Limping Child
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Evaluation of the Limping Child
Current Concept Review Evaluation of the Limping Child Jessica Burns, MD, MPH; Scott Mubarak, MD Rady Children’s Hospital, San Diego, CA Abstract: Prompt evaluation of a younger child (age <5) with gait disturbance or refusal to walk is necessary to distinguish orthopedic urgency (trauma or infection) from relatively benign processes and chronic problems such as arthritis. Physical examination should include evaluation of gait, supine and simulated prone hip examination (on the parent’s lap to keep the child comfortable), and the crawl test. There are six radiographic views of the lower extremities that can assist in the diagnosis. In conjunction with the detailed history, a thorough physical exam, and radiographs from the orthopedic provider can determine the need for laboratory tests and other imaging. Key Concepts: • Evaluation of the limping child begins with a thorough history. • Physical examination of the limping child can be optimized by utilizing the parent to hold the child while the examiner moves the extremities and checks the back. • Six screening radiographs can be obtained to assist in making the correct diagnosis. • Laboratory analysis and magnetic resonance imaging can be obtained if the diagnosis remains elusive. Introduction Evaluation of gait disturbance in the younger child is an symptoms. Utilizing the parent in the physical important skill for the pediatric orthopedic surgeon. examination can help elicit a more detailed examination Although the true incidence is unknown, it is estimated of the child. Focused radiographs can then be utilized to that there are 1.8 per thousand children that will present support a suspected diagnosis. From there, the need for to the pediatric emergency department with complaint of laboratory analysis and further advanced imaging can be gait disturbance. -

Joint Pains UHL Childrens Hospital Guideline
LRI Children’s Hospital Joint Pains in Children Staff relevant to: Children’s Medical and Nursing Staff working within UHL Children’s Hospital Team approval date: March 2019 Version: 2 Revision due: March 2022 Written by: Dr A Sridhar, Consultant Paediatrician/Paediatric Rheumatology Trust Ref: C89/2016 1. Introduction and Who Guideline applies to THIS IS AN AREA WHERE CLINICAL ASSESSMENT IS USUALLY MUCH MORE IMPORTANT THAN “ROUTINE INVESTIGATIONS” SINGLE PAINFUL JOINT The most important diagnosis to consider is SEPTIC ARTHRITIS Can occur: In Any Joint All Age Groups May be co-existing osteomyelitis (particularly in very young) Related documents: Management of the limping child UHL - C13/2016 Septic Arthritis UHL – B47/2017 Differential diagnosis: 1. History of Injury: Traumatic, Acute Joint bleed (May be the first presentation of Haemophilia or other bleeding disorder) - Haemarthroses 2. Significant Fever and Pain: Septic arthritis or Osteomyelitis 3. Recent Viral illness, diarrhoea, Tonsillitis: Reactive Arthritis- 7-14 days after the illness, Fever may not be present 4. History of IBD: Usually monoarthritis of large joints reflects activity 5. Vascultic Rash: HSP or other forms of vasculitis Page 1 of 6 Title: Joint Pains in Children V:2 Approved by Children’s Clinical Practice Group: March 2019 Trust Ref: C89/2016 Next Review: March 2022 NB: Paper copies of this document may not be most recent version. The definitive version is held in the Trust Policy and Guideline Library. 6. Recent Drug ingestion: Serum sickness often associated with Urticarial rash 7. Bone pain, Lymphadenopathy, Hepato-splenomegaly: Leukemia, Lymphoma, Neuroblastoma, bone tumour (h/o nocturnal bone pain) 8. -

Hip Osteoarthritis Information
Bòrd SSN nan Eilean Siar NHS Western Isles Physiotherapy Department Hip Osteoarthritis An Information Guide for Patients and Carers Page 1 Contents Section 1: What is osteoarthritis? 3 Contributing factors to osteoarthritis Section 2: Diagnosis and symptoms 5 Symptoms Diagnosis Flare up of symptoms Section 3: Gentle hip exercises for flare ups 7 Section 4: Living with osteoarthritis 8 How with osteoarthritis affect me? What you can do to help yourself Section 5: Range of movement exercises 9 Section 6: Strengthening exercises 10 Other forms of exercise Section 7: Other treatments 13 Living with osteoarthritis Surgery Section 8: Local groups and activities 14 Page 2 What is osteoarthritis? This booklet is designed to give you some useful information following your diagnosis of osteoarthritis. Osteoarthritis is a very common condition which can affect any joint causing pain, and stiffness. It’s most likely to affect the joints that bear most of our weight, such as the hips, as they have to take extreme stresses, twists and turns, therefore osteoarthritis of the hip is very common and can affect either one or both hips. A normal joint A joint with mild osteoarthritis In a healthy joint, a coating of smooth and slippery tissue, called cartilage, covers the surface of the bones and helps the bones to move freely against each other. When a joint develops osteoarthritis, the bones lose their smooth surfaces and they become rougher and the cartilage thins. The repair process of the cartilage is sometimes not sufficient as we age. Almost all of us will develop osteoarthritis in some of our joints as we get older, though we may not even be aware of it. -

Arthrofibrosis-Ebook-Small.Pdf
Table of Contents About the Authors 3 Introduction 4 Basic Knee Anatomy 6 What is Knee Arthrofibrosis? 10 Basic Definition and Classification Systems 10 Structures Involved With Loss of Knee Flexion 12 Structures Involved With Loss of Knee Extension 13 Effects of Loss of Knee Motion 13 How Does Knee Arthrofibrosis Happen? 15 How the Body Normally Heals After an Injury or Surgery 15 Abnormal Healing Response in Arthrofibrosis 16 Risk Factors Associated with Secondary Arthrofibrosis 16 How is Knee Arthrofibrosis Diagnosed? 19 Early Detection 19 Established Arthrofibrosis 20 Other Reasons for Limitations of Knee Motion 22 Prevention of Knee Arthrofibrosis 23 Physical Therapy: Setting Goals Before Surgery 23 Exercises to Regain Knee Motion 24 Exercises to Regain Strength and Knee Function 25 Treatment of Inflammation, Pain, Hemarthrosis, Infection 32 First-Line Treatment 32 Medications 32 Overpressure Exercises 33 Gentle Ranging of the Knee Under Anesthesia 36 In-Patient Physical Therapy Program 37 Operative Options 38 Arthroscopic Lysis of Adhesions and Removal of Scar Tissues 38 Open Z-Plasty Release Medial and Lateral Retinacular Tissues 41 Open Posterior Capsulotomy 44 Important Comments Regarding These Operations 47 Questionable Treatment Options 47 Ultrasound 47 Extracorporeal Shockwave Therapy 48 Inflammatory Diet 48 Patellar Infera: Recognition, Prevention, Treatment 48 Recognition 48 Prevention 49 Treating Early Patella Infera 49 Treating Chronic Patella Infera 50 Complex Regional Pain Syndrome (CRPS) 51 What is it? 51 The Human Nervous System 51 CRPS Types I and II 52 Potential Causes of CRPS 52 Diagnosis 53 Treatment 54 Acronyms and References 56 3 About the Authors Dr. Frank Noyes is an internationally recognized orthopaedic surgeon and researcher who has specialized in the treatment of knee injuries and disorders for nearly 4 decades. -
Letters to the Editor
Letters to the Editor Peritonitis and cervical arthritis early stages of the disease or as the single as presenting manifestations of joint implicated (6-9). In our patient, who presented with fever, neck stiffness and systemic juvenile idiopathic signs of peritoneal infl ammation, meningi- arthritis tis and peritonitis secondary to appendicitis were excluded. The associated evanescent Sirs, macular salmon-pink rash and cervical Early involvement of the cervical spine is spine involvement suggested sJIA. Diag- uncommon and peritonitis is a rare extra- nosis was confi rmed by the outcome with articular presentation in systemic-onset juv- a relapse. enile idiopathic arthritis (sJIA) (1-3). Over 21 years we observed 264 cases of We describe a previously healthy 4-year- JIA, of whom 3 had monoarticular C1-C2 old boy with C1-C2 arthritis and peritonitis involvement lasting for several months (2 presenting as the initial manifestations of oligoarthritis previous to this case). sJIA. He was admitted following 2 days of We are not aware of any other published fever, lethargy, vomiting, abdominal pain cases of sJIA who presented with C1-C2 and neck stiffness. A blood count showed arthritis and peritonitis simultaneously . 20100 leucocytes/ml (74% neutrophils), the C-reactive protein was 2.8 mg/dl. Cerebral A. VAZ, MD spinal fl uid analysis excluded meningitis. C. VEIGA, MD Twelve hours post admission he appeared P. ESTANQUEIRO, MD clinically septic, developed abdominal M. SALGADO, MD signs suggestive of peritonitis and C-reac- Department of Pediatric Rheumatology, tive protein increased to 10 mg/dl. Antibiot- Fig. 1. Cervical MRI: arrows showing bilateral effu- Hospital Pediátrico de Coimbra, Portugal. -

Evaluating the Limping Child: a Rheumatology Perspective
SCIENCE OF MEDICINE | Evaluating the Limping Child: A Rheumatology Perspective by Reema Syed, MD Taking a detailed Abstract important clues to the underlying history and completing Children often present diagnosis. Inquiring about recent a thorough evaluation to health care providers for travel will help with infectious causes. will help hone in on evaluation of limp. Having Associated pain versus painless limp raises different possibilities. the underlying cause. the knowledge of the different causes of leg pains both in the This article will review acute and chronic settings will Examination important causes of limp help in diagnosis, treatment, Assessing a child’s gait is crucial from the rheumatologist’s and referrals to subspecialists in completing an evaluation for lower viewpoint. in a timely manner. Taking a extremity complaints. Is the child detailed history and completing unable to bear weight or is the child a thorough evaluation will holding the affected joint in a fixed help hone in on the underlying position are important questions to cause. This article will review address and are signs of more serious important causes of limp from the issues. If the child appears toxic or has rheumatologist’s viewpoint. high fevers infectious etiologies need to be excluded. Introduction An antalgic gait signifies pathology A child may present to a primary in the hip, knee or ankle. A child with care provider with a limp due to acute antalgic gait will take a shorter stance on the affected limb to avoid bearing more urgent issues like infections weight on the diseased painful joint. or for more chronic issues like A circumduction motion of the hip is juvenile idiopathic arthritis or other also a clue of a painful joint aggravated rheumatologic issues. -
Limping Child
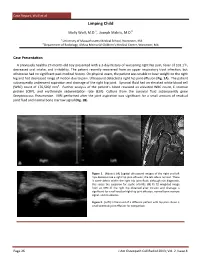
Case Report, Wolf et al Limping Child a b Molly Wolf, M.D. , Joseph Makris, M.D. a University of Massachusetts Medical School, Worcester, MA b Department of Radiology, UMass Memorial Children’s Medical Center, Worcester, MA Case Presentation A previously healthy 27-month-old boy presented with a 3-day history of worsening right hip pain, fever of 103.1oF, decreased oral intake, and irritability. The patient recently recovered from an upper respiratory tract infection, but otherwise had no significant past medical history. On physical exam, the patient was unable to bear weight on the right leg and had decreased range of motion due to pain. Ultrasound detected a right hip joint effusion (Fig. 1A). The patient subsequently underwent aspiration and drainage of the right hip joint. Synovial fluid had an elevated white blood cell (WBC) count of 176,500/ mm3. Further analysis of the patient’s blood revealed an elevated WBC count, C reactive protein (CRP), and erythrocyte sedimentation rate (ESR). Culture from the synovial fluid subsequently grew Streptococcus Pneumoniae. MRI performed after the joint aspiration was significant for a small amount of residual joint fluid and normal bone marrow signal (Fig. 1B). Figure 1. (Above): (A) Sagittal ultrasound images of the right and left hips demonstrate a right hip joint effusion; the left side is normal. There is some debris within the right hip joint fluid; although not diagnostic, this raises the suspicion for septic arthritis. (B) FS T2 weighted image from an MRI of the right hip obtained after incision and drainage is significant for small residual right hip joint effusion, normal bone marrow signal, and no abscess. -

Joint Pain in Children: Initial Evaluation and When to Refer
Joint Pain in Children: Initial Evaluation and When to Refer C. Egla Rabinovich MD, MPH Professor of Pediatrics Division Chief, Duke Pediatric Rheumatology Disclosures • No relevant disclosures Educational Objective • Develop a practical approach to joint pain in children • Understand differential, emphasis on common causes • Discuss rheumatologic causes of arthralgia • Develop plans for initial work-up Musculoskeletal Pain in Children Arthralgia is extremely common in childhood 5-30% of children have chronic pain complaints More common in girls May last years Most have benign etiology Differential of joint pain • Age dependent • 2 year old will not have repetitive use injuries • 15 year old will not develop growing pains • Some gender dependence • Adolescent females and knee pain • Need to keep a broad differential in mind • Think thru the differential • The work up • And then possible referral Common Causes of Joint Pain Trauma 30% Overuse 28% Patello-femoral syndrome, Osgood- Schlatter Structural 18% Hypermobility syndrome Congenital hip dysplasia Growing pains 8% Systemic Illness & Joint Pain Arthralgias are common manifestations of systemic illnesses Infections IBD Malignancy Crohn’s disease Arthralgias: systemic disease • Malignancy • Bone/soft tissue tumor • Bone marrow cancer (ALL/neuroblastoma) • Endocrine disease • Thyroid disease • IDDM • Gastrointestinal disease • Celiac disease • IBD • Autoimmune hepatitis • Infectious disease • Viral (EBV/parvovirus) • Fever • Streptococcus • Genetic • Fabry • Lysosomal storage -

Recurrent Limp in a Young Boy F Falcini, T Giani, a Lippi, M Resti, G Simonini
500 Ann Rheum Dis: first published as 10.1136/ard.2004.023234 on 11 February 2005. Downloaded from LETTERS Recurrent limp in a young boy F Falcini, T Giani, A Lippi, M Resti, G Simonini ............................................................................................................................... Ann Rheum Dis 2005;64:500. doi: 10.1136/ard.2004.026971 child aged 2 years 8 months was referred to our rheumatology unit for evaluation of recurrent acute Apain and limited motion of the left hip. In March 2003 he had been seen at the emergency department of our hospital for a painful, flexed, and abducted left hip. On that occasion, the erythrocyte sedimentation rate (ESR) was 35 mm/1st h, white blood cells (WBC) 8.36109/l, and C reactive protein (CRP) 32.7 mg/l (normal value ,5 mg/l). Ultrasound of the joint showed mild effusion with normal synovial thickness on the left hip, and a transient hip synovitis (THS) was diagnosed. The pain and limp responded to a 3 day course of anti-inflammatory drug treatment. One month later, the boy returned again with a limp and pain in the left hip. Because the symptoms resolved over few days with analgesic administration, laboratory tests or ultrasound were not performed. The child was well up to November 2003, when the hip pain and limping returned without any other musculoskele- tal or constitutional symptoms. Abnormal laboratory results Figure 1 Bone marrow aspirate showing substitution of normal were as follows: ESR 34 mm/1st h, CRP 6.5 mg/l, WBC haematopoiesis with myeloblasts: myeloblastic leukaemia FAB M2. 5.96109/l (neutrophils 45.3%, lymphocytes 44.3%), haemo- globin 109 g/l, platelet count 1276109/l, serum lactate Our case suggests that malignancy should be considered dehydrogenase (LDH) 1216 U/l (normal value ,560). -

The Child with a Limp
The child with a limp MARVIN B HARPER MD DIVISION OF EMERGENCY MEDICINE BOSTON CHILDREN’S HOSPITAL HARVARD MEDICAL SCHOOL No conflicts of interest No financial disclosures Case 18 month old otherwise well limping since this afternoon. Mom notes some limping but mostly child doesn’t want to stand. She isn’t sure which leg has pain PE: afebrile, antalgic gait favoring the left leg. No swelling noted. Seems to have some pain to palpation of the left lower leg. Toddlers fracture Herman and Martinek. Pediatr in Rev. 2015 Case 3 year old male woke up this morning with complaint of pain in the right leg. Still active and playing but can be seen to be limping. PE afebrile, when sitting still is active and playful. Refuses to fully bear weight on right leg when walking. Allows some flexion/extension at the right hip but seems to have pain with full flexion/extension Given ibuprofen with improvement of symptoms No further studies done Focus diagnoses in the ED In the ED focus on diagnosis of ¡ Fracture ¡ Infection (bone, joint, post-infectious) ¡ SCFE ¡ Tumors ¡ +/- Developmental hip dysplasia Not generally ED diagnosis ¡ Leg length discrepancy ¡ Cerebral palsy ¡ Contractures ¡ Rheumatologic causes Differential diagnosis for septic arthritis Trauma Leukemia Hemarthrosis, Tumor Osteomyelitis, Henoch-Schönlein Reactive effusion purpura Pyomyositis Sickle cell anemia w/VOC Septic bursitis Rheumatologic (e.g. JRA) Lyme Acute rheumatic fever SCFE Legg-Calvé-Perthes Etiology – differential diagnosis for joint concern Age 1 – 3 -

Treatment of Knee Osteoarthritis ERIKA RINGDAHL, MD, and SANDESH PANDIT, MD University of Missouri School of Medicine, Columbia, Missouri
Treatment of Knee Osteoarthritis ERIKA RINGDAHL, MD, and SANDESH PANDIT, MD University of Missouri School of Medicine, Columbia, Missouri Knee osteoarthritis is a common disabling condition that affects more than one-third of persons older than 65 years. Exercise, weight loss, physical therapy, intra-articular corticosteroid injections, and the use of nonsteroidal anti-inflammatory drugs and braces or heel wedges decrease pain and improve function. Acetaminophen, glu- cosamine, ginger, S-adenosylmethionine (SAM-e), capsaicin cream, topical nonsteroidal anti-inflammatory drugs, acupuncture, and tai chi may offer some benefit. Tramadol has a poor trade-off between risks and benefits and is not routinely recommended. Opioids are being used more often in patients with moderate to severe pain or diminished quality of life, but patients receiving these drugs must be carefully selected and monitored because of the inherent adverse effects. Intra-articular corticosteroid injections are effective, but evidence for injection of hyaluronic acid is mixed. Arthroscopic sur- gery has been shown to have no benefit in knee osteoarthritis. Total joint arthroplasty of the knee should be considered when conserva- tive symptomatic management is ineffective. (Am Fam Physician. 2011;83(11):1287-1292. Copyright © 2011 American Academy of Family Physicians.) ILLUSTRATION TODD BY BUCK ▲ Patient information: steoarthritis is a degenera- widespread prevalence, however, the precise A handout on knee osteo- tive joint disease occurring etiology, pathogenesis, and progression of arthritis, written by the primarily in older adults. It is osteoarthritis are unknown. Several factors authors of this article, is provided on page 1294. characterized by erosion of the may make a person vulnerable to the disease O articular cartilage, hypertrophy of bone at (Table 1). -

Child with Limp Handout March 2018
www.pmmonline.org A free online interactive information resource for clinicians The limping child Helen Foster Professor of Paediatric Rheumatology Newcastle University Honorary Consultant Great North Children’s Hospital Newcastle Hospitals NHS Foundation Trust Newcastle upon Tyne [email protected] Arch Dis Child Educ Pract Ed 2012;97:185-193 Why is this topic important? • Limp is a common presentation – Spectrum of causes from benign to serious • Diagnosis needs careful clinical assessment – Doctors report low self-confidence in musculoskeletal clinical skills* • Delay in diagnosis is common** – Delay in diagnosis has adverse effect on outcome *Jandial 2009, *Lanyon 2004, Glazier 2004, Bond 2007, Hergenroder 2009 **Foster 2007, 2010, Rapley 2013 Objectives • Define limp • Describe the spectrum of causes • Describe an approach to assessment • Red flags and Pitfalls What is limp ? • Antalgic (painful) gait – Acute (1-2 days) – Chronic (> 6/52)* – Sub-acute • Abnormal gait patterns (usually not acute) – Neurological Causes of limp • Classification by anatomy • Classification by pathology • Classification by age Causes of limp • Classification by anatomy – Skin / Soft tissue – Muscle – Joint – Bone – Referred • Classification by pathology – Trauma – Infection – Malignancy – Inflammatory – Congenital – Psychosocial Causes of limp * * * * * Red flags • Potential life threatening – Malignancy – Infection – Non accidental injury •Systemic upset (fever, malaise, weight loss, sweats, anorexia) •Bone pain / joint pain •Refractory or unremitting