TMEM16F Activation by Ca2+ Triggers Plasma Membrane Expansion And
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Implicating Gene and Cell Networks Responsible for Differential COVID
bioRxiv preprint doi: https://doi.org/10.1101/2021.06.07.447287; this version posted June 16, 2021. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY-NC 4.0 International license. 1 Implicating Gene and Cell Networks Responsible for 2 Differential COVID-19 Host Responses via an Interactive 3 Single Cell Web Portal 4 5 Kang Jin1,2, Eric E. Bardes1, Alexis Mitelpunkt1,3,4, Jake Y. Wang1, Surbhi Bhatnagar1,5, 6 Soma Sengupta6, Daniel Pomeranz Krummel6, Marc E. Rothenberg7, Bruce J. 7 Aronow1,8,9,* 8 9 1Division oF Biomedical InFormatics, Cincinnati Children's Hospital Medical Center, 10 Cincinnati, OH, 45229, USA 11 2Department oF Biomedical InFormatics, University oF Cincinnati, Cincinnati, OH, 45229, 12 USA 13 3Pediatric Rehabilitation, Dana-Dwek Children's Hospital, Tel Aviv Medical Center, Tel 14 Aviv, 6423906, Israel 15 4Sackler Faculty oF Medicine, Tel Aviv University, Tel Aviv, 6997801, Israel 16 5Department oF Electrical Engineering and Computer Science, University oF Cincinnati, 17 Cincinnati, OH, 45221, USA 18 6Department oF Neurology and Rehabilitation Medicine, University oF Cincinnati College 19 oF Medicine, Cincinnati, OH, 45267, USA. 20 7Division oF Allergy and Immunology, Department oF Pediatrics, Cincinnati Children's 21 Hospital Medical Center, University oF Cincinnati, Cincinnati, OH, 45229, USA 22 8Department oF Pediatrics, University oF Cincinnati School oF Medicine, Cincinnati, OH, 23 45256, USA 24 9Lead contact 25 *Correspondence: [email protected] (B.A.) 26 27 28 29 30 31 1 bioRxiv preprint doi: https://doi.org/10.1101/2021.06.07.447287; this version posted June 16, 2021. -

Structural and Functional Characterization of TMEM16 Family Members
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2016 Structural and functional characterization of TMEM16 family members Lim, Novandy Posted at the Zurich Open Repository and Archive, University of Zurich ZORA URL: https://doi.org/10.5167/uzh-129639 Dissertation Published Version Originally published at: Lim, Novandy. Structural and functional characterization of TMEM16 family members. 2016, University of Zurich, Faculty of Science. Structural and Functional Characterization of TMEM16 Family Members Dissertation zur Erlangung der naturwissenschaftlichen Doktorwürde (Dr. sc. nat.) vorgelegt der Mathematisch-naturwissenschaftlichen Fakultät der Universität Zürich von Novandy Karunia Lim aus Indonesien Promotionskomitee Prof. Dr. Raimund Dutzler (Vorsitz) Prof. Dr. Markus Seeger Prof. Dr. Martin Jinek Zürich, 2016 Acknowledgements I would like to take this opportunity to thank all the people who have supported and helped me throughout my stay and project in the lab. Firstly, I would like to thank Prof. Raimund Dutzler for the opportunity to work on this highly exciting project. I am sincerely grateful for his constant support and his faith in me throughout my time in his group. I would like to thank Prof. Martin Jinek and Prof. Markus Seeger for being part of my thesis committee. I would like to thank Janine Brunner and Stephan Schenck for the helpful discussion on TMEM16 project. A big thank you to Alessia Dürst too for helping us with the homologue screen during her Masters thesis. I am grateful to all the past and present members of the Dutzler for their friendship, support and scientific discussions. -

Supp Table 6.Pdf
Supplementary Table 6. Processes associated to the 2037 SCL candidate target genes ID Symbol Entrez Gene Name Process NM_178114 AMIGO2 adhesion molecule with Ig-like domain 2 adhesion NM_033474 ARVCF armadillo repeat gene deletes in velocardiofacial syndrome adhesion NM_027060 BTBD9 BTB (POZ) domain containing 9 adhesion NM_001039149 CD226 CD226 molecule adhesion NM_010581 CD47 CD47 molecule adhesion NM_023370 CDH23 cadherin-like 23 adhesion NM_207298 CERCAM cerebral endothelial cell adhesion molecule adhesion NM_021719 CLDN15 claudin 15 adhesion NM_009902 CLDN3 claudin 3 adhesion NM_008779 CNTN3 contactin 3 (plasmacytoma associated) adhesion NM_015734 COL5A1 collagen, type V, alpha 1 adhesion NM_007803 CTTN cortactin adhesion NM_009142 CX3CL1 chemokine (C-X3-C motif) ligand 1 adhesion NM_031174 DSCAM Down syndrome cell adhesion molecule adhesion NM_145158 EMILIN2 elastin microfibril interfacer 2 adhesion NM_001081286 FAT1 FAT tumor suppressor homolog 1 (Drosophila) adhesion NM_001080814 FAT3 FAT tumor suppressor homolog 3 (Drosophila) adhesion NM_153795 FERMT3 fermitin family homolog 3 (Drosophila) adhesion NM_010494 ICAM2 intercellular adhesion molecule 2 adhesion NM_023892 ICAM4 (includes EG:3386) intercellular adhesion molecule 4 (Landsteiner-Wiener blood group)adhesion NM_001001979 MEGF10 multiple EGF-like-domains 10 adhesion NM_172522 MEGF11 multiple EGF-like-domains 11 adhesion NM_010739 MUC13 mucin 13, cell surface associated adhesion NM_013610 NINJ1 ninjurin 1 adhesion NM_016718 NINJ2 ninjurin 2 adhesion NM_172932 NLGN3 neuroligin -

Anoctamin 1 - a Member of a Novel Family of Ion Channels with Extended Functions and Significance in Disease
UNIVERSIDADE DE LISBOA FACULDADE DE CIÊNCIAS Anoctamin 1 - A Member of a Novel Family of Ion Channels with Extended Functions and Significance in Disease Doutoramento em Biologia Especialidade: Biologia de Sistemas Joana Ramos Rapaz Lérias Tese orientada por: Prof. Dr. Karl Kunzelmann e Prof. Dr. Margarida D. Amaral Documento especialmente elaborado para a obtenção do grau de doutor 2018 UNIVERSIDADE DE LISBOA FACULDADE DE CIÊNCIAS Anoctamin 1 - A Member of a Novel Family of Ion Channels with Extended Functions and Significance in Disease Doutoramento em Biologia Especialidade: Biologia de Sistemas Joana Ramos Rapaz Lérias Tese orientada por: Prof. Dr. Karl Kunzelmann e Prof. Dr. Margarida D. Amaral Júri: Presidente: ● Doutor Rui Manuel dos Santos Malhó, Professor Catedrático da Faculdade de Ciências da Universidade de Lisboa Vogais: ● Doutor Karl Kunzelmann, Kunzelmann, Professor, Faculty of Biology and Pre-Clinical Medicine da University of Regensburg, Alemanha (orientador); ● Doutor Ana Colette Pereira de Castro Osório Maurício, Professora Associada com Agregação, Instituto de Ciências Biomédicas Abel Salazar (ICBAS) da Universidade do Porto; ● Doutor Peter Jordan, Investigador Principal, Departamento de Genética Humana do Instituto Nacional de Saúde Doutor Ricardo Jorge; ● Doutora Maria da Graça Tavares Rebelo de Soveral Rodrigues, Professora Associada com Agregação, Faculdade de Farmácia da Universidade de Lisboa. Documento especialmente elaborado para a obtenção do grau de doutor Fundação para a Ciência e Tecnologia do Ministério da Educação e Ciência (FCT/ SFRH / BD / 52489 / 2014) 2018 De acordo com o disposto no artigo 24º do Regulamento de Estudos de Pós- Graduação da Universidade de Lisboa, Despacho nº 7024/2017, publicado no Diário da República – 2ª Série – nº 155 – 11 de Agosto de 2017, foram utilizados nesta dissertação resultados incluídos nos seguintes artigos: 1. -

Regulation and Function of TMEM16F in Renal Podocytes
International Journal of Molecular Sciences Article Regulation and Function of TMEM16F in Renal Podocytes Laura K. Schenk 1 ID , Jiraporn Ousingsawat 2, Boris V. Skryabin 3 ID , Rainer Schreiber 2,†, Hermann Pavenstädt 1,† and Karl Kunzelmann 2,*,† ID 1 Department of Nephrology, Hypertension and Rheumatology, University Hospital Muenster, 48149 Muenster, Germany; [email protected] (L.K.S.); [email protected] (H.P.) 2 Institut für Physiologie, Universität Regensburg, Universitätsstraße 31, D-93053 Regensburg, Germany; [email protected] (J.O.); [email protected] (R.S.) 3 Transgenic Animal and Genetic Engineering Models (TRAM), Department of Medicine, Westfälischen, Wilhelms–Universität Münster, 48149 Münster, Germany; [email protected] * Correspondence: [email protected]; Tel.: +49-(0)941-943-4302; Fax: +49-(0)941-943-4315 † These authors contributed equally to this work. Received: 6 May 2018; Accepted: 14 June 2018; Published: 18 June 2018 Abstract: The Ca2+-activated phospholipid scramblase and ion channel TMEM16F is expressed in podocytes of renal glomeruli. Podocytes are specialized cells that form interdigitating foot processes as an essential component of the glomerular filter. These cells, which participate in generation of the primary urine, are often affected during primary glomerular diseases, such as glomerulonephritis and secondary hypertensive or diabetic nephropathy, which always leads to proteinuria. Because the function of podocytes is known to be controlled by intracellular Ca2+ signaling, it is important to know about the role of Ca2+-activated TMEM16F in these cells. To that end, we generated an inducible TMEM16F knockdown in the podocyte cell line AB8, and produced a conditional mouse model with knockout of TMEM16F in podocytes and renal epithelial cells of the nephron. -
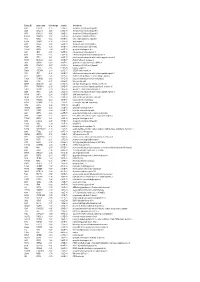

Entrez ID Gene Name Fold Change Q-Value Description
Entrez ID gene name fold change q-value description 4283 CXCL9 -7.25 5.28E-05 chemokine (C-X-C motif) ligand 9 3627 CXCL10 -6.88 6.58E-05 chemokine (C-X-C motif) ligand 10 6373 CXCL11 -5.65 3.69E-04 chemokine (C-X-C motif) ligand 11 405753 DUOXA2 -3.97 3.05E-06 dual oxidase maturation factor 2 4843 NOS2 -3.62 5.43E-03 nitric oxide synthase 2, inducible 50506 DUOX2 -3.24 5.01E-06 dual oxidase 2 6355 CCL8 -3.07 3.67E-03 chemokine (C-C motif) ligand 8 10964 IFI44L -3.06 4.43E-04 interferon-induced protein 44-like 115362 GBP5 -2.94 6.83E-04 guanylate binding protein 5 3620 IDO1 -2.91 5.65E-06 indoleamine 2,3-dioxygenase 1 8519 IFITM1 -2.67 5.65E-06 interferon induced transmembrane protein 1 3433 IFIT2 -2.61 2.28E-03 interferon-induced protein with tetratricopeptide repeats 2 54898 ELOVL2 -2.61 4.38E-07 ELOVL fatty acid elongase 2 2892 GRIA3 -2.60 3.06E-05 glutamate receptor, ionotropic, AMPA 3 6376 CX3CL1 -2.57 4.43E-04 chemokine (C-X3-C motif) ligand 1 7098 TLR3 -2.55 5.76E-06 toll-like receptor 3 79689 STEAP4 -2.50 8.35E-05 STEAP family member 4 3434 IFIT1 -2.48 2.64E-03 interferon-induced protein with tetratricopeptide repeats 1 4321 MMP12 -2.45 2.30E-04 matrix metallopeptidase 12 (macrophage elastase) 10826 FAXDC2 -2.42 5.01E-06 fatty acid hydroxylase domain containing 2 8626 TP63 -2.41 2.02E-05 tumor protein p63 64577 ALDH8A1 -2.41 6.05E-06 aldehyde dehydrogenase 8 family, member A1 8740 TNFSF14 -2.40 6.35E-05 tumor necrosis factor (ligand) superfamily, member 14 10417 SPON2 -2.39 2.46E-06 spondin 2, extracellular matrix protein 3437 -
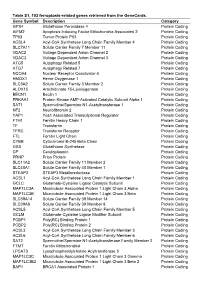
Table S1. 103 Ferroptosis-Related Genes Retrieved from the Genecards
Table S1. 103 ferroptosis-related genes retrieved from the GeneCards. Gene Symbol Description Category GPX4 Glutathione Peroxidase 4 Protein Coding AIFM2 Apoptosis Inducing Factor Mitochondria Associated 2 Protein Coding TP53 Tumor Protein P53 Protein Coding ACSL4 Acyl-CoA Synthetase Long Chain Family Member 4 Protein Coding SLC7A11 Solute Carrier Family 7 Member 11 Protein Coding VDAC2 Voltage Dependent Anion Channel 2 Protein Coding VDAC3 Voltage Dependent Anion Channel 3 Protein Coding ATG5 Autophagy Related 5 Protein Coding ATG7 Autophagy Related 7 Protein Coding NCOA4 Nuclear Receptor Coactivator 4 Protein Coding HMOX1 Heme Oxygenase 1 Protein Coding SLC3A2 Solute Carrier Family 3 Member 2 Protein Coding ALOX15 Arachidonate 15-Lipoxygenase Protein Coding BECN1 Beclin 1 Protein Coding PRKAA1 Protein Kinase AMP-Activated Catalytic Subunit Alpha 1 Protein Coding SAT1 Spermidine/Spermine N1-Acetyltransferase 1 Protein Coding NF2 Neurofibromin 2 Protein Coding YAP1 Yes1 Associated Transcriptional Regulator Protein Coding FTH1 Ferritin Heavy Chain 1 Protein Coding TF Transferrin Protein Coding TFRC Transferrin Receptor Protein Coding FTL Ferritin Light Chain Protein Coding CYBB Cytochrome B-245 Beta Chain Protein Coding GSS Glutathione Synthetase Protein Coding CP Ceruloplasmin Protein Coding PRNP Prion Protein Protein Coding SLC11A2 Solute Carrier Family 11 Member 2 Protein Coding SLC40A1 Solute Carrier Family 40 Member 1 Protein Coding STEAP3 STEAP3 Metalloreductase Protein Coding ACSL1 Acyl-CoA Synthetase Long Chain Family Member 1 Protein -

The Interactome of the Prostate-Specific Protein Anoctamin 7
Cancer Biomarkers 28 (2020) 91–100 91 DOI 10.3233/CBM-190993 IOS Press The interactome of the prostate-specific protein Anoctamin 7 Elina Kaikkonena, Aliisa Takalaa, Juha-Pekka Pursiheimoa, Gudrun Wahlströma and Johanna Schleutkera;b;∗ aInstitute of Biomedicine, University of Turku, Turku, Finland bDepartment of Medical Genetics, Genomics, Laboratory Division, Turku University Hospital, Turku, Finland Abstract. BACKGROUND: Elevated Anoctamin 7 (ANO7) expression is associated with poor survival in prostate cancer patients. OBJECTIVE: The aim was to discover proteins that interact with ANO7 to understand its functions and regulatory mechanisms. METHODS: The proximity-dependent biotin identification (BioID) method was utilized. ANO7 fused to biotin ligase was tran- siently transfected into LNCaP cells, and the biotinylated proteins were collected and analysed by mass spectrometry. Four identi- fied proteins were stained with dual fluorescent immunostaining and visualized using Stimulated emission depletion microscopy (STED). RESULTS: After bioinformatic filtering steps, 64 potentially ANO7-interacting proteins were identified and analysed with the GO enrichment analysis tool. One of the most prominently enriched cellular components was cellular vesicle. Co-localization was showed for staphylococcal nuclease and tudor domain containing 1 (SND1), heat shock protein family A (Hsp70) mem- ber 1A (HSPA1A), adaptor related protein complex 2 subunit beta 1 (AP2B1) and coatomer protein complex subunit gamma 2 (COPG2). CONCLUSIONS: This is the first study in which ANO7 interacting proteins have been identified. Although further studies are needed, the findings reported here expand our understanding of the role and regulation of ANO7 in prostate cancer cells. Furthermore, these results are likely to introduce new targets for the novel cancer therapies. -

Expression Is a Strong and Independent Predictor of Poor Prognosis in Prostate Cancer
Cancer Biol Med 2021. doi: 10.20892/j.issn.2095-3941.2019.0324 ORIGINAL ARTICLE Reduced anoctamin 7 (ANO7) expression is a strong and independent predictor of poor prognosis in prostate cancer Andreas Marx1,*, Lena Koopmann2,*, Doris Höflmayer2, Franziska Büscheck2, Claudia Hube-Magg2, Stefan Steurer2, Till Eichenauer3, Till S. Clauditz2, Waldemar Wilczak2, Ronald Simon2, Guido Sauter2, Jakob R. Izbicki4, Hartwig Huland5, Hans Heinzer5, Markus Graefen5, Alexander Haese5, Thorsten Schlomm6, Christian Bernreuther2, Patrick Lebok2, Sarah Bonk3 1Institute of Pathology, Klinikum Fürth, Fürth 90766, Germany; 2Institute of Pathology, University Medical Center Hamburg- Eppendorf, Hamburg 20246, Germany; 3Department of Urology, University Medical Center Hamburg-Eppendorf, Hamburg 20246, Germany; 4General, Visceral and Thoracic Surgery Department and Clinic, University Medical Center Hamburg- Eppendorf, Hamburg 20246, Germany; 5Martini-Clinic, Prostate Cancer Center, University Medical Center Hamburg- Eppendorf, Hamburg 20246, Germany; 6Department of Urology, Charité – Universitätsmedizin Berlin, Berlin 10117, Germany ABSTRACT Objective: Anoctamin 7 (ANO7) is a calcium2+-dependent chloride ion channel protein. Its expression is restricted to prostate epithelial cells. The exact function is unknown. This study aimed to analyze ANO7 expression and its clinical significance in prostate cancer (PCa). Methods: ANO7 expression was assessed by immunohistochemistry in 17,747 clinical PCa specimens. Results: ANO7 was strongly expressed in normal prostate glandular cells but often less abundant in cancer cells. ANO7 staining was interpretable in 13,594 cancer tissues and considered strong in 34.4%, moderate in 48.7%, weak in 9.3%, and negative in 7.6%. Reduced staining was tightly linked to adverse tumor features [high classical and quantitative Gleason grade, lymph node metastasis, advanced tumor stage, high Ki67 labeling index, positive surgical margin, and early biochemical recurrence (P < 0.0001 each)]. -

Channel ANO1 (TMEM16A)
A network of phosphatidylinositol 4,5-bisphosphate + binding sites regulates gating of the Ca2 -activated − Cl channel ANO1 (TMEM16A) Kuai Yua,1, Tao Jiangb,c,d,1, YuanYuan Cuia, Emad Tajkhorshidb,c,d,2, and H. Criss Hartzella,2 aDepartment of Cell Biology, Emory University School of Medicine, Atlanta, GA 30322; bNIH Center for Macromolecular Modeling and Bioinformatics, Beckman Institute for Advanced Science and Technology, University of Illinois at Urbana–Champaign, Urbana, IL 61801; cDepartment of Biochemistry, University of Illinois at Urbana–Champaign, Urbana, IL 61801; and dCenter for Biophysics and Quantitative Biology, University of Illinois at Urbana– Champaign, Urbana, IL 61801 Edited by Christopher Miller, Howard Hughes Medical Institute and Brandeis University, Waltham, MA, and approved August 19, 2019 (received for review March 26, 2019) + − + − ANO1 (TMEM16A) is a Ca2 -activated Cl channel that regulates di- Ca2 activates Cl flux because of conformational changes in- 2+ verse cellular functions including fluid secretion, neuronal excitabil- duced by direct binding of Ca to the ANO1 protein (21–25). ity, and smooth muscle contraction. ANO1 is activated by elevation Calmodulin is not required for channel activation (21, 26). 2+ Structurally, ANO1 is a dimer with each subunit composed of of cytosolic Ca and modulated by phosphatidylinositol 4,5-bisphos- − phate [PI(4,5)P2]. Here, we describe a closely concerted experimental 10 transmembrane (TM) segments. The Cl selective pore of each subunit is surrounded by TMs 4 to 7 (22, 23, 27, 28), and each and computational study, including electrophysiology, mutagenesis, 2+ – subunit has a Ca binding site formed by amino acids E654, E702, functional assays, and extended sampling of lipid protein interac- – tions with molecular dynamics (MD) to characterize PI(4,5)P binding E705, E734, and D738 in TMs 6 to 8 (22 25, 29). -

Targeting of Intracellular TMEM16 Proteins to the Plasma Membrane and Activation by Purinergic Signaling
International Journal of Molecular Sciences Article Targeting of Intracellular TMEM16 Proteins to the Plasma Membrane and Activation by Purinergic Signaling Rainer Schreiber *, Jiraporn Ousingsawat and Karl Kunzelmann Institut für Physiologie, Universität Regensburg, Universitätsstr. 31, 93053 Regensburg, Germany; [email protected] (J.O.); [email protected] (K.K.) * Correspondence: [email protected]; Tel.: +49 (0)941 943 2935 Received: 3 May 2020; Accepted: 2 June 2020; Published: 5 June 2020 2+ Abstract: Anoctamins such as TMEM16A and TMEM16B are Ca -dependent Cl− channels activated through purinergic receptor signaling. TMEM16A (ANO1), TMEM16B (ANO2) and TMEM16F (ANO6) are predominantly expressed at the plasma membrane and are therefore well accessible for functional studies. While TMEM16A and TMEM16B form halide-selective ion channels, TMEM16F and probably TMEM16E operate as phospholipid scramblases and nonselective ion channels. Other TMEM16 paralogs are expressed mainly in intracellular compartments and are therefore difficult to study at the functional level. Here, we report that TMEM16E (ANO5), -H (ANO8), -J (ANO9) and K (ANO10) are targeted to the plasma membrane when fused to a C-terminal CAAX (cysteine, two aliphatic amino acids plus methionin, serine, alanin, cystein or glutamin) motif. These paralogs produce Ca2+-dependent ion channels. Surprisingly, expression of the TMEM16 paralogs in the plasma membrane did not produce additional scramblase activity. In contrast, endogenous scrambling induced by stimulation of purinergic P2X7 receptors was attenuated, in parallel with reduced plasma membrane blebbing. This could suggest that intracellular TMEM16 paralogs operate differently when compared to plasma membrane-localized TMEM16F, and may even stabilize intracellular membranes. Alternatively, CAAX tagging, which leads to expression in non-raft compartments of the plasma membrane, may antagonize phosphatidylserine exposure by endogenous raft-located TMEM16F. -

Genome-Wide Gene Expression Profiling of Stress Response in A
Chamankhah et al. BMC Genomics 2013, 14:583 http://www.biomedcentral.com/1471-2164/14/583 RESEARCH ARTICLE Open Access Genome-wide gene expression profiling of stress response in a spinal cord clip compression injury model Mahmood Chamankhah1, Eftekhar Eftekharpour2, Soheila Karimi-Abdolrezaee3, Paul C Boutros4,5,6, Serban San-Marina7 and Michael G Fehlings1,8,9* Abstract Background: The aneurysm clip impact-compression model of spinal cord injury (SCI) is a standard injury model in animals that closely mimics the primary mechanism of most human injuries: acute impact and persisting compression. Its histo-pathological and behavioural outcomes are extensively similar to human SCI. To understand the distinct molecular events underlying this injury model we analyzed global mRNA abundance changes during the acute, subacute and chronic stages of a moderate to severe injury to the rat spinal cord. Results: Time-series expression analyses resulted in clustering of the majority of deregulated transcripts into eight statistically significant expression profiles. Systematic application of Gene Ontology (GO) enrichment pathway analysis allowed inference of biological processes participating in SCI pathology. Temporal analysis identified events specific to and common between acute, subacute and chronic time-points. Processes common to all phases of injury include blood coagulation, cellular extravasation, leukocyte cell-cell adhesion, the integrin-mediated signaling pathway, cytokine production and secretion, neutrophil chemotaxis, phagocytosis, response to hypoxia and reactive oxygen species, angiogenesis, apoptosis, inflammatory processes and ossification. Importantly, various elements of adaptive and induced innate immune responses span, not only the acute and subacute phases, but also persist throughout the chronic phase of SCI. Induced innate responses, such as Toll-like receptor signaling, are more active during the acute phase but persist throughout the chronic phase.