Osteogenesis Imperfecta
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Differential Diagnosis: Brittle Bone Conditions Other Than OI
Facts about Osteogenesis Imperfecta Differential Diagnosis: Brittle Bone Conditions Other than OI Fragile bones are the hallmark feature of osteogenesis imperfecta (OI). The mutations that cause OI lead to abnormalities within bone that result in increased bone turnover; reduced bone mineral content and decreased bone mineral density. The consequence of these changes is brittle bones that fracture easily. But not all cases of brittle bones are OI. Other causes of brittle bones include osteomalacia, disuse osteoporosis, disorders of increased bone density, defects of bone, and tumors. The following is a list of conditions that share fragile or brittle bones as a distinguishing feature. Brief descriptions and sources for further information are included. Bruck Syndrome This autosomal recessive disorder is also referred to as OI with contractures. Some people now consider this to be a type of OI. National Library of Medicine Genetics Home Reference: http://ghr.nlm.nih.gov Ehlers-Danlos Syndrome (EDS) Joint hyperextensibility with fractures; this is a variable disorder caused by several gene mutations. Ehlers-Danlos National Foundation http://www.ednf.org Fibrous Dysplasia Fibrous tissue develops in place of normal bone. This weakens the affected bone and causes it to deform or fracture. Fibrous Dysplasia Foundation: https://www.fibrousdysplasia.org Hypophosphatasia This autosomal recessive disorder affects the development of bones and teeth through defects in skeletal mineralization. Soft Bones: www.softbones.org; National Library of Medicine Genetics Home Reference: http://ghr.nlm.nih.gov/condition Idiopathic Juvenile Osteoporosis A non-hereditary transient form of childhood osteoporosis that is similar to mild OI (Type I) National Osteoporosis Foundation: www.nof.org McCune-Albright Syndrome This disorder affects the bones, skin, and several hormone-producing tissues. -

Searching the Genomes of Inbred Mouse Strains for Incompatibilities That Reproductively Isolate Their Wild Relatives
Journal of Heredity 2007:98(2):115–122 ª The American Genetic Association. 2007. All rights reserved. doi:10.1093/jhered/esl064 For permissions, please email: [email protected]. Advance Access publication January 5, 2007 Searching the Genomes of Inbred Mouse Strains for Incompatibilities That Reproductively Isolate Their Wild Relatives BRET A. PAYSEUR AND MICHAEL PLACE From the Laboratory of Genetics, University of Wisconsin, Madison, WI 53706. Address correspondence to the author at the address above, or e-mail: [email protected]. Abstract Identification of the genes that underlie reproductive isolation provides important insights into the process of speciation. According to the Dobzhansky–Muller model, these genes suffer disrupted interactions in hybrids due to independent di- vergence in separate populations. In hybrid populations, natural selection acts to remove the deleterious heterospecific com- binations that cause these functional disruptions. When selection is strong, this process can maintain multilocus associations, primarily between conspecific alleles, providing a signature that can be used to locate incompatibilities. We applied this logic to populations of house mice that were formed by hybridization involving two species that show partial reproductive isolation, Mus domesticus and Mus musculus. Using molecular markers likely to be informative about species ancestry, we scanned the genomes of 1) classical inbred strains and 2) recombinant inbred lines for pairs of loci that showed extreme linkage disequi- libria. By using the same set of markers, we identified a list of locus pairs that displayed similar patterns in both scans. These genomic regions may contain genes that contribute to reproductive isolation between M. domesticus and M. -

Absence of the ER Cation Channel TMEM38B/TRIC-B Disrupts Intracellular Calcium Homeostasis and Dysregulates Collagen Synthesis in Recessive Osteogenesis Imperfecta
RESEARCH ARTICLE Absence of the ER Cation Channel TMEM38B/TRIC-B Disrupts Intracellular Calcium Homeostasis and Dysregulates Collagen Synthesis in Recessive Osteogenesis Imperfecta Wayne A. Cabral1, Masaki Ishikawa2¤a, Matthias Garten3, Elena N. Makareeva4, Brandi M. Sargent1, MaryAnn Weis5, Aileen M. Barnes1, Emma A. Webb6,7, Nicholas J. Shaw7, Leena Ala-Kokko8, Felicitas L. Lacbawan9¤b, Wolfgang Högler6,7, Sergey Leikin4, Paul a11111 S. Blank3, Joshua Zimmerberg3, David R. Eyre5, Yoshihiko Yamada2, Joan C. Marini1* 1 Section on Heritable Disorders of Bone and Extracellular Matrix, NICHD, NIH, Bethesda, Maryland, United States of America, 2 Molecular Biology Section, NIDCR, NIH, Bethesda, Maryland, United States of America, 3 Section on Integrative Biophysics, NICHD, NIH, Bethesda, Maryland, United States of America, 4 Section on Physical Biochemistry, NICHD, NIH, Bethesda, Maryland, United States of America, 5 Department of Orthopaedics and Sports Medicine, University of Washington, Seattle, Washington, United States of America, 6 School of Clinical and Experimental Medicine, Institute of Biomedical Research, OPEN ACCESS University of Birmingham, Birmingham, United Kingdom, 7 Department of Endocrinology and Diabetes, Birmingham Children’s Hospital, Birmingham, United Kingdom, 8 Connective Tissue Gene Tests, Allentown, Citation: Cabral WA, Ishikawa M, Garten M, Pennsylvania, United States of America, 9 Department of Medical Genetics, Children’s National Medical Makareeva EN, Sargent BM, Weis M, et al. (2016) Center, Washington D.C., United States of America Absence of the ER Cation Channel TMEM38B/TRIC- B Disrupts Intracellular Calcium Homeostasis and ¤a Current address: Department of Restorative Dentistry, Division of Operative Dentistry, Tohoku University, Dysregulates Collagen Synthesis in Recessive Graduate School of Dentistry, Sendai, Japan ¤ Osteogenesis Imperfecta. -

Genetic Causes and Underlying Disease Mechanisms in Early-Onset Osteoporosis
From DEPARTMENT OF MOLECULAR MEDICINE AND SURGERY Karolinska Institutet, Stockholm, Sweden GENETIC CAUSES AND UNDERLYING DISEASE MECHANISMS IN EARLY-ONSET OSTEOPOROSIS ANDERS KÄMPE Stockholm 2020 All previously published papers were reproduced with permission from the publisher. Published by Karolinska Institutet. Printed by Eprint AB 2020 © Anders Kämpe, 2020 ISBN 978-91-7831-759-2 Genetic causes and underlying disease mechanisms in early-onset osteoporosis THESIS FOR DOCTORAL DEGREE (Ph.D.) By Anders Kämpe Principal Supervisor: Opponent: Professor Outi Mäkitie Professor André Uitterlinden Karolinska Institutet Erasmus Medical Centre, Rotterdam Department of Molecular Medicine and Surgery Department of Internal Medicine Laboratories Genetic Laboratory / Human Genomics Facility (HuGe-F) Co-supervisor(s): Examination Board: Associate Professor Anna Lindstrand Professor Marie-Louise Bondeson Karolinska Institutet Uppsala University Department of Molecular Medicine and Surgery Department of Immunology, Genetics and Pathology Associate Professor Giedre Grigelioniene Professor Göran Andersson Karolinska Institutet Karolinska Institutet Department of Molecular Medicine and Surgery Department of Laboratory Medicine Professor Ann Nordgren Minna Pöyhönen Karolinska Institutet University of Helsinki Department of Molecular Medicine and Surgery Department of Medical Genetics Associate Professor Hong Jiao Karolinska Institutet Department of Biosciences and Nutrition ABSTRACT Adult-onset osteoporosis is a disorder that affects a significant proportion of the elderly population worldwide and entails a substantial disease burden for the affected individuals. Childhood-onset osteoporosis is a rare condition often associating with a severe bone disease and recurrent fractures already in early childhood. Both childhood-onset and adult-onset osteoporosis have a large genetic component, but in children the disorder is usually genetically less complex and often caused by a single gene variant. -

Skeletal Dysplasias
Skeletal Dysplasias North Carolina Ultrasound Society Keisha L.B. Reddick, MD Wilmington Maternal Fetal Medicine Development of the Skeleton • 6 weeks – vertebrae • 7 weeks – skull • 8 wk – clavicle and mandible – Hyaline cartilage • Ossification – 7-12 wk – diaphysis appears – 12-16 wk metacarpals and metatarsals – 20+ wk pubis, calus, calcaneus • Visualization of epiphyseal ossification centers Epidemiology • Overall 9.1 per 1000 • Lethal 1.1 per 10,000 – Thanatophoric 1/40,000 – Osteogenesis Imperfecta 0.18 /10,000 – Campomelic 0.1 /0,000 – Achondrogenesis 0.1 /10,000 • Non-lethal – Achondroplasia 15 in 10,000 Most Common Skeletal Dysplasia • Thantophoric dysplasia 29% • Achondroplasia 15% • Osteogenesis imperfecta 14% • Achondrogenesis 9% • Campomelic dysplasia 2% Definition/Terms • Rhizomelia – proximal segment • Mezomelia –intermediate segment • Acromelia – distal segment • Micromelia – all segments • Campomelia – bowing of long bones • Preaxial – radial/thumb or tibial side • Postaxial – ulnar/little finger or fibular Long Bone Segments Counseling • Serial ultrasound • Genetic counseling • Genetic testing – Amniocentesis • Postnatal – Delivery center – Radiographs Assessment • Which segment is affected • Assessment of distal extremities • Any curvatures, fracture or clubbing noted • Are metaphyseal changes present • Hypoplastic or absent bones • Assessment of the spinal canal • Assessment of thorax. Skeletal Dysplasia Lethal Non-lethal • Thanatophoric • Achondroplasia • OI type II • OI type I, III, IV • Achondrogenesis • Hypochondroplasia -

Fetal Skeletal Dysplasias
There’s a Short Long Bone, What Now? Fetal Skeletal Dysplasias TERRY HARPER, MD DIVISION CHIEF CLINICAL ASSOCIATE PROFESSOR MATERNAL FETAL MEDICINE UNIVERSITY OF COLORADO Over 450 types of Skeletal Dysplasias X-linked Spondyloepiphyseal Tarda Thanatophoric dysplasia Osteogenesis Imperfecta Hypochondrogenesis Achondrogenesis Achondroplasia Otospondylomegaepiphyseal dysplasia Fibrochondrogenesis (OSMED) Hypochondroplasia Campomelic dysplasia Spondyloepiphyseal dysplasia congenita (SEDC) How will we come across this diagnosis? Third trimester size less than dates ultrasound at 33 4/7 weeks shows: What should our goal be at the initial visit? A. Genetic definitive diagnosis B. Termination of pregnancy C. Detailed anatomic survey including all long bones D. Assessment of likely lethality from pulmonary hypoplasia E. Amniocentesis or Serum Testing/Genetics Referral F. Referral to a Fetal Care Center What should our goal be at the initial visit? A. Genetic definitive diagnosis B. Termination of pregnancy C. Detailed anatomic survey including all long bones D. Assessment of likely lethality secondary to pulmonary hypoplasia E. Amniocentesis or Serum Testing/Genetics Referral F. Referral to a Fetal Care Center Detailed Ultrasound Technique Long bones Thorax Hands/feet Skull Spine Face Long bones Measure all including distal Look for missing bones Mineralization, curvature, fractures If limbs disproportional…. Does the abnormality effect: Proximal (rhizomelic) Middle (mesomelic) Distal (acromelic) Long bones Measure all extremities -

Current Overview of Osteogenesis Imperfecta
medicina Review Current Overview of Osteogenesis Imperfecta Mari Deguchi *, Shunichiro Tsuji , Daisuke Katsura , Kyoko Kasahara, Fuminori Kimura and Takashi Murakami Department of Obstetrics & Gynecology, Shiga University of Medical Science, Otsu 520-2192, Shiga, Japan; [email protected] (S.T.); [email protected] (D.K.); [email protected] (K.K.); [email protected] (F.K.); [email protected] (T.M.) * Correspondence: [email protected] Abstract: Osteogenesis imperfecta (OI), or brittle bone disease, is a heterogeneous disorder charac- terised by bone fragility, multiple fractures, bone deformity, and short stature. OI is a heterogeneous disorder primarily caused by mutations in the genes involved in the production of type 1 collagen. Severe OI is perinatally lethal, while mild OI can sometimes not be recognised until adulthood. Severe or lethal OI can usually be diagnosed using antenatal ultrasound and confirmed by various imaging modalities and genetic testing. The combination of imaging parameters obtained by ultrasound, computed tomography (CT), and magnetic resource imaging (MRI) can not only detect OI accurately but also predict lethality before birth. Moreover, genetic testing, either noninvasive or invasive, can further confirm the diagnosis prenatally. Early and precise diagnoses provide parents with more time to decide on reproductive options. The currently available postnatal treatments for OI are not curative, and individuals with severe OI suffer multiple fractures and bone deformities throughout their lives. In utero mesenchymal stem cell transplantation has been drawing attention as a promising therapy for severe OI, and a clinical trial to assess the safety and efficacy of cell therapy is currently ongoing. -

Mechanisms of Bone Fragility: from Osteogenesis Imperfecta to Secondary Osteoporosis
International Journal of Molecular Sciences Review Mechanisms of Bone Fragility: From Osteogenesis Imperfecta to Secondary Osteoporosis Ahmed El-Gazzar and Wolfgang Högler * Department of Paediatrics and Adolescent Medicine, Johannes Kepler University Linz, Krankenhausstraße 26-30, 4020 Linz, Austria; [email protected] * Correspondence: [email protected]; Tel.: +43-(0)5-7680-84-22001; Fax: +43-(0)5-7680-84-22004 Abstract: Bone material strength is determined by several factors, such as bone mass, matrix composi- tion, mineralization, architecture and shape. From a clinical perspective, bone fragility is classified as primary (i.e., genetic and rare) or secondary (i.e., acquired and common) osteoporosis. Understanding the mechanism of rare genetic bone fragility disorders not only advances medical knowledge on rare diseases, it may open doors for drug development for more common disorders (i.e., postmenopausal osteoporosis). In this review, we highlight the main disease mechanisms underlying the development of human bone fragility associated with low bone mass known to date. The pathways we focus on are type I collagen processing, WNT-signaling, TGF-ß signaling, the RANKL-RANK system and the osteocyte mechanosensing pathway. We demonstrate how the discovery of most of these pathways has led to targeted, pathway-specific treatments. Keywords: bone fragility; type I collagen; post-translational modifications; extracellular matrix; osteogenesis imperfecta; Juvenile Paget disease; osteomalacia; osteopetrosis 1. Introduction Citation: El-Gazzar, A.; Högler, W. Mechanisms of Bone Fragility: From Developing bones consist of cartilaginous joints, the epiphysis, the growth plate carti- Osteogenesis Imperfecta to Secondary lage with adjacent osteogenesis and the cortical and cancellous bone mineralized structure. -

Child Abuse Or Osteogenesis Imperfecta?
Child Abuse or Osteogenesis Imperfecta? A child is brought into the emergency room with a fractured leg. The parents are unable to explain how the leg fractured. X-rays reveal several other fractures in various stages of healing. The parents say they did not know about these fractures, and cannot explain what might have caused them. Hospital personnel call child welfare services to report a suspected case of child abuse. The child is taken away from the parents and placed in foster care. Scenes like this occur in emergency rooms every day. But in this case, the cause of the fractures is not child abuse. It is osteogenesis imperfecta, or OI. OI is a genetic disorder characterized by bones that break easily— often from little or no apparent cause. A person with OI may sustain just a few or as many as several hundred fractures in a lifetime. What Is Osteogenesis Imperfecta? Osteogenesis imperfecta is a genetic disorder. Most cases involve a defect in type 1 collagen—the protein “scaffolding” of bone and other connective tissues. People with OI have a faulty gene that instructs their bodies to make either too little type 1 collagen or poor quality type 1 collagen. The result is bones that break easily plus other connective tissue symptoms. Most cases of OI are caused by a dominant genetic defect. Most children with OI inherit the disorder from a parent who has OI. Some adults with very mild OI may not have been diagnosed as children. Approximately 25% of children with OI are born into a family with no history of the disorder. -
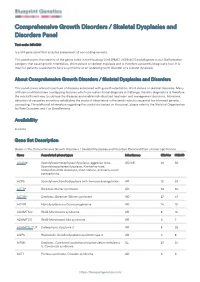
Blueprint Genetics Comprehensive Growth Disorders / Skeletal
Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders Panel Test code: MA4301 Is a 374 gene panel that includes assessment of non-coding variants. This panel covers the majority of the genes listed in the Nosology 2015 (PMID: 26394607) and all genes in our Malformation category that cause growth retardation, short stature or skeletal dysplasia and is therefore a powerful diagnostic tool. It is ideal for patients suspected to have a syndromic or an isolated growth disorder or a skeletal dysplasia. About Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders This panel covers a broad spectrum of diseases associated with growth retardation, short stature or skeletal dysplasia. Many of these conditions have overlapping features which can make clinical diagnosis a challenge. Genetic diagnostics is therefore the most efficient way to subtype the diseases and enable individualized treatment and management decisions. Moreover, detection of causative mutations establishes the mode of inheritance in the family which is essential for informed genetic counseling. For additional information regarding the conditions tested on this panel, please refer to the National Organization for Rare Disorders and / or GeneReviews. Availability 4 weeks Gene Set Description Genes in the Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders Panel and their clinical significance Gene Associated phenotypes Inheritance ClinVar HGMD ACAN# Spondyloepimetaphyseal dysplasia, aggrecan type, AD/AR 20 56 Spondyloepiphyseal dysplasia, Kimberley -

Osteogenesis Imperfecta: Recent Findings Shed New Light on This Once Well-Understood Condition Donald Basel, Bsc, Mbbch1, and Robert D
COLLABORATIVE REVIEW Genetics in Medicine Osteogenesis imperfecta: Recent findings shed new light on this once well-understood condition Donald Basel, BSc, MBBCh1, and Robert D. Steiner, MD2 TABLE OF CONTENTS Overview ...........................................................................................................375 Differential diagnosis...................................................................................380 Clinical manifestations ................................................................................376 In utero..........................................................................................................380 OI type I ....................................................................................................376 Infancy and childhood................................................................................380 OI type II ...................................................................................................377 Nonaccidental trauma (child abuse) ....................................................380 OI type III ..................................................................................................377 Infantile hypophosphatasia ....................................................................380 OI type IV..................................................................................................377 Bruck syndrome .......................................................................................380 Newly described types of OI .....................................................................377 -

Blueprint Genetics Comprehensive Skeletal Dysplasias and Disorders
Comprehensive Skeletal Dysplasias and Disorders Panel Test code: MA3301 Is a 251 gene panel that includes assessment of non-coding variants. Is ideal for patients with a clinical suspicion of disorders involving the skeletal system. About Comprehensive Skeletal Dysplasias and Disorders This panel covers a broad spectrum of skeletal disorders including common and rare skeletal dysplasias (eg. achondroplasia, COL2A1 related dysplasias, diastrophic dysplasia, various types of spondylo-metaphyseal dysplasias), various ciliopathies with skeletal involvement (eg. short rib-polydactylies, asphyxiating thoracic dysplasia dysplasias and Ellis-van Creveld syndrome), various subtypes of osteogenesis imperfecta, campomelic dysplasia, slender bone dysplasias, dysplasias with multiple joint dislocations, chondrodysplasia punctata group of disorders, neonatal osteosclerotic dysplasias, osteopetrosis and related disorders, abnormal mineralization group of disorders (eg hypopohosphatasia), osteolysis group of disorders, disorders with disorganized development of skeletal components, overgrowth syndromes with skeletal involvement, craniosynostosis syndromes, dysostoses with predominant craniofacial involvement, dysostoses with predominant vertebral involvement, patellar dysostoses, brachydactylies, some disorders with limb hypoplasia-reduction defects, ectrodactyly with and without other manifestations, polydactyly-syndactyly-triphalangism group of disorders, and disorders with defects in joint formation and synostoses. Availability 4 weeks Gene Set Description