An Aerodigestive Perspective
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Management of Airway Obstruction and Stridor in Pediatric Patients
November 2017 Management of Airway Volume 14, Number 11 Obstruction and Stridor in Authors Ashley Marchese, MD Department of Pediatrics, Yale-New Haven Hospital, New Haven, CT Pediatric Patients Melissa L. Langhan, MD, MHS Associate Professor of Pediatrics and Emergency Medicine; Fellowship Director, Director of Education, Pediatric Emergency Abstract Medicine, Yale University School of Medicine, New Haven, CT Peer Reviewers Stridor is a result of turbulent air-flow through the trachea from Steven S. Bin, MD upper airway obstruction, and although in children it is often Associate Clinical Professor of Emergency Medicine and Pediatrics; Medical Director, Emergency Department, UCSF School of Medicine, due to croup, it can also be caused by noninfectious and/or con- Benioff Children’s Hospital, San Francisco, CA genital conditions as well as life-threatening etiologies. The his- Alexander Toledo, DO, PharmD, FAAEM, FAAP tory and physical examination guide initial management, which Chief, Section of Pediatric Emergency Medicine; Director, Pediatric Emergency Department, Arizona Children’s Center at Maricopa includes reduction of airway inflammation, treatment of bacterial Medical Center, Phoenix, AZ infection, and, less often, imaging, emergent airway stabilization, Prior to beginning this activity, see “Physician CME Information” or surgical management. This issue discusses the most common on the back page. as well as the life-threatening etiologies of acute and chronic stridor and its management in the emergency department. Editor-in-Chief -

Domestic Violence: the Shaken Adult Syndrome
138 J Accid Emerg Med 2000;17:138–139 J Accid Emerg Med: first published as 10.1136/emj.17.2.139 on 1 March 2000. Downloaded from CASE REPORTS Domestic violence: the shaken adult syndrome T D Carrigan, E Walker, S Barnes Abstract Her initial blood pressure was 119/72 mm A case of domestic violence is reported. Hg, pulse 88 beats/min, her pupils were equal The patient presented with the triad of and reactive directly and consensually, and her injuries associated with the shaking of Glasgow coma score was 13/15 (she was infants: retinal haemorrhages, subdural confused and was opening her eyes to com- haematoma, and patterned bruising; this mand). Examination of the head showed bilat- has been described as the shaken adult eral periorbital ecchymoses, nasal bridge swell- syndrome. This case report reflects the ing and epistaxis, a right frontal abrasion, and diYculties in diagnosing domestic vio- an occipital scalp haematoma. Ecchymoses lence in the accident and emergency were also noted on her back and buttocks, setting. being linear in fashion on both upper arms, (J Accid Emerg Med 2000;17:138–139) and her underpants were torn. Initial skull and Keywords: domestic violence; women; assault facial x ray films were normal, and she was admitted under the care of A&E for neurologi- cal observations. Domestic violence is an under-reported and Over the next 24 hours, her Glasgow coma major public health problem that often first score improved to 15/15, but she had vomited presents to the accident and emergency (A&E) five times and complained that her vision department. -

Stridor in the Newborn
Stridor in the Newborn Andrew E. Bluher, MD, David H. Darrow, MD, DDS* KEYWORDS Stridor Newborn Neonate Neonatal Laryngomalacia Larynx Trachea KEY POINTS Stridor originates from laryngeal subsites (supraglottis, glottis, subglottis) or the trachea; a snoring sound originating from the pharynx is more appropriately considered stertor. Stridor is characterized by its volume, pitch, presence on inspiration or expiration, and severity with change in state (awake vs asleep) and position (prone vs supine). Laryngomalacia is the most common cause of neonatal stridor, and most cases can be managed conservatively provided the diagnosis is made with certainty. Premature babies, especially those with a history of intubation, are at risk for subglottic pathologic condition, Changes in voice associated with stridor suggest glottic pathologic condition and a need for otolaryngology referral. INTRODUCTION Families and practitioners alike may understandably be alarmed by stridor occurring in a newborn. An understanding of the presentation and differential diagnosis of neonatal stridor is vital in determining whether to manage the child with further observation in the primary care setting, specialist referral, or urgent inpatient care. In most cases, the management of neonatal stridor is outside the purview of the pediatric primary care provider. The goal of this review is not, therefore, to present an exhaustive review of causes of neonatal stridor, but rather to provide an approach to the stridulous newborn that can be used effectively in the assessment and triage of such patients. Definitions The neonatal period is defined by the World Health Organization as the first 28 days of age. For the purposes of this discussion, the newborn period includes the first 3 months of age. -

Snoring and Stertor Are Associated with More Sleep Disturbance Than Apneas and Hypopneas in Pediatric SDB
Sleep and Breathing (2019) 23:1245–1254 https://doi.org/10.1007/s11325-019-01809-3 SLEEP BREATHING PHYSIOLOGY AND DISORDERS • ORIGINAL ARTICLE Snoring and stertor are associated with more sleep disturbance than apneas and hypopneas in pediatric SDB Mark B. Norman1 & Henley C. Harrison2 & Karen A. Waters1,3 & Colin E. Sullivan1,3 Received: 2 November 2018 /Revised: 26 January 2019 /Accepted: 19 February 2019 /Published online: 1 March 2019 # The Author(s) 2019 Abstract Purpose Polysomnography is not recommended for children at home and does not adequately capture partial upper airway obstruction (snoring and stertor), the dominant pathology in pediatric sleep-disordered breathing. New methods are required for assessment. Aims were to assess sleep disruption linked to partial upper airway obstruction and to evaluate unattended Sonomat use in a large group of children at home. Methods Children with suspected obstructive sleep apnea (OSA) had a single home-based Sonomat recording (n = 231). Quantification of breath sound recordings allowed identification of snoring, stertor, and apneas/hypopneas. Movement signals were used to measure quiescent (sleep) time and sleep disruption. Results Successful recordings occurred in 213 (92%) and 113 (53%) had no OSA whereas only 11 (5%) had no partial obstruc- tion. Snore/stertor occurred more frequently (15.3 [5.4, 30.1] events/h) and for a longer total duration (69.9 min [15.7, 140.9]) than obstructive/mixed apneas and hypopneas (0.8 [0.0, 4.7] events/h, 1.2 min [0.0, 8.5]); both p < 0.0001. Many non-OSA children had more partial obstruction than those with OSA. -
PE3334 Difficulty Swallowing (Dysphagia)
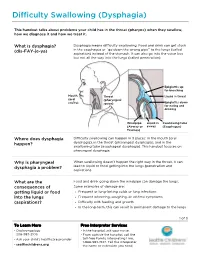
Difficulty Swallowing (Dysphagia) This handout talks about problems your child has in the throat (pharynx) when they swallow, how we diagnose it and how we treat it. What is dysphagia? Dysphagia means difficulty swallowing. Food and drink can get stuck (dis-FAY-je-ya) in the esophagus or “go down the wrong pipe” to the lungs (called aspiration) instead of the stomach. It can also go into the voice box but not all the way into the lungs (called penetration). Epiglottis up for breathing Mouth Throat Liquid in throat (oral (pharyngeal cavity) space) Epiglottis down for eating and drinking Windpipe Liquid in Swallowing tube (Airway or airway (Esophagus) Trachea) Where does dysphagia Difficulty swallowing can happen in 3 places: in the mouth (oral happen? dysphagia), in the throat (pharyngeal dysphagia), and in the swallowing tube (esophageal dysphagia). This handout focuses on pharyngeal dysphagia. Why is pharyngeal When swallowing doesn’t happen the right way in the throat, it can dysphagia a problem? lead to liquid or food getting into the lungs (penetration and aspiration). What are the Food and drink going down the windpipe can damage the lungs. consequences of Some examples of damage are: getting liquid or food • Frequent or long-lasting colds or lung infections into the lungs • Frequent wheezing, coughing, or asthma symptoms (aspiration)? • Difficulty with feeding and growth • In the long-term, this can result in permanent damage to the lungs 1 of 3 To Learn More Free Interpreter Services • Otolaryngology • In the hospital, ask your nurse. 206-987-2105 • From outside the hospital, call the • Ask your child’s healthcare provider toll-free Family Interpreting Line, 1-866-583-1527. -

INITIAL APPROACH to the EMERGENT RESPIRATORY PATIENT Vince Thawley, VMD, DACVECC University of Pennsylvania, Philadelphia, PA
INITIAL APPROACH TO THE EMERGENT RESPIRATORY PATIENT Vince Thawley, VMD, DACVECC University of Pennsylvania, Philadelphia, PA Introduction Respiratory distress is a commonly encountered, and truly life-threatening, emergency presentation. Successful management of the emergent respiratory patient is contingent upon rapid assessment and stabilization, and action taken during the first minutes to hours often has a major impact on patient outcome. While diagnostic imaging is undoubtedly a crucial part of the workup, patients at presentation may be too unstable to safely achieve imaging and clinicians may be called upon to institute empiric therapy based primarily on history, physical exam and limited diagnostics. This lecture will cover the initial evaluation and stabilization of the emergent respiratory patient, with a particular emphasis on clues from the physical exam that may help localize the cause of respiratory distress. Additionally, we will discuss ‘cage-side’ diagnostics, including ultrasound and cardiac biomarkers, which may be useful in the working up these patients. Establishing an airway The first priority in the dyspneic patient is ensuring a patent airway. Signs of an obstructed airway can include stertorous or stridorous breathing or increased respiratory effort with minimal air movement heard when auscultating over the trachea. If an airway obstruction is present efforts should be made to either remove or bypass the obstruction. Clinicians should be prepared to anesthetize and intubate patients if necessary to provide a patent airway. Supplies to have on hand for difficult intubations include a variety of endotracheal tube sizes, stylets for small endotracheal tubes, a laryngoscope with both small and large blades, and instruments for suctioning the oropharynx. -

Severe Peri-Ictal Respiratory Dysfunction Is Common in Dravet Syndrome
The Journal of Clinical Investigation RESEARCH ARTICLE Severe peri-ictal respiratory dysfunction is common in Dravet syndrome YuJaung Kim,1,2 Eduardo Bravo,1 Caitlin K. Thirnbeck,1 Lori A. Smith-Mellecker,1 Se Hee Kim,3 Brian K. Gehlbach,4 Linda C. Laux,3 Xiuqiong Zhou,1 Douglas R. Nordli Jr.,3 and George B. Richerson1,5,6 1Department of Neurology and 2Department of Biomedical Engineering, University of Iowa, Iowa City, Iowa, USA. 3Division of Pediatric Neurology, Northwestern University, Chicago, Illinois, USA. 4Department of Internal Medicine and 5Department of Molecular Physiology and Biophysics, University of Iowa, Iowa City, Iowa, USA. 6Neurology Service, Veterans Affairs Medical Center, Iowa City, Iowa, USA. Dravet syndrome (DS) is a severe childhood-onset epilepsy commonly due to mutations of the sodium channel gene SCN1A. Patients with DS have a high risk of sudden unexplained death in epilepsy (SUDEP), widely believed to be due to cardiac mechanisms. Here we show that patients with DS commonly have peri-ictal respiratory dysfunction. One patient had severe and prolonged postictal hypoventilation during video EEG monitoring and died later of SUDEP. Mice with an Scn1aR1407X/+ loss- of-function mutation were monitored and died after spontaneous and heat-induced seizures due to central apnea followed by progressive bradycardia. Death could be prevented with mechanical ventilation after seizures were induced by hyperthermia or maximal electroshock. Muscarinic receptor antagonists did not prevent bradycardia or death when given at doses selective for peripheral parasympathetic blockade, whereas apnea, bradycardia, and death were prevented by the same drugs given at doses high enough to cross the blood-brain barrier. -

Proceedings from the 2011 Annual Meeting of the American College of Physicians, Wisconsin Chapter
PROCEEDINGS Proceedings from the 2011 Annual Meeting of the American College of Physicians, Wisconsin Chapter The Wisconsin Chapter of the American College of Physicians held its annual meeting in evaluate the temporal relationship between Wisconsin Dells, September 9-11, 2011. Internal medicine residents from each of Wisconsin’s 5 onset of atopic dermatitis (AD) and EE residency programs presented their research and/or unusual clinical experiences via posters diagnosis. and vignettes. Methods: A retrospective cohort study was conducted in a population-based cohort. PRESENTED POSTERS ger length of hospitalization (OR, 0.72, Esophageal biopsy reports from 1995- Effect of Hyperglycemia on Outcomes 95% CI, 0.54-0.96, P = 0.03). Forty-one 1997 and 2005-2007 were screened using in Acute Exacerbations of Chronic patients (19%) were readmitted to the SNOMED (Systematized Nomenclature Obstructive Pulmonary Disease hospital within 30 days of discharge from of Medicine) to identify patients with Narendranath Epperla, MD, Yusuf Kasirye, index hospitalization. Adjusting for previ- pathologic confirmed or suspected EE. MD, Melissa Simpson, PhD, Hong Liang, PhD, ous covariates and length of hospitalization, Histopathology reports in which EE could Chaitanya Mamillapalli, MD, Steven Yale, MD; BG was not associated with 30-day hospital not be excluded and those with features sug- Departments of Internal Medicine, Biostatistics, readmission (OR, 0.82, 95% CI, 0.54-1.22, and Clinical Research and Marshfield Clinic gestive of EE were reviewed. Cases of esoph- Research Foundation; Marshfield Clinic, P = 0.32). Nine patients (4%) died within agitis due to chemicals, drugs, infections, Marshfield, Wis 90 days of their index hospitalization. -

Diagnostic and Therapeutic Approach to Upper Airway Obstructions
Diagnostic and therapeutic approach to upper airway obstructions Gerhard Oechtering University of Leipzig, Veterinary Faculty, Small Animal Department, ENT-Unit Leipzig, Germany Overview of the Issue The diagnostic approach to obstructions of the upper airways bases on both a thorough anamnesis (including among other things questions on breathing at rest, after exercise, during sleep, through mouth or nose) and a careful adspection and listening to breathing sounds and possible stridores. Distinguishing stenoses of the oro-laryngeal airway from those of the nasal and nasopharyngeal airway is a primary goal and can be very helpful for planning subsequent examinations. If an obstruction of the nasal and or nasopharyngeal airway is suspected, usually an examination under anesthesia is necessary. These passageways are not accessible for the naked eye and we need diagnostic aids like endoscopy and/or computed tomography. Plain radiographs of this region can be helpful but usually are clearly inferior to CT information. Key Clinical Diagnostic Points In dogs and cats, endoscopic examination of the upper respiratory tract from the nares down to the carina is done primarily with ridging endoscopes. Several factors determine the quality of the results. 1. Quality of endoscopes, light source, camera and documentation unit 2. Endoscopic experience and technique of the examiner 3. The examiners anatomic knowledge of the specific region 4. Patient preparation and positioning 5. Anesthesia and ventilatory support 6. Variety of supporting equipment Endoscopes for anterior and posterior rhinoscopy differ in size and angle of view. Common types are: 1. Diameter: Ø 2.7 mm (most dog breeds) and 1.9 mm (small dogs and cats) 2. -

Respiratory Distress in the Newborn
Respiratory Distress in the Newborn Suzanne Reuter, MD,* Chuanpit Moser, MD,† Michelle Baack, MD*‡ *Department of Neonatal-Perinatal Medicine, Sanford School of Medicine–University of South Dakota, Sanford Children’s Specialty Clinic, Sioux Falls, SD. †Department of Pediatric Pulmonology, Sanford School of Medicine–University of South Dakota, Sanford Children’s Specialty Clinic, Sioux Falls, SD. ‡Sanford Children’s Health Research Center, Sioux Falls, SD. Educational Gap Respiratory distress is common, affecting up to 7% of all term newborns, (1) and is increasingly common in even modest prematurity. Preventive and therapeutic measures for some of the most common underlying causes are well studied and when implemented can reduce the burden of disease. (2)(3)(4)(5)(6)(7)(8) Failure to readily recognize symptoms and treat the underlying cause of respiratory distress in the newborn can lead to short- and long-term complications, including chronic lung disease, respiratory failure, and even death. Objectives After completing this article, the reader should be able to: 1. Use a physiologic approach to understand and differentially diagnose the most common causes of respiratory distress in the newborn infant. 2. Distinguish pulmonary disease from airway, cardiovascular, and other systemic causes of respiratory distress in the newborn. 3. Appreciate the risks associated with late preterm (34–36 weeks’ gestation) and early term (37–38 weeks’ gestation) deliveries, especially AUTHOR DISCLOSURES Drs Reuter, Moser, by caesarean section. and Baack have disclosed no financial 4. Recognize clinical symptoms and radiographic patterns that reflect relationships relevant to this article. This commentary does not contain information transient tachypnea of the newborn (TTN), neonatal pneumonia, about unapproved/investigative commercial respiratory distress syndrome (RDS), and meconium aspiration products or devices. -

Evaluation of Pediatric Upper Airway
Evaluation of pediatric upper airway C. Gysin ORL-Unit University Children’s Hospital Zurich SSORL-Ecole d’été – SGORL-Sommerschule 2019 Pediatric airway – anatomy • large head • short neck • small nares • small mandible • pliable trachea and chest wall • immature alveolae • gastric dilatation, reflux • high metabolic rate • friable mucosa Pediatric airway – anatomy • high larynx • cricoid cartilage = C4 • long epiglottis • lies against the soft palate • long uvula • neonate obligate nasal breather Pediatric airway – anatomy prominent cuneiform cartilages short aryepiglottic folds tendency to collapse during inspiration epiglottis omega-shaped glottic length 50% ligamentous – 50% cartilaginous (adults 80-20) Pediatric airway – anatomy • subglottis: – from conus elasticus to inferior part of cricoid cartilage – only complete ring of the larynx and trachea – narrowest region of the pediatric airway • subglottic diameter at birth: – cricoid cartilage: 5.5mm – full-term baby: 4.5-5.5mm – premature baby: 3.5mm Pediatric airway – anatomy ↓ diameter 1mm = ↓ surface 50% ⇒ resistance R = 8µL/πr4 Pediatric airway – anatomy Newborn Child Adult Normal subglottic diameter (mm) 4 8 14 subglottic radius (mm) 2 4 7 subglottic surface (mm2) 12 6 12 1mm edema subglottic diameter (mm) 2 6 12 subglottic radius (mm) 1 3 6 subglottic surface (mm2) 3 27 108 Diminution of subglottic surface 75% 44% 27% Clinical approach 1. age of onset of respiratory symptoms? 2. level of obstruction? 3. investigations? 4. what is the lesion? Pediatric airway obstruction acquired congenital tumor foreign body infection trauma • newborn = congenital • 1-3 years = acquired more likely • >3 years = acquired likely (congenital highly unlikely) Diagnosis and age of onset of respiratory symptoms . since birth: . bilateral vocal cord paralysis . -

Injection Augmentation and Endoscopic Repair of Type 1
Isaac et al. Journal of Otolaryngology - Head and Neck Surgery (2020) 49:49 https://doi.org/10.1186/s40463-020-00447-0 ORIGINAL RESEARCH ARTICLE Open Access Injection augmentation and endoscopic repair of type 1 laryngeal clefts: development of a management algorithm Andre Isaac1* , Orysya Svystun2, Wendy Johannsen1,3 and Hamdy El-Hakim1,3 Abstract Objectives: To describe indications for injection augmentation (IA), endoscopic repair (ER) and conservative methods for the management of type 1 laryngeal cleft (LC1) and propose a management algorithm. We also aimed to compare success of IA and ER and determine independent predictors of treatment failure. Methods: Retrospective study of patients diagnosed with LC1 at a Pediatric Otolaryngology referral centre between 2004 and 2016. All had pre-operative instrumental swallowing evaluation (VFSS/FEES), and were managed with a combination of conservative measures, IA and/or ER. We collected demographics, symptoms, comorbidities, VFSS/ FEES results, and operative details. The primary outcome was symptom resolution by parental report. The secondary outcome was predictors of treatment failure. Results: 88 patients were included in the analysis, with mean age 26 ± 25 months. Most presented with choking events (68%) or recurrent pneumonias (48%). In total, there were 55 IA performed and 45 ER. Of the patients who received IA, 19 required subsequent ER. 95% had symptom improvement, 67% had complete resolution. IA had a 56% long-term success rate, whereas that for ER was 85%. Tube feeding at initial evaluation was an independent predictor of treatment failure (HR 11.33 [1.51–84.97], p = 0.018). Conclusions: LC1 can be effectively managed with a combination of IA and ER with favorable results.