Molluscum Contagiosum of the Areola and Nipple: Case Report and Literature Review
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Vasospasm of the Nipple
Vasospasm of the Nipple A spasm of blood vessels (vasospasm) in the nipple can result in nipple and/or breast pain, particularly within 30 minutes after a breastfeeding or a pumping session. It usually happens after nipple trauma and/or an infection. Vasospasms can cause repeated disruption of blood flow to the nipple. Within seconds or minutes after milk removal, the nipple may turn white, red, or purple, and a burning or Community stabbing pain is felt. Occasionally women feel a tingling sensation or itching. As the Breastfeeding nipple returns to its normal color, a throbbing pain may result. Color change is not Center always visible. 5930 S. 58th Street If there is a reason for nipple damage (poor latch or a yeast overgrowth), the cause (in the Trade Center) Lincoln, NE 68516 needs to be addressed. This can be enough to stop the pain. Sometimes the (402) 423-6402 vasospasm continues in a “vicious” cycle, as depicted below. While the blood 10818 Elm Street vessels are constricted, the nipple tissue does not receive enough oxygen. This Rockbrook Village causes more tissue damage, which can lead to recurrent vasospasm, even if the Omaha, NE 68144 (402) 502-0617 original cause of damage is “fixed.” For additional information: (Poor Latch or Inflammation) www ↓ Tissue Damage ↙ ↖ Spasm of blood vessels → Lack of oxygen to tissues To promote improved blood flow and healing of the nipple tissue: • See a lactation consultant (IBCLC) or a breastfeeding medicine specialist for help with latch and/or pumping to reduce future nipple damage. • When your baby comes off your nipple, or you finish a pumping session, immediately cover your nipple with a breast pad or a towel to keep it warm and dry. -
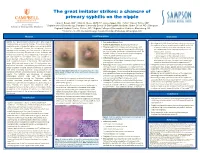
A Chancre of Primary Syphilis on the Nipple
The great imitator strikes: a chancre of primary syphilis on the nipple Falon V. Brown, DO 1, Mikél E. Muse, OMS IV2, James Appel, MD, FAAD1, Warren White, MD3 1Department of Dermatology; Campbell University School of Osteopathic Medicine, Buies Creek, NC | Sampson Regional Medical Center, Clinton, NC. 2Virginia College of Osteopathic Medicine, Blacksburg, VA 3Department of Dermatopathology; Coastal Carolina Pathology, Wilmington, NC Abstract Case Description Discussion Syphilis, the “great imitator,” presents with a wide range of § Past medical history: Gout mucocutaneous and systemic findings. The primary chancre • According to the CDC, there has been a drama4c increase in § Family medical history: Breast cancer (mother) the incidence of primary and secondary syphilis in the U.S. classically occurs in the genital region, however up to 6.33% • Physical exam: Erythematous, ulcerated, plaque with can be extragenital. Among the extragenital chancres • In 2016, a total of 27,814 cases reported 8.7 cases serosanguinous drainage and crusting at the 12 o’clock per 100,000 popula4on spanning equally across all reported in the literature, very few occurred on the breast, position of nipple. Tenderness with palpation noted. No and of these cases only 5% occurred in men. A 43-year-old regions of the country. palpable axillary or supraclavicular lymphadenopathy • An increase of 17.6% compared to 2015 healthy man visited our clinic complaining of drainage from noted. No penile ulceration was found. the right nipple for one month. Exam was notable for a • An increase of 74.0% compared to 2012 • Differential diagnosis: Nipple eczema, erosive • Ini4ally, increase in incidence was associated with men poorly defined, scaly erythematous plaque on the areola with a superficial erosion of the nipple. -

Breast & Nipple Orgasms 101
Breast & Nipple Orgasms 101: Embody Deeper Sensuality, Pleasure & Orgasmic Ecstasy through breast, heart & nipple awakening. WELCOME TO BREAST & NIPPLE ORGASMS! In this bonus module you'll uncover the true pleasure, sexual energy and orgasmic potential of your breasts and nipples. You'll discover techniques for pleasuring your breasts, awakening sensuality and feminine power PLUS how to stimulate your nipples and breasts to orgasm. You'll learn a Tantric Breast & Heart breathing technique, powerful Nipple Activation Meditation and how to penetrate the heart and soul of your partner or others through your devotional erotic love, sensuality and orgasmic power. YOUR BREASTS ARE THE FORCE FOR WHICH YOU PENETRATE THE WORLD & YOUR LOVER(S) HEART WITH YOUR DEVOTION, LOVE, PASSION & SEXUAL ENERGY THE BREAST & PUSSY CONNECTION There is an energetic channel that runs directly from the positive & penetrative pole in your breasts down to your vagina, the negative & receptive pole. Our breasts have a deep connection with our heart and with our pussy so the more you open, stroke and massage your breasts, the more you open your heart and your pussy. During sex a man penetrates, warms and softens a woman’s negative pole with his cock. She receives this cock energy in her vagina and raises it up her spine, transmuting it not only in her vagina, but in her heart, and through her breasts she penetrates her man’s heart with her breasts and heart. (S)He receives this love and warmth in his chest and heart, which flows down his spine into his cock only to be sent like an infinite loop of electrical current and energy between them. -

Details of the Available Literature on Sex for Induction of Labour
Appendix 1: Details of the available literature on sex for induction of labour At term, nipple and genital stimulation have been advocated as a way of naturally promoting the release of endogenous oxytocin. 1 In 2005, a Cochrane Review examined the evidence for breast stimulation as a method for inducing labour and found six trials of 719 women, showing a decrease in the number of women not in labour at 72 hours with nipple stimulation compared with no intervention. 2 However, this finding was only significant among women who already had a favourable Bishop score (a cervical assessment used to predict the success of achieving a vaginal delivery). When breast stimulation was compared with intravenous oxytocin in the review, there was no difference in rates of cesarean delivery, number of women in labour at 72 hours or rates of meconium staining. However, the included studies did not look at time to vaginal delivery as an outcome. Overall, nipple stimulation seems to have minimal or no effect for women with an unripe cervix, but may be helpful for inducing labour in those with a ripe cervix. Few studies have looked at the role of intercourse as a cervical-ripening technique. However, prostaglandin concentrations have been shown to be 10 to 50 times higher in the cervical mucous of pregnant women two to four hours after intercourse, compared with concentrations before intercourse. 3 In a study of 47 women who had sex at term compared with 46 who abstained, there was no significant difference in Bishop scores. On average, the sexually active group delivered four days earlier, which was not considered clinically significant. -

Preparing to Breastfeed Ome Women Wonder What They Need to Do • Room for Expansion
Preparing to Breastfeed ome women wonder what they need to do • Room for expansion. Your breasts may go up a full cup during pregnancy to prepare for breastfeeding. size when your milk comes in. Actually, your body knows what to do. Lactation • Breathable fabrics are best while breastfeeding. S(milk production) naturally follows pregnancy. The • Consider buying only 1 or 2 bras during the final hormones produced during pregnancy prepare your weeks of pregnancy and waiting until a couple of breasts to make milk once your baby is born. The best weeks postpartum to add more to your wardrobe. preparation, and what most women need in order (A gift certificate for a new bra makes a great shower to breastfeed effectively, is accurate information and gift.) Many mothers-to-be like to know that their someone to provide support and encouragement. breast size will settle into a moderately larger size after about three months. During Pregnancy At one time a great deal of emphasis was placed on Concerns About Nipple Size or Shape preparing your nipples during pregnancy. However, it is In order for the baby to suck effectively, he needs to now recognized that correct positioning and latch-on draw your nipple far back into his mouth. Babies can of the baby in the early days is the best prevention for breastfeed effectively with a large variety of nipple nipple soreness. So what shapes. The nipple is only a part of the breast called the should you expect before nipple-areola complex. The softness and stretchiness the baby is born? of the tissue just behind the nipple is actually more • Your breasts will likely important than the nipple shape. -

Sexual Anatomy
anatomy • Vulva includes Labia Minora, Majora, Clitoris, Vestibule (area around the opening) • Many shapes and sizes of labia- normal • Urethral opening- can be inside vagina, or just above opening • Perineum- space between vaginal opening and the anal opening Perineum • G-Spot- front wall just inside the vagina- concentration of nerve endings • Sexual Pleasure can be derived from pressure or stimulation to the: Clitoral area (bigger than just the glans) G-Spot G Spot Perineum Labia Nipples and breasts • Glans – tip of the penis • Penile shaft- length of the penis- erectile tissue G Spot • Scrotum- soft sac holds the testicle • Perineum- space behind the scrotum and in front of the anal opening Perineum • G-Spot- behind the prostate www.PelvicHealthWellness.com MASTURBATION, FOREPLAY, and orgasm 40-60% of women masturbate, while 90-95% of men masturbate. It is reported that only 30% of women can have a vaginal orgasm…. Journal of Sex Research reported 80% heterosexual women fake orgasm during intercourse 50% of the time. 25% of women fake every time. 10-15% of women have never had an orgasm. I think we can unlock the potential for our own pleasure by understanding the anatomy, erogenous zones, and engaging our pelvic floor! Starts with knowing your body and exploring what makes you feel good. Masturbation: By knowing what makes you feel good, you can then tap into your own orgasm and teach your partner what feels good. Study the anatomy, use some lubrication and a small vibrator and explore. There are many instructional videos on YouTube and on some adult film websites. -

Quick Reference Chart for Clinical Breast Examination Normal Breast Lump Change in Volume/Shape
Quick reference chart for clinical breast examination Clinical breast examination (CBE) Normal breast includes careful history-taking, visual inspection, palpation of both breasts, arm pits and root of the neck as well as educating women on breast self- examination and awareness, particularly on breast lumps. History-taking should include the following: 123 456age at menarche, marital status, parity, Normal female breasts: Note Lateral view of normal female breasts: Note Normal female breasts: Note Normal nippple Inverted nipple, horizontal age at first child birth, history of lactation similar size and shape, similar size and shape, nipples at the same similar size and shape, nipples and areola slit is a normal variation. It and breast-feeding, age at menopause, nipples at the same level, level, normal nipples, areola and skin at the same level, normal should not be diagnosed family history of breast and ovarian normal nipples, areola and nipples, areola and skin as retracted nipple as skin there is no underlying cancers in first degree relatives (mother, lump or other sign of sisters, aunts, grandmothers), history and breast cancer duration of oral contraceptive use, hormone replacement therapy (HRT), Lump treatment for infertility and tobacco use. After taking history, both breasts should be visually inspected, both in the sitting and lying down positions and with arms down and up, for any of the following: swelling, lumps, changes in size and shape, skin dimpling, skin retraction, skin thickening, 789101112skin nodules, skin ulceration, the level of Single, painless, hard lump in Single, painless, hard lump Painless, hard lump in the upper outer quadrant of the left Lobulated hard Large, lobulated hard both nipples, retraction of either nipple, the lower outer quadrant of in the lower quadrants of breast with restricted mobility. -

Genital Molluscum Contagiosum – Patient Information Leaflet
Genital molluscum contagiosum – Patient information leaflet Key points Genital molluscum contagiosum is a sexually transmitted infection. It is caused by the Molluscum contagiosum virus and is a benign skin infection. Diagnosis is established on clinical grounds. In healthy individuals, it usually resolves spontaneously in 6–12 months. Active treatment is required in case of patient preference and in selected cases. It is contagious, and the use of condoms is not always protective. What is genital molluscum contagiosum? ❖ Genital molluscum contagiosum is a sexually transmitted infection. It is caused by the Molluscum contagiosum virus which leads to a benign skin infection. How do you get genital molluscum contagiosum? ❖ Direct skin-to-skin contact during sexual intercourse is the most common way of transmitting genital Molluscum contagiosum. ❖ Other ways of transmission might include swimming or co-bathing and spread via the sharing of towels/sponges. ❖ Transmission to newborns during birth is also possible. What are the symptoms of genital molluscum contagiosum? ❖ Genital molluscum contagiosum may appear after 2 weeks or up to 6 months after contact. ❖ Lesions are dome-shaped, with smooth surface, pearly, skin-coloured, pink, yellow or white, 2–5 mm in diameter, firm, usually located on the external genitalia. ❖ Other affected regions may be the inguinal folds, the inner thighs or the suprapubic region, the areola and nipple, cervix, the oral mucosa or the palms and feet. ❖ Genital molluscum contagiosum is usually asymptomatic; local itch or discomfort may appear in some cases. ❖ Lesions may vary in number from 1 to hundreds and may appear grouped or in lines. Do I need any tests? ❖ Genital molluscum contagiosum is usually diagnosed on clinical grounds. -

Infant Feeding - Breast and Nipple Thrush
Guideline Infant Feeding - Breast and Nipple Thrush 1. Purpose This guideline provides details for the diagnosis and management of women with breast and nipple thrush (Candida) at the Women’s. This guideline/procedure is related to Breastfeeding Policy 2. Definitions Breast and nipple thrush is the over-growth of Candida species, on the nipples and in breast ducts, which can cause significant breast and nipple pain. There are over 20 species of Candida of which Candida albicans is the most common. 3. Responsibilities Maternity and neonatal medical, nursing and midwifery staff need awareness of the condition and to refer women to appropriate care. Lactation consultants and medical staff should be aware of the guideline and be able to treat accordingly. 4. Guideline 4.1 Breast and nipple thrush diagnosis The diagnosis of breast or nipple thrush is usually made after consideration of the mother’s symptoms; for example, mother may complain of ‘nipple pain’ that does not resolve despite improved attachment of the baby to the breast. The pain of maternal thrush infections may lead to early weaning, which can be avoided with early diagnosis and treatment. There may be a history of antibiotic treatment preceding thrush symptoms. This may have been prescribed postnatally, for example, to prevent infection following a caesarean section birth or for mastitis. The mother may have a past history of vaginal thrush. Nipple trauma commonly precedes nipple thrush symptoms. It is assumed that the break in the skin allows organisms to enter. 4.2 Signs and symptoms Nipple/areola Mother may describe burning, stinging nipple pain which continues during and after the feed. -

Breast Changes During Pregnancy
Breast Changes During Pregnancy During pregnancy, hormones in your body Areola enlarged, are preparing your breasts for lactation. nipple more sensitive You may experience enlargement of the breasts, nipples and areolas. The breast tissue may extend up into the armpit, and Montgomery glands some women may have additional breast tissue (accessory breast tissue) under Nipple the armpit. Areola You may find darkening of the nipples and areolas due to hormones that affect pigmentation of the skin. You may also find veins along your breasts more noticeable due to increased blood supply to your breasts. Small glands on the surface of the areolas called Montgomery’s tubercles will become raised bumps Tips Your breasts will continue to grow throughout the pregnancy. This can cause discomfort and sometimes pain. This can be helped by wearing a well-fitting bra. You may need to change your bra to fit the growth of your breasts every trimester. 54 The milk ducts are growing and being Anatomy of breast Early Pregnancy stretched as they fill with milk early in pregnancy. All this causes your breasts to be more sensitive, particularly your Chest muscle nipples. This may cause you discomfort. Lobes Ducts Nipple Fatty tissue Ribs Colostrum Your breasts may start leaking a yellowish, thick substance known as colostrum. It can happen as early as 14 weeks into your pregnancy. Women who do not experience colostrum secretion in pregnancy still produce milk for their baby after birth. When should you seek medical care? If you notice any of the following, it is advisable to seek medical advice: - new lumps - pain (especially if it locates at one place or gets worse) - redness - skin or nipple changes such as thickening, dimpling or ulcers - any coloured substance (other than colostrum) from your nipple - discrete lump in the armpit ( Please refer to the details of “Breast awareness” in FHS website at http://s.fhs.gov.hk/7g38e) 55 mniocent. -

Incest Is Best 4 Tuesday, September 29, 2009 [email protected]
Incest Is Best 4 Tuesday, September 29, 2009 [email protected] Bi Incest Adult Youth Mb Wb gg gb bb Wg Mb I am sure that I am going to hear from some poor soul that was looking for a powerful plot…not this chapter…sorry we have all of these beautiful characters with run-away sex drive that needs fulfillment. This chapter has 4 red hot love scenes…If you are looking for a heavy plot, then you might want to save this for another occasion. First we have the three beautiful 12 year olds united as one with a powerful love scene. Nine year old Becki feels left out and Devin senses her need and the 12 year old sex god makes passionate love to Becki. Bruce has always had a thing for beautiful boys. Imagine having alone time with an incredibly sexy 12 year old boy and being able to make wild passionate love to him…a dream come true for Bruce. Then Ted asks Jack if he has ever made love to a beautiful 9 year old girl. Megan’s reaction is interesting. She watches her handsome husband make love to this beautiful little girl. Please let me know if this is a story that you like and want it to continue at [email protected] and what it is that turns you on about the story. As always, if you are not supposed to be reading this story…then please don’t…please practice safe sex. This story is a total fantasy. Thanks to everyone who has taken the time to write me. -

Male and Female Nipples As a Test Case for the Assumption That Functional Features Vary Less Than Nonfunctional Byproducts
Male and Female Nipples as a Test Case for the Assumption that Functional Features Vary Less than Nonfunctional Byproducts Ashleigh J. Kelly, Shelli L. Dubbs, Fiona Kate Barlow & Brendan P. Zietsch Adaptive Human Behavior and Physiology e-ISSN 2198-7335 Adaptive Human Behavior and Physiology DOI 10.1007/s40750-018-0096-1 1 23 Your article is protected by copyright and all rights are held exclusively by Springer International Publishing AG, part of Springer Nature. This e-offprint is for personal use only and shall not be self-archived in electronic repositories. If you wish to self-archive your article, please use the accepted manuscript version for posting on your own website. You may further deposit the accepted manuscript version in any repository, provided it is only made publicly available 12 months after official publication or later and provided acknowledgement is given to the original source of publication and a link is inserted to the published article on Springer's website. The link must be accompanied by the following text: "The final publication is available at link.springer.com”. 1 23 Author's personal copy Adaptive Human Behavior and Physiology https://doi.org/10.1007/s40750-018-0096-1 ORIGINAL ARTICLE Male and Female Nipples as a Test Case for the Assumption that Functional Features Vary Less than Nonfunctional Byproducts Ashleigh J. Kelly1 & Shelli L. Dubbs1 & Fiona Kate Barlow1 & Brendan P. Zietsch1 Received: 19 April 2018 /Revised: 16 May 2018 /Accepted: 17 May 2018 # Springer International Publishing AG, part of Springer Nature 2018 Abstract Objectives Evolutionary researchers have sometimes taken findings of low variation in the size or shape of a biological feature to indicate that it is functional and under strong evolutionary selection, and have assumed that high variation implies weak or absent selection and therefore lack of function.