inconclusive. This review highlights the recent progress of MEG within epilepsy, including advances in the OPMs technique itself such as simultaneous EEG/MEG and intracranial EEG/MEG recording and room temperature MEG recording using optically pumped magnetometers, as well as improved post processing of the data during interictal and ictal activity for accurate source localisation of the epileptogenic focus. These advances should broaden the scope of MEG as an important part of epilepsy diagnostics in the future. 1. Introduction one large study of 1000 consecutive cases of refractory focal epilepsy demonstrated that MEG provided additional information to existing pre- A mainstay in epilepsy diagnostics over the last century has been the surgical methods (including scalp EEG, single photon emission electroencephalogram or EEG. Simply explained, EEG records electrical computed tomography (SPECT) and MRI) in 32% of cases, and complete currents reflecting synchronous neuronal activity attributable to the magnetoencephalography resection was associated with significantly brain surface, and can identify abnormal activity related to epilepsy with higher chances to achieve seizure freedom in the short and long-term good temporal resolution. -

Syntaxin Binding Mechanism and Disease-Causing Mutations In
Syntaxin binding mechanism and disease-causing PNAS PLUS mutations in Munc18-2 Yvonne Hackmanna, Stephen C. Grahama,1,2, Stephan Ehlb, Stefan Höningc, Kai Lehmbergd, Maurizio Aricòe, David J. Owena, and Gillian M. Griffithsa,2 aCambridge Institute for Medical Research, University of Cambridge Biomedical Campus, University of Cambridge, Cambridge CB2 0XY, United Kingdom; bCentre of Chronic Immunodeficiency, 79106 Freiburg, Germany; cInstitute for Biochemistry I and Center for Molecular Medicine Cologne, University of Cologne, 50931 Cologne, Germany; dDepartment of Paediatric Haematology and Oncology, University Medical Center Hamburg Eppendorf, 20246 Hamburg, Germany; and ePediatric Hematology Oncology Network, Istituto Toscana Tumori, 50139 Florence, Italy Edited* by Peter Cresswell, Yale University School of Medicine, New Haven, CT, and approved October 11, 2013 (received for review July 18, 2013) Mutations in either syntaxin 11 (Stx11) or Munc18-2 abolish Munc18-2 belongs to the Sec1/Munc18-like (SM) protein cytotoxic T lymphocytes (CTL) and natural killer cell (NK) cytotox- family, whose members are all ∼600 residues long and are in- icity, and give rise to familial hemophagocytic lymphohistiocytosis volved in regulation of SNARE-mediated membrane fusion (FHL4 or FHL5, respectively). Although Munc18-2 is known to events (9, 10). The two closest homologs of Munc18-2 are interact with Stx11, little is known about the molecular mecha- Munc18-1, which is crucial for neurotransmitter secretion in nisms governing the specificity of this interaction or how in vitro neurons (11, 12), and Munc18-3, which is more widely expressed IL-2 activation leads to compensation of CTL and NK cytotoxicity. and is involved in Glut4 translocation (13). -

A Computational Biomarker of Idiopathic Generalized
University of Birmingham A computational biomarker of idiopathic generalized epilepsy from resting state EEG Schmidt, H.; Woldman, W.; Goodfellow, M.; Chowdhury, F.A.; Koutroumanidis, M.; Jewell, S.; Richardson, M.P.; Terry, J.R. DOI: 10.1111/epi.13481 License: Creative Commons: Attribution (CC BY) Document Version Publisher's PDF, also known as Version of record Citation for published version (Harvard): Schmidt, H, Woldman, W, Goodfellow, M, Chowdhury, FA, Koutroumanidis, M, Jewell, S, Richardson, MP & Terry, JR 2016, 'A computational biomarker of idiopathic generalized epilepsy from resting state EEG', Epilepsia, vol. 57, pp. e200-e204. https://doi.org/10.1111/epi.13481 Link to publication on Research at Birmingham portal Publisher Rights Statement: Schmidt, H. , Woldman, W. , Goodfellow, M. , Chowdhury, F. A., Koutroumanidis, M. , Jewell, S. , Richardson, M. P. and Terry, J. R. (2016), A computational biomarker of idiopathic generalized epilepsy from resting state EEG. Epilepsia, 57: e200-e204. doi:10.1111/epi.13481 General rights Unless a licence is specified above, all rights (including copyright and moral rights) in this document are retained by the authors and/or the copyright holders. The express permission of the copyright holder must be obtained for any use of this material other than for purposes permitted by law. •Users may freely distribute the URL that is used to identify this publication. •Users may download and/or print one copy of the publication from the University of Birmingham research portal for the purpose of private study or non-commercial research. •User may use extracts from the document in line with the concept of ‘fair dealing’ under the Copyright, Designs and Patents Act 1988 (?) •Users may not further distribute the material nor use it for the purposes of commercial gain. -

Download of the Event Diaries Database for Future Research
JMIR RESEARCH PROTOCOLS Biondi et al Protocol Remote and Long-Term Self-Monitoring of Electroencephalographic and Noninvasive Measurable Variables at Home in Patients With Epilepsy (EEG@HOME): Protocol for an Observational Study Andrea Biondi1, MSc; Petroula Laiou1, PhD; Elisa Bruno1, MD, PhD; Pedro F Viana1,2, MSc, MD; Martijn Schreuder3, PhD; William Hart4, PhD; Ewan Nurse4,5, PhD; Deb K Pal1, PhD; Mark P Richardson1, BMBCh, PhD 1Institute of Psychiatry, Psychology & Neuroscience, King©s College London, London, United Kingdom 2Faculty of Medicine, University of Lisbon, Hospital de Santa Maria, Lisbon, Portugal 3ANT Neuro UK, Ltd, Stevenage, United Kingdom 4Seer Medical Inc, Melbourne, Australia 5Department of Medicine, St. Vincent's Hospital Melbourne, The University of Melbourne, Melbourne, Australia Corresponding Author: Andrea Biondi, MSc Institute of Psychiatry, Psychology & Neuroscience King©s College London 5 Cutcombe Rd London, SE5 9RT United Kingdom Phone: 44 7753986485 Email: [email protected] Abstract Background: Epileptic seizures are spontaneous events that severely affect the lives of patients due to their recurrence and unpredictability. The integration of new wearable and mobile technologies to collect electroencephalographic (EEG) and extracerebral signals in a portable system might be the solution to prospectively identify times of seizure occurrence or propensity. The performances of several seizure detection devices have been assessed by validated studies, and patient perspectives on wearables have been explored to better match their needs. Despite this, there is a major gap in the literature on long-term, real-life acceptability and performance of mobile technology essential to managing chronic disorders such as epilepsy. Objective: EEG@HOME is an observational, nonrandomized, noninterventional study that aims to develop a new feasible procedure that allows people with epilepsy to independently, continuously, and safely acquire noninvasive variables at home.