Cutaneous Manifestations in Confirmed COVID-19 Patients
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Cutaneous Manifestations of COVID-19: a Systematic Review and Analysis of Individual Patient-Level Data
Volume 26 Number 12| December 2020 Dermatology Online Journal || Review 26(12):2 Cutaneous manifestations of COVID-19: a systematic review and analysis of individual patient-level data David S Lee1 MD, Paradi Mirmirani2,3 MD, Patrick E McCleskey4 MD, Majid Mehrpouya5 PhD, Farzam Gorouhi6,7 MD Affiliations: 1Department of Dermatology, The Permanente Medical Group, Pleasanton, California, USA, 2Department of Dermatology, University of California, San Francisco, California, USA, 3Department of Dermatology, The Permanente Medical Group, Vallejo, California, USA, 4Department of Dermatology, The Permanente Medical Group, Oakland, California, USA, 5Faculty of Engineering, University of Calgary, Calgary, Alberta, Canada, 6Department of Dermatology, The Permanente Medical Group, South Sacramento, California, USA, 7Department of Dermatology, University of California, Davis, California, USA Corresponding Author: Farzam Gorouhi MD FAAD, Kaiser Permanente, South Sacramento, 6600 Bruceville Road, Sacramento, CA 95823, Tel: 415-298-1345, Email: [email protected] Introduction Abstract In December 2019, reports from Wuhan, China Distinctive patterns in the cutaneous manifestations described new clusters of patients with severe of COVID-19 have been recently reported. We pneumonia linked to a novel coronavirus strain, now conducted a systematic review to identify case reports and case series characterizing cutaneous referred to as severe acute respiratory syndrome manifestations of confirmed COVID-19. Key coronavirus 2 (SARS-CoV-2), [1]. Coronavirus disease demographic and clinical data from each case were 2019 (COVID-19) has since reached pandemic extracted and analyzed. The primary outcome proportions, with over 12·7 million cases worldwide, measure was risk factor analysis of skin related 566,000 deaths, and 188 countries affected at the outcomes for severe COVID-19 disease. -

Dermatologic Manifestations and Complications of COVID-19
American Journal of Emergency Medicine 38 (2020) 1715–1721 Contents lists available at ScienceDirect American Journal of Emergency Medicine journal homepage: www.elsevier.com/locate/ajem Dermatologic manifestations and complications of COVID-19 Michael Gottlieb, MD a,⁎,BritLong,MDb a Department of Emergency Medicine, Rush University Medical Center, United States of America b Department of Emergency Medicine, Brooke Army Medical Center, United States of America article info abstract Article history: The novel coronavirus disease of 2019 (COVID-19) is associated with significant morbidity and mortality. While Received 9 May 2020 much of the focus has been on the cardiac and pulmonary complications, there are several important dermato- Accepted 3 June 2020 logic components that clinicians must be aware of. Available online xxxx Objective: This brief report summarizes the dermatologic manifestations and complications associated with COVID-19 with an emphasis on Emergency Medicine clinicians. Keywords: COVID-19 Discussion: Dermatologic manifestations of COVID-19 are increasingly recognized within the literature. The pri- fi SARS-CoV-2 mary etiologies include vasculitis versus direct viral involvement. There are several types of skin ndings de- Coronavirus scribed in association with COVID-19. These include maculopapular rashes, urticaria, vesicles, petechiae, Dermatology purpura, chilblains, livedo racemosa, and distal limb ischemia. While most of these dermatologic findings are Skin self-resolving, they can help increase one's suspicion for COVID-19. Emergency medicine Conclusion: It is important to be aware of the dermatologic manifestations and complications of COVID-19. Knowledge of the components is important to help identify potential COVID-19 patients and properly treat complications. © 2020 Elsevier Inc. -

Dermatological Findings in Common Rheumatologic Diseases in Children
Available online at www.medicinescience.org Medicine Science ORIGINAL RESEARCH International Medical Journal Medicine Science 2019; ( ): Dermatological findings in common rheumatologic diseases in children 1Melike Kibar Ozturk ORCID:0000-0002-5757-8247 1Ilkin Zindanci ORCID:0000-0003-4354-9899 2Betul Sozeri ORCID:0000-0003-0358-6409 1Umraniye Training and Research Hospital, Department of Dermatology, Istanbul, Turkey. 2Umraniye Training and Research Hospital, Department of Child Rheumatology, Istanbul, Turkey Received 01 November 2018; Accepted 19 November 2018 Available online 21.01.2019 with doi:10.5455/medscience.2018.07.8966 Copyright © 2019 by authors and Medicine Science Publishing Inc. Abstract The aim of this study is to outline the common dermatological findings in pediatric rheumatologic diseases. A total of 45 patients, nineteen with juvenile idiopathic arthritis (JIA), eight with Familial Mediterranean Fever (FMF), six with scleroderma (SSc), seven with systemic lupus erythematosus (SLE), and five with dermatomyositis (DM) were included. Control group for JIA consisted of randomly chosen 19 healthy subjects of the same age and gender. The age, sex, duration of disease, site and type of lesions on skin, nails and scalp and systemic drug use were recorded. χ2 test was used. The most common skin findings in patients with psoriatic JIA were flexural psoriatic lesions, the most common nail findings were periungual desquamation and distal onycholysis, while the most common scalp findings were erythema and scaling. The most common skin finding in patients with oligoarthritis was photosensitivity, while the most common nail finding was periungual erythema, and the most common scalp findings were erythema and scaling. We saw urticarial rash, dermatographism, nail pitting and telogen effluvium in one patient with systemic arthritis; and photosensitivity, livedo reticularis and periungual erythema in another patient with RF-negative polyarthritis. -

Dermatology DDX Deck, 2Nd Edition 65
63. Herpes simplex (cold sores, fever blisters) PREMALIGNANT AND MALIGNANT NON- 64. Varicella (chicken pox) MELANOMA SKIN TUMORS Dermatology DDX Deck, 2nd Edition 65. Herpes zoster (shingles) 126. Basal cell carcinoma 66. Hand, foot, and mouth disease 127. Actinic keratosis TOPICAL THERAPY 128. Squamous cell carcinoma 1. Basic principles of treatment FUNGAL INFECTIONS 129. Bowen disease 2. Topical corticosteroids 67. Candidiasis (moniliasis) 130. Leukoplakia 68. Candidal balanitis 131. Cutaneous T-cell lymphoma ECZEMA 69. Candidiasis (diaper dermatitis) 132. Paget disease of the breast 3. Acute eczematous inflammation 70. Candidiasis of large skin folds (candidal 133. Extramammary Paget disease 4. Rhus dermatitis (poison ivy, poison oak, intertrigo) 134. Cutaneous metastasis poison sumac) 71. Tinea versicolor 5. Subacute eczematous inflammation 72. Tinea of the nails NEVI AND MALIGNANT MELANOMA 6. Chronic eczematous inflammation 73. Angular cheilitis 135. Nevi, melanocytic nevi, moles 7. Lichen simplex chronicus 74. Cutaneous fungal infections (tinea) 136. Atypical mole syndrome (dysplastic nevus 8. Hand eczema 75. Tinea of the foot syndrome) 9. Asteatotic eczema 76. Tinea of the groin 137. Malignant melanoma, lentigo maligna 10. Chapped, fissured feet 77. Tinea of the body 138. Melanoma mimics 11. Allergic contact dermatitis 78. Tinea of the hand 139. Congenital melanocytic nevi 12. Irritant contact dermatitis 79. Tinea incognito 13. Fingertip eczema 80. Tinea of the scalp VASCULAR TUMORS AND MALFORMATIONS 14. Keratolysis exfoliativa 81. Tinea of the beard 140. Hemangiomas of infancy 15. Nummular eczema 141. Vascular malformations 16. Pompholyx EXANTHEMS AND DRUG REACTIONS 142. Cherry angioma 17. Prurigo nodularis 82. Non-specific viral rash 143. Angiokeratoma 18. Stasis dermatitis 83. -
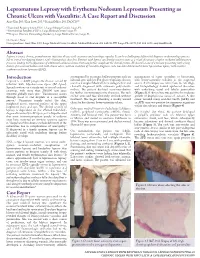
Lepromatous Leprosy with Erythema Nodosum Leprosum Presenting As
Lepromatous Leprosy with Erythema Nodosum Leprosum Presenting as Chronic Ulcers with Vasculitis: A Case Report and Discussion Anny Xiao, DO,* Erin Lowe, DO,** Richard Miller, DO, FAOCD*** *Traditional Rotating Intern, PGY-1, Largo Medical Center, Largo, FL **Dermatology Resident, PGY-2, Largo Medical Center, Largo, FL ***Program Director, Dermatology Residency, Largo Medical Center, Largo, FL Disclosures: None Correspondence: Anny Xiao, DO; Largo Medical Center, Graduate Medical Education, 201 14th St. SW, Largo, FL 33770; 510-684-4190; [email protected] Abstract Leprosy is a rare, chronic, granulomatous infectious disease with cutaneous and neurologic sequelae. It can be a challenging differential diagnosis in dermatology practice due to several overlapping features with rheumatologic disorders. Patients with leprosy can develop reactive states as a result of immune complex-mediated inflammatory processes, leading to the appearance of additional cutaneous lesions that may further complicate the clinical picture. We describe a case of a woman presenting with a long history of a recurrent bullous rash with chronic ulcers, with an evolution of vasculitic diagnoses, who was later determined to have lepromatous leprosy with reactive erythema nodosum leprosum (ENL). Introduction accompanied by an intense bullous purpuric rash on management of sepsis secondary to bacteremia, Leprosy is a slowly progressive disease caused by bilateral arms and face. For these complaints she was with lower-extremity cellulitis as the suspected infection with Mycobacterium leprae (M. leprae). seen in a Complex Medical Dermatology Clinic and source. A skin biopsy was taken from the left thigh, Spread continues at a steady rate in several endemic clinically diagnosed with cutaneous polyarteritis and histopathology showed epidermal ulceration countries, with more than 200,000 new cases nodosa. -

Review Cutaneous Patterns Are Often the Only Clue to a a R T I C L E Complex Underlying Vascular Pathology
pp11 - 46 ABstract Review Cutaneous patterns are often the only clue to a A R T I C L E complex underlying vascular pathology. Reticulate pattern is probably one of the most important DERMATOLOGICAL dermatological signs of venous or arterial pathology involving the cutaneous microvasculature and its MANIFESTATIONS OF VENOUS presence may be the only sign of an important underlying pathology. Vascular malformations such DISEASE. PART II: Reticulate as cutis marmorata congenita telangiectasia, benign forms of livedo reticularis, and sinister conditions eruptions such as Sneddon’s syndrome can all present with a reticulate eruption. The literature dealing with this KUROSH PARSI MBBS, MSc (Med), FACP, FACD subject is confusing and full of inaccuracies. Terms Departments of Dermatology, St. Vincent’s Hospital & such as livedo reticularis, livedo racemosa, cutis Sydney Children’s Hospital, Sydney, Australia marmorata and retiform purpura have all been used to describe the same or entirely different conditions. To our knowledge, there are no published systematic reviews of reticulate eruptions in the medical Introduction literature. he reticulate pattern is probably one of the most This article is the second in a series of papers important dermatological signs that signifies the describing the dermatological manifestations of involvement of the underlying vascular networks venous disease. Given the wide scope of phlebology T and its overlap with many other specialties, this review and the cutaneous vasculature. It is seen in benign forms was divided into multiple instalments. We dedicated of livedo reticularis and in more sinister conditions such this instalment to demystifying the reticulate as Sneddon’s syndrome. There is considerable confusion pattern. -

Erythema Nodosum (En)
Buffalo Medical Group, P.C. Robert E. Kalb, M.D. Phone: (716) 630-1102 Fax: (716) 633-6507 Department of Dermatology 325 Essjay Road Williamsville, New York 14221 ERYTHEMA NODOSUM (EN) Erythema Nodosum (EN) is a relatively uncommon reaction in the skin consisting of red shiny tender nodular lesions most commonly found on the legs. The erythema refers to the red color that is seen at the surface of the skin. The nodosum refers to the fact that these lesions feel like bumps or nodules underneath the skin surface. Erythema nodosum is a reaction pattern occurring in the subcutaneous tissue and fat. It may be preceded by a low grade fever, fatigue, and joint pains. In about half of the cases, there is an internal condition occurring in the body which contributes to its formation. These include the use of certain medications, certain infections, and a number of other less likely causes. In order to identify cause for the erythema nodosum, it may be necessary to perform blood and laboratory tests. At times, however, the cause cannot be determined and erythema nodosum is considered to be idiopathic in nature. Erythema nodosum often runs an acute course lasting for a brief period from weeks to months. In a small percentage of cases, it can be a more chronic condition. The red nodules are usually confined to the lower legs, but can develop anywhere there is fat under the skin including the thighs, arms, and trunk. Initially, the lesions are more red and inflamed in appearance, but with time become more bruise like. -

MYELOPATHY ASSOCIATED with SYSTEMIC LUPUS ERYTHEMATOSUS (Erythema Nodosum)
Paraplegia 16 (1978-79) 282-294 Original Articles MYELOPATHY ASSOCIATED WITH SYSTEMIC LUPUS ERYTHEMATOSUS (Erythema Nodosum) L. S. KEWALRAMANI, M.D., M.S.Orth., S. SALEEM, M.D. and D. BERTRAND, M.T. (ASCP) Texas Institute for Rehabilitation and Research and Department of Pathology, Baylor College of Medicine, Houston, Texas 77030, U.S.A. Abstract. Two patients with sudden onset of myelopathy associated with Systemic Lupus Erythematosus (Erythema Nodosum) are described. Pertinent literature is extensively reviewed and these two new patients are added to previously reported 26 patients. Key words: Myelopathy; Meningoencephalomyelopathy; Systemic lupus erythematosus. NEUROLOGICAL manifestations of systemic lupus erythematosus (SLE) have only recently been emphasised although they were mentioned by Kaposi in 1875, who observed stupor and coma as terminal manifestations of the disease. But focal neurological abnormalities were first reported by Osler (1903) and since then there have been several reports in the literature. Most commonly reported entities have been acute organic brain syndrome, seizures and cerebrovascular disorders. Chorea, Guillain Barre syndrome, subarachnoid haemorrhage, peripheral neuro pathy and cranial nerve palsies associated with SLE have also been reported on a few occasions. Myelopathy, however, has not received adequate emphasis as a complication of SLE. Fisher and Gilmour reported the first case of flaccid paraplegia in a female with SLE in 1939. Since then only 25 additional cases have been reported in the medical literature over the past 38 years. Twenty cases have been described in sufficient detail and six briefly, to permit a meaningful review of the spinal cord involvement in this disease. We feel that there are probably many more unreported cases of myelopathy associated with SLE. -

Cutaneous Reactions Reported After Moderna and Pfizer COVID-19 Vaccination: a Registry-Based Study of 414 Cases
Journal Pre-proof Cutaneous Reactions Reported after Moderna and Pfizer COVID-19 Vaccination: A Registry-Based Study of 414 Cases Devon E. McMahon, BA, Erin Amerson, MD, Misha Rosenbach, MD, Jules B. Lipoff, MD, Danna Moustafa, BS, Anisha Tyagi, BA, Seemal R. Desai, MD, Lars E. French, MD, Henry W. Lim, MD, Bruce H. Thiers, MD, George J. Hruza, MD MBA, Kimberly Blumenthal, MD MSc, Lindy P. Fox, MD, Esther E. Freeman, MD PhD PII: S0190-9622(21)00658-7 DOI: https://doi.org/10.1016/j.jaad.2021.03.092 Reference: YMJD 15862 To appear in: Journal of the American Academy of Dermatology Received Date: 23 February 2021 Revised Date: 16 March 2021 Accepted Date: 26 March 2021 Please cite this article as: McMahon DE, Amerson E, Rosenbach M, Lipoff JB, Moustafa D, Tyagi A, Desai SR, French LE, Lim HW, Thiers BH, Hruza GJ, Blumenthal K, Fox LP, Freeman EE, Cutaneous Reactions Reported after Moderna and Pfizer COVID-19 Vaccination: A Registry-Based Study of 414 Cases, Journal of the American Academy of Dermatology (2021), doi: https://doi.org/10.1016/ j.jaad.2021.03.092. This is a PDF file of an article that has undergone enhancements after acceptance, such as the addition of a cover page and metadata, and formatting for readability, but it is not yet the definitive version of record. This version will undergo additional copyediting, typesetting and review before it is published in its final form, but we are providing this version to give early visibility of the article. Please note that, during the production process, errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain. -

WFR Outline.Cwk
WILDERNESS FIRST RESPONDER Nine Days (80 hours) Our Wilderness First Responder course is designed with the outdoor professional in mind. It focuses on developing skills for treating problems outside the “ golden hour” of first response. It is based on the protocols set by the Wilderness Medical Society and instruction encourages the students ability to think through body systems in an effort to determine the best response to traumatic, environmental or medical situations. Classroom sessions are followed with hands on practice to integrate the information in a field setting. 100% attendance is required and there will be a night scenario included. The students will get to see their skills in action as video coverage of intensive scenarios will be reviewed towards the end of the class. A comprehensive written exam is also administered. The course includes American CPR certification. General Syllabus Day 1: Basic Life Support Skills/ Anatomy and Physiology *Opening and Course Paperwork *Course Introduction and Expectations *Student and Instructor Introductions *Medical Legal Overview * Evolution of Patient Care System and how WFR’s fit in *Patient Assessment System (PAS) Part 1 How to approach a scene! General Review of Anatomy and Physiology (All Systems) *Specific exploration of Respiratory System *Hands on practice establishing an airway/airway management *Specific exploration of the Circulatory System * Hands on practice for checking for pulse, controlling bleeding, cpr *Specific exploration of Nervous System * Evaluating Level of Consciousness -

Erythema Marginatum
Figurative Erythemas Michelle Goedken, DO Affiliated Dermatology Scottsdale, AZ Figurative Erythemas • Erythema annulare centrifugum • Erythema marginatum • Erythema migrans • Erythema gyratum repens • Erythema multiforme Erythemas • Erythemas represent a change in the color of the skin that is due to the dilation of blood vessels, especially those in the papillary and reticular dermis • The color is blanchable and most last for days to months • Figurative erythemas have an annular, arciform or polycyclic appearance ERYTHEMA ANNULARE CENTRIFUGUM ERYTHEMA ANNULARE CENTRIFUGUM • Pathogenesis: EAC represents a reaction pattern or hypersensitivity to one of many antigens – IL-2 and TNF-alpha may have a role – Most patients do not have an underlying disease identified ERYTHEMA ANNULARE CENTRIFUGUM • Associated with: – Infection » Dermatophytes and other fungi (Candida and Penicillium in blue cheese) » Viruses: poxvirus, EBV, VZV, HIV » Parasites and ectoparasites – Drugs: diuretics, antimalarials, gold, NSAIDs, finasteride, amitriptyline, etizolam, Ustekinumab (2012) ERYTHEMA ANNULARE CENTRIFUGUM – Foods – Autoimmune endocrinopathies – Neoplasms (lymphomas and leukemias) – Pregnancy – Hypereosinophilic syndrome – Lupus (2014) ERYTHEMA ANNULARE CENTRIFUGUM http://www.dermaamin.com Rongioletti, F., Fausti, V., & Parodi, A ERYTHEMA ANNULARE CENTRIFUGUM • 2 major forms: – Superficial: classic trailing scale, may have associated pruritus – Deep: infiltrated borders, usually no scale, edges are elevated, usually not pruritic ERYTHEMA ANNULARE CENTRIFUGUM -

Acroangiodermatitis (Pseudo-Kaposi's Sarcoma) in An
Revista5Vol89ingles_Layout 1 8/8/14 10:17 AM Página 792 792 DERMATOPATHOLOGY s Acroangiodermatitis (pseudo-Kaposi's sarcoma) in an HIV sero- positive patient with syphilis and hepatitis C virus coinfection: clinical and dermatopathological features* Fred Bernardes Filho1 Gustavo Martins2 José Augusto da Costa Nery1,3 Cecília Vianna de Andrade3,4 Bernard Kawa Kac1,5 DOI: http://dx.doi.org/10.1590/abd1806-4841.20143036 Abstract: Acroangiodermatitis is an angioproliferative disease usually related to chronic venous insufficiency, and it is considered a clinical and histological simulator of Kaposi's sarcoma (KS). Immunohistochemistry is the suit- able method to differentiate between these two entities. It reveals the following immunostaining profile: immunopositivity with anti-CD34 antibody is restricted to the vascular endothelium in acroangiodermatitis, and diffuse in the KS (endothelial cells and perivascular spindle cells); immunopositivity with anti-HHV-8 only in KS cases. We report the case of an HIV seropositive patient without apparent vascular disease, who presented viola- ceous and brownish erythematous lesions on the feet, and whose histopathology and immunohistochemistry indi- cated the diagnosis of acroangiodermatitis. Keywords: AIDS Serodiagnosis; Herpesvirus 8, human; Immunohistochemistry; Sarcoma, Kaposi; Syphilis, cutaneous INTRODUCTION Acroangiodermatitis is an unsual angioprolife- tantly with other manifestations or late in the course of rative disease related to chronic venous insufficiency, disease. The clinical presentation of KS is highly varia- arteriovenous malformations or fistulas, paralyzed ble, generally beginning with purplish or brownish, limbs, amputation stumps and thrombotic condi- erythematous, asymptomatic macules that later evolve tions.1,2 It is generally characterized by purpuric macu- into papules, plaques, nodules or tumor lesions.4,5 les, papules or plaques on the dorsum of the feet and Histopathologic distinction between acroangio- the malleolus.