Suprapubic Catheter Insertion Using an Ultrasound-Guided Technique and Literature Review BJUIBJU INTERNATIONAL Preman Jacob , Bhavan Prasad Rai * and Alistair W
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Melanoma of Urinary Bladder Presented As Acute Urine Retention. Nirmal Lamichhane1, Hari P Dhakal2 1Department of Surgical Oncology and 2Pathology, B
dd] fl] /on Sof fnf G;/ O] / c f : =s k L t k f = n L a B L . P A . T K I O P S IR O Nepalese Journal of Cancer (NJC) Volume 1 Issue 1 Page 67 - 70 A 2049BS/1992AD H BPKMCH LA BPKMCH,NEPAL R M CE EMORIAL CAN Case report Melanoma of Urinary Bladder presented as acute urine retention. Nirmal Lamichhane1, Hari P Dhakal2 1Department of Surgical Oncology and 2Pathology, B. P. Koirala Memorial Cancer Hospital, Bharatpur, Chitwan, Nepal. ABSTRACT This report is of a 50-year-old man with a rare urinary bladder melanoma. He presented with hematuria followed by bladder outlet obstruction at the time of presentation. Ultrasonogram of the pelvis revealed a mass in the bladder outlet, suggestive of enlarged prostate. Suprapubic cystostomy was then performed. Subsequent transvesical exploration revealed a dark coloured mass at the outlet of bladder, which on histopathology confirmed to be melanoma. After ruling out other possible primary sites, he underwent radical cysto-urethrectomy with urinary diversion. Disease was confirmed with immunohistochemistry. Patient died after 3 months with bilateral lung metastasis. Keywords: Melanoma, Urinary bladder, Cystectomy, Prognosis. INTRODUCTION but was not successful. Sonography was performed Malignant melanoma of urinary bladder is a very rare which showed enlarged prostate and distended bladder. entity and scantly reported in medical literature. Wheelock Suprapubic cystostomy was performed that comforted was the first to report a primary melanoma of the urinary the patient. bladder in 1942, and Su et al. reported the next case in 1962.1, 2 Approximately 50 patients with this tumour On asking, he had voiding type lower urinary tract have been reported in the literature shown by Medline symptoms for 2 and half months, but had no haematuria search. -

Urology 1 Cystoscopes
Urology 1 Cystoscopes 2 Urethrotomes 3 Resectoscopes 4 Uretero-Renoscopes 5 Nephroscopes 6 Lithotripsy (UreTron) 7 Laser Therapy 8 Small Caliber 9 Fluid Management 10 Accessories Richard Wolf Medical Instruments Corporation assumes no responsibility or liability for any errors or omissions in the content of this catalog. The information contained in this catalog is provided on an “as is” basis with no guarantees of completeness, accuracy, usefulness, or timeliness, and without warranties of any kind whatsoever, expressed or implied. 1777- 02.01-1118USA Cysto-Urethroscopes 8650 E-line design CYSTOSCOPES The E-line design guarantees optimum handling and safe, fatigue-free operation as well as a wide range of possible combinations. Basic Set for Cystoscopy Cysto-urethroscope sheath, 19.5 Fr. with obturator 8650.0341 Adapter with 1 instrument port 8650.264 Insert with Albarran deflector, 2 instrument ports 8650.204 Sterile universal sealing valve (pack of 5) 4712348 Viewing obturator 8650.724 Biopsy forceps Marburg 8650.614 Grasping forceps 8650.684 PANOVIEW telescope, 0° 8650.414 PANOVIEW telescope, 70° 8650.415 Otis urethrotome 8517.00 822.31 822.13 822.31 Flexible connector 822.13 Tray 8585030 1777- 02.01-1118USA 2 PANOVIEW Telescopes Overview CYSTOSCOPES Ø Viewing direction Color code Application mm 0° blue Standard 4 8650.414 12° orange Standard 4 8654.431 Standard 4 8654.422 30° red Long sheath 4 8668.433* 70° yellow Standard 4 8650.415 * Only 25° available. 1777- 02.01-1118USA 3 Cysto-Urethroscope 8650 for telescope 4 mm, 0°, 12°, 30°, 70° and adapters CYSTOSCOPES Sheaths and obturators Adapters Sheath incl. -
Cystoscopy to Understand a Cystoscopy, It Is Helpful to Become Familiar with the Urinary System (Figure 1)
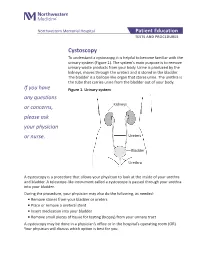
Northwestern Memorial Hospital Patient Education TESTS AND PROCEDURES Cystoscopy To understand a cystoscopy, it is helpful to become familiar with the urinary system (Figure 1). The system’s main purpose is to remove urinary waste products from your body. Urine is produced by the kidneys, moves through the ureters and is stored in the bladder. The bladder is a balloon-like organ that stores urine. The urethra is the tube that carries urine from the bladder out of your body. If you have Figure 1. Urinary system any questions or concerns, Kidneys please ask your physician or nurse. Ureters Bladder Urethra A cystoscopy is a procedure that allows your physician to look at the inside of your urethra and bladder. A telescope-like instrument called a cystoscope is passed through your urethra into your bladder. During the procedure, your physician may also do the following, as needed: ■ Remove stones from your bladder or ureters ■ Place or remove a ureteral stent ■ Insert medication into your bladder ■ Remove small pieces of tissue for testing (biopsy) from your urinary tract A cystoscopy may be done in a physician’s office or in the hospital’s operating room (OR). Your physician will discuss which option is best for you. Preparation and procedure If the test is done in the OR, you will be asked to sign a written consent. The OR procedure and any special preparation will be explained to you. There may be some discomfort during the examination. Some patients may require sedation or anesthesia. Depending on the type of medication used for your procedure, you will be told if you need to stop eating and drinking before your procedure. -

Urology Services in the ASC
Urology Services in the ASC Brad D. Lerner, MD, FACS, CASC Medical Director Summit ASC President of Chesapeake Urology Associates Chief of Urology Union Memorial Hospital Urologic Consultant NFL Baltimore Ravens Learning Objectives: Describe the numerous basic and advanced urology cases/lines of service that can be provided in an ASC setting Discuss various opportunities regarding clinical, operational and financial aspects of urology lines of service in an ASC setting Why Offer Urology Services in Your ASC? Majority of urologic surgical services are already outpatient Many urologic procedures are high volume, short duration and low cost Increasing emphasis on movement of site of service for surgical cases from hospitals and insurance carriers to ASCs There are still some case types where patients are traditionally admitted or placed in extended recovery status that can be converted to strictly outpatient status and would be suitable for an ASC Potential core of fee-for-service case types (microsurgery, aesthetics, prosthetics, etc.) Increasing Population of Those Aged 65 and Over As of 2018, it was estimated that there were 51 million persons aged 65 and over (15.63% of total population) By 2030, it is expected that there will be 72.1 million persons aged 65 and over National ASC Statistics - 2017 Urology cases represented 6% of total case mix for ASCs Urology cases were 4th in median net revenue per case (approximately $2,400) – behind Orthopedics, ENT and Podiatry Urology comprised 3% of single specialty ASCs (5th behind -

Clinical Significance of Cystoscopic Urethral Stricture
UCSF UC San Francisco Previously Published Works Title Clinical significance of cystoscopic urethral stricture recurrence after anterior urethroplasty: a multi-institution analysis from Trauma and Urologic Reconstructive Network of Surgeons (TURNS). Permalink https://escholarship.org/uc/item/3f57n621 Journal World journal of urology, 37(12) ISSN 0724-4983 Authors Baradaran, Nima Fergus, Kirkpatrick B Moses, Rachel A et al. Publication Date 2019-12-01 DOI 10.1007/s00345-019-02653-6 Peer reviewed eScholarship.org Powered by the California Digital Library University of California World Journal of Urology https://doi.org/10.1007/s00345-019-02653-6 ORIGINAL ARTICLE Clinical signifcance of cystoscopic urethral stricture recurrence after anterior urethroplasty: a multi‑institution analysis from Trauma and Urologic Reconstructive Network of Surgeons (TURNS) Nima Baradaran1 · Kirkpatrick B. Fergus2 · Rachel A. Moses3 · Darshan P. Patel3 · Thomas W. Gaither2 · Bryan B. Voelzke4 · Thomas G. Smith III5 · Bradley A. Erickson6 · Sean P. Elliott7 · Nejd F. Alsikaf8 · Alex J. Vanni9 · Jill Buckley10 · Lee C. Zhao11 · Jeremy B. Myers3 · Benjamin N. Breyer2 Received: 13 December 2018 / Accepted: 24 January 2019 © Springer-Verlag GmbH Germany, part of Springer Nature 2019 Abstract Purpose To assess the functional Queryoutcome of patients with cystoscopic recurrence of stricture post-urethroplasty and to evaluate the role of cystoscopy as initial screening tool to predict future failure. Methods Cases with cystoscopy data after anterior urethroplasty in a multi-institutional database were retrospectively studied. Based on cystoscopic evaluation, performed within 3-months post-urethroplasty, patients were categorized as small-caliber (SC) stricture recurrence: stricture unable to be passed by standard cystoscope, large-caliber (LC) stricture accommodating a cystoscope, and no recurrence. -

Suprapubic Cystostomy: Urinary Tract Infection and Other Short Term Complications A.T
Suprapubic Cystostomy: Urinary Tract Infection and other short term Complications A.T. Hasan,Q. Fasihuddin,M.A. Sheikh ( Department of Urological Surgery and Transplantation, Jinnah Postgraduate Medical Center, Karachi. ) Abstract Aims: To evaluate the frequency of urinary tract infection in patients with suprapubic cystostomy and other complications of the procedure within 30 days of placement. Methods: Patients characteristics, indication and types of cystostomy and short term (within 30 days); complications were analyzed in 91 patients. Urine analysis and culture was done in all patients to exclude those with urinary tract infection. After 15 and 30 days of the procedure, urine analysis and culture was repeated to evaluate the frequency of urinary tract infection. The prevalence of symptomatic bacteriuria with its organisms was assessed. Antibiotics were given to the postoperative and symptomatic patients and the relationship of antibiotics on the prevention of urinary tract infection was determined. Results: Of the 91 cases 88 were males and 3 females. The mean age was 40.52 ± 18.95 with a range of 15 to 82 years.Obstructive uropathy of lower urinary tract.was present in 81% cases and 17(18.6%) had history of trauma to urethra. All these cases had per-urethral bleeding on examination while x-ray urethrogram showed grade H or grade III injury of urethra. Eighty two of the procedures were performed per-cutaneously and 7 were converted to open cystostomies due to failure of per-cutaneous approach. Nine patients had exploratory laparotomy. Duration of catheterization was the leading risk factor for urinary tract infection found in 24.1% at 15 days and 97.8% at 30 days. -
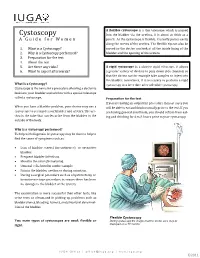
Cystoscopy Into the Bladder Via the Urethra, It Is About As Thick As a a Guide for Women
A flexible cystoscope is a thin telescope which is passed Cystoscopy into the bladder via the urethra, it is about as thick as a A Guide for Women pencil. As the cystoscope is flexible, it usually passes easily 1. What is a Cystoscopy? moved so the doctor can look at all the inside lining of the along the curves of the urethra. The flexible tip can also be 2. Why is a Cystoscopy performed? bladder and the opening of the ureters. 3. Preparation for the test 4. About the test 5. Are there any risks? A rigid cystoscope is a shorter rigid telescope, it allows 6. What to expect afterwards? a greater variety of devices to pass down side channels so that the doctor can for example take samples or inject into the bladder. Sometimes, it is necessary to perform a rigid What is a Cystoscopy? Cystoscopy is the name for a procedure allowing a doctor to look into your bladder and urethra with a special telescope cystoscopy at a later date after a flexible cystoscopy. called a cystoscope. Preparation for the test If you are having an outpatient procedure in most cases you When you have a bladder problem, your doctor may use a will be able to eat and drink normally prior to the test. If you cystoscope to see inside your bladder and urethra. The ure- are having general anesthesia, you should refrain from eat- thra is the tube that carries urine from the bladder to the ing and drinking for 6 to 8 hours prior to your cystoscopy. -

Long-Term Indwelling Double-J Stent and Multiple Encrusted Stones in the Ureter and Bladder: a Case Report on Holmium Laser Treatment
Pediatr Urol Case Rep 2018; 5(6):161-164 DOI: 10.14534/j-pucr.2018645052 PEDIATRIC UROLOGY CASE REPORTS ISSN 2148-2969 http://www.pediatricurologycasereports.com Long-term indwelling double-J stent and multiple encrusted stones in the ureter and bladder: A case report on Holmium laser treatment Mehmet Hanifi Okur, Selcuk Otcu Department of Pediatric Surgery, Dicle University, School of Medicine, Diyarbakir, Turkey ABSTRACT Double-J (D-J) stents are widely used in a variety of urological interventions. Forgotten D-J stents may lead to complications, such as migration, fragmentation and encrustation. We report the case of a forgotten stent, concomitant with ureteral and bladder stones. The forgotten D-J stent was placed four years prior to our intervention, during treatment for multiple right renal stones. Holmium laser lithotripsy was used to disrupt encrustations on a ureteral orifice and the ureteral stent. The percutaneous suprapubic cystostomy was removed without breaking the stent. The patient was discharged without further complications. Key Words: Double-J (D-J) stents; forgotten stent; encrustation; stone; Holmium laser lithotripsy. Copyright © 2018 pediatricurologycasereports.com Corresponding Author: Dr. Mehmet Hanifi Okur. endourological and open surgical methods Department of Pediatric Surgery, Dicle University, have been reported for the management of School of Medicine, Diyarbakir, Turkey. forgotten D-J stents, there is no standardized E mail: [email protected] ORCID ID: https://orcid.org/0000-0002-6720-1515 approach for their removal in adults and Received 2018-10-09, Accepted 2018-10-21 children [4]. Publication Date 2018-11-01 We report on a case of a forgotten D-J ureteral stent that had been placed during a Introduction percutaneous nephrolithotomy, four years Although Double-J (D-J) stents are widely prior to our intervention. -

An Unusual Consequence of Urinary Catheter Neglect: a Giant Bladder Stone
Int J Case Rep Images 2014;5(6):427–430. Agarwal et al. 427 www.ijcasereportsandimages.com CASE REPORT OPEN ACCESS An unusual consequence of urinary catheter neglect: A giant bladder stone Archana Agarwal, Justin Gould ABSTRACT How to cite this article Introduction: Indwelling urinary catheters cause Agarwal A, Gould J. An unusual consequence of a variety of complications including infections, urinary catheter neglect: A giant bladder stone. Int J pain and bleeding. Sometimes, the catheter Case Rep Images 2014;5(6):427–430. becomes encrusted and blocked. Case Report: A 66-year-old male was presented with increasing suprapubic pain for about two months because doi:10.5348/ijcri-201481-CR-10392 of a poorly draining Foley catheter. Two years earlier, the patient had undergone a transurethral resection of the prostate (TURP) gland. He was given a Foley catheter and asked to follow-up in a week. He did not follow-up or change the catheter INTRODUCTION for two years. The catheter could not be removed. A computed tomography scan of the abdomen Indwelling urinary catheters cause a variety of showed a large encrustation of 5.0x5.2x5.5 cm complications including infections, pain and bleeding [1]. surrounding the Foley. The patient underwent Sometimes, the catheter becomes encrusted and blocked open suprapubic cystostomy with intact retrieval [1]. We present a case of a giant bladder stone formation of stone along with the catheter. Conclusion: in a patient who did not change the catheter for more Indwelling Foley catheters frequently become than two years. encrusted and may become difficulty to remove. -

EAU Guidelines on Bladder Stones 2019
EAU Guidelines on Bladder Stones C. Türk (Chair), A. Skolarikos (Vice-chair), J.F. Donaldson, A. Neisius, A. Petrik, C. Seitz, K. Thomas Guidelines Associate: Y. Ruhayel © European Association of Urology 2019 TABLE OF CONTENTS PAGE 1. INTRODUCTION 3 1.1 Aims and Scope 3 1.2 Panel Composition 3 1.3 Available Publications 3 1.4 Publication History and Summary of Changes 3 1.4.1 Publication History 3 2. METHODS 3 2.1 Data Identification 3 2.2 Review 4 3. GUIDELINES 4 3.1 Prevalence, aetiology and risk factors 4 3.2 Diagnostic evaluation 4 3.2.1 Diagnostic investigations 5 3.3 Disease Management 5 3.3.1 Conservative treatment and Indications for active stone removal 5 3.3.2 Medical management of bladder stones 5 3.3.3 Bladder stone interventions 5 3.3.3.1 Suprapubic cystolithotomy 5 3.3.3.2 Transurethral cystolithotripsy 5 3.3.3.2.1 Transurethral cystolithotripsy in adults: 5 3.3.3.2.2 Transurethral cystolithotripsy in children: 6 3.3.3.3 Percutaneous cystolithotripsy 6 3.3.3.3.1 Percutaneous cystolithotripsy in adults: 6 3.3.3.3.2 Percutaneous cystolithotripsy in children: 6 3.3.3.4 Extracorporeal shock wave lithotripsy (SWL) 6 3.3.3.4.1 SWL in Adults 6 3.3.3.4.2 SWL in Children 6 3.3.4 Treatment for bladder stones secondary to bladder outlet obstruction (BOO) in adult men 7 3.3.5 Urinary tract reconstructions and special situations 7 3.3.5.1 Neurogenic bladder 7 3.3.5.2 Bladder augmentation 7 3.3.5.3 Urinary diversions 7 4. -
Discharge Instructions for Ureteroscopy, Laser Lithotripsy and Stent Insertion
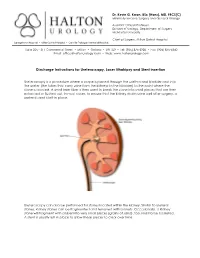
Dr. Kevin G. Kwan, BSc (Hons), MD, FRCS(C) Minimally Invasive Surgery and General Urology Assistant Clinical Professor Division of Urology, Department of Surgery McMaster University Chief of Surgery, Milton District Hospital Georgetown Hospital • Milton District Hospital • Oakville Trafalgar Memorial Hospital Suite 205 - 311 Commercial Street • Milton • Ontario • L9T 3Z9 • Tel: (905) 875-3920 • Fax: (905) 875-4340 Email: [email protected] • Web: www.haltonurology.com Discharge Instructions for Ureteroscopy, Laser lithotripsy and Stent insertion Ureteroscopy is a procedure where a scope is passed through the urethra and bladder and into the ureter (the tubes that carry urine from the kidneys to the bladder) to the point where the stone is located. A small laser fiber is then used to break the stone into small pieces that are then extracted or flushed out. In most cases, to ensure that the kidney drains urine well after surgery, a ureteral stent is left in place. Ureteroscopy can also be performed for stones located within the kidney. Similar to ureteral stones, kidney stones can be fragmented and removed with baskets. Occasionally, a kidney stone will fragment with a laser into very small pieces (grains of sand), too small to be basketed. A stent is usually left in place to allow these pieces to clear over time. Ureteral Stenting: Almost always after ureteroscopy, a ureteral stent will be placed. This is a thin, hollow, plastic tube that is used temporarily to keep the ureter open and facilitates drainage of urine down to the bladder until it heals. It also allows the urine to drain and any small stone fragments to pass freely. -
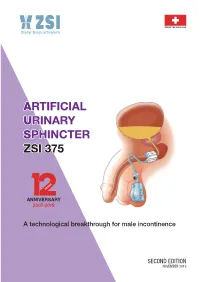
Artificial Urinary Sphincter Zsi 375
SWISS TECHNOLOGY ARTIFICIAL URINARY SPHINCTER ZSI 375 YEARS ANNIVERSARY 2007-2019 A technological breakthrough for male incontinence SECOND EDITION NOVEMBER 2019 ZSI 375 MANUAL Easy to implant Easy to use ‘Let every man judge according to his own standards, by what he has himself read, not by what others tell him.’ Albert Einstein (1949) The World As I See It ZSI 375 MANUAL ORIGINS AND GRATITUDE TO EARLY IMPLANTERS HISTORY OF THE ZSI 375 MANUAL This manual is a summary of the knowledge acquired to date on the Artificial Urinary Sphincter ZSI 375. It gathers in a single volume, the pedagogical sheets that have been developed and continuously improved for 12 years; it offers readers a better understanding of the functioning of the ZSI 375 Artificial Urinary Sphincter to optimise its use. We hope that this manual will provide you with additional information on the videos available on our website www.zsimplants.ch and complement our local technical team’s support. If you have any questions, do not hesitate to contact ZSI directly at [email protected] or your local ZSI team. Raphaël Gomez Llorens Global Marketing Manager Head of Training ACKNOWLEDGEMENTS TO EARLY IMPLANTERS From 2009 to 2019, over 4500 Artificial Urinary Sphincters (AUS) ZSI 375 were implanted in different versions. This success would not have been possible without the trust and motivation from visionary surgeons and distributors from Argentina, Austria, Colombia, Costa Rica, Germany, Italy, Poland, Portugal, Spain and Turkey. From as early as between 2009 and 2011, they promoted the technology and quality of ZSI products around the world.