Table of Contents
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

The Influence of Iatrogenic Atrial Septal Defect On
Bioscience Reports (2020) 40 BSR20193128 https://doi.org/10.1042/BSR20193128 Research Article The influence of iatrogenic atrial septal defect on the prognosis of patients with atrial fibrillation between cryoablation and radiofrequency ablation Ying Yang, Jinglan Wu, Lixia Yao, Yue Liu, Chenfeng Zhang, Ling You, Jing Yang and Ruiqin Xie Downloaded from http://portlandpress.com/bioscirep/article-pdf/40/2/BSR20193128/867399/bsr-2019-3128.pdf by guest on 02 October 2021 Department of Cardiology, The Second Hospital of Hebei Medical University, Shijiazhuang 050000, China Correspondence: Ruiqin Xie ([email protected]) Objective: The present study was to compare the incidence of septal defect (SD) in patients with atrial fibrillation (AF) who received radiofrequency ablation or cryoablation. Methods: A total of 293 AF patients were performed with radiofrequency ablation and cryoablation. Cardiac ultrasonography was performed to calculate left atrial diameter (LAD), left atrial ejection fraction (LAEF%), strain rate (SR), left ventricular systolic (SRs), left ven- tricular diastolic (SRe), and left atrial systole (SRa) before surgery, 3 months and 1 year after surgery. The patients were followed up to observe statin and angiotensin-converting enzyme inhibitor (ACEI)/angiotensin receptor blocker (ARB) medication, AF recurrence, 6-min walk test, stroke, any symptoms caused by arrhythmia, and re-hospitalization. Results: The lev- els of LAD and SD were higher, while SRe and SRa were lower in the cryoablation group in the comparison with the radiofrequency ablation group after surgery (P<0.05). LAEF was lower in the cryoablation group than the radiofrequency ablation group after 3 months (P<0.05). After 1-year follow-up, no right-to-left shunt occurred in all patients with SD. -

Scimitar Syndrome: Pathology, Clinical Presentation, Radiographic Features, and Treatment *Yazdan Ghandi1, Alireza Farsi21
http:// ijp.mums.ac.ir Review Article (Pages: 10611-10620) Scimitar Syndrome: Pathology, Clinical Presentation, Radiographic Features, and Treatment *Yazdan Ghandi1, Alireza Farsi21 1Associate Professor, Pediatric Cardiologist, Amirkabir Hospital, Arak University of Medical Sciences, Arak, Iran. 2 Medical Student, Amirkabir Hospital, School of Medicine, Arak University of Medical Sciences, Arak, Iran. Abstract Scimitar syndrome is characterized by partial or total anomalous pulmonary venous return from the right lung along with pulmonary hypoplasia. We searched the mail databases such as Medline (via PubMed), Scopus and EMBASE and Google Scholar. Diagnosing infantile scimitar syndrome requires meticulous attention and high suspicion of the early referral and management. The association of the syndrome with pulmonary hypertension leads to recurrent and prolonged hospitalization. Scimitar syndrome can be initially suspected from a chest X-ray, but it is typically confirmed via Computed Tomography (CT) angiography. The clinical spectrum of Scimitar syndrome ranges from severely ill infants to asymptomatic adults, which may present respiratory or cardiac failure, hemoptysis and pulmonary hypertension, tachypnea, chest infection, and failure to thrive. The diagnosis can be made by transthoracic or transesophageal echocardiography, angiography, or by CT or MR angiography. Considering the wide clinical spectrum of scimitar syndrome, the medical intervention depends on the severity of presentation and the amount of blood flowing to the Inferior Vena Cava (IVC) from completely or partially anomalous pulmonary veins. In the presence of significant left to right shunting and pulmonary hypertension, surgical intervention should be considered. Key Words: Congenital Anomaly, Pulmonary Hypertension, Scimitar Syndrome. *Please cite this article as: Ghandi Y, Farsi A. Scimitar Syndrome: Pathology, Clinical Presentation, Radiographic Features, and Treatment. -

Pulmonary in Trisomy 18 (T18) and Has Been Described Also in Several Disorders Other Than T18
ANNUAL MEETING ABSTRACTS 449A 1867 Infections in a Children’s Hospital Autopsy Population abstract, is useful and may serve as a guideline to define CH, with linear regression +20% J Springer, R Craver. Louisiana State University Health Science Center, New Orleans, of T18 cases and/or linear regression -20% of control cases being the borderline for CH. LA. Background: Despite advances in antimicrobial therapy, infections/inflammatory 1869 Expression of Disialoganglioside GD2 in Neuroblastomas of lesions may frequently cause or contribute to death in children. Patients Treated with Immunotherapy Design: We retrospectively reviewed all autopsies performed at a children’s hospital T Terzic, P Teira, S Cournoyer, M Peuchmaur, H Sartelet. Centre Hospitalier from 1986-2009 and categorized infectious complications as 1)underlying cause Universitaire Sainte-Justine, Montreal, QC, Canada; Hopital Universitaire Robert- of death,2) mechanism of death complicating another underlying cause of death,3) Debre, Paris, France. contributing to death 4) agonal or infections immediately before death 5) incidental. Background: Neuroblastoma, a malignant neoplasm of the sympathetic nervous Infectious complications were then separated into 3-8 year groups to identify trends system, is one of the most aggressive pediatric cancers with a tendency for widespread over the years. dissemination, relapse and a poor long term survival, despite intensive multimodal Results: There were 1369 deaths over 24 years, 608 (44%) underwent autopsy at treatments. Recent use of immunotherapy (a chimeric human-murine monoclonal the hospital, another 122 (8.9%) were coroner’s cases not performed at the hospital. antibody ch14.18 directed against a tumor-associated antigen GD2, a disialoganglioside) There were 691 infectious conditions in 401 children (66%, 1.72 infections/infected to treat minimal residual disease has shown improvement in event-free and overall patient).There were no differences in the percentage of autopsies with infections over survival of high-risk neuroblastomas. -

Radical Views... Oct 2013 from the Department of Radiology Beth Israel Deaconess a Teaching Hospital of Medical Center Harvard Medical School ®
Volume 6, Number 3 Radical Views... Oct 2013 from the Department of Radiology Beth Israel Deaconess A teaching hospital of Medical Center Harvard Medical School ® Congratulations Drs. Faintuch, Brook and Kung! I am pleased to announce that the following promotions have been approved by HMS: Salomao Faintuch, MD - Justin Kung, MD - Assistant Professor of Radiology, Assistant Professor of Radiology, Interventional Radiology MSK/Community Radiology FROM THE CHIEF Jonathan B. Kruskal, MD PhD Olga R. Brook, MD - Assistant Professor of Radiology, Interventional Radiology / Abdominal Imaging Congratulations Alexander Bankier, MD, PhD - Secretary, Fleischner Society - At its annual meeting in Jeju, South Korea, in June 2013, Alex Bankier was elected secretary of the Fleischner Society. After serving as chairman of the Scientifi c Program Planning Committee of the society for the past two years, Alex will now serve as secretary for three more years, to later move to president-elect and, eventually, president of the society in 2017-2018. The Fleischner Society is an international, multidisciplinary society for thoracic radiology, dedicated to the diagnosis and treatment of diseases of the chest. Founded in 1969, the Society was named in memory of Felix Fleischner, former chairman of Radiology at the Beth Israel Hospital, and an inspiring educator, clinician, and researcher who made seminal contributions to the fi eld of chest radiology. The Fleischner Society has an active membership of approximately 65 members worldwide, as well as approximately 35 senior members. The Fleischner Society maintains a diverse membership that includes experts in adult and pediatric radiology, pathology, adult and pediatric pulmonary medicine, thoracic surgery, physiology, morphology, epidemiology and other related sciences. -

Postoperative Pulmonary Artery Stenosis: Current Options and Future Directions
Commentary Postoperative pulmonary artery stenosis: current options and future directions David Kalfa Pediatric Cardiac Surgery, Morgan Stanley Children’s Hospital - NewYork-Presbyterian, Columbia University Medical Center, New York, USA Correspondence to: David Kalfa, MD, PhD. Pediatric Cardiac Surgery, Morgan Stanley Children’s Hospital - NewYork-Presbyterian, Columbia University Medical Center, New York, USA. Email: [email protected]. Provenance: This is a Guest Commentary commissioned by the Section Editor Xicheng Deng (Department of Cardiothoracic Surgery, Hunan Children’s Hospital, Changsha, China). Comment on: Kim H, Chan Sung S, Choi KH, et al. Sutureless Patch Angioplasty for Postoperative Pulmonary Artery Stenosis in Congenital Cardiac Surgeries. Ann Thorac Surg 2016;101:1031-6. Submitted Jul 05, 2016. Accepted for publication Jul 10, 2016. doi: 10.21037/tp.2016.08.01 View this article at: http://dx.doi.org/10.21037/tp.2016.08.01 This study by Kim et al. (1) addresses an important and clamp time. frequent issue in pediatric cardiac surgery, which is the Kim et al. report a sutureless patch angioplasty. This management of postoperative pulmonary artery (PA) technique is based on the concept that postoperative branches stenoses. Different options are currently available adhesions and peel tissue around the previous patch material to treat a PA branch stenosis, including a conventional can be used as an autologous vascular support. This concept surgical plasty using (or not) a biological patch (autologous of suturing a patch -

Mercy General Provides New Options for Atrial Fibrillation Treatment
C AR DI AC MERRCY HEARRT MONITOR INSTITUTE For healthcare pro fes sion als Spring 2005 Mercy General provides new options for atrial fi brillation treatment By Gearoid O’Neill, MD Vision Statement Atrial fi brillation is the most common cardiac fi brillation. The most popular approaches are In conjunction with the arrhythmia prompting hospitalization. It is associated “segmental pulmonary vein isolation” and “circum- Sisters of Mercy, our with a doubling of mortality due principally to the ferential pulmonary vein ablation.” In the former, cardiovascular care related stroke risk and development of heart failure. strands of myocardial fi bres coming from the out- team is dedicated to providing patients with Symptoms of atrial fi brillation, including fatigue, side sleeves of the pulmonary veins are interrupted com pas sion ate, quality, dyspnea and palpitations, can have a profound im- using radiofrequency ablation (RF). In the latter, cost-effective care pact on quality of life. wide circles are drawn with RF, enclosing each pair through state-of-the of pulmonary veins without necessarily setting out art ad vance ments in research, diagnostic Rhythm maintenance to prove electrical disconnection of the veins to the screen ing, surgical The mainstay of treatment is stroke prevention and left atrium. In addition, a line is drawn from the and interventional the strategic choice of rate or rhythm control. High- bottom of the circle surrounding the left pair of pro ce dures, clinical education and risk patients should receive coumadin anticoagulation. veins to the mitral valve. In some centers an addi- preventive/wellness An alternative of plavix plus aspirin is currently tional line is drawn across the roof of the left atrium. -
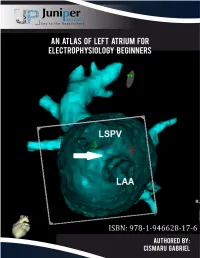
An Atlas of Left Atrium for Electrophysiology Beginners
An Atlas of Left Atrium for Electrophysiology Beginners ISBN: 978-1-946628-17-6 1 An Atlas of Left Atrium for Electrophysiology Beginners Cismaru Gabriel* Department of Cardiology, Rehabilitation Hospital-Iuliu Hatieganu University of Medicine and Pharmacy, Romania *Corresponding Author Department of Cardiology, Electrophysiological laboratory, Rehabilitation Hospital-Iuliu Hatieganu University of Medicine and Pharmacy, Cluj-Napoca, Romania Published By : Juniper publishers Inc. United States March 25, 2019 2 Gabriel Cismaru M.D., PhD., Dr. Cismaru Gabriel received his doctorate in medicine from the “Iuliu Hatieganu” University of Medicine and Pharmacy, Cluj- Napoca in 2016 and earned his MD degree from the same university in 2005. After completing his residency in cardiology, Dr. Cismaru began his electrophysiology fellowship at the Institute Lorrain du Coeur et des vaisseaux Louis Mathieu, Nancy-France. In 2011 started to work at the Electrophysiology Laboratory of the Rehabilitation Hospital Cluj-Napoca. He has authored or coauthored The new advances in cardiac arrhythmias techniques increased the success rate of complete treatment peer-reviewed articles, book chapters in the field of electrophysiology and cardiac pacing. centers. Knowing the anatomy of the left atrium is a cornerstone for the EP beginner. The topic is of great interestfor patients to electrophysiologists suffering from arrhythmias. dealing with Catheter catheter ablation ablation of atrial of all fibrillation types of left is routinely atrial arrhythmias performed (atrial in EP fibrillation, atrial tachycardia, atrial flutter, premature atrial contractions). An Atlas of Left Atrium for Electrophysiology Beginners List of Contents S.No. Content Page No. 1 Foreword 5 2 Introduction 6 3 Chapter 1: Anatomy of the Left Atrium 7-19 3.1. -

Venoatrial Compression by Lymphadenopathy in Sarcoidosis
" a)1000 # ● D. Constantinescu*, M. Vornicu , C. Grigoriu , C. Cozmei* + ● # ● and B.D. Grigoriu # " ● *Institute of Public Health, Clinic of Pulmonary Diseases, Depts 800 ● -1 + ● of Forensic Pathology, and Dept of Pulmonary Diseases, ● ● ● ● University of Medicine and Pharmacy ‘‘Gr. T. Popa’’, Iasi, 600 ● ● ● Romania. ● ● ● ● ● ● ● ● ● ● ● ● ● ● ● ● ● ● ● Correspondence: B.D. Grigoriu, Dept of Pulmonary Diseases, 400 ● ● ● ● ● ● ● ● ● ● ● ● ● ● University of Medicine and Pharmacy ‘‘Gr. T. Popa’’ Iasi, Str ● ● ● ● ● ● ● ● ● ● ● ● ● ● ● ● Universitatii 16, 700115 Iasi, Romania. E-mail: b_grigoriu@ Osteopontin IBL ng·mL Osteopontin IBL ● ● 200 ● ● ● hotmail.com ● ● ● ● 0 ● Support Statement: This research has been funded by the 0 25 50 75 100 125 National Council for Scientific Research in Higher Education Osteopontin R&D ng·mL-1 (CNCSIS) by the grant number 1191/2007. b) 0 ● ● ● Statement of Interest: None declared. ● ● ● ● ● -150 ● ● ● ●● ●●●●● ●● ● ●● ●● ● REFERENCES -300 ● ● ●●● ●●● 1 Isa S-I, Kawaguchi T, Teramukai S, et al. Serum osteopontin levels are ● ● ● ● ● ●●● ● highly prognostic for survival in advanced non-small cell lung ● ●● -450 ● ● ● ● cancer: results from JMTO LC 0004. J Thorac Oncol 2009; 4: 1104–1110. ● ● ● ● Difference 2 Inomata S, Shijubo N, Kon S, et al. Circulating interleukin-18 and ● ● ● -600 ● osteopontin are useful to evaluate disease activity in patients with ● tuberculosis. Cytokine 2005; 30: 203–211. ● 3 Pardo A, Gibson K, Cisneros J, et al. Up-regulation and profibrotic -750 ● ● role of osteopontin in human idiopathic pulmonary fibrosis. PLoS ● Med 2005; 2: e251. -900 4 Chung KF, Adcock IM. Multifaceted mechanisms in COPD: 0 100 200 300 400 500 inflammation, immunity, and tissue repair and destruction. Eur Average Respir J 2008; 31: 1334–1356. 5 Scherpereel A, Astoul P, Baas P, et al. -

Neurological Consequences of Atrioesophageal Fistula After Radiofrequency Ablation in Atrial Fibrillation
ORIGINAL CONTRIBUTION Neurological Consequences of Atrioesophageal Fistula After Radiofrequency Ablation in Atrial Fibrillation Claudia Stöllberger, MD; Thomas Pulgram, MD; Josef Finsterer, MD, PhD Background: Radiofrequency ablation for atrial fibril- 21 of 28 patients. Blood tests showed leukocytosis, el- lation (RAF) is an increasingly performed procedure. It evated serum C-reactive protein levels, and thrombocy- is performed during cardiac surgery or percutaneously topenia. Blood cultures were frequently positive for bac- by catheter. A dangerous complication of RAF is atrio- teria. Lumbar puncture revealed pleocytosis, elevated esophageal fistula (AEF), which predominantly mani- protein levels, increased lactate levels, and bacteria. Di- fests neurologically owing to food embolism. Because neu- agnosis was established by thoracic contrast computed rologists may not be familiar with AEF and the prognosis tomography. Endoscopy, insertion of nasogastric tubes, is dependent on a prompt diagnosis, awareness of AEF and transesophageal echocardiography were detrimen- by the neurologist may play a crucial role. tal, leading to an increase in fistula size and food or air embolism. Therapy comprised surgery (n=11) or tem- Objective: To summarize for the neurologist the knowl- porary esophageal stenting (n=1). The remaining pa- edge about fistula between the left atrium and esopha- tients died before attempted surgery or confirmation of gus occurring after RAF. the diagnosis. A neurological deficit persisted in 3 of the 9 surviving patients. Design, Setting, and Patients: Using a MEDLINE search, we collected reports about AEF after RAF in 28 patients. Conclusions: In patients with meningitis, stroke, sei- zures, or impaired consciousness and fever, it should be Main Outcome Measures: From the collected re- determined whether they have had a previous RAF. -

Important Newborn Cardiac Diagnostic Dilemmas for the Neonatologist and Cardiologist–A Clinical Perspective
Tech Science Press DOI: 10.32604/CHD.2021.014903 REVIEW Important Newborn Cardiac Diagnostic Dilemmas for the Neonatologist and Cardiologist–A Clinical Perspective Samuel Menahem1,2,* and Arvind Sehgal3,4 1Department of Paediatrics, University of Melbourne, Melbourne, Australia 2School of Clinical Sciences, Monash University, Melbourne, Australia 3Monash Newborn, Cardiovascular Research, Monash Children’s Hospital, Melbourne, Australia 4Department of Paediatrics, Monash University, Melbourne, Australia *Corresponding Author: Samuel Menahem. Email: [email protected] Received: 06 November 2020 Accepted: 16 November 2020 ABSTRACT Most congenital heart disease (CHD) is readily recognisable in the newborn. Forewarned by previous fetal scan- ning, the presence of a murmur, tachypnoea, cyanosis and/or differential pulses and saturations all point to a car- diac abnormality. Yet serious heart disease may be missed on a fetal scan. There may be no murmur or clinical cyanosis, and tachypneoa may be attributed to non-cardiac causes. Tachypnoea on day 1 is usually non-cardiac except arising from ventricular failure or a large systemic arteriovenous fistula. A patent ductus arteriosus (PDA) may support either pulmonary or systemic duct dependent circulations. The initially high pulmonary vascular resistance (PVR) limits shunts so that murmurs even from large communications between the systemic and pul- monary circulations take days/weeks to develop. At times despite expert input, serious CHD maybe difficult to diagnose and warrants close interaction between the neonatologist and cardiologist to reach a timely diagnosis. Such conditions include obstructed total anomalous pulmonary venous connections (TAPVC) and the need to distinguish it from persistent pulmonary hypertension in the newborn (PPHN)–the treatment of the former is surgical the latter medical. -

The Real Need for Regenerative Medicine in the Future of Congenital Heart Disease Treatment
biomedicines Review The Real Need for Regenerative Medicine in the Future of Congenital Heart Disease Treatment Yuichi Matsuzaki 1,†, Matthew G. Wiet 1,†, Brian A. Boe 2 and Toshiharu Shinoka 1,3,* 1 Center for Regenerative Medicine, The Abigail Wexner Research Institute at Nationwide Children’s Hospital, 700 Children’s Drive, T2294, Columbus, OH 43205, USA; [email protected] (Y.M.); [email protected] (M.G.W.) 2 Department of Cardiology, The Heart Center, Nationwide Children’s Hospital, 700 Children’s Drive, T2294, Columbus, OH 43205, USA; [email protected] 3 Department of Cardiothoracic Surgery, The Heart Center, Nationwide Children’s Hospital, 700 Children’s Drive, T2294, Columbus, OH 43205, USA * Correspondence: [email protected]; Tel.: +1-614-722-3103; Fax: 614-722-3111 † Co-first author. Abstract: Bioabsorbable materials made from polymeric compounds have been used in many fields of regenerative medicine to promote tissue regeneration. These materials replace autologous tissue and, due to their growth potential, make excellent substitutes for cardiovascular applications in the treatment of congenital heart disease. However, there remains a sizable gap between their theoretical advantages and actual clinical application within pediatric cardiovascular surgery. This review will focus on four areas of regenerative medicine in which bioabsorbable materials have the potential to alleviate the burden where current treatment options have been unable to within the field of pediatric cardiovascular surgery. These four areas include tissue-engineered pulmonary valves, tissue-engineered patches, regenerative medicine options for treatment of pulmonary vein Citation: Matsuzaki, Y.; Wiet, M.G.; stenosis and tissue-engineered vascular grafts. -

Patient and Family-Centered Care for Pediatric Intraluminal Pulmonary Vein Stenosis: Case of a 3 Year Old Patient with Focus on Nurse Practitioner Role
children Case Report Patient and Family-Centered Care for Pediatric Intraluminal Pulmonary Vein Stenosis: Case of a 3 Year Old Patient with Focus on Nurse Practitioner Role Christina M. Ireland 1,*, Ryan Callahan 1,2 and Kathy J. Jenkins 1,2 1 Department of Cardiology, Boston Children’s Hospital, Boston, MA 02115, USA; [email protected] (R.C.); [email protected] (K.J.J.) 2 Department of Pediatrics, Harvard Medical School, Boston, MA 02115, USA * Correspondence: [email protected] Abstract: A nurse practitioner’s experience in managing children with intraluminal pulmonary vein stenosis. A case study of a 3-year-old patient with multi–vessel intraluminal pulmonary vein stenosis. Keywords: pulmonary vein stenosis; nurse practitioner; management 1. Introduction Intraluminal Pulmonary Vein Stenosis (PVS) is a rare disorder which involves pro- gressive narrowing of the pulmonary veins and can lead to pulmonary hypertension, Citation: Ireland, C.M.; Callahan, R.; right heart failure and death [1]. PVS can occur in young infants independently, in those Jenkins, K.J. Patient and with chronic lung disease and more commonly in conjunction with complex congenital Family-Centered Care for Pediatric heart disease. Managing this disease is unlike other cardiac defects because reoccurrence Intraluminal Pulmonary Vein of the stenosis is expected due to the mechanism of the disease and is not completely Stenosis: Case of a 3 Year Old Patient understood or easily treatable. Although the pathophysiology of PVS is similar among with Focus on Nurse Practitioner patients, each patient and family brings a unique set of circumstances, and no one patient Role.