Selecting Candidates for Transcatheter Mitral Valve Repair
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Stent Technology Takes Two Steps Forward
Inside This Issue Heart and Vascular Update Hybrid operating room, provides information to PRESORTED HEART and VASCULAR healthcare providers on the latest FIRST CLASS MAIL a regional first in cardiovascular medicine and surgery U.S. POSTAGE at The Christ Hospital. PAID Stent technology takes CINCINNATI, OH Heart and Vascular Update PERMIT #5489 two steps forward Editorial Board 2139 Auburn Avenue | Cincinnati, Ohio 45219 Stent technology Dean J. Kereiakes, MD, FDA advisory panel: Medical Director SPRING 2013 The Christ Hospital Heart and Vascular Center Update MitraClip could serve as takes two steps forward Carl and Edyth Lindner Research Center an alternative treatment Ian Sarembock, MD, Executive Medical Director for reducing mitral Resorbable Absorb scaffold and flexible Absorb takes bioabsorbability to next level The Christ Hospital Heart and Vascular Service Line regurgitation For the past two decades, incremental improvements in stent Mike Keating Synergy stent expected to improve technology have improved outcomes for hundreds of thousands of President and CEO outcomes in coronary artery disease people with coronary artery blockages. These devices have evolved Michael W. Schwebler from short, bare-metal mesh tubes that could be deployed only The Carl and Eydth Lindner Research Center at The Christ Hospital is Executive Director in the largest coronary vessels to a variety of thinner, longer stents The Christ Hospital Heart and Vascular Service Line leading two major clinical trials that will significantly advance stent coated with -

Program PDF Saturday, March 28, 2020 Updated: 02-14-20
Program PDF Saturday, March 28, 2020 Updated: 02-14-20 Special ‐ Events and Meetings Congenital Heart Disease ‐ Scientific Session #5002 Session #602 Fellowship Administrators in Cardiovascular Education and ACHD Cases That Stumped Me Training Meeting, Day 2 Saturday, March 28, 2020, 8:00 a.m. ‐ 9:30 a.m. Saturday, March 28, 2020, 7:30 a.m. ‐ 5:30 p.m. Room S105b Marriott Marquis Chicago, Great Lakes Ballroom A CME Hours: 1.5 / CNE Hours: CME Hours: / CNE Hours: Co‐Chair: C. Huie Lin 7:30 a.m. Co‐Chair: Karen K. Stout Fellowship Administrators in Cardiovascular Education and Training Meeting, Day 2 8:00 a.m. LTGA, Severe AV Valve Regurgitation, Moderately Reduced EF, And Atrial Acute and Stable Ischemic Heart Disease ‐ Scientific Arrhythmia Session #601 Elizabeth Grier Treating Patients With STEMI: What They Didn't Teach You in Dallas, TX Fellowship! Saturday, March 28, 2020, 8:00 a.m. ‐ 9:30 a.m. 8:05 a.m. Room S505a ARS Questions (Pre‐Panel Discussion) CME Hours: 1.5 / CNE Hours: Elizabeth Grier Dallas, TX Co‐Chair: Frederick G. Kushner Co‐Chair: Alexandra J. Lansky 8:07 a.m. Panelist: Alvaro Avezum Panel Discussion: LTGA With AVVR And Reduced EF Panelist: William W. O'Neill Panelist: Jennifer Tremmel Panelist: Jonathan Nathan Menachem Panelist: Joseph A. Dearani 8:00 a.m. Panelist: Michelle Gurvitz Case of a Young Women With STEMI Panelist: David Bradley Jasjit Bhinder Valhalla, NY 8:27 a.m. ARS Questions (Post‐Panel Discussion) 8:05 a.m. Elizabeth Grier Young Women With STEMI: Something Doesn't Make Sense... -

Surgical Management of Transcatheter Heart Valves
Corporate Medical Policy Surgical Management of Transcatheter Heart Valves File Name: surgica l_management_of_transcatheter_heart_valves Origination: 1/2011 Last CAP Review: 6/2021 Next CAP Review: 6/2022 Last Review: 6/2021 Description of Procedure or Service As the proportion of older adults increases in the U.S. population, the incidence of degenerative heart valve disease also increases. Aortic stenosis and mitra l regurgita tion are the most common valvular disorders in adults aged 70 years and older. For patients with severe valve disease, heart valve repair or replacement involving open heart surgery can improve functional status and qua lity of life. A variety of conventional mechanical and bioprosthetic heart valves are readily available. However, some individuals, due to advanced age or co-morbidities, are considered too high risk for open heart surgery. Alternatives to the open heart approach to heart valve replacement are currently being explored. Transcatheter heart valve replacement and repair are relatively new interventional procedures involving the insertion of an artificial heart valve or repair device using a catheter, rather than through open heart surgery, or surgical valve replacement (SAVR). The point of entry is typically either the femoral vein (antegrade) or femora l artery (retrograde), or directly through the myocardium via the apical region of the heart. For pulmonic and aortic valve replacement surgery, an expandable prosthetic heart valve is crimped onto a catheter and then delivered and deployed at the site of the diseased native valve. For valve repair, a small device is delivered by catheter to the mitral valve where the faulty leaflets are clipped together to reduce regurgitation. -

Blood Flow DHO8 7.8, Pg
Blood Flow DHO8 7.8, pg. 190 HS1/2017-2018 Circuits •Pulmonary circuit –The blood pathway between the right of the heart, to the lungs, and back to the left side of the heart. •Systemic circuit –The pathway between the left side of the heart, to the body, and back to the right side of the heart. The Pathway of Blood •Superior & Inferior Vena •Left Atrium Cava •Mitral Valve •Right Atrium •Left Ventricle •Tricuspid Valve •Aortic Semilunar Valve •Right Ventricle •Aorta •Pulmonary Semilunar -Arteries Valve -Arterioles •Pulmonary Artery -Capillaries •Lungs -Venules –Pulmonary Arterioles -Veins –Pulmonary Capillaries –Pulmonary Venules •Pulmonary Vein Blood Flow Through Heart Do You Know? • When blood leaves the left atrium, where does it go next? a) Aorta b) Left ventricle c) Right atrium d) Pulmonary artery And the answer is….A Do You Know? • After blood leaves the right atrium, what valve prevents the back flow? a) Pulmonary b) Mitral c) Tricuspid d) Aortic And the answer is…C Do You Know? • The right ventricle is the chamber of the heart that pumps blood for the pulmonary circulation. Based on this information, blood from the right ventricle is on its way to the _____. a) Liver b) Lungs c) Hands and feet And the answer is…B Do You Know? • Which of the following is correct order of blood flow for the right side of the heart? a) RA, Tricuspid valve, RV, PSLV, pulmonary artery b) RA, PSLV, RV, Tricuspid valve, pulmonary artery c) RA, Tricuspid valve, RV, pulmonary artery , PSLV And the answer is…A Do You Know? • Which of the following is correct order of blood flow for the left side of the heart? a) LA, Bicuspid valve, LV, ASLV, aorta b) LA, ASLV, LV, Bicuspid valve, aorta c) LA, Bicuspid valve, LV, ASLV, aorta And the answer is…C. -

Mitral Valve Prolapse, Arrhythmias, and Sudden Cardiac Death: the Role of Multimodality Imaging to Detect High-Risk Features
diagnostics Review Mitral Valve Prolapse, Arrhythmias, and Sudden Cardiac Death: The Role of Multimodality Imaging to Detect High-Risk Features Anna Giulia Pavon 1,2,*, Pierre Monney 1,2,3 and Juerg Schwitter 1,2,3 1 Cardiac MR Center (CRMC), Lausanne University Hospital (CHUV), 1100 Lausanne, Switzerland; [email protected] (P.M.); [email protected] (J.S.) 2 Cardiovascular Department, Division of Cardiology, Lausanne University Hospital (CHUV), 1100 Lausanne, Switzerland 3 Faculty of Biology and Medicine, University of Lausanne (UniL), 1100 Lausanne, Switzerland * Correspondence: [email protected]; Tel.: +41-775-566-983 Abstract: Mitral valve prolapse (MVP) was first described in the 1960s, and it is usually a benign condition. However, a subtype of patients are known to have a higher incidence of ventricular arrhythmias and sudden cardiac death, the so called “arrhythmic MVP.” In recent years, several studies have been published to identify the most important clinical features to distinguish the benign form from the potentially lethal one in order to personalize patient’s treatment and follow-up. In this review, we specifically focused on red flags for increased arrhythmic risk to whom the cardiologist must be aware of while performing a cardiovascular imaging evaluation in patients with MVP. Keywords: mitral valve prolapse; arrhythmias; cardiovascular magnetic resonance Citation: Pavon, A.G.; Monney, P.; Schwitter, J. Mitral Valve Prolapse, Arrhythmias, and Sudden Cardiac Death: The Role of Multimodality 1. Mitral Valve and Arrhythmias: A Long Story Short Imaging to Detect High-Risk Features. In the recent years, the scientific community has begun to pay increasing attention Diagnostics 2021, 11, 683. -

Valve Repair for Mitral Insufficiency Without Stenosis Richard B
Journal of Insurance Medicine Volume 20, No. I 1988 Mortality Abstract Valve Repair for Mitral Insufficiency Without Stenosis Richard B. Singer, M.D. Consultant Association of Life Insurance Medical Directors of America References: (1) JW Kirklin, ’WIitral Valve Repair for Mitral those with isolated MVR, with or without tricuspid an- Incompetence." Mod Concepts of CV Dis, 56:7-11 (Feb. nuloplasty. The highest perioperative rate of 11.1% was ex- 1987). perienced in the group with associated CBPS, and the rate (2) ALIMDA and Society of Actuaries, ’~¢Iedical was nearly as high when the associated surgery was aortic Risks 1987: Analysis of Mortality and Survival." In final valve replacement. preparation (1988). Despite the complete lack of age/sex information, the author Subjects Studied: A series of 210 patients diagnosed at the has provided an expected survival curve based on "an age- Medical Center of the University of Alabama at Birmingham, sex-race-matched general population," but the source tables 1967-1985 as having mitral insufficiency without stenosis, are not cited. From this curve it has been possible to derive and treated by surgical repair of the mitral valve (MVR) in- and graduate expected annual rates, q/or ~/, as shown in stead of mitral valve replacement. The largest group in the Table B. Although the derivation is reasonably accurate for series consisted of 86 patients with isolated MVR, although the first year, the reader should be cautioned that the an- a few of these also had tricuspid valve annuloplasty. The nual increase of about 8% per year in qZ may be much too remaining patients had associated cardiac surgery: 63 patients high as compared with an increase of about 1% per year with coronary bypass (CBPS); 31 patients with aortic valve found for qZ, all ages combined, from data by age group replacement (AVR); 27 patients with repair of a congenital and sex for a series of patients with mitral valve replace- cardiac defect; two patients with pericardiectomy and one ment in one of the abstracts in reference 2. -

Highlights from the Latest Articles in Ablation and Endovascular Valve Repair
NEWS & VIEWS Research Highlights Highlights from the latest articles in ablation and endovascular valve repair Torsten Konrad*1 Relationship between electrical & Thomas Rostock1 1II Medical Clinic, Department of Electrophysiology, University Medical Center, Johannes pulmonary vein reconnection and Gutenberg-University Mainz, Langenbeckstraße 1, D-55131 Mainz, Germany *Author for correspondence: Tel.: +49 613 117 7218 contact force during initial pulmonary Fax: +49 613 117 5534 [email protected] vein isolation Financial & competing interests disclosure All PVs were initially successfully isolated The authors have no relevant affiliations or financial Evaluation of: Neuzil P, Reddy V, with this technique. In almost half of the involvement with any organization or entity with a Kautzner J et al. Electrical patients, a deflectable sheath was used financial interest in or financial conflict with the reconnection after pulmonary vein during the initial ablation procedure subject matter or materials discussed in the manu- isolation is contingent on contact (mean CF was not different when using script. This includes employment, consultancies, force during initial treatment: a deflectable or conventional sheath). honoraria, stock ownership or options, expert testi- results from the EFFICAS I study. In general, CF was higher in the right mony, grants or patents received or pending, or Circ. Arrhythm. Electrophysiol. 6, PVs than the left PVs. Lowest CFs were royalties. 327–333 (2013). observed during ablation of the left PVs No writing assistance was utilized in the at the anterior superior and anterior infe- production of this manuscript. Pulmonary vein (PV) isolation is the rior aspect of the PVs. The highest CFs most common and effective interven- were documented at the anterior inferior tional treatment for paroxysmal atrial aspect of the right PVs. -

Development of a Simultaneous Cryo-Anchoring and Radiofrequency Ablation Catheter for Percutaneous Treatment of Mitral Valve Prolapse
DEVELOPMENT OF A SIMULTANEOUS CRYO-ANCHORING AND RADIOFREQUENCY ABLATION CATHETER FOR PERCUTANEOUS TREATMENT OF MITRAL VALVE PROLAPSE By Steven Michael Boronyak Thesis Submitted to the Faculty of the Graduate School of Vanderbilt University in partial fulfillment of the requirements for the degree of MASTER OF SCIENCE in Biomedical Engineering May, 2012 Nashville, Tennessee Approved: W. David Merryman, Ph.D. Robert L. Galloway, Ph.D. ACKNOWLEDGEMENTS First, I would like to thank Dr. David Merryman for his guidance and support throughout the last two years. Second, I would like to thank my fellow lab members for making work more fun than it needs to be. Third, this work was funded by the Wallace H. Coulter Foundation, and I thank them, too. Cheers. ii TABLE OF CONTENTS Page ACKNOWLEDGEMENTS ................................................................................................ ii LIST OF FIGURES .......................................................................................................... v I. INTRODUCTION ......................................................................................................... 1 Background.......................................................................................................... 1 Mitral Valve Anatomy and Function ......................................................... 1 Mitral Regurgitation and Mitral Valve Prolapse ........................................ 2 MVP Due to Degenerative MR ................................................................ 3 Repair of the -

Chapter 12 the Cardiovascular System: the Heart Pages
CHAPTER 12 THE CARDIOVASCULAR SYSTEM: THE HEART PAGES 388 - 411 LOCATION & GENERAL FEATURES OF THE HEART TWO CIRCUIT CIRCULATORY SYSTEM DIVISIONS OF THE HEART FOUR CHAMBERS Right Atrium Left Atrium Receives blood from Receives blood from the systemic circuit the pulmonary circuit FOUR CHAMBERS Right Ventricle Left Ventricle Ejects blood into the Ejects blood into the pulmonary circuit systemic circuit FOUR VALVES –ATRIOVENTRICULAR VALVES Right Atrioventricular Left Atrioventricular Valve (AV) Valve (AV) Tricuspid Valve Bicuspid Valve and Mitral Valve FOUR VALVES –SEMILUNAR VALVES Pulmonary valve Aortic Valve Guards entrance to Guards entrance to the pulmonary trunk the aorta FLOW OF BLOOD MAJOR VEINS AND ARTERIES AROUND THE HEART • Arteries carry blood AWAY from the heart • Veins allow blood to VISIT the heart MAJOR VEINS AND ARTERIES ON THE HEART Coronary Circulation – Supplies blood to the muscle tissue of the heart ARTERIES Elastic artery: Large, resilient vessels. pulmonary trunk and aorta Muscular artery: Medium-sized arteries. They distribute blood to skeletal muscles and internal organs. external carotid artery of the neck Arteriole: Smallest of arteries. Lead into capillaries VEINS Large veins: Largest of the veins. Superior and Inferior Vena Cava Medium-sized veins: Medium sized veins. Pulmonary veins Venules: the smallest type of vein. Lead into capillaries CAPILLARIES Exchange of molecules between blood and interstitial fluid. FLOW OF BLOOD THROUGH HEART TISSUES OF THE HEART THE HEART WALL Pericardium Outermost layer Serous membrane Myocardium Middle layer Thick muscle layer Endocardium Inner lining of pumping chambers Continuous with endothelium CARDIAC MUSCLE Depend on oxygen to obtain energy Abundant in mitochondria In contact with several other cardiac muscles Intercalated disks – interlocking membranes of adjacent cells Desmosomes Gap junctions CONNECTIVE TISSUE Wrap around each cardiac muscle cell and tie together adjacent cells. -

Heart Valve Disease: Mitral and Tricuspid Valves
Heart Valve Disease: Mitral and Tricuspid Valves Heart anatomy The heart has two sides, separated by an inner wall called the septum. The right side of the heart pumps blood to the lungs to pick up oxygen. The left side of the heart receives the oxygen- rich blood from the lungs and pumps it to the body. The heart has four chambers and four valves that regulate blood flow. The upper chambers are called the left and right atria, and the lower chambers are called the left and right ventricles. The mitral valve is located on the left side of the heart, between the left atrium and the left ventricle. This valve has two leaflets that allow blood to flow from the lungs to the heart. The tricuspid valve is located on the right side of the heart, between the right atrium and the right ventricle. This valve has three leaflets and its function is to Cardiac Surgery-MATRIx Program -1- prevent blood from leaking back into the right atrium. What is heart valve disease? In heart valve disease, one or more of the valves in your heart does not open or close properly. Heart valve problems may include: • Regurgitation (also called insufficiency)- In this condition, the valve leaflets don't close properly, causing blood to leak backward in your heart. • Stenosis- In valve stenosis, your valve leaflets become thick or stiff, and do not open wide enough. This reduces blood flow through the valve. Blausen.com staff-Own work, CC BY 3.0 Mitral valve disease The most common problems affecting the mitral valve are the inability for the valve to completely open (stenosis) or close (regurgitation). -
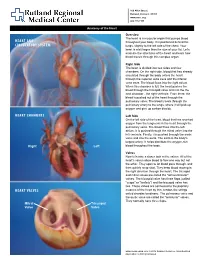
Heart and Circulatory System Heart Chambers
160 Allen Street Rutland, Vermont 05701 www.rrmc.org 802.775.7111 Anatomy of the Heart Overview The heart is a muscular organ that pumps blood HEART AND throughout your body. It is positioned behind the CIRCULATORY SYSTEM lungs, slightly to the left side of the chest. Your heart is a bit larger than the size of your fist. Let's examine the structures of the heart and learn how blood travels through this complex organ. Right Side The heart is divided into two sides and four chambers. On the right side, blood that has already circulated through the body enters the heart through the superior vena cava and the inferior vena cava. The blood flows into the right atrium. When this chamber is full, the heart pushes the blood through the tricuspid valve and into the the next chamber - the right ventricle. From there, the blood is pushed out of the heart through the pulmonary valve. The blood travels through the pulmonary artery to the lungs, where it will pick up oxygen and give up carbon dioxide. HEART CHAMBERS Left Side On the left side of the heart, blood that has received oxygen from the lungs enters the heart through the pulmonary veins. The blood flows into the left atrium. It is pushed through the mitral valve into the left ventricle. Finally, it is pushed through the aortic valve and into the aorta. The aorta is the body's largest artery. It helps distribute the oxygen-rich Right Left blood throughout the body. Valves Now let's take a closer look at the valves. -

Evolution of Risk Factors Influencing Early Mortality of the Arterial Switch
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Elsevier - Publisher Connector Journal of the American College of Cardiology Vol. 33, No. 6, 1999 © 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00071-6 Evolution of Risk Factors Influencing Early Mortality of the Arterial Switch Operation Elizabeth D. Blume, MD,*‡ Karen Altmann, MD,*§ John E. Mayer, MD, FACC,†‡ Steven D. Colan, MD, FACC,*‡ Kimberlee Gauvreau, ScD,*‡ Tal Geva, MD, AFACC*‡ Boston, Massachusetts and New York, New York OBJECTIVES The present study was undertaken to determine the independent risk factors for early mortality in the current era after arterial switch operation (ASO). BACKGROUND Prior reports on factors affecting outcome of the ASO demonstrated that abnormal coronary arterial patterns were associated with increased risk of early mortality. As diagnostic, surgical and perioperative management techniques continue to evolve, the risk factors for the ASO may have changed. METHODS All patients who underwent the ASO at Children’s Hospital, Boston between January 1, 1992 and December 31, 1996 were included. Hospital charts, echocardiographic and cardiac catheterization data and operative reports of all patients were reviewed. Demographics and preoperative, intraoperative and postoperative variables were recorded. RESULTS Of the 223 patients included in the study (median age at ASO 5 6 days and median weight 5 3.5 kg), 26 patients had aortic arch obstruction or interruption, 12 had Taussig-Bing anomaly, 12 had multiple ventricular septal defects, 8 had right ventricular hypoplasia and 6 were premature.