Trifascicular Block in Patient with Acute Coronary Syndrome
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Definition of Terms Related to Cardiac Rhythm*
EUROPEAN JOURNAL OF CARDIOLOGY, 1978, 8/2,127-144 127 © Elsevier/North-Holland Biomedical P:-ess Definition of terms related to cardiac rhythm* WHO/ISFC Task Force Etienne O. Robles de Medina (editor) Department of Cardiology, University Hospital, Utrecht Roland Bernard Intensive Care Research Group of the EEC Philippe Coumel French Society of Cardiology Anthony N. Damato American Heart Association Charles Fisch American College of Cardiology Dennis Krikier British Cardiac Society Nicolai A. Mazur Cardiological Society of the USSR Frits L. Meijler In teruniversity Cardiological Institute, The Netherlands Lars Mogensen Swedish Society of Cardiology Pierre Moret International Society and Federation of Cardiology Zbynek Pisa World Health Organization Hein J.J. Wellens European Society of Cardiology KEY WORDS : arrhythmias; cardiac electrogram; conduction disturbances ; electrocardio gram; electrocardiographic nomenclature I ntroduction In recent years several individuals and working groups have been con cerned with definition and classification of electrocardiographic findings. Both increasing international communication, exchange of data and intro- * Supported by a grant from the Dutch Heart Foundation. Reproduced with permission from Amer. Heart J., Vol. 95, pp. 796-806, 1978, copy righted by The C.V. Mosby company, St. Louis, MO, U.S.A. 128 duction of new techniques like computer aided interpretation of the electro cardiogram, have promoted the need for common language in electrocardiol ogy. Sponsored by the World Health Organization (WHO) and the International Society and Federation of Cardiology (ISFC), and financially supported by the Dutch Heart Foundation (DHF), this Task Force was composed of mem bers nominated by various cardiological societies. It has been engaged primar ily with the definition of terms related to cardiac rhythm. -

Triage EKG—Unit 7, Case 28
Triage EKG—Unit 7, Case 28 Courtesy of Edward Burns of Life in the Fast Lane Creative Commons License Unit 7, Case 28 - Bifascicular Block with 1st Degree AV Block What is your interpretation of the EKG? History/Clinical Picture— elderly woman with CHF who presents with syncope Rate— 70 Rhythm— Sinus rhythm Axis— left axis deviation P Waves— present Q, R, S Waves— no clear pathologic q waves, S-waves inferiorly and laterally, early R-wave progression T Waves— inversions inveriorly U Waves— not present PR Interval— consistently prolonged at 220 ms consistent with 1st Degree AV Block. No progressive prolongation that would be consistent with 2nd Degree Type I or intermittent dropped beats that would be consistent with 2nd Degree Type II QRS Width— prolonged at just over 120 ms with RBBB and LAFB RBBB: RSR’ in V1 and QRS > 120ms LAFB: 1. Left axis deviation 2. Small q waves with large R waves (“qR complexes”) in I and aVL 3. Small r waves with large S waves (“rS complexes”) in II, III, and aVF 4. Normal or slightly prolonged QRS duration(80 -110 ms). ST Segment— no marked elevation or depression QT Interval— normal Diagnosis: Bifascicular block (RBBB + LAFB) with first degree AV block Management: This EKG shows severe disease of the interventricular conduction system. A right bundle branch block with a left anterior fascicular block (or left posterior fascicular block) in the presence of a 1st degree AV nodal block is sometimes erroneously called a “trifascicular block”. Conduction between the atria and the ventricles is reliant on the remaining fasci- cle, in this case the left posterior fascicle. -

A Patient with Atrioventricular Block and Ventricular Tachycardia: Think Sarcoid! Suchit Majumdar1, Arindam Chatterjee2, Suvro Banerjee3
J R Coll Physicians Edinb 2020; 50: 284–6 | doi: 10.4997/JRCPE.2020.314 CASE REPORT A patient with atrioventricular block and ventricular tachycardia: think sarcoid! Suchit Majumdar1, Arindam Chatterjee2, Suvro Banerjee3 ClinicalCardiac involvement in sarcoidosis is often dif cult to diagnose, and most Correspondence to: alarmingly can lead to sudden cardiac arrest as its rst manifestation. We Suvro Banerjee Abstract report the case of a 45-year-old Indian woman with an implanted permanent Department of Cardiology pacemaker for atrioventricular block, who presented with haemodynamically Apollo Gleneagles Hospital stable ventricular tachycardia and was found to have impaired left ventricular 58 Canal Circular Road function. Subsequent investigations established the diagnosis of cardiac Kolkata 700 054 sarcoidosis. The patient was treated with prednisolone initially at 40 mg a day for 3 months. India Left ventricular function improved over 3 months of treatment and there was no further recurrence of ventricular tachycardia. Screening for cardiac sarcoidosis should be considered Email: in a patient with unexplained atrioventricular block and ventricular tachycardia, particularly if [email protected] young, even in the absence of clinical ndings of extracardiac sarcoidosis. Treatment of the cardiac sarcoidosis could control ventricular tachycardia and improve left ventricular function. Keywords: cardiac pacemaker, ventricular tachycardia, atrioventricular block, cardiac sarcoidosis, left ventricular function, imaging Financial and Competing Interests: No confl ict of interests declared Informed consent: Written informed consent for the paper to be published (including images, case history and data) was obtained from the patient for publication of this paper, including accompanying images. Introduction waves were seen in the jugular venous pulsation. -

Initial Management of Cardiac Arrhythmias
THEME ACUTE CARE Jaycen Cruickshank MBBS, FACEM, is Director of Emergency Medicine, Ballarat Health Services, and Lecturer, Rural Clinical School, School of Rural Health, University of Melbourne, Victoria. [email protected] Initial management of cardiac arrhythmias Diagnosis of arrhythmias can be a challenge, in particular Background if a patient has no symptoms and a normal electrocardiogram Diagnosis of acute arrhythmias requires recognition and (ECG) between symptomatic episodes. Ideally, the patient interpretation of important electrocardiogram (ECG) findings, and should be managed in an area with access to ECG monitoring, knowledge of Australian resuscitation guidelines. oxygen and an external defibrillator. Acute arrhythmias may Objective require urgent intervention including resuscitation. All clinical This article aims to provide a guide for general practitioners in staff should be trained in basic life support (BLS) and managing patients who present with acute arrhythmias in the advanced life support (ALS) (see Resource). rural or regional setting. Discussion Assessment of the patient with an abnormal rhythm Rural GPs need to be familiar with acute management of History bradycardias, supraventricular tachycardia, atrial fibrillation Cardiac arrhythmia is an important differential diagnosis in any and ventricular tachyarrhythmias, despite the fact that they patient with palpitations, syncope, near syncope or chest pain. may deal with these problems infrequently. A good local or Palpitations are a sensitive but not particularly specific symptom of regional network will help determine which patients can be arrhythmias. They are usually of benign origin. An association with treated locally, versus the need to refer to a hospital emergency 1 department or outpatient setting. This might include a colleague syncope, near syncope or dizziness, is more worrying. -

View Pdf Copy of Original Document
Phenotype definition for the Vanderbilt Genome-Electronic Records project Identifying genetics determinants of normal QRS duration (QRSd) Patient population: • Patients with DNA whose first electrocardiogram (ECG) is designated as “normal” and lacking an exclusion criteria. • For this study, case and control are drawn from the same population and analyzed via continuous trait analysis. The only difference will be the QRSd. Hypothetical timeline for a single patient: Notes: • The study ECG is the first normal ECG. • The “Mildly abnormal” ECG cannot be abnormal by presence of heart disease. It can have abnormal rate, be recorded in the presence of Na-channel blocking meds, etc. For instance, a HR >100 is OK but not a bundle branch block. • Y duration = from first entry in the electronic medical record (EMR) until one month following normal ECG • Z duration = most recent clinic visit or problem list (if present) to one week following the normal ECG. Labs values, though, must be +/- 48h from the ECG time Criteria to be included in the analysis: Criteria Source/Method “Normal” ECG must be: • QRSd between 65-120ms ECG calculations • ECG designed as “NORMAL” ECG classification • Heart Rate between 50-100 ECG calculations • ECG Impression must not contain Natural Language Processing (NLP) on evidence of heart disease concepts (see ECG impression. Will exclude all but list below) negated terms (e.g., exclude those with possible, probable, or asserted bundle branch blocks). Should also exclude normalization negations like “LBBB no longer present.” -

Radiofrequency Catheter Ablation for Treatment of Bundle Branch Reentrant Ventricular Tachycardia : Results and Long-Term Follow-Up TODD J
15CC Vel . la. Nn. 7 1767 D- robe, 1991 :1767-A Radiofrequency Catheter Ablation for Treatment of Bundle Branch Reentrant Ventricular Tachycardia : Results and Long-Term Follow-Up TODD J . COHEN . MD, WALTER W . CHIEN . M D . KEITH G . LURIE, MD, CHARLIE YOUNG, MD, FACC . HAROLD F . GOLDBERG, MD, FACC, YIN-SHI W ANG . M D. JONATHAN J . LANGBERG, MD. FACC, MICHAEL D. LESH . MD, FACC, MICHAEL A . LEE, MD, JERRY C . GRIFFIN, MD . FACC . MELVIN M . SCHEINMAN . MD, FACC San Francisco, California Seven of 120 consecutive patients with inducible sustained ventric . vclve with the distal electrode tip of the catheter near the right ular tachycardia (from September 1 . 1988 to January 1, 1991) had bundle branch . One to three applications of continuous nemndu- bundle branch reentrant tachycardia and underwent percutane . lated radiofrequency current at 300 kHz between the distal tuts radiofrequency ablation of the right bundle branch. The seven electrode and a large posterior skin patch resulted in complete patients had been unsuccessfully treated with a mean of 3 ± t right bundle branch block in all patients, after which none had drugs. Four patients presented with syncope and three with inducible bundle branch reentrant tachycardia on restudy. On aborted sudden death. The baseline electrocardiogram revealed a restudy, three of the seven patients had ventricular tacbycardia of left bundle branch black pattern in three patients and an intro. myocardial origin (not bundle branch reentry). One patient ventricular conduction defect in four. required no therapy ; drug re defibrillator therapy was used in the The baseline HV interval was prolonged in each case (79 z others. -

LBBB, RBBB, Bifascicular, Trifascicular Block
10/18/2019 Section 5 LBBB, RBBB Bifascicular, Trifascicular Block Objectives • At the conclusion of this presentation the participant will be able to – Outline a systematic approach to 12 lead ECG interpretation – Dysrhythmias – Demonstrate the process for determining axis – List criteria for LVH, RVH, RAE, LAE LBBB, RBBB, Bifasicular and trifasicular block, acute and chronic MI changes – Define QTc significance and other EKG Abnormalities 10/18/2019 2 Bundle Branches • Bundle of His divides into right and left bundle branches • Left bundle branch divides into septal, anterior and posterior fascicles I 10/18/2019 3 1 10/18/2019 Conduction Abnormalities BBB • Causes of BBB • Arterial occlusion total • Arterial occlusion partial • Structural changes Helpful hints r/t BBB ST segment and the T wave are opposite deflection of QRS If T waves same deflection, may mean ischemia 10/18/2019 4 Normal QRS Complex • Narrow ‐ < 0.12 seconds in duration • Electrical axis between 0° and +90° I 10/18/2019 5 QRS Interval/Bundle Branch Block Assess QRS Duration 1. QRS duration can be measured from any of the 12 leads 2. All that matters is whether the QRS is normal or wide 3. Judge QRS prolongation from the lead where the QRS appears longest 10/18/2019 6 2 10/18/2019 QRS Interval/Bundle Branch Block Assess QRS Duration cont. 4. If the QRS is: < 0.12 seconds than the QRS is normal > 0.12 seconds than the QRS is wide (greater than half a large box) 5. The limits given do not hold for children 10/18/2019 7 Bundle Branch Block • Leads to one or both bundle -

Transient Trifascicular Block in Severe Hyperkalemia: a Case Report
Medical Case Studies Vol. 2(5), pp. 44-46, August 2011 Available online at http://www.academicjournals.org/MCS ISSN 2141-6532 ©2011 Academic Journals Case Report Transient trifascicular block in severe hyperkalemia: A case report AGARWAL Navnit, SINGH Anurag, GABA Ripudaman*, SHUKLA Ranjeet, AGARWAL Mandavi and JAISWAL Pankaj Department of Medicine, MLB Medical College, Jhansi Uttar Pradesh, 284128, India. Accepted 17 June, 2011 Hyperkalemia is a commonly encountered electrolyte abnormality that can significantly alter normal cardiac conduction. Potentially lethal dysrhythmias associated with hyperkalemia include complete heart block and Mobitz type II second-degree atrioventricular (AV) block. We report a case of trifascicular block, due to hyperkalemia. The patient's symptoms and electrocardiogram (ECG) evidence of trifascicular block resolved with lowering of serum potassium levels, with subsequent ECG showing left anterior hemiblock. This paper highlights an infrequently reported dysrhythmia associated with hyperkalemia that emergency physicians should be familiar with. Key words: Hyperkalemia, trifascicular block, right bundle branch block, left anterior fascicular block, first degree AV block, isoprenaline, hemodialysis, emergency. INTRODUCTION Hyperkalemia is life threatening electrolyte abnormality interval lengthening and QRS widening (Bashour et al., requiring urgent management. Serum potassium levels 1975). Reversible fascicular blocks, as well as bundle greater than 5.5 mmol/l is considered hyperkalemia. branch blocks or intraventricular conduction delay can be Hyperkalemia is a common and potentially life- seen. Moreover, hyperkalemia is known to cause threatening electrolyte abnormality (Sood et al., 2007). potentially lethal dysrhythmias including ventricular Hyperkalemia is often asymptomatic until plasma tachycardia, ventricular fibrillation, idioventricular potassium concentration is above 6.5-7 mmol/L when it rhythms, and asystole (Alfonzo et al., 2006; Sood et al., results in fatal arrhythmias, hence it’s called silent killer. -

Trifascicular Heart Block, Genetically Inherited Or Hyperkalemia-Induced; a Rare Case Report
Journal of Cardiology & Current Research Clinical Images Open Access Trifascicular heart block, genetically inherited or hyperkalemia-induced; a rare case report Abstract Volume 11 Issue 6 - 2018 We report a case of trifascicular block with hyperkalemia, due to a familial heart 1, 4 block and/or hyperkalemia. The patient’s symptoms and electrocardiogram (ECG) Seyyed-Mohsen Hosseininejad , Fateme- *2 1 evidence of trifascicular block resolved with correcting serum potassium level. This Sadat Hosseininejad , Kourosh Ghamsari , patient was also diagnosed with a progressive familial heart block (PFHB) type I. This Negin Akbari3, Mansoor Mirza’ali3 would be the first report of a PFHB type I documented in Iran; this paper highlights 1Student Research Committee, Golestan University of Medical an infrequently reported dysrhythmia associated with hyperkalemia which emergency Sciences, Gorgan, Iran. physicians should be familiar with. 2Student Research Committee, School of Public Health, Shahroud University of Medical Sciences, Shahroud, Iran. Keywords: hyperkalemia, trifascicular block, hereditary bundle branch system 3Clinical Research Development Unit (CRDU), Sayad Shirazi defect Hospital, Golestan University of Medical Sciences, Gorgan, Iran. 4North Khorasan University of Medical Sciences, Bojnurd, Iran. Correspondence: Fateme-Sadat Hosseininejad, School of Public Health, Shahroud University of Medical Sciences, Shahroud, Iran, Email Received: July 03, 2018 | Published: November 19, 2018 Introduction electrocardiogram showed heart rate of 78/min, PR interval of 253milli-sec, and QRS duration of 144milli-sec with mean QRS axis Progressive familial heart block (PFHB) type I am an autosomal which was 264°. ECG showed as trifascicular block i.e. first degree dominant congenital cardiac conduction disorder which might atrioventricular (AV) block, right bundle branch block (RBBB), left 1 develop into complete atrioventricular (AV) heart block. -

Intraventricular Trifascicular Block Bundle-Branch System
British I971, 33, 626-628. Heart_Journal, Br Heart J: first published as 10.1136/hrt.33.4.626 on 1 July 1971. Downloaded from Intraventricular trifascicular block Observations on conduction disturbance in bundle-branch system Nabil El-Sherif From the Cardiology Department, Faculty of Medicine, Cairo University, Cairo, Egypt, U.A.R. A case of intraventricular trifascicular block secondary to an inferior myocardial infarction is reported. The case denonstrates instances of 2: I atrioventricular conduction due to alternating block in the right bundle-branch and block in the right bundle and both anterior and posterior divisions of the left bundle (trifascicular block). Instances of I: i A V conduction with grade I block and periods of type I (Mobitz) block are ascribed to a delayed and a Wenckebach type of conduction respectively in the posterior division of the left bundle. Recent recognition of the trifascicular nature but experienced two separate attacks of fainting of the bundle-branch system has changed sensation not mounting to actual syncope within some of the concepts about AV conduction I2 hours and suddenly expired 24 hours later. disturbances and the pathways of impulse Description of cardiogram (Fig.) The record propagation in the ventricular myocardium. reveals two different QRS patterns and three In a recent review by Rosenbaum et al. (I969) types of AV conduction disturbance. no more than 20 cases of intraventricular The first QRS pattern (type A) is always pre- http://heart.bmj.com/ trifascicular block were found while the ceded by a normal PR interval of O-I9 sec and has authors recognized the various combinations a duration of O'i2 sec. -
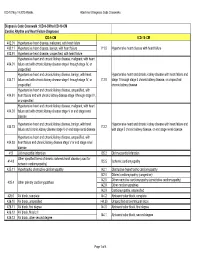

ICD-10 May 19 2015 Webex Attachment Diagnosis Code Crosswalks
ICD-10 May 19 2015 WebEx Attachment Diagnosis Code Crosswalks Diagnosis Code Crosswalk : ICD-9-CM to ICD-10-CM Cardiac Rhythm and Heart Failure Diagnoses ICD-9-CM ICD-10-CM 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure I11.0 Hypertensive heart disease with heart failure 402.91 Hypertensive heart disease, unspecified, with heart failure Hypertensive heart and chronic kidney disease, malignant, with heart 404.01 failure and with chronic kidney disease stage I through stage IV, or unspecified Hypertensive heart and chronic kidney disease, benign, with heart Hypertensive heart and chronic kidney disease with heart failure and 404.11 failure and with chronic kidney disease stage I through stage IV, or I13.0 stage 1 through stage 4 chronic kidney disease, or unspecified unspecified chronic kidney disease Hypertensive heart and chronic kidney disease, unspecified, with 404.91 heart failure and with chronic kidney disease stage I through stage IV, or unspecified Hypertensive heart and chronic kidney disease, malignant, with heart 404.03 failure and with chronic kidney disease stage V or end stage renal disease Hypertensive heart and chronic kidney disease, benign, with heart Hypertensive heart and chronic kidney disease with heart failure and 404.13 I13.2 failure and chronic kidney disease stage V or end stage renal disease with stage 5 chronic kidney disease, or end stage renal disease Hypertensive heart and chronic kidney disease, unspecified, with 404.93 heart -
Impulse Conduction
MODULEMODULE 11 RhythmRhythm BasicsBasics ModuleModule 1:1: RhythmRhythm BBaasicssics OverviewOverview •• TheThe ConductionConduction SystemSystem –– ImpulseImpulse FormationFormation –– ImpulseImpulse ConductionConduction –– PropertiesProperties ofof CardiacCardiac FunctionFunction –– 55 PhasesPhases ofof ActionAction PotentialPotential •• RhythmRhythm DisordersDisorders –– MechanisMechanismsms –– ArrhythmArrhythmiaia RecognitionRecognition •• CausesCauses ofof RhythmRhythm DisordersDisorders ModuleModule 1:1: RhythmRhythm BBaasicssics ObjectivesObjectives •• IdentifyIdentify thethe componentscomponents thatthat makemake upup thethe electricalelectrical pathwaypathway knownknown asas thethe conductionconduction systemsystem •• StateState thethe 55 phasesphases ofof actionaction potentialpotential •• DescribeDescribe thethe mechanismsmechanisms causingcausing rhythmrhythm disordersdisorders •• IdIdentifyentify rhythmrhythm ddiisorderssorders onon anan EKGEKG THETHE CONDUCTIONCONDUCTION SYSTEMSYSTEM HeartHeart BeBeatat AnatomyAnatomy SINUS NODE • The Heart’s ‘Natural Pacemaker’ Sinus Node (SA Node) - 60-100 BPM at rest HeartHeart BeBeatat AnatomyAnatomy AV NODE • Receives impulse from Sinus Node SA Node (SA Node) • Delivers impulse to the His- Purkinje System Atrioventricular Node (AV Node) • 40-60 BPM if SA Node fails to deliver an impulse HeartHeart BeBeatat AnatomyAnatomy BUNDLE OF HIS •Begins conduction to Sinus Node the Ventricles (SA Node) • AV Junctional Tissue: 40-60 BPM Atrioventricular Node (AV Node) Bundle of His HeartHeart